Small Bowel Transplantation l yekehfallahphd student of nursing
Small Bowel Transplantation l. yekehfallah-phd student of nursing education 2012 1

Intestinal Transplantation Small-intestine transplantation continues to evolve as a surgical procedure used in the management of intestinal failure in children and adults n Intestinal transplantation offers the hope of increased longevity & improved quality of life to patients with intestinal failure and life -threatening complications of chronic TPN n l. yekehfallah-phd student of nursing education 2012 2

Intestinal Transplantation n Over the last three decades, intestinal transplantation has evolved from experimental to a standard therapeutic option for intestinal failure patients Primarily a pediatric procedure with ~2/3 s performed on children Remains less successful to other solid organ transplantation -> presumably due to the preponderance of lymphocytes in the bowel (strong stimulus for rejection) l. yekehfallah-phd student of nursing education 2012 3
Intestinal Transplantation n Indications include: n n n n Short-bowel syndrome with complications associated with parenteral nutrition Irreversible intestinal failure End-stage liver disease for combined liver and smallintestine transplantation Congenital mucosal disorders Chronic pseudo-obstruction of intestine Locally invasive tumors at the base Transplant options include: n n Isolated intestinal (cadaveric or living-related) Multivisceral transplantation (combined liver and multivisceral) l. yekehfallah-phd student of nursing education 2012 4

Intestinal Transplantation Contraindications n Absolute contraindications n n n Congenital immunodeficiency syndromes, systemic malignancy, metastatic disease, AIDs, cardiopulmonary insufficiency & overwhelming sepsis Because of the risk of unrestrained graft versus host disease (GVHD) Relative contraindications are evolving, but concern about transplantation from CMV- or EBV-positive donors to CMV- or EBV-negative recipients, weight (<5 kg) and elderly pts n n High morbidity & mortality rates associated with the development of CMV or lymphoproliferative disease in pediatric intestinal transplants Although critically ill patients should be excluded, a history of multiple abdominal surgeries is not a contraindication for l. yekehfallah-phd student of nursing transplantation education 2012 5

Indications for Small Bowel Transplant as recommend by the American Gastroenterology Association AGA recommends SBT on patients who have Short Bowel Syndrome ( Functional Small Intestine of less than 200 cm) and have developed severe complications from Total Parental Nutrion. n Small Bowel transplants have been performed on children with motility disorders and malignancy n l. yekehfallah-phd student of nursing education 2012 6

Common Causes of Short Bowel Syndrome Neonates: Necrotizing enterocolitis n Children: Congenital abnormalities such as necrotizing entercolitis, intestinal atresia, mid gut volvulus, gastrochisis n Adults: Chron’s Disease, Mesenteric Thrombosis, Trauma, Desmoid Tumors, mesenteric occlusion, midgut volvulus, traumatic disruption of SMA/SMV n l. yekehfallah-phd student of nursing education 2012 7

Complications of TPN requiring Small Bowel Transplant 1. Frequent Central- Line related Sepsis: 2 episodes of systemic sepsis secondary to line infection per year, 1 episode of line related fungemia, 1 episode of septic shock, or Acute Respiratory Distress Syndrome 2. Liver Failure : Increased Billirubin, Increased Liver enzymes, splenomegaly, gastroesophageal varcices, thrombocytopenia, coagulopthy, hepatic fibrosis, or cirrhosis 3. More than ½ of the sites used for TPN ( jugular, subclavain, femoral) have become inaccessible due to thrombosis 4. Severe Dehydration l. yekehfallah-phd student of nursing education 2012 8

Contraindications of Small Bowel Transplant Presence of Active Infection n Aggressive Malignancy n Multi-System Organ Failure n Cerebral Edema n AIDS n l. yekehfallah-phd student of nursing education 2012 9

History of the Procedure Lillehei et al reported the first case of human bowel transplantation in October 1967 n Alexis Carrel was the first one to perform it in an animal model n Before 1970, 8 clinical cases of smallintestine transplantation were reportedly performed worldwide n maximum graft survival time was 79 days n All patients died of technical complications, l. yekehfallah-phd student of nursing sepsis, or rejection education 2012 n 10

History of the Procedure n This continued until the early 1980 s, with the advent of cyclosporine, immunosuppressive medications (azathioprine), steroids, and antilymphocyte globulin (ALG) n n Deltz reported the first successful long-term transplantation in Germany n n n However, clinical results with cyclosporine were disappointing (most grafts lost to rejection) 1988 - 42 -year-old woman received a segment of her sister's jejunum and ileum The graft survived until 1992 -> lost to chronic rejection Goulet reported on 9 patients in 1990 (including a 9 -monthold infant who received 2 intestinal transplants) with poor success rates under cyclosporine-based immunosuppression n Graft survival time ranged from 10 days to 49 months. l. yekehfallah-phd student of nursing education 2012 11

History of the Procedure n n The most significant advance in the development of intestinal transplantation was the introduction of TACROLIMUS (1990) The Starzl group (1998) reported that in 55 children who underwent small-intestine transplantations with tacrolimus n n n 28 girls and 27 boys Median age = 3. 2 years of age Patient survival rates were 55% Graft survival rates were 52% Greater understanding of the unique immunologic properties of the intestine has furthered the advancement of small-intestine l. yekehfallah-phd student of nursing education 2012 transplantation 12

History of the Procedure As a result of these advances and a growing appreciation of the phenomenon of chimerism, the number of intestinal transplants has steadily increased n More than 100 intestinal transplants being performed each year in the United States n Most active programs in North America: n n Univ of Pittsburgh, Univ of Nebraska, Univ of Miami, and the Toronto Hospital l. yekehfallah-phd student of nursing education 2012 13

Intestinal Transplantation Etiology TPN = current standard of care for patients unable to maintain adequate nutrition via the intestinal tract alone n Patients with poor intestinal function who cannot be maintained on TPN are potential candidates for transplantation n l. yekehfallah-phd student of nursing education 2012 14

Intestinal Transplantation Etiology n Intestinal failure—defined as the inability to maintain sufficient electrolyte, nutrient, and fluid balance for more than 1 month without TPN and no adaptive potential to meet these needs in the future n May result from surgical short-bowel syndrome or intestinal dysfunction in children l. yekehfallah-phd student of nursing education 2012 15

Intestinal Transplantation Etiology n Worldwide, the leading cause of intestinal failure is short-bowel syndrome caused by surgical removal n n n ~10 -20 cm of small bowel needed with an ileocecal valve 40 cm without a ileocecal valve Conditions leading to short-bowel syndrome include n n Midgut volvulus Gastroschisis Trauma l. yekehfallah-phd student of nursing Necrotizing enterocolitis (NEC) education 2012 16
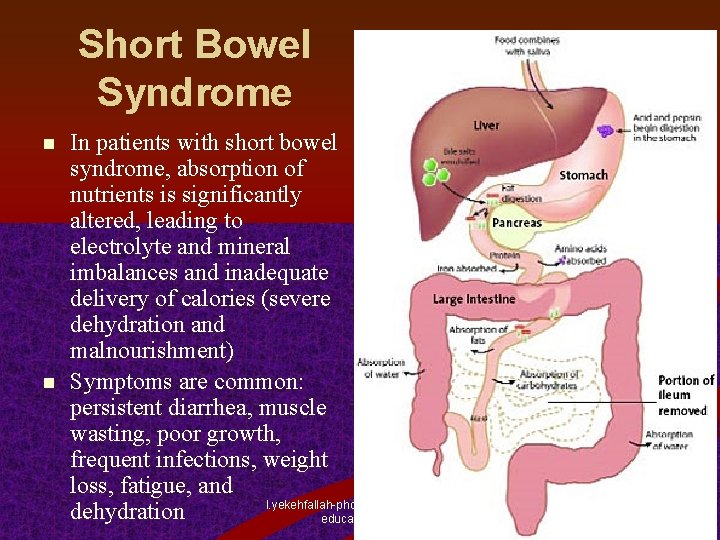
Short Bowel Syndrome n n In patients with short bowel syndrome, absorption of nutrients is significantly altered, leading to electrolyte and mineral imbalances and inadequate delivery of calories (severe dehydration and malnourishment) Symptoms are common: persistent diarrhea, muscle wasting, poor growth, frequent infections, weight loss, fatigue, and l. yekehfallah-phd student of nursing dehydration education 2012 17

Intestinal Transplantation Etiology n Other causes of intestinal dysfunction are n Absorptive disorders n Microvillus inclusion n Secretory diarrhea n Autoimmune enteritis n Dysmotiliy disorders n Pseudo-obstruction n Hirschsprung disease n Visceral neuropathy n A tumor (desmoid tumor and familial polyposis (eg, l. yekehfallah-phd student of nursing Gardner disease)) education 2012 18

n Intestinal Transplantation Etiology Leading causes of intestinal failure in children (in order of decreasing frequency) n n n n n Leading causes of intestinal failure in adults n n Crohn’s disease Superior mesenteric artery thrombosis Superior mesenteric vein thrombosis Trauma Desmoid tumor Volvulus Pseudo-obstruction Massive resection secondary to tumor Radiation enteritis Intestinal atresia Gastroschisis n Crohn’s disease Microvillus involution disease n NEC n Midgut volvulus (leading to n infarction) n Chronic intestinal pseudon obstruction Massive resection secondary n to tumor Hirschsprung diseasel. yekehfallah-phd student of nursing education 2012 19

Intestinal Transplantation Etiology n Intestinal transplantation is reserved for TPN-dependent patients with permanent intestinal insufficiency n Pts become intolerant of TPN -> which manifests in potentially fatal complications n Recurrent sepsis n Thrombosis of access sites n Metabolic disorders n Cholestasis n Hepatic dysfunction l. yekehfallah-phd student of nursing education 2012 20

Intestinal Transplantation n Isolated intestinal grafting n n Combined small-intestine and liver transplantation n n Poor venous access or moderate hepatic dysfunction and for those who develop severe fluid and electrolyte abnormalities that cannot be managed with TPN Intestinal insufficiency & irreversible hepatic failure or coagulopathy Multivisceral transplants (ie, combined stomach, duodenum, pancreas, small intestine) n Following extensive surgical resection of abdominal l. yekehfallah-phd student of nursing organs for aggressiveeducation 2012 tumor or severe abdominal 21

Preoperative evaluation and selection Preoperative evaluation requires a complete multidisciplinary assessment to clearly define the cause of isolated intestinal or intestinal/hepatic failure n Evaluation of comorbidities and organ dysfunction n n Optimization of preoperative morbid conditions (infection, malnutrition) can significantly affect outcome l. yekehfallah-phd student of nursing education 2012 22

Preoperative evaluation and selection n Referral criteria: Intestinal failure with impending lifethreatening complications (i. e. end-stage liver disease) n Recurrent sepsis (bacterial translocation 2 ndary chronic TPN) n Impending loss of central venous access n Locally invasive tumors of the abdomen (desmoid) n n Rescue therapy for visceral vascular thrombosis, primary intestinal graft loss, and poor quality of life secondary to l. yekehfallah-phd student of nursing education 2012 23

Preoperative evaluation and selection n Referring patients before the onset of hepatic dysfunction is important Progression of liver injury, as manifested by jaundice, significantly influences life expectancy n Bilirubin concentrations >3 mg/d. L have 1 - and 2 -year survival rates of 42% and 20% n Bilirubin <3 mg/d. L have a survival rate of 80% n p. T >15 and p. TT >40 also associated with poorer outcomes l. yekehfallah-phd student of nursing n education 2012 24
Isolated intestinal transplantation n Transplantation may not be indicated for patients who have complications of their disease but maintain a borderline length of intestine n n May respond to intensive medical management Medical management may involve Modified administration of TPN n Selective gut decontamination l. yekehfallah-phd student of nursing n Optimized enteral feedings ( at least 20 -30% education 2012 n 25
Isolated intestinal transplantation Must evaluate liver function n Suspected progression of liver dysfunction requires prompt evaluation for intestinal transplantation and a liver biopsy to determine whether a combined liver and small-intestine transplantation is needed n l. yekehfallah-phd student of nursing education 2012 26
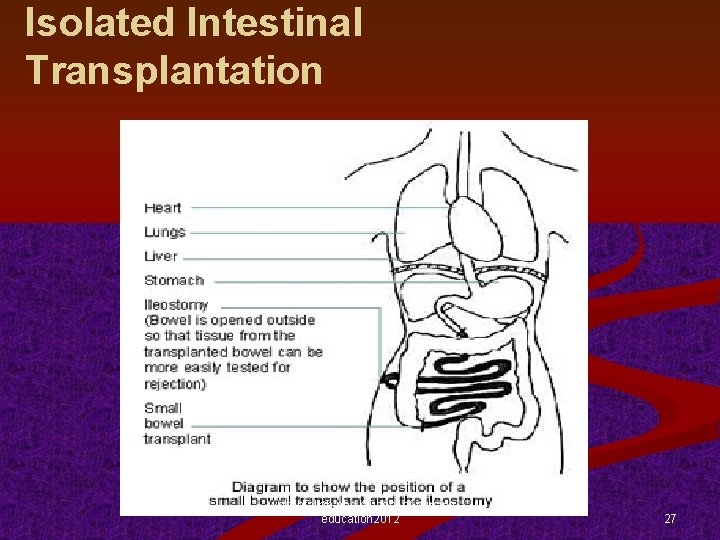
Isolated Intestinal Transplantation l. yekehfallah-phd student of nursing education 2012 27
Combined liver and smallintestine transplantation n Patients with end-stage liver disease (often TPNrelated liver disease) & intestinal failure n n n The highest mortality rate of all patients on the waiting lists for organ transplantations Chronic TPN -> cholestatic liver disease (esp. children) Very few size-match quality organs are available, and these patients are competing for organs with patients on longer waiting lists who are waiting for an isolated liver transplantation n n Represent only 2% of the patients on the liver waiting list Do not rank well in the MELD (model for end-stage liver disease) and PELD (pediatric end-stage liver l. yekehfallah-phd student of nursing education 2012 28 disease) scoring system

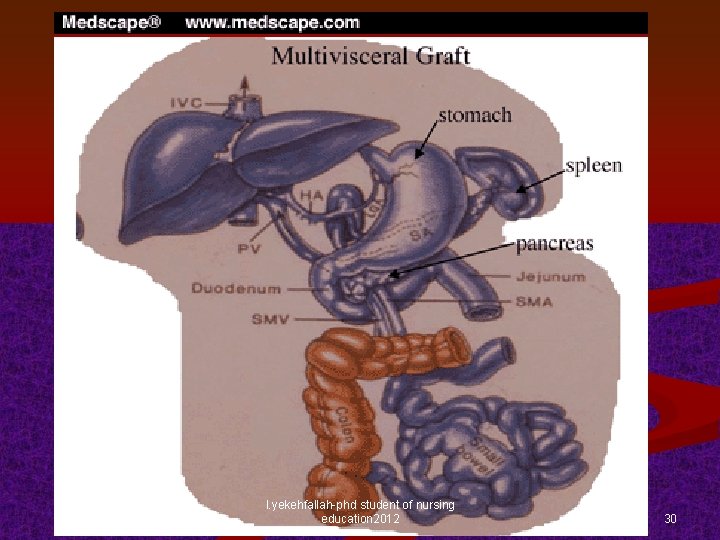
Multivisceral transplantation Pts with permanent intestinal dysfunction, those with TPN dependency with complications, and those with a systemic motility disorder (e. g. , chronic pseudoobstruction, traumatic loss of the stomach or duodenum) n Can receive a stomach, duodenum, pancreas, and small intestine, with or without the liver n l. yekehfallah-phd student of nursing education 2012 29
l. yekehfallah-phd student of nursing education 2012 30

Intestinal Transplantation Workup Preoperative workup: n All potential transplant recipients require a review of n Comorbidities n Relevant laboratory n Imaging studies n l. yekehfallah-phd student of nursing education 2012 31

Intestinal Transplantation Workup n Laboratory studies include the following: n n n n CBC Chem-20 Prothrombin time (PT) Activated partial thromboplastin time (a. PTT) Blood group and screen Serologic testing for HIV, hepatitis B virus (HBV), hepatitis C virus (HCV), CMV, EBV, syphilis, blood group system (ABO), and human leukocyte antigen (HLA) status When indicated, a hypercoagulable workup (i. e. , protein C, protein S, antithrombin III, factor V mutation) l. yekehfallah-phd student of nursing education 2012 32

Intestinal Transplantation Workup n n Imaging Studies: Perform angiography and or additional Duplex studies n Assess the vascular supply for potential isolated living -related intestine donors n n n Angiography helps evaluate the SMA to ensure a normal vascular intestinal distribution Duplex and Doppler studies help asses for possible inflow/outflow stenosis Adequate assessment & preservation of the descending branch of the right colic artery are important to provide adequate blood supply to the areas of the terminal ileum and ileocecal valve l. yekehfallah-phd student of nursing education 2012 33

n n Intestinal Transplantation Workup Diagnostic Procedures: Dysmotility disorders require assessment of the stomach to exclude functional abnormalities n n Pediatric pseudo-obstruction pts require urologic assessment n n Up to 1/3 may have a dysfunctional urinary tract NEC -> full neurologic and pulmonary workup n n Manometry of the stomach, esophagus, and rectum may be required to exclude sphincter achalasia and gastroparesis Exclude the possibility of associated intraventricular hemorrhage & bronchopulmonary dysplasia student of nursing Liver biopsy in l. yekehfallah-phd patients with intestinal failure education 2012 34

n Transplantation – Preoperative Details Cadaveric small-intestine procurement n n Perform selective gut decontamination with antibiotic and antifungal preparations administered via a NGT along with standard IV antibiotic prophylaxis Use University of Wisconsin Universal Organ Preservation (UW) solution for both in situ flushing and cold storage n n Choose smaller donors than the intended recipient Preferentially direct CMV– donors to CMV– recipients Polyethylene glycol electrolyte solution Obtain wide exposure to the abdominal cavity, and encircle the abdominal aorta distally for subsequent insertion of the infusion cannula and proximally above l. yekehfallah-phd student of nursing education 2012 35 the celiac axis for cross-clamping

Transplantation – Preoperative Details n Cadaveric small-intestine procurement n n Perform dissection, in situ cooling of abdominal organs, and exsanguination before removing the organs to the back table for preparation. Mobilize and devascularize the cecum and ascending colon with care to preserve the ileal branches of the ileocolic artery. n n n Divide and close the ileum with the GIA stapler near the ileocecal valve Devascularize the colon by ligating and dividing the middle colic, left colic, and inferior mesenteric arteries near their origin After transection of the gastrocolic ligament and transection of the stapled sigmoid colon, remove the student of nursing large bowel andl. yekehfallah-phd greater omentum education 2012 36

n Transplantation – Preoperative Details Cadaveric small-intestine procurement n Free the small-bowel mesentery from its retroperitoneal attachments n n Preserve the vascular supply to the fourth part of the duodenum and the proximal part of the jejunum. Transect the proximal jejunum after mobilizing and dividing the ligament of Treitz and the IMV n n Expose the mesenteric root, abdominal aorta, and infrahepatic vena cava (including renal veins entry) Divide the highest jejunal vascular arcades Suture the jejunal end of the intestine to help orient the allograft At this stage, the intestine is attached to the donor only by the superior mesenteric pedicle (SMA & l. yekehfallah-phd student of nursing SMV) n education 2012 Divide the mesenteric root distal to the level of the ligated 37

Transplantation – Intra-operative Details n In situ organ cooling and removal Transaortic cooling requires perfusion with UW solution, 50 -100 m. L/kg, for pediatric donors n Remove the small-intestine graft by dissection of the SMA & SMV below the origin of the inferior pancreaticoduodenal artery n Excise a large Carrel patch from the anterior aortic wall containing the celiac axis and superior mesenteric artery. n n Procure iliac and carotid arteries and veins as l. yekehfallah-phd student of nursing potential vascular grafts education 2012 38
Transplantation – Intraoperative Details n Back-table preparation of organs Small-intestine grafts require little revision n If the pedicle of the superior mesenteric artery is too short, it may be lengthened with free vascular grafts n The anastomoses are made to the recipient aorta and portal vein or vena cava n l. yekehfallah-phd student of nursing education 2012 39
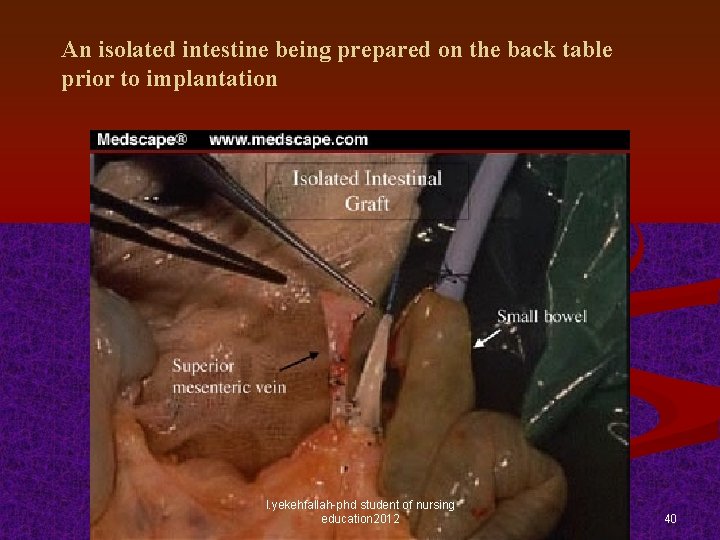
An isolated intestine being prepared on the back table prior to implantation l. yekehfallah-phd student of nursing education 2012 40
Transplantation – Intra-operative Details n Transplantation surgical therapy n Isolated living-related intestinal grafting requires as much as 150 -200 cm of distal jejunum and ileum to ensure that the recipient has a sufficient amount of small bowel to be completely free of TPN l. yekehfallah-phd student of nursing education 2012 41
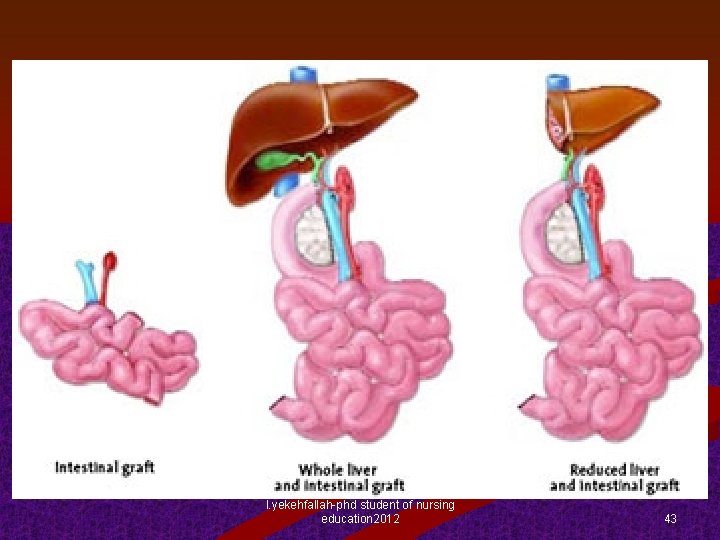
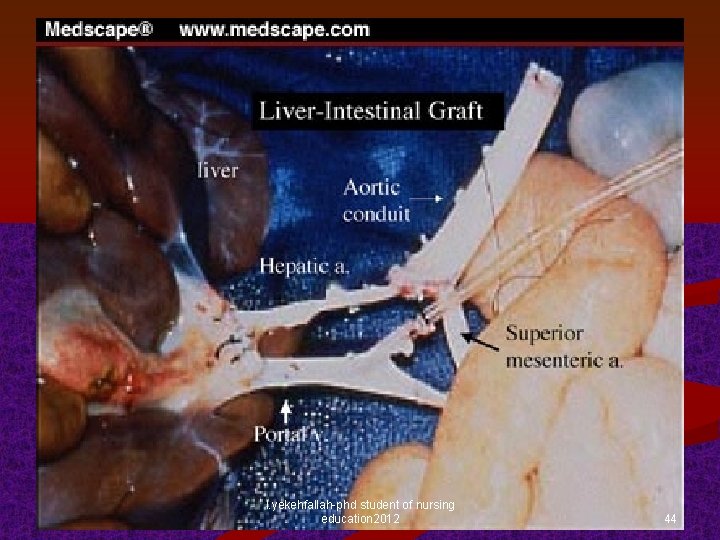
Transplantation – Intra-operative Details n Transplantation surgical therapy n n Carefully preservation of the vascular pedicle comprising the ileocolic artery & vein with end-to-side anastomoses to the recipient's infrarenal aorta & vena cava For cadaveric intestinal grafting, arteries are anastomosed directly to the infrarenal aorta with a Carrel patch n n Venous drainage through an anastomosis or patch to the recipient's IVC (combined) Isolated cadaveric intestinal grafting -> preferred venous drainage =portal vein In addition, a gastrostomy or jejunostomy is usually performed for continuous enteral feeding student of nursingendoscopic and Graft ileostomy l. yekehfallah-phd permits frequent education 2012 histologic postoperative monitoring 42
l. yekehfallah-phd student of nursing education 2012 43
l. yekehfallah-phd student of nursing education 2012 44

Transplantation – Postoperative Details n n Require ICU monitoring postoperatively Induction therapy with tacrolimus and steroids is typically begun most often in conjunction with an interleukin-2 (IL-2) receptor antibody n n Maintain high levels of immunosuppression early in the postoperative period (risk of rejection is greatest) Then follow with a lower dose for maintenance therapy n n n Consider the variable absorption and bioavailability of whichever immunosuppression regimen is used (ie, tacrolimus, cyclosporine microemulsion) Because the bioavailability of these drugs depends on intestinal surface area and transit time, the function of the grafts directly affects drug availability In addition, multiple immunosuppressive agents are used (as in other organ l. yekehfallah-phd student of nursing transplants) to minimize toxicity and to maximize therapeutic efficacy education 2012 45
Intestinal Transplantation – Follow-up care n At regular intervals, perform CMV antigenemia n Quantitative EBV polymerase chain reaction (PCR) surveillance n Routine cultures n Transplant ileostomal endoscopy & biopsy (as often as twice weekly) n n Additionally, monitor fluid status, stool losses, and serum electrolytes l. yekehfallah-phd student of nursing education 2012 46

Major Post Operative Complications Bleeding n Thrombosis n Anastomatic Leaks n Sepsis from bacterial translocation of Graft n GVHD n Acute Rejection n l. yekehfallah-phd student of nursing education 2012 47

Intestinal Transplantation Complications n Infectious complications account for ~60% of intestinal graft losses n n Bacterial and fungal infections in intestinal transplantation are similar to those found in other solid -organ transplantations Rejection and technical errors accounting for a further 36% An autopsy series found 94% had a coexisting infection, even in cases in which sepsis was not the immediate cause of death Post-transplant lymphoproliferative disease and graft rejection can lead to breakdown of the mucosal barrier, resulting in bacteremia or l. yekehfallah-phd student of nursing fungemia education 2012 48

Monitoring Intestinal Function Post- Transplant D-xlyose absorption Test: Decreased absorption might indicate rejection, or CMV infection n Fecal Fat Determination n Intestinal Motility: Assessed via Bowel Sounds and Stoma Output n TPN is continued post-transplant until intestinal function and motility return to baseline, enteral feeds begin, and TPN is tapered over a 4 -6 week period. n l. yekehfallah-phd student of nursing education 2012 49

Intestinal Transplantation Complications n CMV infection n n Immunosuppression is maintained to avoid breakthrough rejection but is decreased if the patient's condition worsens. ~ 15 -30% of patients (most often involves an allograft intestine) One of the most serious infections that can occur, because it can lead to loss of the transplanted organ and even death Incidence is highest in CMV-negative recipients who receive CMV-positive grafts (thus avoided) Infection is diagnosed by measuring CMV antigenemia and by findings on endoscopic examination n Endoscopy shows superficial l. yekehfallah-phd studentulcers, of nursing and histopathology education 2012 confirms CMV inclusion bodies 50

Intestinal Transplantation Complications n CMV infection n Treatment consists of IV ganciclovir in combination with CMV immune globulin (Cyto. Gam) and valganciclovir (Valcyte) tablets n Valganciclovir is the oral prodrug of ganciclovir (ester prodrug converted by intestinal & hepatic esterases) n Valganciclovir delivers the same active drug ingredient with up to 10 times more bioavailability n Ganciclovir is a synthetic analogue of 2'deoxyguanosine, which inhibits replication of human CMV l. yekehfallah-phd student of nursing education 2012 51

Intestinal Transplantation Complications n EBV-associated lymphoproliferative disease n Posttransplantation lymphoproliferative disease occurs more often in children > adults (29% vs. 11%) n n Occurs more commonly within 24 months after multivisceral transplantation than after isolated intestinal transplantation Linked to EBV infection in association with the use of anti. CD 3 monoclonal antibody (OKT 3) and steroids The high incidence in small-intestine recipients is presumably caused by the large amount of immunosuppression necessary to prevent transplant rejection EBV may lead to a wide spectrum of clinical disease, ranging from a benign mononucleosis syndrome to a polyclonal proliferative tumor or monoclonal type lymphoma. n n Present with fever, abdominal pain, & either lymphadenopathy or masses on abdominal imaging l. yekehfallah-phd student of nursing In addition, low-grade EBV infections often precede education 2012 posttransplantation lymphoproliferative disease 52

Intestinal Transplantation Complications n EBV-associated lymphoproliferative disease n Treatment of posttransplantation lymphoproliferative disease involves n Reduction of immunosuppression n Administration of ganciclovir (10 mg/kg/d) n Mortality has decreased with improved early diagnosis n In situ hybridization staining for EBV n Early ribonucleic acid (RNA) and EBV PCR surveillance l. yekehfallah-phd student of nursing n Combined with early intervention education 2012 53

Intestinal Transplantation Complications n Acute allograft rejection n Early diagnosis of allograft rejection, a major contributor to both the high morbidity and the high mortality associated with smallintestine transplantation, is essential Allograft rejection incidence rates as high as 87% have been reported Manifests clinically n n n n Fever abdominal pain increased output from the ostomy abdominal distention Acidosis Malabsorption and electrolyte abnormalities occur in some patients Bacterial & fungal sepsis can be life threatening because of the intestine's loss of barrier function, making early diagnosis and effective treatmentl. yekehfallah-phd of the rejection student ofvital nursing education 2012 54

Intestinal Transplantation Complications n Acute allograft rejection n Rejection is diagnosed by endoscopic intestinal biopsy n n Histologic evidence -> mucosal necrosis and loss of villous architecture with transmural cellular infiltrate n n Histopathology -> crypt cell apoptosis, cryptitis or crypt loss, necrosis, and endotheliitis Treatment -> n n n Diagnosis can be difficult because of the patchy nature of rejection and the presence of bleeding & perforation complications IV bolus of methylprednisolone (10 mg/kg), followed by steroid recycle and optimization of the tacrolimus level OKT 3 therapy may be used to treat steroid-resistant rejection Some centers report that combined liver-intestine of nursing protective benefit transplantation l. yekehfallah-phd provides student a greater education 2012 (i. e. , lower incidence and severity of acute rejection) 55

Intestinal Transplantation Complications n Chronic allograft rejection n n With improvements in immunosuppressive drugs, chronic rejection has become an increasingly important cause of late allograft dysfunction Little is known of the clinical and pathophysiologic course of chronic intestinal rejection n In 1990, Goulet reported muscular fibrosis & chronic infiltrate with intact mucosal and epithelial structures in a smallintestine transplant removed from a 17 -month-old infant n n Obliterative arteritis, atrophic Peyer patches and mesenteric lymph nodes Possibly caused by injury to the vascular endothelium, with a complex inflammatory cascade occurring in the vessel wall n Therefore, prevention and treatment of chronic intestinal rejection arel. yekehfallah-phd difficult student of nursing education 2012 56

Intestinal Transplantation Complications n Graft versus host disease n Small intestine = immunocompetent organ n Although animal models have shown that GVHD is a common occurrence and GVHD has not been a significant clinical problem Acute GVHD presents 1 -8 weeks post-transplantation with n n n n Population of lymphoid cells can mount an immunologic response to the host—a GVHD reaction Fever Leukopenia Diarrhea Rash Other symptoms may include malaise, anorexia, arthralgia, and abdominal pain. Confirm diagnosis by biopsy Treatment -> high-dose steroids & antithrombocyte globulin or l. yekehfallah-phd student of nursing with OKT 3 education 2012 57

Intestinal Transplantation Complications n Technical errors (up to 50%) More common in children than in adults n May cause graft loss n The errors include n n Anastomotic leaks n Hepatic artery thrombosis n Biliary anastomosis leaks or stricture n Intra-abdominal hemorrhage n Intra-abdominal abscess l. yekehfallah-phd student of nursing n Chylous ascites education 2012 58

Intestinal Transplantation Outcome and Prognosis n In 1999, Mazariegos reported a 55% patient survival rate and 52% graft survival rate at 5 years following intestinal transplantation n Matched group of patients (no transplantation) demonstrated 30% 1 -year and 22% 2 -year survival rates Isolated intestinal grafts reportedly provide better patient and graft survival rates than multivisceral grafts Graft and patient survival rates are improving as centers gain experience (51 worldwide centers) n Main centers – l. yekehfallah-phd U of Pittsburgh, U of Nebraska, U of student of nursing education 2012 Miami, Hopital Necker-Enfants-Malades, & London 59
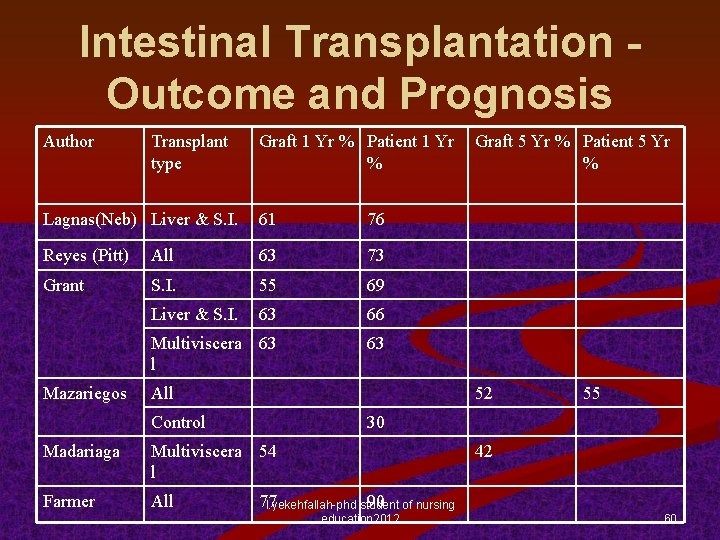
Intestinal Transplantation Outcome and Prognosis Author Transplant type Graft 1 Yr % Patient 1 Yr % Lagnas(Neb) Liver & S. I. 61 76 Reyes (Pitt) All 63 73 Grant S. I. 55 69 Liver & S. I. 63 66 Multiviscera 63 l 63 Mazariegos All Graft 5 Yr % Patient 5 Yr % 52 Control 55 30 Madariaga Multiviscera 54 l Farmer All 42 77 90 of nursing l. yekehfallah-phd student education 2012 60

Intestinal Transplantation Outcome and Prognosis n Small-intestine transplantation has higher incidences of rejection, sepsis, and posttransplantation lymphoproliferative disease than other organ transplantations n n These outcomes may be secondary to bacterial translocation Overall, 78% of intestinal transplant patients can be expected to be free of TPN and to tolerate oral nutrition following surgery l. yekehfallah-phd student of nursing education 2012 61

Intestinal Transplantation – Outcome and Prognosis The introduction of tacrolimus immunosuppression, in combination with decontamination protocols, antibiotic regimens, and antiviral measures against CMV and EBV, has improved patient and graft survival rates n Survival rates at 1 year as high as 90% have been achieved for patients receiving isolated intestinal grafts n n 3 year survival > 70% l. yekehfallah-phd student of nursing education 2012 62

Intestinal Transplantation n Patient survival & graft survival rates have improved with The introduction of tacrolimus (FK 506)–based immunosuppression (calcineurin inhibitor) n Used in combination with n n Decontamination protocols n Antibiotic regimens n Antiviral measures against cytomegalovirus (CMV) and Epstein-Barr virus (EBV). Pre-tacrolimus – pt survival 0 -28% and graft survival 0 -11% n With tacrolimus – pt & graft survival exceed l. yekehfallah-phd student of nursing education 2012 50% n 63

? l. yekehfallah-phd student of nursing education 2012 64
- Slides: 64