Small intestine SUCCUS ENTERICUS Small intestinal secretion Brunners
Small intestine
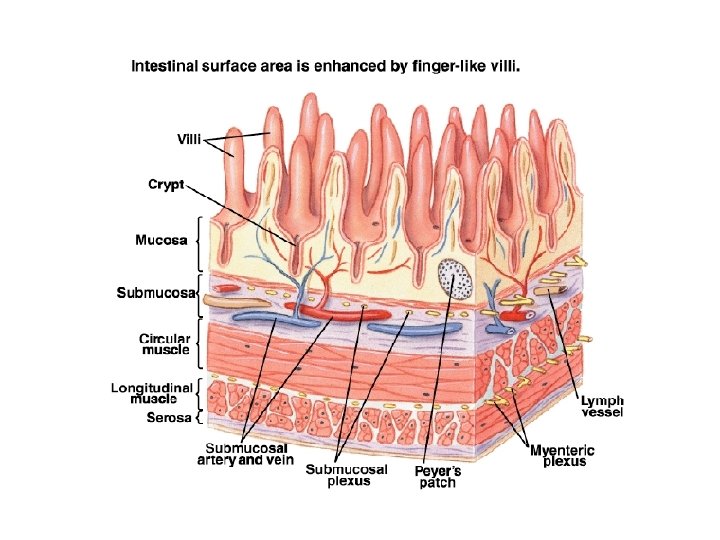
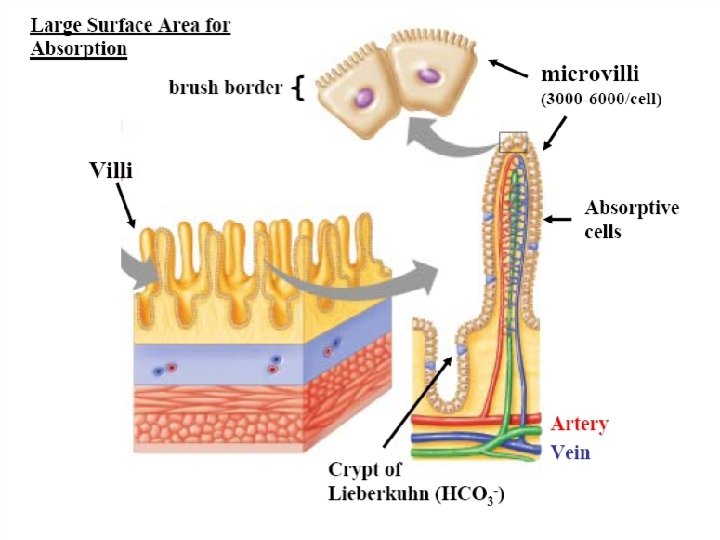

SUCCUS ENTERICUS:

Small intestinal secretion: • • • Brunner’s gland. Crypts of Lieberkuhn. Mucus from goblet cells. EC Cell : IF Paneth Cell: Cytokines called Defensins.

Composition: Watery, Colorless. p. H = 8 -9 (Alkaline fluid). Water – 99%. Solid - 1 %. Organic: Mucus , Enzymes. Inorganic : Na+ , K+, Ca+, Cl-, HCO-, PO 4 -

Enzymes: 1. Amylase. Starch maltose. 2. Lipase. Fatty acid +Glycerol. 3. Peptidases. Protein Amino acid. 4. Maltase. Maltose Glucose.

5. Lactase: Lactose Galactose + Glucose. 6. Nucleotidases: Nucleotides Nucleosides. 7. Nucleosidases: Nucleosides Purines + Pyramidines

Functions: Complete digestion of: • Carbohydrates. • Proteins. • Fats.

Functions: • Mixing of food • Spreading of chyme • Propulsive movement

Types of movement: 1. Rhythmic segmental movements 2. Pendular movements 3. Peristalsis 4. Interdigestive peristalsis 5. Villi movements

Rhythmic segmental movements: Ø A loop of intestine is divided in to number of segments with nearly equal size. Ø Each of this again quickly divide and the neighouring halves suddenly unite to form a new segment.
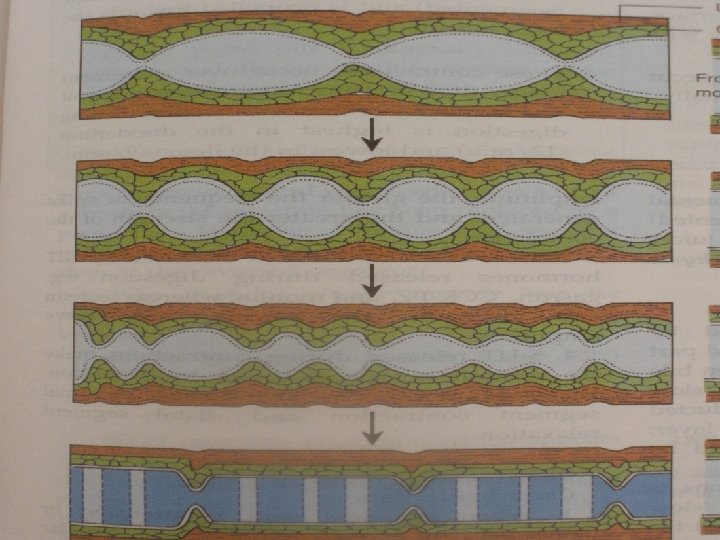

Function : • Cut the larger food particles in to smaller one. • Mixing of the food with the intestinal and other digestive juices. • Changing the layer of food in contact with the mucosa thus facilitating absorption.

Pendular movement: Side to side movements accompanied by lengthening and shortening of the intestine. One entire loop of intestine is involved. Function: Similar to that of rhythmic segmental contraction.

Peristalsis: • It is defined as a wave of contraction preceded by a wave of relaxation that travels aborally. • It is neurogenic and depends on Myenteric plexus. • When the intestine is stretched due to the presence of food, a contraction above and relaxation below appears. (MYENTERIC REFLEX)
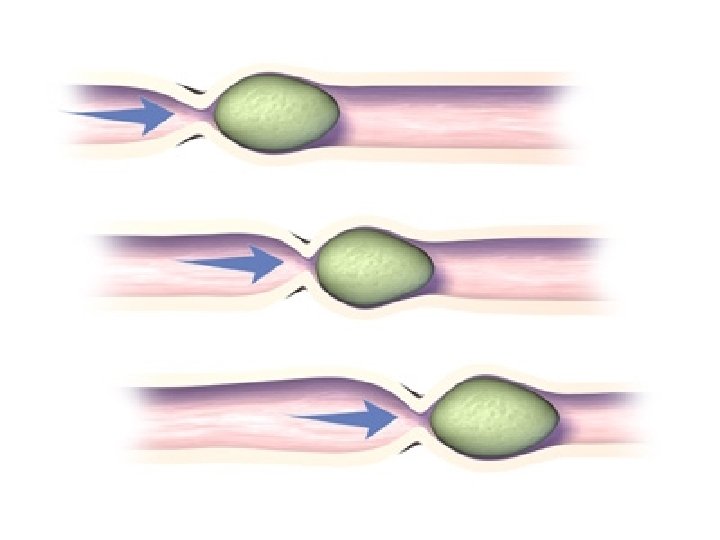

• The rate of movement is 0. 5 -2 cm/sec. • Faster in the proximal part and slower in the terminal part. Functions: • Progression of the chyme towards the ileocaecal valve. • Spreading of the chyme along the intestine.

Interdigestive peristalsis. This occurs when the food is absent in the small intestine. Takes Orgin in the duodenum and spreads towards the ileum.

Function: • It helps to clear off any food residue that remains after previous meal. • Inhibits the migration of colon bacteria in to the distal ileum

Movements of Villi: They are initiated by local nervous reflexes that occurs in response to the chyme in the small intestine. 1. Lashing movements 2. Lengthening and shortening movements
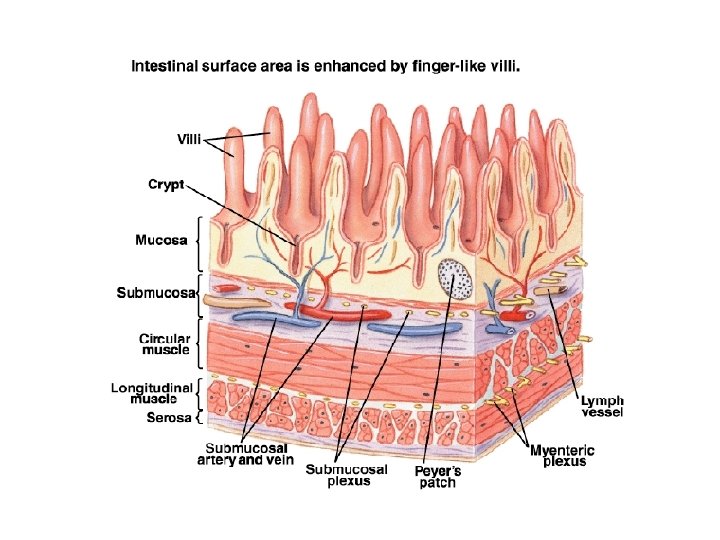
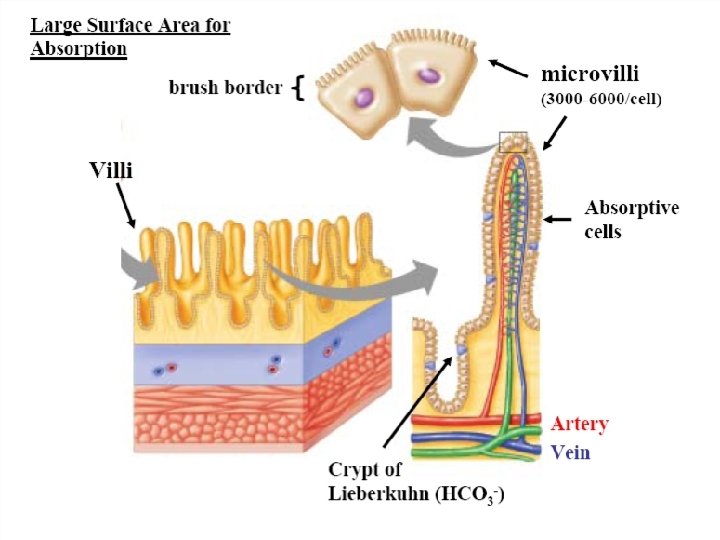
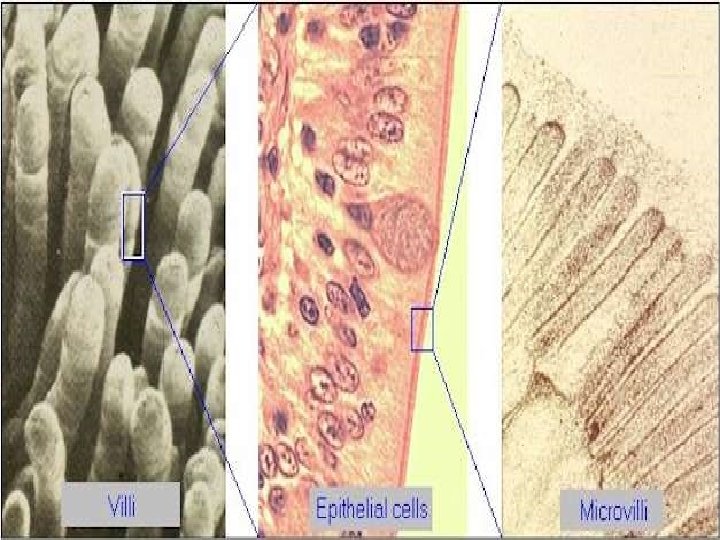

Functions: • These movements facilitate the flow of blood and lymph. • Increase absorption

Large intestine:
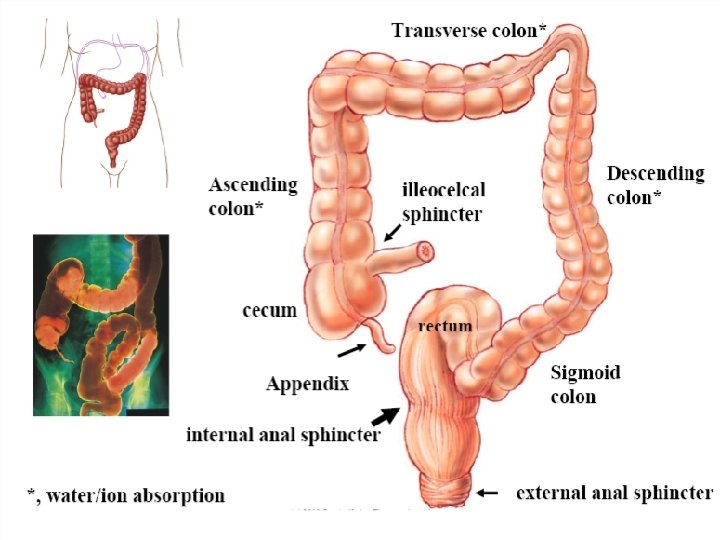

No villi on mucosa Short glands with numerous goblet cells

Functions • Absorption of water and electrolytes. • Storage of fecal matters. • Synthesis of various substances. Vit B complex, Vit K , Gases like CO 2, H 2 S etc • Secretion Watery fluid containing K+ & HCO 3 - + Mucin

• Bacterial digestion. Cellulose, Hemicellulose, some undigested Fat, Proteins, Carbohydrates.

Movements are sluggish. 2 types : 1. Mixing movements / Haustrations. 2. Propulsive movement / Mass movement.

Mixing movements /Haustrations: • Same as that of segmental movements in small intestine but involve larger segments. • Bag like sac =Haustrations formed.

Functions: • Faecal matter is slowly rolled over so that the faecal matter is exposed to the mucosa of large intestinal and this facilitates fluid absorption.

Mass peristalsis: • Occurs once or twice a day Stimulus: Filling of the stomach /over distention of the colon. Ø Evacuation of the colon contents.

Applied aspects: § Constipation - motility is less. § Diarrhoea – motility is more. § A ganglionic megacolon: congenital absence of the ganglionic cells in myenteric and submucosal plexus of a segment of the distal colon. • Faecal matter accumulates in this region.

Defaecation

Process by which the unwanted food residue or faeces is evacuated at regular intervals

Nerve supply:

Parasympathetic: Vagus(X) and S 2, S 3, S 4 Afferent: Detect pressure changes in the rectum. Efferent: Contraction of the rectum, SC, DC, TC. Relaxation of the internal sphincter.
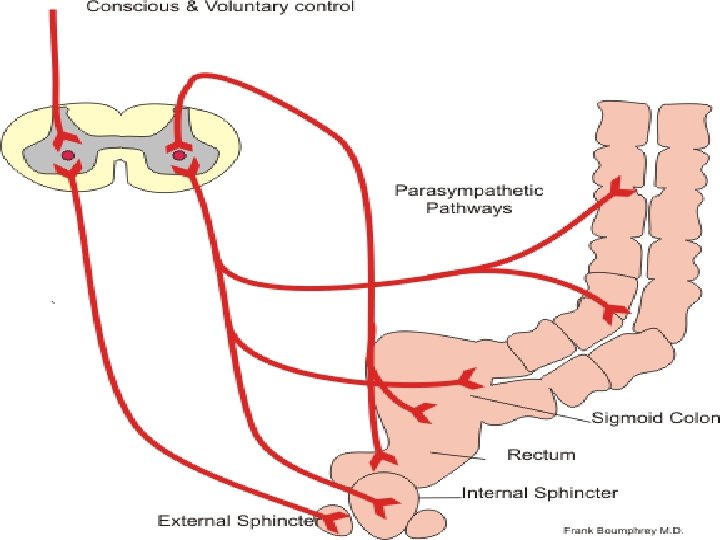

Sympathetic: • Presacral nerve (T 12, L 1, L 2). • Afferent: Carry pain sensation from rectum. • Efferent: Cause the contraction of the internal sphincter.

Somatic: Pudendal nerve(S 2, S 3, S 4). Supplies the external sphincter and keeps it in a tonic contractile state.

Intrinsic reflex: Faeces enter the rectum Distension of the rectal wall Afferent impulses Myenteric plexus Peristaltic wave DC, SC, Rectum Forces faeces towards the Anus External sphincter relaxes

Parasympathetic reflex: Nerve endings of the rectum stimulated Signals to spinal cord(sacral segments) Reflexly to DC, SC, Rectum, Anus. • Intensify the peristalsis • Relaxes the internal anal sphincter.

Vomiting / Emesis:

Is a reflex act by which the upper GIT is relieved of its contents through the mouth. Initiated by stimulating vomiting centre.

Three phases: Nausea: Conscious recognition of subconscious excitation in the area in the medulla closely associated with vomiting centre. • Development of duodenal, jejanal contractions • Increase salivation, Yawning, Rapid deep irregular breathing.

Retching: Intermittent forceful contractions of diaphragm and abdominal wall. Ø LES closes. Ø Pyloric part contact , Stomach relaxes. Ø LES opens , Oesophagus relaxes. Ø UES relaxes , soft palate pushes upwards.

Gastric evacuation/vomiting: • • Deep breath. Glottis closed Oesophagus contracts. Contents of the stomach is thrown out.

Thank you

Gastric Empting

The rate at which substances leaves the stomach and enters the duodenum. Regulated by: • • Stomach factors. Duodenal factors. Neural factors. Hormonal factors

Stomach factors: 1. Volume of gastric contents: Increase in gastric content facilitates gastric emptying. 2. Consistency of food: • Liquids-Semisolids-Solids • Chemical composition: Carbohydrates-proteins -fats.

3. Acidity: Weak acids and neutral solutions -Strong acids. 4. Osmolar concentration : Higher the Osmolar concentration – slower emptying.

Duodenal factors: 1. Distension of duodenum: Reflexly inhibit gastric emptying through sympathetic nerves. Prevent the overloading of the duodenum with partially digested food. 3. Acid in the duodenum: Reduces the gastric motility mediated through CCK-PZ , Secretin , VIP etc

Neural: Parasympathetic : increase. Sympathetic : decrease. Hormonal: Gastrin –facilitates VIP , CCK-PZ, Secretin etc – decrease
- Slides: 56