SHORT BOWEL SYNDROME TOM THOMAS MATHEW 2002 BATCH
SHORT BOWEL SYNDROME TOM THOMAS MATHEW 2002 BATCH

DEFINITION • A GROUP OF SIGNS AND SYMPTOMS THAT RESULT FROM A SMALL BOWEL LENGTH THAT IS INADEQUATE TO SUPPORT NUTRITION.

AETIOLOGY ADULTS 1. CROHNS DISEASE 2. MESENTERIC ISHEMIA 3. MALIGNANCY 4. RADIATION ENTERITIS 5. TUBERCULOSIS 6. MULTIPLE FISTULAS TB INTESTINE
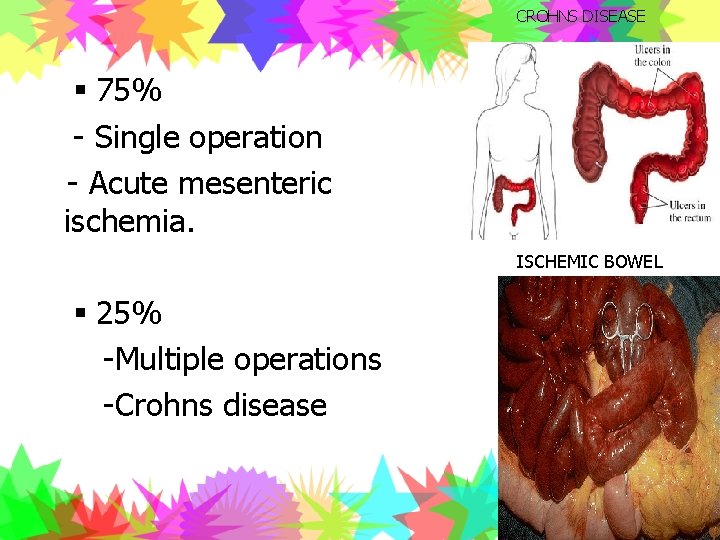
CROHNS DISEASE § 75% - Single operation - Acute mesenteric ischemia. ISCHEMIC BOWEL § 25% -Multiple operations -Crohns disease
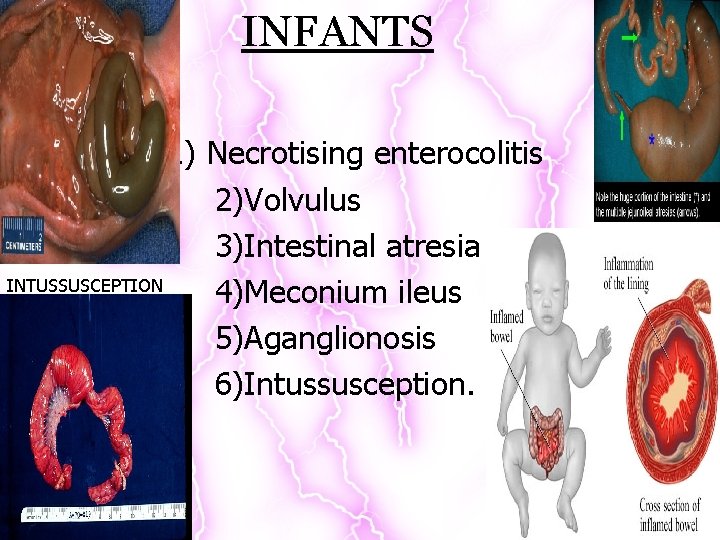
INFANTS 1) Necrotising enterocolitis 2)Volvulus 3)Intestinal atresia INTUSSUSCEPTION 4)Meconium ileus 5)Aganglionosis 6)Intussusception.

PATHOPHYSIOLOGY • Resection of less than 50%- tolerated • Length of bowel and site –important • Intact colon, iliocaecalvalve, terminal illeum-70% resected

• Colon-absorb large amount of fluid and electrolyte. • illeocecal valve – - delay transit time. - colonization by colonic bacteria. • Terminal illeum- bile salt and vitamin. B 12 -specific

• Divided into three clinical stages 1. Acute phase 2. Adaptive phase 3. Chronic phase

ACUTE PHASE • From recovery of postoperative ileus to 4 weeks • Profuse watery diarrhoea(5 to 10 L) - Acute loss of surface area - Rapid intestinal transit

• Severe - illeocaecal value or colon is resected. • Hypergastrinemia-- Diarrhoea 1. Hypersecretion. 2. Steatorrhea - pancreatic lipase 3. Acid enteritis

• Delayed gastric emptying –Vomiting and nasogastric aspiration. • Acute peptic ulceration may develop • Adequate fluid and electrolyte should be given • With proper nutrition the patient will survive to enter the adaptive stage

ADAPTIVE PHASE • • • It takes upto 2 years More effective in illeum than jejunum Attempt to increase the surface area. Increase in the circumference of intestine. Only minimal increase in length Villous height

• • depth of crypts. number of crypts. total mucosal turnover rate. migration of epithelial cell from crypt bases to tip of villi • Age of individual cell is unaffected.

FACTORS RESPONSIBLE FOR ADAPTATION • Luminal nutrients. • Trophic gut hormones 1. Gastrin 2. CCK and secretin 3. Neurotensin – Most potent 4. Peptide y 5. Bombesin. GASTRIN NEUROTENSIN

• Pancreatic and biliary secretions GROWTH HORMONE • Gut derived peptides- GLP-2 • Dietary fibre -Increase stool acidity -increase colonic absorption • Other hormones - Growth hormone - Insulin like growth factor.

CHRONIC PHASE • • • Begins after the adaptive changes occur Unstable Easily disturbed by minor illness Acute disturbances may develop Deficiencies should be recognised and should be treated.

Factors Affecting Severity of Malabsorption, Number of Complications, and Dependence on Parenteral Nutrition • Loss of ileum, especially distal one third • Length of remaining small intestine • Loss of ileocecal valve

• Loss of colon • Disease in remaining segments of gastrointestinal tract • Coexisting malnutrition

SBS Induced Malnutrition • Fat soluble nutrients and vitamins -poorly absorbed • Water soluble vitamin deficiencies - rare.
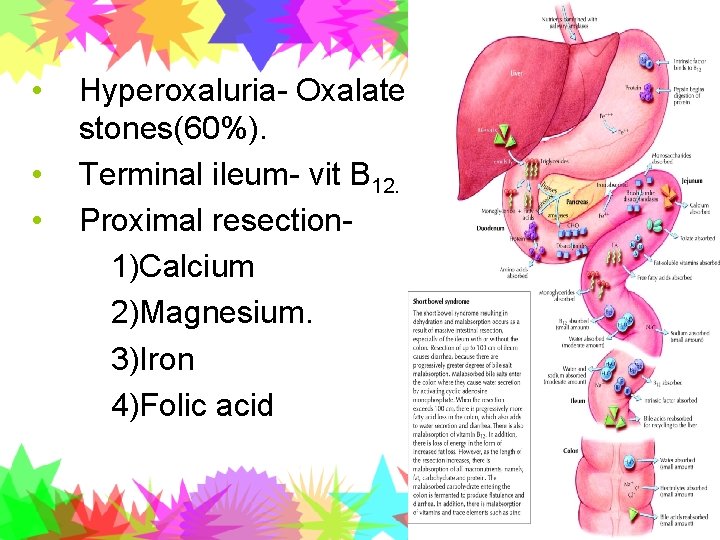
• • • Hyperoxaluria- Oxalate stones(60%). Terminal ileum- vit B 12. Proximal resection 1)Calcium 2)Magnesium. 3)Iron 4)Folic acid

• • • CLINICAL FEATURES Diarrhea Steatorrhoea Weight loss Fluid and Electrolyte deficiency Nutritional Deficiency

COMPLICATIONS • Gastric hypersecretion - Proximal resection(common) - Basal acid secretion. - Clearance of gastrin. • Cholesterol and Pigment stones -Due to reduced bile salt pool
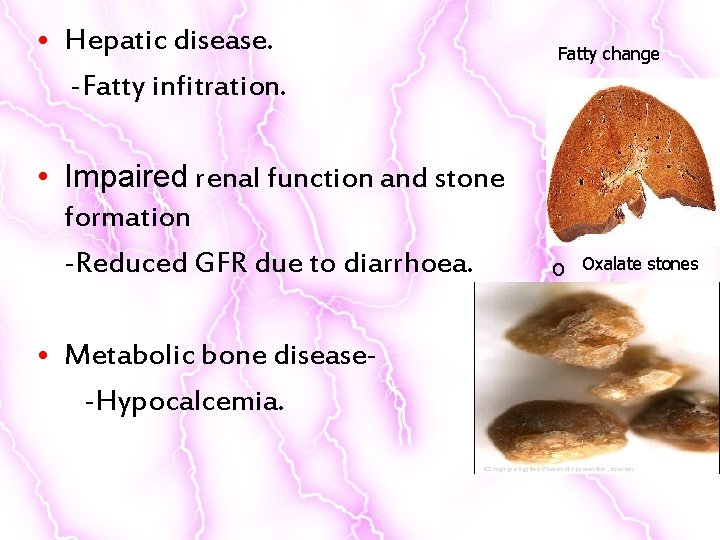
• Hepatic disease. -Fatty infitration. • Impaired renal function and stone formation -Reduced GFR due to diarrhoea. • Metabolic bone disease-Hypocalcemia. Fatty change O Oxalate stones

DIAGNOSIS • Clinical features and knowledge of extent of bowel resection

TEST OF MALABSORPTION • Assessment of severity 1) Estimation of faecal fat >6 g per day – abnormal 2) Breath test for carbohydrate malabsorption -Oral administration of 14 C-lactose -Breath is analysed for 14 CO 2

3) Bile absorption test. -ability of terminal illeum to absorb bile acid. STEPS - A dose of 17 Se labelled synthetic bile is administered orally or iv - A gamma counter measures absorption.

4)Hydrogen breath test -Measure small bowel transit time -Repeated measurements of the hydrogen in the end expiratory air are taken every few minutes after ingestion of meal.

Schilling test -To assess the absorption of vit. B 12 STEPS - Parenteral injection of unlabelled vitamin. B 12 - Radiolabelled Vit. B 12(0. 1 microgram)orally. Normal-excretion of 10% or more in urine.

TREATMENT • Important principle is prevention. • Intestinal viability doutful - smallest possible resection. - second look operation(24 h)

• Crohn, s disease – limited resections. • Treatment divided into TPN 1) Early phase 2) Late phase Early phase AIM 1)Control of diarrhea 2)Replacement of fluid and electrolyte 3)Prompt institution of TPN
• Output and input measurement. • Adequate replacement. • Control of diarrhea 1) Codeine, Diphenoxylate 2) H 2 receptor antagonists. 3) Cholestyramine 4) Octreotide

Late phase • Enteral nutrition should be started as soon as patient recovers from acute phase • Enteral nutrition -adaptation begin early. • Enteral diet are elemental(vivonex) or polymeric(isocal) • Milk products- avoided.

• Diet should begin at isoosmolar concentration and in small volume • As gut adapts osmolality, volume and caloric content should be increased. • Combination of Glutamine, GH and modified oral diet is efficious. • Typical diet –High carbohydrate, high protein and low fat. • Fat in the form of medium chain fattyacid.

• Antacids avoided • Vitamins especially fat soluble and calcium. magnesium and zinc should be supplemented.

SURGICAL METHODS • AIM - Increase the length - Delay transit 1)REVERSED INTESTINAL SEGMENT - Optimum length- 10 cm -Delay transit and increase absorption

LONGITUDINAL INTESTINAL LENGTHENING AND TAILORING (LILT) • • First described by Bianchi in 1980 Dilatation and ineffective peristalsis corrected. Double the intestinal length. Ideal in paediatric patients.
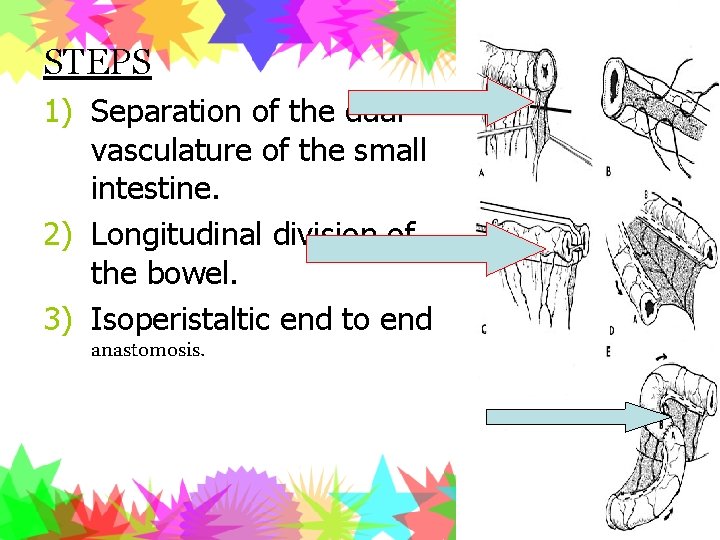
STEPS 1) Separation of the dual vasculature of the small intestine. 2) Longitudinal division of the bowel. 3) Isoperistaltic end to end anastomosis.

SERIAL TRANSVERSE ENTEROPLASY PROCEDURE(STEP) • Lengthening of dilated small bowel. § Dual vasculature not separated. Serial Transverse Enteroplasty (STEP) can lengthen the bowel in some patients. The surgeons make multiple incisions into a short, dilated segment to create a longer, thinner segment of intestine. Although the new segment is initially a zig zag in shape, it becomes straight as it heals.
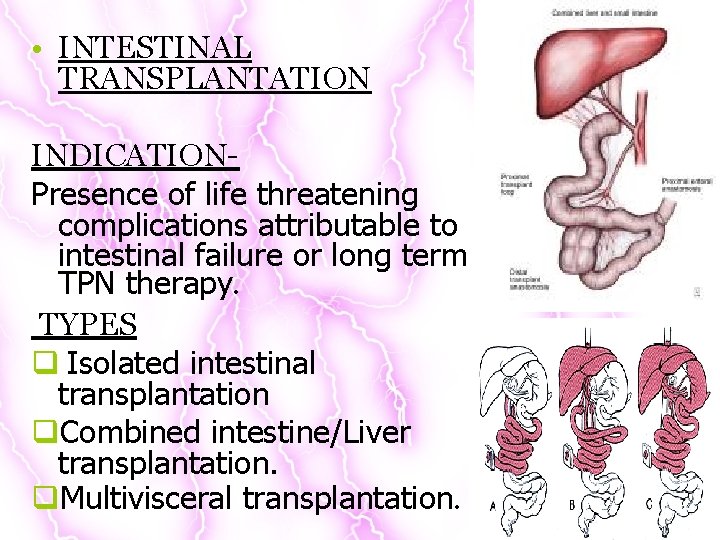
• INTESTINAL TRANSPLANTATION INDICATIONPresence of life threatening complications attributable to intestinal failure or long term TPN therapy. TYPES q Isolated intestinal transplantation q. Combined intestine/Liver transplantation. q. Multivisceral transplantation.

COMPLICATIONS 1)REJECTION 2)CMV INFECTION 3)Lympho proliferative d/s

OTHER SURGICAL METHODS • Interposition of colon between small segments of small bowel. • Construction of valves. • Electrical pacing of small intestine
NEWER TECHNIQUES • GLP-2 • GLUTAMINE, GH WITH MODIFIED HIGH CARBOHYDRATE DIET. • STEM CELL TRANSPLANTATION. GH AND GLUTAMINE
OUTCOME LIFE LONG TPN(ADULTS) Intact colon absent-<100 cm Intact colon -<60 cm • 50% TO 70% patients achieve independence from TPN. • Prognosis is better among paediatric patients.

SUMMARY • Total small bowel length that is in adequate to support nutrition • Cause include crohn’s disease, acute mesenteric ischaemia in adults and necrotizing enterocolitis in infants
• Diagnosis on the basis on symptoms and on the extent of resection. TREATMENT • TPN, replacement of fluids and electrolytes, control of diarrhoea in the initial stage • Parenteral nutrition and gradually increasing enteral feed in the later stage.

THANK YOU
- Slides: 46