Sidedness gender and BMI as prognostic factors of

Sidedness, gender and BMI as prognostic factors of colorectal cancer in the real-world setting Nicola Tinari Oncologia Medica Università G. D’Annunzio Chieti

New non-stage related clinical factors • Stage is still the best prognostic factor. However, there is important within-stage variability • Recent research efforts have examined new stage-independent predictive/prognostic markers: - Gender - Body mass index (BMI) - Sidedness
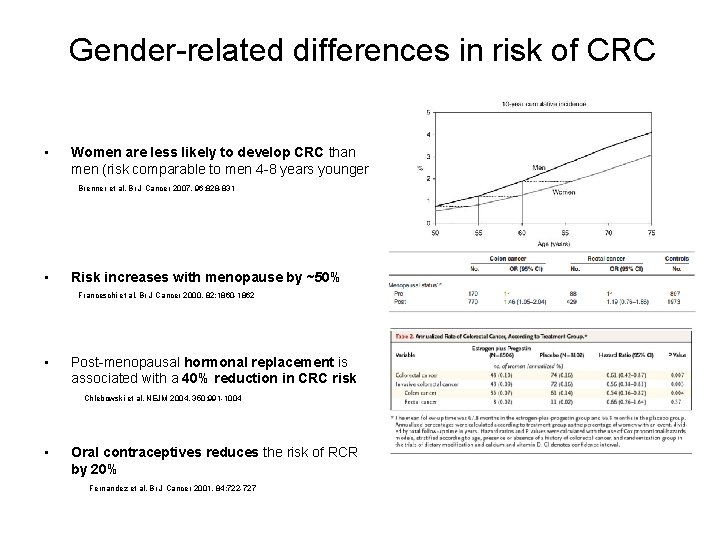
Gender-related differences in risk of CRC • Women are less likely to develop CRC than men (risk comparable to men 4 -8 years younger Brenner et al. Br J Cancer 2007, 96: 828 -831 • Risk increases with menopause by ~50% Franceschi et al. Br J Cancer 2000, 82: 1860 -1862 • Post-menopausal hormonal replacement is associated with a 40% reduction in CRC risk Chlebowski et al. NEJM 2004, 350: 991 -1004 • Oral contraceptives reduces the risk of RCR by 20% Fernandez et al. Br J Cancer 2001, 84: 722 -727
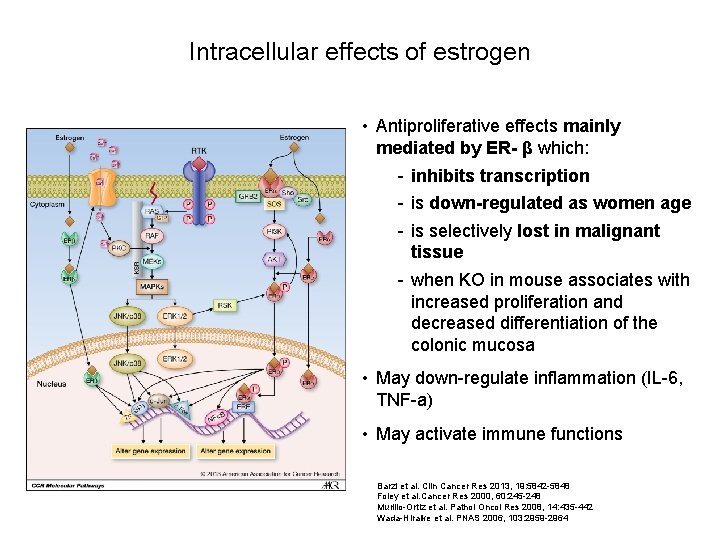
Intracellular effects of estrogen • Antiproliferative effects mainly mediated by ER- β which: - inhibits transcription - is down-regulated as women age - is selectively lost in malignant tissue - when KO in mouse associates with increased proliferation and decreased differentiation of the colonic mucosa • May down-regulate inflammation (IL-6, TNF-a) • May activate immune functions Barzi et al. Clin Cancer Res 2013, 19: 5842 -5848 Foley et al. Cancer Res 2000, 60: 245 -248 Murillo-Ortiz et al. Pathol Oncol Res 2008, 14: 435 -442 Wada-Hiraike et al. PNAS 2006, 103: 2959 -2964

Role of gender in localized CRC • After curative resection available real-life data indicate a significant OS and DFS advantage for women 1 -2 • The survival advantage appears to be higher in women < 65 years or >75 years 3 • In multicenter retrospective study of >600 consecutive patients survival benefit of adjuvant chemotherapy is higher for women after median follow-up of 54 months 4 • Women experience greater toxicity with fluorouracil-based chemotherapy (G 3 -4 toxicity in 50% vs 33%) 5 1. 2. 3. 4. 5. Wichmann et al. Br J Surg 2001, 88(8): 1092 -8 Mc. Ardle et al Br J Cancer 2003, 90: 711 -715 Majek et al. PLos. One 2013, 8: e 68077 Elsaleh et al. Lancet 2000, 355: 1745 -1750 Sloan et al. J Clin Oncol 2002, 20: 1491 -1498
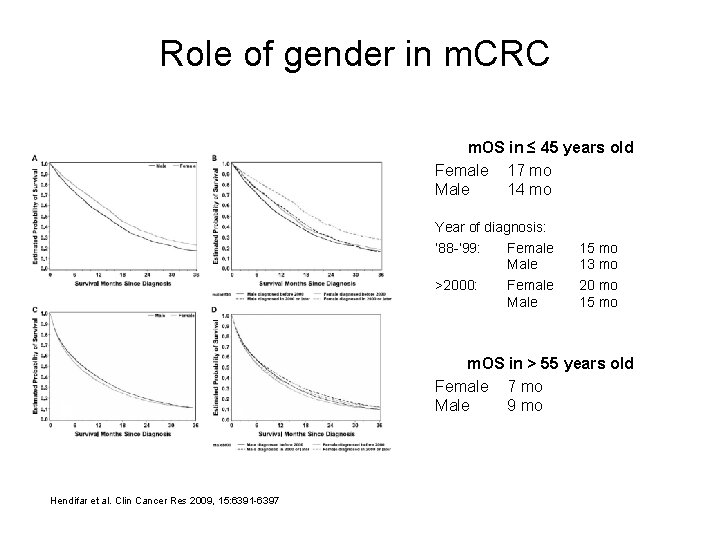
Role of gender in m. CRC m. OS in ≤ 45 years old Female 17 mo Male 14 mo Year of diagnosis: ’ 88 -’ 99: Female Male >2000: Female Male 15 mo 13 mo 20 mo 15 mo m. OS in > 55 years old Female 7 mo Male 9 mo Hendifar et al. Clin Cancer Res 2009, 15: 6391 -6397
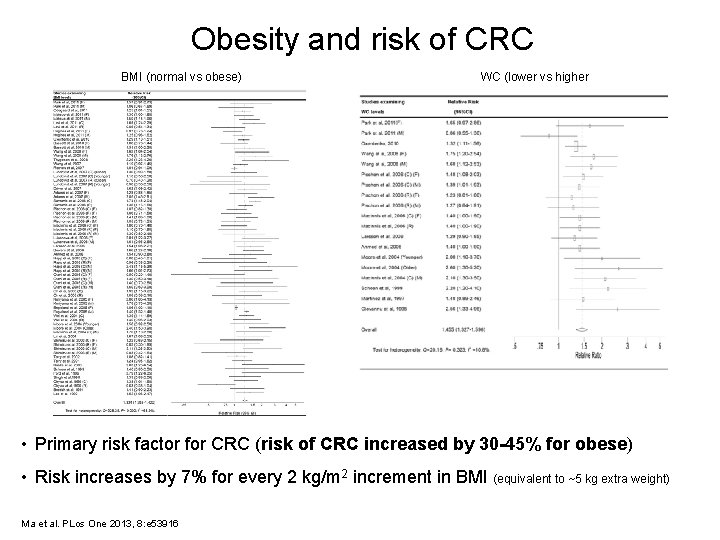
Obesity and risk of CRC BMI (normal vs obese) WC (lower vs higher • Primary risk factor for CRC (risk of CRC increased by 30 -45% for obese) • Risk increases by 7% for every 2 kg/m 2 increment in BMI (equivalent to ~5 kg extra weight) Ma et al. PLos One 2013, 8: e 53916
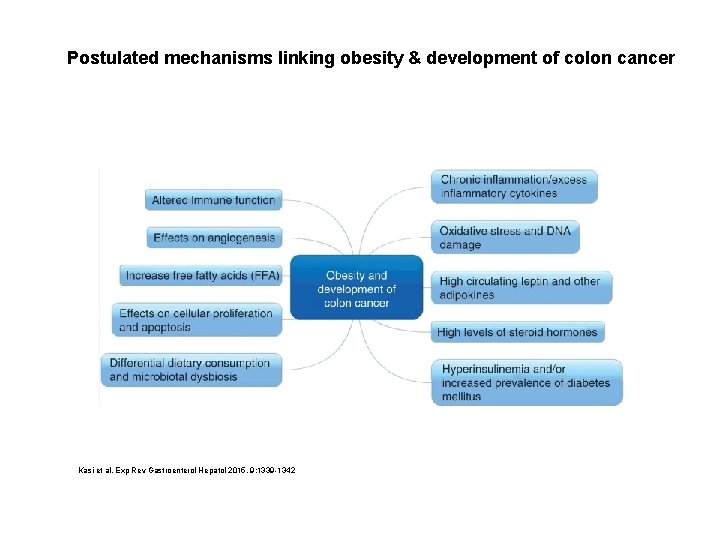
Postulated mechanisms linking obesity & development of colon cancer Kasi et al. Exp Rev Gastroenterol Hepatol 2015, 9: 1339 -1342

BMI as a prognostic factor in CRC • Association with prognosis of CRC is less clear, since studies show mixed results (protective tendencies, no tendencies or detrimental associations) • Current evidence limited by heterogeneity across studies in terms of inclusion and exclusion criteria, BMI categories, stage of disease, time to BMI assessment, adjustment for confounders • Time of BMI assessment may account for the variable association of BMI with prognosis • BMI is usually treated as a categorical variable while in fact it is a continous one: this might obscure subgroups with different prognosis Wu et al. Cancer Causes Control 2014, 25: 1489 -1502 Campbell et al. J Clin Oncol 2012, 30: 42 -52
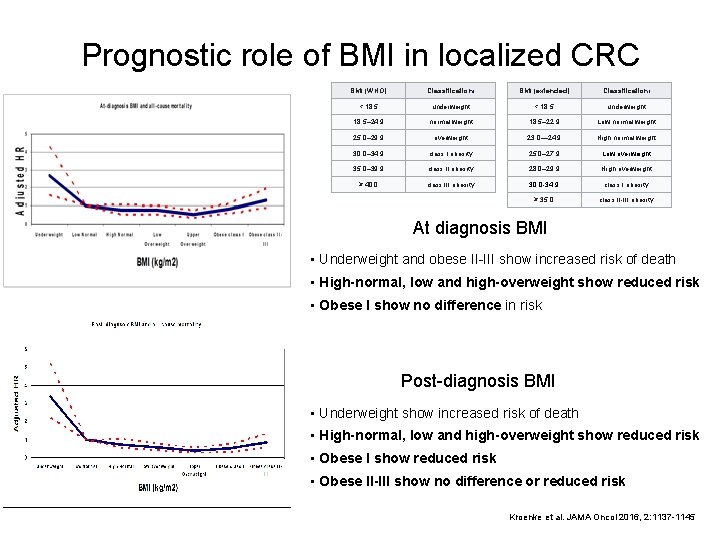
Prognostic role of BMI in localized CRC BMI (WHO) Classification[ BMI (extended) Classification[ < 18. 5 underweight 18. 5– 24. 9 normal weight 18. 5– 22. 9 Low normal weight 25. 0– 29. 9 overweight 23. 0— 24. 9 High normal weight 30. 0– 34. 9 class I obesity 25. 0– 27. 9 Low overweight 35. 0– 39. 9 class II obesity 28. 0– 29. 9 High overweight ≥ 40. 0 class III obesity 30. 0 -34. 9 class I obesity ≥ 35. 0 class II-III obesity At diagnosis BMI • Underweight and obese II-III show increased risk of death • High-normal, low and high-overweight show reduced risk • Obese I show no difference in risk Post-diagnosis BMI • Underweight show increased risk of death • High-normal, low and high-overweight show reduced risk • Obese II-III show no difference or reduced risk Kroenke et al. JAMA Oncol 2016, 2: 1137 -1145
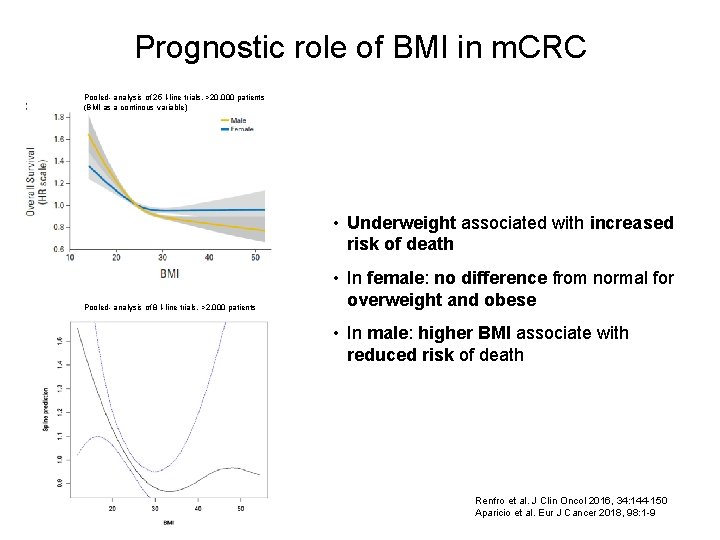
Prognostic role of BMI in m. CRC Pooled- analysis of 25 I-line trials, >20. 000 patients (BMI as a continous variable) • Underweight associated with increased risk of death Pooled- analysis of 8 I-line trials, >2. 000 patients • In female: no difference from normal for overweight and obese • In male: higher BMI associate with reduced risk of death Renfro et al. J Clin Oncol 2016, 34: 144 -150 Aparicio et al. Eur J Cancer 2018, 98: 1 -9

The obesity paradox Counterintuitively, overweight and possibly obese patients show a reduced risk of mortality Variably attributed to: - Selection bias - Reverse causality (underweight category may include cachectic patients) - Collider bias (underweight patients may be exposed to other risk factors, i. e. smoking) - Inadequacy of BMI as a measure of adiposity - Better nutritional status, with greater muscle and fat mass to cope with metabolic demand of tumor and treatment - Different pharmacokinetis of chemotherapics in obese “Findings suggest that recommendations for weight loss in the immediate post-diagnosis period may be unwarranted” Flegal et al. Am J Epidemiol 2011, 173: 1 -9 Casas-Vara et al. Nutrition 2012, 28: 616 -622 Lennon et al. Curr Oncol Rep 2016, 18: 56 Hanley et al. Clin Pharmacokinet 2010, 49: 71 -87 Kroenke et al. JAMA Oncol 2016, 2: 1137 -1145
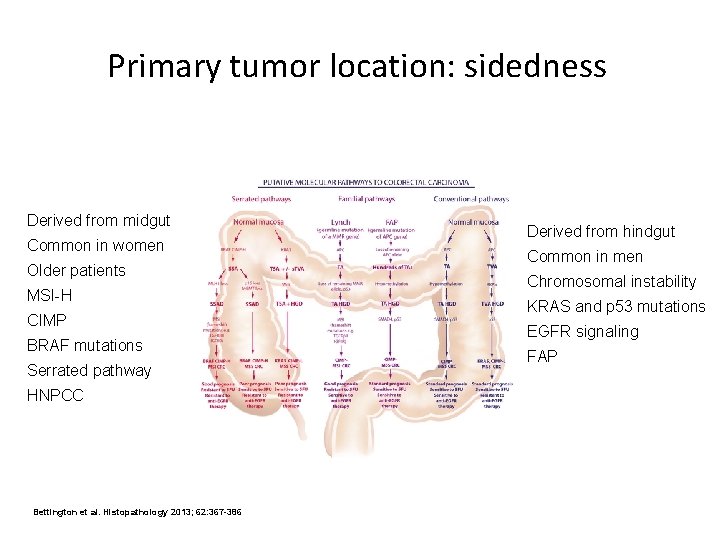
Primary tumor location: sidedness Derived from midgut Common in women Older patients MSI-H CIMP BRAF mutations Serrated pathway HNPCC Bettington et al. Histopathology 2013; 62: 367 -386 Derived from hindgut Common in men Chromosomal instability KRAS and p 53 mutations EGFR signaling FAP
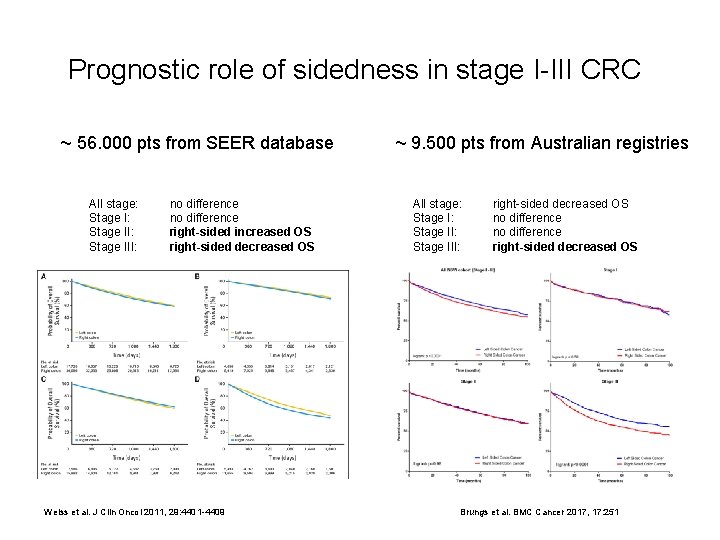
Prognostic role of sidedness in stage I-III CRC ~ 56. 000 pts from SEER database All stage: Stage II: Stage III: no difference right-sided increased OS right-sided decreased OS Weiss et al. J Clin Oncol 2011, 29: 4401 -4409 ~ 9. 500 pts from Australian registries All stage: Stage II: Stage III: right-sided decreased OS no difference right-sided decreased OS Brungs et al. BMC Cancer 2017, 17: 251
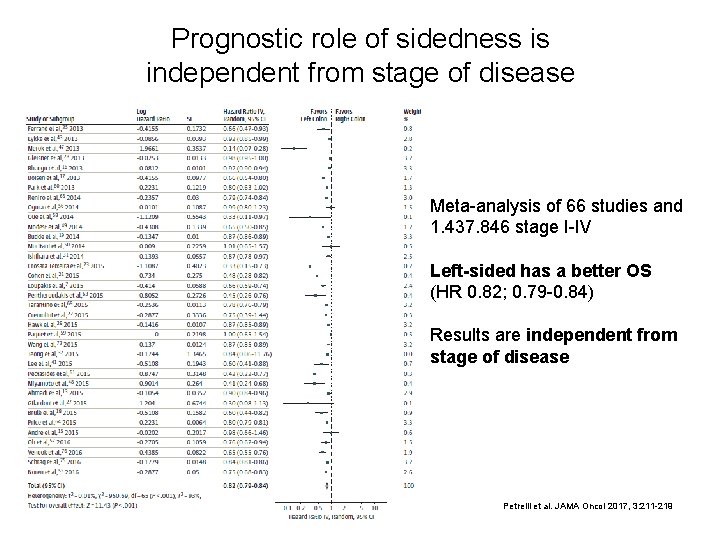
Prognostic role of sidedness is independent from stage of disease Meta-analysis of 66 studies and 1. 437. 846 stage I-IV Left-sided has a better OS (HR 0. 82; 0. 79 -0. 84) Results are independent from stage of disease Petrelli et al. JAMA Oncol 2017, 3: 211 -219
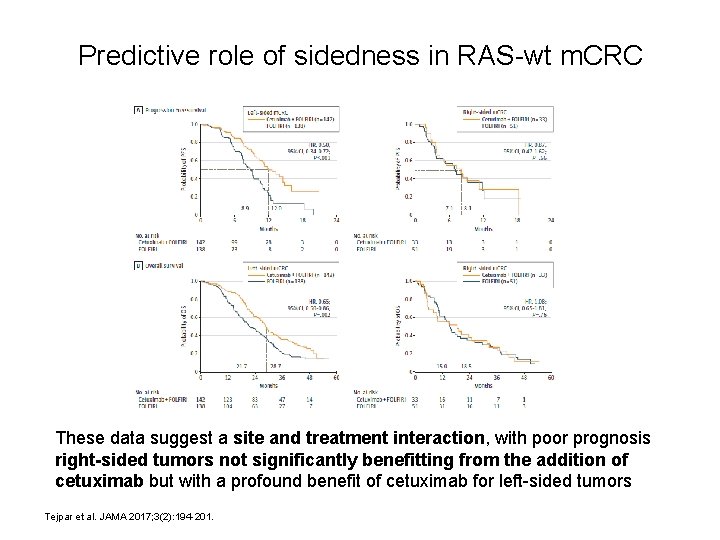
Predictive role of sidedness in RAS-wt m. CRC These data suggest a site and treatment interaction, with poor prognosis right-sided tumors not significantly benefitting from the addition of cetuximab but with a profound benefit of cetuximab for left-sided tumors Tejpar et al. JAMA 2017; 3(2): 194 -201.
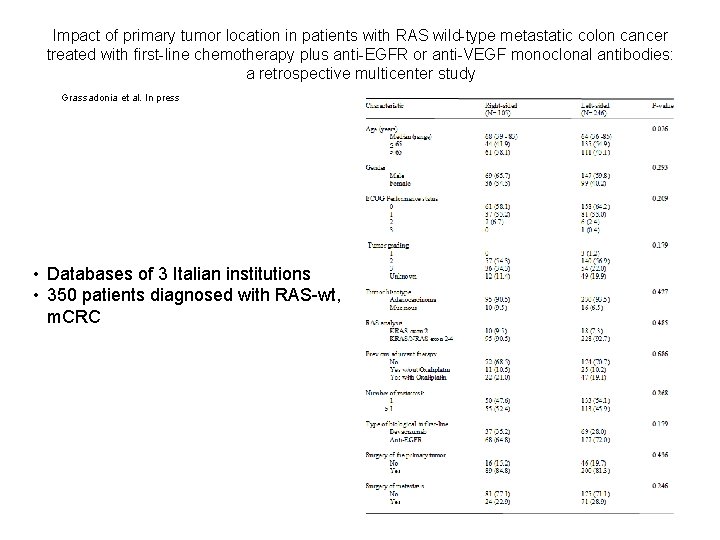
Impact of primary tumor location in patients with RAS wild-type metastatic colon cancer treated with first-line chemotherapy plus anti-EGFR or anti-VEGF monoclonal antibodies: a retrospective multicenter study Grassadonia et al. In press • Databases of 3 Italian institutions • 350 patients diagnosed with RAS-wt, m. CRC
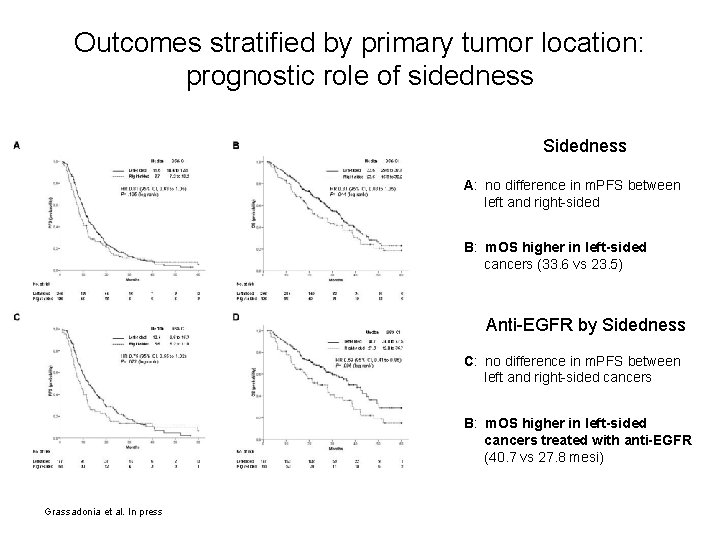
Outcomes stratified by primary tumor location: prognostic role of sidedness Sidedness A: no difference in m. PFS between left and right-sided B: m. OS higher in left-sided cancers (33. 6 vs 23. 5) Anti-EGFR by Sidedness C: no difference in m. PFS between left and right-sided cancers B: m. OS higher in left-sided cancers treated with anti-EGFR (40. 7 vs 27. 8 mesi) Grassadonia et al. In press
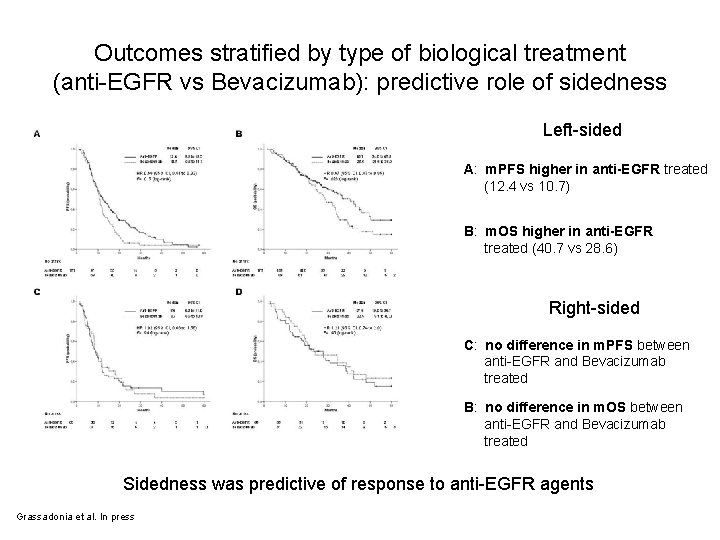
Outcomes stratified by type of biological treatment (anti-EGFR vs Bevacizumab): predictive role of sidedness Left-sided A: m. PFS higher in anti-EGFR treated (12. 4 vs 10. 7) B: m. OS higher in anti-EGFR treated (40. 7 vs 28. 6) Right-sided C: no difference in m. PFS between anti-EGFR and Bevacizumab treated B: no difference in m. OS between anti-EGFR and Bevacizumab treated Sidedness was predictive of response to anti-EGFR agents Grassadonia et al. In press

Conclusions • Data are often conflicting, due to the heterogeneity of the available studies • Overall real-life studies indicate an association with risk and prognosis of CRC for gender, BMI and sidedness • Female display a reduce risk, and a better prognosis if ≤ 45 years old • The obesity paradox operates also in CRC, with risk of death reduced or not increased for overweight and obese patients • Right-sided cancer have generally a worst prognosis and appears to respond less to anti-EGFR, even when RAS-wt

Consensus molecular subtypes of CRC Guinney et al. Nat Med. 2015, 21(11): 1350– 1356
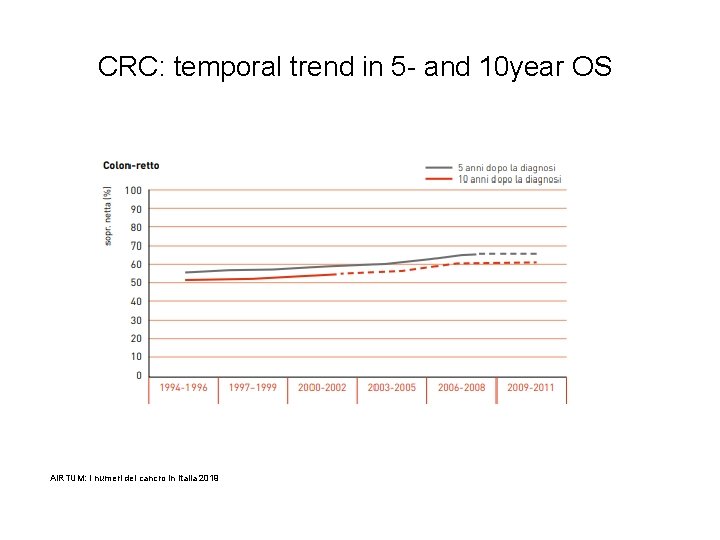
CRC: temporal trend in 5 - and 10 year OS AIRTUM: I numeri del cancro in Italia 2019
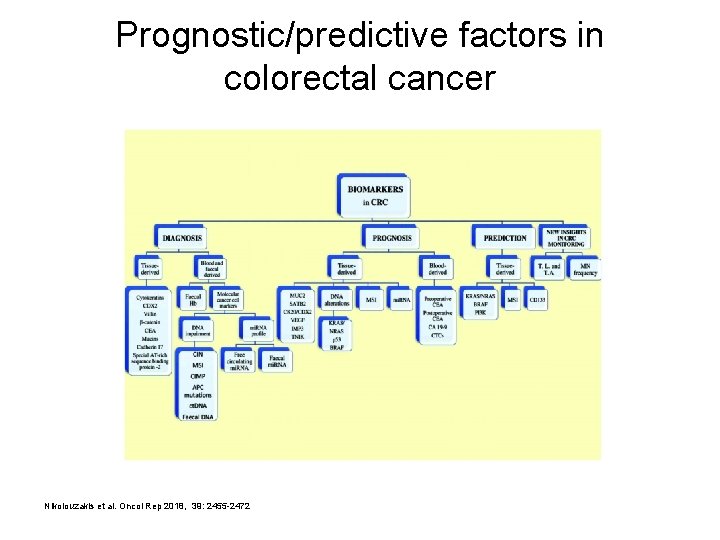
Prognostic/predictive factors in colorectal cancer Nikolouzakis et al. Oncol Rep 2018, 39: 2455 -2472
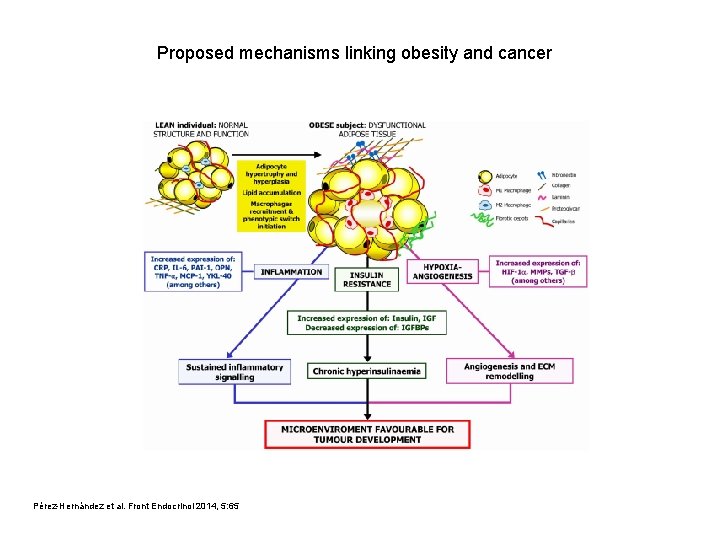
Proposed mechanisms linking obesity and cancer Pérez-Hernández et al. Front Endocrinol 2014, 5: 65
- Slides: 24