Spinal Cord Injury Chapter 61 Copyright 2014 by

Spinal Cord Injury Chapter 61 Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Spinal Cord Injury (SCI) Damage or trauma to spinal cord 12, 000 new SCIs each year 260, 000 Americans living with SCI Highest in males ages 16 -30 ↑ In older adults Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

SCI ↓Mortality Long-term issues remain § Disruption in growth and development § Altered family dynamics § Economic loss 90% non-institutionalized Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Etiology Causes § 42% motor vehicle collisions § 27% falls § 15% violence § 7% sports injuries § 8% other miscellaneous cases Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Comstock/Thinkstock • J. N. , a 32 -yr-old woman, was brought to the ED after being thrown from her car following a motor vehicle accident. • She was not wearing a seat belt. • She is awake and crying. • She states she cannot move or feel her legs. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Comstock/Thinkstock • J. N. anxiously asks you if she “broke her back” and cut her spinal cord. • She also asks if she will be paralyzed for life or if it can be reversed. • Based on your knowledge of the pathophysiology underlying spinal cord injury, how will you respond to J. N. ? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Etiology and Pathophysiology Initial Injury SCI due to cord compression by § Bone displacement § Interruption of blood supply § Traction from pulling on cord Penetrating trauma → tearing and transection Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Etiology and Pathophysiology Initial Injury Primary injury § Initial mechanical disruption of axons as a result of stretch or laceration Secondary injury § Ongoing, progressive damage that occurs after initial injury Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Etiology and Pathophysiology Initial Injury Several theories on what causes ongoing damage at molecular and cellular levels § Free radical formation § Uncontrolled calcium influx § Ischemia § Lipid peroxidation Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Etiology and Pathophysiology Initial Injury Apoptosis (cell death) for weeks or months after initial injury Complete cord damage related to autodestruction § Hemorrhages appear within 1 hour § Infarction by 4 hours Care management critical to limit permanent loss Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
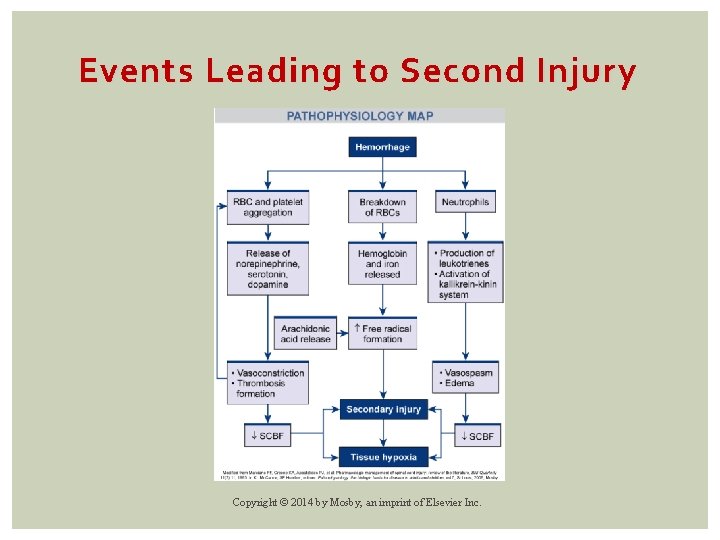
Events Leading to Second Injury Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Etiology and Pathophysiology Initial Injury By ≤ 24 hours, permanent damage may occur because of edema. Extent of damage from both primary injury and secondary injury Prognosis cannot be determined for at least 72 hours. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Comstock/Thinkstock • J. N. ’s cervical spine x-rays and CT reveal fractured C 7 -8 vertebrae. • Physical exam demonstrates total loss of reflexes, sensation, and movement below the level of injury. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Comstock/Thinkstock • You recognize these symptoms as being caused by spinal shock. • What is spinal shock, and how does it differ from neurogenic shock? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Spinal Shock Characterized by § ↓ Reflexes § Loss of sensation § Flaccid paralysis below level of injury Lasts days to months Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Neurogenic Shock Characterized by § Hypotension § Bradycardia Loss of SNS innervation § Peripheral vasodilation § Venous pooling § ↓Cardiac output T 6 or higher injury Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Classification of SCI Major mechanisms of injury are § Flexion § Hyperextension § Flexion-rotation § Extension-rotation § Compression Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Level of Injury Skeletal vs. neurologic level Level of injury may be § Cervical § Thoracic § Lumbar Tetraplegia (quadraplegia) Paraplegia Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
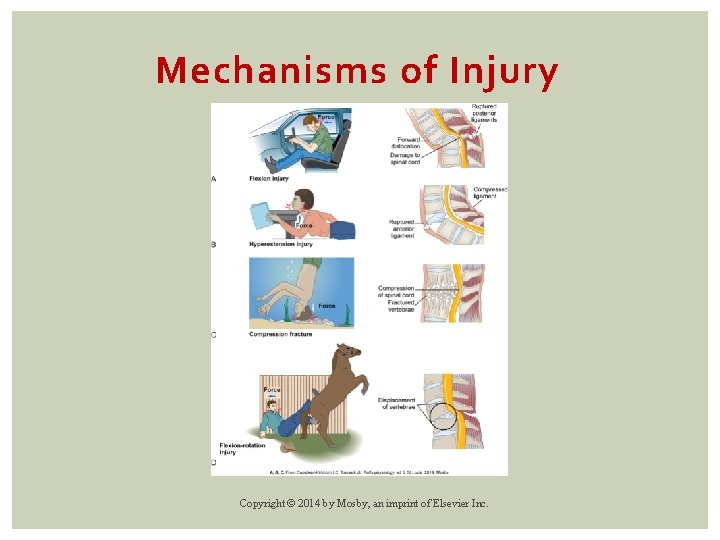
Mechanisms of Injury Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Degree of Injury Complete § Total loss of sensory and motor function below level of injury Incomplete (partial) § Mixed loss of voluntary motor activity and sensation § Some tracts intact Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
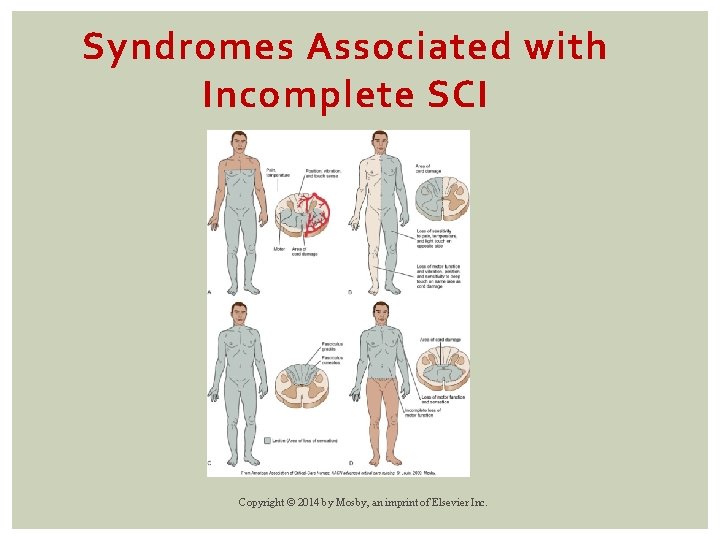
Syndromes Associated with Incomplete SCI Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Incomplete SCI Central Cord Syndrome Damage to central spinal cord Most commonly cervical region More common in older adults Motor weakness and sensory loss Upper extremities affected more than lower Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
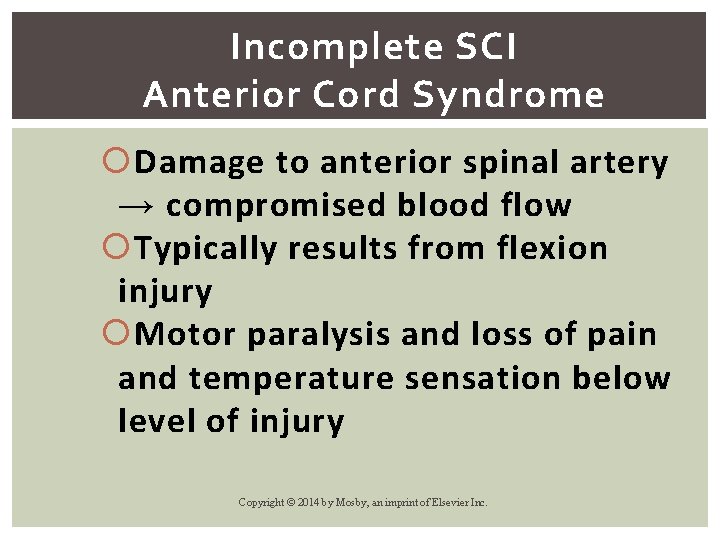
Incomplete SCI Anterior Cord Syndrome Damage to anterior spinal artery → compromised blood flow Typically results from flexion injury Motor paralysis and loss of pain and temperature sensation below level of injury Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Incomplete SCI Brown-Séquard Syndrome Damage to one-half of cord Ipsilateral loss of motor function and position and vibration sense Contralateral loss of pain and temperature sensation Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Incomplete SCI Posterior Cord Syndrome Compression or damage to posterior spinal artery Loss of proprioception Pain, temperature sensation, and motor function below level of lesion remain intact. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Degree of Injury Conus Medullaris Syndrome/ Cauda Equina Syndrome Result from damage to very lowest portion of spinal cord (conus) and lumbar and sacral nerve roots (cauda equina) Injury to these areas produces flaccid paralysis of lower limbs and areflexic (flaccid) bladder and bowel. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Conus Medullaris Syndrome and Cauda Equina Syndrome Conus – lowest portion of cord Cauda equina – lumbar and sacral nerve roots Flaccid paralysis of lower limbs Areflexic (flaccid) bladder and bowel Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

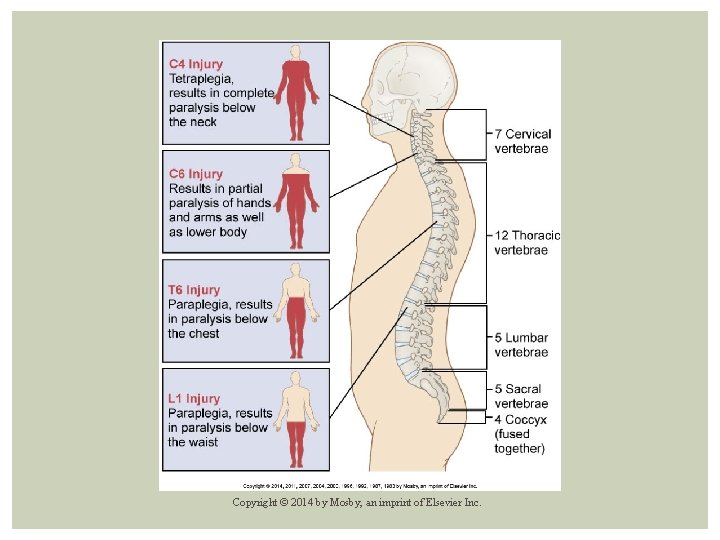
Clinical Manifestations Related to level and degree of injury Incomplete → variable Sequelae more serious with higher injury Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
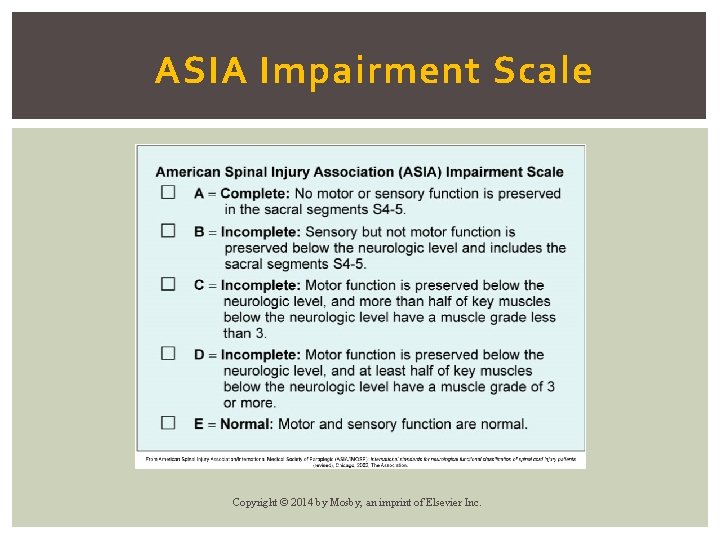
ASIA Impairment Scale Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Clinical Manifestations Respiratory System Closely correspond to level of injury Above level of C 4 § Total loss of respiratory muscle function → mechanical ventilation Below level of C 4 § Diaphragmatic breathing → respiratory insufficiency Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Clinical Manifestations Respiratory System Cervical and thoracic injuries § Paralysis of abdominal and intercostal muscles → ineffective cough → atelectasis or pneumonia ↑Risk for infection Risk for neurogenic pulmonary edema Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Clinical Manifestations Cardiovascular System Injury above level T 6 ↓influence of sympathetic nervous system Bradycardia Peripheral vasodilation → hypotension Relative hypovolemia because of ↑ in venous capacitance Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Clinical Manifestations Cardiovascular System Cardiac monitoring necessary Atropine to ↑ heart rate Peripheral vasodilation § ↓ Venous return of blood to heart § ↓ Cardiac output IV fluids or vasopressor drugs to ↑ BP Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Clinical Manifestations Urinary System Acute phase § Urinary retention § Bladder atonic and overdistended § Indwelling catheter Postacute phase § Bladder may become hyperirritable. § Loss of inhibition from brain § Reflex emptying Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Clinical Manifestations Gastrointestinal System Above T 5→ hypomotility § Paralytic ileus § Gastric distention § Nasogastric tube § Metoclopramide (Reglan) Stress ulcers Intra-abdominal bleeding Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Clinical Manifestations Gastrointestinal System Neurogenic bowel § Injury level of T 12 or below § Bowel initially areflexic with ↓ sphincter tone § When reflexes return § Sphincter tone is enhanced. § Reflex emptying occurs. § Regular bowel program § Coordinate with gastrocolic reflex Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Clinical Manifestations Integumentary System Potential for skin breakdown Poikilothermism § Interruption of SNS § ↓Ability to sweat or shiver § More common with high cervical injury Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Clinical Manifestations Metabolic Needs NG suctioning → metabolic alkalosis ↓Tissue perfusion → acidosis Electrolyte imbalances ↑Nutritional needs § High protein diet Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Clinical Manifestations Peripheral Vascular Problems Deep vein thrombosis (DVT) § Difficult to detect Pulmonary embolism § Leading cause of death Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Diagnostic Studies CT scan Cervical x-rays MRI Comprehensive neurologic examination CT angiogram Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care Immediate goals § Patent airway § Adequate ventilation § Adequate circulating blood volume § Prevent extension of cord damage Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care Emergency Management Initial care § Ensure patent airway. § Stabilize cervical spine. § Administer oxygen. § Establish IV access. § Assess for other injuries. § Control external bleeding. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care Emergency Management Initial care § Obtain imaging. § Prepare for stabilization with tongs and traction. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care Emergency Management Ongoing monitoring § VS, LOC, O 2 sat, cardiac rhythm, urine output § Keep warm. § Monitor for urinary retention, hypertension. § Anticipate need for intubation if no gag reflex. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care Emergency Management Thoracic and lumbar vertebrae injuries § Systemic support less intense § Less respiratory compromise § No bradycardia § Treat symptomatically Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care Acute Care Once stabilized § Obtain history of incident. § Thorough assessment § Muscle groups § Sensory exam § Associated brain injury § Other injuries § Logroll § Continuous monitoring Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care Nonoperative Stabilization To stabilize and decompress injured spinal segment Traction or realignment Eliminate damaging motion. Prevent secondary damage. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care Surgical Therapy Early surgery indicated if § Evidence of cord compression § Progressive neurologic deficit § Compound fracture § Bony fragments § Penetrating wounds Laminectomy Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Comstock/Thinkstock • J. N. ’s cervical spine is immobilized. • A neurosurgeon is consulted. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care Drug Therapy Vasopressor agents § Maintain mean arterial pressure > 90 mm Hg Altered drug metabolism → ↑ risk for interactions Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment Subjective Data § Health history § Functional health patterns § Health perception–health management § Activity-exercise § Cognitive-perceptual § Coping–stress tolerance Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment Objective Data § Poikilothermism § Warm, dry skin (neurogenic shock) § Respiratory difficulties § Bradycardia, hypotension § Decreased or absent bowel sounds § Addominal distention § Constipation, incontinence, impaction Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment Objective Data § Urinary retention § Flaccid or spastic bladder § Priapism § Loss of sexual function § Paralysis § Hyperactive deep tendon reflexes § Muscle atony, contractures Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Diagnoses Ineffective breathing pattern Impaired skin integrity Impaired urinary elimination Constipation Risk for autonomic dysreflexia Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Planning Overall Goals § Optimal level of neurologic functioning § Minimal to no complications of immobility § Learn skills, gain knowledge, and acquire behaviors to care for self. § Return to home and community. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Implementation Health Promotion § Identify § High-risk populations § Counseling § Education § Support legislation on seat belt use, helmets for motorcyclists/bicyclists, and child safety seats. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Implementation Health Promotion § Education § Counseling § Referral to programs § Facilitate wheelchair-accessible health care screening, exam rooms, etc. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Immobilization Maintain neutral position. Stabilize to prevent lateral rotation. § Blanket or towel § Hard cervical collar § Backboard Keep body correctly aligned. Log roll Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Comstock/Thinkstock • J. N. is sent to the OR for surgical stabilization of her spine. • Her family tells you they had a friend with a cervical fracture who was treated with traction. • They ask you to explain the difference in treatment. • What is cervical traction? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Immobilization Skeletal traction § Realignment or reduction of injury § Rope, pulley, and weights § Traction maintained at all times. § Stabilize head in neutral position if dislodged and then summon help. § Pin site care Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
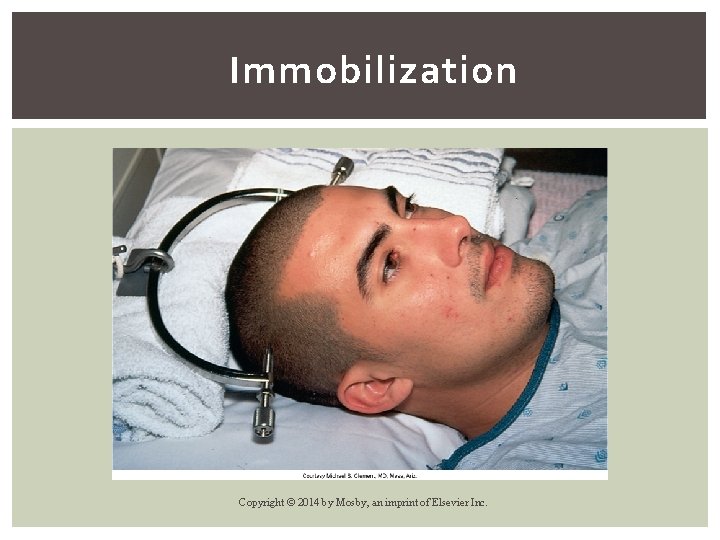
Immobilization Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Immobilization Kinetic therapy § Continual side-to-side slow rotation § >200 turns/day § Manual or automatic § Decreases pressure sores and cardiopulmonary complications § Risk for motion sickness Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Roto. Rest Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
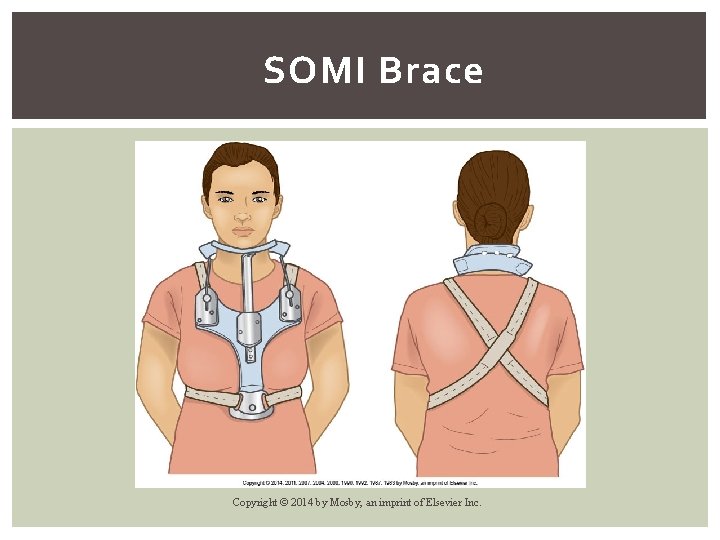
SOMI Brace Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
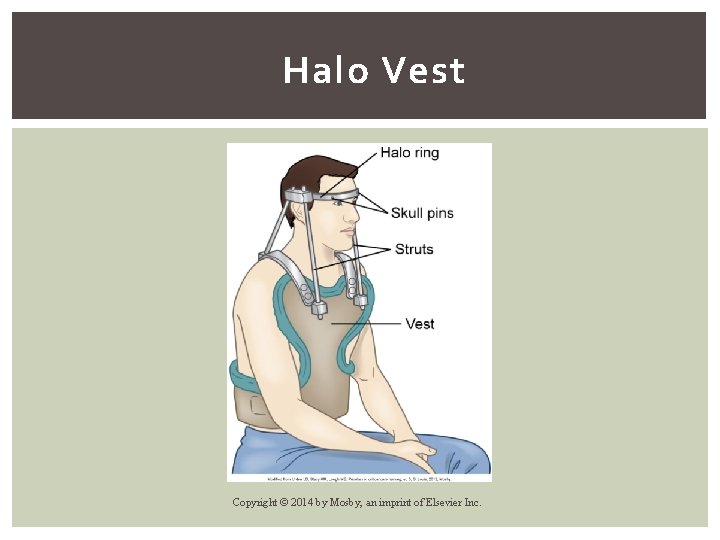
Halo Vest Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Immobilization Thoracic or lumbar spine injuries § Custom thoracolumbar orthosis (“body jacket”) Meticulous skin care critical with all types of immobilization Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Comstock/Thinkstock • What would be your priority assessment of J. N. ’s condition upon her return from surgery? • Explain your answer. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Respiratory Dysfunction May increased during first 48 hours May need intubation and mechanical ventilation ↑ Risk for pneumonia and atelectasis Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Respiratory Dysfunction Regular assessment Aggressive chest physiotherapy Adequate oxygenation Proper pain management Assisted coughing Tracheal suctioning Incentive spirometry Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Cardiovascular Instability Risk for bradycardia and cardiac arrest Chronic low blood pressure with postural hypotension ↑ Risk for DVT Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Cardiovascular Instability Frequent assessment Anticholinergic drug/pacemaker Vasopressor agent Sequential compression devices and/or gradient stockings Range-of-motion exercises Prophylactic heparin Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Fluid and Nutritional Maintenance Initial paralytic ileus and nasogastric tube Monitor fluid and electrolytes. Gradually introduce oral food and fluids. § High-protein, high-calorie diet Copyright © 2014 by Mosby, an imprint of Elsevier Inc. 74

Fluid and Nutritional Maintenance Inadequate nutritional intake § Assess for cause § Contract with patient § Pleasant eating environment § Calorie count § Dietary supplements § Dietary fiber Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Comstock/Thinkstock • J. N. is concerned about how she will be able to control her bladder and bowel with her current status. • How will you respond to J. N. ? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Bladder Management Indwelling urinary catheter initially § Strict aseptic technique § ↑Fluid intake Intermittent catheterization program § Every 3 -4 hours § Monitor for s/s of urinary tract infections Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Bowel Management Bowel program started during acute care § Daily rectal stimulant § Digital stimulation or manual evacuation § Upright position when able Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Temperature Control No vasoconstriction, piloerection, or heat loss through perspiration below level of injury Temperature control external Monitor environment and body temperature. Do not overload or unduly expose patient. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Stress Ulcers ↑Risk secondary to severe trauma and physiologic stress Monitor stool, gastric contents, and hematocrit. Prophylactic medications Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Sensory Deprivation Secondary to absent sensations § Stimulate patient above level of injury. § Conversation, music, strong aromas, and interesting flavors § Prism glasses to read and watch TV § Prevent patient from withdrawing. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Reflexes Return may complicate rehab. § Hyperactive § Exaggerated responses § Penile erections § Spasms Patient teaching Antispasmodic drugs Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Comstock/Thinkstock • Some of J. N. ’s reflexes have returned. • You walk into her room one morning to find her pale and diaphoretic. • She is complaining of a pounding headache. • You assess her vital signs and find her BP is 206/100 and her heart rate is 56 bpm. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Comstock/Thinkstock • What do you suspect is going on with J. N. ? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Autonomic Dysreflexia Massive uncompensated cardiovascular reaction mediated by sympathetic nervous system § SNS responds to stimulation of sensory receptors – parasympathetic nervous system unable to counteract these responses. § Hypertension and bradycardia Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Comstock/Thinkstock • What would be the most likely cause of autonomic dysreflexia in J. N. ? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Autonomic Dysreflexia Most common precipitating factor is distended bladder or rectum. Manifestations § Hypertension § Throbbing headache § Marked diaphoresis above level of injury § Bradycardia Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Comstock/Thinkstock • For what other clinical manifestations of autonomic dysreflexia will you assess J. N. ? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Autonomic Dysreflexia Manifestations § Piloerection § Flushing of skin above level of injury § Blurred vision or spots in visual field § Nasal congestion § Anxiety § Nausea Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Comstock/Thinkstock • What are appropriate nursing interventions for J. N. at this point? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Autonomic Dysreflexia Nursing interventions § Elevate head, notify HCP § Assess for and remove cause § immediate catheterization § remove stool impaction if cause § remove constrictive clothing and tight shoes § Patient and family teaching Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Rehabilitation and Home Care Complex Goal to function at highest level of wellness Retraining focus Interdisciplinary endeavor Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Rehabilitation and Home Care Organized around individual patient’s goals and needs Patient expected § To be involved in therapies § To learn self-care Can be very stressful Frequent encouragement Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Rehabilitation and Home Care Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Respiratory Rehabilitation Phrenic nerve stimulator Diaphragmatic pacemaker Mobile ventilators Patient teaching § Home ventilator care § Assisted coughing § Incentive spirometry § Deep breathing exercises Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Neurogenic Bladder Areflexic (flaccid), hyperreflexic (spastic), or dyssynergia Common problems § Urgency, frequency, incontinence, inability to void, and high bladder pressures resulting in reflux of urine into kidneys Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Neurogenic Bladder Drug therapy § Anticholinergic drugs § α-Adrenergic blockers § Antispasmodic drugs Drainage methods § Bladder reflex training § Indwelling, intermittent, external catheterization § Urinary diversion surgery Patient teaching Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Neurogenic Bowel Voluntary control may be lost. High-fiber diet Adequate fluid intake Suppositories Small-volume enemas Digital stimulation § Mandatory for upper motor neuron injury Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Neurogenic Bowel Stool softener Oral stimulant laxatives Valsalva maneuver with manual stimulation § For lower motor neuron injuries Use of gastrocolic reflex Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Neurogenic Skin Prevention essential Patient teaching Comprehensive daily exam Carefully reposition every 2 hours. Pressure-relieving cushion or mattress Adequate nutrition Avoid thermal injury. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Comstock/Thinkstock • J. N. is worried how this SCI will affect her sexual abilities. • What will you teach her? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Sexuality Important issue regardless of patient’s age or gender Nurse must § Have an awareness and an acceptance of personal sexuality. § Have knowledge of human sexual responses. § Use medical terminology. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Sexuality Injury level and completeness of injury impacts function. Psychogenic versus reflex erection Treatments for erectile dysfunction § Drugs § Vacuum devices § Surgical procedures Fertility issues Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Sexuality Female sexual issues § Lubrication § Orgasm in about 50% of women Fertility not usually affected § Pregnancy complicated § Risk for precipitous delivery Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Sexuality Open discussion Alternative methods Urinary catheterization Planning for bowel evacuation prior Water-soluble lubricant Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Grief and Depression Overwhelming sense of loss Loss of control Adjustment more than acceptance Wide fluctuation in emotions Allow mourning while encouraging hope. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Grief and Depression Caregiver and family counseling Support group Sympathy not helpful Encourage patient participation. Consistency of care Psychiatric consult if needed Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Evaluation Adequate ventilation Intact skin Bowel management Bladder management No autonomic dysreflexia Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Evaluation Establishes a bowel management program based on neurologic function and personal preference. Maintains a bowel movement every other day. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Evaluation Establishes a bladder management program based on neurologic function, caregiver status, and lifestyle choices. Develops no complications of immobility. Experiences no episodes of dysreflexia. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Gerontologic Considerations Increased incidence Increased complications Health promotion and screening Rehabilitation lengthened Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Audience Response Question A patient is just admitted to the hospital following a spinal cord injury at the level of T 4. A priority of nursing care for the patient is monitoring for a. b. c. d. return of reflexes. bradycardia with hypoxemia. effects of sensory deprivation. fluctuations in body temperature. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Audience Response Question A young adult is hospitalized after an accident that resulted in a complete transection of the spinal cord at the level of C 7. The nurse informs the patient that after rehabilitation, the level of function that is most likely to occur is the ability to a. b. c. d. breathe with respiratory support. drive a vehicle with hand controls. ambulate with long-leg braces and crutches. use a powered device to handle eating utensils. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Audience Response Question During assessment of a patient with a spinal cord injury at the level of T 2 at the rehabilitation center, which finding would concern the nurse the most? a. A heart rate of 92 b. A reddened area over the patient’s coccyx c. Marked perspiration on the patient’s face and arms d. A light inspiratory wheeze on auscultation of the lungs Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
- Slides: 114