State Health Agency Uttar Pradesh Ayushman Bharat Capacity

State Health Agency – Uttar Pradesh Ayushman Bharat Capacity Building Presentation
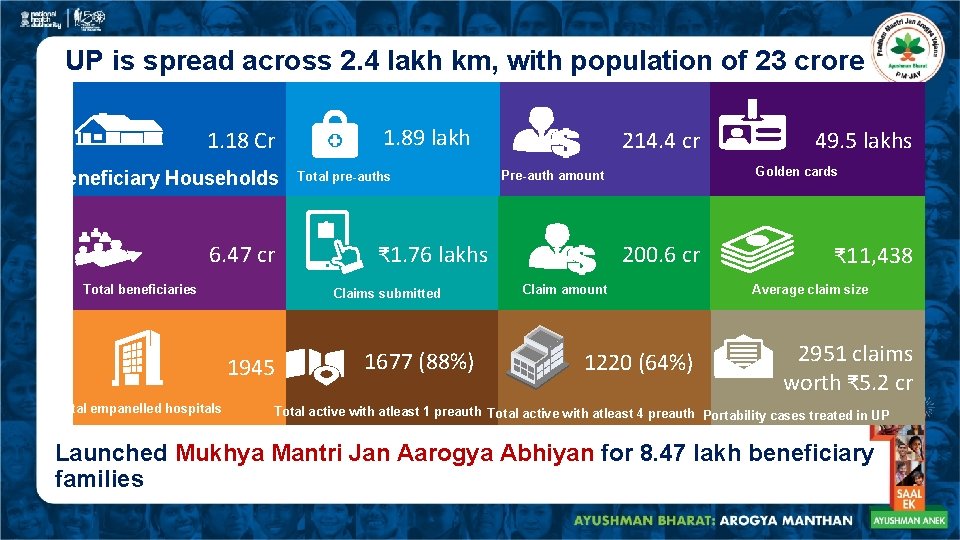
UP is spread across 2. 4 lakh km, with population of 23 crore 1. 18 Cr Beneficiary Households 6. 47 cr Total beneficiaries Total pre-auths 214. 4 cr 1677 (88%) 49. 5 lakhs Golden cards Pre-auth amount ₹ 1. 76 lakhs Claims submitted 1945 Total empanelled hospitals 1. 89 lakh 200. 6 cr Claim amount 1220 (64%) ₹ 11, 438 Average claim size 2951 claims worth ₹ 5. 2 cr Total active with atleast 1 preauth Total active with atleast 4 preauth Portability cases treated in UP Launched Mukhya Mantri Jan Aarogya Abhiyan for 8. 47 lakh beneficiary families

What makes Uttar Pradesh unique for PMJAY implementation? 1 Ayushman Implementation is Greenfield 2 Shares border with 8 States 3 Widespread Geographical and Cultural Differences 4 Large number of districts (75) 5 For PMJAY implementation, state divided into 4 clusters 66 SHA operates through not 1 but 4 ISAs given the large size of UP 7 Time taken to travel extent of State is >=2 days

2 How does Uttar Pradesh approach Capacity Building Assessment? 1 • Primary Training Conducted for all Stakeholders 2 • Gaps are then identified both from inputs received and on-scheme performance 3 • Accordingly, requests are raised for training modules/changes in software 4 5 l • Training Calendar is then prepared • Requires huge effort in communication for small changes • Quantum of stakeholders and widespread geography • Eg: DMR form requirement was abolished • State Training Calendar • Trainings related to on-ground fraud management • Maintenance of capacity-related metrics at SHA level

2 A Identified Stakeholder Gaps - resolved by training Arogya Mitra • • Low Technical Knowledge Errors in document upload Wrong package selection High Attrition Rate additional trainings • Data from 2011 - multiple requests for name change • Soft Skills to be developed ISA • Constant handholding reqd (high attrition) • Multiple cases of erroneously approved cases • Weak on technical strength • Lack of standard operating protocols Private and Public EHCPs • Regular Trainings to Newly added EHCPs • Issue with package cost • Issues with procurement & usage of drugs and logistics • Lack of standard treatment guideline • Lack of Infra and permanent AM staff (Public)
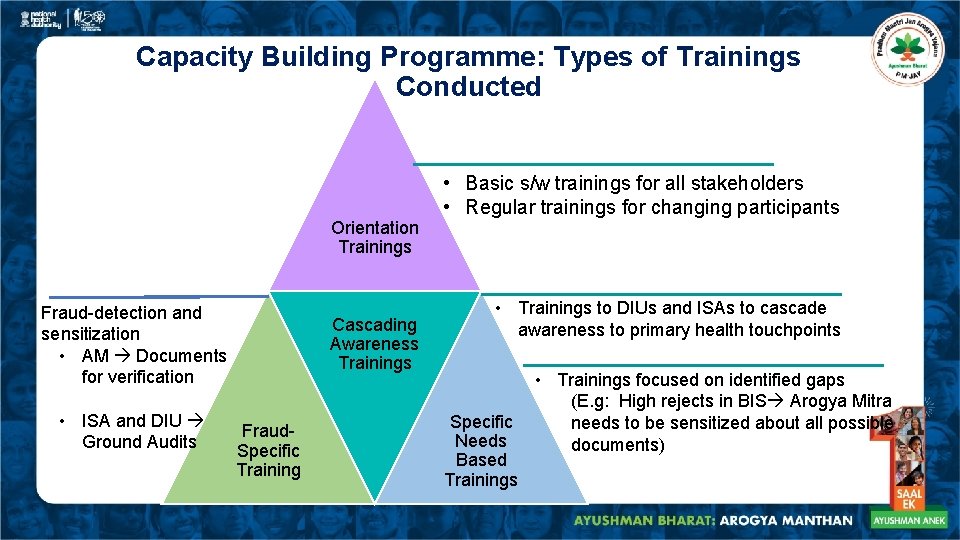
Capacity Building Programme: Types of Trainings Conducted Orientation Trainings Fraud-detection and sensitization • AM Documents for verification • ISA and DIU Ground Audits Cascading Awareness Trainings Fraud. Specific Training • Basic s/w trainings for all stakeholders • Regular trainings for changing participants • Trainings to DIUs and ISAs to cascade awareness to primary health touchpoints Specific Needs Based Trainings • Trainings focused on identified gaps (E. g: High rejects in BIS Arogya Mitra needs to be sensitized about all possible documents)

Best Practices of UP SHA Overall and Capacity-Specific
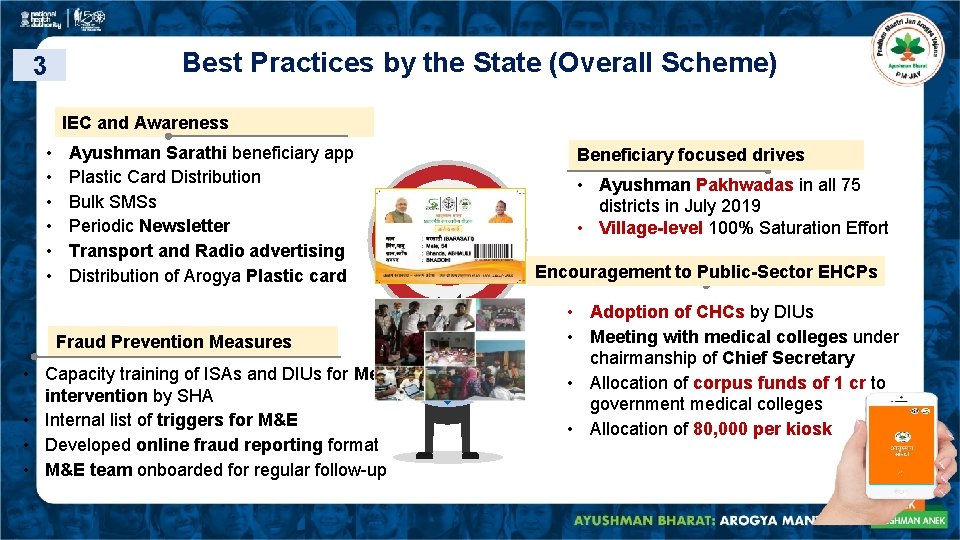
3 Best Practices by the State (Overall Scheme) IEC and Awareness • • • Ayushman Sarathi beneficiary app Plastic Card Distribution Bulk SMSs Periodic Newsletter Transport and Radio advertising Distribution of Arogya Plastic card Fraud Prevention Measures • Capacity training of ISAs and DIUs for Medical intervention by SHA • Internal list of triggers for M&E • Developed online fraud reporting format • M&E team onboarded for regular follow-up Beneficiary focused drives • Ayushman Pakhwadas in all 75 districts in July 2019 • Village-level 100% Saturation Effort Encouragement to Public-Sector EHCPs • Adoption of CHCs by DIUs • Meeting with medical colleges under chairmanship of Chief Secretary • Allocation of corpus funds of 1 cr to government medical colleges • Allocation of 80, 000 per kiosk
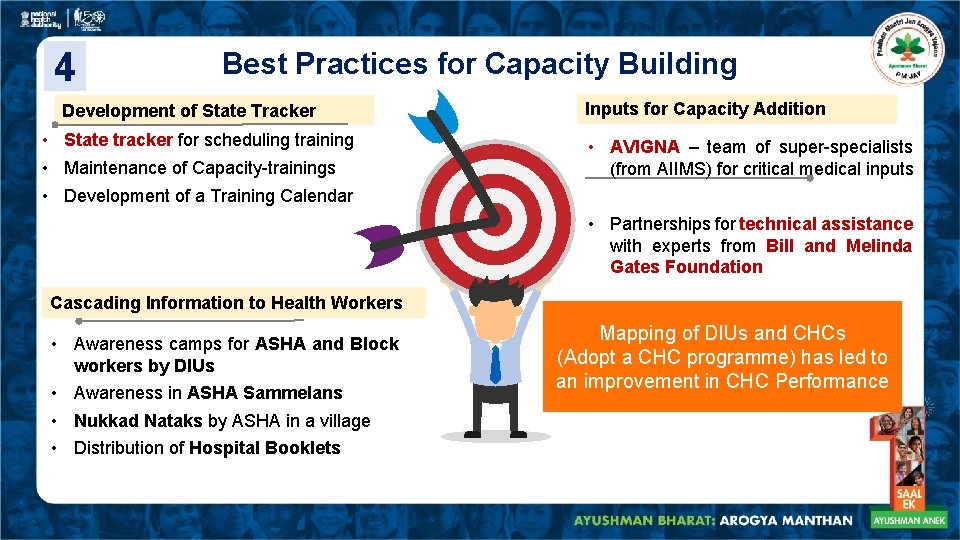
4 Best Practices for Capacity Building Development of State Tracker • State tracker for scheduling training • Maintenance of Capacity-trainings • Development of a Training Calendar Inputs for Capacity Addition • AVIGNA – team of super-specialists (from AIIMS) for critical medical inputs • Partnerships for technical assistance with experts from Bill and Melinda Gates Foundation Cascading Information to Health Workers • Awareness camps for ASHA and Block workers by DIUs • Awareness in ASHA Sammelans • Nukkad Nataks by ASHA in a village • Distribution of Hospital Booklets Mapping of DIUs and CHCs (Adopt a CHC programme) has led to an improvement in CHC Performance

4 A Uttar Pradesh has undertaken a total of 150+ trainings across >=3 rounds for each stakeholders Nodal Officers Training presided by CEO and JD SHA Direct Trainings in Govt Medical Colleges by SHA (15) Private EHCPs (All empaneled given hands-on training) • District Manager of VLEs and District Program Manager (DPM) DIUs from all 75 districts were trained twice at state office Cluster-wise ISA trainings by SHA Weekly Reviews 700 Arogya Mitras trained through NSDC -programmes Other Field Functionaries – ASHA, An. Ms, TB Health Worker, Anganwadi, DCPM, BMC, DMC
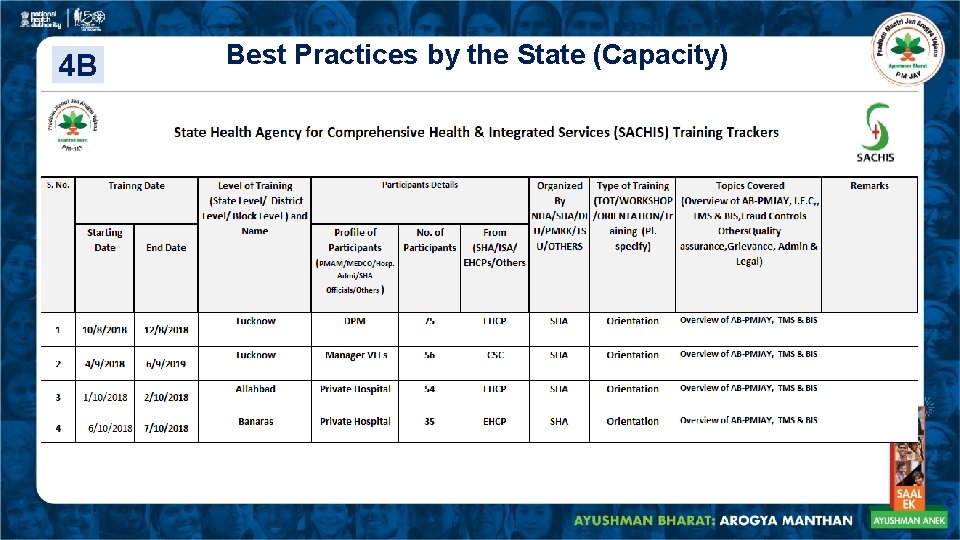
4 B Best Practices by the State (Capacity)
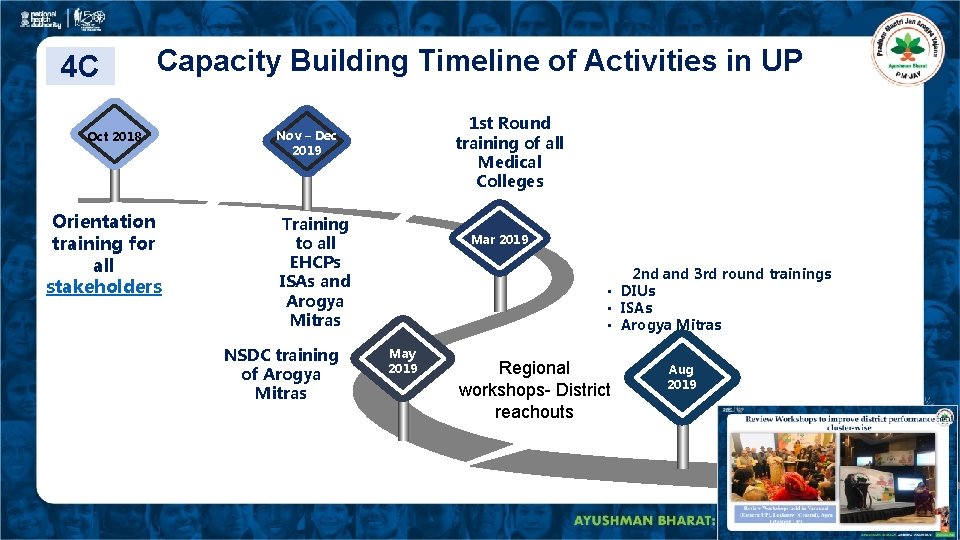
4 C Capacity Building Timeline of Activities in UP Oct 2018 Orientation training for all stakeholders 1 st Round training of all Medical Colleges Nov – Dec 2019 Training to all EHCPs ISAs and Arogya Mitras NSDC training of Arogya Mitras Mar 2019 2 nd and 3 rd round trainings • DIUs • ISAs • Arogya Mitras May 2019 Regional workshops- District reachouts Aug 2019

Case Study: Medical Colleges given specific trainings to resolve grievances • Medical Colleges faced a host of operational issues w. r. t scheme implementation • 15 Medical colleges trained to improve the pre authorization and claim processing • Process Flow to be followed from all department • Hands on training for BIS and TMS software • Resolving queries in claim processing which increased flow of cases

Impact of SHA-adopted Initiatives Number of Rejections Reduced in BIS/TMS Beneficiary Satisfaction recorded as 95% Less Grievances Registered Reduction in queries posed by CPD and Auditors Greater empanelment and participation of public health facilities Claim payment disposal increased by 30% to 75% Minimal Fraud recorded

Way Forward • Capacity Building of all new EHCPs and Arogya Mitras • Round-Table Conference with Top-Tertiary Care Hospitals • Orientation for new Bronze Certification programme introduced by NHA • Exploration of potential partnerships with progressive health academia and think -tanks (e. g Gramvani) • Awareness and outreach with Gram Pradhans in Villages through PRI dept • Trainings of Anganwadi workers in unexplored districts • Distribution of Hospital Booklets to Field Functionaries

Thank you

Case Study: Field Officers train other health workers • Asha Workers are the primary touch points for all health-related queries in villages • Hence, their awareness is of primary importance for the scheme to run smoothly Return

Review Workshops to improve district performance held cluster-wise Review Workshops held in Varanasi (Eastern UP), Lucknow (Central), Agra (Western UP) Return Slide
- Slides: 18