Splints for the NBCOT Stephanie Shane OTRL NBCOT

Splints for the NBCOT Stephanie Shane OTR/L NBCOT Tutor

C bar splint Median Nerve Injury Used to maintain web space No joint stabilization

Flail arm splint Brachial Plexus Injury (BPI)
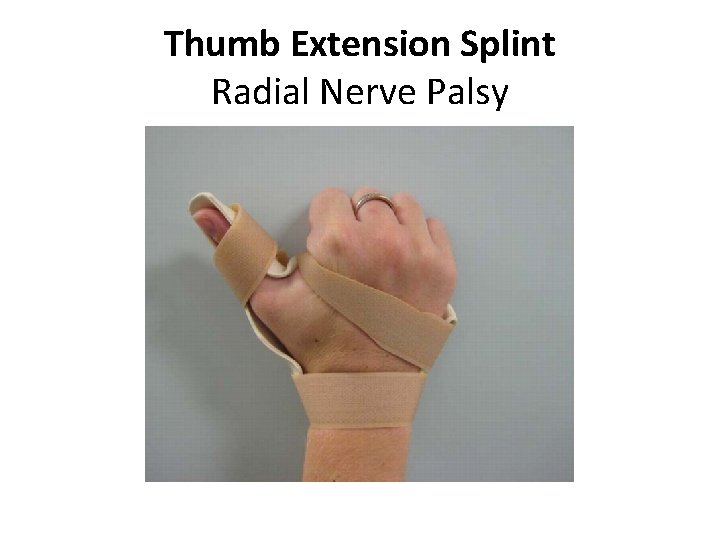
Thumb Extension Splint Radial Nerve Palsy
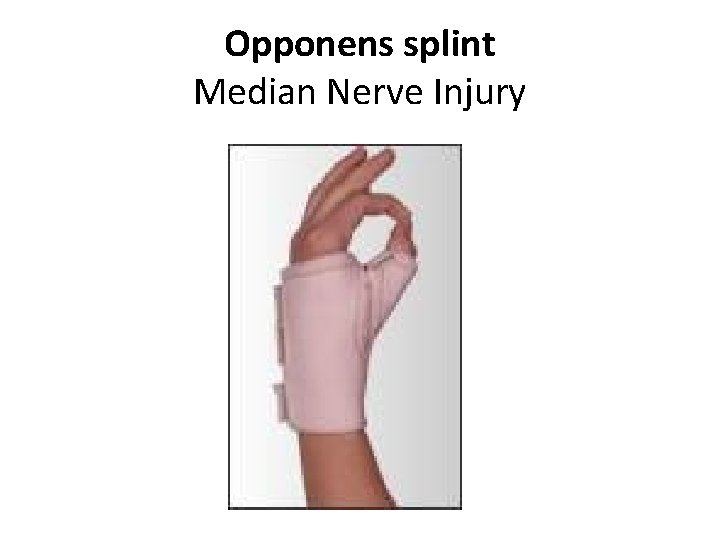
Opponens splint Median Nerve Injury
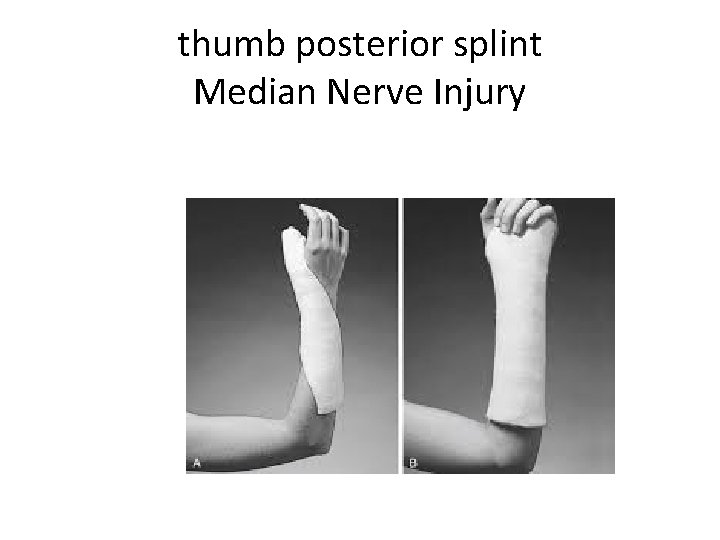
thumb posterior splint Median Nerve Injury
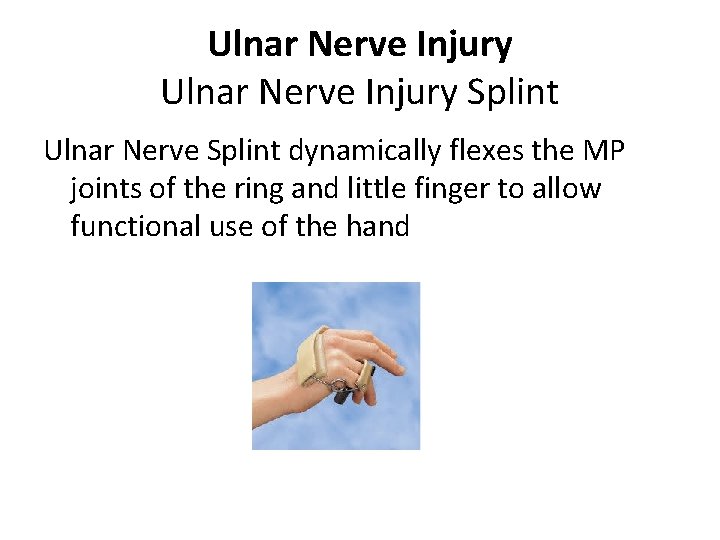
Ulnar Nerve Injury Splint Ulnar Nerve Splint dynamically flexes the MP joints of the ring and little finger to allow functional use of the hand
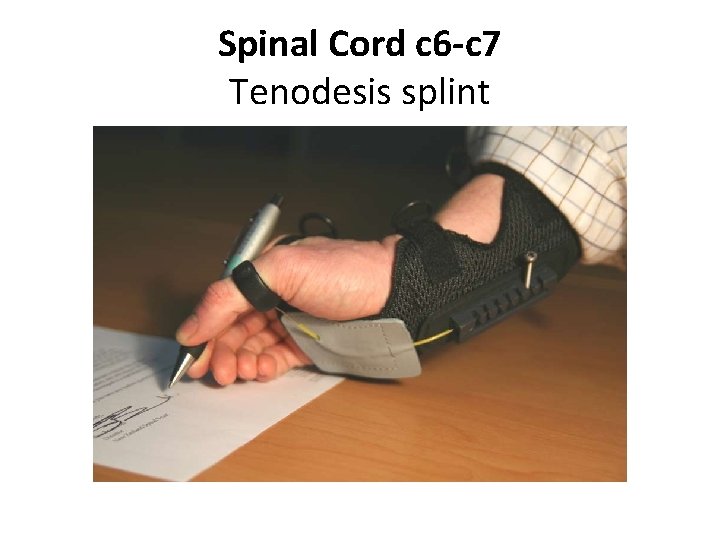
Spinal Cord c 6 -c 7 Tenodesis splint
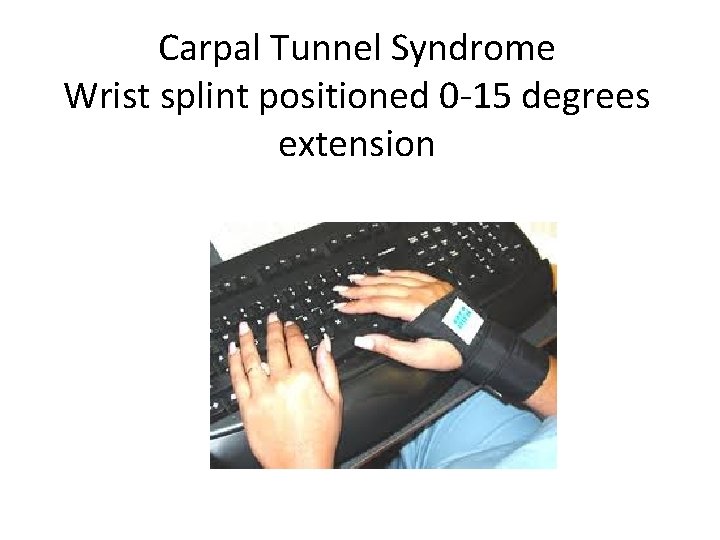
Carpal Tunnel Syndrome Wrist splint positioned 0 -15 degrees extension
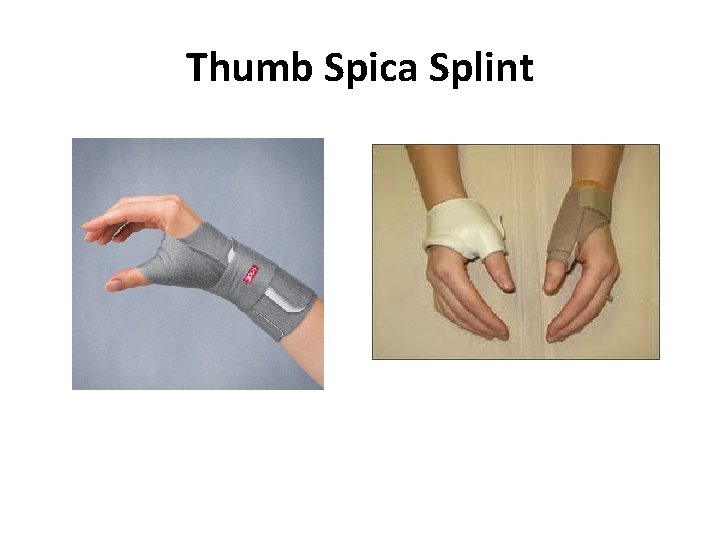
Thumb Spica Splint
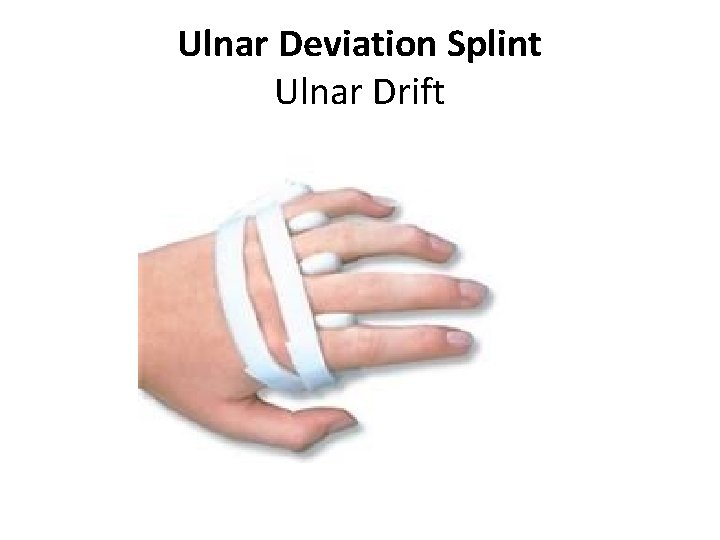
Ulnar Deviation Splint Ulnar Drift
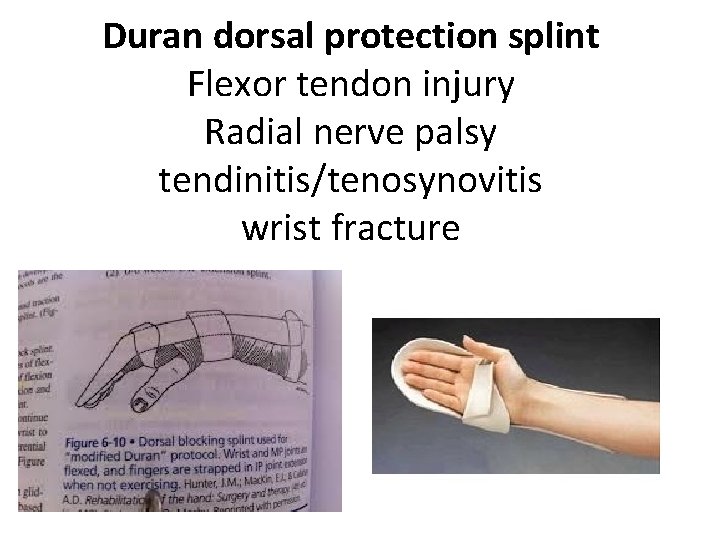
Duran dorsal protection splint Flexor tendon injury Radial nerve palsy tendinitis/tenosynovitis wrist fracture

Silver rings Swan Neck Deformity

Boutonniere

Resting splint Flaccidity
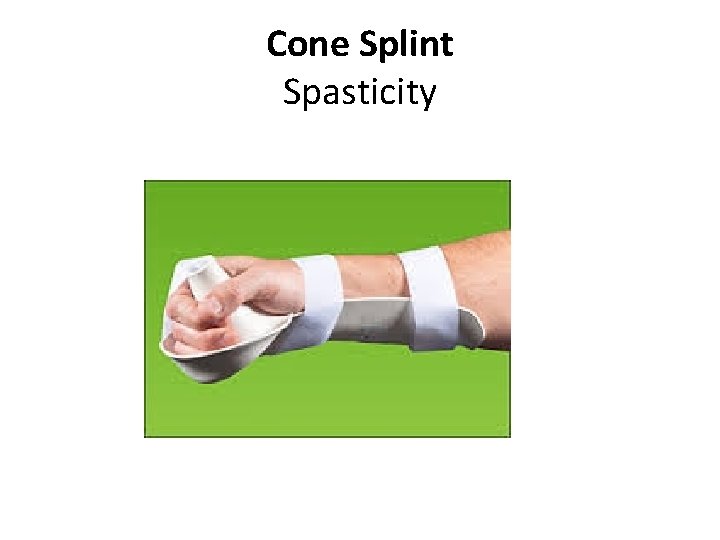
Cone Splint Spasticity

Airplane Splint Burns
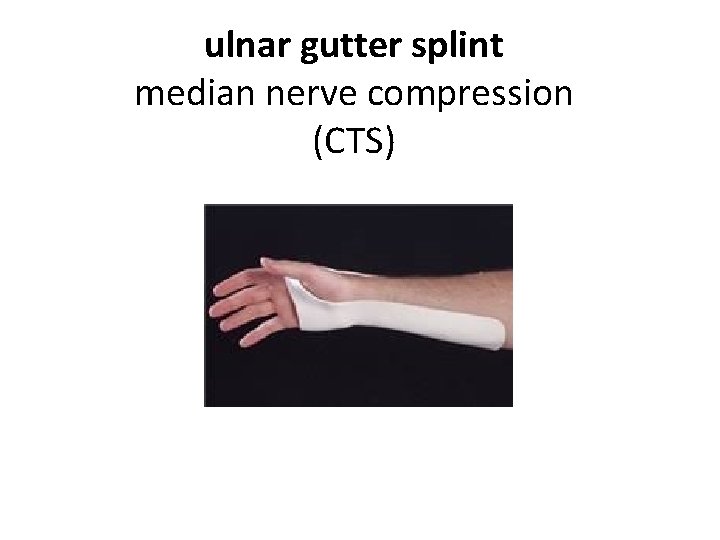
ulnar gutter splint median nerve compression (CTS)
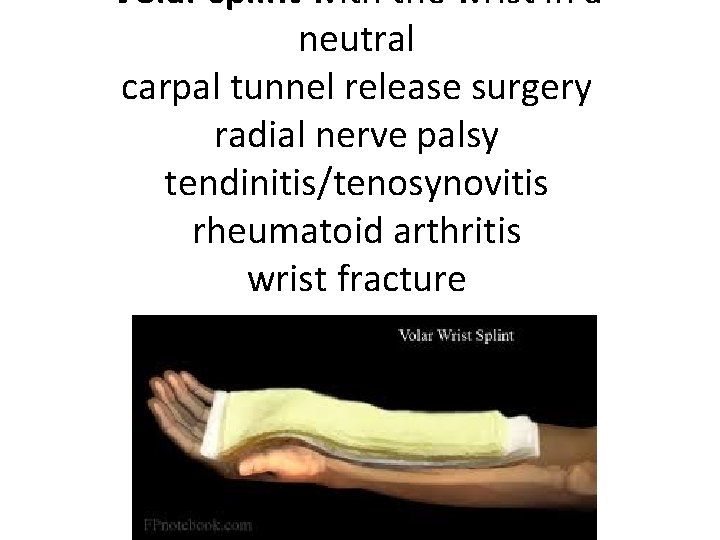
Volar splint with the wrist in a neutral carpal tunnel release surgery radial nerve palsy tendinitis/tenosynovitis rheumatoid arthritis wrist fracture

general considerations of splinting • • • Comfort - Function - Cosmesis - Patient acceptance and compliance - Patient education - Tratment plan integration

common splinting precautions • • Preexisting skin problems -Bony prominences -Friction -Pressure spots

NBCOT QUESTIONS • When assessing an individual who is suspected of having carpal tunnel syndrome, the OT tests for Tinel’s sign by gently tapping the median nerve at the level of the: – elbow – mid-forearm – palmar crease – carpal tunnel

• An OT practitioner documents that an individual exhibits elbow flexion strength of grade 1. according to the manual muscle test system of letters and numbers, the word that would be the equivalent of grade 1 would be: – absent – trace – good – normal

• An individual is able to complete the full range of shoulder flexion while in a side-lying position during an evaluation. However, against gravity, the individual is not quite able to achieve 75% of the range for shoulder flexion. This muscle should be graded as: – Good (4) – Fair (3) – Fair minus (3 -) – Poor plus (2+)

• A method that an OT practitioner can use to document total finger flexion without recording the measurement in degrees would be to measure the: – Passive flexion at each joint and total the numbers. – Distance from the fingertip to the distal palmar crease with the hand in a fist. – Active flexion at each joint and total the measurements. – Distance between the tip of the thumb and the tip of the fourth finger.

• An OT practitioner is assessing the range of motion of an individual who actively demonstrates internal rotation of the shoulder to 70 degrees. The practitioner would MOST likely document this measurement as: – Within normal limits. – Within functional limits. – Hypermobility that requires further treatment.

• An OT practitioner measures an individual’s elbow PROM three times, and gets three different measurements, varying by up to 10 degrees. The BEST action for therapist to take is to: – Check the alignment of the goniometer. – Use a larger goniometer. – Use a smaller goniometer. – Attempt to force the individual’s arm further into flexion.

• An OT practitioner is evaluating two-point discrimination in an individual with median nerve injury. The MOST appropriate procedure is to: – Apply the stimuli beginning at the little finger and progress toward the thumb. – Test the thumb area first, then progress toward the little finger. – Present test stimuli in an organized pattern to improve reliability during retesting. – Allow the individual unlimited time to respond.

• An individual’s PIP joint appears flexed, and the DIP joint appears hyperextended. The OT can BEST document this condition as a: – Mallet deformity. – Boutonniere deformity. – Subluxation deformity. – Swan neck deformity.
- Slides: 29