Shoulder Replacement Daniel Blackmon Hillcrest Hospital Inservice Summer

Shoulder Replacement Daniel Blackmon Hillcrest Hospital Inservice Summer 2012

Objectives 1. Review and discuss basic shoulder anatomy 2. Discuss the articulations of the shoulder, primarily the glenohumeral joint 3. Introduce the types of shoulder replacements available to individuals with severe pain and/or loss of shoulder function 4. Discuss why each procedure is used, what patients they are indicated for, and the advantages and disadvantages of each. 5. Review the research findings on selected studies investigating the types of activities individuals with shoulder replacement participate in post-surgery
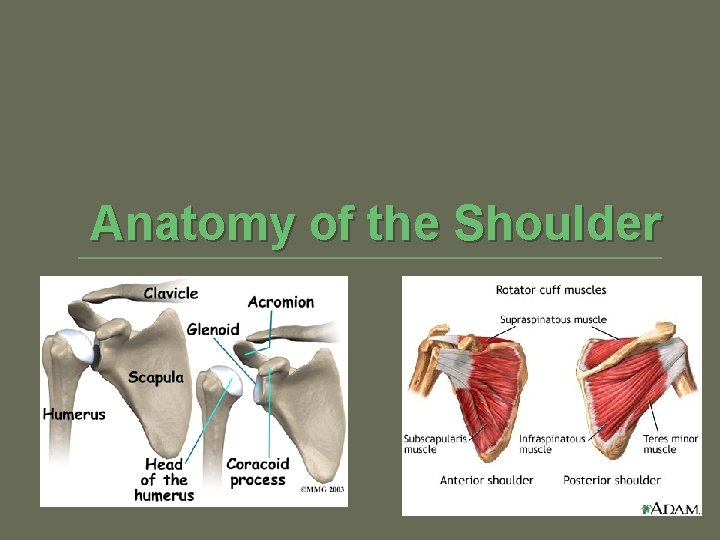
Anatomy of the Shoulder
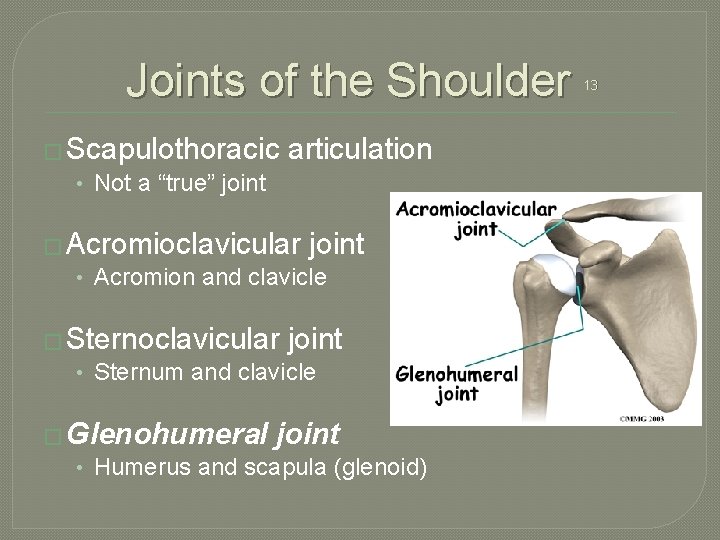
Joints of the Shoulder � Scapulothoracic • Not a “true” joint articulation � Acromioclavicular joint • Acromion and clavicle � Sternoclavicular joint • Sternum and clavicle � Glenohumeral joint • Humerus and scapula (glenoid) 13
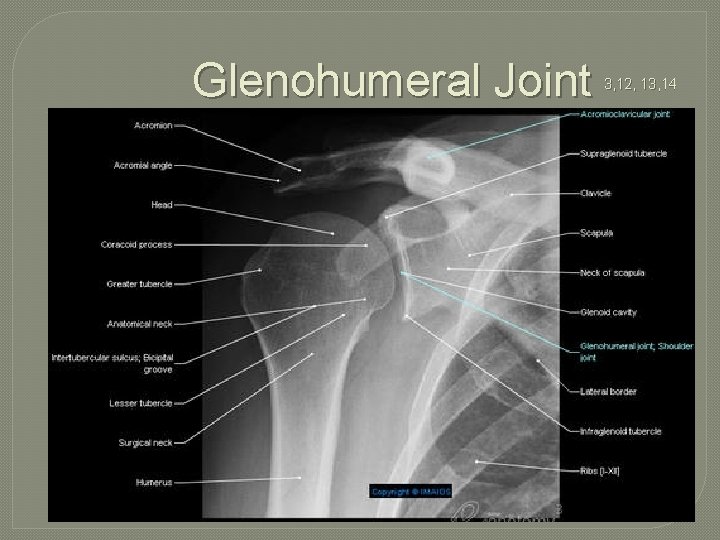
Glenohumeral Joint 3, 12, 13, 14

�Articulation between humeral head and glenoid fossa of scapula �“Ball and Socket” • Convex on concave �Convex humerus on concave glenoid �Roll and glide �More mobility than stability • Most commonly dislocated joint in the body

� 3 Degrees of Freedom • Frontal, saggital and transverse plane movement �Flexion/Extension �Abduction/Adduction �Horizontal abduction/adduction �Internal/External Rotation • Surface area of humeral head 3 -4 x larger than glenoid � Stability • Active �Rotator cuff muscles and tendons • Passive �Ligaments, labrum, bony anatomy, scapular positioning, negative intra-articular pressure
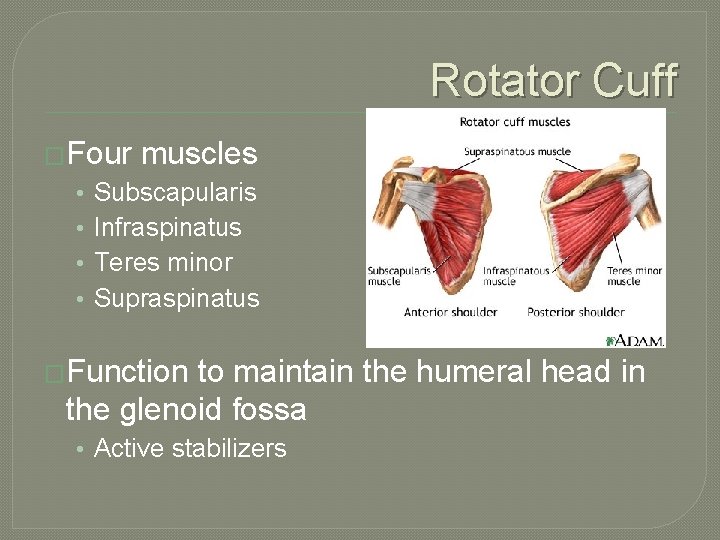
Rotator Cuff �Four • • muscles Subscapularis Infraspinatus Teres minor Supraspinatus �Function to maintain the humeral head in the glenoid fossa • Active stabilizers

Shoulder Arthroplasties

Shoulder Pathology 1, 4 � Shoulder is the 2 nd most commonly reported site of chronic joint pain behind the knee � Accounts for approximately 10% of all physical therapy referrals � Shoulder disorders are a common cause of musculoskeletal disorders affecting between 730% of adults at any time � Rotator cuff disease is the most common cause of shoulder pain seen by physicians

Shoulder Replacements 1, 5, 7 � 3 rd most common large joint to require surgical reconstruction • 3% of arthroplasties � 96% are hip and knee • Estimated that >10, 000 TSA are performed each year in the US � 2/3 performed on individuals > age 65 � 2/3 performed on women
�Etiologies • Primary osteoarthritis �Relatively uncommon disorder/site for OA • Rotator cuff disease • Post-traumatic arthritis �Proximal humeral fractures • Avascular necrosis • Rheumatoid arthritis �Unsuccessful activity modification and nonoperative treatments
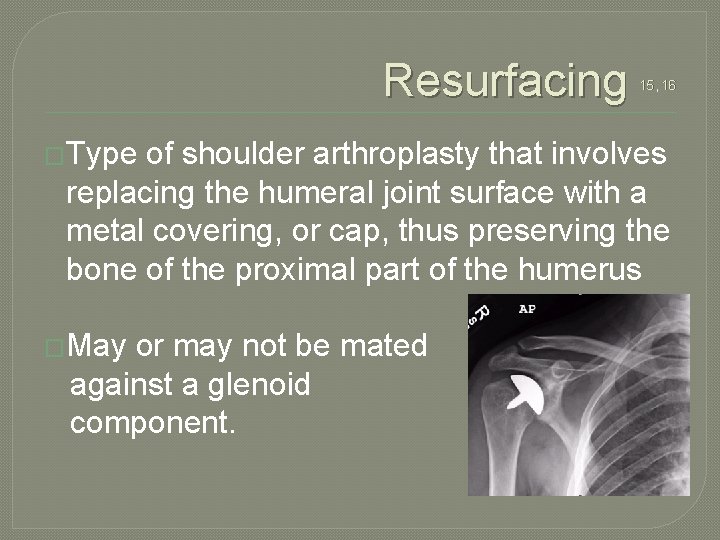
Resurfacing �Type 15, 16 of shoulder arthroplasty that involves replacing the humeral joint surface with a metal covering, or cap, thus preserving the bone of the proximal part of the humerus �May or may not be mated against a glenoid component.

� Indications • Pain and/or decreased function that are not successfully treated nonoperatively �Osteoarthritis, rheumatoid arthritis, osteonecrosis, posttraumatic arthritis, cuff tear arthropathy and chronic instability of the joint • Patients indicated for arthropathy but have extra- articular deformities of the proximal humerus that make placement of a conventional prosthesis impossible � Contraindicated for patients with four-part fractures and inadequate bone stock • Humeral head fragment is separate from the shaft and both tuberosities, and is dislocated out of the glenoid

Advantages/Disadvantages • Humeral neck and >50% of the humeral head are • • retained Low complication rates in studies with follow-up times of 8 months – 7 years Head-shaft angle is retained Minimal bone resection Short operative time Low prevalence of humeral periprosthetic fractures Easily converted to TSA if needed Revision rates comparable to TSA Component loosening is most frequent complication
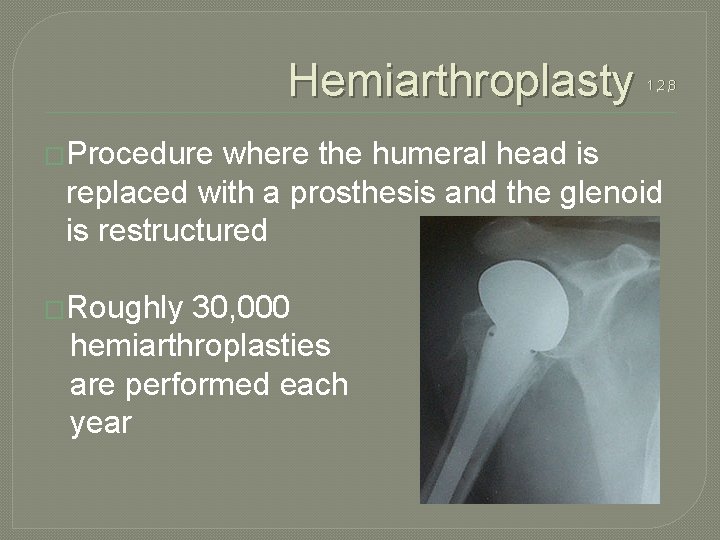
Hemiarthroplasty �Procedure 1, 2, 8 where the humeral head is replaced with a prosthesis and the glenoid is restructured �Roughly 30, 000 hemiarthroplasties are performed each year
�Indications • Isolated articular involvement of the humerus • Early stage avascular necrosis and post-traumatic arthritis who may have relatively normal glenoid articular surfaces • Rheumatoid arthritis patients with rotator cuff disease or erosion • Younger patients (<50 years of age) who are more active

Advantages/Disadvantages � Process shoulder requires a shorter operating time than total � Decreased � Can risk of instability vs. TSA be revised at a later date to a TSA � Offers less predictable results than TSA � Revision to a TSA is a more complicated surgery with less predictable results than having a primary TSA � TSA yields more reliable pain relief than hemiarthroplasty 1, 7
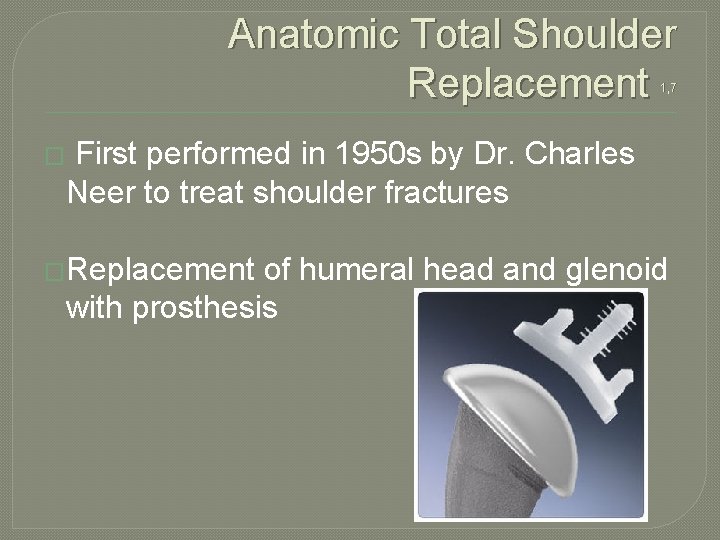
Anatomic Total Shoulder Replacement 1, 7 � First performed in 1950 s by Dr. Charles Neer to treat shoulder fractures �Replacement of humeral head and glenoid with prosthesis

� Research shows TSA to be highly successful in the treatment of primary and secondary degenerative conditions of the shoulder � Preferred treatment for advanced glenohumeral osteoarthritis � Indications: • Patients who have arthritic involvement of both the glenoid and humerus and an intact rotator cuff • RC is intact and glenoid wear is present • Patients with Rheumatoid Arthritis and intact RC, avascular necrosis and post-traumatic arthritis with glenoid involvement

Advantages/Disadvantages 1, 7, 8 � Patients with RA and intact RC have better outcomes and lower revision rates than with hemiarthroplasty � Over 95% of patients will achieve satisfactory results (improvements in pain relief, ROM, and function) � 85% of prostheses are intact 20 years after implantation � Total shoulder replacement in the presence of rotator cuff tears is associated with early glenoid implant loosening and failure

� High-density polyethylene wear debris may cause loosening of both components • Glenoid loosening associated with bone loss � Loosening of glenoid and humeral components is a common event - 39% of complications - 83% involved failure of the glenoid component � Lavard et al. (2011) found glenoid migration occurred more in total shoulders than reverse shoulders (28. 5% vs. 3. 4%; p < 0. 001) � TSA Complications (in order of frequency): • Component loosening, instability, prosthetic fracture, rotator cuff tears, neural injury, infection, and deltoid muscle dysfunction
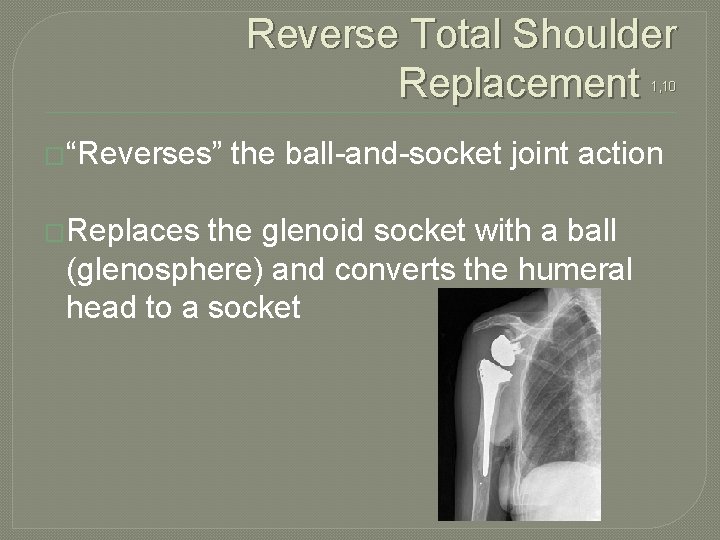
Reverse Total Shoulder Replacement 1, 10 �“Reverses” �Replaces the ball-and-socket joint action the glenoid socket with a ball (glenosphere) and converts the humeral head to a socket

�“Reversed” Joint Action �This allows for the deltoid to be the primary elevator of the arm even without the presence of the rotator cuff �Relative to normal glenohumeral articulation, in reverse total shoulder the humerus is inferiorly displaced, providing a greater lever arm for the deltoid �However, this limits the amount of force the implant can endure �Reverse total shoulder typically indicated for older patients due to this constraint
� Indicated for patients with insufficient rotator cuffs • Patients with chronic, massive, unrepairable rotator cuff tears with or without GH arthritis • RA patients with rotator cuff tears • Patients with severe proximal humerus fractures • Cases requiring revision of a failed previous anatomic shoulder replacement. � Has been shown to improve pain and function in patients with the combination of glenohumeral arthritis and rotator cuff disease � Less active patients older than 65 years of age

Advantages/Disadvantages 1, 9, 10, 12 �Allows the deltoid to replace the rotator cuff as the primary elevator and abductor of the shoulder �More post-surgical activity restrictions • Implant can endure less wear than TSA or hemiarthroplasties �Scapular notching -Defined as glenoid neck erosion caused by repetitive abutment of the humeral component with the inferior scapular neck -Typically occurs within the first few months after reverse TSA -Incidence ranges from 44% - 96%. - Unclear the significance of scapular notching clinically, but it is believed to contribute to implant loosening. �Neurovascular injury, infection, hematoma

�Risk of complications is higher when the reverse shoulder prosthesis is implanted as a revision procedure than when it is the primary operation • Revision rates for these surgeries may be as high as 33% �Instability usually occurs within the first year after surgery • Studies have reported instability in 5 -30% • Revision rates are highest within first 3 years

Activites After Shoulder Replacement

Reverse Total Shoulder � Lawrence et al. (2012) • Survey of 78 patients (81 shoulders) who had undergone reverse total shoulder replacement �Mean age: 73; 49 women, 32 men. � 49 women, 32 men �Average time since surgery: 3. 6 years (3 -5 years) �Rotator cuff arthropathy: 70 shoulders �Massive rotator cuff tear: 6 shoulders �Failed treatment of proximal humeral fractures: 5 shoulders • Participants completed a survey concerning pain, motion, strength, and 72 activities they were able to return to post-surgery �ADL and sporting activities

� Results • General activities �Light demand �Cooking, baking, driving �Medium demand �Gardening, leaf raking, lawn mowing �High demand �Snow shoveling, wheelbarrow use, shoveling dirt • Sporting activities �Low demand �Stationary cycling, treadmill and horseshoes �Medium demand �Fishing, dancing, swimming �High demand �Road biking, free weights, hunting/shooting

� The most commonly reported activities in both general and sporting activities are comparable to the reports of TSA and HA patients � The 4 most commonly reported activities patients did not return to were overhead activities, reaching behind for dressing/gowning, swimming/golf, and heavy lifting

Total Shoulder Replacement �Schumann et al. (2010) �Return to sports activity following total shoulder arthroplasty • N=100 patients with unilateral TSA followed > 1 year � 39 females, 61 males �Mean age �At time of study: 68. 9 + 10. 8 yrs �At operation: 66. 2 + 10. 9 yrs • Assessed preoperatively and at 1 and 2 years post -arthroplasty

• Of the 55 patients who participated in sports prior to surgery, 49 (89%) returned to activity following surgery � 18 (36. 7%) had limitations with sports after TSA due to their shoulder � 9 (18. 4%) had restrictions not related to TSA � 2 (4. 1%) had restrictions not related to TSA plus cardiovascular limitations � 20 (40. 8%) had no limitations following TSA • 11/17 (65%) who had given up sports prior to TSA returned after surgery • No patients had to stop sports participation after surgery • The mean age of individuals in the sports group was significantly younger than the non-sports group (63 vs. 70; p = 0. 002)

�Sports most commonly returned to were swimming (10 patients), golf (8 patients), cycling (8 patients), and fitness training (8 patients) � 33/49 (67%) were able to resume sport activities within 6 months post-op • 12/49 within 3 mo. • 21/49 between 3 and 6 mo.

�Authors concluded that total shoulder arthroplasty allows patients to participate in sports without restriction of their level of activity • Probability of being able to do sports postoperatively – if done pre-operatively – is high. • More studies are needed to determine the effect of sports on wear and rate of loosening

Activity Recommendations � Magnussen et al. 2011 • Online survey sent to members of the American Shoulder and Elbow Surgeons (ASES) and the European Society for Surgery of the Shoulder and Elbow (SECEC) • Participants received a list of 37 activities and asked to categorize their postoperative recommendations for each as: �Allowed with experience �Not allowed �Undecided • Recommendations given for total shoulder, reverse shoulder and hemiarthroplasty patients

�Allowed • • activities for all procedures Jogging/running Walking Stationary bicycling Ballroom dancing �Reverse shoulder replacement had more limitations • Low-impact aerobics, stairclimber, hiking, road cycling, golf, swimming, table tennis allowed “with experience” for RSA �Allowed for both hemi and TSA

�Golant et al. 2012 • Survey distributed to 310 members of the American Shoulder and Elbow Surgeons concerning participation in 28 different athletic activities after 5 types of shoulder arthroplasty �TSA, HA, humeral resurfacing, total shoulder resurfacing, and reverse shoulder arthroplasty) � 28 activities grouped into four categories: �Contact �Noncontact high load �Noncontact low load �Non-upper extremity sports • 74. 1% of respondents allowed some return to athletic activiites following shoulder arthroplasty

� 51% of respondents allowed participation in contact sports � 90% allowed some participation in noncontact low-load sports �Humeral resurfacing patients had highest return to sports at 92% • Reverse arthroplasty had the lowest rate at 45. 2% �TSA: 76. 5% �Hemiarthroplasty: 87. 5% �Cycling, yoga, swimming and golf had highest rates of allowed return irrespective of arthroplasty type (>90% of respondents)

Conclusions �Type of arthroplasty is dependent on the involvement of the glenoid, humerus and sufficiency of the rotator cuff • Resurfacing: replacement of humeral head/possibly glenoid • Hemiarthroplasty: replacement of humeral head and proximal humerus with glenoid resurfacing • Total shoulder: Patients with intact rotator cuff • Reverse total shoulder: Patients without sufficient rotator cuff

�Resurfacing and hemiarthroplasty usually indicated for younger, more active patients than TSA and RSA �Reverse shoulder arthroplasty has more activity modifications than TSA, HA or resurfacing �Glenoid loosening appears to be primary complication with all arthroplasties �Golf, swimming, cycling appear to be well tolerated by patients post-operatively and allowed by most physicians

References 1. ) Kaback L, Green A, Blaine T. Glenohumeral Arthritis and Total Shoulder Replacement. Medicine and Health 2012; 95 (4): 120 -124 2. ) Eichenseer P, Nowinski R, Patel D. Shoulder Hemiarthroplasty. Medscape 2011. http: //emedicine. medscape. com/article/2000818 -overview. Retrieved July 7, 2012. 3. ) Afsari A. Anterior Glenohumeral Instability. 2012. http: //emedicine. medscape. com. libproxy. lib. unc. edu/article/1262004 -overview. Retrieved July 14, 2012. 4. ) Coghlan JA, Buchbinder R, Green S, Johnston RV, Bell SN. Surgery for Rotator Cuff Disease (Review). 2009. http: //onlinelibrary. wiley. com. libproxy. lib. unc. edu/doi/10. 1002/14651858. CD 0056 19. pub 2/pdf. Retrieved July 14, 2012. 5. ) Oh LS, Wolf BR, Hall MP, Levy BA, Marx RG. Indications for Rotator Cuff Repair: A Systematic Review. Clinical Orthopaedics and Related Research. 2007; 455: 52 -63. http: //moonshoulder. com/Publications/indications%20 for%20 repair%20 systemati c%20 review. pdf

6. ) Favard L, Katz D, Colmar M, Benkalfate T, Thomazeau H, Emily S. Total shoulder arthroplasty — Arthroplasty for glenohumeral arthropathies: Results and complications after a minimum follow-up of 8 years according to the type of arthroplasty and etiology. Orthopaedics & Traumatology: Surgery & Research (2012) 98; 41 -47. 7. ) Kirkley S. Hemiarthroplasty vs. Total Shoulder Arthroplasty. San Diego Shoulder Course. San Diego, CA. Presented June 14 -17, 2000. http: //www. arthroclub. egydoc. com/sites/arthroclub/AC_Files/Articles/article 41. pdf. Retrieved July 14, 2012. 8. ) Bohsali K, Wirth M, Rockwood C. Complications of Total Shoulder Arthroplasty. The Journal of Bone & Joint Surgery. 2006; 88 (10): 2279 -2292. 9) Magnussen R, Mallon W, Willems WJ, Moorman C. Long-term activity restrictions after shoulder arthroplasty: an international survey of experienced shoulder surgeons. Journal of Shoulder and Elbow Surgery. 2011; 20: 281 -289. 10) De. Franco MJ, Walch G. Current issues in reverse total shoulder arthroplasty. The Journal of Musculoskeletal Medicine. 2011; 28 (3). http: //www. musculoskeletalnetwork. com/display/article/1145622/1815306. Retrieved July 26, 2012.
11. ) Nicholson GP, Strauss EJ, Sherman SL. Scapular Notching: Recognition and Strategies to Minimize Clinical Impact. Clinical Orthopedics and Related Research. 2010. http: //www. sportssurgerynewyork. com/articles/scapularnotching. pdf. Retrieved July 31, 2012. ) Mc. Morris M. Shoulder Complex – PHYT 732. Spring 2012. University of North Carolina – Chapel Hill. 13. ) Lewek M. Shoulder Girdle – PHYT 730. Fall 2011. University of North Carolina – Chapel Hill. 14. ) Golant A, Christoforou D, Zuckerman J, Kwon Y. Return to sports after shoulder arhtroplasty: a survey of surgeons’ preferences. Journal of Shoulder and Elbow Surgery. 2012; 21(4): 554 -560. 15) Burgess D, Mc. Grath M, Bonutti P, Marker D, Delanois R, Mont M. Shoulder Resurfacing. The Journal of Bone & Joint Surgery. 2009; 91 (5): 1228 -1238. 16. ) Bigliami L, Flatow E. The Complete Shoulder Solution. 4 -Part Fracture of the Humerus Surgical Technique. Retrieved August 7, 2012. http: //depts. washington. edu/shoulder/Surgery/Zimmerbigliani_flatow_shoulder 2. p df.
- Slides: 44