SMALL BOWEL OBSTRUCTION SBO SOME BASIC OVERTURES Authors

SMALL BOWEL OBSTRUCTION (SBO) – SOME BASIC OVERTURES Author(s): Shiva Sarraf-Yazdi, MD Level: Basic Academic Affiliation: Assistant Professor, Duke-NUS Graduate Medical School Version No: 1. 0 Submitted: March 2012 Editors’ Review:

2 Learning Objectives To review adult small bowel obstruction (SBO): • common (mechanical) etiologies; • pathophysiology; • clinical presentation; • diagnostic tools; • nonoperative management principles; & • warning signs
SBO Overview • Most common disorder afflicting the small bowel • "Categories" - Non-mechanical/functional (e. g. pseudoobstruction, ileus) - Mechanical (e. g. adhesive band, tumor) - Partial vs. complete - Simple vs. closed loop - From extraluminal or intraluminal causes - Gangrenous vs. non-gangrenous • What’s the worry? closed loop obstruction - Delayed or missed diagnosis can evolve into strangulation, increasing both morbidity & mortality

4 Etiology of SBO • Age dependent • In adults, most common causes are: - 1) adhesions, and 2) hernias (groin) - Without hernias or prior operations, cancer accounts for half of cases; otherwise, it comprises 5– 10% of cases • Pattern has changed over past few decades: - Hernias used to be more frequent cause than adhesions - In Western world, inflammatory bowel disease now a leading cause
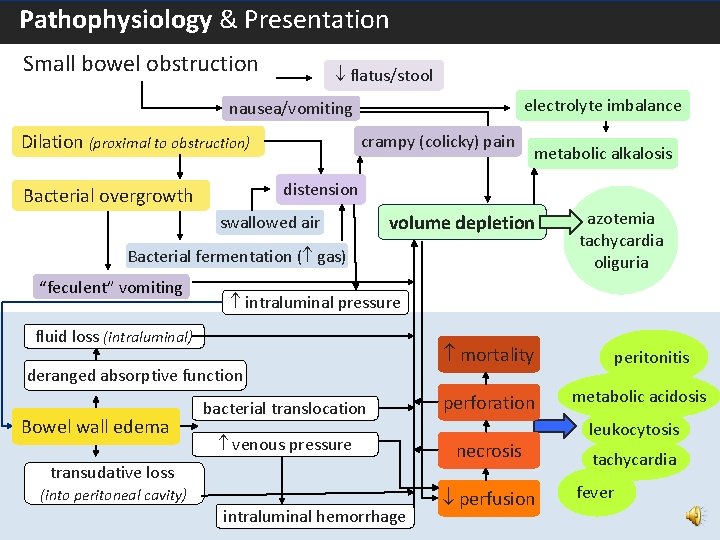
Pathophysiology & Presentation – Proximal Bowel Obstruction Small bowel obstruction flatus/stool electrolyte imbalance nausea/vomiting Dilation (proximal to obstruction) crampy (colicky) pain metabolic alkalosis distension Bacterial overgrowth swallowed air volume depletion Bacterial fermentation ( gas) “feculent” vomiting azotemia tachycardia oliguria intraluminal pressure fluid loss (intraluminal) deranged absorptive function Bowel wall edema 5 mortality bacterial translocation perforation venous pressure necrosis transudative loss (into peritoneal cavity) intraluminal hemorrhage perfusion peritonitis metabolic acidosis leukocytosis tachycardia fever
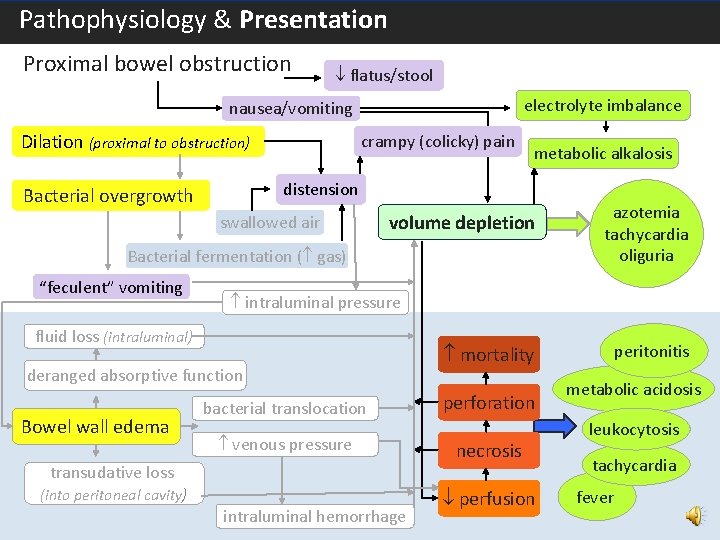
Pathophysiology & Presentation – Proximal Bowel Obstruction Proximal bowel obstruction flatus/stool electrolyte imbalance nausea/vomiting Dilation (proximal to obstruction) crampy (colicky) pain metabolic alkalosis distension Bacterial overgrowth swallowed air volume depletion Bacterial fermentation ( gas) “feculent” vomiting azotemia tachycardia oliguria intraluminal pressure fluid loss (intraluminal) deranged absorptive function Bowel wall edema 6 mortality bacterial translocation perforation venous pressure necrosis transudative loss (into peritoneal cavity) intraluminal hemorrhage perfusion peritonitis metabolic acidosis leukocytosis tachycardia fever
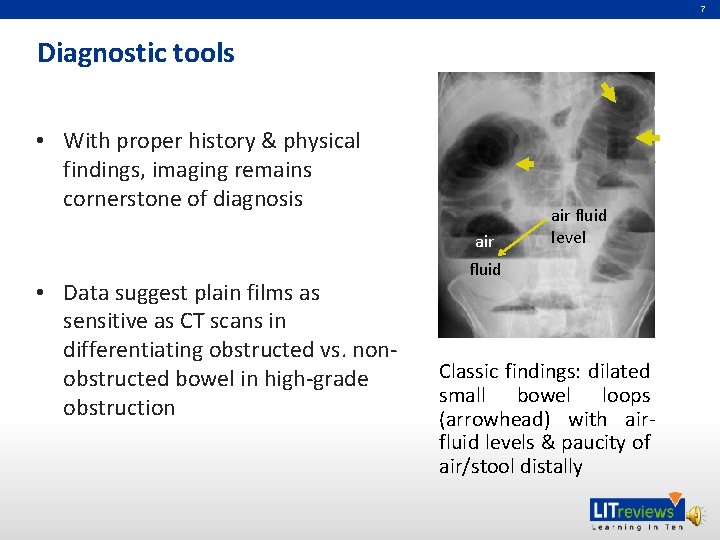
7 Diagnostic tools (SBO) • With proper history & physical findings, imaging remains cornerstone of diagnosis • Data suggest plain films as sensitive as CT scans in differentiating obstructed vs. nonobstructed bowel in high-grade obstruction air fluid level fluid Classic findings: dilated small bowel loops (arrowhead) with airfluid levels & paucity of air/stool distally

8 Diagnostic tools (SBO) • If plain films inconclusive, CT scan may delineate degree and etiology of obstruction • CT sensitivity depends on obstruction, rising with higher grades of obstruction • Multiple signs on CT may suggest strangulation: e. g. ongoing proximal bowel dilation, presence of transition zone, intraluminal fluid, colonic contents, reduced wall enhancement, feces sign, mesenteric attenuation Collapsed distal small bowel loops air fluid level dilated SB loop (proximal to obstruction) & ‘feces’ sign

9 Principles of (nonoperative) management • • • Frequent clinical monitoring/exam Bowel rest (nothing by mouth) Bowel decompression (nasogastric tube) Monitoring and replacement of fluid losses Adjustment of electrolyte imbalances No routine indication for antibiotics
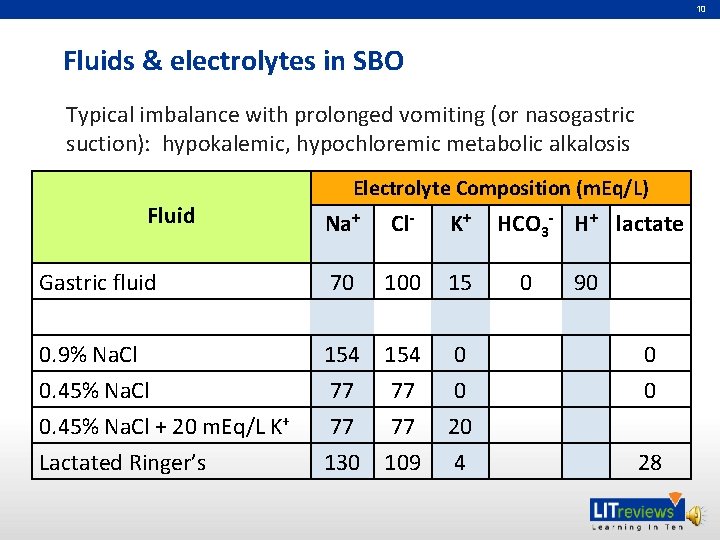
10 Fluids & electrolytes in SBO Typical imbalance with prolonged vomiting (or nasogastric suction): hypokalemic, hypochloremic metabolic alkalosis Fluid Electrolyte Composition (m. Eq/L) Na+ Cl- K+ Gastric fluid 70 100 15 0. 9% Na. Cl 0. 45% Na. Cl + 20 m. Eq/L K+ Lactated Ringer’s 154 77 77 130 109 0 0 20 4 HCO 3 - H+ lactate 0 90 0 0 28

11 Nonoperative management: until when? • No prospective, randomized studies on operative timing for SBO • Assuming neither peritonitis nor clinical deterioration, nonoperative management generally safe • Successful in 65 to 90% of partially obstructed small bowel cases, with improvement seen in vast majority within 48 hours • In absence of clinical change, 48 hours roughly marked as time when management revisited
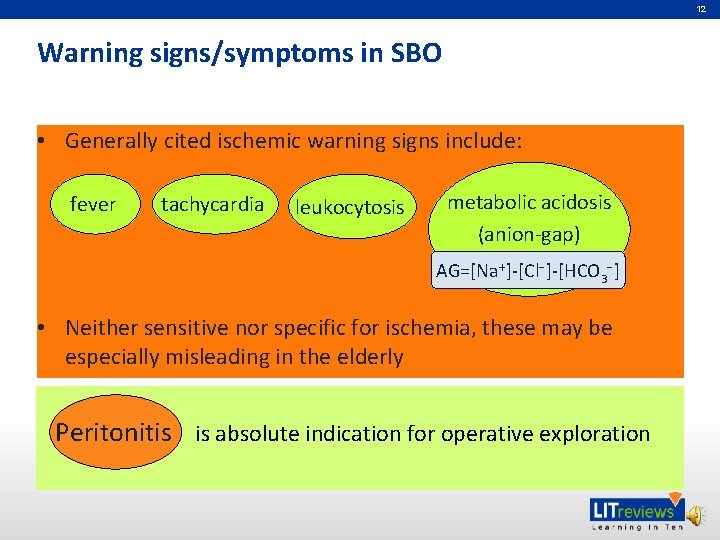
12 Warning signs/symptoms in SBO • Generally cited ischemic warning signs include: fever tachycardia leukocytosis metabolic acidosis (anion-gap) AG=[Na++]-[Cl−−]-[HCO 3−] − AG=[Na ]-[Cl ]-[HCO 3 ] • Neither sensitive nor specific for ischemia, these may be especially misleading in the elderly is absolute indication for operative exploration Peritonitis

13 Summary (SBO Basics) • Incidence of SBO same, but associated mortality declined • Despite imaging advances, ability to predict ischemic portions of bowel imperfect • Tenets of nonoperative management involve bowel rest and correction of fluid & electrolyte imbalances • No prospective, randomized studies on optimal operative timing • Imperative to pay heed to clinical indicators to avert delayed diagnosis of ischemia (increased morbidity & mortality) • Peritonitis remains absolute indication for surgical exploration

14 Key References 1. Cappell MS, Batke M: Mechanical obstruction of the small bowel and colon. Med Clin North Am 2008; 92: 575– 97. 2. Diaz JJ, Bokhari F, Mowery NT et al: Guidelines for management of small bowel obstruction. J Trauma 2008; 64: 1651– 64. 3. Fevang BT, Fevang J, Stangeland L et al: Complications and death after surgical treatment of small bowel obstruction: A 35 -year institutional experience. Ann Surg 2000; 231: 529– 37. 4. Rocha FG, Theman TA, Matros E et al: Nonoperative management of patients with a diagnosis of high-grade small bowel obstruction by computed tomography. Arch Surg 2009; 144: 1000– 4.

15 Disclaimer/Liability • The information provided in the VAP is made available in good faith and is derived from sources believed to be reliable and accurate at the time of release. • The materials presented on the VAP may include links to external Internet sites. These external information sources are outside the control of Duke-NUS. The user of the Internet links is responsible for making his or her own decision about the accuracy, reliability and correctness of the information found. • In no event shall Duke-NUS be liable for any indirect, special, incidental, or consequential damages arising out of any use of reliance of any information contained in the VAP. Nor does Duke-NUS assume any responsibility for failure or delay in updating or removing the information contained in the VAP. • Moreover, information provided on the VAP does not constitute medical advice or treatment nor should it be considered as a replacement of the patient/physician relationship or a physician’s professional judgment. Duke-NUS expressly disclaims all liability for treatment, diagnosis, decisions and actions taken or not taken in reliance upon information contained in the VAP. This work is licensed under a Creative Commons Attribution-Non. Commercial-No. Derivs 3. 0 Unported License To view a copy of this license, visit [http: //creativecommons. org/licenses/by-nc-nd/3. 0/]

16 Financial Disclosures (past 3 years) No Disclosures.

Partners in Academic Medicine
- Slides: 17