Spinal Cord Tumors Done by Roaa Jaradat Aya

Spinal Cord Tumors Done by: Roa’a Jaradat Aya Tawalbeh
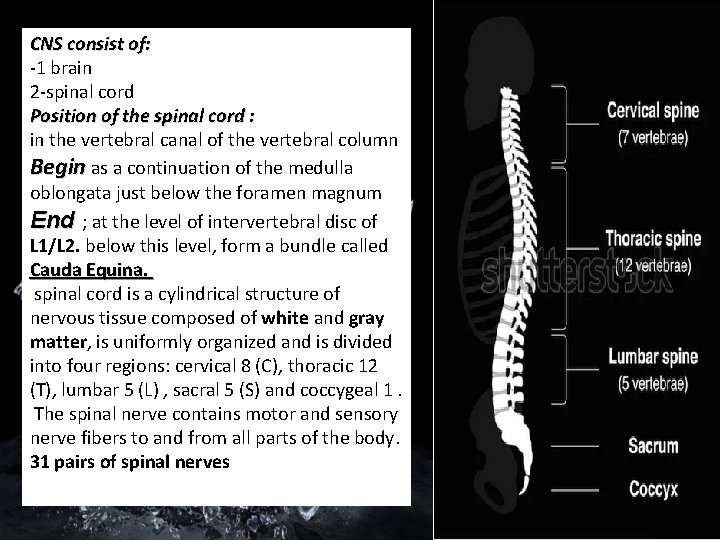
CNS consist of: -1 brain 2 -spinal cord Position of the spinal cord : in the vertebral canal of the vertebral column Begin as a continuation of the medulla oblongata just below the foramen magnum End ; at the level of intervertebral disc of L 1/L 2. below this level, form a bundle called Cauda Equina. spinal cord is a cylindrical structure of nervous tissue composed of white and gray matter, is uniformly organized and is divided into four regions: cervical 8 (C), thoracic 12 (T), lumbar 5 (L) , sacral 5 (S) and coccygeal 1. The spinal nerve contains motor and sensory nerve fibers to and from all parts of the body. 31 pairs of spinal nerves
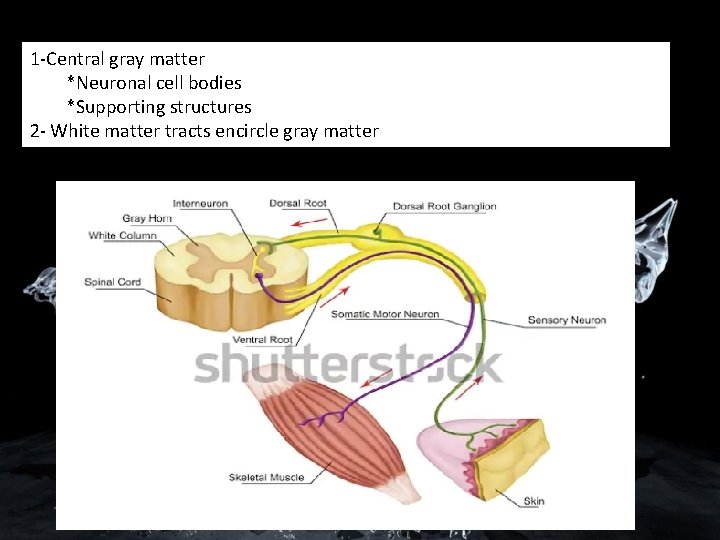
1 -Central gray matter *Neuronal cell bodies *Supporting structures 2 - White matter tracts encircle gray matter

Arterial supply: The vertebral blood supply for the spinal cord comes from many different sources in the body depending on the region. The main blood supply to the spinal cord is via the single anterior spinal artery (ASA) and the two posteriorspinal arteries (PSA). Venous supply: The spinal cord drains via the single anterior spinal vein and single posterior spinal vein which in turn drain into the internal vertebral venous plexus located in the epidural space within the extradural fat. These veins eventually empty into the external vertebral venous plexus via the basivertebral veins.

Spinal tumors Are neoplasmas located in either the vertebral column or the spinal cord. Primary spinal cord tumors arise from the different elements of the CNS, including neurons, supporting glial cells, and meninges. Metastatic lesions cause 85% of the cases of neoplastic spinal cord compression. The clinical presentation tends to be indistinguishable from that of primary cancers of the spine. There are three main types of spinal tumors classified based on their location: extradural and intradural (intradural-intramedullary and intradural-extramedullary). Extradural tumors are located outside the dura matter lining and are most commonly metastatic. Intradural tumors are located inside the dura mater lining and are further subdivided into intramedullary and extramedullary tumors. Intradural-intramedullary tumors are located within the dura and spinal cord parenchyma, while intradural-extramedullary tumors are located within the dura but outside the spinal cord parenchyma.

Metastatic spinal cord compression usually follows hematogenous dissemination of malignant cells to the vertebral bodies, with subsequent expansion into the epidural space. Spread into the epidural space may occur by means of tumor extension through the intervertebral foramina or hematogenous spread by way of the Batson venous plexus. Most frequently, metastatic seeding appears in the thoracic spine (accounting for about 70% of cases), with the lumbar (20% of cases) *cervical 10% of cases. *Multiple spinal levels , 30% of patients. Systemic cancers with a tendency for spinal cord metastasis include the following: breast, prostate, renal, or lung neoplasms; lymphoma; sarcoma; and multiple myeloma. Gastrointestinal and pelvic malignancies tend to affect the lumbosacral spine lung and breast cancers are more likely to affect the thoracic spine. Metastases to the substance of the cord (intramedullary) are relatively rare.

Symptoms 1 -Pain at the site of the tumor due to tumor growth 2 -Back pain, often radiating to other parts of your body and worse at night 3 -Feeling less sensitive to pain, heat and cold 4 -Loss of bowel or bladder function 5 -Difficulty walking, sometimes leading to falls 6 -Loss of sensation or muscle weakness, especially in your arms or legs NOTE : Muscle weakness , which may be mild or severe, in different parts of your body Back pain is a common early symptom of spinal tumors. Complications Spinal tumors can compress spinal nerves, leading to a loss of movement or sensation below the location of the tumor. This can sometimes cause changes in bowel and bladder function. Nerve damage may be permanent. However, if caught early and treated aggressively, it may be possible to prevent further loss of function and regain nerve function. Depending on its location, a tumor that presses against the spinal cord itself may be life-threatening. Spinal tumors progress at different rates depending on the type of tumor
Benign: Extradural tumors 1. Hemangioma. 2. Osteoid osteoma. 3. Osteoblastoma. 4. Osteochondroma. 5. Giant cell tumor. MALIGNANT : 1. osteosarcoma 2. chondrosarcoma 3. multiple myeloma 4. chordoma 5. lymphoma 6. mets
Benign extradural tumor
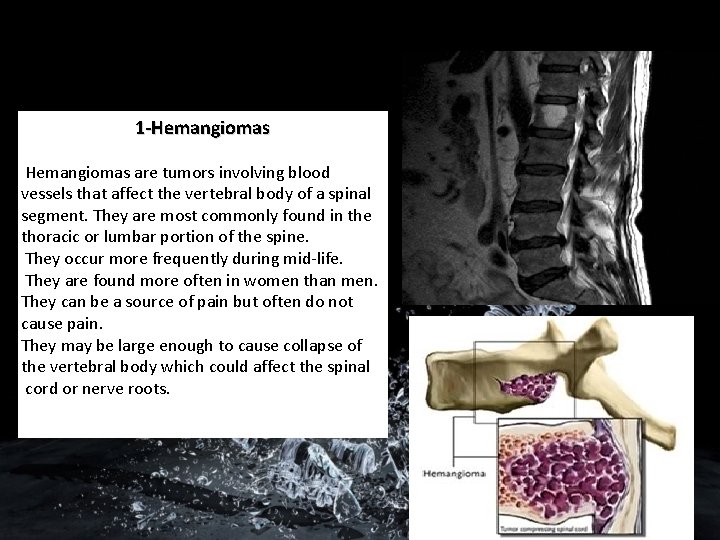
1 -Hemangiomas are tumors involving blood vessels that affect the vertebral body of a spinal segment. They are most commonly found in the thoracic or lumbar portion of the spine. They occur more frequently during mid-life. They are found more often in women than men. They can be a source of pain but often do not cause pain. They may be large enough to cause collapse of the vertebral body which could affect the spinal cord or nerve roots.
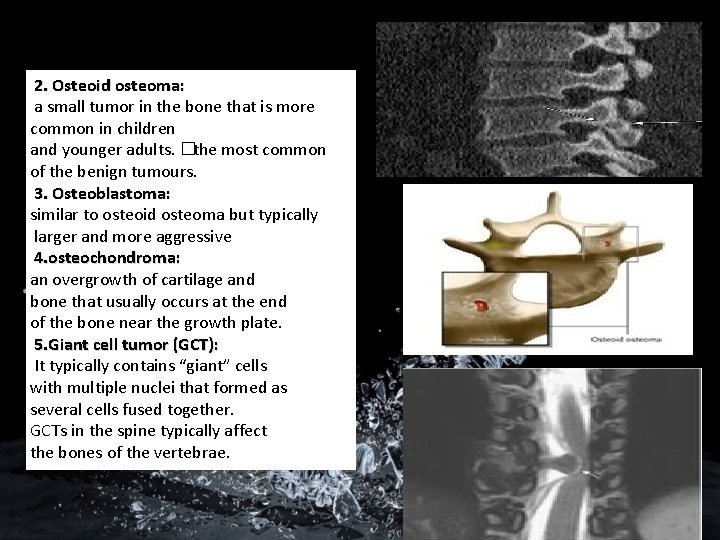
2. Osteoid osteoma: a small tumor in the bone that is more common in children and younger adults. �the most common of the benign tumours. 3. Osteoblastoma: similar to osteoid osteoma but typically larger and more aggressive 4. osteochondroma: an overgrowth of cartilage and bone that usually occurs at the end of the bone near the growth plate. 5. Giant cell tumor (GCT): It typically contains “giant” cells with multiple nuclei that formed as several cells fused together. GCTs in the spine typically affect the bones of the vertebrae.

Malignant Extradural tumors
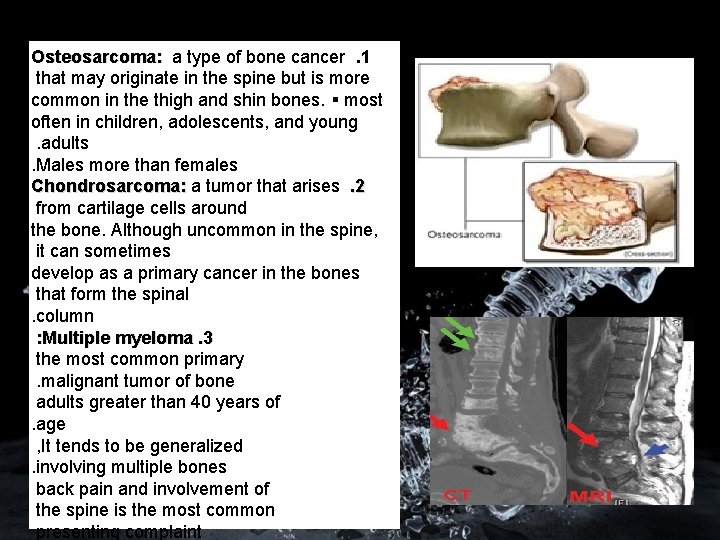
Osteosarcoma: a type of bone cancer. 1 that may originate in the spine but is more common in the thigh and shin bones. most often in children, adolescents, and young. adults. Males more than females Chondrosarcoma: a tumor that arises. 2 from cartilage cells around the bone. Although uncommon in the spine, it can sometimes develop as a primary cancer in the bones that form the spinal. column : Multiple myeloma. 3 the most common primary. malignant tumor of bone adults greater than 40 years of. age , It tends to be generalized. involving multiple bones back pain and involvement of the spine is the most common presenting complaint
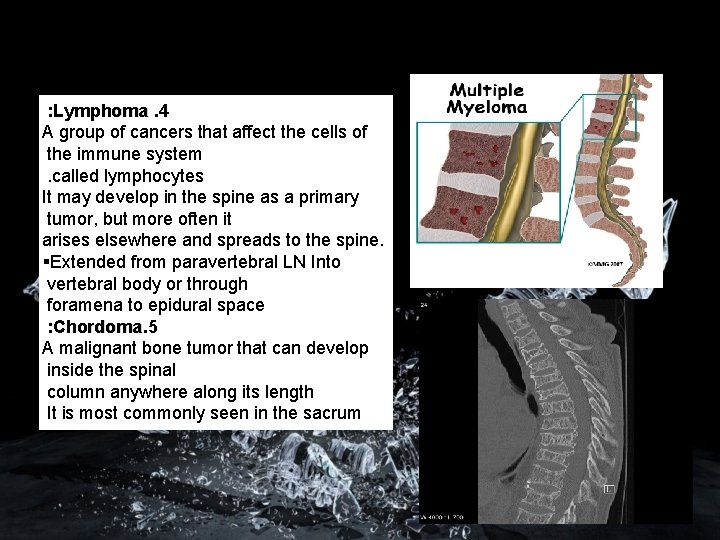
: Lymphoma. 4 A group of cancers that affect the cells of the immune system. called lymphocytes It may develop in the spine as a primary tumor, but more often it arises elsewhere and spreads to the spine. Extended from paravertebral LN Into vertebral body or through foramena to epidural space : Chordoma. 5 A malignant bone tumor that can develop inside the spinal column anywhere along its length It is most commonly seen in the sacrum

. . Testing & Diagnosis : X-Ray (1. They are not very reliable in diagnosing tumors. CT scan (2 MRI(modality of choice for diagnosis and pre operative evaluation) (3. Bone Scan (4 Biopsy (5 may be needed if diagnosis is unclear or if concern for malignancy. vs benign tumor type If the tumor is malignant, a biopsy also helps determine the. cancer's type, which subsequently determines treatment options

Treatment. . . Pharmacological treatment: limited benefit Chemotherapeutic regimens : imited success in the treatment of. spinal cord neoplasms * This may be partly due to the inability of the chemotactic agents to cross the blood-brain barrier. Surgical Therapy *gross total resection. * The neoplasm is identified and then biopsy is performed. *Surgery then proceeds based on the histology from the frozen specimen. * If the lesion is an astrocytoma, then the goal is debulking the tumor while not injuring the normal neural tracts. Ependymomas are attempted to be resected completely as long as a viable plane can be established and normal neural tracts are not disturbed.
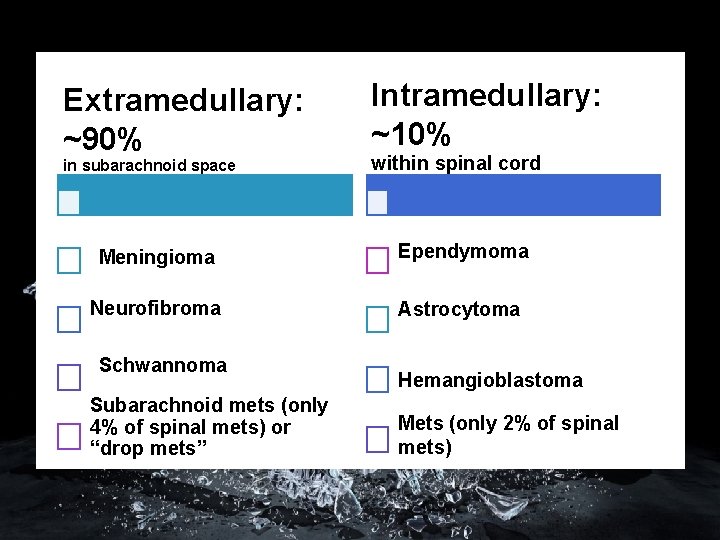
Extramedullary: ~90% in subarachnoid space Intramedullary: ~10% within spinal cord Meningioma Ependymoma Neurofibroma Astrocytoma Schwannoma Subarachnoid mets (only 4% of spinal mets) or “drop mets” Hemangioblastoma Mets (only 2% of spinal mets)
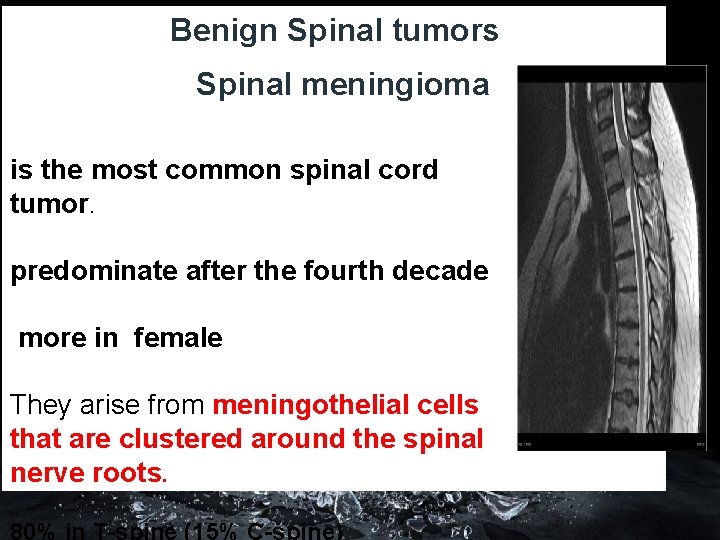
Benign Spinal tumors Spinal meningioma is the most common spinal cord tumor. predominate after the fourth decade more in female They arise from meningothelial cells that are clustered around the spinal nerve roots.

Spinal Meningioma • symptoms generally don’t occur unless your tumor has begun to press on your spinal cord. • Spinal meningioma symptoms may include: • Difficulty walking or maintaining balance • Weakness • Pain at the tumor site • Loss of bowel or bladder control • Loss of sensation
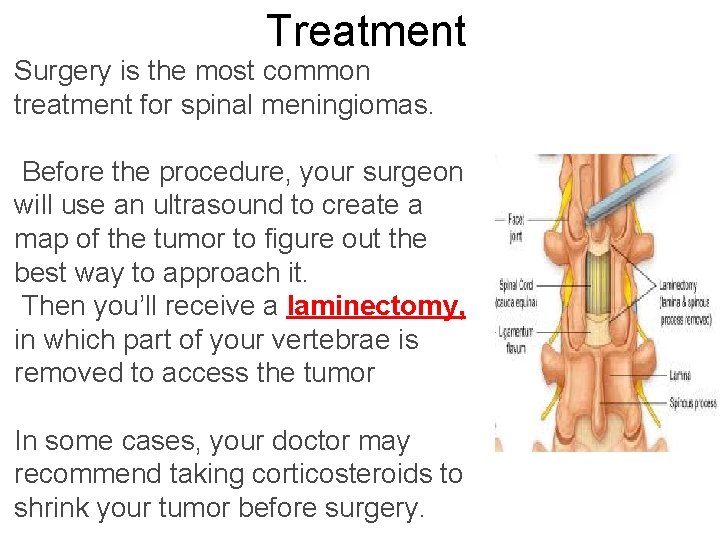
Treatment Surgery is the most common treatment for spinal meningiomas. Before the procedure, your surgeon will use an ultrasound to create a map of the tumor to figure out the best way to approach it. Then you’ll receive a laminectomy, in which part of your vertebrae is removed to access the tumor In some cases, your doctor may recommend taking corticosteroids to shrink your tumor before surgery.
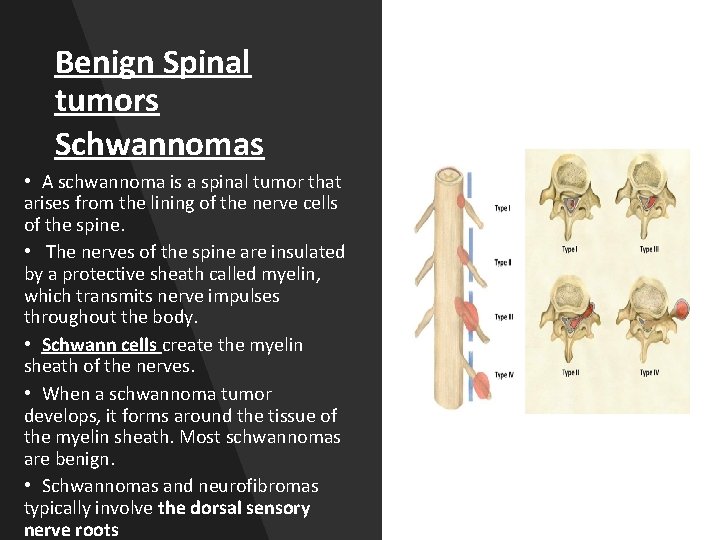
Benign Spinal tumors Schwannomas • A schwannoma is a spinal tumor that arises from the lining of the nerve cells of the spine. • The nerves of the spine are insulated by a protective sheath called myelin, which transmits nerve impulses throughout the body. • Schwann cells create the myelin sheath of the nerves. • When a schwannoma tumor develops, it forms around the tissue of the myelin sheath. Most schwannomas are benign. • Schwannomas and neurofibromas typically involve the dorsal sensory nerve roots
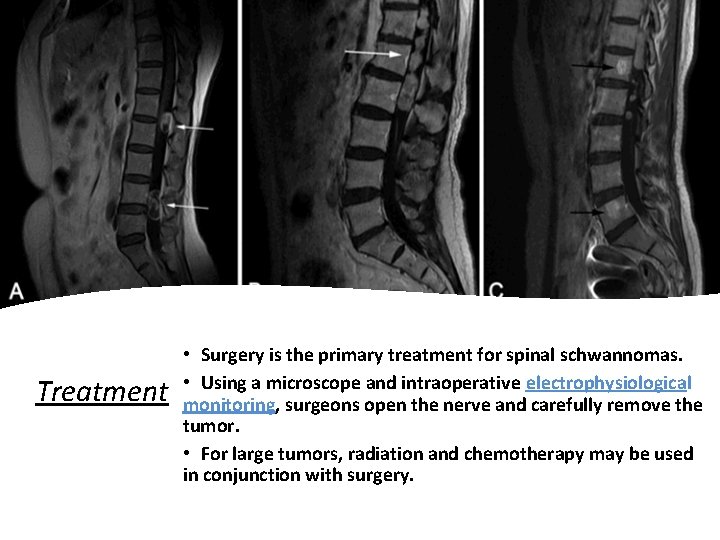
Treatment • Surgery is the primary treatment for spinal schwannomas. • Using a microscope and intraoperative electrophysiological monitoring, surgeons open the nerve and carefully remove the tumor. • For large tumors, radiation and chemotherapy may be used in conjunction with surgery.
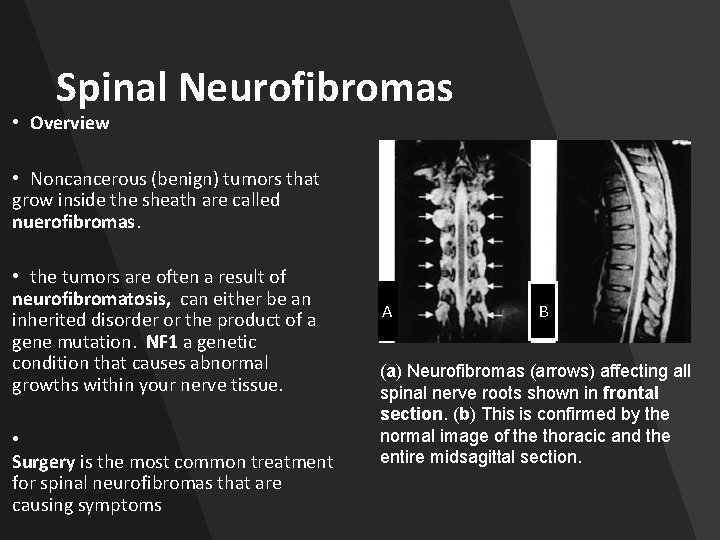
Spinal Neurofibromas • Overview • Noncancerous (benign) tumors that grow inside the sheath are called nuerofibromas. • the tumors are often a result of neurofibromatosis, can either be an inherited disorder or the product of a gene mutation. NF 1 a genetic condition that causes abnormal growths within your nerve tissue. • Surgery is the most common treatment for spinal neurofibromas that are causing symptoms A B (a) Neurofibromas (arrows) affecting all spinal nerve roots shown in frontal section. (b) This is confirmed by the normal image of the thoracic and the entire midsagittal section.
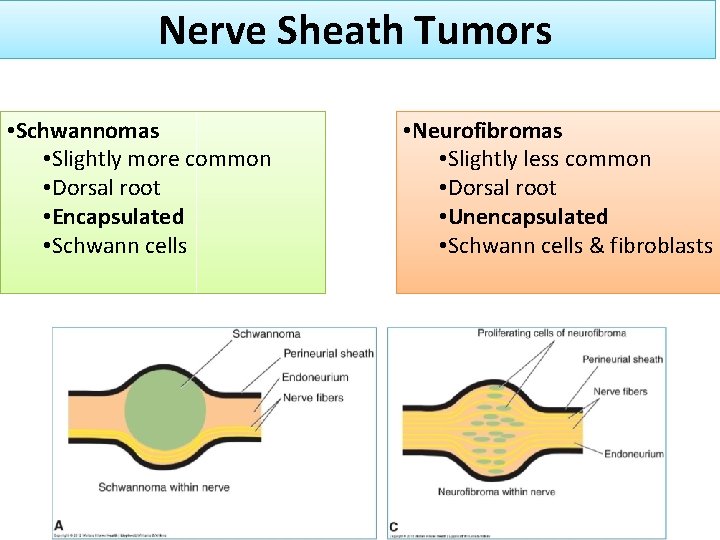
Nerve Sheath Tumors • Schwannomas • Slightly more common • Dorsal root • Encapsulated • Schwann cells • Neurofibromas • Slightly less common • Dorsal root • Unencapsulated • Schwann cells & fibroblasts

Intramedullary tumor Overview: Intramedullary tumors are located inside the substance of the spinal cord. These tumors usually arise from glia (supporting cells) within the spinal cord. Astrocytomas and ependymomas account for the majority and occur with about equal frequency< although astrocytomas are more common in children and ependymomas more common in adults. Hemangioblastomas, tumors of blood vessels, are less common
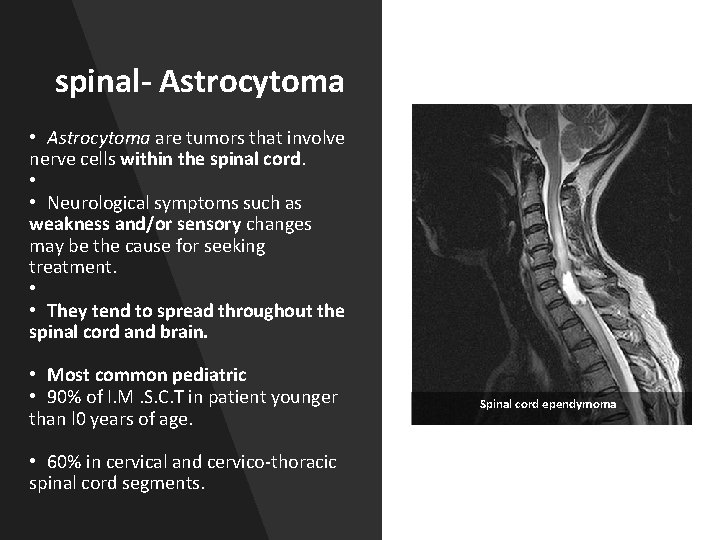
spinal- Astrocytoma • Astrocytoma are tumors that involve nerve cells within the spinal cord. • • Neurological symptoms such as weakness and/or sensory changes may be the cause for seeking treatment. • • They tend to spread throughout the spinal cord and brain. • Most common pediatric • 90% of I. M. S. C. T in patient younger than l 0 years of age. • 60% in cervical and cervico-thoracic spinal cord segments. Spinal cord ependymoma
Eependymomas Most common I. M. T in adults. Middle age adult (most frequent) Men = women Mostly in filium terminale and lower thoracic spine Variety of histological subtypes. • Cellular ependymoma (most common) • Epithelial • Tanycytic (fibrillary) • Sub ependymomas • myxopapillary • mixed • almost All are histologically benign • Unencapsulated and well circumscribed glial derived tumor. • • •
Surgical Therapy • If the lesion is an astrocytoma, then the goal is debulking the tumor while not injuring the normal neural tracts. • Ependymomas are attempted to be resected completely as long as a viable plane can be established and normal neural tracts are not disturbed.

Hemangioblastomas • are vascular tumors of the central nervous system that originate from the vascular system • 15 -25% occur in association with von hippel- lindau Syndrome. • Rare in childhood. (common in middle age) • Benign tumor of vascular origin. • Sharply circumscribed not encapsulated. • Most are dorsally or dorsolaterally located.
• Spinal arteriography: • This is beneficial only if a hemangioblastoma is suggested as a differential diagnosis. Hemangioblastoma arteriography findings include a vascular blush with a prominent draining vein.

THANK YOU
- Slides: 31