ST P CHRONIC BACK PAIN Selfmanagement and Timely

ST P! CHRONIC BACK PAIN Self-management and Timely Intervention: An Opportunity for the Prevention of Chronic Back Pain

STOP! CHRONIC BACK PAIN

T Das F n U i z H r D e , h t s e i M log o h c y s P l t i a c n i U n i l t C n e d e m r age n a Charte M n i a P et s r o D , ty i d s a r e e L v l i a n c i U n i h Cl ut o m e n r u o , B w o l l e F g n i t Visi ale d l O a r a b t r s i Ba p a r e h T l ona i t a p u c c O Senior rr a C e n i l o r Ca r o s i v d A r e Service Us ps i l l i h P r e h Christop r o s i v d A t n e Pati STOP! CHRONIC BACK PAIN

STOP! CHRONIC BACK PAIN

1. Our challenge : local and national conditions STOP! CHRONIC BACK PAIN

PAIN “An unpleasant sensory and emotional experience associated with real or potential tissue damage, or described in terms of such damage. . . ” -International Association for the Study of Pain Musculo-skeletal pain – BACK PAIN Neuropathic pain Post-surgical pain Idiopathic pain STOP! CHRONIC BACK PAIN

THE HORRIFYING CURRENT SITUATION 7. 8 million people in UK suffer from chronic pain. 3. 3 m people p. a. with first episode back pain don’t recover. . . Actual cost to the NHS is over £ 1 billion p. a. (Manadiakis, 2000) 4. 6 m GP appointments + 796, 000 pain management appointments each year (Belsey 2002) 25% of all appointments are cancelled or missed by patients £ 584 million for medication which includes wastage for noncompliance (2007) STOP! CHRONIC BACK PAIN

TRADITIONAL CARE PATHWAY FOR PEOPLE IN CHRONIC NON-MALIGNANT PAIN GP: ANALGESICS & PHYSICAL THERAPY INTERVENTION IF APPROPRIATE, ESCALATE ANALGESIA REFER TO PAIN CLINIC ABOUT YOUR BACK PROGRAMME OR EQUIVALENT REFERRAL TO RHEUMATOL OGY PAIN MANAGEMENT PROGRAMME RETURN TO GP SEEK INVESTIGATIO N REVIEW STOP! CHRONIC BACK PAIN

CONSTANTLY WORKING AT IMPROVEMENT. . STOP! CHRONIC BACK PAIN

STOP! CHRONIC BACK PAIN 2. So here’s what we did. .

PARTNER ORGANISATIONS THROUGH THE DORSET PAIN SOCIETY Poole Hospital NHS Foundation Trust: Dorset Pain Management Unit Self-help group of the Dorset Pain Management Unit Physiotherapy Department Bournemouth University: School of Health and Social Care Dorset Health. Care University NHS Foundation Trust (DHUFT): Orthopaedic Treatment Service Buckland Centre Volunteer Service University Department of Mental Health Royal Bournemouth and Christchurch Hospitals NHS Foundation Trust: Physiotherapy Department NHS Dorset Providence Surgery, Bournemouth Pfizer BHLive STOP! CHRONIC BACK PAIN

Physical pain Anger, frustration minishing self nfidence cial ation Loss of occupation CHRONIC BACK PAIN Increased visits to clinics Depression, hopelessness, helplessness Trapped in one’s body Reduced well -being Fear and Redu P D P s e s Changing role within family

3 CENTRES, 3 LOCATIONS 1 2 3 Coh ort Setting Date of delivery Number recruited completed 1 Dorset Pain Management Unit, Poole Hospital, Poole 15/06/11 – 8 7 2 Littledown Leisure Centre, Bournemouth 12/10/11 - 30/11/11 14 12 13 13 3 27/7/11 Weymouth Community Hospital, 08/02/12 – 21/3/12 Weymouth STOP! CHRONIC BACK PAIN
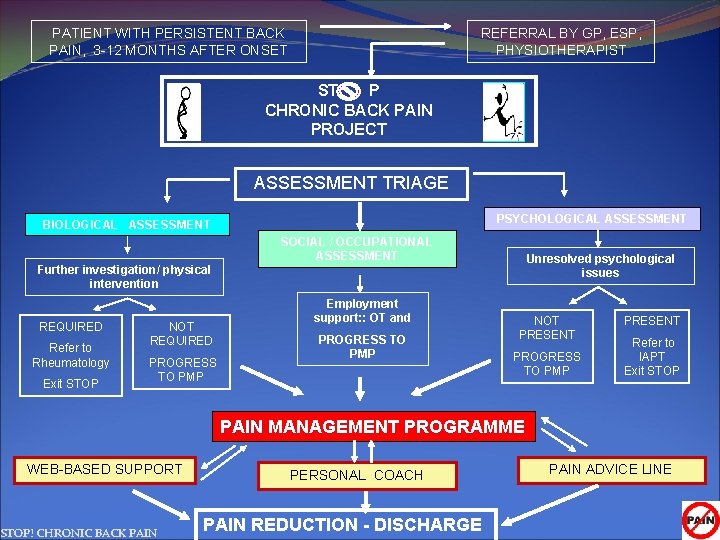
PATIENT WITH PERSISTENT BACK PAIN, 3 -12 MONTHS AFTER ONSET REFERRAL BY GP, ESP, PHYSIOTHERAPIST ST P CHRONIC BACK PAIN PROJECT ASSESSMENT TRIAGE PSYCHOLOGICAL ASSESSMENT BIOLOGICAL ASSESSMENT SOCIAL / OCCUPATIONAL ASSESSMENT Unresolved psychological issues Further investigation/ physical intervention REQUIRED Refer to Rheumatology Exit STOP Employment support: : OT and NOT REQUIRED PROGRESS TO PMP NOT PRESENT PROGRESS TO PMP PRESENT Refer to IAPT Exit STOP PAIN MANAGEMENT PROGRAMME WEB-BASED SUPPORT STOP! CHRONIC BACK PAIN PERSONAL COACH PAIN REDUCTION - DISCHARGE PAIN ADVICE LINE
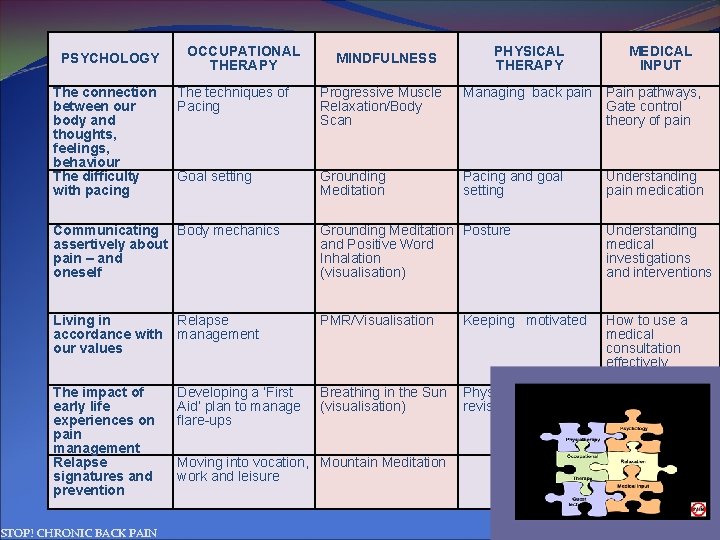
PSYCHOLOGY The connection between our body and thoughts, feelings, behaviour The difficulty with pacing OCCUPATIONAL THERAPY MINDFULNESS PHYSICAL THERAPY MEDICAL INPUT The techniques of Pacing Progressive Muscle Relaxation/Body Scan Managing back pain Pain pathways, Gate control theory of pain Goal setting Grounding Meditation Pacing and goal setting Understanding pain medication Communicating Body mechanics assertively about pain – and oneself Grounding Meditation Posture and Positive Word Inhalation (visualisation) Understanding medical investigations and interventions Living in accordance with our values Relapse management PMR/Visualisation How to use a medical consultation effectively The impact of early life experiences on pain management Relapse signatures and prevention Developing a ‘First Aid’ plan to manage flare-ups Breathing in the Sun Physiotherapy (visualisation) revisited STOP! CHRONIC BACK PAIN Moving into vocation, Mountain Meditation work and leisure Keeping motivated
SUPPORTED SELF-MANAGEMENT TIER 1 : WEB SUPPORT STOP! CHRONIC BACK PAIN

SUPPORTED SELF-MANAGEMENT TIER 2 TIER 3 OUR INNOVATIVE PAIN CHAIN EACH ONE REACH ONE STOP! CHRONIC BACK PAIN ADVICE LINE STAFF-MANNED TELEPHONE LINE

WHAT WERE WE HOPING TO ACHIEVE THROUGH EARLY INTERVENTION? The Individual with pain Reduced disability – physical + emotional Enhanced quality of life The Clinical Team Collaborative working Better self-management, earlier in the journey The Commissioners Decreased dependence on health/social services Affordable health economy through prevention of chronicity STOP! CHRONIC BACK PAIN

3. Measurement and outcomes STOP! CHRONIC BACK PAIN

OUTCOME DATA A. CLINICAL OUTCOMES B. COST EFFECTIVENESS – HEALTH ECONOMY C. QUALITATIVE FEEDBACK STOP! CHRONIC BACK PAIN
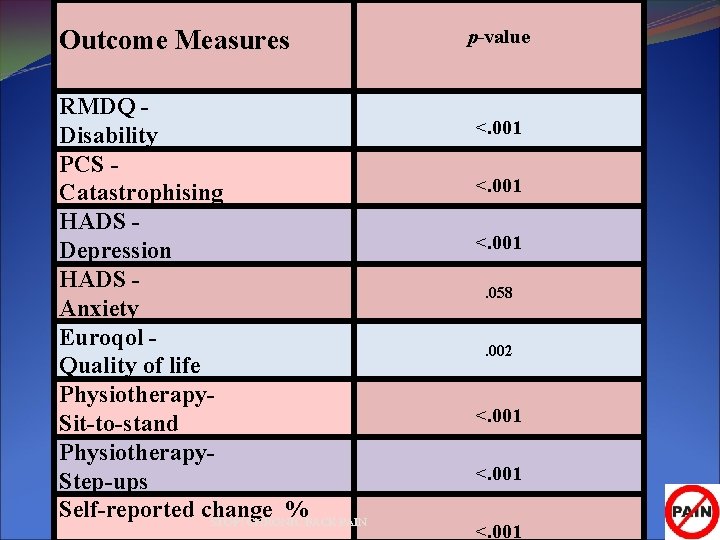
Outcome Measures RMDQ Disability PCS Catastrophising HADS Depression HADS Anxiety Euroqol Quality of life Physiotherapy. Sit-to-stand Physiotherapy. Step-ups Self-reported change % STOP! CHRONIC BACK PAIN p-value <. 001. 058. 002 <. 001
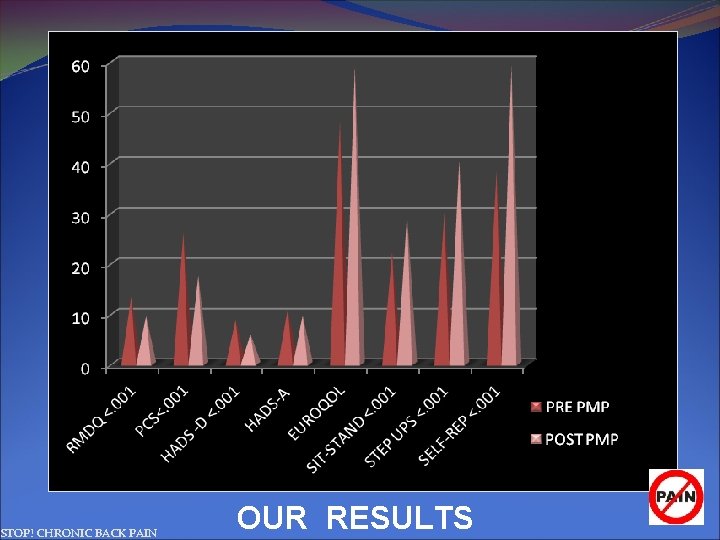
STOP! CHRONIC BACK PAIN OUR RESULTS

OUTCOME DATA A. CLINICAL OUTCOMES B. COST EFFECTIVENESS – HEALTH ECONOMY: YUHASS questionnaire C. QUALITATIVE FEEDBACK STOP! CHRONIC BACK PAIN

Total Number of Appointments for each type of HCP across 30 patients in 3 months STOP! CHRONIC BACK PAIN

Appointment costs per patient in 3 months, one bar per patient STOP! CHRONIC BACK PAIN

Total Appointment Cost per profession across 30 patients in 3 months STOP! CHRONIC BACK PAIN

Number of medicines used by each patient STOP! CHRONIC BACK PAIN

Type of paid household help used in 3 months STOP! CHRONIC BACK PAIN

OUTCOME DATA A. CLINICAL OUTCOMES B. COST EFFECTIVENESS – HEALTH ECONOMY C. QUALITATIVE FEEDBACK: forms, interviews STOP! CHRONIC BACK PAIN

“I thought that the actual programme was very good. It covered a lot of things, we had questions raised and they were addressed, I think they got it spot on with the content. ” Programme participant “The pain chain was lovely. It worked well for me – it’s still a pleasure to work with my coach”. Programme participant “As a service user I was thrilled to have a chance to promote the patients' perspective and work with health professionals who impressed me throughout with their compassion, professionalism and determination to meet their patients’ needs. Caroline, Service User Advisor STOP! CHRONIC BACK PAIN “Life has changed. Can move around better. Still some pain. But I’ve now got a part time job. ” Programme participant

STOP! CHRONIC BACK PAIN

4. Sharing Our learning STOP! CHRONIC BACK PAIN

GOLD STARS FOR OUR SERVICE USERS Inspiring courage Determination, resilience Capacity for hard work Commitment to sessions Willingness to participate, to risk. . . . to change and a hearty dose of humour! STOP! CHRONIC BACK PAIN

OUTSTANDING ACHIEVEMENTS Earlier intervention = psychoneurobiological plasticity ! Statistically significant results: emotional/physical disability pain catastrophising Enhanced quality of life STOP! CHRONIC BACK PAIN Half the time =half the cost! Non-clinical settings YUHASS: monitor costs: Prescription HCP Appointments Personal costs Social/welfare costs
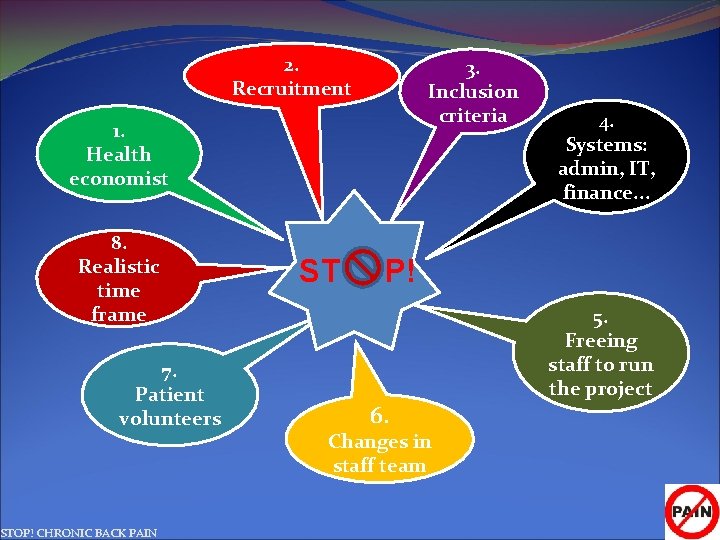
2. Recruitment 3. Inclusion criteria 1. Health economist 8. Realistic time frame 7. Patient volunteers STOP! CHRONIC BACK PAIN 4. Systems: admin, IT, finance. . . ST P! 6. Changes in staff team 5. Freeing staff to run the project

RECRUITMENT DURATION OF OVER-ALL PAIN 6 - 36 months: 8 pts 37 mths – 35 years: 27 pts DURATION OF CURRENT EPISODE PSST. . . WHERE IS THE ‘LOST PATIENT’ ? 2 – 36 months: 30 pts 37 mths – 25 years: 5 pts STOP! CHRONIC BACK PAIN

ACCESSIBILITY = Matching service to need MIND BODY Prevention PREVENTION STOP! CHRONIC BACK PAIN HOLISTIC support – e. g. employment

5. Spread STOP! CHRONIC BACK PAIN

STOP! CHRONIC BACK PAIN SPREADING THE MESSAGE : PAN DORSET PAIN SERVICES

Do your work with mastery The Buddha Like the moon, come out from behind the clouds Shine

THANK YOU. . to. . . . the real stars. . . our patients. . . our fantastic team. . . Springfield Consultancy. . . HEALTH FOUNDATION STOP! CHRONIC BACK PAIN
- Slides: 41