Specialized Recovery Services Program Ohios 1915i program Front














- Slides: 16

Specialized Recovery Services Program: Ohio’s 1915(i) program Front Door Policy Section Bureau of Long-Term Services and Supports

Agenda Program Overview Eligibility Criteria Referral and Assessment Process Recovery Management Entities SRS and Pre-Termination Reviews Q&A 2

Program Overview 3

SRS Program Overview The Specialized Recovery Services Program (SRSP) is a 1915(i) program that provides continued Medicaid coverage for individuals who were on ABD Spenddown before 8/1/2016 • Income between 75% - 225% FPL who are diagnosed with a serious and persistent mental illness (SPMI) or a diagnosed chronic condition (DCC) • Receive the following additional services: » Recovery Management* » Individualized Placement and Support-Supported Employment » Peer Support Implemented for the SPMI population in August, 2016 and now includes the DCC population as of July, 2017. *Individuals with a diagnosed chronic condition will only receive Recovery Management. 4

OAC Rules • Medicaid eligibility rule: – 5160: 1 -5 -07 Medicaid: specialized recovery services (SRS) program. • Providers and services rules: – 5160 -43 -01 to 5160 -43 -09 http: //codes. ohio. gov/oac/5160 -43 -01 5

SRSP: Pre-Termination Review Process ODM is taking a two-pronged approach to ensure individuals who may be eligible for the SRS Program and spent-down between August 2015 – July 2016 do not experience gaps in coverage due to the redetermination process. Protection • ODM has established a policy that will protect SRS eligible beneficiaries from losing Medicaid coverage if they have been referred and are in the assessment process , even if that process extends beyond their redetermination date. • ODM has established a process to alert the CDFJS and protect these individuals from losing coverage while they are being assessed. Prioritization • SPMI referrals have been prioritized by redetermination date as much as possible to ensure that individuals with redetermination dates in the first half of 2017 are assessed accordingly. • Redetermination dates for DCC individuals pre-identified by ODM have been deferred until 2018 to allow time for the SRS assessments to take place. 6

SRSP Referrals 7

SRSP Referrals • 4 Points of Entry: 1) Medical provider via referral template 2) CDJFS – must ask for SRSP 3) OBLTSS agency – must ask for SRSP 4) Self referral • BHCP@medicaid. ohio. gov • Every individual will receive a NOA notifying them of the eligibility decision. • The time it takes for an eligibility determination can vary significantly from person to person due to a variety of factors. 8

Eligibility Criteria 9

SRSP: Eligibility Criteria To be eligible for enrollment an individual must: • Be at least 21 years of age • Be determined financially eligible for Medicaid • Receive Social Security Disability Benefits* • Reside in a Home and Community-Based Services (HCBS) setting • Demonstrate a need for SRS, and not otherwise receive those services • Have needs that can be safely met in an HCBS setting • Participate in the development of a person-centered care plan *Currently revising policy regarding receipt of SSD benefits 10

SRSP: Eligibility Criteria To be eligible for enrollment an individual must: • Be diagnosed with an SPMI, be active on the solid organ or soft tissue waiting list, or have a DCC per the attachment to OAC rule 5160 -43 -02 • Adult Needs and Strengths Assessment (ANSA) - demonstrate needs related to the management of the behavioral health or Score at least a 2 in one of the items in the “mental health needs” or “risk behaviors” section or score a 3 on at least one of the items in “life domains section” • Demonstrate needs related to the management of the behavioral health or diagnosed chronic condition 11

SRSP: Eligibility Criteria To be eligible for enrollment an individual must also have at least one of the following risk factors prior to enrollment: • One or more psychiatric inpatient admissions at an inpatient psychiatric hospital; or • A discharge from a correctional facility with a history of inpatient or outpatient behavioral health treatment while residing in that facility; or • Two or more emergency department visits with a psychiatric diagnosis; or • A history of treatment in an intensive outpatient rehab program for greater than ninety days; or • One or more hospital admissions due to a diagnosed chronic condition 12

SRSP: Eligibility Criteria To be eligible for enrollment an individual must meet at least one of the following: • Have a need for a SRS to maintain stability, improve functioning, prevent relapse, be maintained in the community and if not for the provision of the SRS the individual would decline to a prior level of need; or • Previously have met the eligibility criteria and but for the provision of the SRS, would decline to a prior level of need 13

Recovery Management Entities 14

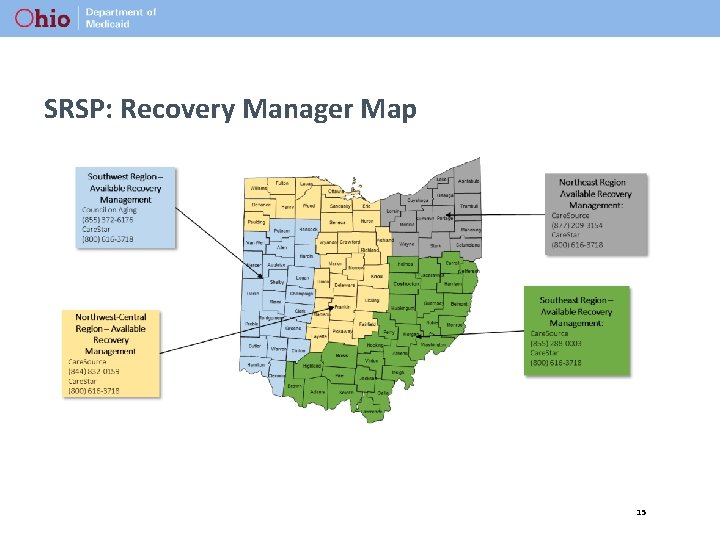
SRSP: Recovery Manager Map 15

Questions? ODM Point of Contact: Alicia Hullinger alicia. hullinger@medicaid. ohio. gov 3