Should Clinical Indication Be Required on Prescriptions Anita

Should Clinical Indication Be Required on Prescriptions? Anita C. Murcko, MD, FACP Terri Warholak, BS Pharm, Ph. D, FAPh. A, CPHQ Michael T. Rupp, BS Pharm, Ph. D, FAPh. A

Disclosures v The speakers declare no conflicts of interest

Learning Objectives 1. Explain the benefits derived from indication-based prescribing 2. Explain the benefits of providing pharmacists with clinical indications 3. Explore the potential challenges and barriers to including the indication on prescriptions in Arizona

Learning Objective #1 Explain the benefits derived from indicationbased prescribing

What must a prescription contain in Arizona? • ARS 32 -1968 C. A prescription order shall contain: • The date it was issued • The name and address of the person for whom or owner of the animal for which the drug is ordered • Refills authorized (if any) • The legibly printed name, address and telephone number of the prescribing medical practitioner • The name, strength, dosage, form and quantity of the drug ordered • Directions for its use Is anything missing?

Safety • Prevents wrong-patient medication errors • • Galanter et al Indication-based prescribing prevents wrong-patient medication errors in computerized provider order entry. J Am Med Inform Assoc 2013; 20: 477– 481. Intercepts drug name confusion errors • Galanter WL, Bryson ML, Falck S, Rosenfield R, Laragh M, et al. (2014) Indication Alerts Intercept Drug Name Confusion Errors during Computerized Entry of Medication Orders. PLo. S ONE 9(7): e 101977. doi: 10. 1371/journal. pone. 0101977 • May avert dosing errors • Stultz et al. Sensitivity and specificity of dosing alerts for dosing errors among hospitalized pediatric patients. J Am Med Inform Assoc 2014; 21: 219– 225. • Aids recognition of prescribing errors • Kennedy et al. Evaluation of a modified prescription form to address prescribing errors. Am J Health-Syst Pharm. 2011; 68: 151 -7.

Quality • Helps identify non-evidence-based prescriptions • Walton et al. A trial of inpatient indication based prescribing during computerized order entry with medications commonly used off-label Appl Clin Inf 2011; 2: 94– 103 http: //dx. doi. org/10. 4338/ACI-2010 -11 -RA-0072 • Off-label use can increase adverse effects • Eguale et al. Association of Off-label Drug Use and Adverse Drug Events in an Adult Population. JAMA Intern Med. 2016; 176(1): 55 -63. • Reduces utilization of “never-indicated” drugs • Samore et al. Clinical Decision Support and Appropriateness of Antimicrobial Prescribing: A Randomized Trial. JAMA. 2005; 294: 2305 -2314. • Improves appropriate use • Litvin et al. Use of an electronic health record clinical decision support tool to improve antibiotic prescribing for acute respiratory infections: The ABX-TRIP study. J Gen Intern Med 28(6): 810– 6

Efficiency and Workflow • Reduces calls from pharmacy Warholak et al. Assessing the effect of providing a pharmacist with patient diagnosis on electronic prescription orders: A pilot study. Research in Social and Administrative Pharmacy. 2014; 10: 246 -251. PMID: 23688539 • • Improves health problem list documentation • • • Eguale et al. Enhancing pharmacosurveillance with systematic collection of treatment indication in electronic prescribing: a validation study in Canada. Drug Safety. 2010; 33(7): 559 -567. PMID: 20553057 Galanter et al Indication-based prescribing prevents wrong-patient medication errors in computerized provider order entry. J Am Med Inform Assoc 2013; 20: 477– 481. Galanter WL, Bryson ML, Falck S, Rosenfield R, Laragh M, et al. (2014) Indication Alerts Intercept Drug Name Confusion Errors during Computerized Entry of Medication Orders. PLo. S ONE 9(7): e 101977. doi: 10. 1371/journal. pone. 0101977

Summary of benefits • Improve medication safety • Better educate and empower patients about medications • Improve health care team communication (physicians, pharmacists, patients, family, home care nurses) • Facilitate medication reconciliation • Increase speed and efficiency of prescribing by presenting drug choices for that indication • Improve documentation of health problem list • Improve appropriate use of medications by prescribers • Facilitate reimbursement coding, streamline prior authorization process • Support quality, outcomes, and effectiveness research Schiff G, Seoane-Vazquez E, Wright A. Incorporating indications into medication ordering: Time to enter the age of reason. N Engl J Med. 2016; 375(4): 306 -309. doi: 10. 1056/NEJMp 1603964

Learning Objective #2 Explain the benefits of providing pharmacists with clinical indication

What is the role of the pharmacist?

Omnibus Reconciliation Act of 1990 (OBRA 90) • Section 4401 1. Prospective drug utilization review (Pro. DUR) 2. Counseling obligations 3. Record-keeping mandates

OBRA ‘ 90 Pro. DUR Requirements • The review shall include screening for potential drug therapy problems due to: • Therapeutic duplication • Drug-disease contraindications • Drug-drug interactions • Incorrect drug dosage or duration • Drug-allergy interactions • Clinical abuse / misuse Omnibus Budget Reconciliation Act of 1990 (OBRA ‘ 90)

Warholak TL, Zale A, Brandon M, Park S, Rupp MT. Check it out: A practical approach for improving medication safety. Journal of the American Pharmacists Association. 2015; 55: 621– 625. doi: 10. 1331

Arizona Administrative Code, Title 4, Ch. 23 – Board of Pharmacy • ARS 32 -1904 • R 4 -23 -402 Pharmacist, Graduate Intern, and Pharmacy Intern • A. A pharmacist or graduate intern or pharmacy intern under the supervision of a pharmacist shall perform the following professional practices in dispensing a prescription medication from a prescription order: • 3. Obtain, or assume responsibility to obtain, from the patient, patient’s agent, or medical practitioner and record, or assume responsibility to record, in the patient’s profile: • b. individual history including known diseases and medical conditions. . . • 6. verify that a dosage is within proper limits • 7. interpret the prescription order, which includes exercising professional judgment in determining whether to dispense a particular prescription

Effect of Patient Information on the Quality of Pharmacists’ Drug Use Review Decisions Information Level 1 Level 2 Level 3 Level 4 Legal Rx + + Med. Profile + + + Diagnosis + + Encounter Form + Warholak-Juarez T, Rupp MT, Salazar TA, Foster S. The effect of patient information on pharmacists’ drug use review decisions. Journal of the American Pharmacists Association. 2000; 40: 500 -8. PMID: 10932459.
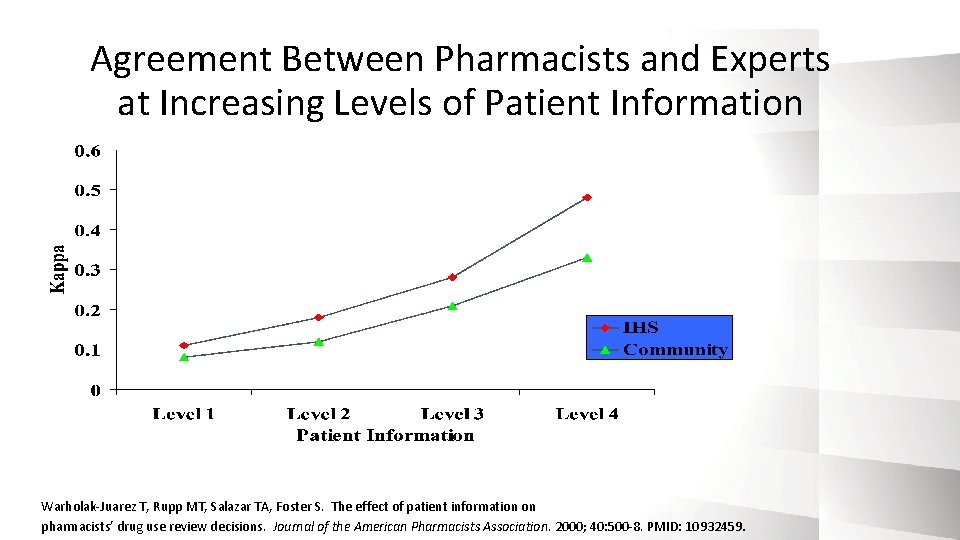
Agreement Between Pharmacists and Experts at Increasing Levels of Patient Information Warholak-Juarez T, Rupp MT, Salazar TA, Foster S. The effect of patient information on pharmacists’ drug use review decisions. Journal of the American Pharmacists Association. 2000; 40: 500 -8. PMID: 10932459.
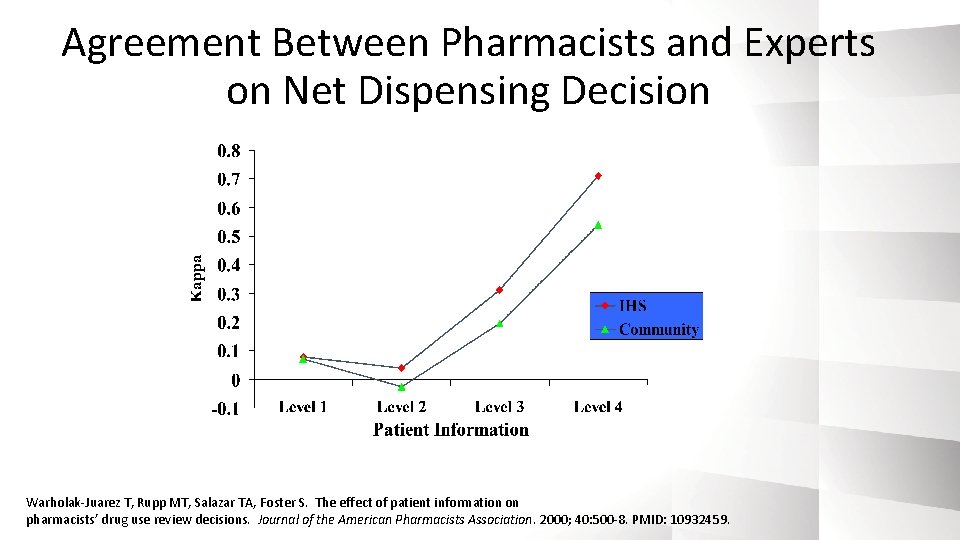
Agreement Between Pharmacists and Experts on Net Dispensing Decision Warholak-Juarez T, Rupp MT, Salazar TA, Foster S. The effect of patient information on pharmacists’ drug use review decisions. Journal of the American Pharmacists Association. 2000; 40: 500 -8. PMID: 10932459.

Assessing the effect of providing pharmacists with patient diagnosis on electronic prescription orders: A pilot study • Pharmacist intervention rates on e-prescription orders were significantly lower after adding patient diagnosis to the e-prescription • 3. 9% pre- vs. 1. 0% post- (p< 0. 001) Warholak TL, Rupp MT, Leal S, Kurniawan G, Patel N. Assessing the effect of providing a pharmacist with patient diagnosis on electronic prescription orders: A pilot study. Research in Social and Administrative Pharmacy. 2014; 10: 246 -251. PMID: 23688539

International Experience Canada: built into system (MOXXI) Spain: developing database associating indication, diagnosis (when available) and prescription UK: best practice recommendation Netherlands: required for high risk medications Belgium: required for discharge prescriptions for transitions from inpatient setting Australia: ~13% of hospital prescriptions include indication China: Some hospitals require Dx in CPOE with every script Computerized Physician Order Entry (CPOE)

Learning Objective #3 Explore the potential challenges and barriers to including indication on prescriptions in Arizona

What do pharmacists say would help them do their job better? • Ideal – Access to all patient information that was considered by the prescriber • Adequate - Clinical information relevant to the appropriateness of the prescribed medication therapy • Minimal - Why the medication is being prescribed • • • Diagnosis Indication Problem Reason Purpose Therapeutic objective

Organizations Endorsing the Inclusion of Diagnosis or Indication on Prescriptions • NCC MERP (1997) – “Prescriptions should include a brief notation of purpose (e. g. , for cough) unless considered inappropriate by the prescriber” • ISMP (2001) – “A current written diagnosis or identified need and relevant diagnostic data must support medication orders” (Michael Cohen) • APh. A (2001) – “APh. A supports the inclusion of the diagnosis or indication for use for which the medication is ordered (updated from 1993 resolution) • NABP (2004) – “National and state medical associations and other interested parties should support legislation and regulatory efforts in the states to require prescribers to include the indication for the medication on all prescription and medication orders issued orally, in writing or transmitted electronically” • NCPDP (2016) – “A current written diagnosis or identified need and relevant diagnostic data must support medication orders”
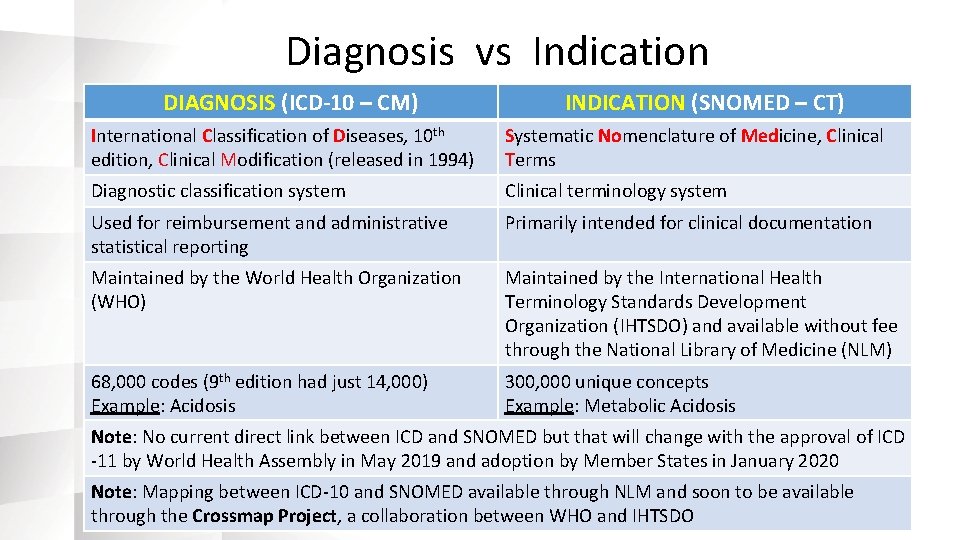
Diagnosis vs Indication DIAGNOSIS (ICD-10 – CM) INDICATION (SNOMED – CT) International Classification of Diseases, 10 th edition, Clinical Modification (released in 1994) Systematic Nomenclature of Medicine, Clinical Terms Diagnostic classification system Clinical terminology system Used for reimbursement and administrative statistical reporting Primarily intended for clinical documentation Maintained by the World Health Organization (WHO) Maintained by the International Health Terminology Standards Development Organization (IHTSDO) and available without fee through the National Library of Medicine (NLM) 68, 000 codes (9 th edition had just 14, 000) Example: Acidosis 300, 000 unique concepts Example: Metabolic Acidosis Note: No current direct link between ICD and SNOMED but that will change with the approval of ICD -11 by World Health Assembly in May 2019 and adoption by Member States in January 2020 Note: Mapping between ICD-10 and SNOMED available through NLM and soon to be available through the Crossmap Project, a collaboration between WHO and IHTSDO
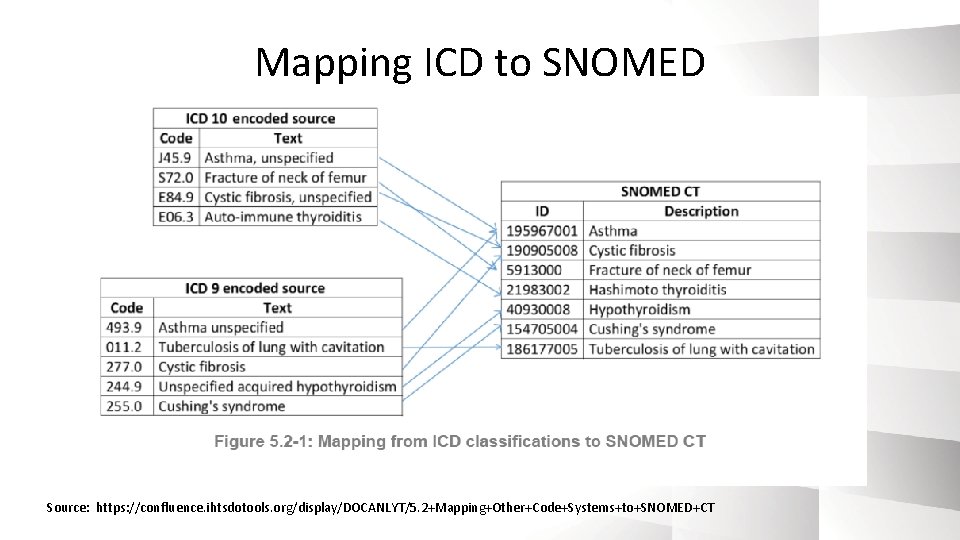
Mapping ICD to SNOMED Source: https: //confluence. ihtsdotools. org/display/DOCANLYT/5. 2+Mapping+Other+Code+Systems+to+SNOMED+CT

Using Natural Language Processing to encode SNOMED from encounter documentation Source: https: //confluence. ihtsdotools. org/display/DOCANLYT/5. 1+Natural+Language+Processing

Barriers Eliminated • Internationally recognized and widely used coding terminologies are now available for the accurate and efficient communication of either diagnosis or indication • Electronic prescribing is now the rule (77%) and NCPDP’s SCRIPT telecommunications standard supports the transmission of both diagnosis (ICD) and Indication (SNOMED-CT) • Mapping algorithms enable either ICD or SNOMED-CT to be used interchangeably with virtually no loss of clinical information • Advances in natural language processing allow for accurate encoding of clinical indication from providers’ encounter documentation, thereby minimizing or eliminating the time and expense of coders

Remaining Barriers and Possible Solutions?

Please tell us what YOU think! https: //uarizona. co 1. qualtrics. com/jfe/form /SV_bjbh. F 6 UNdjm. R 0 r. P
- Slides: 29