Solutions for difficult situations in bariatric surgery What

Solutions for difficult situations in bariatric surgery : What to do ? The real risk patient in Anaesthesia J P Mulier, MD Ph. D B Dillemans, MD CHL 12 06 2009 J P Mulier

High risk in bariatric surgery n Pulmonary diseases n n n Cardiac disease n n n Right ventricular failure Coronary atheromatose Muscle disease n n Asthma COPD Seldom obese patients, however Other rarities n Search active for them / dangerous for every anesthesia CHL 12 06 2009 J P Mulier

Is there a risk ? n According to the media: yes! Bariatric surgery kills 5 percent of patients: Weight loss surgery takes deadly toll Wednesday, March 22, 2006 by: Mike Adams, the Health Ranger, Natural. News Editor n According to the scientific publications: overall 10 year mortality decreased with 24 % SOS study Sjöström 2008 CHL 12 06 2009 J P Mulier

Individual risk pre op? Which patient is at risk ? 1. 2. Very high BMI ? 70 > 60 > 50 CHL 12 06 2009 J P Mulier

The higher the BMI the higher the risk? n Not the BMI itself but n n Central fat intra abdominal: apple > pear No weight reduction is a risk n n Not absolute weight. -30 kg creates space to breath, laparoscopic work space, improved liver function Higher BMI more difficult but not a higher risk? Table positioning n Intubation positioning n Mobilization in bed n n n Aspiration risk at induction Post operative insufficient breathing CHL 12 06 2009 J P Mulier

Individual risk pre op? Which patient is at risk ? 1. 2. High BMI ? Older patient ? 1. Less frequent in bariatrics, but … CHL 12 06 2009 J P Mulier

Individual risk pre op? Which patient is at risk ? 1. 2. 3. High BMI ? Older patient ? Diabetes ? Many co morbidities 2. Frequent glucose follow up lower risks? 1. CHL 12 06 2009 J P Mulier

Individual risk pre op? Which patient is at risk ? 1. 2. 3. 4. High BMI ? Older patient ? Diabetes ? Sleep apnea ? CHL 12 06 2009 J P Mulier

Sleep apnea patient high risk? 1. Is a clinical diagnosis of sleep disturbance, 1. 2. 3. not of post operative hypoxia no study yet confirms risk. No numbers of resp obstruction post op! Use cpap mask post op if used at home Active search pre op ? CHL 12 06 2009 J P Mulier

Individual risk pre op? Which patient is at risk ? 1. 2. 3. 4. High BMI ? Older patient ? Diabetes ? Sleep apnea ? Which patient has complications ? 1. What are the most frequent complications? CHL 12 06 2009 J P Mulier

30 days Complications in 2606 gastric bypass sint Jan Brugge B Dillemans 2009 hemorrhage 89 3, 41% blood transfusion 46 1, 89% re operation 35 1, 47% re admission 34 1, 43% intestinal obstruction 9 0, 38% pneumonia 6 0, 25% CPAP and re intubation 5 0, 21% pulm emboli DVT 5 0, 21% leak 5 0, 17% food stenosis 4 0, 17% death 1 0, 04% perforation 1 0, 04% pancreatic injury 1 0, 04% intra abd abscess CHL 12 06 2009 J P Mulier

Complications and anaesthesia 1. Hemorrhage Surgical problem but we can help to prevent it 2. Post operative re-intubation, ventilation -> pneumonia Anaesthesiological problem: 3. Leakage Surgical problem but we can help to prevent. Transdisciplinary: we as anesthesiologists must think: Ask not what the surgeon can do for you, ask what you can for the surgeon CHL 12 06 2009 J do P Mulier

1. Post operative hemorrhage Ask your anesthesiologist to raise the blood pressure above 140 mm. Hg SAP at end of procedure. n Inspect and stop local bleeding n n Coagulate, n clip, stitch Ask to control intra luminal bleeding by pouch aspiration test before extubation. CHL 12 06 2009 J P Mulier
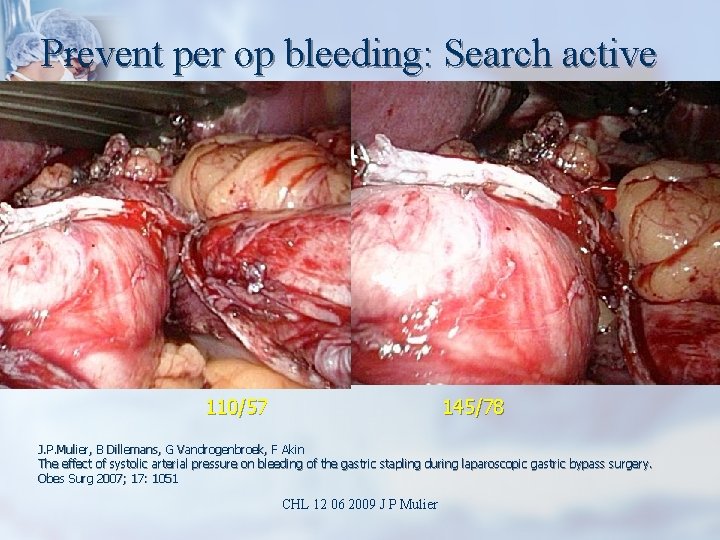
Prevent per op bleeding: Search active 110/57 145/78 J. P. Mulier, B Dillemans, G Vandrogenbroek, F Akin The effect of systolic arterial pressure on bleeding of the gastric stapling during laparoscopic gastric bypass surgery. Obes Surg 2007; 17: 1051 CHL 12 06 2009 J P Mulier
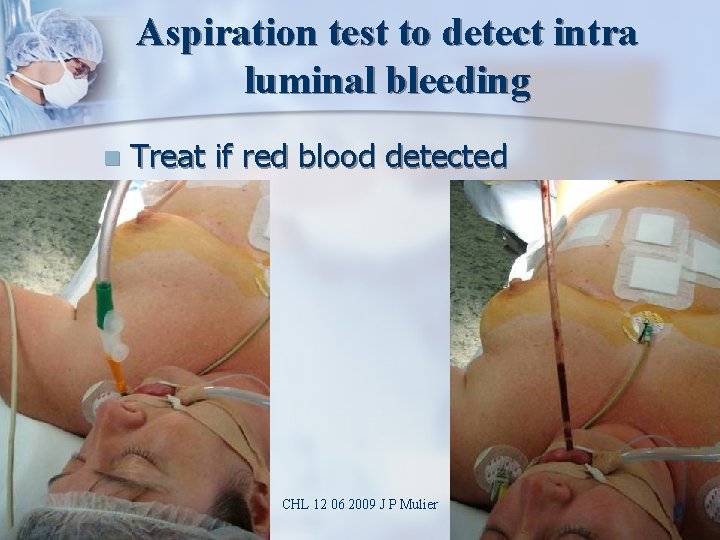
Aspiration test to detect intra luminal bleeding n Treat if red blood detected CHL 12 06 2009 J P Mulier

2. Leakage n Ask your anesthesiologist n To perform a good leakage test. n To keep blood pressure sufficient during inspection for ischemia n JPMulier B Dillemans 2007 n To increase cardiac output and splanchnic perfusion by n Raising end tidal CO 2 n Give sufficient volume expansion n Work at lowest IAP possible n JPMulier B Dillemans 2008 CHL 12 06 2009 J P Mulier

Post operative pneumonia due to A: Aspiration at induction Mask ventilation with oxygen? Sufficient O 2 when mask cpap Rapid sequence? No mask ventilation Risk of hypoxia ! Re-intervention after band, bypass, stenosis, … Crush induction? (Crocoid pressure) Sellick maneuver even more dangerous! Difficult intubation: risk of blood aspiration Empty stomach, use. J P safety bird, CHL 12 06 2009 Mulier
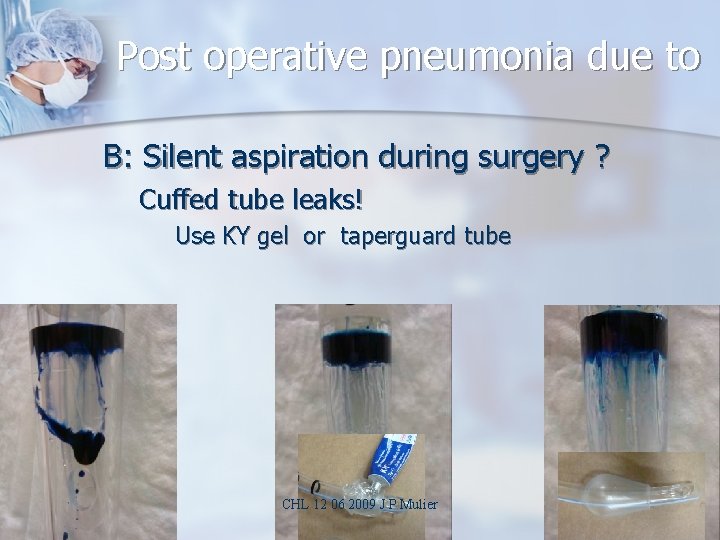
Post operative pneumonia due to B: Silent aspiration during surgery ? Cuffed tube leaks! Use KY gel or taperguard tube CHL 12 06 2009 J P Mulier
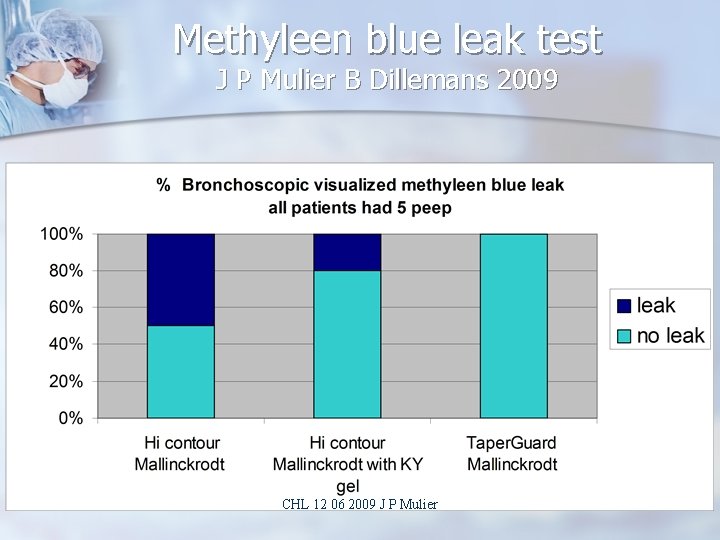
Methyleen blue leak test J P Mulier B Dillemans 2009 CHL 12 06 2009 J P Mulier

Post operative pneumonia due to C: Post extubation aspiration ? 1. Superficial breathing 1. Use pressure support during end of operation 2. Non invasive support ventilation 2. Insufficient 1. Use 3. Not decurarization Brideon fully awake 1. Use short acting desflurane, remifentanyl, pressure support, … CHL 12 06 2009 J P Mulier

Hypercapnic pressure support ventilation JPMulier 2008 n Increases cardiac output n n Lowers airway pressures Improves saturation per op Rapid awakening and spontaneous breathing n n Non surgical time between OP < 20 min Less pain when awakening n n Less wound infections Extra doses morphine given during end of surgery Better post op breathing n less post op. CHL aspiration pneumonia 12 06 2009 J P Mulier
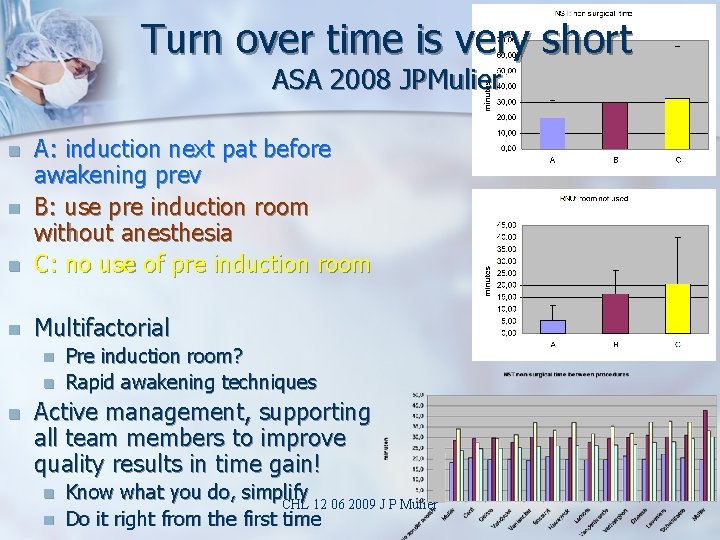
Turn over time is very short ASA 2008 JPMulier n A: induction next pat before awakening prev B: use pre induction room without anesthesia C: no use of pre induction room n Multifactorial n n n Pre induction room? Rapid awakening techniques Active management, supporting all team members to improve quality results in time gain! n n Know what you do, simplify CHL 12 06 2009 J P Mulier Do it right from the first time

Conclusion n J F Kennedy: n Inventor n of the transdisciplinarity ‘Ask not only what the anaesthesiologist can do for you, ask also what you can do for the anaesthesiologist. ’ CHL 12 06 2009 J P Mulier

Make your anaesthesiologist member of ESPCOP n And he will ask you what he can do for you! CHL 12 06 2009 J P Mulier

Scientific meeting CHL 12 06 2009 J P Mulier

Be a transdisciplinary team n n n Jan. Mulier@azbrugge. be www. publicationslsit. org/jan. mulier www. espcop. org CHL 12 06 2009 J P Mulier
- Slides: 26