Sinazongwe District 2019 medicshealthlog Justin K Ngandwe Objectives

Sinazongwe District. © 2019 medicshealthlog® Justin K. Ng’andwe.

Objectives. At the end of the presentation the Audience will be able to: i. Define STI’s ii. Understand Identify STI syndromes and Management (2017 STI Guidelines for Zambia) iii. Understand what to look for and ask during History taking on Clients with sings and symptoms presumptive of an STI

• Sexually transmitted infections (formally known as STDs) are infections that are ‘Commonly’ spread by sexual activities, especially Vaginal intercourse, anal sex and Oral sex. • They are Many types of STI • In Zambia it’s one of the most common cause of all out patient department (OPD) attendance. • They are among the most common causes of illness in the world and have far-reaching health, social and economic consequences for many countries. In addition, socio-economic determinants such as unemployment, poverty, polygamous relationships seem to play an important role in the spread of STIs. • It has continued to be one of the major causes of morbidity and remain the major contributor to new HIV infections in Zambia in the reproductive age group 14 -49 year old.

FACTS ABOUT STIs; § Rank among the top 5 disease categories for which adults seek health care § >1 million people acquires an STI every day § 500 million people become ill with one of the 4 STIs (Chlamydia, Gonorrhea, Syphilis and Trichomoniasis. § >290 Million women have HPV § HPV infections causes about 530 000 cases of CC and 275 000 CC deaths are recorded every year. § Majority of STI are asymptomatic § STI can present in any of the opening, genital, Anal or oral § STIs increase the risk of HIV transmission § STI can be transmitted from mother-to-Child § Are major causes of PID, adverse pregnant out come and infertility in women

• RELATIONSHIP WITH HIV: • They are all STIs • Similar risky behaviors are involved • Prevention and treatment of STIs reduces the number of new HIV infection • STIs increases the risk of both acquiring and transmitting HIV • In people with HIV, having an STI increases VL in blood and genital secretions

SIX KEY ELEMENTS IN A TYPICAL HEALTH CONSULTATION 1. Hx taking 2. Physical examination and specimen collection (where possible) 3. Early Diagnosis and treatmen 4. STI prevention counseling 5. Prevention Methods 6. - Sexual partners, Confidentiality and reporting (HMIS) Patient referral Provider referral Conditional referral
CONDITION THAT MASK THE DEFINATE DIAGNOSIS FOR STIs • • • • UTI GASTLITIS MUMPS ENT MSD ATHRITIS Non-blood Diarrhea dermatitis Urticaria/hives Conjunctivitis PUO Clinical Malaria Anemia Genitalia Elephantiasis Other STIs

Approaches in the management of STIs There are three traditional approaches utilized in the diagnosis and treatment of STIs. The following are three main approaches of diagnosis and treatment of STIs: 1. The etiologic approach This approach requires the use of laboratory tests to identify the causative agent. It is the ideal approach in clinical medicine. It allows evidence-based diagnosis and management of STIs. 2. The clinical approach This approach involves the use of clinical experience to identify symptoms typical for a specific STI, then treatment is targeted to the suspected pathogen. 3. The syndromic approach The syndromic management approach is based on the identification of consistent groups of symptoms and easily recognized signs, and provision of treatment that covers the majority of organisms responsible for producing that syndrome. Flowcharts have been developed to guide health workers in the implementation of syndromic management of STIs. It is especially useful at primary health-care level where resources are limited. It allows treatment of the patient at the first visit and enables treatment of mixed infections. However, it fails to identify asymptomatic infectio
- The Sydronic approach is adopted by the Ministry of health in Zambia for management of STI in public health institutions. - There 8 common syndromes identified, namely 1. Urethral Discharge 2. Vaginal discharge 3. Genital Ulcer 4. Genital Growth 5. Lower Abdominal pain 6. Inguinal bubo 7. Scrotal swelling 8. Neonatal Conjuctivitis
URETHRAL DISCHARGE: Common Causes. 1. Gonococcal Urethriti (Gra – Intracellular diplococcus, neisseria gonorrhea). CF. - icubation period 3 -7 days - Dysuria/difficulty in micturition - Urethral discharge of copious mucoid/pussy fluid The examination of the discharge shows a purulent, yellowish-green discharg with a red swollen meatus sometimes 1. Non-Conococcal Urethrytis( other causes apart from N. Gonorrhea, eg, Chlamydia trachomatis, among other 20 comong causes). CF. – Symptoms usually occur 7 -28 days after intercourse - with mild dysuria and disconfort - clear-purulent mucoid discharge (more marked in the morning On examination the meatus may be red, with evidence of dried secretion on underwear
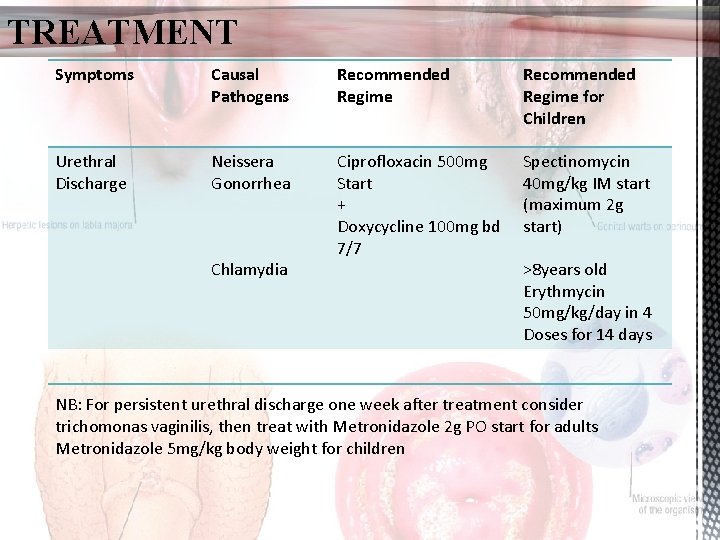
TREATMENT Symptoms Causal Pathogens Recommended Regime for Children Urethral Discharge Neissera Gonorrhea Ciprofloxacin 500 mg Start + Doxycycline 100 mg bd 7/7 Spectinomycin 40 mg/kg IM start (maximum 2 g start) Chlamydia >8 years old Erythmycin 50 mg/kg/day in 4 Doses for 14 days NB: For persistent urethral discharge one week after treatment consider trichomonas vaginilis, then treat with Metronidazole 2 g PO start for adults Metronidazole 5 mg/kg body weight for children

VAGINAL DISCHARGE AND LOWER ABDOMINAL PAIN IN WOMEN - Various gynecological conditions present with Vaginal discharge and lower abdominal pain. These includes; - 1. Pelvic inflammatory Disease (PID)# the condition involving the pelvic organs ie, cervix (cervicitis), uterus (endometritis), salpinx (salpingitis) and ovaries (oophoritis). Responsible Organisms: * Symptoms: L/abdominal pain, Vaginal discharge (sometimes absent) High-grade fever, nausea, vomiting, painful coitus (dyspareunia) 2. Vulvoginitis Condition affectin the Vulva and the Vagina Causative organsms: * Symptoms: Vaginal itching, Burning Sensation 3. Urinary tract infections (UTI) Condition involving the urethra, bladder and sometimes the Kidneys Symptoms: Painful urination, urge to urinate, back ache, blood in urine * Refer to treatment table
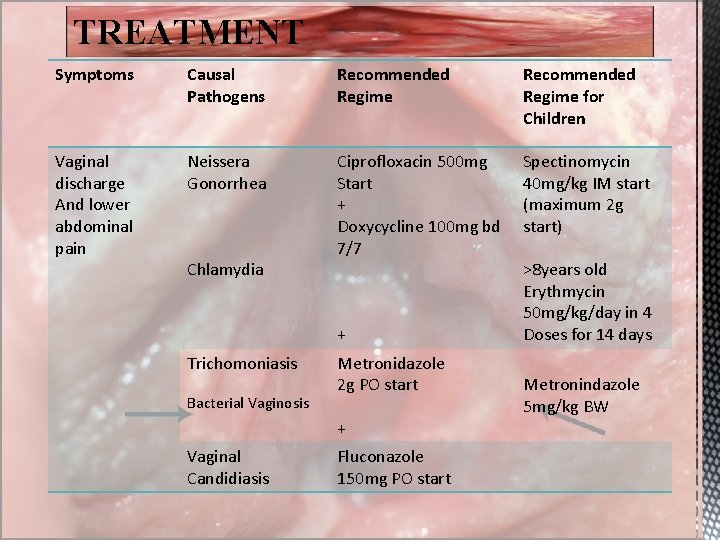
TREATMENT Symptoms Causal Pathogens Recommended Regime for Children Vaginal discharge And lower abdominal pain Neissera Gonorrhea Ciprofloxacin 500 mg Start + Doxycycline 100 mg bd 7/7 Spectinomycin 40 mg/kg IM start (maximum 2 g start) Chlamydia + Trichomoniasis Bacterial Vaginosis Metronidazole 2 g PO start + Vaginal Candidiasis Fluconazole 150 mg PO start >8 years old Erythmycin 50 mg/kg/day in 4 Doses for 14 days Metronindazole 5 mg/kg BW

COMPLICATIONS (DISCHARGES AND LOWER ABDOMINAL PAIN) Male Female • Epididymo-orchitis • Uretral stricture • Perihepatitis could also occur • • • Peritinitis Tubo-ovarian abscess Hydrosalpinx Ectopic Pregnancy Chronic Pelvic pain Infertility Mortality Abnormal vaginal bleeding Abdominal mass
GENITAL ULCERATION DEFINITION: - loss of continuity in the epithelial surface covering the genital are - Men are commonly affected than women CAUSES: • Granuloma anguinale (Donovanosis) • Herpes genitalis • Lymphogranuloma venereum • Syphilis
SYPHILIS • Caused by Treponema pallidum • Incubation period of 9 -90 days Clinical features: - painless papule…which later ulcerate to form a chancre - Chancre is firm with indurated base; referred to as a hard sore - Chancre can be found on; MEN; WOMEN; - glans penis - vulva - shaft - cervix - anus - perineum - rectum - The chanre may also be found on the skin or mucous membrane of the anogenital area as well as lips, toungue, buccal mucosa, tonsils or fingers - there may be bilateral inguinal lymphadenopathy NB: the ulcer heals 3 -6 weeks

TYPES OF SYPHILIS EARLY SYPHILIS (history of contact or Symptom within a year) LATE SYPHILIS ( no history of contact or symptom in one year) Primary Tertiary Syphilis • • • identified by the presence of an ulcer or chancre at the site of inoculation. A chancre is usually indurated and painless. Chancre forms approximately 21 days after initial exposure to T. pallidum. Secondary • • Presents 6 -12 weeks after infection Generalized Cutaneous rash which may affect the soles and pulms The rash can mimic any skin disease Snail track ulcer in the mouth Condylomata lata on the genitalia perineal skin Lyphdenopathy May involve the eyes, bones, joints, meninges, kidneys, liver and spleen • Present 10 to 25 years after initial infection • Presents with cardiovascular complication • Includes dilated aneurysm of the ascending aorta • Narrowing of the coronary aorta NS complication • Dementia • Psychosis • Meningovascular neurosyphilis Note: Congenital syphilis presents with features like those of secondary syphilis in adults
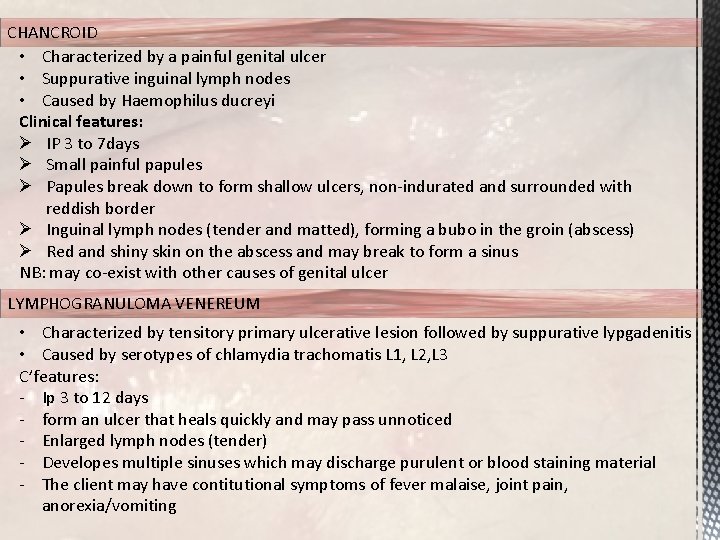
CHANCROID • Characterized by a painful genital ulcer • Suppurative inguinal lymph nodes • Caused by Haemophilus ducreyi Clinical features: Ø IP 3 to 7 days Ø Small painful papules Ø Papules break down to form shallow ulcers, non-indurated and surrounded with reddish border Ø Inguinal lymph nodes (tender and matted), forming a bubo in the groin (abscess) Ø Red and shiny skin on the abscess and may break to form a sinus NB: may co-exist with other causes of genital ulcer LYMPHOGRANULOMA VENEREUM • Characterized by tensitory primary ulcerative lesion followed by suppurative lypgadenitis • Caused by serotypes of chlamydia trachomatis L 1, L 2, L 3 C’features: - Ip 3 to 12 days - form an ulcer that heals quickly and may pass unnoticed - Enlarged lymph nodes (tender) - Developes multiple sinuses which may discharge purulent or blood staining material - The client may have contitutional symptoms of fever malaise, joint pain, anorexia/vomiting

LYMPHOGRANULOMA VENEREUM cont…… - The client may have contitutional symptoms of fever malaise, joint pain, anorexia/vomiting - In women, backache is common in whom the lesion may be on the cervix or upper vagina resulting in the enlargement suppuration of perirectal and pelvic lymp nodes. - This results into rectovaginal vistulas HERPES SIMPLEX - caused by herpes simplex virus - Spread by sexual contact - The condition tend to recure because the virus establish a latent infection C’ features; • Lesion develop 4 to 7 days after sexual contact • Painful lesions, prolonged and widespread • Genital itching and soreness • Develops a small group of painful vesicles which later erode and form several superficial, circular ulcer • Ulcer become crusted after a few days and generally heal with scarring in 10 days • Slightly enlarged inguinal lymph nodes • The patient may experience generalized malaise, fever, difficulty uriting and walking
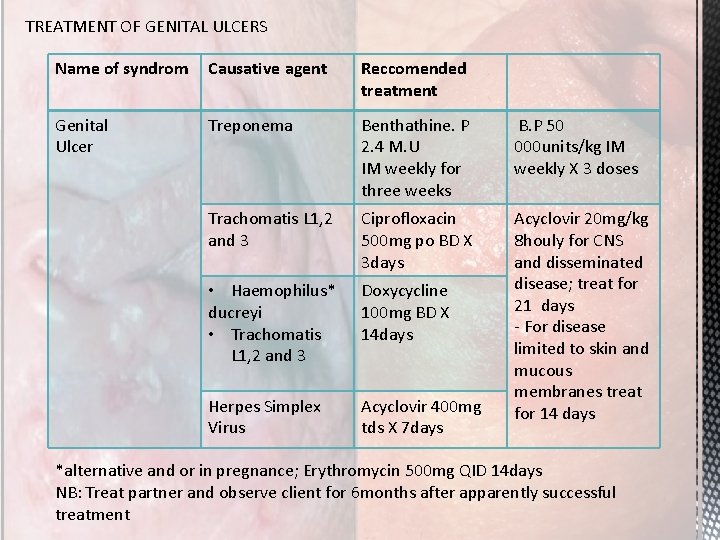
TREATMENT OF GENITAL ULCERS Name of syndrom Causative agent Reccomended treatment Genital Ulcer Treponema Benthathine. P 2. 4 M. U IM weekly for three weeks B. P 50 000 units/kg IM weekly X 3 doses Trachomatis L 1, 2 and 3 Ciprofloxacin 500 mg po BD X 3 days • Haemophilus* ducreyi • Trachomatis L 1, 2 and 3 Doxycycline 100 mg BD X 14 days Herpes Simplex Virus Acyclovir 400 mg tds X 7 days Acyclovir 20 mg/kg 8 houly for CNS and disseminated disease; treat for 21 days - For disease limited to skin and mucous membranes treat for 14 days *alternative and or in pregnance; Erythromycin 500 mg QID 14 days NB: Treat partner and observe client for 6 months after apparently successful treatment

STIs in NEONATES • All neonatal and Congenital STIs are transmitted from motherto-child • The most common are Ophthalmia Neonatum, Congenital Syphilis and HIV infection OPHTHALMIA NEONATUM: • • Inflammation of the conjuctiva in the neonatal period due to infection with Neisseria gonorrheae Infection is acquired during birth Has the incubation period of 3 to 5 days Chlamydia, trachomatis, staphylococcus aureus and streptococcus pneumoniae can also cause neonatal conjustivitis • CF: presents with purulent, copious eye discharge (birateral), itching and redness, fever, rash, joint sweelling and septicaemia CONGENITAL SYPHILIS Cf; • Malaise, headache, anorexia, nausea, bone pain and fatigibility • Including fever, jaundice, albuminuria and neck stiffness
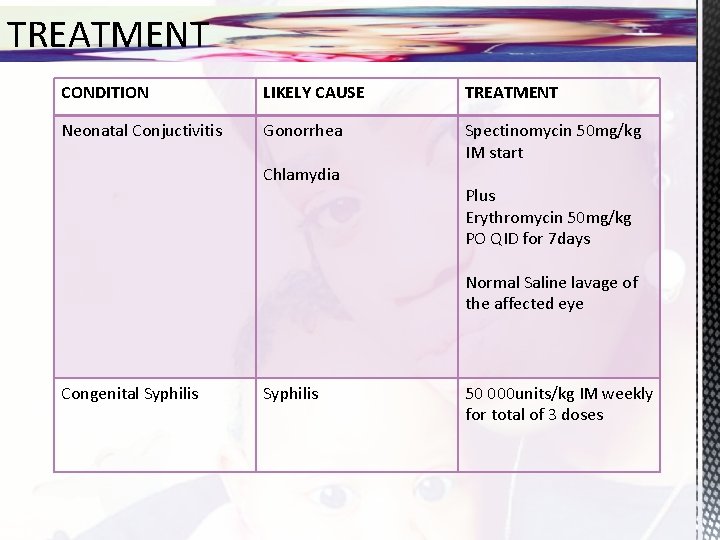

TREATMENT CONDITION LIKELY CAUSE TREATMENT Neonatal Conjuctivitis Gonorrhea Spectinomycin 50 mg/kg IM start Chlamydia Plus Erythromycin 50 mg/kg PO QID for 7 days Normal Saline lavage of the affected eye Congenital Syphilis 50 000 units/kg IM weekly for total of 3 doses

Granuloma Inguinal (Donovanosis) Chronic Granulomatous condition usually involving the genitalia and spread by sexual contact Caused by Calymmatobacterium granulomatis Clinical Features: • Painlession • Beefy-red nodules • Large nodules appear and form a large elevated, velvety, granulomatous mass • Incubation period 1 -12 weeks • Sites: MEN: WOMEN: Penis Vulva Scrotum Vagina Groin Perineum Thighs Face Anus Buttocks • There is no lyphodenopathy • Slow progress but eventually may cause lymphetic obstruction and Elephantiasis of the Genitalia • May result into Anemia and Weight loss • Treatment: Erythromycin 500 mg QID for 14 to 21 days • Note: Rare in Zambia
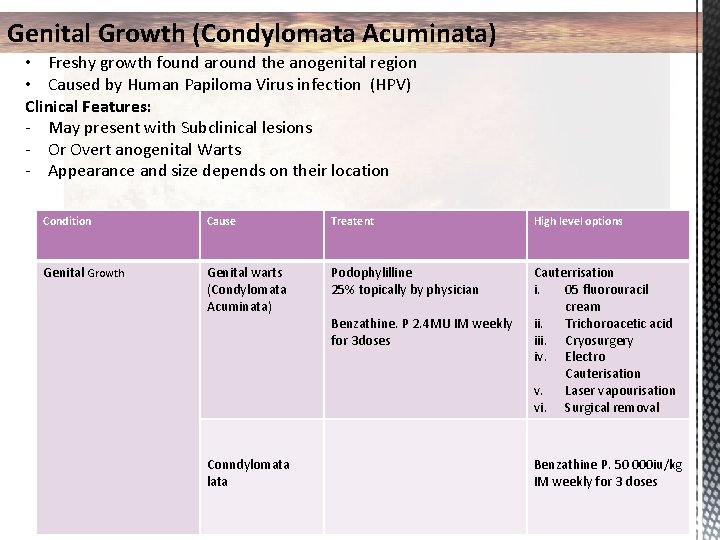
Genital Growth (Condylomata Acuminata) • Freshy growth found around the anogenital region • Caused by Human Papiloma Virus infection (HPV) Clinical Features: - May present with Subclinical lesions - Or Overt anogenital Warts - Appearance and size depends on their location Condition Cause Treatent High level options Genital Growth Genital warts (Condylomata Acuminata) Podophylilline 25% topically by physician Cauterrisation i. 05 fluorouracil cream ii. Trichoroacetic acid iii. Cryosurgery iv. Electro Cauterisation v. Laser vapourisation vi. Surgical removal Conndylomata lata Benzathine. P 2. 4 MU IM weekly for 3 doses Benzathine P. 50 000 iu/kg IM weekly for 3 doses
HEPATITIS • An acute inflammation of the liver caused by primary human virus A to E; B and C Mode of Transmission: ü Cutaneous ü Mucous membrane exposed to contaminated blood ü Unprotected sex by infected partner ü Contaminated needle by injection ü Perinatal transmission Clinical Features: • Malaise • Nausea • Abdominal pain • Anorexia • Jaundice • Dark urine • Fever • Rash • Athralgia
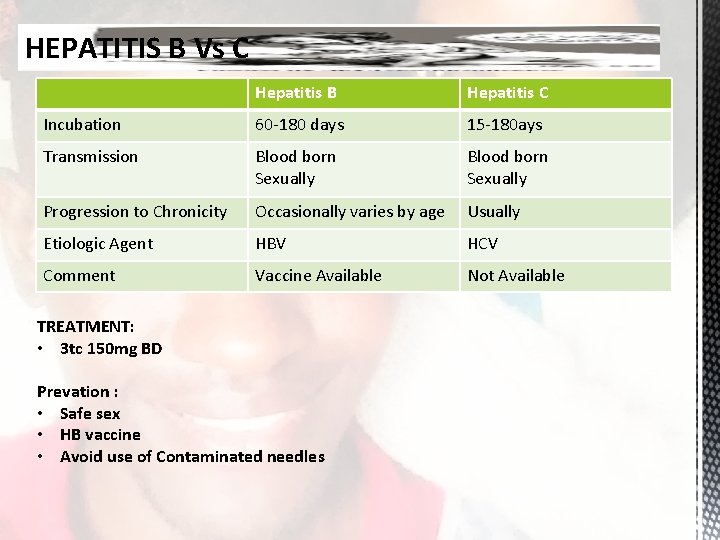
HEPATITIS B Vs C Hepatitis B Hepatitis C Incubation 60 -180 days 15 -180 ays Transmission Blood born Sexually Progression to Chronicity Occasionally varies by age Usually Etiologic Agent HBV HCV Comment Vaccine Available Not Available TREATMENT: • 3 tc 150 mg BD Prevation : • Safe sex • HB vaccine • Avoid use of Contaminated needles

STI FREE ZAMBIA IS PRODUCTIVE
- Slides: 27