Sponge Set up Cornell Notes on pg 67






- Slides: 33

Sponge: Set up Cornell Notes on pg. 67 Topic: 22. 1 Male and Female reproductive systems 22. 1 Male and female reproductive systems Describe the major functions of the uterus. Essential Question: Describe the major functions of the uterus. Text: 849/866 • Get your Textbook • Paper from tray

Objective SWU: the locations and functions of the major parts of the male and female reproductive system SW: research the locations and functions of all major parts of the male and female reproductive system

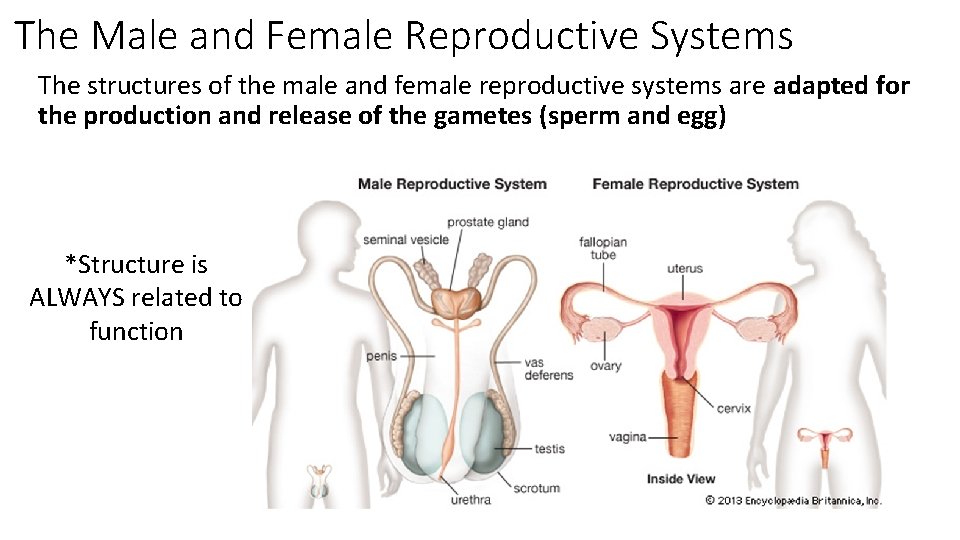
The Male and Female Reproductive Systems The structures of the male and female reproductive systems are adapted for the production and release of the gametes (sperm and egg) *Structure is ALWAYS related to function

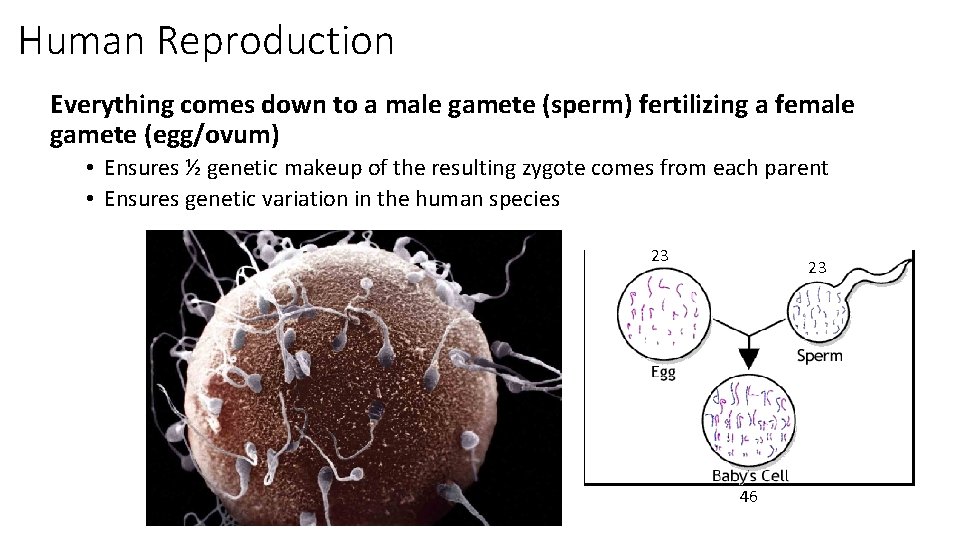
Human Reproduction Everything comes down to a male gamete (sperm) fertilizing a female gamete (egg/ovum) • Ensures ½ genetic makeup of the resulting zygote comes from each parent • Ensures genetic variation in the human species 23 23 46

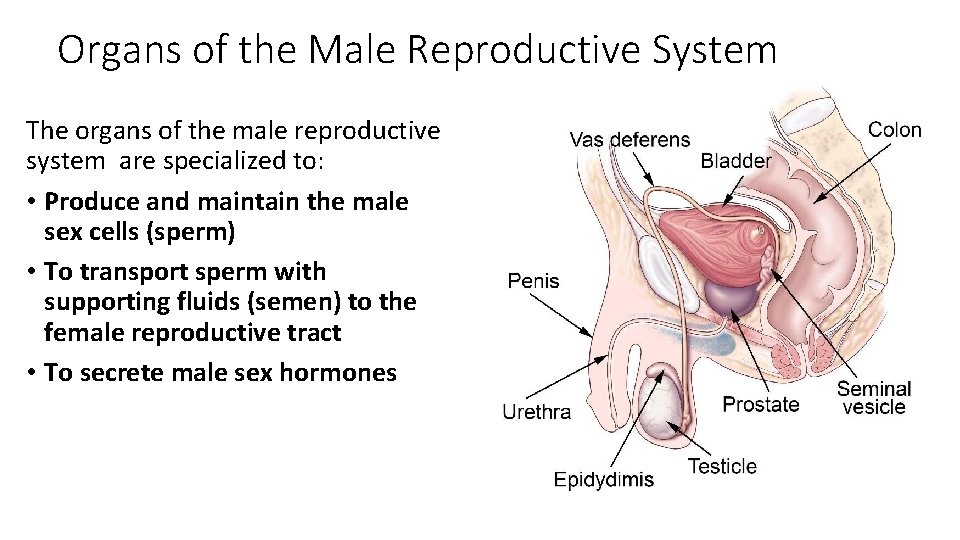
Organs of the Male Reproductive System The organs of the male reproductive system are specialized to: • Produce and maintain the male sex cells (sperm) • To transport sperm with supporting fluids (semen) to the female reproductive tract • To secrete male sex hormones

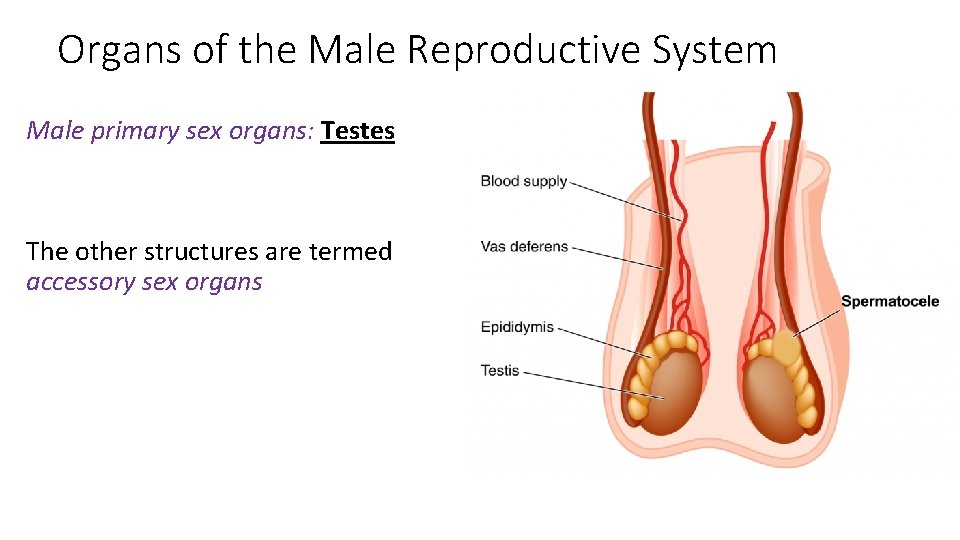
Organs of the Male Reproductive System Male primary sex organs: Testes The other structures are termed accessory sex organs

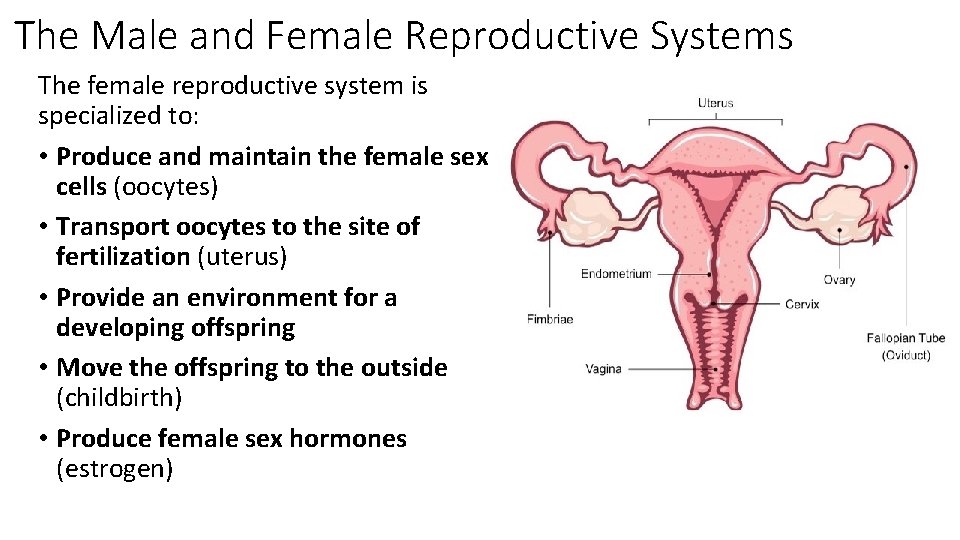
The Male and Female Reproductive Systems The female reproductive system is specialized to: • Produce and maintain the female sex cells (oocytes) • Transport oocytes to the site of fertilization (uterus) • Provide an environment for a developing offspring • Move the offspring to the outside (childbirth) • Produce female sex hormones (estrogen)

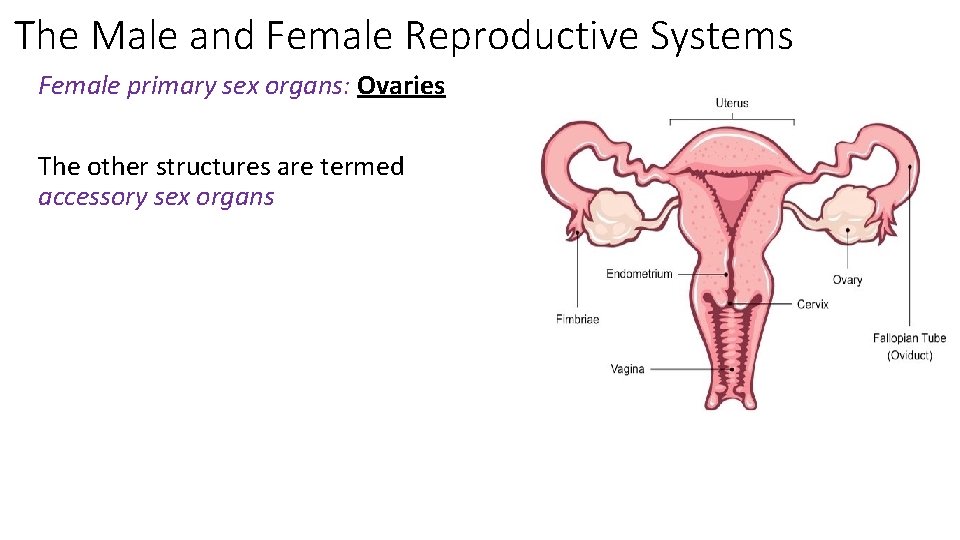
The Male and Female Reproductive Systems Female primary sex organs: Ovaries The other structures are termed accessory sex organs

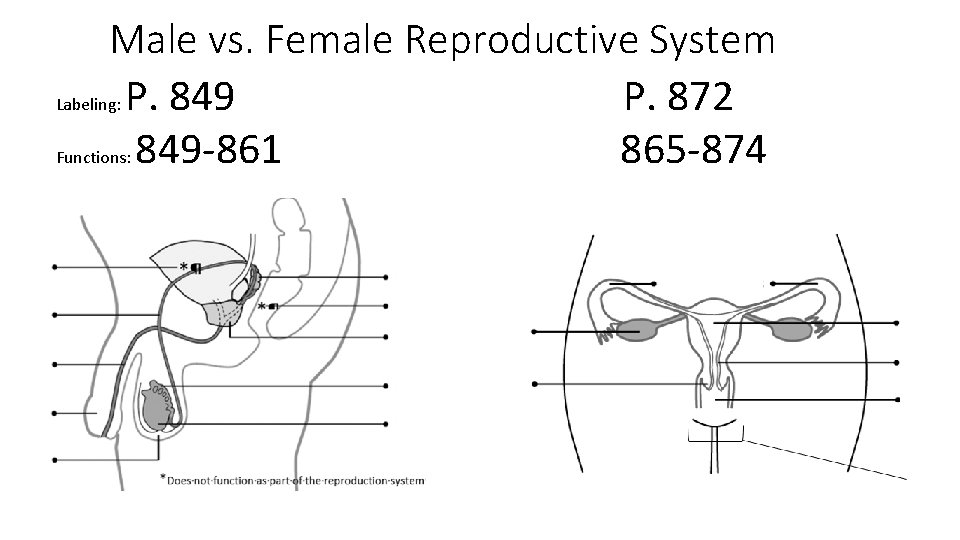
Male vs. Female Reproductive System Labeling: P. 849 P. 872 Functions: 849 -861 865 -874

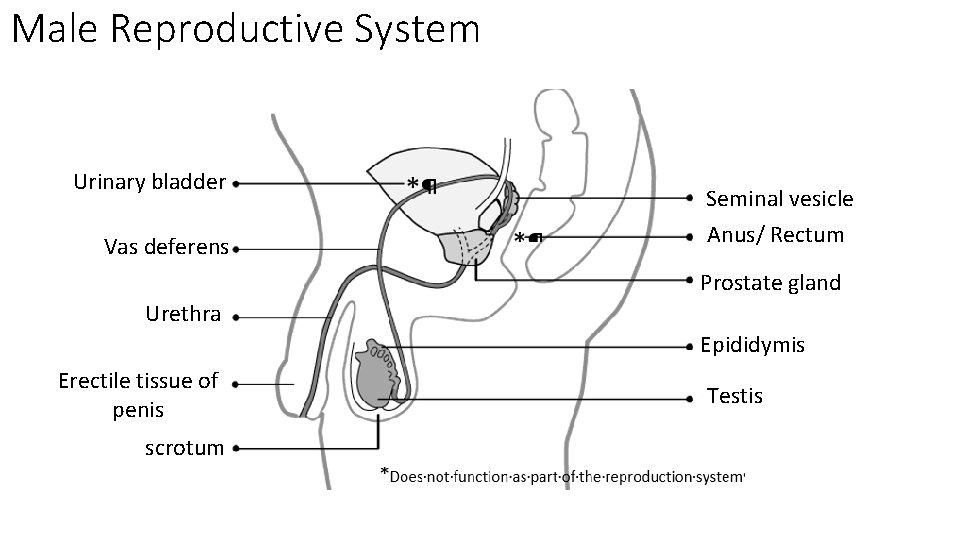
Male Reproductive System Urinary bladder Vas deferens Seminal vesicle Anus/ Rectum Prostate gland Urethra Epididymis Erectile tissue of penis scrotum Testis

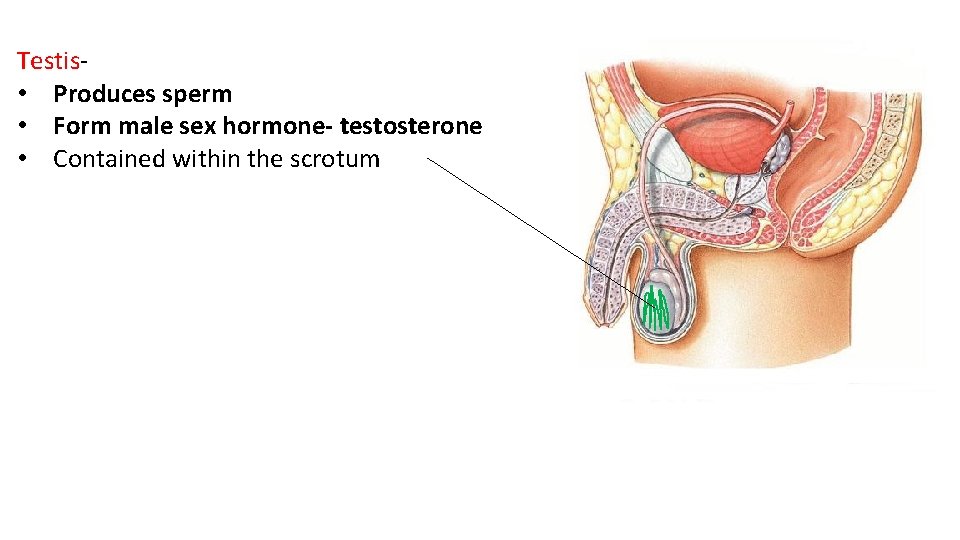
Testis- • Produces sperm • Form male sex hormone- testosterone • Contained within the scrotum

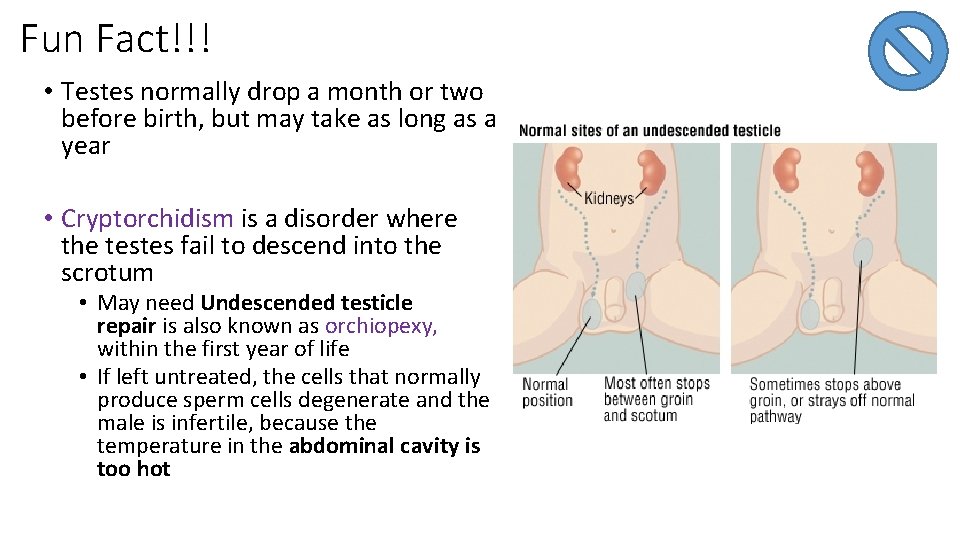
Fun Fact!!! • Testes normally drop a month or two before birth, but may take as long as a year • Cryptorchidism is a disorder where the testes fail to descend into the scrotum • May need Undescended testicle repair is also known as orchiopexy, within the first year of life • If left untreated, the cells that normally produce sperm cells degenerate and the male is infertile, because the temperature in the abdominal cavity is too hot

Critical Thinking Question What changes, if any, might occur in the secondary sex characteristics of an adult male following removal of one testis? Following the removal of both?

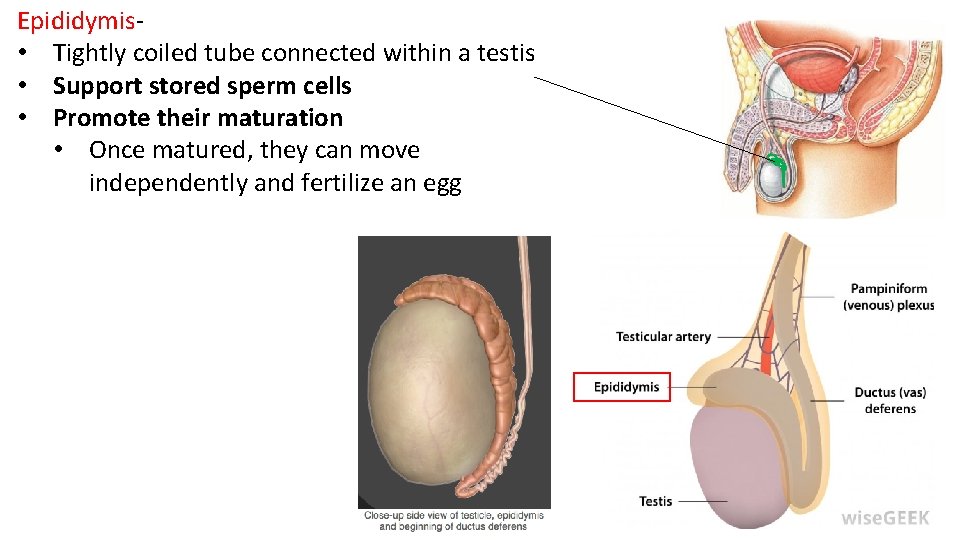
Epididymis- • Tightly coiled tube connected within a testis • Support stored sperm cells • Promote their maturation • Once matured, they can move independently and fertilize an egg

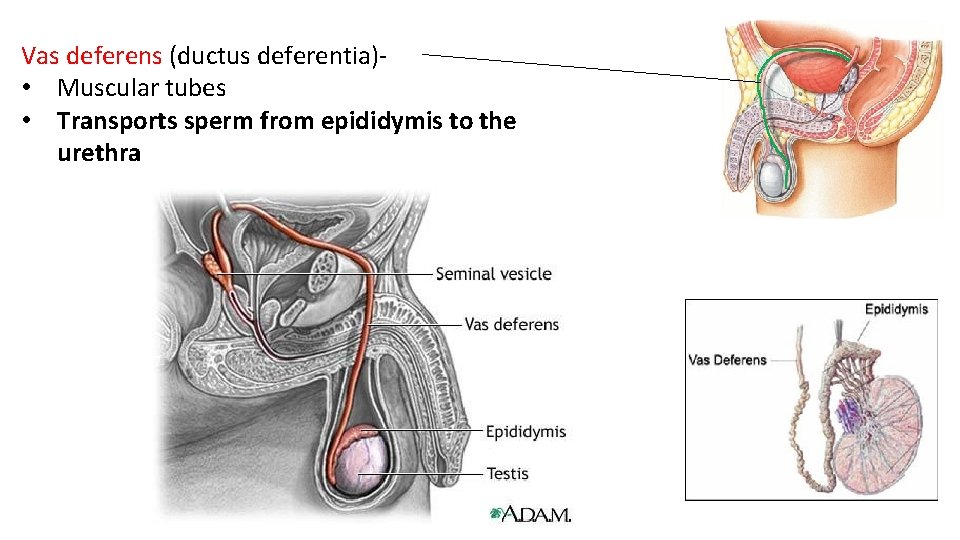
Vas deferens (ductus deferentia)- • Muscular tubes • Transports sperm from epididymis to the urethra

Fun Fact!!! A vasectomy is an operation that makes a man permanently unable to get a woman pregnant. • It involves cutting the vas deferens so that sperm can no longer get into the semen. F. A. Q: Q. Will I still be able to ejaculate after vasectomy? A. Yes, semen is made in the seminal vesicles and the prostate gland. These are not affected by a vasectomy. Sperm make up only 2 to 5 per cent of the ejaculate so you will not be able to notice any difference in the volume of your ejaculate. Q. Will I still make sperm after my vasectomy? A. Yes, sperm continue to be made in the testes after a vasectomy. After time, however, production of sperm is often reduced. Q. After my vasectomy where do the sperm go? A. The sperm, which are made in the testicles, cannot pass through the vas deferens once they have been cut and tied, so they are reabsorbed by the body.

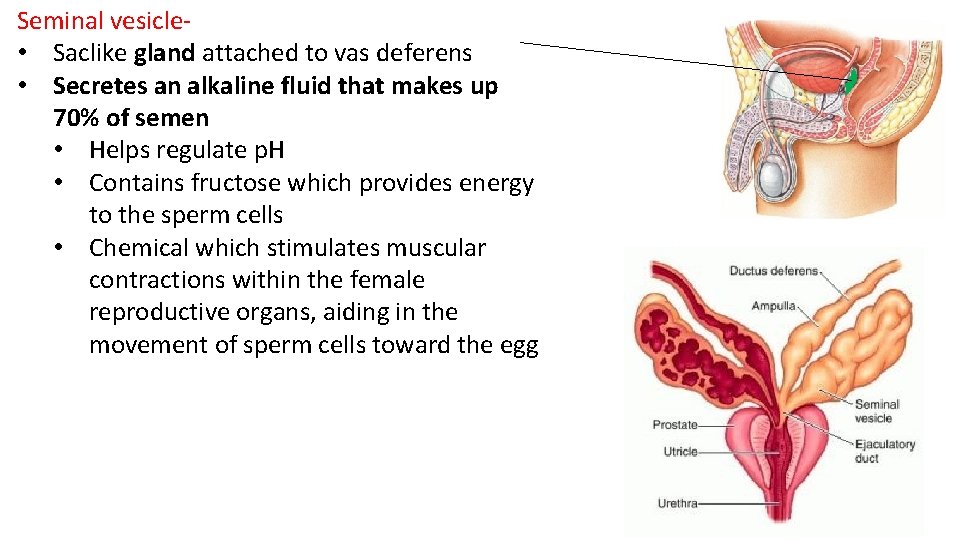
Seminal vesicle- • Saclike gland attached to vas deferens • Secretes an alkaline fluid that makes up 70% of semen • Helps regulate p. H • Contains fructose which provides energy to the sperm cells • Chemical which stimulates muscular contractions within the female reproductive organs, aiding in the movement of sperm cells toward the egg

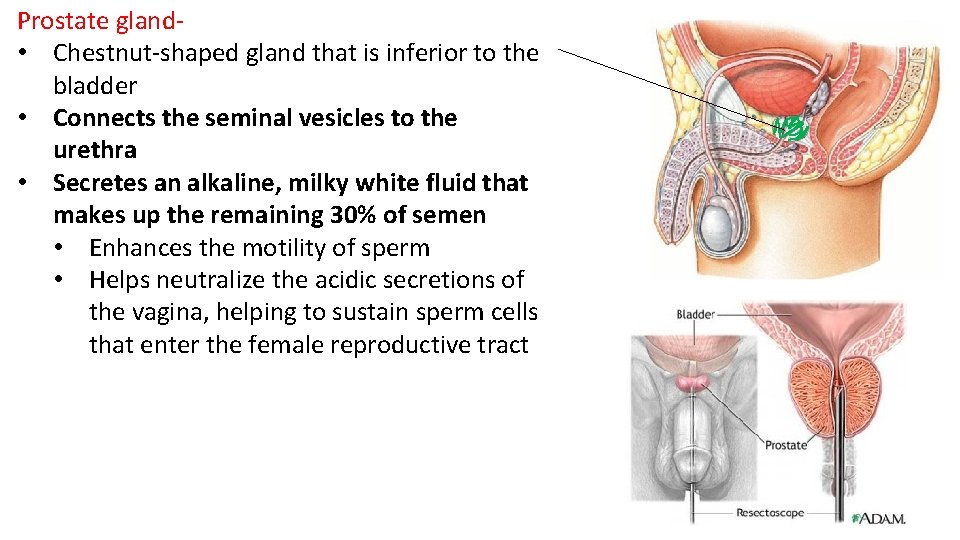
Prostate gland- • Chestnut-shaped gland that is inferior to the bladder • Connects the seminal vesicles to the urethra • Secretes an alkaline, milky white fluid that makes up the remaining 30% of semen • Enhances the motility of sperm • Helps neutralize the acidic secretions of the vagina, helping to sustain sperm cells that enter the female reproductive tract

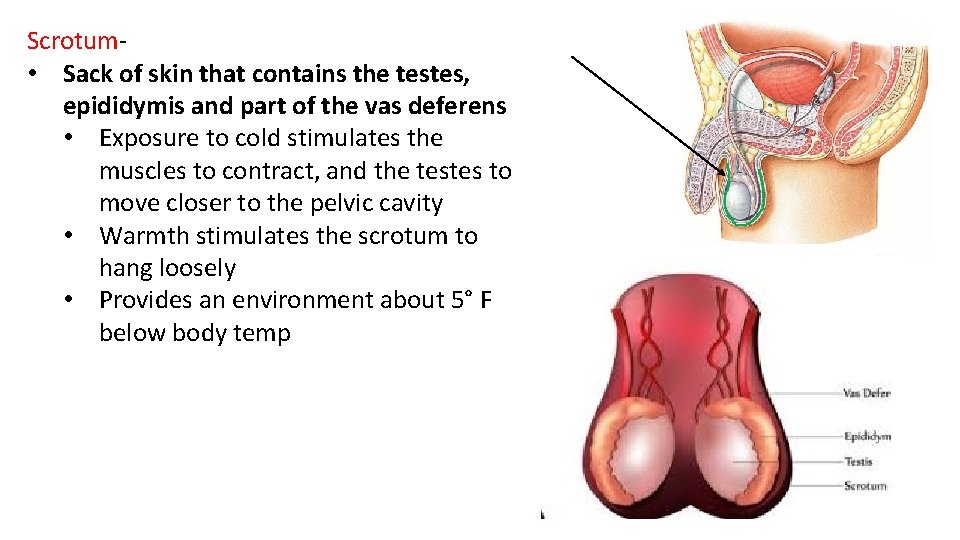
Scrotum- • Sack of skin that contains the testes, epididymis and part of the vas deferens • Exposure to cold stimulates the muscles to contract, and the testes to move closer to the pelvic cavity • Warmth stimulates the scrotum to hang loosely • Provides an environment about 5° F below body temp

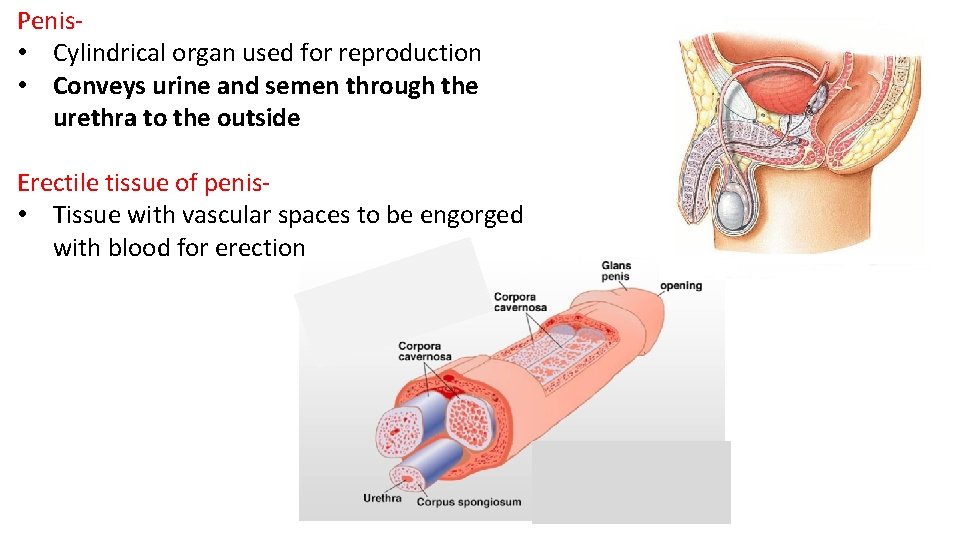
Penis- • Cylindrical organ used for reproduction • Conveys urine and semen through the urethra to the outside Erectile tissue of penis- • Tissue with vascular spaces to be engorged with blood for erection

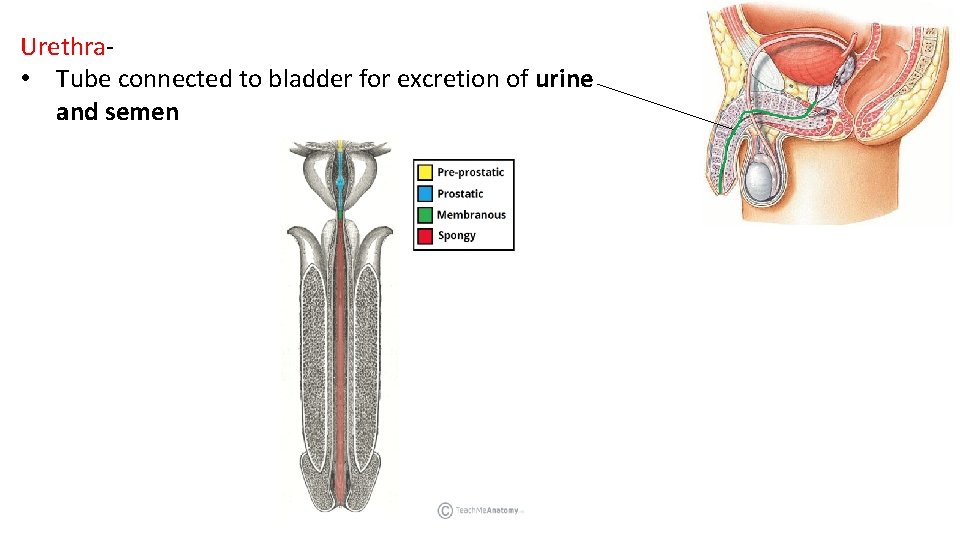
Urethra- • Tube connected to bladder for excretion of urine and semen

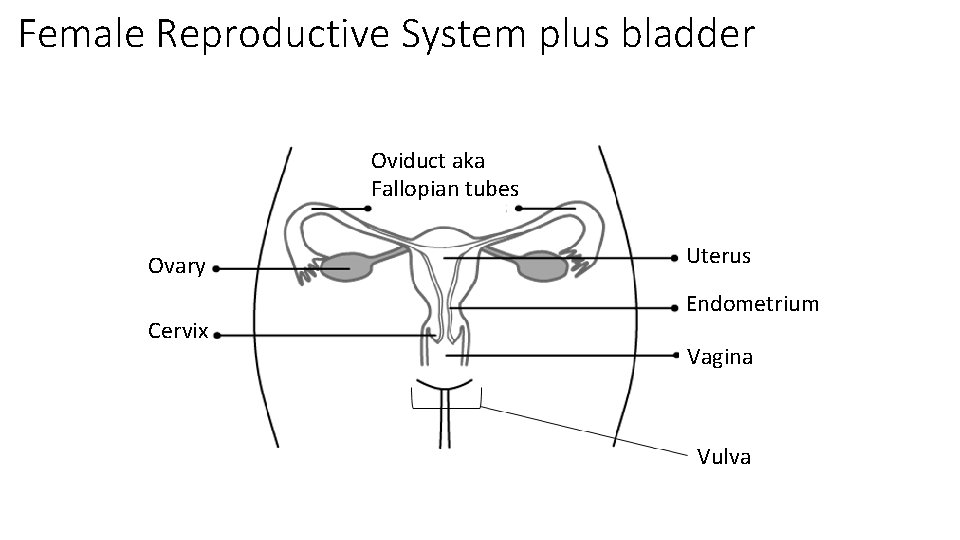
Female Reproductive System plus bladder Oviduct aka Fallopian tubes Ovary Cervix Uterus Endometrium Vagina Vulva

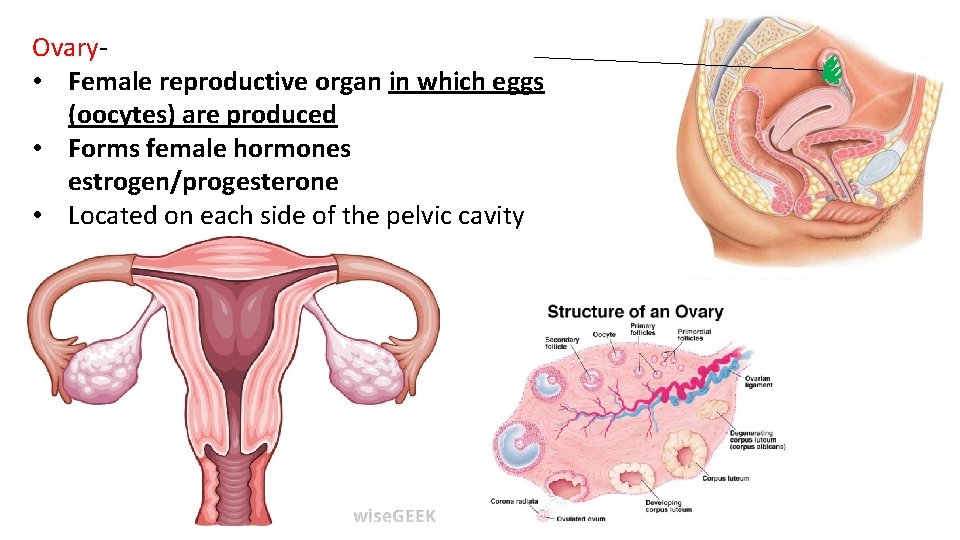
Ovary- • Female reproductive organ in which eggs (oocytes) are produced • Forms female hormones estrogen/progesterone • Located on each side of the pelvic cavity

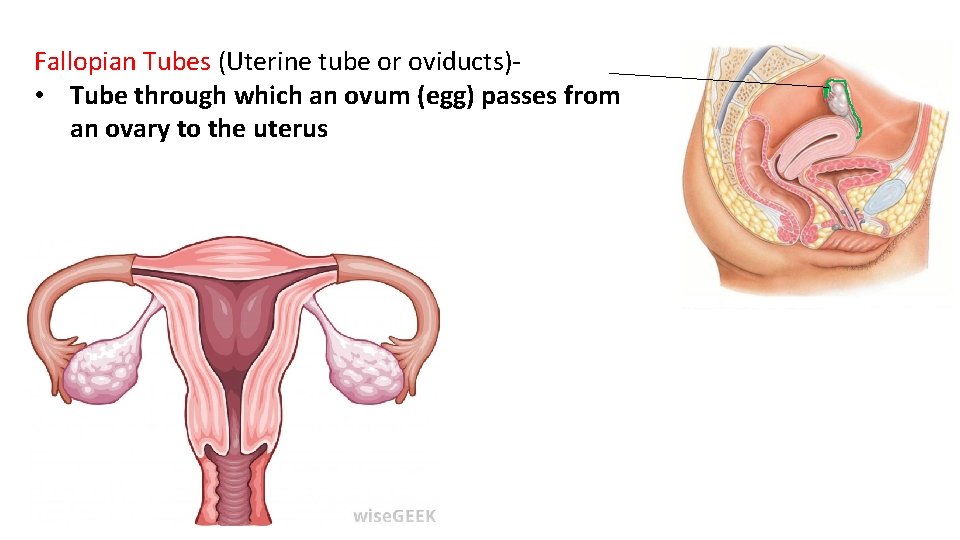
Fallopian Tubes (Uterine tube or oviducts) • Tube through which an ovum (egg) passes from an ovary to the uterus

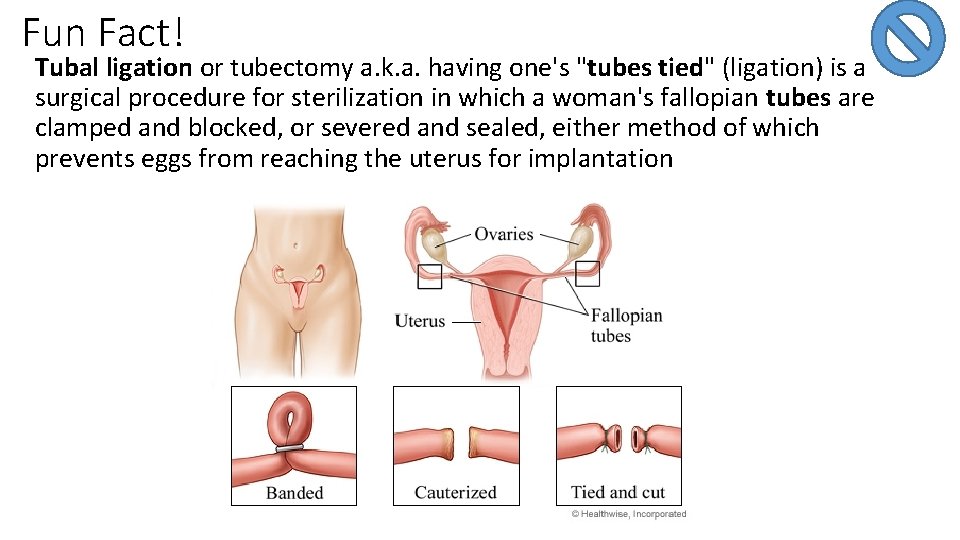
Fun Fact! Tubal ligation or tubectomy a. k. a. having one's "tubes tied" (ligation) is a surgical procedure for sterilization in which a woman's fallopian tubes are clamped and blocked, or severed and sealed, either method of which prevents eggs from reaching the uterus for implantation

Critical Thinking Question If a woman who is considering having tubal ligation asks, “Will the operation cause me to go though my change of life early? ”, how would you answer?

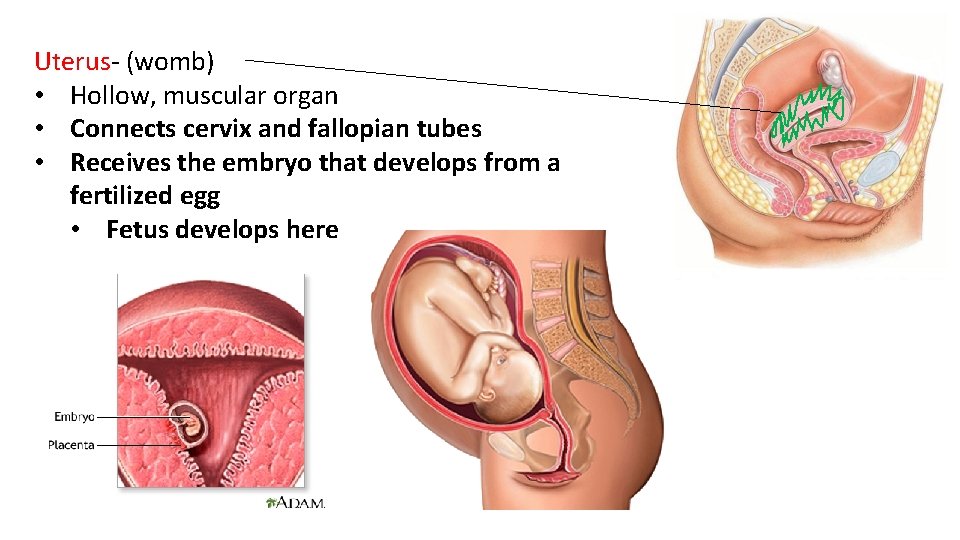
Uterus- (womb) • Hollow, muscular organ • Connects cervix and fallopian tubes • Receives the embryo that develops from a fertilized egg • Fetus develops here

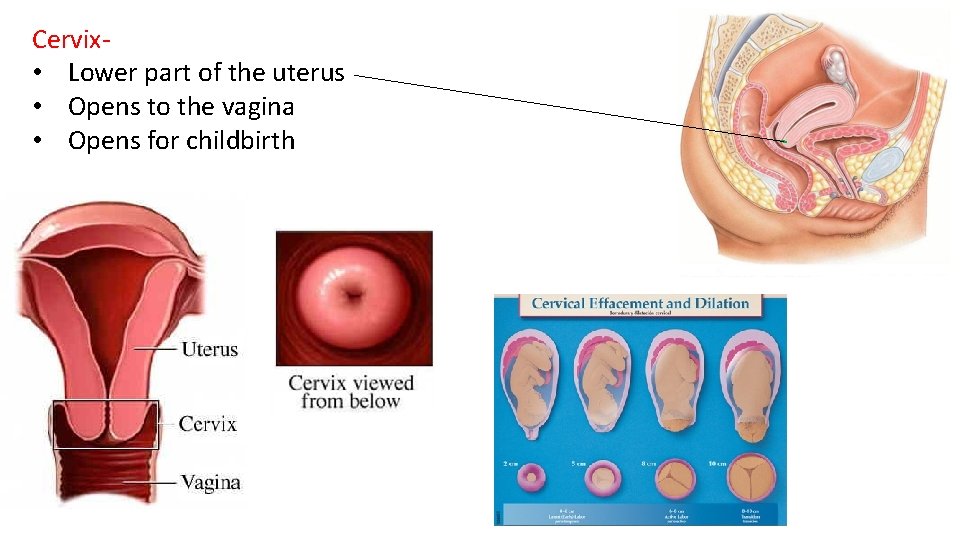
Cervix- • Lower part of the uterus • Opens to the vagina • Opens for childbirth

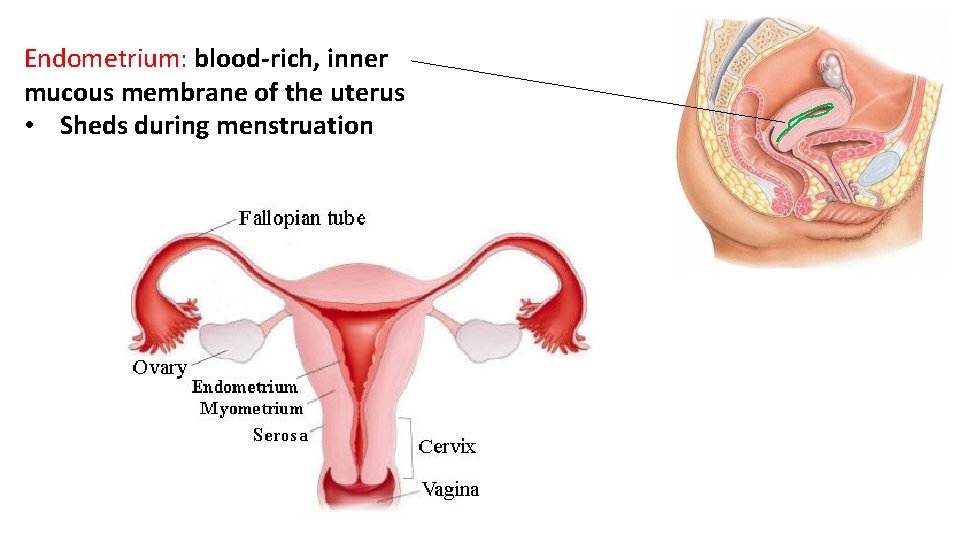
Endometrium: blood-rich, inner mucous membrane of the uterus • Sheds during menstruation

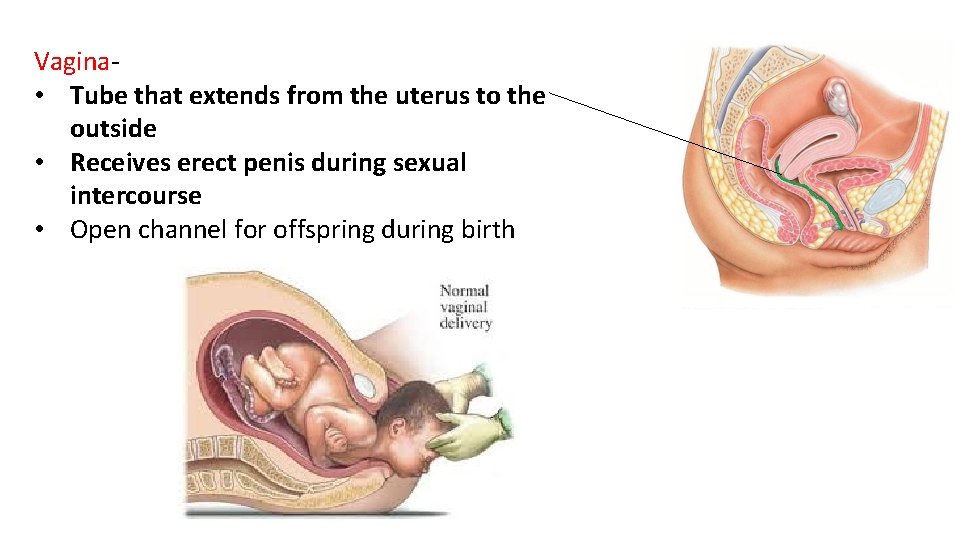
Vagina- • Tube that extends from the uterus to the outside • Receives erect penis during sexual intercourse • Open channel for offspring during birth

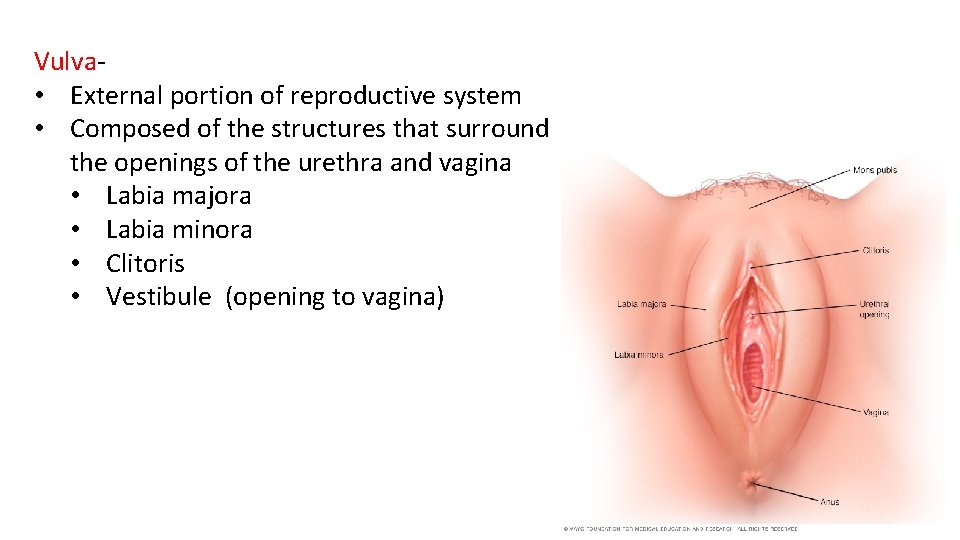
Vulva • External portion of reproductive system • Composed of the structures that surround the openings of the urethra and vagina • Labia majora • Labia minora • Clitoris • Vestibule (opening to vagina)

Crash Course: Reproduction System 12 m 3 s • 10 -15 bullets on p. 66 • https: //www. youtube. com/watch? v=_7 rs. H 2 lo. IY 8

Disorder of Reproductive System Use the internet to write a short summary on a disorder/disease of either the male or female reproductive system: • Name/short description of disorder: • Cause: • Symptoms: • Treatment: • If left untreated? : • Does it affect fertility? : Bottom ½ of p. 66