Spinal Cord Injury and Bowel Dysfunction Presented by

Spinal Cord Injury and Bowel Dysfunction Presented by Angela Stancil January 10 , 2014
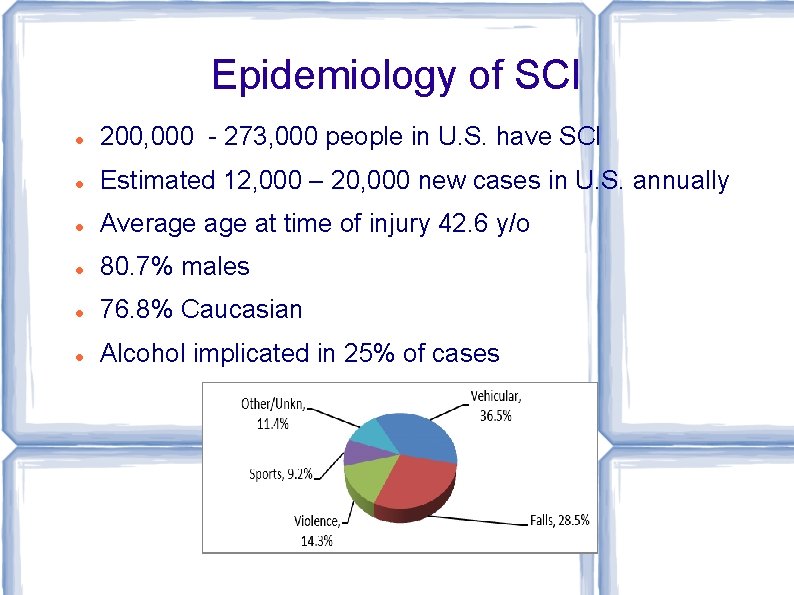
Epidemiology of SCI 200, 000 - 273, 000 people in U. S. have SCI Estimated 12, 000 – 20, 000 new cases in U. S. annually Average at time of injury 42. 6 y/o 80. 7% males 76. 8% Caucasian Alcohol implicated in 25% of cases
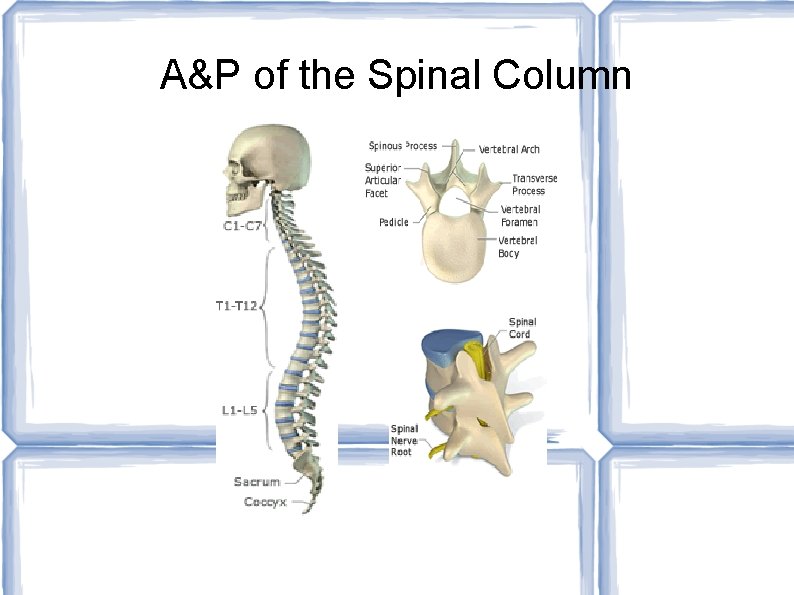
A&P of the Spinal Column
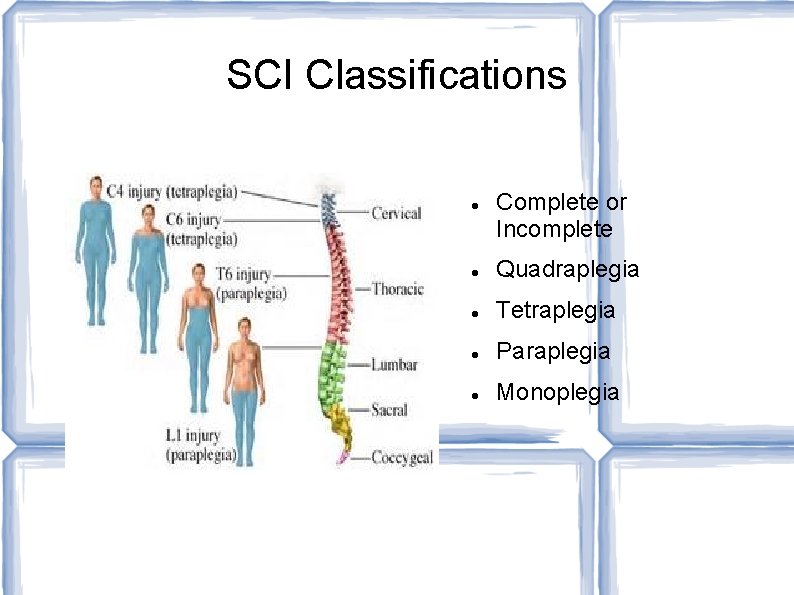
SCI Classifications Complete or Incomplete Quadraplegia Tetraplegia Paraplegia Monoplegia

Complications of SCI Lack of bladder control Bowel Dysfunction Spacisity Altered or missing skin sensation Flaccidity Muscle atrophy Problems with circulatory control Altered muscle tone Weight loss (new injury) Orthostatic hypotension Loss of Mobility Autonomic Hyperreflexia Sexual Dysfunction Edema Depression Pain Respiratory problems
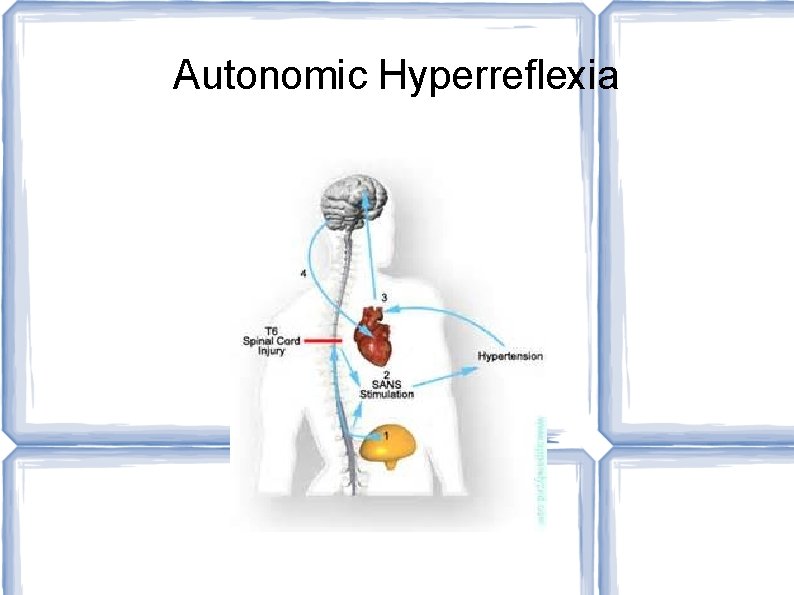
Autonomic Hyperreflexia
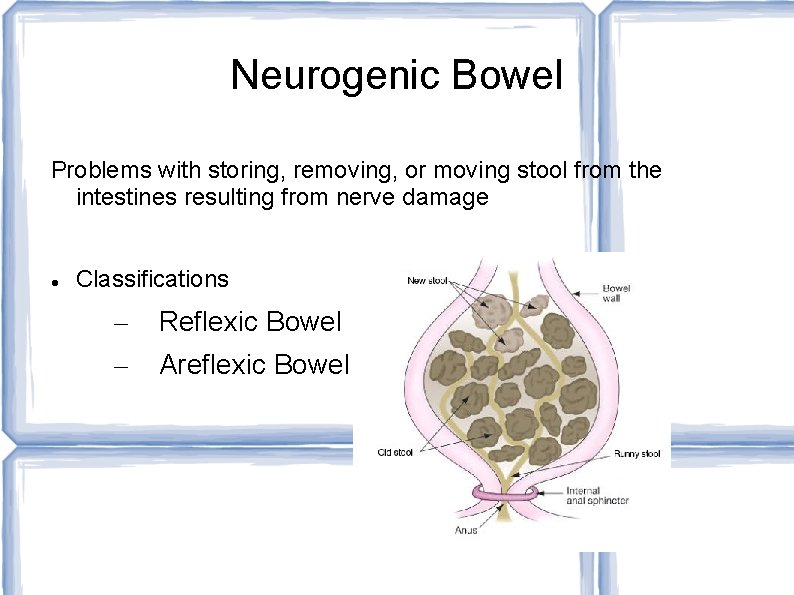
Neurogenic Bowel Problems with storing, removing, or moving stool from the intestines resulting from nerve damage Classifications – – Reflexic Bowel Areflexic Bowel
Symptoms of Neurogenic Bowel Trouble having a bowel movement Repeated bowel accidents Swollen abdomen Feeling full (not hungry) quickly Loose stools or very hard stools Bleeding from the rectum Abdominal pain

Treatment/Bowel Training Dietary changes Exercise/PA program Specific times, assistance, and positions for BMs Medications (stool softeners, laxatives, colonic stimulants, bulking agents) Digital Stimulation (mechanical, enemas, suppositories) Surgery (Colostomy or Ileostomy)


Rationale and Study Objectives Moisture content of stool remains 70 -75% Low fiber intake does not = constipation Symptoms may increase with increased fiber intake Other treatments (i. e. lactulose) may be more beneficial than fiber Patients with constipation already have high fiber intake Objective: to study the effect of decreasing fiber in patients with constipation Hypothesis: Reducing dietary fiber reduces fecal bulk making defecation easier

Study Design Prospective longitudinal case study Inclusion criteria: Straining to expel bulky stools Bowel frequency <1 per 3 days over 3 months Exclusion criteria: Colorectal cancer, previous colonic surgery, melanosis coli, thyroid disorders, anal problems 63 subjects enrolled in the study

Methods Each patient acted as their own control No dietary intake of fiber for 2 weeks Normal CHOs and protein No laxatives Sieved juices and clear vegetables soups Low fiber diet F/U at 1 month and 6 months

Methods Data Collection: Age & sex Fiber intake Frequency of BMs Straining difficulty Evacuation difficulty Abdominal pain and bloating Anal Bleeding Statistical analysis Paired t tests using SPSS software

Results 16 males, 47 females Median age 47 years High fiber diet + fiber supplement At 6 months: 41 no fiber, 16 reduced fiber, 6 high fiber
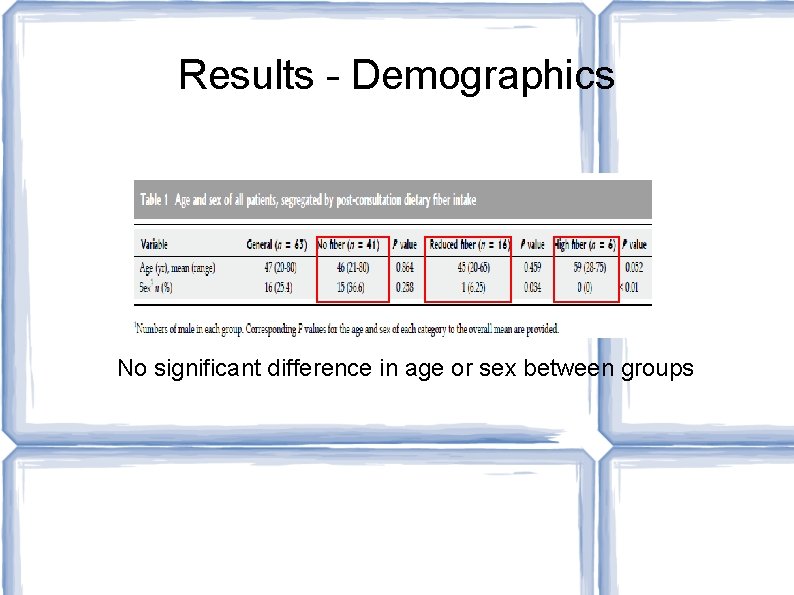
Results - Demographics No significant difference in age or sex between groups
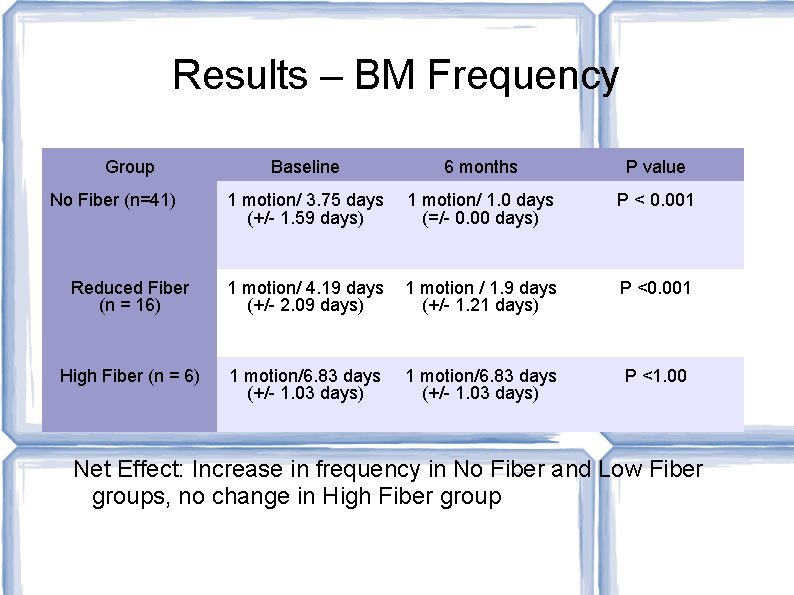
Results – BM Frequency Group Baseline 6 months P value 1 motion/ 3. 75 days (+/- 1. 59 days) 1 motion/ 1. 0 days (=/- 0. 00 days) P < 0. 001 Reduced Fiber (n = 16) 1 motion/ 4. 19 days (+/- 2. 09 days) 1 motion / 1. 9 days (+/- 1. 21 days) P <0. 001 High Fiber (n = 6) 1 motion/6. 83 days (+/- 1. 03 days) P <1. 00 No Fiber (n=41) Net Effect: Increase in frequency in No Fiber and Low Fiber groups, no change in High Fiber group
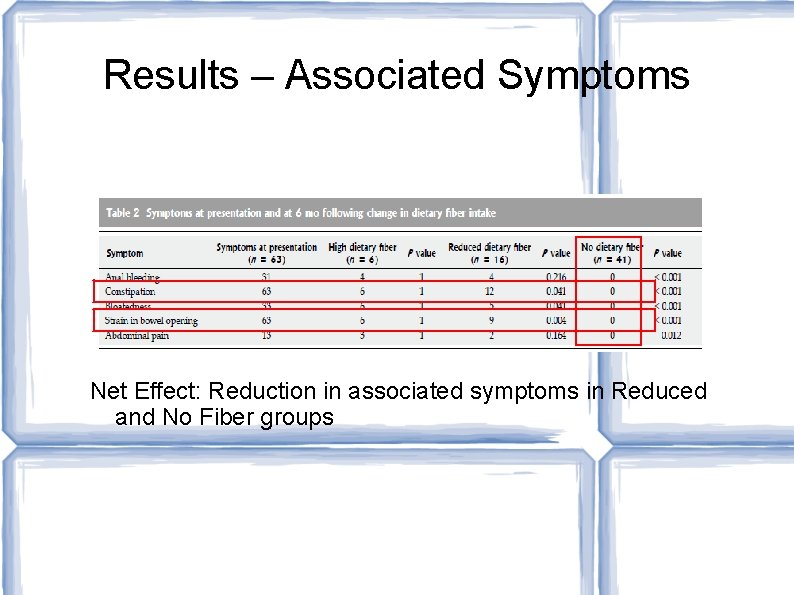

Results – Associated Symptoms Net Effect: Reduction in associated symptoms in Reduced and No Fiber groups

Conclusions Authors' Conclusions: Removing dietary fiber improves constipation and associated symptoms Study Limitations Small sample size No baseline symptoms by group P values Results not generalizable


Rationale IBS is a functional bowel disorder characterized by abdominal pain and discomfort related to bowel disturbances Probiotics are a safe candidate for controlling IBS symptoms Dietary fiber is commonly used in the treatment of IBS Objective: Evaluate the effect of probiotics on patients with IBS and determine if dietary fiber has an additive effect

Study Design Single center, randomized, control trial Recruited volunteers ages 18 – 70 y/o Exclusion criteria: Severe liver, lung, renal, hematological, or major psychiatric disorder Adults > 50 y/o who had not had colonoscopy or sigmoidoscopy in past 5 years Abnormal thyroid function, blood counts, serum chemistry Antipsychotics or anticholergenics in past month Pregnant or lactating Receiving medications for IBS

Methods 142 participants Each participant received a fermented milk product taken 2 x/day for 4 weeks Control group: 150 ml milk + Probiotics Test group: same + 3. 15 g dietary fiber Questionnaire Primary endpoint: difference in defecation frequency, duration, and VAS score

Statistical Analysis Shapiro-Wilk test Student t tests Paired t tests P < 0. 05
Results
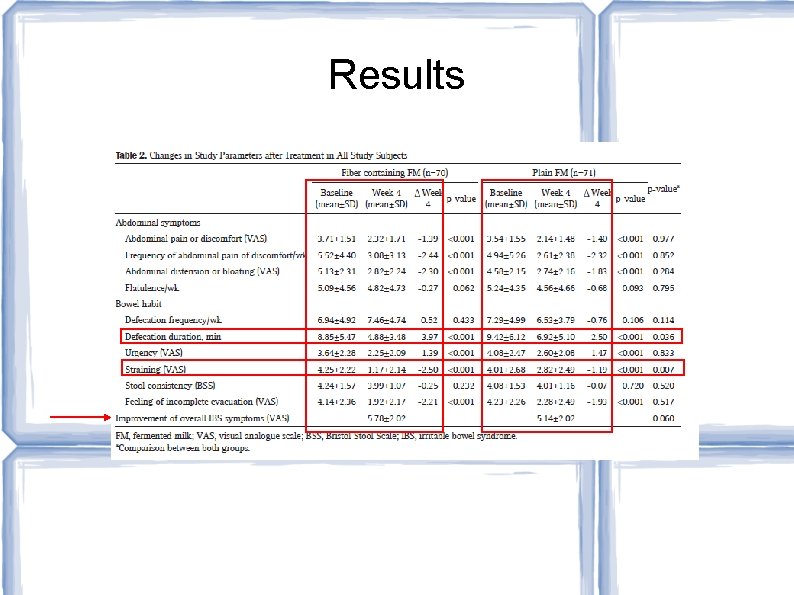
Results
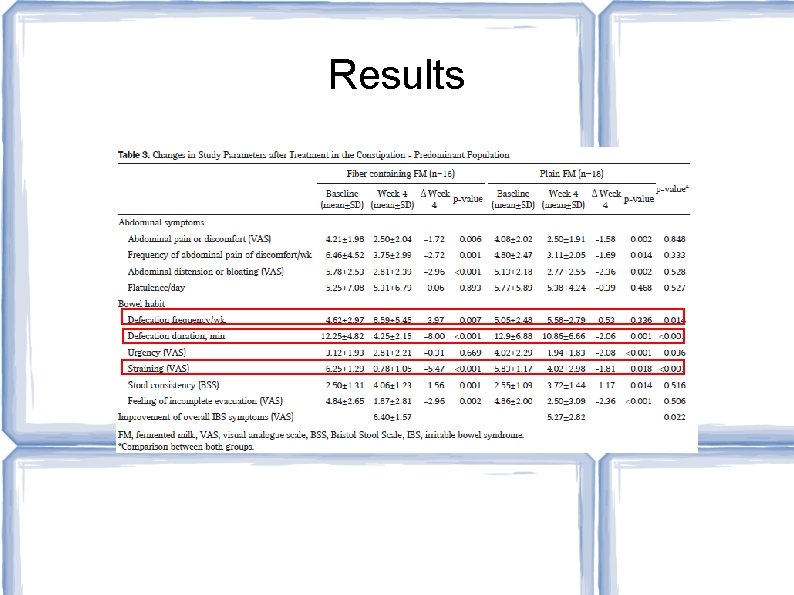
Results
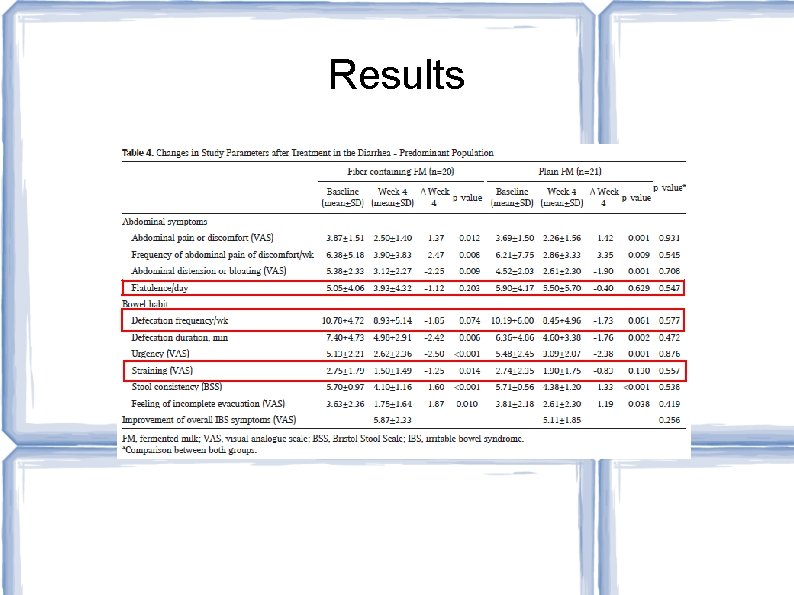
Results

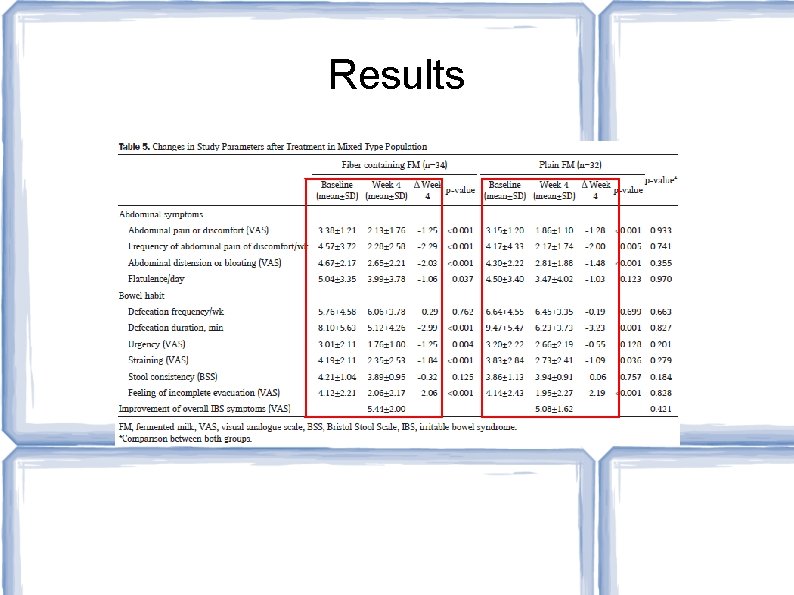
Authors' Conclusions: Plain probiotic milk and probiotic milk containing fiber are safe and effective. Probiotic milk containing fiber was more effective for the constipation dominant subtype of IBS Study Limitations: No placebo group
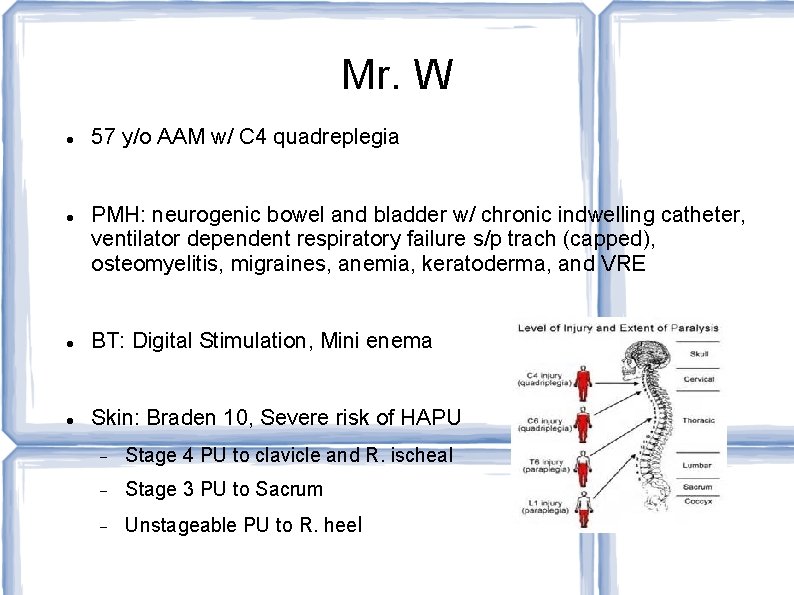
Mr. W 57 y/o AAM w/ C 4 quadreplegia PMH: neurogenic bowel and bladder w/ chronic indwelling catheter, ventilator dependent respiratory failure s/p trach (capped), osteomyelitis, migraines, anemia, keratoderma, and VRE BT: Digital Stimulation, Mini enema Skin: Braden 10, Severe risk of HAPU Stage 4 PU to clavicle and R. ischeal Stage 3 PU to Sacrum Unstageable PU to R. heel

Mr. W Laboratory Data: No new lab data Previously, low pre – albumin (17. 39) Anthropometrics HT: 74 in. WT: 130. 1 lbs (12/8/13) 130. 2 lbs (11/21/13) 126 lbs. (11/15/13) DBW: 162 – 171 lbs. (adjusted 5 -10% for tetraplegia) %DBW: 80% Pertinent Medications: Omeprazole, Acidophilus, Docusate, Tizanidine, Baclofen

Nutrition Assessment Estimated Nutrition Needs Calories: 1776 – 2072 kcals/day (30 -35 kcals/kg) Protein: 74 – 89 g (1. 25 – 1. 5 g/kg) Fluid: 1 ml/kcal + 500 ml or per PCP Diet Hx: PO: Liberal diet EN: Two. Cal @ 60 ml/hr x 12 hrs Free water @ 250 ml/hr q 4 h Prostat supplement 10 am: orange/mango applesauce (meds only) 8 pm snack: PB &J, 1 choc milk, 1 cookie

Nutrition Assessment Appetite: “so so” No V/C/D Tolerating TF w/o problems Physical Assessment Moderate deficits in temples and OFP 24 hour calorie count: 381 kcals, 16. 1 g protein Nitrogen Balance: + 2. 57 (PO + EN+ Prostat)

Mr. W Nutrition Dx: Increased protein/energy needs related to malnutrition and wound healing as evidenced by presence of multiple PUs and Braden of 9. Inadequate oral intake related to poor appetite as evidenced by ongoing need for nutrition support and results of 24 hour calorie count. Nutrition Prescription: Increase intake by 10% by next visit utilizing supplements, snacks, and select menus thereby decreasing dependence on EN

Mr. W Nutrition Interventions Continue Liberal diet Continue Prostat and evening snack Continue EN : Two. Cal @ 60 ml/hr from 7 p - 7 a Nutrition Monitors Wound healing Tolerating TF Prevent Unintentional Weight loss Lab values WNL Consume >80% nutrition needs

Mr. W Nutrition Evaluation Patient's PO intake remains suboptimal. With EN, patient's nitrogen balance is positive. Recommend continuing Liberal diet and EN. Encourage PO intake to decrease dependence on nutrition support. Will continue to follow while admitted. Prognosis: ? ?

References The University of Alabama at Birmingham NSCISC National Spinal Cord Injury Statistical Center. Spinal Cord Injuries Facts and Figures at a Glance. Updated February 2013. Accessed January 5, 2014. Available at https: //www. nscisc. uab. edu/. The Centers for Disease Control and Prevention. Spinal Cord Injury (SCI): Fact Sheet. CDC's Injury Center webpage. Updated November 4, 2010. Accessed January 5, 2014. Available at http: //www. cdc. gov/traumaticbraininjury/scifacts. html. The Mayo Clinic. Spinal Cord Injury. Diseases and conditions webpage. Updated Oct. 22, 2011. Accessed January 5, 2014. Available athttp: //www. mayoclinic. org/diseases-conditions/spinal-cordinjury/basics/definition/con-20023837. National Institutes of Health Clinical Center. Managing Bowel Dysfunction patient education handout. Accessed January 5, 2014. Available at http: //www. cc. nih. gov/ccc/patient_education/pepubs/bowel. pdf. NYU Langone Medical Center. Neurogenic Bowel. Diseases and conditions webpage. Updated March 2013. Accessed January 5, 2014. Available at http: //medicine. med. nyu. edu/conditions-wetreat/conditions/neurogenic-bowel. http: //medicine. med. nyu. edu/conditions-we-treat/conditions/neurogenicbowel. Ho, K, Tan, CY, Daud MA, Seow-Choen, F. Stopping or reducing dietary fiber intake reduces constipation and its associated symptoms. World J Gastroenterology. 2012; 18(33): 4593 -4596. Choi, SC, Kim BJ, Rhee P, et al. Probiotic fermented milk containing dietary fiber has additive effects in IBS with constipation compared to plain probiotic fermented milk. Gut and Liver; 2011. (5): 22 – 28.
- Slides: 37