Social Care Health in Newcastle Cathy Bull Newcastle

Social Care & Health in Newcastle Cathy Bull, Newcastle City Council Guy Pilkington, Newcastle Gateshead Clinical Commissioning Group

The journey towards integration • Marathon • Sprint • Or Steeplechase. . .

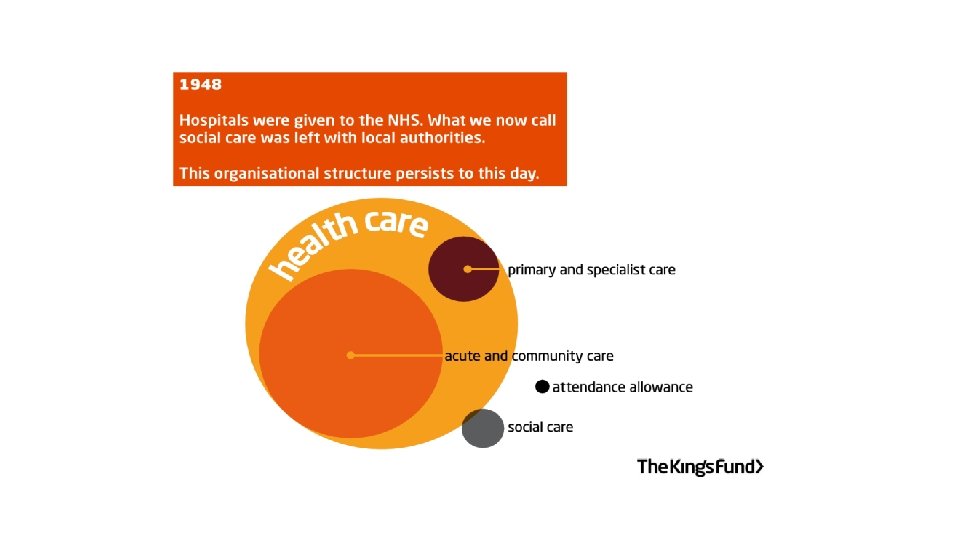
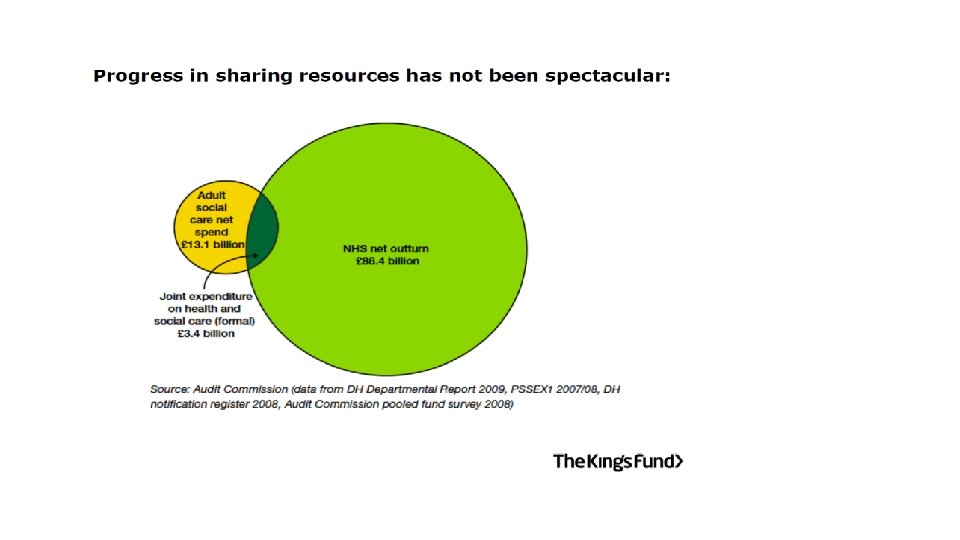

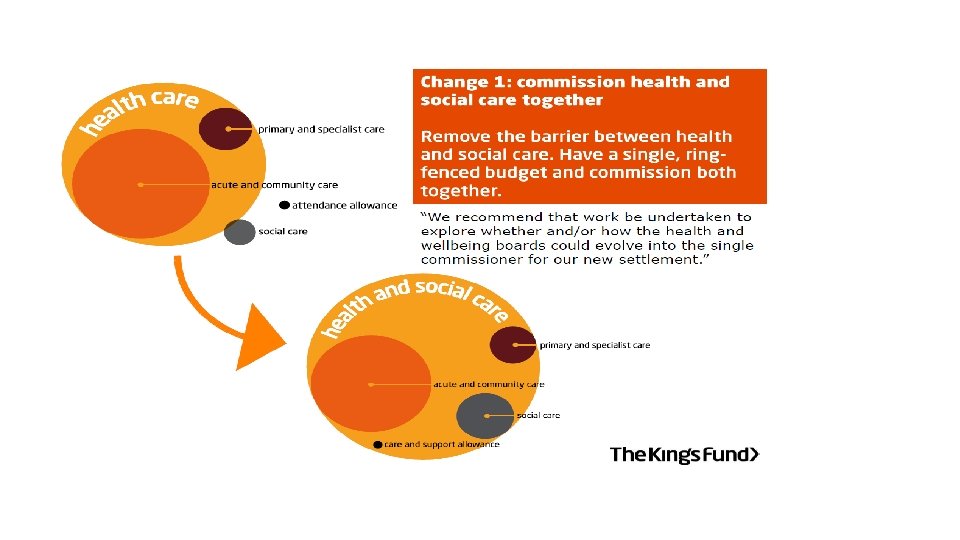


Local landscape in Newcastle • 280, 200 population • 1 CCG for Newcastle & Gateshead • 1 large high performing Acute Trust providing tertiary services and Community Health Services also • 1 MH & LD Trust covering 6 LAs • 1 LA • 34 GP Practices

Newcastle’s health and care challenge § Demographic shift already impacting heavily § Health improving, but not fast enough to catch up with the best for many decades without much greater prevention § How to secure preventive spend while running-to-stand-still on treatment § Need to simultaneously embed best-start in early life, while acting to relieve service demand through secondary prevention § How to make rational choices across a very diverse range of wellbeing options (from parks to cancer drugs)

Newcastle’s financial challenge § Overall health and social care budget of around 700 m § Gap between growth in demand expected funding over next five years around 25% § Significant impact of continued reductions in social care and demand growth in NHS § This is a shared problem – cannot be tackled at an organisational level

Our history of integration • Strategic partnerships historically strong but weakened during PCT era • Proliferation of small MDT initiatives developed incrementally in the years of plenty • Series of Joint Commissioning posts with mixed success • Co location of social workers and district nurses didn’t achieve anticipated results • Strong leadership but pulling in different directions

How far have we come? We have now… • Co located social care and community health in a single point of access and developed single operating model for rapid response/reablement, consolidating all the small teams (over 80 staff) • Expanded it with more social workers to fulfil Care Act prevention duties • Looking at next stage of developing a shared record and “trusted assessment. ” • Bed based intermediate care model jointly delivered • But system demand pressures growing and financial resources reducing • Still no joint teams for LD • Mental Health still on the periphery but want to be at the heart of any new model

More of the same isn’t enough “Insanity is doing the same things over and over, expecting to get a different result” “Problems cannot be solved by the same level of thinking that created them”

Did the Better Care Fund help? § BCF accelerated the “whole system” conversation § Pooled budget requirement generated learning for the future § Emerging priorities – Intermediate Care; Falls Prevention; Ways to wellness § BUT § Not new money – the Pooled budget already underpins key services in social care and community health § National policy constraint – narrowed focus to reducing admissions to hospital § BCF national rhetoric – the answer to social care financial pressures despite the operational guidance being clear that it would not solve the underfunding of social care

System integration - vision “Our vision for Newcastle in 2018/19 is a fully integrated health and care system designed to meet people’s needs in a sustainable way”

System integration in Newcastle – key principles § Leadership Commitment – to promote a whole system culture § Financial Framework – to develop a financial framework that incentivises better health and wellbeing outcomes for the population § Model Configuration – to build new models of care around a locality model of c. 50, 000 – 70, 000 population as a basis for building an integrated response § Model Design – to be designed to address the needs of the local population § Future Workforce – to develop ways of removing silos created by professional and organisational cultures

What can bring us together? • Health – the ability to adapt and self-manage in the face of social physical and emotional challenges • Person-centred approaches • Care and support planning • Holism • Population approaches • Focus on inequalities • Shifting the curve • Multiple levels of integration • • Health and social care Physical and mental health Primary / community and secondary care Statutory and voluntary sectors
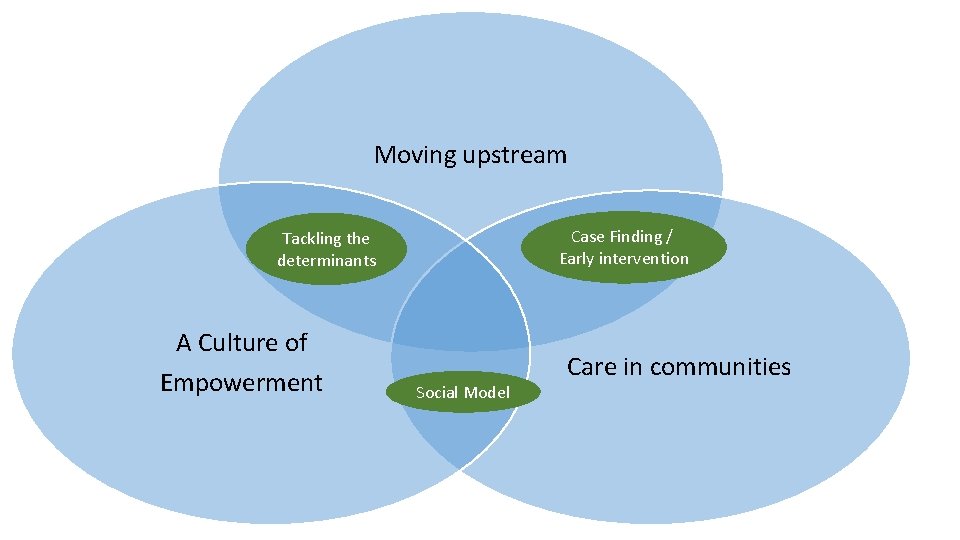
Moving upstream Case Finding / Early intervention Tackling the determinants A Culture of Empowerment Social Model Care in communities

Developing our new model of care • Bottom up approach • Coalescing around principles and culture not organisational form • Development of a common purpose across clinical and care communities to achieve culture change • Focus on better experience and outcomes for people • Better value for money • Involves all front line staff in chosen locality in collaborative co design approach with local people and voluntary organisations • Will “road test” new approaches then think organisational form

Risks and organisational concerns § Capacity for change § Resources § Organisational form takes precedence over outcomes § Untested innovation – building the case § Over-focus on high risk / high use cohorts § Leadership challenge § This will not be easy


System Enablers § Shared vision, collective system leadership and commitment to long term sustainability of vision and purpose by all organisations § Flexibility to develop local incentives § Local control of decisions on commissioning and co-operation § Workforce-commitment § Genuine engagement and involvement-service users as experts in design of care § Joined up approach to managing and influencing national government and agencies
What does this mean for us all? Don’t Do § Organisational thinking § System thinking § Activity planning § Population planning § Disease/organ focused care § Whole-person care § Service/task delivery § Pathway delivery § Service accountability + responsibility § System accountability + responsibility

Is it worth the effort? Benefits for people § Improved experience and satisfaction for people through provision of joined up care and smoother pathways § Delivering better outcomes for people living with long term conditions, supporting people to regain as much independence as they can § Shifting the curve from crisis management to supported self management § Better informed and empowered people with increased confidence to have more control over their own health § Promoting better long term health outcomes and tackling inequalities rather than measuring inputs and processes
- Slides: 25