SHOULD NSTEMI be Treated Like STEMI William S

SHOULD NSTEMI be Treated Like STEMI William S. Weintraub, MD, MACC, FAHA, FESC Med. Star Washington Hospital Center Washington, DC USA

SHOULD NSTEMI be Treated Like STEMI William S. Weintraub, MD, MACC, FAHA, FESC Med. Star Washington Hospital Center Washington, DC USA COI: None

Case • It’s Friday evening 5 pm and you are called by the ER: – 84 y/o man with “prior stents” p/w new onset of chest pain x 3 h while walking to the grocery store. Pain is now subsided after administration of nitro and morphine. – Vitals: BP 110/70 HR 102 RR 12, O 2 sat 97% on RA, no signs of heart failure – Labs: Cr 1. 4, Tn 0. 2
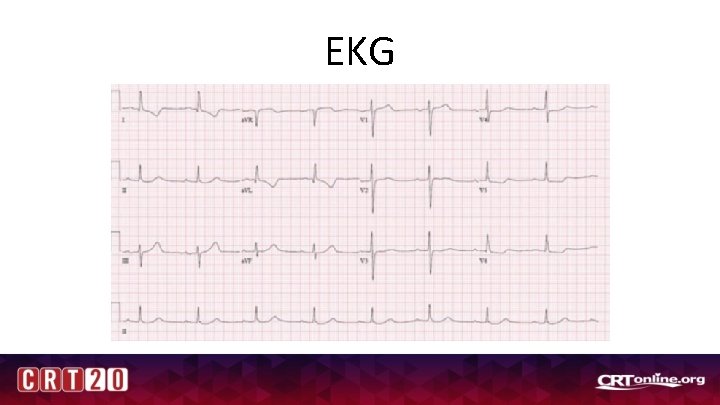
EKG
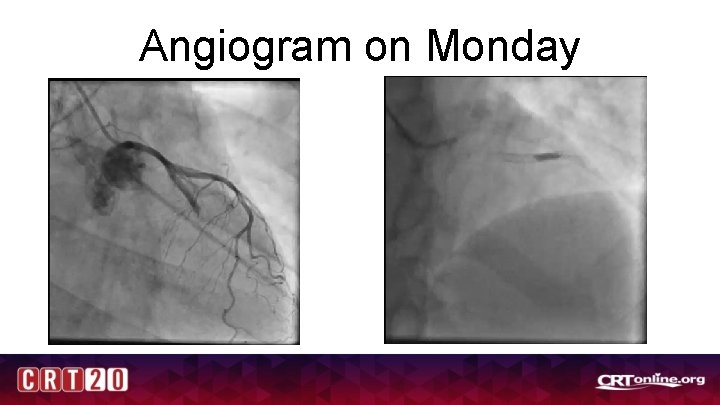
Angiogram on Monday
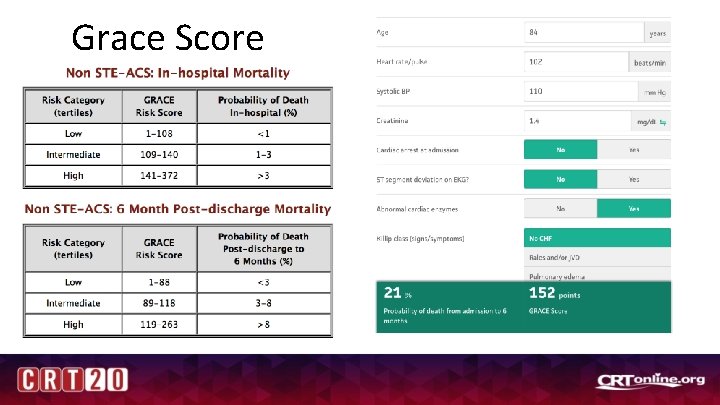
Grace Score

Acute MI • An estimated 540, 000 NSTEMI cases occur in the United States every year, including approximately 60, 000 deaths • If mortality was reduced by 25%, this would save 15, 000 lives in the United States and ~150, 000 lives worldwide every year
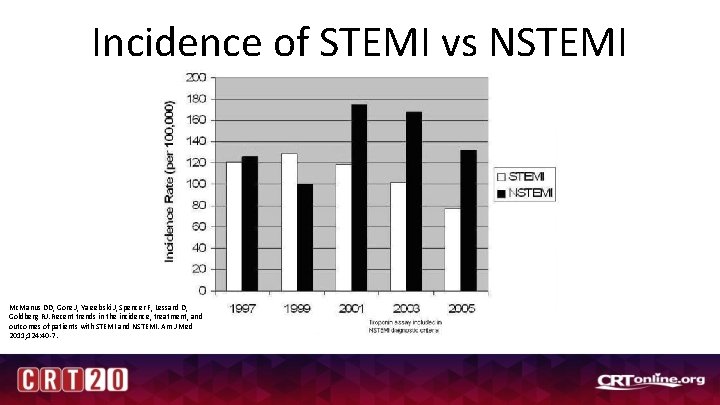
Incidence of STEMI vs NSTEMI Mc. Manus DD, Gore J, Yarzebski J, Spencer F, Lessard D, Goldberg RJ. Recent trends in the incidence, treatment, and outcomes of patients with STEMI and NSTEMI. Am J Med 2011; 124: 40 -7.
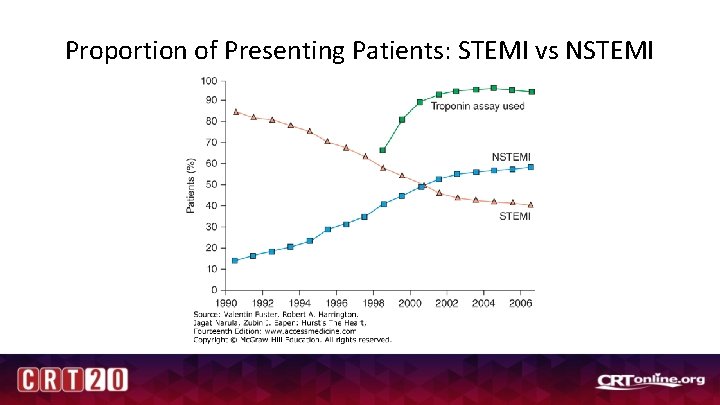
Proportion of Presenting Patients: STEMI vs NSTEMI
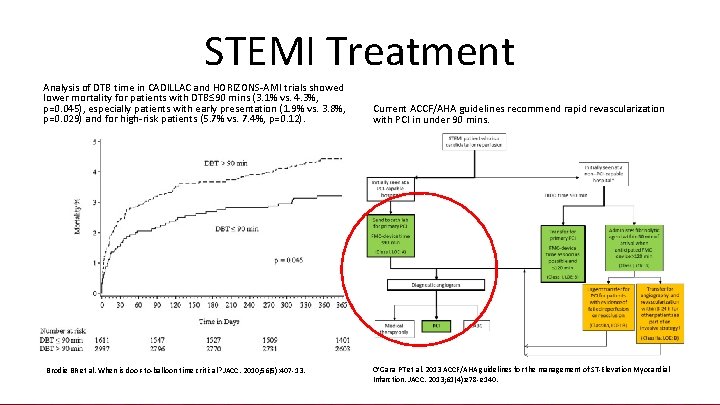
STEMI Treatment Analysis of DTB time in CADILLAC and HORIZONS-AMI trials showed lower mortality for patients with DTB≤ 90 mins (3. 1% vs. 4. 3%, p=0. 045), especially patients with early presentation (1. 9% vs. 3. 8%, p=0. 029) and for high-risk patients (5. 7% vs. 7. 4%, p=0. 12). Brodie BR et al. When is door-to-balloon time critical? JACC. 2010; 56(5): 407 -13. Current ACCF/AHA guidelines recommend rapid revascularization with PCI in under 90 mins. O’Gara PT et al. 2013 ACCF/AHA guidelines for the management of ST-Elevation Myocardial Infarction. JACC. 2013; 61(4): e 78 -e 140.
NSTEMI Patient Population • Heterogenous patients ranging from those who are stable upon presentation to those in cardiogenic shock

NSTEMI Treatment • Clinical trial data show the benefit of an invasive strategy for NSTEMI • However, the timing for an invasive approach for NSTEMI patients is largely uniform, regardless of clinical severity

ESC and ACC/AHA Guidelines Amsterdam EA, et al. 2014 J Am Coll Cardiol 2014; 64: e 139– 228. Roffi M et al. 2016. Eur Heart Journal 2016
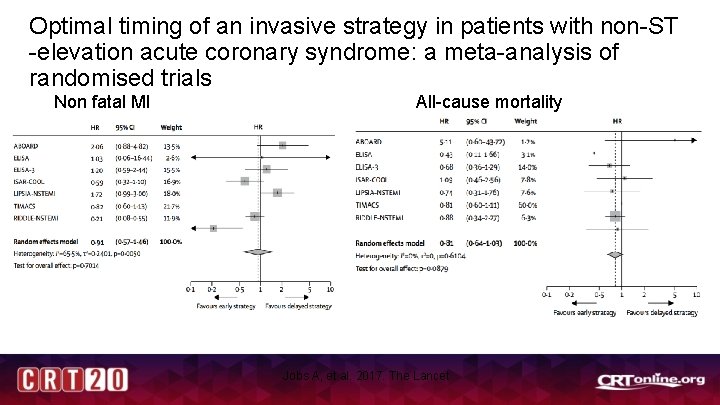
Optimal timing of an invasive strategy in patients with non-ST -elevation acute coronary syndrome: a meta-analysis of randomised trials Non fatal MI All-cause mortality Jobs A, et al. 2017. The Lancet
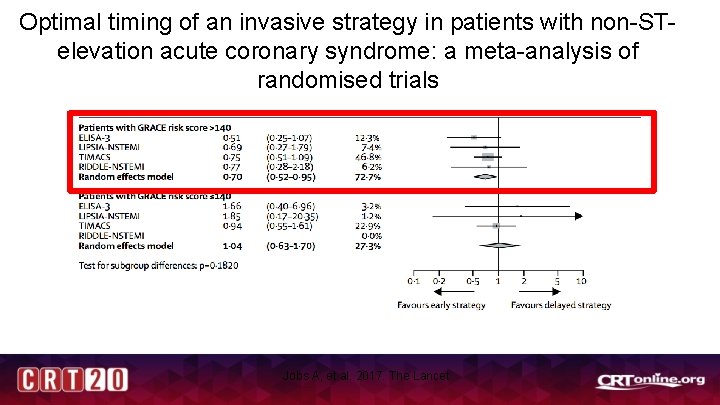
Optimal timing of an invasive strategy in patients with non-STelevation acute coronary syndrome: a meta-analysis of randomised trials Jobs A, et al. 2017. The Lancet
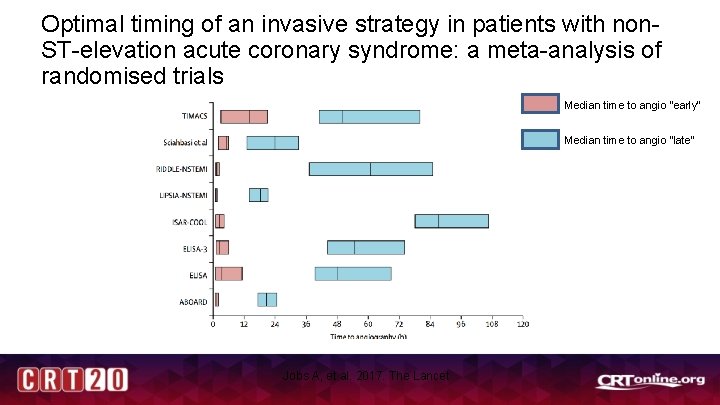
Optimal timing of an invasive strategy in patients with non. ST-elevation acute coronary syndrome: a meta-analysis of randomised trials Median time to angio “early” Median time to angio “late” Jobs A, et al. 2017. The Lancet

Circulation. 2018; 138: 2741– 2750

VERDICT Trial • Nov 2010 -June 2016 • N= 1075 ”very early invasive” • N= 1072 “standard” – Primary Outcome: -- All-cause death -- Nonfatal MI -- Hospital refractory ischemia -- Hospita for heart failure Circulation. 2018; 138: 2741– 2750
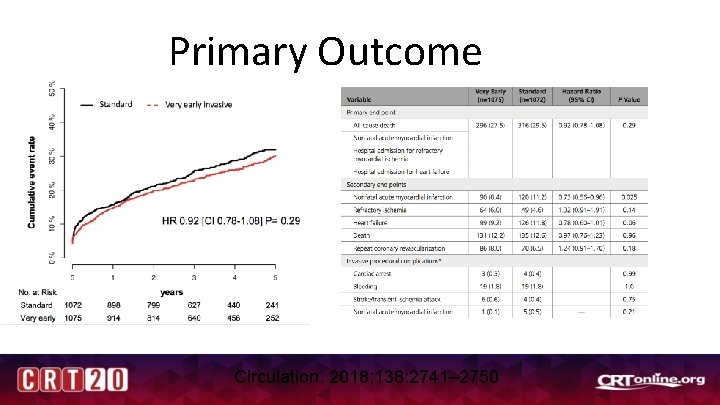
Primary Outcome Circulation. 2018; 138: 2741– 2750
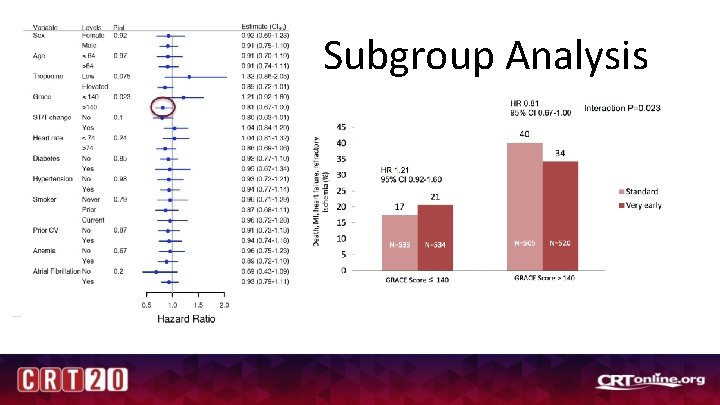
Subgroup Analysis

Time is Myocardium Not enough data for clearly defined guidelines

The Issue is Equipoise • The timing of an invasive approach remains of considerable interest • Clinical trial data are not definitive • The guidelines note that the optimum time for an invasive strategy remains uncertain

Conclusions • As underlined by the guidelines, the optimal time to intervention in patients with NSTEMI and in particular in high risk patients, is still unknown • Randomized trials are needed focused on patients with GRACE score>140 to improve outcome in the critical clinical setting
- Slides: 23