Spontaneous abortion Dr Renu Singh Definition Clinically recognised

Spontaneous abortion Dr. Renu Singh

Definition • Clinically recognised pregnancy loss before 20 th week of gestation • Expulsion or extraction of an embryo or fetus weighing 500 gm or less(WHO) • Synonymous with miscarriage • Latin : aboriri: to miscarry

Incidence • MC early pregnancy complication • Frequency decreases with increasing gestational age • Incidence: 8 -20%(clinically recognised pregnancies) • Women who had a child: 5% incidence of miscarriage • 80% spontaneous abortion : < 12 wks

Risk factors Advanced maternal age Previous spontaneous abortion Medications & substances (smoking) Mechanisms responsible for abortion: not apparent • Death of fetus precedes spont. expulsion, finding cause involves ascertaining the cause of fetal death • •

Maternal age • Most important risk factor in healthy women • • 30 yrs: 9 -17% 35 yrs: 20% 40 yrs: 40% 45 yrs: 80%

Previous spontaneous abortion • Previous successful pregnancy: 5% risk • 1 miscarriage: 20% • 2 consecutive miscarriages: 28% • ≥ 3 consecutive miscarriages: 43%

Medications or substances • Heavy smoking(>10 cigarettes/day) : vasoconstrictive & antimetabolic effects of tobacco smoke • Moderate to high alcohol consumption(>3 drinks/week) • NSAIDS use(acetaminophen) : abnormal implantation & pregnancy failure due to antiprostaglandin effect

Other factors • Low plasma folate levels(≤ 2. 19 ng/ml): no specific evidence to support • Extremes of maternal weight: prepregnancy BMI<18. 5 OR >25 kg/m 2 • Maternal fever: 100°F(37. 8°C), no evidence to support

Etiology • Fetal • Maternal • unexplained

Etiology • Foetal factors – Chromosomal abnormalities(50% ), • aneuplodies , monosomy X, Triploidy • Trisomy 16 : mc autosomal trisomy, lethal • Abnormalities arise de novo – Congenital anomalies – Trauma: invasive prenatal diagnostic procedures

Aetiology : Maternal factors – Maternal endocrinopathies: hypothyroidism, insulin dependant diabetes – Congenital or acquired uterine abnormalities: interfere with implantation & growth – Maternal diseases: acute maternal infection (listeria, toxo, parvo B 19, rubella, CMV) : inconclusive – Radiation in therapeutic doses – Hypercoagulable state(thrombophillias) : RPL

Clinical presentation • Vaginal bleeding – Scant brown spotting to heavy vaginal bleeding – Amount /pattern does not predict outcome – May be accompanied by passage of fetal tissue • Pelvic pain – Crampy /dull in character – Constant/intermittent • Incidental finding on pelvic ultrasound in asymptomatic patient

Diagnostic evaluation • History – Period of amenorrhea , LMP/USG • Physical examination: Complete pelvic examination: – P/S, : source, amount of bleeding, dilated cervix, POC visible at Os/in vagina – P/V: uterine size(consistent with GA) • Pelvic ultrasound

Pelvic ultrasound • Most useful test in diagnostic evaluation of women with suspected spontaneous abortion • Foetal cardiac activity: most important (5. 56 wks) • Foetal heart rate • Size & contour of G. sac • Presence of yolk sac • Best evaluated , transvaginal approach(TVS)

Pelvic USG: criteria for spontaneous abortion • Gestational sac ≥ 25 mm in mean diameter that does not contain a yolk sac or embryo • An embryo with CRL ≥ 7 mm with no cardiac activity If the GS or embryo is smaller than these dimensions: repeat pelvic USG in 1 -2 weeks

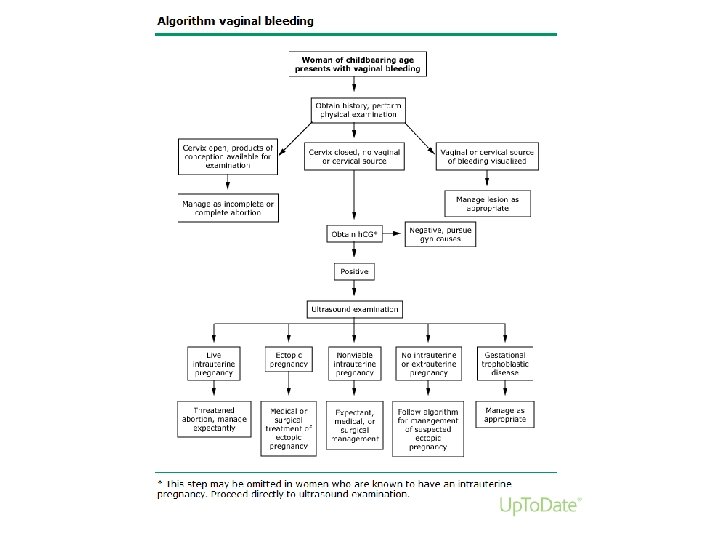
Differential diagnosis • • Physiologic: placental sign Ectopic pregnancy Gestational trophoblastic disease Cervical/vaginal/uterine pathology • Physical examination • Transvaginal sonography(TVS) • Serial quantitative ßh. CG

Lab evaluation • Human chorionic gonadotropin: serial, quantitative, useful in inconclusive USG findings • ABO , Rh: need for 50/300µg anti D • Haemoglobin/hematocrit • Serum progesterone<5 ng/ml(nonviable pregnancy)

Post diagnostic classification • • Based upon the location of POC Degree of cervical dilatation(pelvic exam) Pelvic ultrasound Categorization impacts clinical management – Threatened – Inevitable – Incomplete/complete – Missed

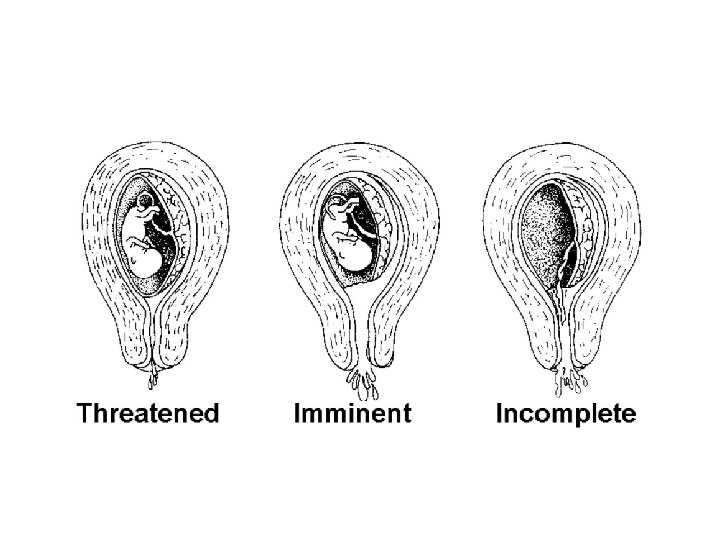
Threatened abortion • Vaginal bleeding has occurred • The cervical os is closed • Diagnostic criteria for spontaneous abortion has not met • Managed expectantly: until symptoms resolve or progresses

Threatened abortion: m/m • Expectant • Progestin treatment: most promising, efficacy not established • Bed rest: randomised trials have refuted the role • Avoid vigorous activity • Avoid heavy lifting • Avoid sexual intercourse

Threatened abortion : m/m • Counsel about risk of miscarriage • Return to hospital in case of additional vaginal bleeding, pelvic cramping or passage of tissue from vagina • Repeat pelvic USG until a viable pregnancy is confirmed or excluded • Viable pregnancy, resolved symptoms: prenatal care • If symptoms continue: monitor for progression to inevitable, incomplete, or complete abortion
Inevitable abortion • Vaginal bleeding, typically accompanied by crampy pelvic pain • Dilated cervix( internal os) • Products of conception felt or visualised through the internal os

Incomplete abortion • • Vaginal bleeding and/or pain present Cervix is dilated Products of conception partially expelled out Uterine size less than period of amenorrhea

Missed abortion • • Non viable intrauterine pregnancy Cervical os is closed POC not expelled May notice that symptoms associated with early pregnancy have abated

Management • Complete evacuation of uterine contents(POC) • Surgical methods: suction evacuation/suction curettage/dilation & evacuation • Medical methods: Misoprostol, mifepristone • Expectant • All have similar efficacy

Surgical evacuation • Performed under IV sedation & paracervical block • Prophylactic antibiotics • Operating room/procedure room • Potential complications • Anaesthesia related, • uterine perforation, cervical trauma, • infection, intrauterine adhesions

Medical methods • Misoprostol: drug of choice • Efficacy depends on dose & route of administration • 400 mcg vaginally every 4 hours for 4 doses • Expulsion rate : 50 -70% • Low cost, low incidence of side effects, stable at room temperature, readily available, timing of use can be controlled by patient

Misoprostol • WHO consensus report on misoprostol regimen – Missed abortion: 800 mcg vaginally, or 600 mcg sublingually – Incomplete abortion: 600 mcg orally • Expulsion rate: 70 -90%

Choosing the method • Surgical evacuation : heavy bleeding, intrauterine sepsis, medical co morbidities, misoprostol is contraindicated – Shorter time to completion of treatment – Lowers risk of unplanned admissions – Lower need for subsequent treatment

Expectant m/m • • Stable vital signs No evidence of infection Offered after proper counseling If unsuccessful after 4 wks , surgical evacuation is needed

Complete abortion • POC expelled completely from uterus & cervix • Cervical os is closed • Uterus small in size (GA) • Resolved or minimal vaginal bleeding & pain • Aim of t/t: ensure that bleeding is not excessive & all POC have expelled • Theoretically does not need treatment

Abortion : complications • • • Hemorrhage Uterine perforation Retained products of conception Endometritis Septic abortion: abortion accompanying intrauterine infection

Summary • Clinically recognised pregnany losses <20 wks gestation • Most common complication of early pregnancy • Advanced maternal age, previous spontaneous abortion, maternal smoking: risk factors • Mostly due to fetal structural/chromosomal abnormalities

Summary • Present with menstrual delay, vaginal bleeding& pelvic pain • D/D: uterine or other genital tract bleeding in viable pregnancy, ectopic, & GTD • Pelvic examination & pelvic ultrasound: key elements for diagnosis • Spontaneous abortion diagnosed based on USG criteria • Categorised as threatened/incomplete/missed

Summary • Preconceptual & prenatal counseling & care regarding modifiable aetiologies , risk factors are most imp intervention • Normal menstrual cycle resumes in 4 -6 weeks • h. CG returns to normal 2 -4 wks

Prevention of spont. abortion • Preconception & prenatal counseling • Routine screening & optimal disease control(diabetes, thyroid, thrombophilia) • Correction of uterine structural anomalies(septum, submucosal myoma, intrauterine adhesions) prior to pregnancy • Avoiding exposure to teratogen or infections • Modifiable risk factors
- Slides: 38