Skeletal Muscles Anatomy and innervation of skeletal muscle
























- Slides: 43

Skeletal Muscles

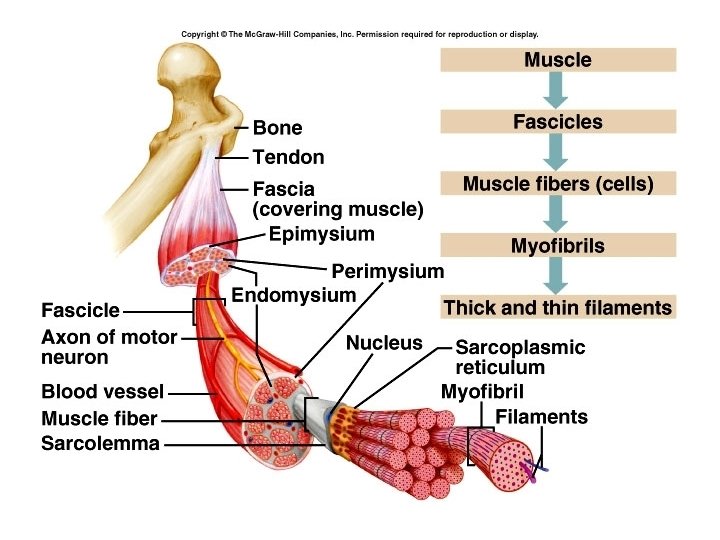
Anatomy and innervation of skeletal muscle tissue • Connective tissue components: – Fascia (“bandage”) –sheet or band of fibrous C. T. under the skin or around organs – Superficial fascia (subcutaneous fascia): • Areolar C. T. and adipose tissue • Stores water and fat • Reduces heat loss (insulates) • Protects against trauma • Framework for nerves and blood vessels

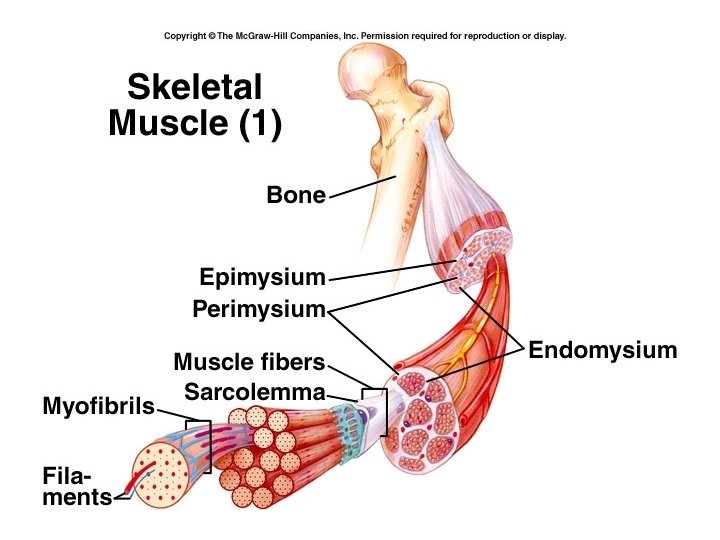
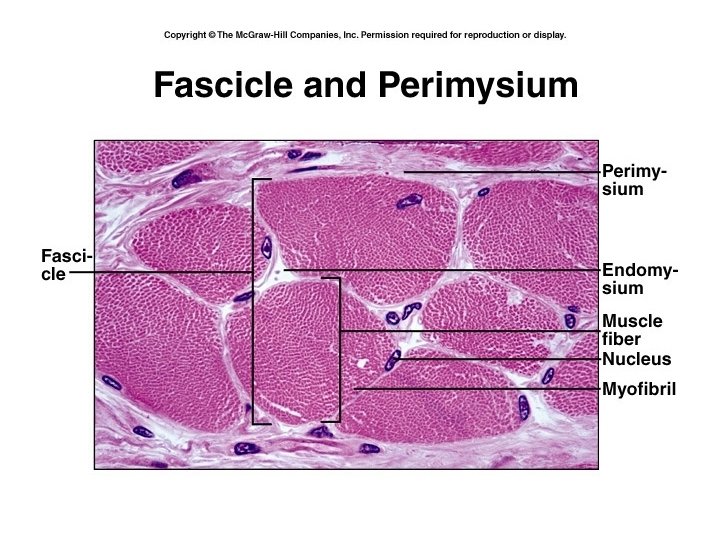
• Deep fascia: – Dense irregular C. T. – holds muscles together and separates them into groups – 3 layers: • Epimysium – surrounds the whole muscle • Perimysium – separates muscle into bundles of muscle fibers – fascicles • Endomysium – covers individual fibers



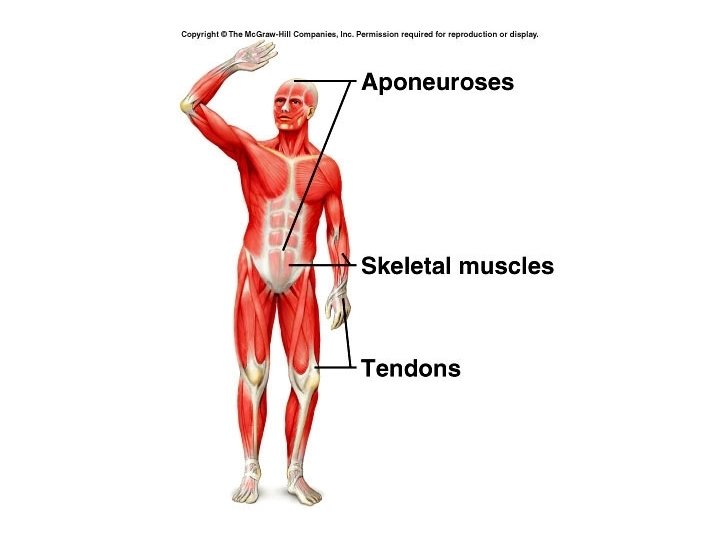
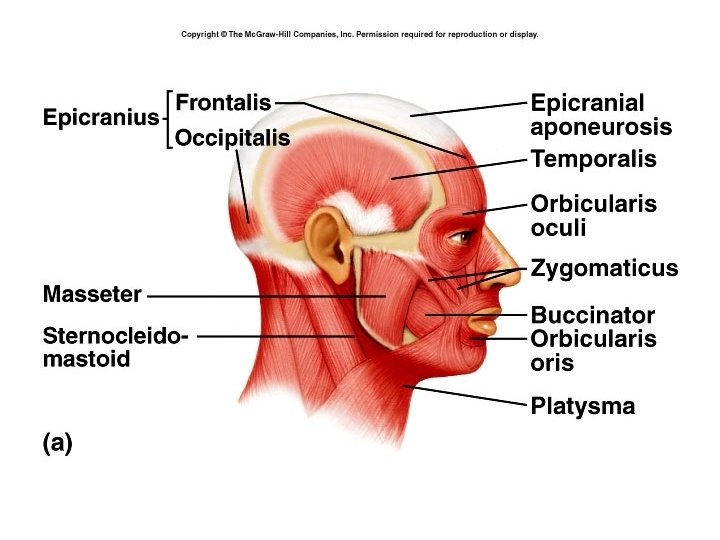
• These three layers come together to form cords of dense, regular connective tissue called tendons. Tendons attach muscle to the periosteum of bones. • When the connective tissues form a broad, flat layer, the tendon is called an aponeurosis.



Microscopic Anatomy • Muscle cells are called muscle fibers or myofibers • Plasma membrane – sarcolemma • Cytoplasm – sarcoplasm • Myoblasts fuse to form one myofiber – several nuclei • Myofibrils run lengthwise

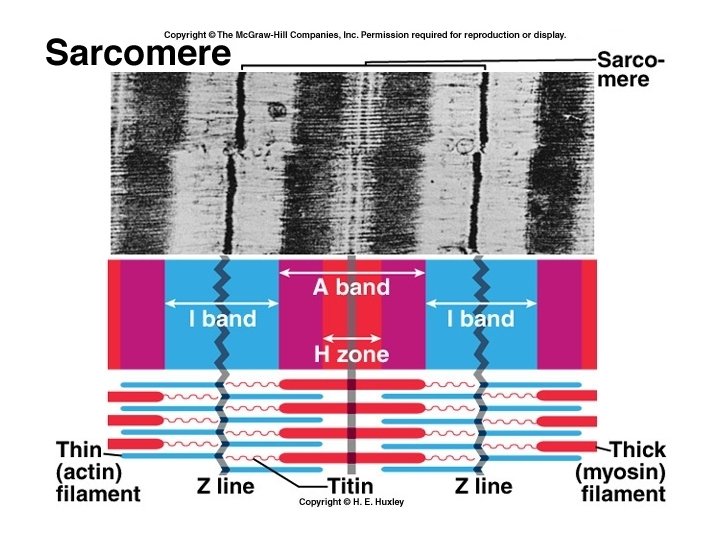
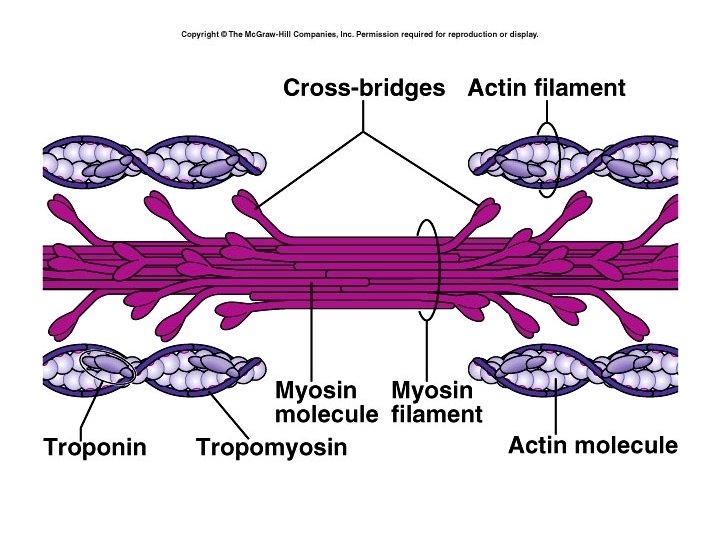
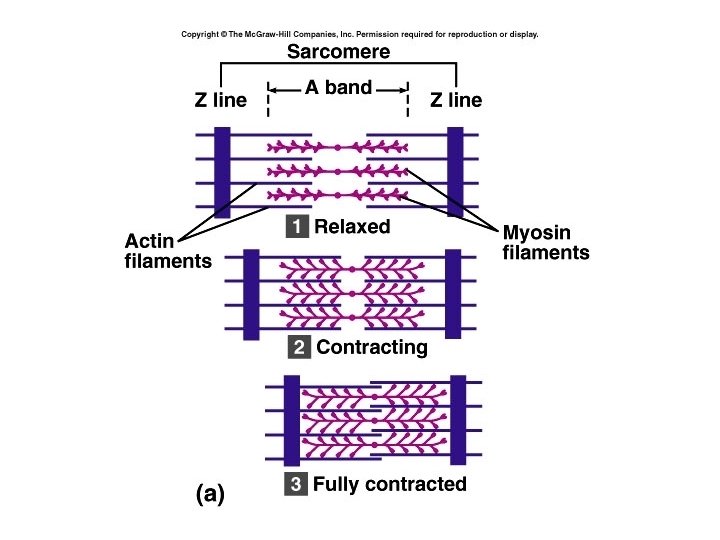
Myofibrils are made of filaments • Thin filaments – primarily actin • Thick filament – myosin • Elastic filaments • Sarcomeres are the basic, functional units of striated muscle fibers.



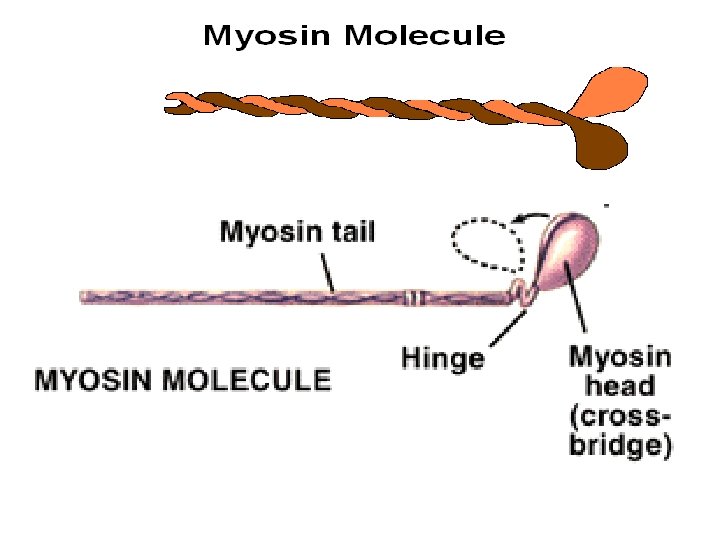
Thick filaments • Made of about 200 molecules of myosin • Each myosin molecule has two “heads” • Each head has an actin binding site and an ATP binding site • The ATP site splits ATP and transfers energy to myosin head; which remains charged (“cocked”) until contraction.



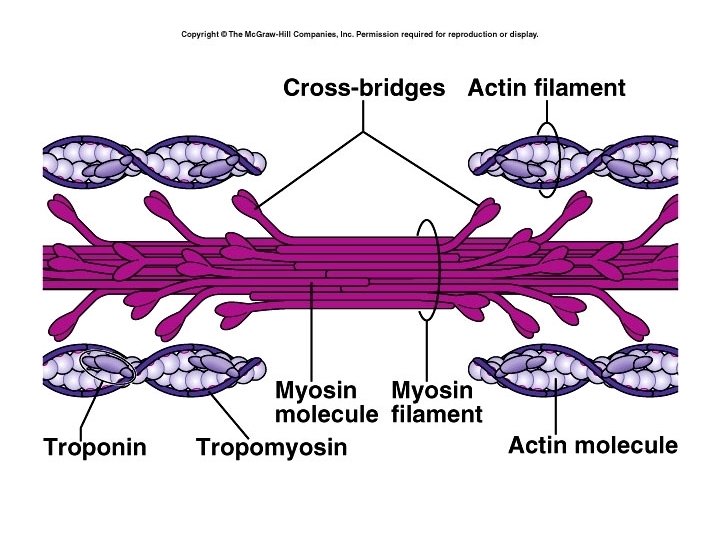
Thin Filaments • Actin molecules form a helix – Each actin molecule has a myosin binding site • Other proteins: • Tropomyosin – long, filamentous protein, it wraps around the actin and covers the myosin binding sites • Troponin – a smaller molecule bound to tropomyosin, it has calcium binding sites.


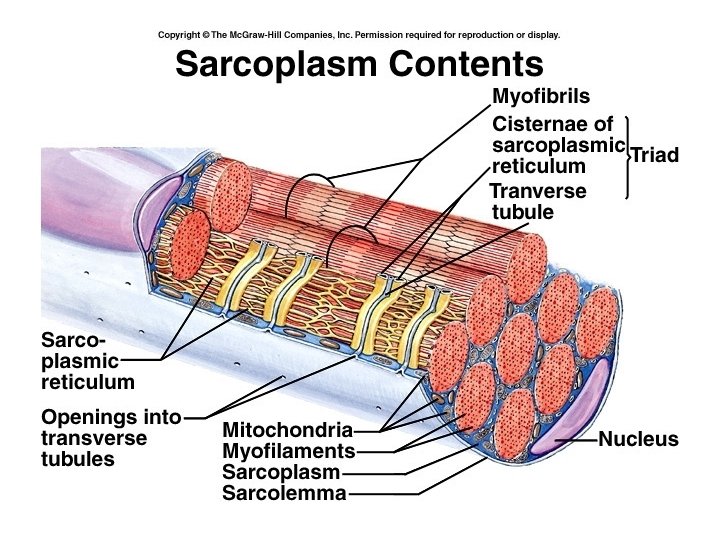
Sarcoplasmic reticulum • Specialized smooth E. R. • Tubes fuse to form cisternae • In a relaxed muscle, S. R. stores Ca++ (Ca++ active transport pumps) • When stimulated, Ca++ leaves through Ca++ release channels.

Transverse tubules (T-tubules) • Infoldings of sarcolemma that penetrate into muscle fiber at right angles to filaments. They are filled with extracellular fluid. • T-tubules and the cisternae on either side form a triad.


Blood and nerve supply • Muscle contraction uses a lot of ATP • To generate ATP, muscles need oxygen • Each muscle fiber is in close contact with one or more capillaries • Motor neurons – originate in brain and spinal cord; cause muscle contraction

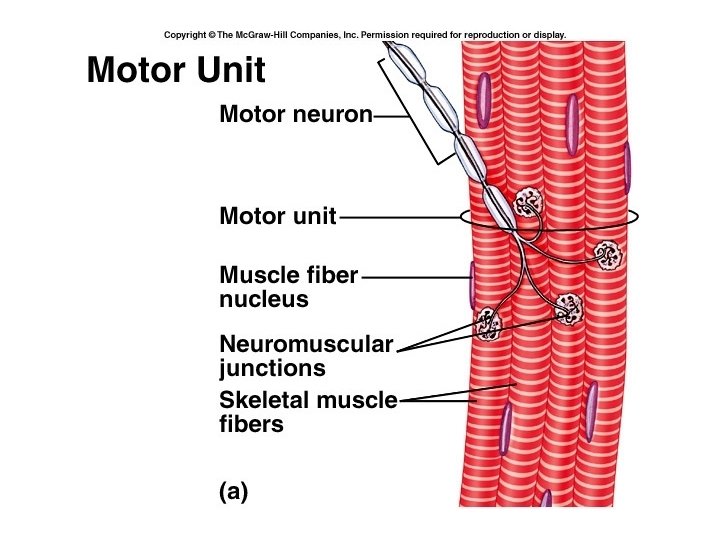
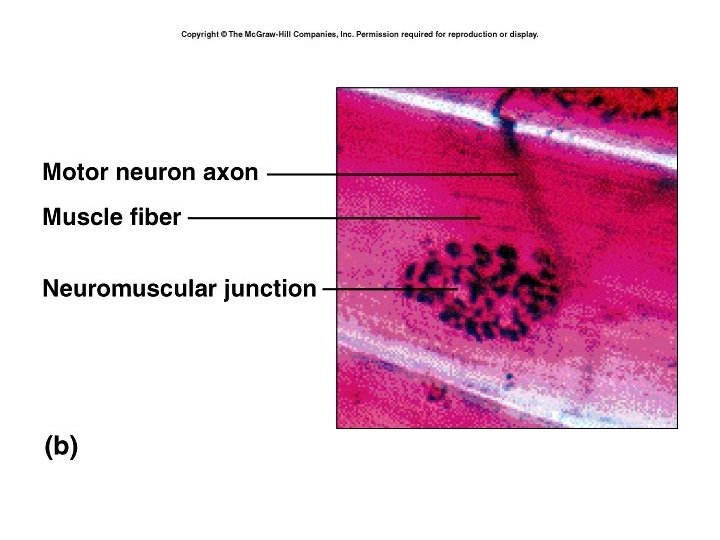
Motor unit • A Motor Unit is made of one motor neuron and all the muscle fibers it innervates. • These cells all contract together. • A single motor unit can have 2 – 2, 000 muscle fibers. • Precise movements are controlled by small motor units, and large movements by large motor units.


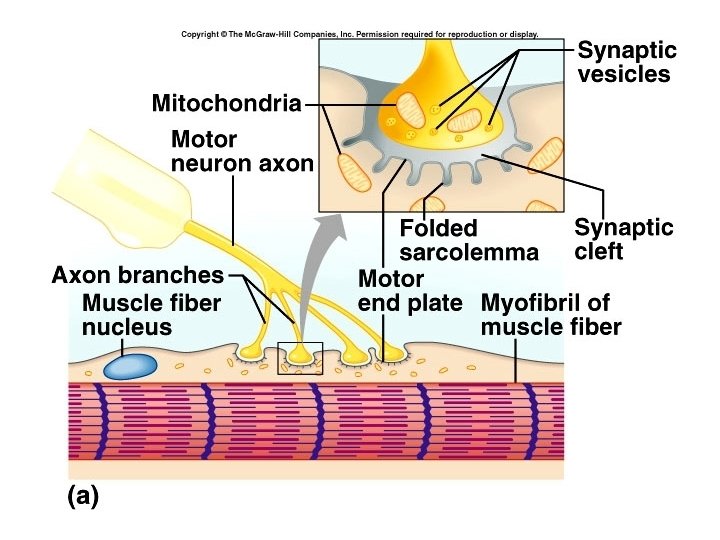
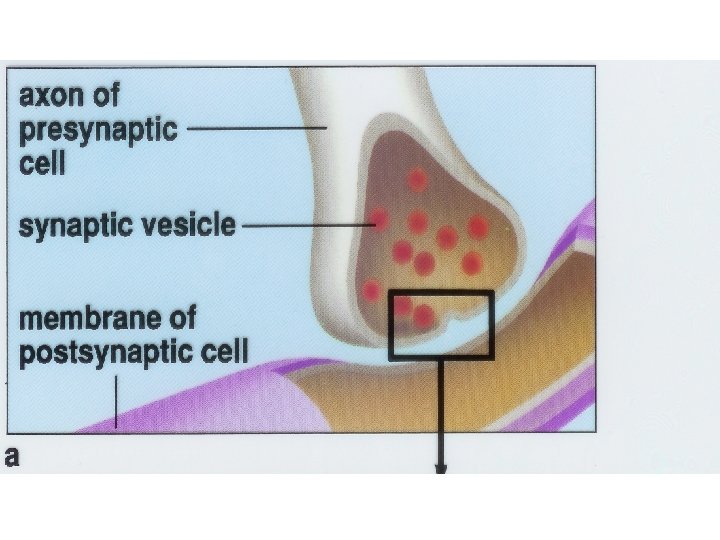
Neuromuscular Junction (NMJ) • Nerves communicate with muscles and other organs at structures called synapses. • Synaptic cleft – gap between neuron and sarcolemma • Axon releases a chemical called a neurotransmitter – Acetylcholine (Ach) • Axon branches into axon terminals. • At the end of each axon terminal is a swelling called the synaptic end bulb.



• The region across the synaptic cleft from the synaptic end bulb is called the motor end plate. • The sarcolemma of the motor end plate is folded and contains many receptors for ACh. • When a nerve impulse reaches the synaptic end bulbs, it causes synaptic vesicles to fuse with the membrane and release ACh by exocytosis.



• Acetylcholine diffuses across the synaptic cleft, and binds with receptors on the motor end plate. • This binding causes the receptor to change shape, and opens Na+ channels in the membrane. • When enough Na+ channels are opened, an electrical current is generated and is carried along the sarcolemma. This is called a muscle impulse or muscle action potential. This electrical activity can be recorded in an electromyogram.

Sliding Filament Mechanism • When a nerve impulse reaches an axon terminal, the synaptic vesicles release acetylcholine (ACh) • ACh crosses the synaptic cleft and binds with receptors on the motor end plate. • This binding opens channels that allow sodium to rush in, beginning a muscle action potential in the sarcolemma.

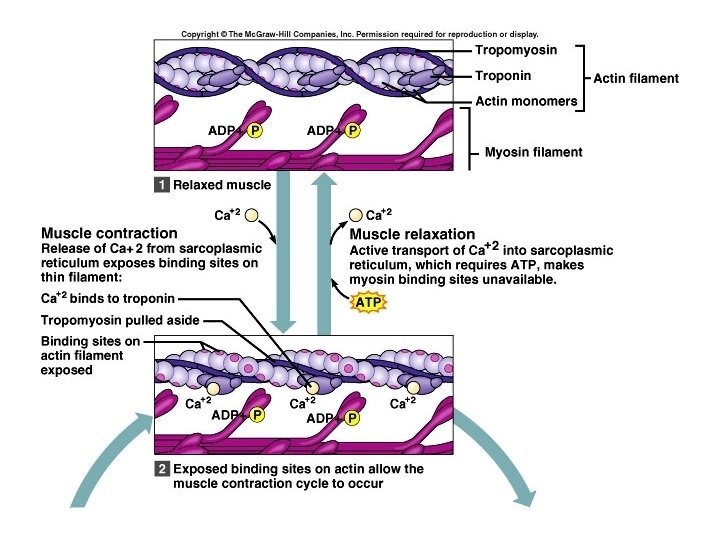
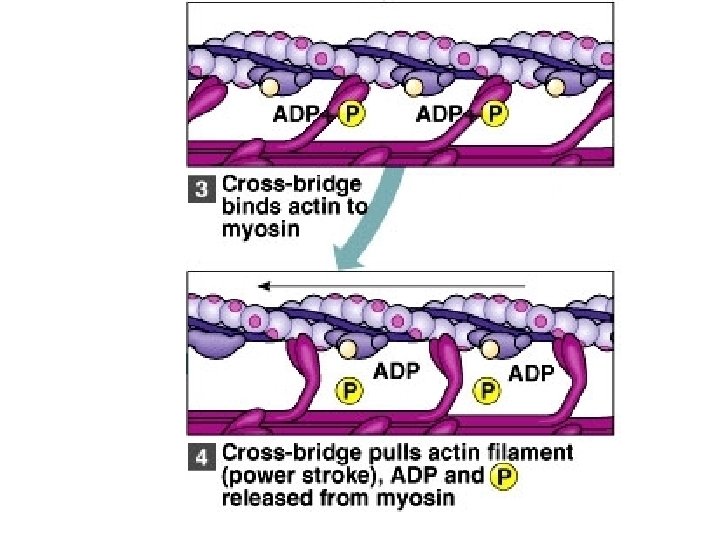
• The action potential or impulse travels down the sarcolemma and into the T-tubules, causing the sarcoplasmic reticulum to release Ca++ into the sarcoplasm. • The Ca++ binds to the troponin, which changes shape, pulling the tropomyosin away from the myosin binding sites on the actin. • The activated myosin attaches to the actin, forming actin/myosin crossbridges. • The myosin head moves toward the center of the sarcomere, pulling the actin filaments past the myosin. This is called a power stroke.

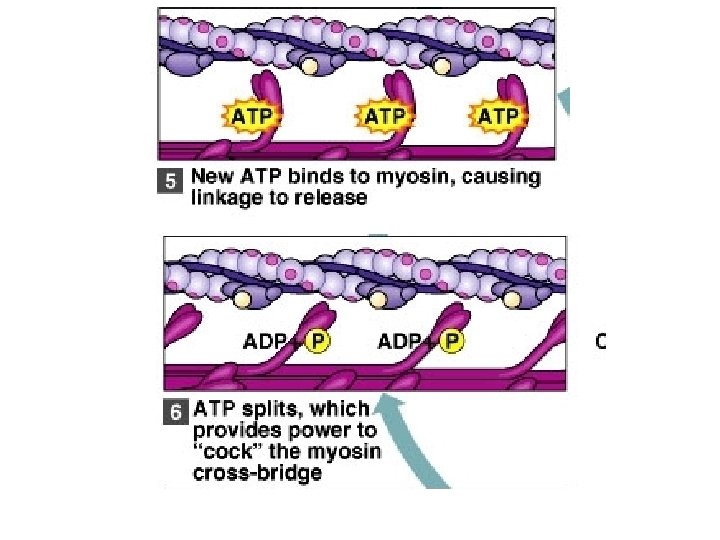
• When the myosin heads turn, they release ADP, and ATP binds to the heads. • When ATP binds, it causes the myosin to release the actin. • ATP is split, and the myosin heads again bind to the actin, but further down the filament. • The myosin again pulls the actin. • This action is repeated many times. • The Z lines (discs) get closer together as the actin and myosin filaments slide past each other, and the muscle fiber shortens.





Relaxation • ACh is broken down by an enzyme called acetylcholinesterase. • Action potentials are no longer generated, so the Ca++ release channels in the S. R. close. • Ca++ active transport pumps take Ca++ out of the sarcoplasm and into the S. R. where it binds to a protein called calsequestrin.

• As the Ca++ levels in the sarcoplasm fall, troponin releases tropomyosin, which falls back and covers the myosin binding sites on the actin. • The thin filaments slip back into their relaxed positions.

Rigor mortis • After death, muscle cells begin autolysis, and Ca++ leaks out of the S. R. • This causes muscles to begin to contract. • Since the body is dead, no more ATP is produced. • Without the ATP to recharge the myosin heads, they remain linked to the actin, and neither relax nor contract any further. • After about 24 - 72 hours it disappears as the tissues begin to disintegrate.

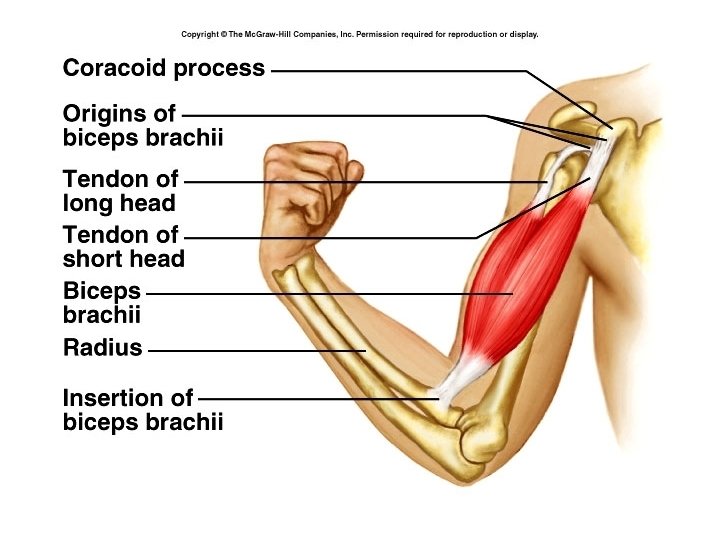
Origin and Insertions • Origin – the attachment of a muscle to the less movable part (torso, etc. ) • Insertion – the attachment of a muscle to the more movable part


Interactions of muscles • Prime mover – the muscle primarily responsible for a movement • Synergist – stabilizes or assists prime mover • Antagonist – opposes action of prime mover and must relax for prime mover to contract completely