Spontaneous rupture of the oesophagus Boerhaave syndrome Dr

Spontaneous rupture of the oesophagus Boerhaave syndrome Dr Kylie JY Szeto Tuen Mun Hospital 15 Dec 2018
Outline • Case presentation • Background • Investigation • Management

Our patient • 71/M • History of perforated DU with patch repair 2001, severe AS with AVR on warfarin • Admitted in 4/2018 for epigastric discomfort after food intake v 4 episodes of vomiting
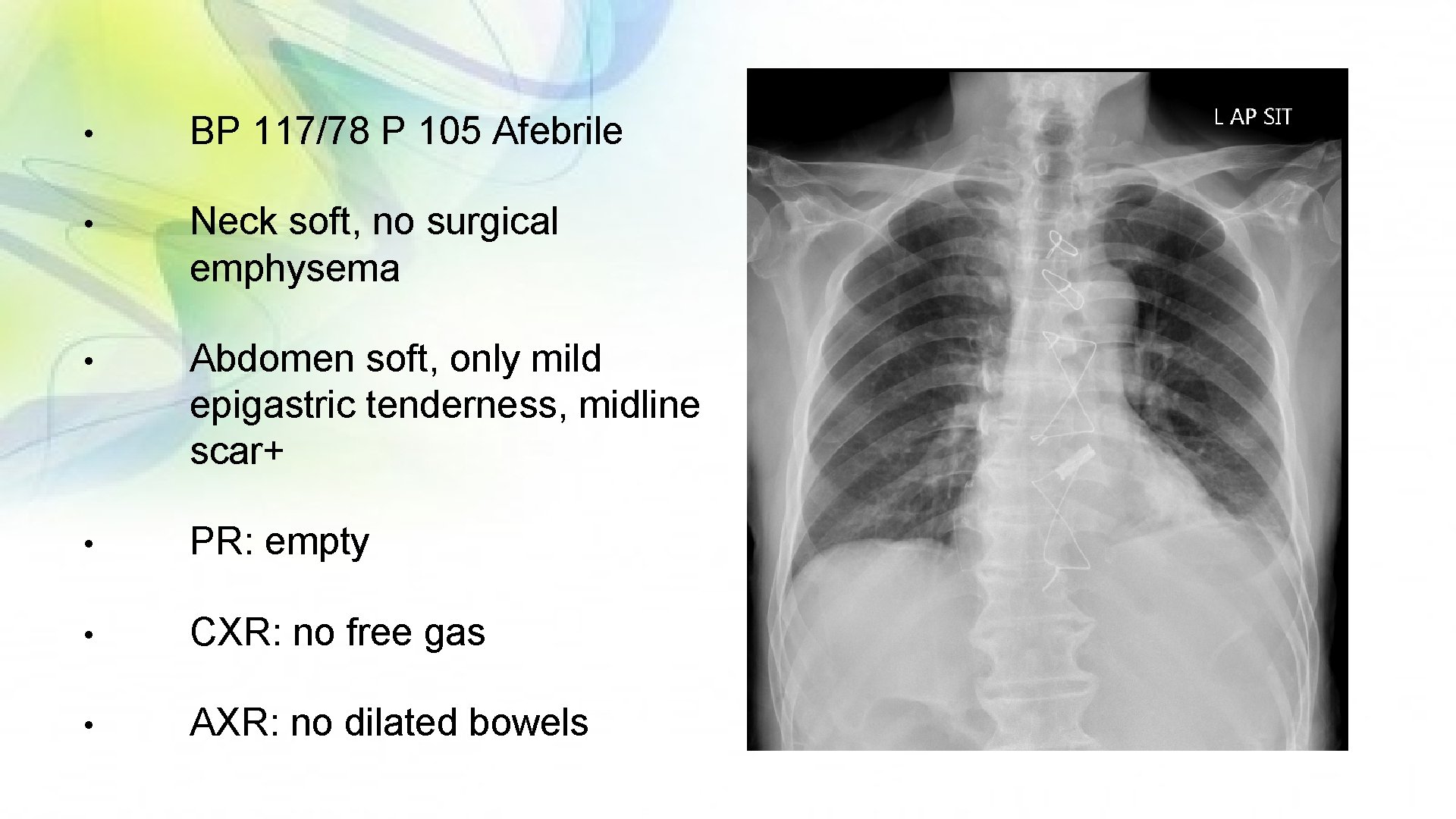
• BP 117/78 P 105 Afebrile • Neck soft, no surgical emphysema • Abdomen soft, only mild epigastric tenderness, midline scar+ • PR: empty • CXR: no free gas • AXR: no dilated bowels
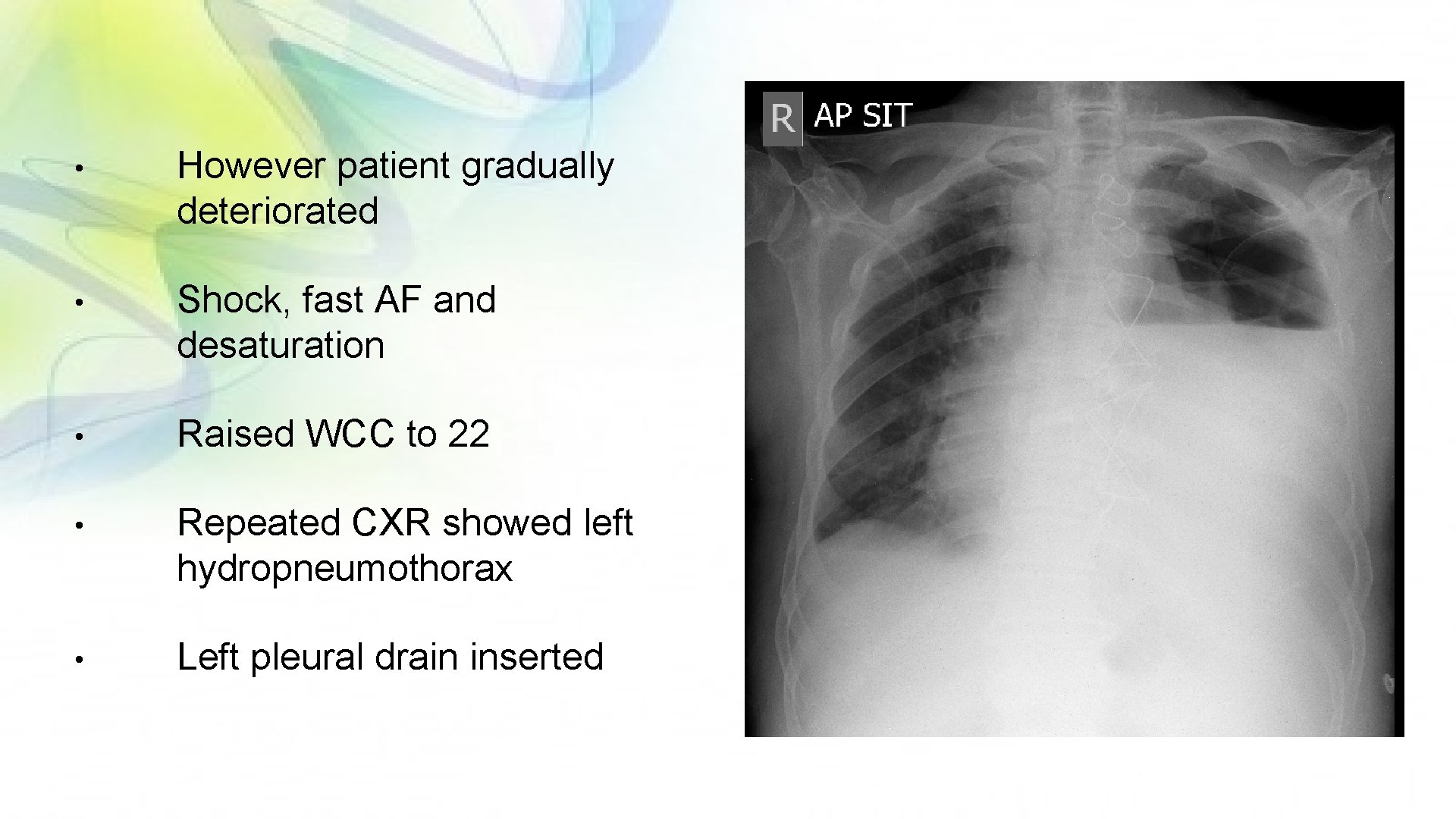
• However patient gradually deteriorated • Shock, fast AF and desaturation • Raised WCC to 22 • Repeated CXR showed left hydropneumothorax • Left pleural drain inserted
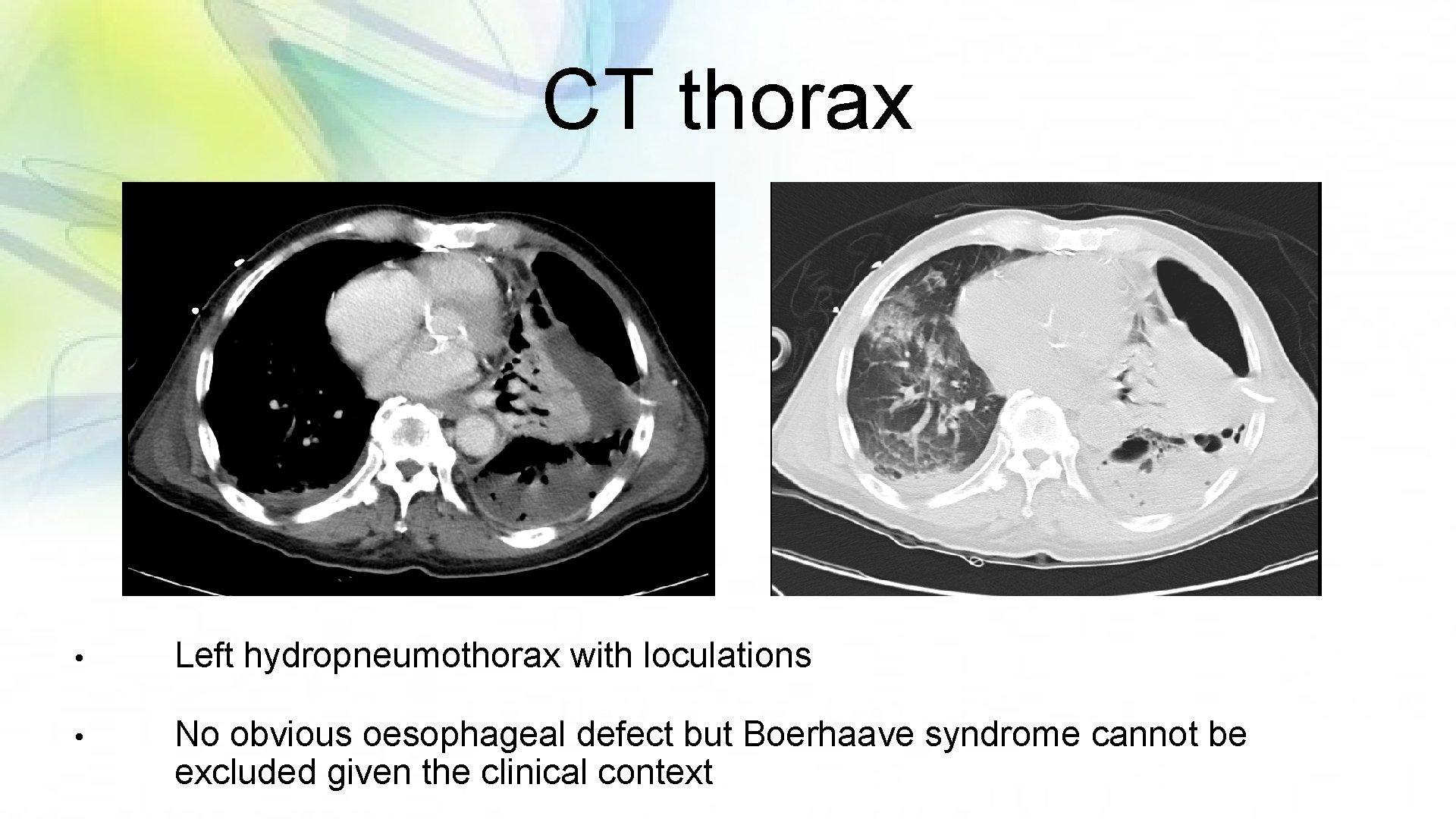
CT thorax • Left hydropneumothorax with loculations • No obvious oesophageal defect but Boerhaave syndrome cannot be excluded given the clinical context
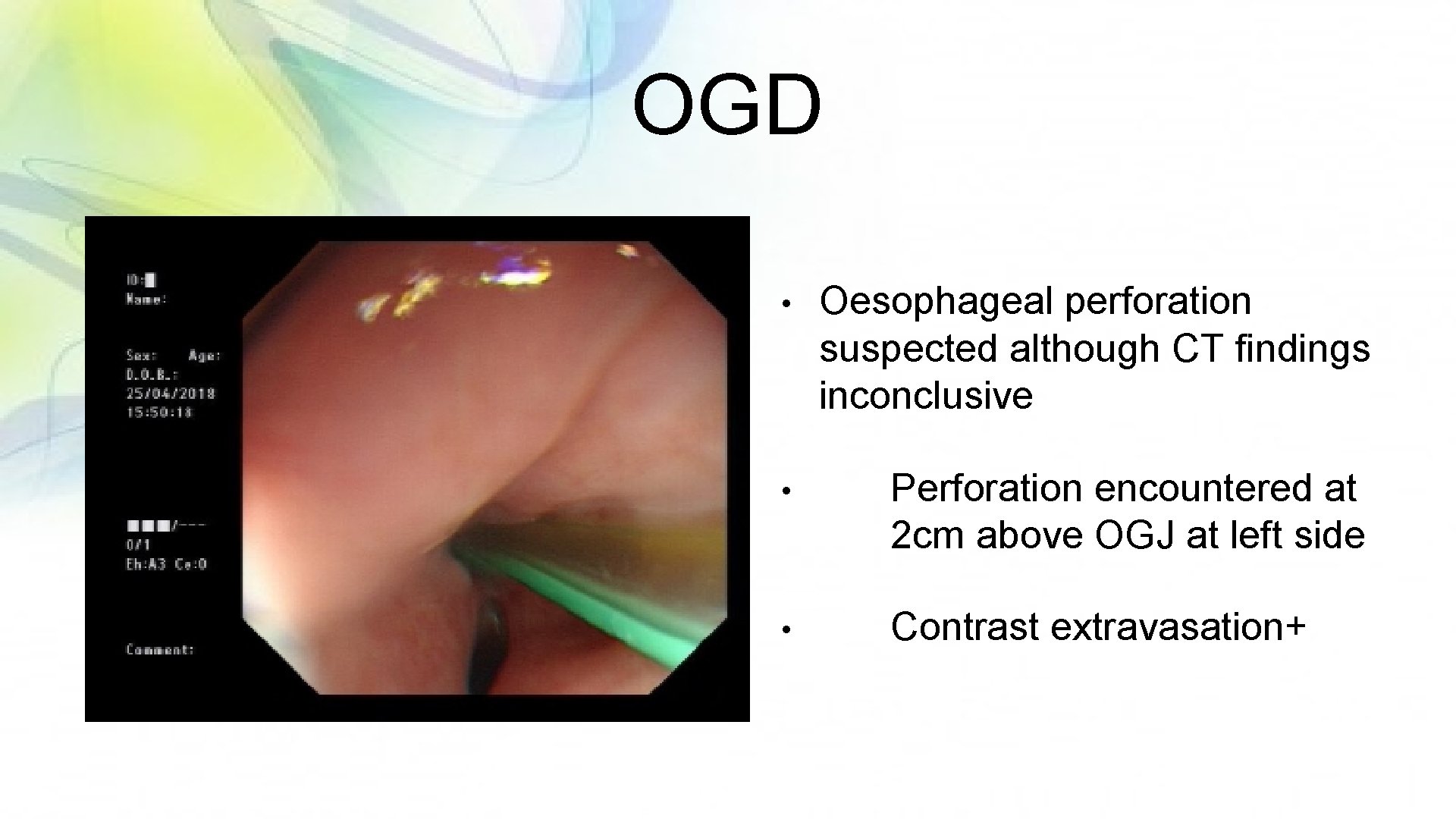
OGD • Oesophageal perforation suspected although CT findings inconclusive • Perforation encountered at 2 cm above OGJ at left side • Contrast extravasation+

Background • Defined as spontaneous rupture of the oesophagus after forceful emesis • First described by Herman Boerhaave in 1724 • Transmural rupture • Rare condition accountable for 15% of oesophageal perforation • Almost always fatal in the past • High mortality even now 9 (35 -40%)
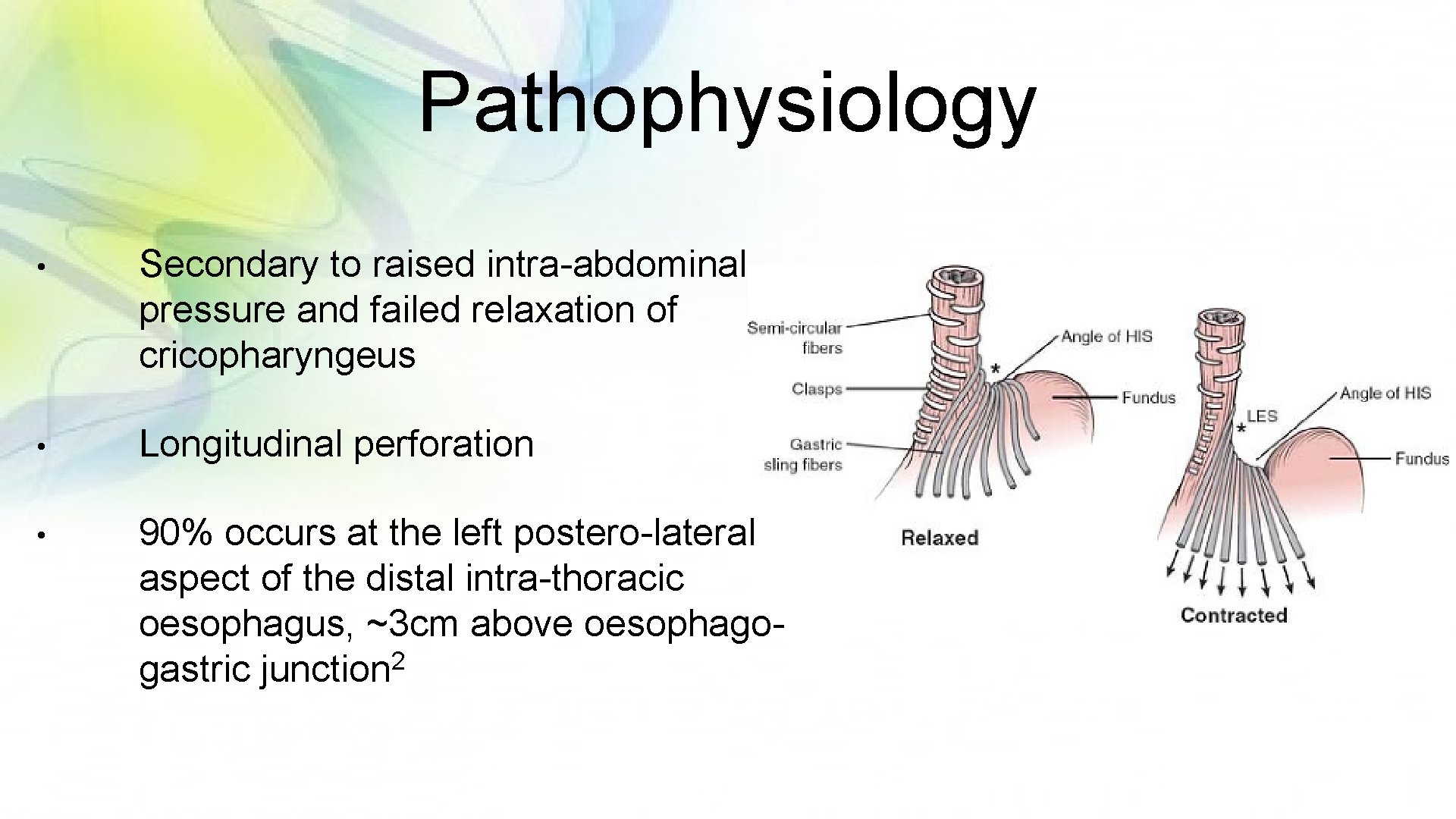
Pathophysiology • Secondary to raised intra-abdominal pressure and failed relaxation of cricopharyngeus • Longitudinal perforation • 90% occurs at the left postero-lateral aspect of the distal intra-thoracic oesophagus, ~3 cm above oesophago 2 gastric junction
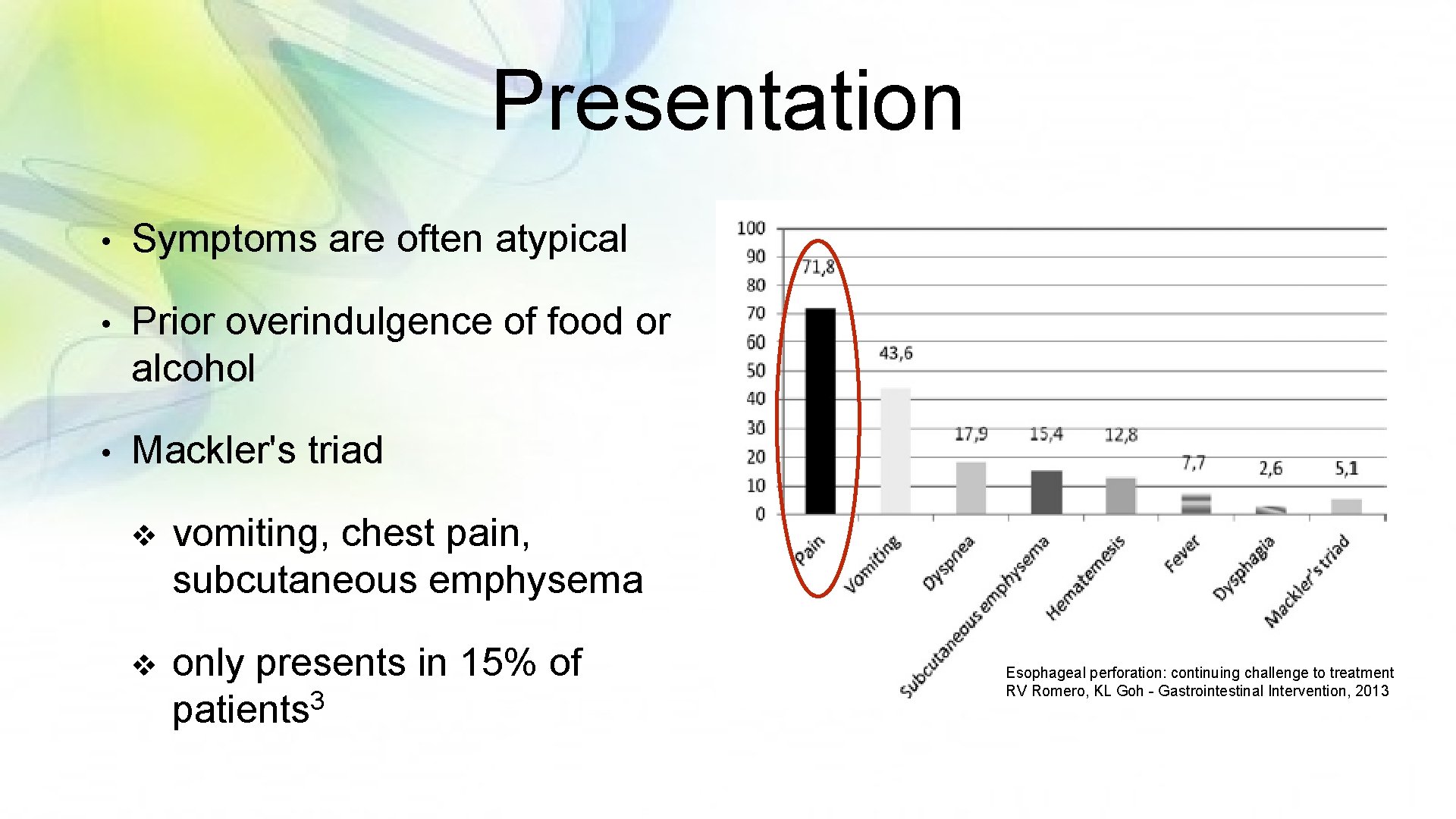
Presentation • Symptoms are often atypical • Prior overindulgence of food or alcohol • Mackler's triad v vomiting, chest pain, subcutaneous emphysema v only presents in 15% of 3 patients Esophageal perforation: continuing challenge to treatment RV Romero, KL Goh - Gastrointestinal Intervention, 2013
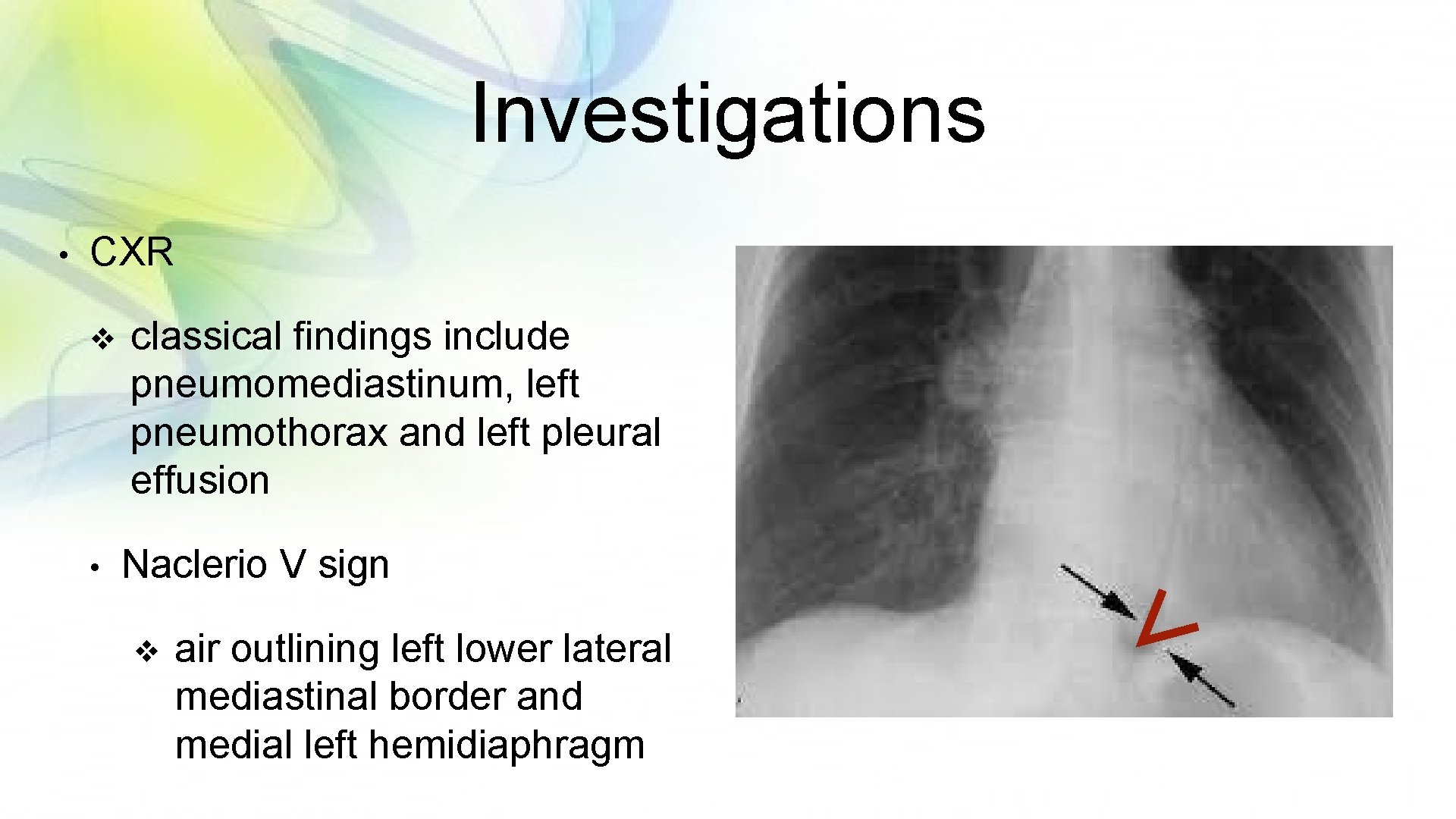
Investigations • CXR v • classical findings include pneumomediastinum, left pneumothorax and left pleural effusion Naclerio V sign v air outlining left lower lateral mediastinal border and medial left hemidiaphragm
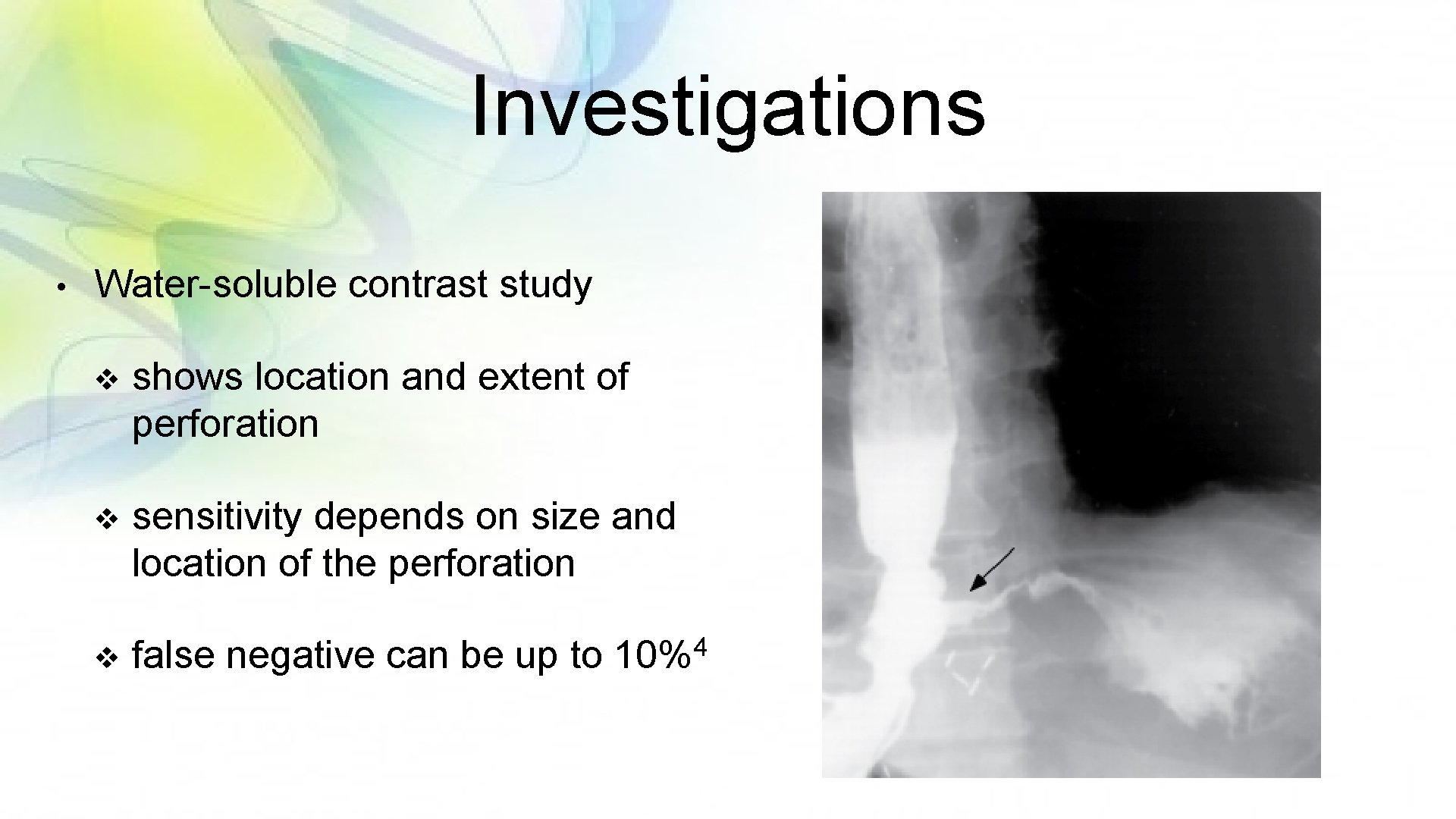
Investigations • Water-soluble contrast study v shows location and extent of perforation v sensitivity depends on size and location of the perforation v false negative can be up to 4 10%

Investigations CT • v sensitive in detecting intra-peritoneal gas or mediastinal gas v assess extent of contamination Endoscopy • v reserved for patients with unclear diagnosis on imaging v enables lesion characterisation and shows viability of oesophageal mucosa v ? turns concealed perforation into free perforation

• Early diagnosis and treatment are crucial for successful outcome in oesophageal perforation • Mortality rate with a delayed diagnosis was 40% compared to 5 6. 2% who were diagnosed in <24 hrs (p = 0. 047)

Management principles • Broad spectrum antibiotics • Drainage • Debridement of necrotic tissue • Restore GI tract integrity and continuity • Maintain nutrition
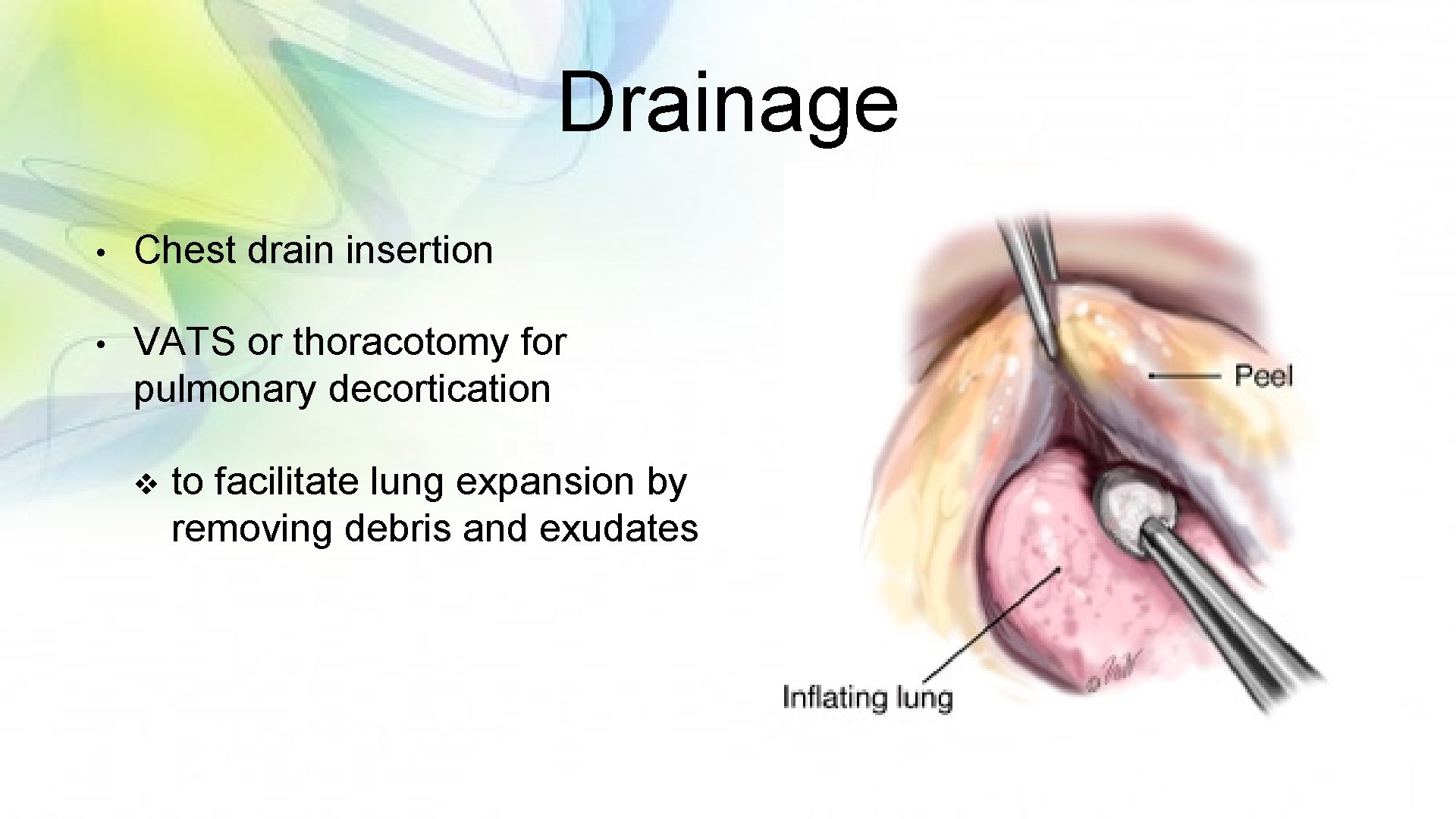
Drainage • Chest drain insertion • VATS or thoracotomy for pulmonary decortication v to facilitate lung expansion by removing debris and exudates

Management • Non-operative v Conservative v Endoscopic treatment • Operative v Primary closure +/reinforcement v Exclusion and diversion v Oesophagectomy
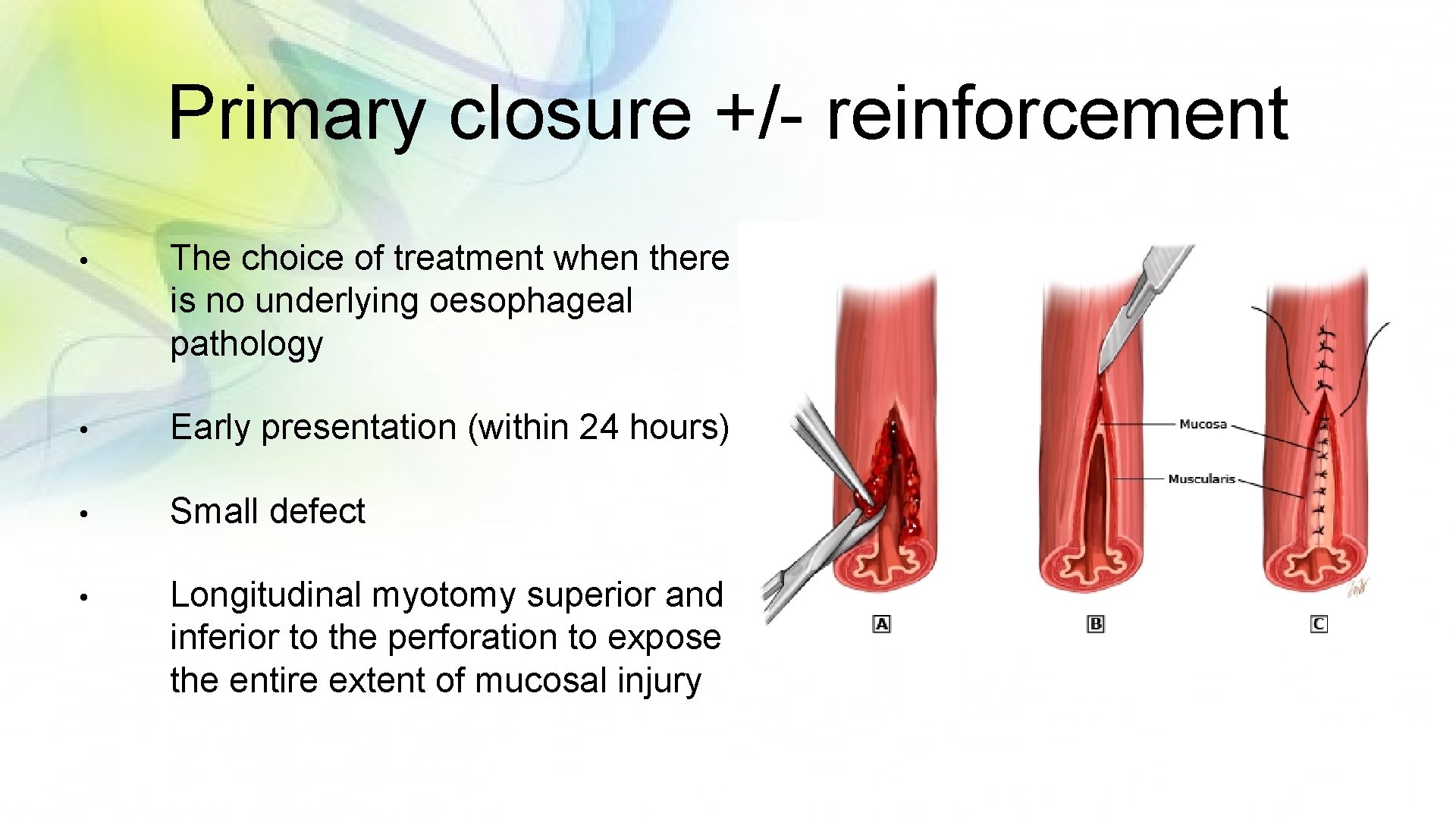
Primary closure +/- reinforcement • The choice of treatment when there is no underlying oesophageal pathology • Early presentation (within 24 hours) • Small defect • Longitudinal myotomy superior and inferior to the perforation to expose the entire extent of mucosal injury

Reinforcement can reduce rate of 8 post-operative leakage • v 54. 5% vs 7. 1% (p=0. 021) v no significant difference in death or need of revision v no difference in hospital stay v small sample size
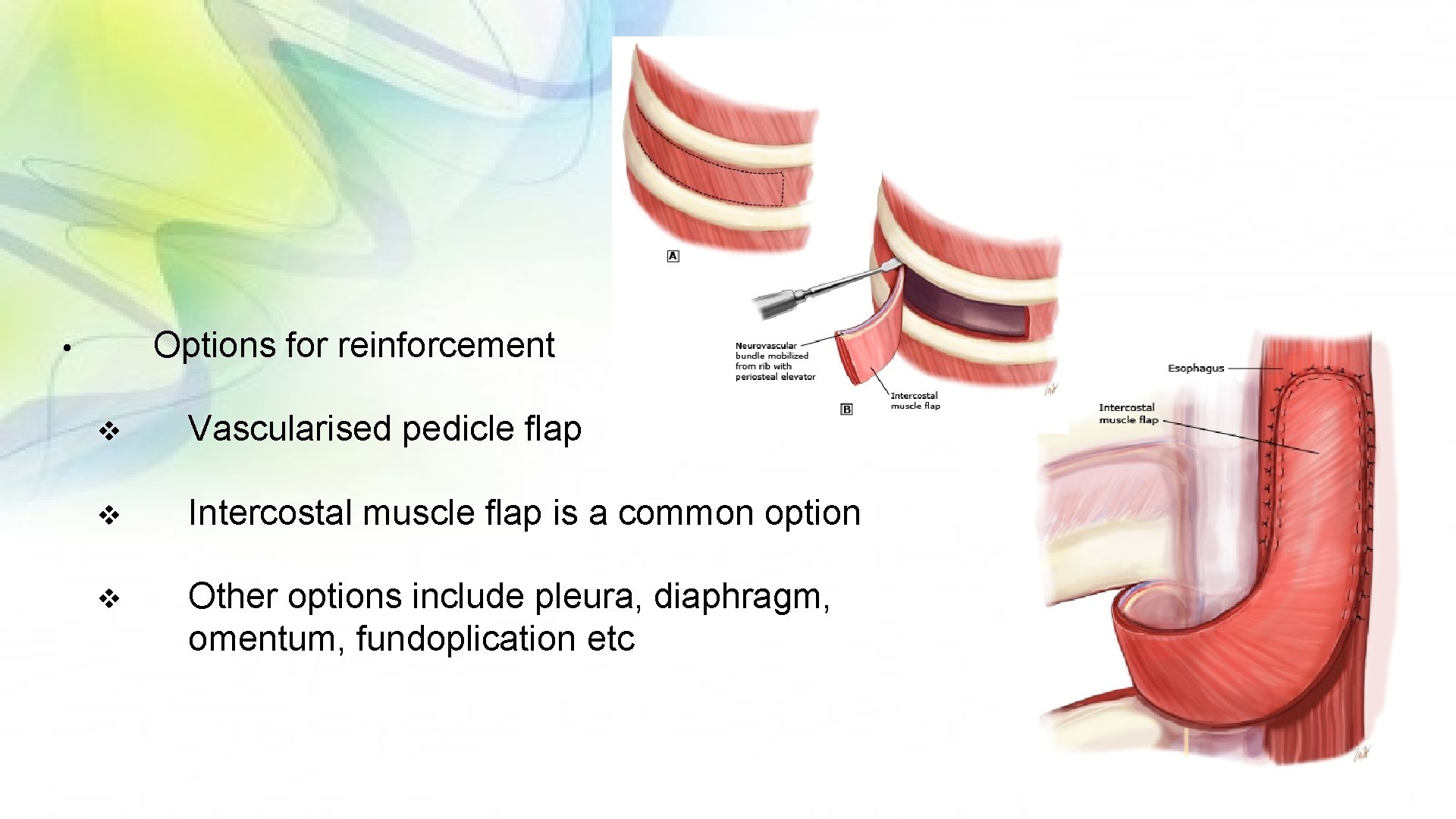
Options for reinforcement • v Vascularised pedicle flap v Intercostal muscle flap is a common option v Other options include pleura, diaphragm, omentum, fundoplication etc
Oesophagectomy • For patients with underlying oesophageal pathologies • Emergency oesophagectomy carries high mortality rate reaching 10 up to 67%

Exclusion and diversion When primary repair is not feasible • v late presentation v poor tissue condition • Or when patient is haemodynamically unstable • Followed by reconstruction of the oesophagus later • Aim to divert oesophageal contents in order to control and drain extraluminal contamination
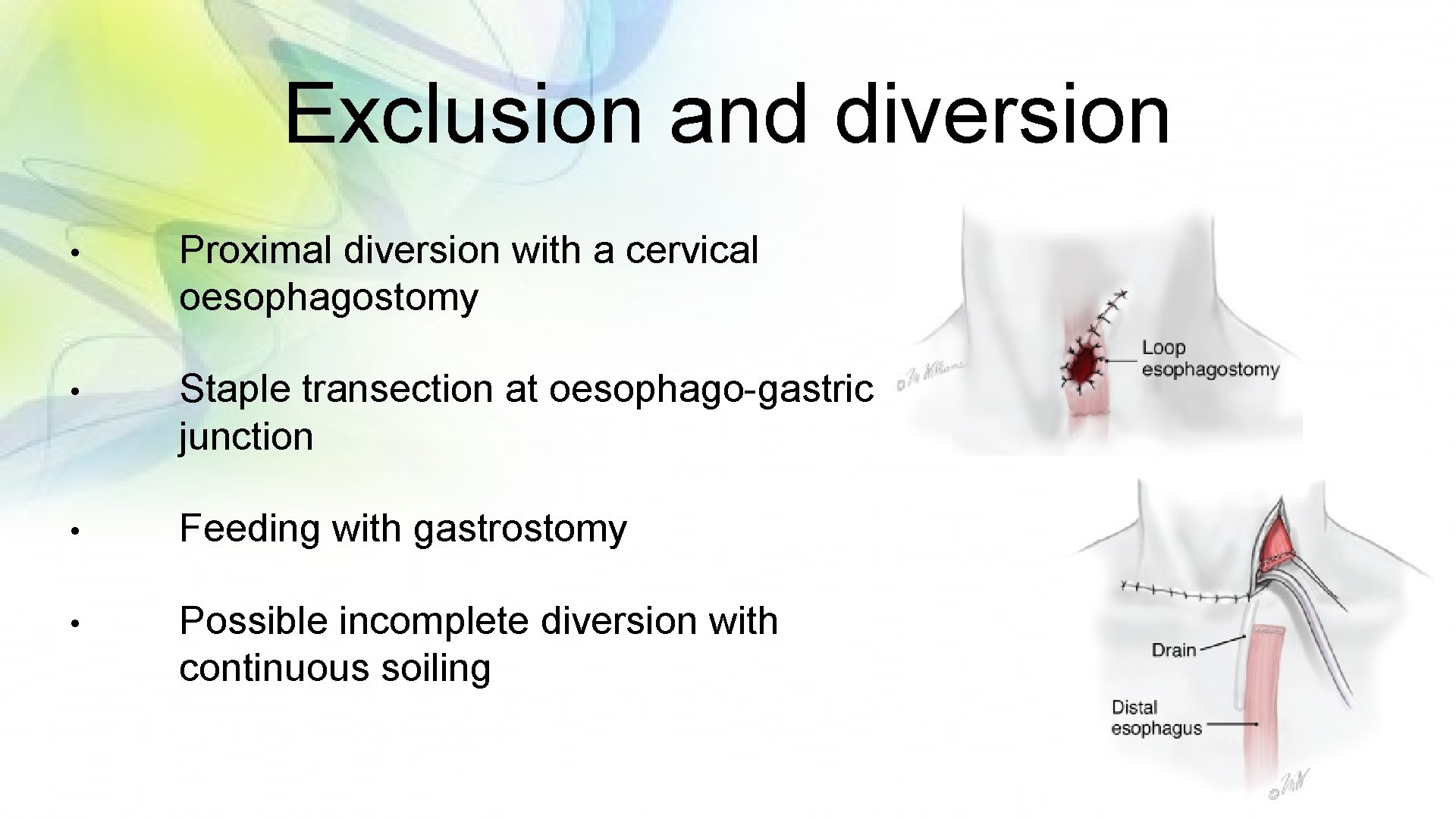
Exclusion and diversion • Proximal diversion with a cervical oesophagostomy • Staple transection at oesophago-gastric junction • Feeding with gastrostomy • Possible incomplete diversion with continuous soiling

Conservative management • Controversial v NPO for at least 7 days v Intravenous broad spectrum antibiotics v ICU care v Drainage of fluid collections v Nutritional support • Only in highly selected patients with contained leak and minimal sepsis • Any deterioration should be followed by an immediate change of treatment plan towards surgery
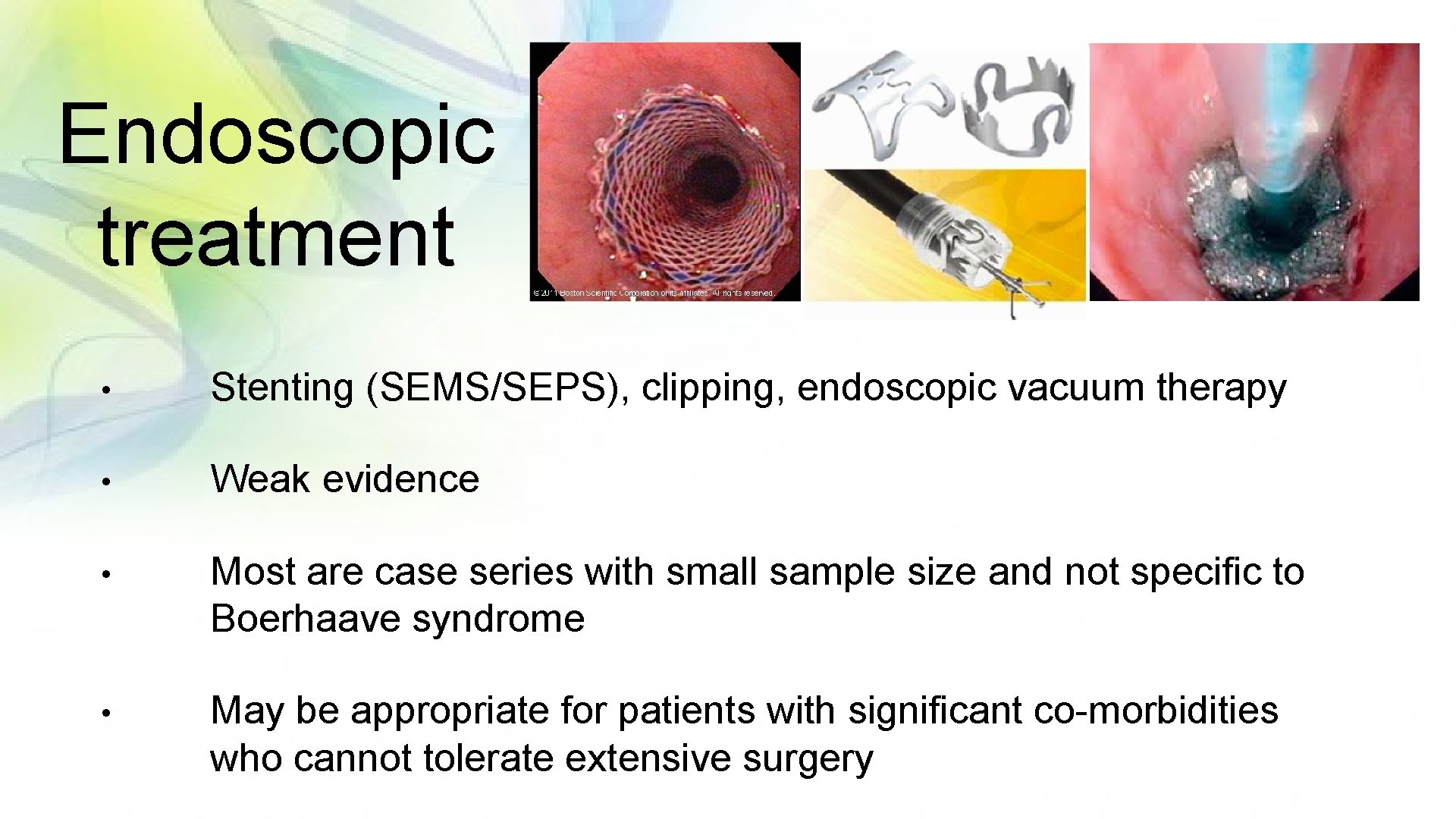
Endoscopic treatment • Stenting (SEMS/SEPS), clipping, endoscopic vacuum therapy • Weak evidence • Most are case series with small sample size and not specific to Boerhaave syndrome • May be appropriate for patients with significant co-morbidities who cannot tolerate extensive surgery
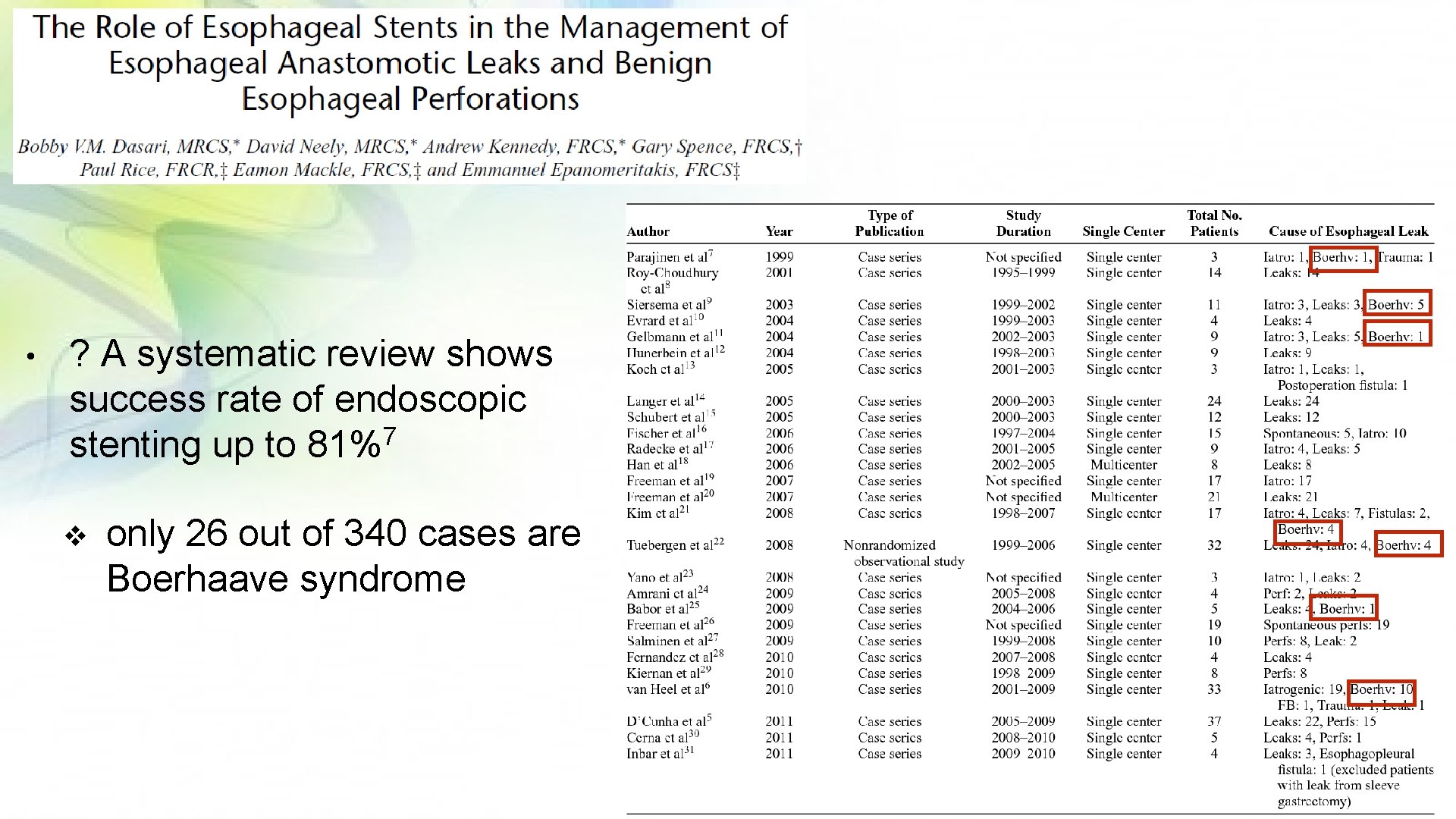
• ? A systematic review shows success rate of endoscopic 7 stenting up to 81% v only 26 out of 340 cases are Boerhaave syndrome

• A retrospective comparative study shows no advantage in 8 endoscopic stenting in Boerhaave syndrome v pulmonary decortication included as surgical re-intervention as well
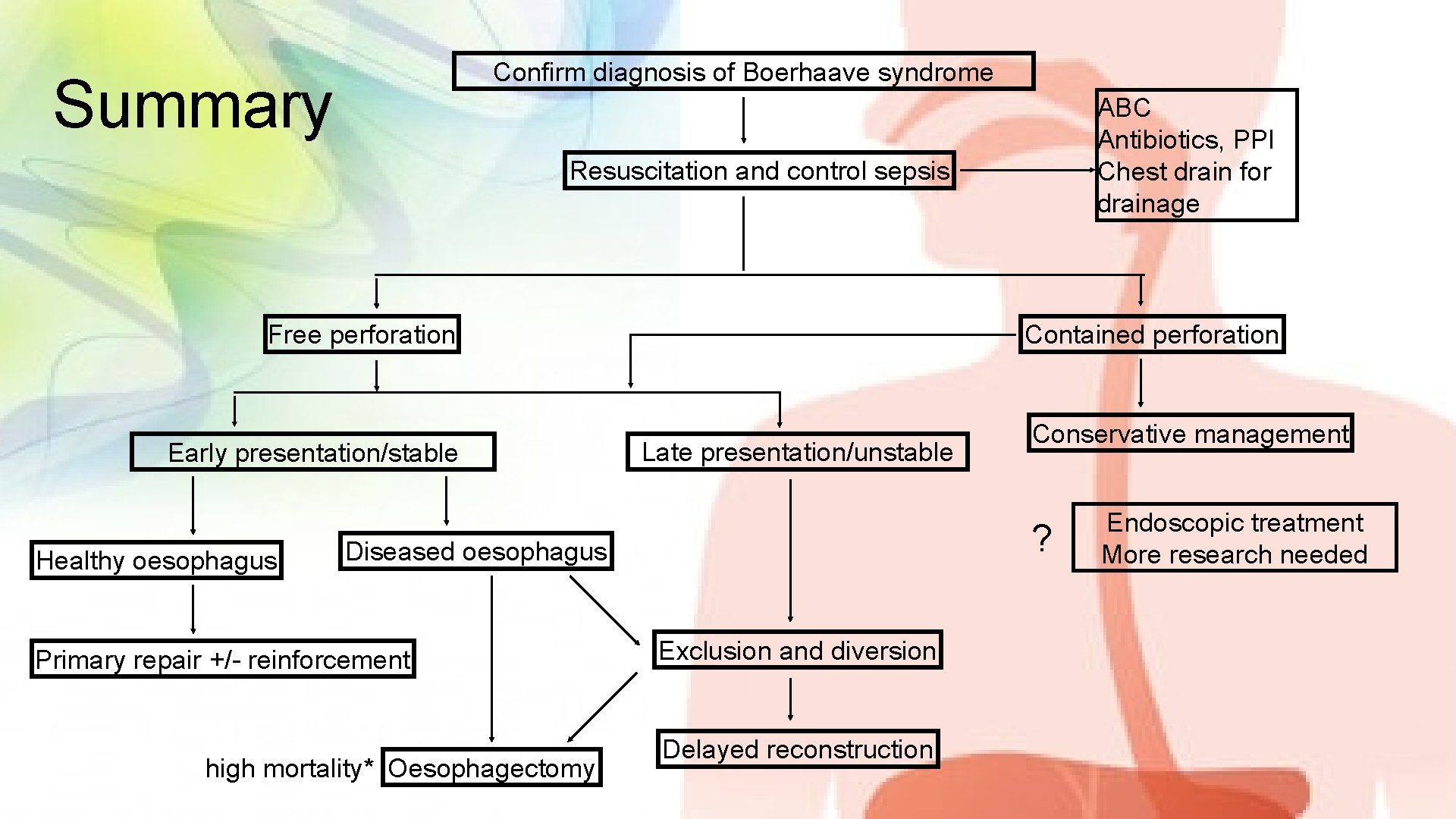
Confirm diagnosis of Boerhaave syndrome Summary ABC Antibiotics, PPI Chest drain for drainage Resuscitation and control sepsis Free perforation Early presentation/stable Healthy oesophagus Contained perforation Late presentation/unstable ? Diseased oesophagus Primary repair +/- reinforcement high mortality* Oesophagectomy Conservative management Exclusion and diversion Delayed reconstruction Endoscopic treatment More research needed
Back to our patient • Open trans-abdominal repair of oesophagus with fundoplication • Findings v • 2 cm oesophageal perforation over left postero-lateral aspect, 2 cm above OGJ VATS for decortication of left lung

Bring home message • Prompt recognition of this potential lethal condition is crucial to ensure appropriate treatment • High index of suspicion is important • Management plan has to be tailored for every patient

Reference 1. Brinster CJ, Singhal S, Lee L, et al. Evolving options in the management of esophageal perforation. Ann Thorac Surg 2004; 77: 1475. 2. de Schipper JP, Pull ter Gunne AF, Oostvogel HJ et-al. Spontaneous rupture of the oesophagus: Boerhaave's syndrome in 2008. Literature review and treatment algorithm. Dig Surg. 2009; 26 (1): 1 -6. doi: 10. 1159/000191283 3. Woo, Kar-mun C. ; Schneider, Jeffrey I. (2009). "High-Risk Chief Complaints I: Chest Pain—The Big Three". Emergency Medicine Clinics of North America. 27 (4): 685– 712, x. doi: 10. 1016/j. emc. 2009. 07. 007 4. Bladergroen MR, Lowe JE, Postlethwait RW. Diagnosis and recommended management of esophageal perforation and rupture. Ann Thorac Surg 1986; 42: 235. Shaker H, Elsayed H, Whittle I et-al. The influence of the 'golden 24 -h rule' on the prognosis of oesophageal perforation in the modern era. Eur J Cardiothorac Surg. 2010; 38 (2): 216 -22. doi: 10. 1016/j. ejcts. 2010. 01. 030 6. Sulpice L, Dileon S, Rayar M, Badic B, Boudjema K, Bail J, et al. Conservative surgical management of Boerhaave's syndrome: Experience of two tertiary referral centers. International Journal of Surgery 2013; 11(1): 64 -67 7. Dasari BV, Neely D, Kennedy A, Spence G, Rice P, Mackle E, et al. The role of esophageal stents in the management of esophageal anastomotic leaks and benign esophageal perforations. Ann Surg 2014 May; 259(5): 852 -860. 8. Schweigert M, Beattie R, Solymosi N, Booth K, Dubecz A, Muir A, et al. Endoscopic stent insertion versus primary operative management for spontaneous rupture of the esophagus (Boerhaave syndrome): an international study comparing the outcome. Am Surg 2013; 79(6): 634 -640. 9. Turner AR, Turner SD. Boerhaave syndrome. Stat. Pearls [Internet]. 2018 Jan 10. Evaluation of urgent esophagectomy in esophageal perforation. José Luis Braga de AQUINO, José Gonzaga Teixeira de CAMARGO, Gustavo Nardini CECCHINO, Douglas Alexandre Rizzanti PEREIRA, Caroline Agnelli BENTO, Vânia Aparecida LEANDRO-MERHI. Arq Bras Cir Dig. 2014 Oct-Dec; 27(4): 247– 250. doi: 10. 1590/S 0102 -6720201400005

Local experience • Total 11 cases of Boerhaave syndrome in TMH from 2004 – 2013

DDx for unilateral pleural effusion • • Malignancy Infection Haemorrhage Iatrogenic DDx for loculated pneumomediastinum unilateral pleural effusion • • • Tuberculosis • Trauma Haemorrhage • ARDS Empyema • Pneumonitis • Necrotising mediastinitis
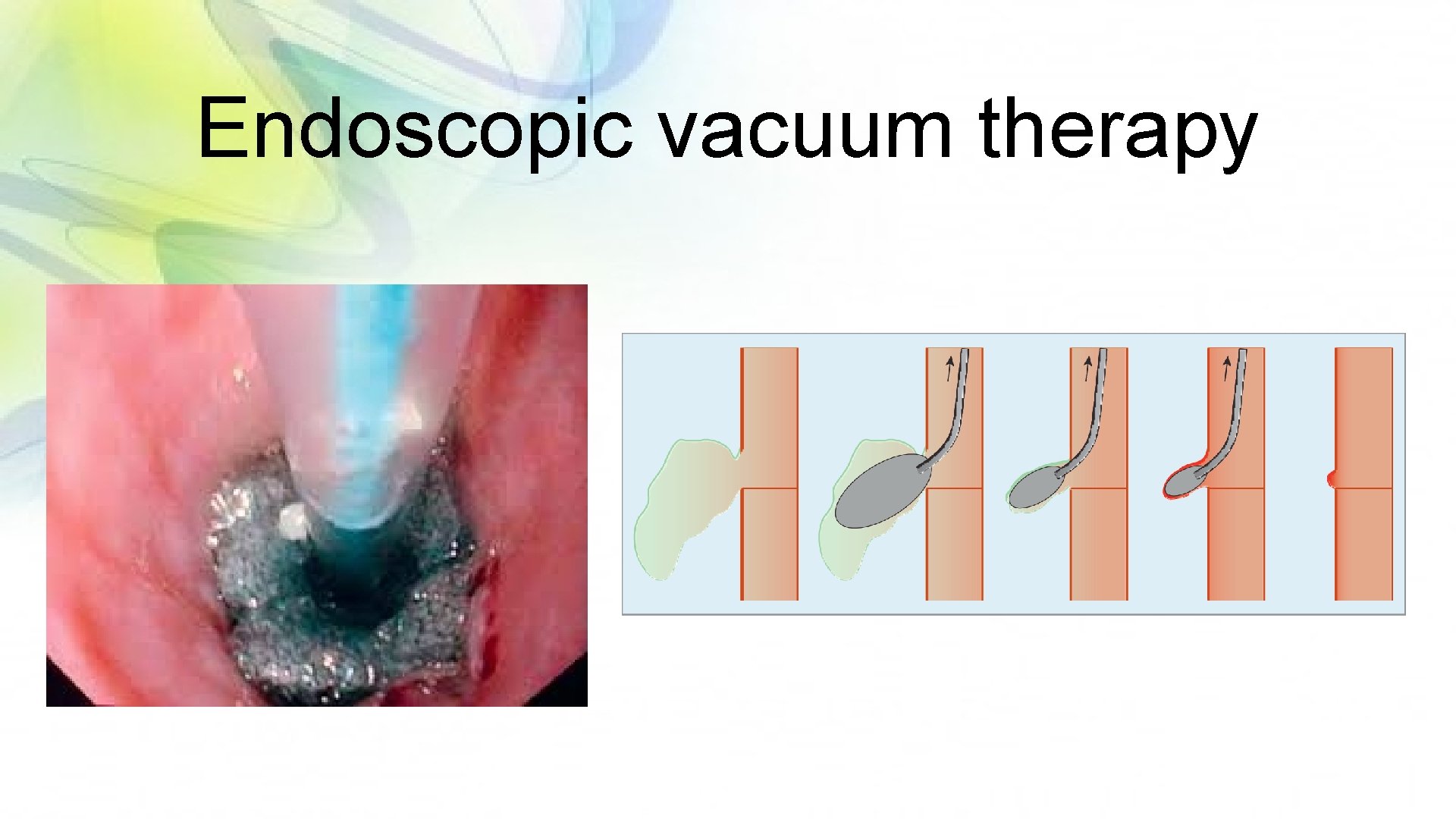
Endoscopic vacuum therapy
- Slides: 34