South Gloucestershire Positive Behaviour Support Team PBS Network

South Gloucestershire Positive Behaviour Support Team PBS Network Meeting 18/03/16 Nicholas Wood – Lead Nurse Emily Greentree – Behaviour Nurse

What is Positive Behavioural Support? Positive Behavioural Support (PBS) is about values and rights for people with disabilities. It looks at why people behave the way they do. It aims to improve quality of life for individuals and the people who live and work with them. (based on Horner, 1999)

Positive Behaviour Support Team South Glos. CLDT Our Aims are: 1. To ensure people who challenge have a good quality of life and equal opportunities. 2. To support people who challenge to stay within their local community. 3. To use the most up to date, evidence based practice. 4. For people who challenge to have timely, person-centred support from our service.

The Team Our team works to support people with behaviour that challenges. The team come from different backgrounds but all have skills in Positive Behavioural Support: • Behaviour Nursing • Positive Behaviour Support Practitioner • Occupational Therapy, • Speech and Language Therapy • Psychology • Psychiatry

The Past (ICS) • Team primarily focussed on crisis management/reactive strategies • Referrals screened differently • Team held a large caseload – low discharges • Limited preventative work • Dependence by care providers on crisis support from the team

Our PBS Approach • Multi-disciplinary working is core to approach • 2 professionals for every initial assessment • This is not a crisis service • Integrated assessment and intervention • Broader staff involvement - not just home manager / key worker

Our PBS Approach • Strong emphasis on person-centredness / Quality of Life • One assessment that is enduring and reviewed • Flexibility • Carers direct involvement in developing responses / strategies.

What Differences should I be able to see? • • • Clearer process and more standardised practice Written reports detailing: Information gained Formulation of needs Recommendations A Multi-Disciplinary meeting involving the PBS team and yourselves to discuss report and agree action plan

Carers PBS process involves parents and carers as equal partners in the PBS Pathway (where consent is obtained or best interests route has been established) Assessments can be undertaken with parents and carers to identify function of behaviour Invited to formulation meetings and input is encouraged We will signpost parents and carers to other services for further support – such as the Carers’ Centre or support them to receive a Carers’ Assessment Self reflection is an important part of the formulation process for everyone involved

Service Users PBS is heavily focussed on person centeredness We put the service user at the centre of all input and interaction We are currently developing more accessible assessment documents for service users who can contribute to the assessment process We endeavour to include the service user at all stages of the pathway, in whatever way they can participate

Behaviour Assessment • - Toolbox: Functional Analysis Prioritising Behaviours Brief Behaviour Assessment Tool Contextual Assessment Inventory Motivational Assessment Scale PCP: Timeline, Important To/For, Motivators System Analysis (strengths/weaknesses) Direct observation Use notes and ABC charts as evidence

Formulation • Multi-disciplinary team approach – service user, family, support workers, professionals • Person Centered Focus • Predisposing Factors • Presenting Issues • Precipitating Factors • Perpetuating Factors • Protective Factors • Agree Short Term and Long Term Goals
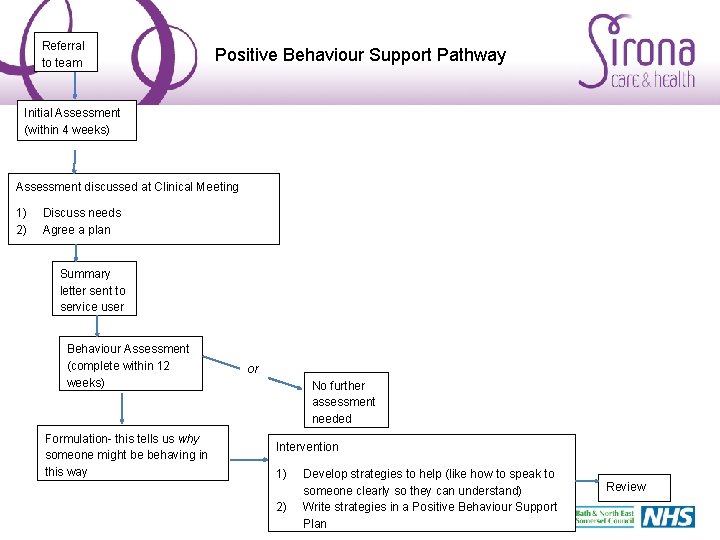
Referral to team Positive Behaviour Support Pathway Initial Assessment (within 4 weeks) Assessment discussed at Clinical Meeting 1) 2) Discuss needs Agree a plan Summary letter sent to service user Behaviour Assessment (complete within 12 weeks) Formulation- this tells us why someone might be behaving in this way or No further assessment needed Intervention 1) 2) Develop strategies to help (like how to speak to someone clearly so they can understand) Write strategies in a Positive Behaviour Support Plan Review

What about crisis management? • If a service user is in crisis then referrals are still accepted. • It is likely a Nurse will visit to complete an initial assessment and identify any immediate support or recommendations we can offer. • Often this is joint with Psychiatry • We will signpost to out of hours crisis services and on-call psychiatry • We may liaise with social services • We differentiate these referrals and post-crises will assess if PBS input is required.

Outcomes • 84 referrals Received • Initial Assessment reports are being produced and sent to Service Users / carers • Formulation meetings with Service Users and carers are happening. • We are producing PBS plans focussing on pro-active strategies • Some services are referring more Service Users to our Service following experience of the process • Initial positive feedback from those who have completed parts of the pathway such as Formulation

Challenges • Many referrals were already in process or some of the MDT work was already on-going • Specialist PBS training is on-going • Not a Crisis Team • Where organisations already have PBS Practitioner/Plans in place • Difficulties in working with some staff teams • Where Service Users do not see a need for intervention • Limited knowledge of PBS approaches within the area • Conflict between families/paid carers • Age of referrals - many referrals of older adults with LD (60+) • Health / behaviour / Dementia / Mental health differential diagnosis • Staffing changes • Changing ways of working

. Challenges PBS approach can help but plan to diagnose needs vital Commitment to referrals and process. PBS process asks for a lot of engagement and creativity from staff. The move away from the Professional as the ‘expert’ and focus on what support staff need to do can be challenging for services.

Future Development of Service • Assessments with service users - accessible information • Assessments that work well for people with mild LD / those with limited support • Outcome measures/feedback • Increased intervention types • Crisis pathway development

Speech & Language Therapy within a PBS framework. Louise Mc. Millan. Speech and Language Therapist (SLT). South Glos CLDT. Louise. mcmillan@sirona-cic. org. uk. Tel no; 01225 831277.

Why is communication important? • It is a significant risk factor contributing to mental health issues and behaviour described as challenging • Up to 90% of people with LD have communication difficulties • Around ½ have significant difficulties with both expressing themselves and understanding what others say (RCSLT Position paper) • 5 -10% of PWLD have literacy skills • Incidence of sensory impairments is much greater than general population. Up to 40% have hearing loss missed or undiagnosed

• People with autism have lifelong communication impairments around social communication, social interaction and social imagination • As communication difficulties increase, behaviours that are considered challenging typically increase in frequency, intensity or duration (Royal college of Psychiatry, 1997)

Risks of having communication difficulties • Individuals are misunderstood, experience failure and exclusion from events, activities and relationships. • Environmental risks – evidence that staff do not generally interact with people they support in a way that enables individuals to achieve greater levels of independence, participation or integration ( Mansell 2007) • Staff need skills to make reasonable adjustments to maximise engagement, involvement and inclusion.

Good communication Without good communication people may be at risk of • lack of choices/ involvement in everyday decisions • Limited relationships • Increased vulnerability • Low mood, anxiety, depression, withdrawal • Increased use of behaviour that challenges, mental health issues, distress or offending • Increased placement breakdowns

Good communication • Reduces these risks • Enables inclusive relationships • Supports individuals to have choice, control, greater independence, improved health outcomes. • Need a whole systems approach to reasonable adjustments, including • Training for staff • Access to resources, skills, and knowledge to support communication • Effective communication strategies, guidelines and standards

Role of the SLT • Assessment of understanding & communication, frequently overestimated by staff (Bradshaw 2011, 2013; Clarke-Kehoe & Harris 1992) • Need to “ enable the person to find more appropriate, that is socially acceptable forms of communication. ” (Stansfield & Cheseldine 1994) • Training for service users and staff (College report 2007; Allen et al 2005)

SLT team approach. • Communication is understood as a partnership (Bartlett & Bunning 1997) • Joint working as essential –” it is necessary that any intervention is multi-element. ” (Baker et al 1997) • Contributing to active support in a timely manner (Mansell 2007) • Communication is impacted by stress (Bradshaw 2002)

RCSLT 5 good communication standards (RCSLT 2013). • ‘Everyone needs to know what good communication support looks like and what reasonable adjustments they can expect. ’

Standard 1. There is a detailed description of how best to communicate with individuals. • Eg communication passport • Passports particularly useful where the individual cannot report information themselves • Communication profiles, dictionaries and guidelines • Whether communication & behaviour is intentional • If very sensory oriented, work through sensory means.

Standard 2. Services demonstrate how they support individuals with communication needs to be involved with decisions about their care and services. . • Service users need information accessible to them. • Service users usually need extra processing time. • If the service user cannot report themselves, they require family members / significant others to be able to contribute to planning. • May use social stories to impart information in a clear repeated way.

Visual schedules. • Visual schedules are created in a very bespoke way made for the individual. • Some people can only cope with a Now and next board containing 2 activities. • Some people need to see a key event coming up to reinforce that it is in 3 days time and not now.

Visual shopping lists. • Preplanning a visual shopping list can assist some who may want to buy additional items in the shop & who have no concept of money.

Standard 3 Staff value and competently use the best approaches to communication with each individual they support. • Staff may need to adapt their communication / language. • An example of this may be signing support for the individual. Staff training may be required around an. individual.

Signing support. • Signalong – a signing support system used as part of total communication. • Sign key words along with adapted simple language. • One sign per concept, using iconic signs taken from BSL. • Finger spelling only for initial letters.

Examples of signs. • Hello • Good or really good • My name is • What’s your name? • Goodbye
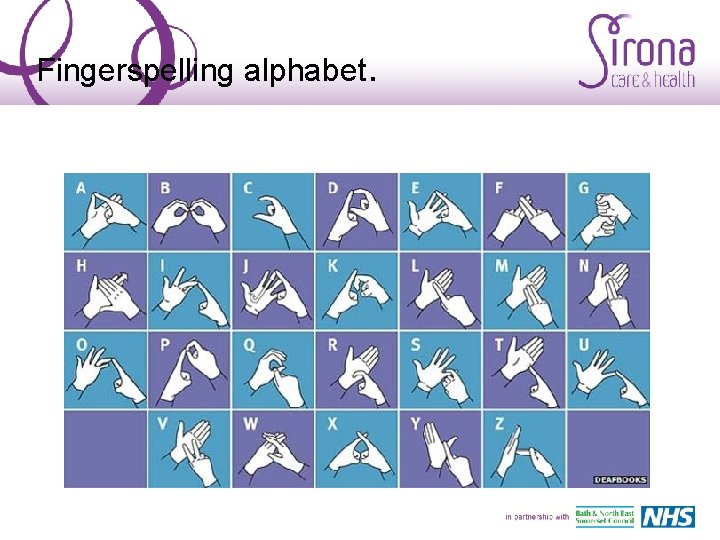
Fingerspelling alphabet.

Standard 4. Services create opportunities, relationships and environments that make individuals want to communicate. • SLT often advising on creating opportunities for choice ( La Vigna 2003). Choices can be made with objects & pictures. • Starting point is the service users motivations. • Looking at physical and social environment.

Communication environments. • Promoting positive communication between staff and service users as a result of looking at environments (Mc. Gill 1993). • Adopting a total communication approach. This involves using any modes that are understood by the individual; objects, pictures, signing, body language, facial expression. • May want to provide more general communication training in core areas. This could be around sensory issues, Intensive Interaction, how to use resources that we have provided or recommended.

Standard 5. Individuals are supported to understand express their needs in relation to their health and wellbeing. • Talking mats. This involves a conversation using pictures to record the service users views. • Used for presenting accessible health information. • We also make use of hospital liaison nurses to inform hospital staff of needs and communication styles.

Conclusions & contacts. • Any questions ? • Telephone number - 01225 831277.

References; • Allen, D. , James, W. , Evans, J. , et al (2005) Positive Behavioural Support: Definition, Current Status and Future Directions. Learning Disability Review, 10, 4 -11. • Baker, P. , La Vigna, G. , & Willis, T. (1997) Understanding & responding to challenging behaviour: a multi-element approach. In Fraser, W. , Sines, D. , & Kerr, M. , HALLAS. Caring for people with learning disabilities. 9 th Ed. Heinemann. Oxford. • Bartlett, C. & Bunning, K. (1997) The Importance of communication partnerships; a study to investigate the communicative exchanges between staff & adults with Learning Disabilities. British Journal of learning Disabilities. 25, 148 -153. • Bradshaw, J. (2002). The management of challenging behaviour within a communicative framework. In Management of Communication Needs of People with Learning Disability. (Eds. Abudarham, S & Hurd, A ). Whurr. London. • Bradshaw, J. (2011) Communication & Challenging behaviour. In Challenging Behaviour & People with Learning Disabilities. (Eds. Hardy, S & Joyce, T. ). Pavilion. Brighton. • Bradshaw, J. (2013) Communication & Challenging behaviour. Information sheet. Challenging Behaviour Foundation. Kent. • Clarke – Kehoe, A. & Harris, P. (1992) It’s the way you say it. Practise; challenging behaviour. July. • La Vigna, G. (2003) Non aversive Behavioural Support & Basic Principles of Positive Programming. Lecture notes in Positive Practise in Behavioural Support.

References; • Mansell, J. (2007) Services for people with Learning Disability & Challenging Behaviour. In Michael, J. (2008) Healthcare for all: A report of the Independent Inquiry into access to health care for people with Learning Disabilities. Dept of Health. London. • Mc. Gill, P. (1993) Challenging Behaviour, challenging environments & challenging needs. Clinical Psychology forum, 56, June, 14 -18. • Positive Behavioural Support awareness raising course. Positive & Safe. (2014) Dept of Health. • Royal College of Psychiatrists, British Psychological Society, & Royal College of Speech & Language Therapists. (2007) Challenging Behaviour: a unified approach. College Report CR 144. Royal College of Psychiatrists. • Royal College of Speech & Language Therapists. (2010). Adults with Learning Disabilities: Position Paper. • Royal College of Speech & Language Therapists. Five good communication standards. London: RCSLT, 2013. • Stansfield, J. & Cheseldine, S. (1994) Challenging to Communicate. Human Communication. June.

Arts Therapies Annie March, Art Therapist

ART- using different art materials like paint, clay, pencils, pens and collage to express thoughts and feelings with the art therapist. MUSIC – use musical instruments, voice, song writing and music that is important to you. Sharing making music with therapist to explore emotional issues. DRAMA – includes story- telling, role play, movement, playing and puppets to connect to feelings, thoughts and make life stories. Arts Therapies

-verbally (without talking) and verbally (talking). The therapist works with their client to build a safe and trusting relationship. The client’s art works, thoughts and feelings are shared in confidence with therapist. The arts therapies are person centred offering flexible and dynamic communication through image making/ creative processes which is especially useful to service users with a learning disability. You do not have to be ‘good’ at art, music or drama to come to art therapy. Arts Therapies

Struggling with change this may be communicated by changes in behaviour Experienced trauma Mental health issues Psychological Therapies and the PBS Arts therapist work alongside other professions in the CLDT to offer an MDT approach to service users. Arts Therapies

Consultation to support clients and staff teams Referrals from PBS to support clients with psychological distress alongside their PBS support plan. Art therapy provides a psychologically safe and contained experience for clients to be able to express themselves non verbally which can be useful to understand service users narrative and needs. The psychological containment that arts therapy can provide is often a help to clients in distress which can support a client alongside a integrated MDT approach. Arts Therapies

Break

Kath Finlay, Assistant Psychologist Mindfulness

The role of Occupational Therapy in Positive Behavioural Support • Eva Nakopoulou

Primary Prevention • Reduction in the possibility of an aggressive incident occurring by assessing and changing aspects of peoples lives i. e. environment, personal, working and recreational conditions, where necessary. • This where the role of OT is significant.

Primary Prevention 1. 2. 3. 4. Is sensory or is it behaviour? Is the environment meeting this person’s needs? Does the behaviour stem from lack of skills? Does the behaviour stem from lack of meaningful occupations?
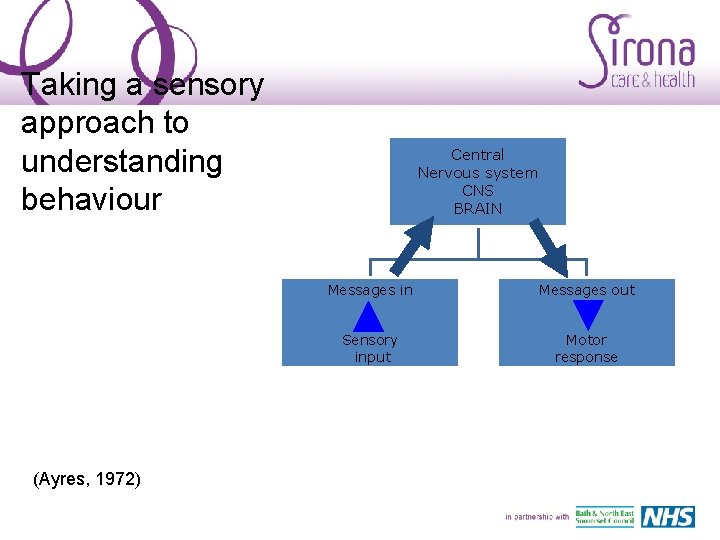
Taking a sensory approach to understanding behaviour (Ayres, 1972) Central Nervous system CNS BRAIN Messages in Messages out Sensory input Motor response

Taking a sensory approach to understanding behaviour

What sense?

What sense?

Aspects of the Environment Social Cultural Environme nt Physical Institution al

vel • Meaningful roles • Motivation • Sense of achievement

vel • Promoting independence • Learning new skills • Learning new ways to do the activity

Occupational Deprivation • A state in which a person is unable to do what is meaningful and necessary in their lives due to external restrictions • This state of deprivation arises not as a result of limitations inherent within the individual but due to forces outside his or her control ‘Occupation is not something nice to do, rather it is hardwired into the human’ (Whiteford, 2000)

Exercise • Think of 3 activities that you regularly do, to which you perceive as essential.

Exercise • Think of 3 activities that are meaningful to you.

Discussion • Emotions? • Behaviours? ------------------- • Meaningful? • Not Meaningful?

Occupation What is meaningful Occupation? What is a meaningful role?

Questions?

References: • Ayres, A. J. , 1972. Sensory integration and learning disorders. Los Angeles: Western Psychological Association. • Creek, J. (2003) Occupational therapy defined as a complex intervention. London: College of Occupational Therapists. • Whiteford, G (2000). Occupational Deprivation: Global Challenge in the New Millennium. British Journal of Occupational Therapy. 65 (5). • Wilcock, A. A. (2006). An Occupational Perspective of Health. 2 nd ed. U. S. A. : Slack Incorporated.

South Gloucestershire Positive Behaviour Support Team Case Study This is a composite case study illustrating the Multidisciplinary nature of our work

MDT Assessments An older gentleman who frequently destroyed property 1 Assessment led to an understanding that the behaviours are related to underlying anxiety and his lack of conscious control of the behaviour. (Psychiatry) 2 Additionally it was identified that although the gentleman communicates verbally he did not express his personal thoughts, feelings and anxieties verbally (SALT) 3 It had been thought there was likely to be a sensory element to the behaviour. This was assessed not to be the case (OT)

MDT Assessments 4 A time line identified all the negative experiences and losses the man had experienced in his life (Nursing) 5 Analysis showed key triggers were ‘disappointment’ and ‘negative social interactions’ (CAI, Nursing) 6 Arts therapy showed the Gentleman’s need for self-control and low self-esteem 7 Staff have difficulty supporting individual with personal care and different strategies are used by different staff 8 The Individual is ageing and is starting to have difficulty walking longer distances 9 behaviours had led to negative attitudes towards him from other service users

Formulation Meeting 1 Carers developed greater understanding of the needs of the Gentleman 2 This process led to reduced ‘blame’ and increased empathy for him 3 Unintentionally the carers felt a reduced responsibility to try and ‘stop’ behaviours and felt less responsible when they occurred

Key Interventions Agreed 1 Increasing independence – going to shops on own 2 Changing responses from trying to stop behaviour to supporting the individual (RAG) 3 Reduced questioning of the individual as to ‘why’ he was doing it 4 Increased focus on household tasks that the individual finds rewarding and receives social praise for 5 Developing structured routines around personal care

Key Interventions Agreed 6 Work with all residents about relationships and how people should treat each other (Psychology) 7 Physiotherapy assessment and work to maintain independence and ability to walk to local shops unaided

Outcomes 1 Increased self-esteem through praise from completing tasks 2 Increased independence through going to shops on own 3 Reduced incidents and severity of incidents over time. Incidents are on-going but people understand this better 4 Improved relationships with other service users – but also other service users getting on better with each other 5 Further referrals to PBS team from the home …. .

If you are concerned regarding someone's behaviour then (after recording): • Support the service user to GP to rule out any physical cause for behaviour such as ear infections, ear, Urinary Tract Infections, Thyroid Function • Consider Opticians and Dentist Appointments • Is pain relief or more regular pain relief needed? • Identify any significant changes or events which have happened recently • Talk to the individual

Contact us South Gloucestershire Learning Disability Service Church House 1 Church Road Soundwell Bristol BS 16 4 RH Tel: 01225 831277 Nick Wood, Lead Nurse Emily Greentree, Behaviour Nurse Eva Nakopoulou Occupational Therapist Louise Mc. Millan, Speech and Language Therapist Annie March, Art Therapist

Further Information about PBS An introduction to Positive Behaviour Support free E-Learning Course is available at: https: //elearning. nsahealth. org. uk Positive Behaviour Support Network Meetings: http: //positivebehaviour. org/
- Slides: 75