Small Bowel Obstruction Medical Nutrition Therapy Case Study

Small Bowel Obstruction. Medical Nutrition Therapy Case Study Samira Jones, Ph. D, MPH Baptist Health Systems Dietetic Internship

Presentation Outline �Introduction- Anatomy & Phys of Intestine �Background- SBO �Hospital Admission- “R. L. ” Patient Profile �Nutrition Care Process- Pt. LOS in Hospital �Summary/Conclusions
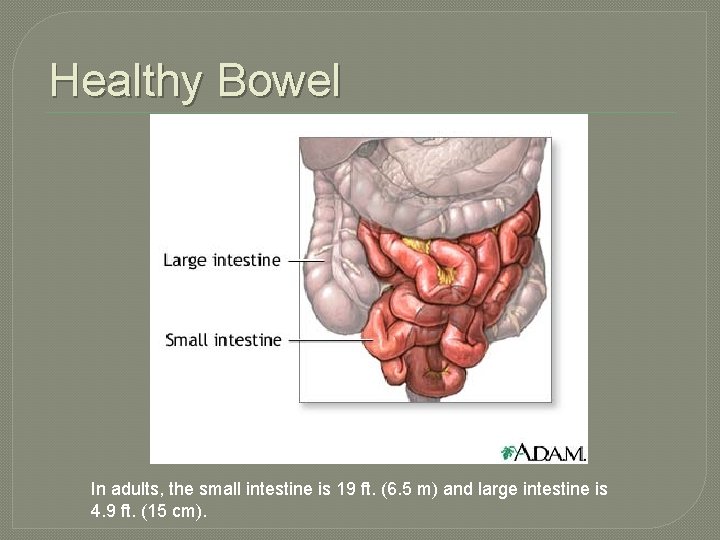
Healthy Bowel In adults, the small intestine is 19 ft. (6. 5 m) and large intestine is 4. 9 ft. (15 cm).
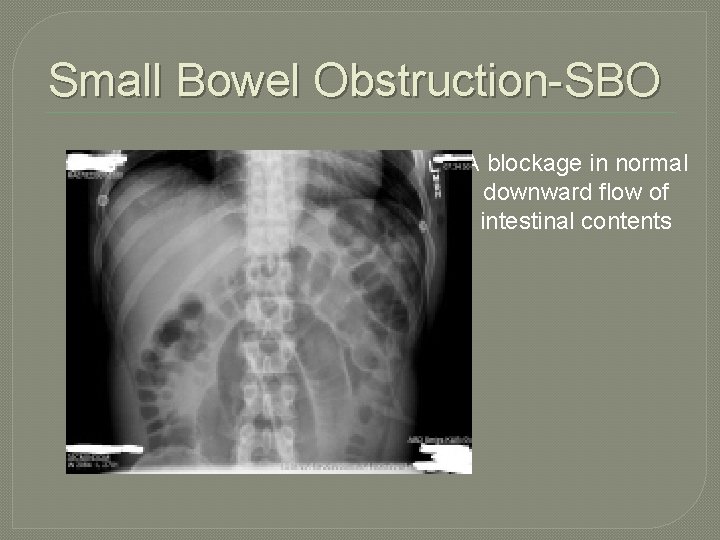
Small Bowel Obstruction-SBO A blockage in normal downward flow of intestinal contents

Background-SBO Etiology Ø Mechanical Obstruction - Crohn’s Disease 7% *Luminal *Extramural Misc. 11% Adhesions Hernia 74% 2% Neoplasia 5%

Background- SBO � Epidemiology- Adhesiolysis accounts for 300, 000 hospitalizations; 800, 000 days of inpatient hospital care, and $1. 3 billion in healthcare costs (2006). � Etiology- 75% are caused by post-operative adhesions and hernia from prior GI surgery. � Pathophysiology- SBO may occur in as many as 15% of laparotomy pts. up to 2 yrs s/p procedure. • Pts. Have high risk for re-current obstruction of 42% over 10 yrs. More than ½ SBO pts. require surgery with a 5% mortality rate d/t complications.

Background-SBO cont’d �Clinical Diagnosis • Ultrasonography • Intraluminal contrast studies • CT scan �Once SBO is confirmed… • Laparotomy is performed to differentiate between simple and complicated obstruction, severity, and location.
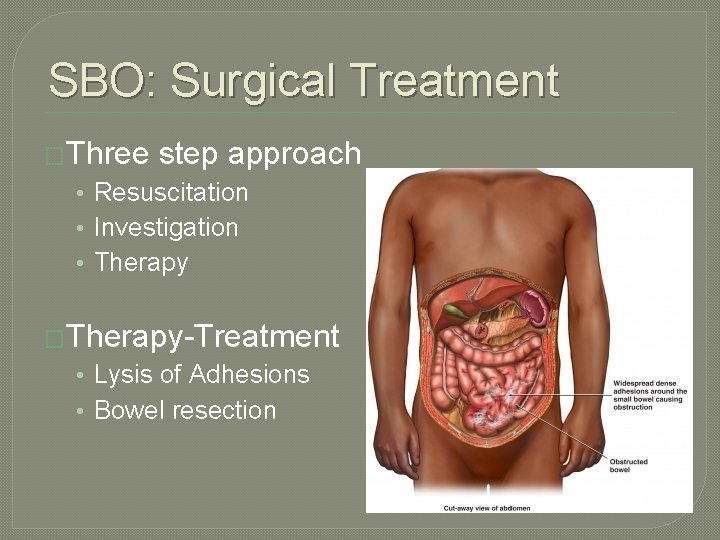
SBO: Surgical Treatment �Three step approach • Resuscitation • Investigation • Therapy �Therapy-Treatment • Lysis of Adhesions • Bowel resection

SBO: Medications �Motility Agents • Octreotide • Metoclopramide �Stool softeners, laxatives �Multiple Pain Medications

SBO: Macro & Micronutrients � Carbohydrates-CHO • Simple CHO rather than complex CHO � Protein • Severe malnutrition is rare � Fats & Fat Soluble Vitamins • Higher risk of malabsorption � B-12 • High risk of malabsorption

SBO: Fluids and Electrolytes �Fluids • Challenging to manage with ostomies �Electrolytes • Alleviate Na/K+ imbalances

SBO: Medical Nutrition Therapy �NPO-TPN • Bowel rest �PO • Clear Liquid • Regular Liquid • Small frequent meals & low fiber *Individualized

SBO: MNT �ADA Nutrition Care Manual Recommendations • Calories: 25 -30 kcal/kg IBW • Protein: 1 -1. 2 or 1. 2 -1. 4 g/kg IBW • Fluids: 30 ml/kg or Per MD
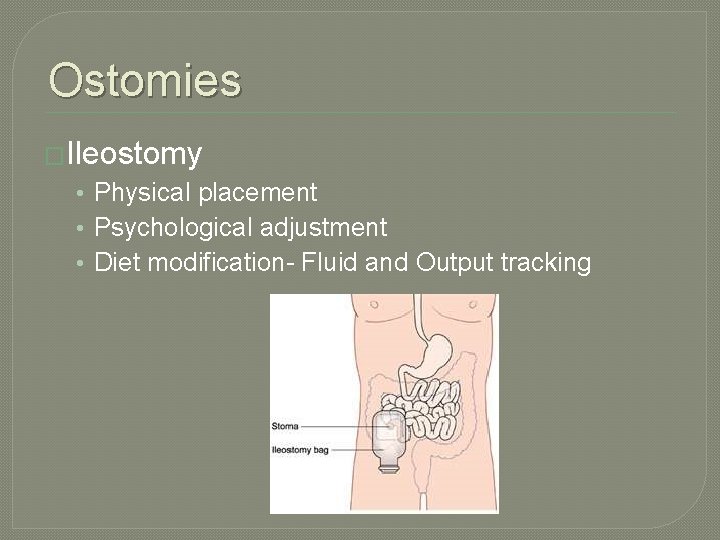
Ostomies �Ileostomy • Physical placement • Psychological adjustment • Diet modification- Fluid and Output tracking

Patient Profile �R. L. 22 y. o. , AA male; Adopted by foster parents at age 2 yrs • Non-ambulatory: Uses wheelchair �Med Hx: Cerebral palsy, Paraplegiamultiple BLE osteotomies for severe contractures, Hiatal hernia-Nissen fundoplication s/p 10 yrs, VP shunt s/p 20 yrs • Prior UCDMC admissions- 3 since 2004

Current UCDMC Admission- R. L. �Admit date: 5/2/11 • Diagnosis: SBO with large hiatal hernia & stomach in thoracic cavity (CT scan) • Signs/Symptoms: PTA �Pt. screened in from nursing for nausea & vomiting for > 3 days �Complained of left/right abdominal pain for several days �Poor intake and appetite > 5 days

Nutrition Care Process �Nutrition • • • Assessment Diet order Anthropometrics Labs Diet history Estimated needs �Nutrition Diagnosis �Nutrition Intervention- PES statement �Nutrition Monitoring/Evaluation

MNT 1. � Initial Nut Assessment 5/5/11 - RD Intern • Anthropometrics �Wt. = 71. 7 kg (standing scale); Ht= 5’ 6”=167. 6 cm �IBW= 64. 5 kg; %IBW= 111 • Estimated Nutrition needs � 1612 -1935 kcal/day (25 -30 kcal/kg IBW) � 64 -97 g protein/day (1. 0 -1. 5 g/kg IBW) � Physical � Labs: appearance: Abdominal distension Na 131 L, Glu 115 H, BUN 2 L, ALT 68 H � Eating hx: Per parents, “pt. had good appetite and ate typical American diet PTA. He likes spaghetti, burgers & fries, ice cream, and ‘junk’ food. ”
MNT 1. cont’d � Diet Order: NPO for GI surgery; TPN- AA 100 g, Dex 150 g, lipids 20% 250 ml= 1410 kcal @ 58. 75 ml/hr � PES: Inadequate oral intake r/t altered GI function d/t small bowel obstruction, as evidenced by nausea/vomiting 3 days PTA and current NPO x 5 days. NI-2. 1 � Risk: High � Monitoring & Eval: Pt. will begin at 1400 kcal and advance to goal of 1600 kcal/ml/day as medically appropriate to meet estimated needs.

MNT 2. � Follow-up assessment: RD Intern 5/10/11 � Diet order: NPO-TPN 1602 kcal @ 66 ml/hr providing 280 g Dex, 100 g Amino acids, and 28 g Lipid � Labs: Na 131 L, Glu 111 H, BUN 7 L � PES: Increased nutrient needs r/t altered GI function as evidenced by pt. currently on TPN because of NPO > 8 days. NI- 5. 1 � Risk: High � Monitoring & Eval: Pt. will meet 1000% of estimated needs at goal TPN rate to preserve LBM while unable to meet PO nutrition.

Surgery 1. � 9 days post hospital admission: 5/11/11 • Laparospopic Lysis of adhesions • Hiatal hernia repair �Checked Fundoplication- Functional • Bowel Exploration- MD discovered 50 cm of dead ileum*
MNT 3. GI surgery (s/p 5 days) � Follow-up assessment- RD 5/16/11 � Diet order: NPO-TPN (100 g AA, 280 g Dex, 250 ml 20% lipids)= 1852 kcal @ 66. 6 ml/hr (up from 58. 4 ml/hr from last assessment) � Labs: � PES: Glu 162 H Altered GI fxn r/t to GI surgery as evidenced by KUB findings of severe postoperative ileus. NC-1. 4

Surgeries 2 & 3. � 7 days s/p GI surgery (2) • Externalization of VP Shunt � 9 days s/p GI surgery (3) • Laparotomy • Abdominal washout • End Ileostomy- lower left quadrant

MNT 3. S/p 3 days w/ Ileostomy � Diet order: NPO-TPN = 100 g of AA, 280 g Dex and 250 ml of 20% lipids daily = 1852 kcal/d � Labs: Glu, TG, Na, K all WNL; Phosphorus slightly elevated but pharmacy aware and was addressing it. � RD recommendations: • Once GI status permits, Osmolite 1. 0 @ 10 ml/hr advancing 10 -20 ml/hr every 6 -8 hrs. as tolerated. Goal= 70 ml/hr, provides 1780 kcals, 75 g protein, 1411 ml free water; flushes and fluids per MD. • Taper PN with goal to discontinue as EN increases. • Modified diet- Low fiber diet once medical status permits.

MNT 4. S/p 7 days Ileostomy � Diet order: NPO-TPN= 100 g of AA, 280 g Dex and 250 ml of 20% lipids daily, provides 1602 kcals � Labs: Glu 142 H � Osteomy output= 710 ml � RD recommendations: • Advancement to low fiber diet once GI status permits. • Continue PN, but taper with goal to D/C as PO intake improves. • Monitor total energy intake over next 5 days for goal of 1600 kcals, 77 g protein

MNT 5. S/p 13 days Ileostomy �Pt. NG tube removed �Diet order: PO diet- Regular, low residue over 24/48 hrs, and PN at same level �Output= 1150 ml; 970 ml (1 day prior) �RD recommendations: • Pt. tolerated 100% CL diet and 1 meal of regular diet w/ no complaints of nausea/vomiting, so PN recommended to d/c with continual advancement to PO at adequate level to meet needs.

Surgery 4. �Conversion of ventriculoperitoneal (VP) shunt to ventricular atrial (VA) shunt d/t pt. experiencing hydrocephalus

MNT 7. S/p 20 days Ileostomy � Diet order: PO- Modified puree diet � Meds: Imodium, Gas-X, Metamucil � Pt. parents requested puree diet b/c they believe pt. would tolerate it better d/t smoother texture (pt. with poor dentition) and not completely eating whole foods. � Output= 550 ml � RD recommendations: • Provide Ensure plus TID and supplemental EN if inadequate nutrition remains b/c pt. meeting ~65%68% of estimated kcal & protein needs from current PO intake over last 5 days.

MNT 8. S/p 24 days Ileostomy � Diet order: 75 -90 g CHO controlled diet � Pt. parents provided with Ostomy nutrition education handout. Parents advised of foods to avoid like simple CHO and to consume small, freq meals, and importance of electrolyte balance and adequate hydration while pt. has ileostomy. � Output= � Pt. 1350 ml weight status unable to be assessed d/t shifts in fluid status.

MNT 9. S/p 29 days Ileostomy � Diet order: Low fiber, Pediasure TID, snacks (bananas, white bread PB&J sandwich, tea-BRAT diet) TID � Wt. 147 # =66. 5 kg � Output= 1400 ml � Meds: Protonix, Metamucil, X � RD Lomotil, Imodium, Gas- rec’d: Pt. will meet at least 70% of est. needs with current diet. D/C metamucil b/c of its effects on high ostomy output. Provide MV supplement and monitor fluids. Ostomy output should estimate < 1 L per 24 hrs.

Summary & Conclusions �Malnutrition is common in patients with partial or complete SBO. �In complicated SBO cases, the patient may end up with an ostomy if part of the bowel is removed or resected. �MNT for SBO has to be individualized based on the location, type, and severity of obstruction (partial, complete).

Summary & Conclusions �Several factors must be considered before diet advancement is made to ensure optimal nutrition for the patient. �Even when a team is assertive with delivery of nutrition, the role of the RD is still crucial to monitor the adequacy of the intake and appropriateness of the order.

References � Foster NM, Mc. Gory ML, Zingmond DS and Ko CY. Small Bowel Obstruction: A population-based appraisal. Journal of American College of Surgeons, 2006; 203: 170 -176. � Agresta F, Piazza A, Michelet I, Bedin N, and Sartori A. Small bowel obstruction- Laparascopic Approach. Surgical Endoscopy, 2000; 14: 154156. � Miller G, Boman J, Shrier I, and Gordon PH. Etiology of Small Bowel Obstruction. American Journal of Surgery, 2000; 180: 33 -36. � Kulaylat MN and Doerr RJ. Small Bowel Obstruction Surgical Treatment: Evidence- based and Problem-oriented. National Library of Medicine, National Institutes of Health, 2001: Washington, D. C. � Ihedioha U, Alani A, Modak P, Chong P, and O'Dwyer PJ. Hernias are the most common cause of strangulation in patients presenting with small bowel obstruction. Hernia, 2006; 10: 338 -340. � Mahan LK and Escott-Stump S. Krause's Food & Nutrition Therapy, 12 th Edition. 2008; copyright Saunders Elsevier, St. Louis, Missouri.

Thank You!
- Slides: 34