SHOCK IN THE OBSTETRIC PATIENT WILLIAM SCHNETTLER MD

SHOCK IN THE OBSTETRIC PATIENT WILLIAM SCHNETTLER, MD FACOG @WSCHNETTLER #TRIHEALTHCRITICALCAREOB

Next Events: - October 16, 2017 CCOB Team Meeting 5 pm GSH - February 24, 2018 CCOB #3 (GSH)

CRITICAL CARE OBSTETRIC WORKSHOP SERIES DISCLOSURES None

CRITICAL CARE OBSTETRIC WORKSHOP SERIES Learning Objectives: • Scope of the Problem • Pathophysiology of Shock • Types of Shock • Management of Shock in Pregnancy

CRITICAL CARE OBSTETRIC WORKSHOP SERIES Scope of the Problem • MMR (Maternal Mortality Ratio) = # Maternal Deaths / 100, 000 live births (per year) • Worldwide – MMR dropped 2. 3% annually from 1990 -2015 (216/100, 000 L. B’s. ) • U. S. – 1. 7% annual increase (17. 2/100, 000 L. B’s. ) • Tri. Health – equates to potentially 1 -2 per year • Attributable Factors • Increased: Maternal Age, BMI, Co-Morbidities • Race (Non-Hispanic Black Women)
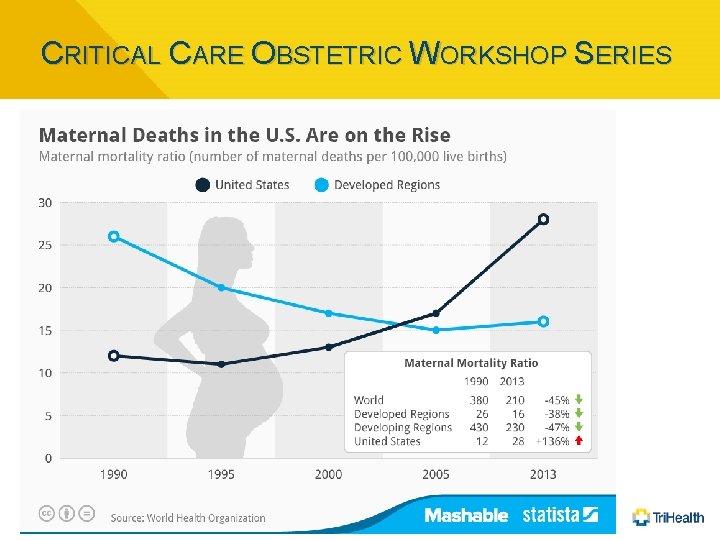
CRITICAL CARE OBSTETRIC WORKSHOP SERIES
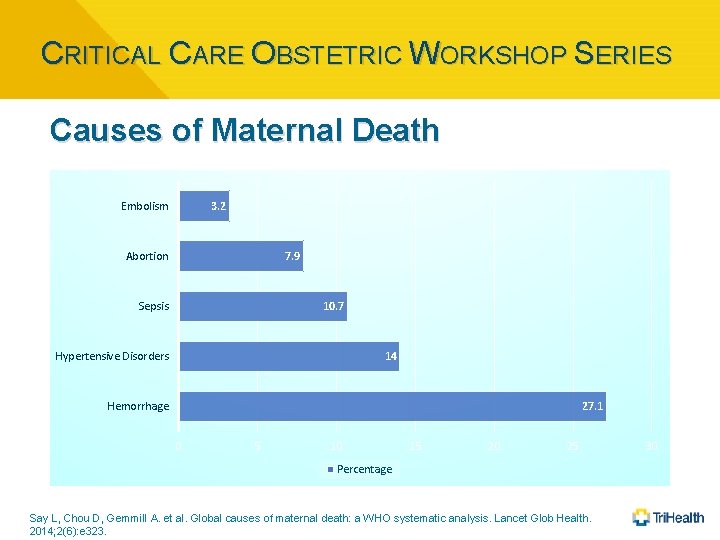
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Causes of Maternal Death Embolism 3. 2 Abortion 7. 9 Sepsis 10. 7 Hypertensive Disorders 14 Hemorrhage 27. 1 0 5 10 15 20 25 Percentage Say L, Chou D, Gemmill A. et al. Global causes of maternal death: a WHO systematic analysis. Lancet Glob Health. 2014; 2(6): e 323. 30

ICU Admissions Pregnancy-related • 0. 07 -0. 89% of all live births ~ 10 -90 / year @ Tri. Health • > 50% due to hemorrhage & hypertensive disorders • Mortality rate = 8. 4%

PATHOPHYSIOLOGY OF SHOCK
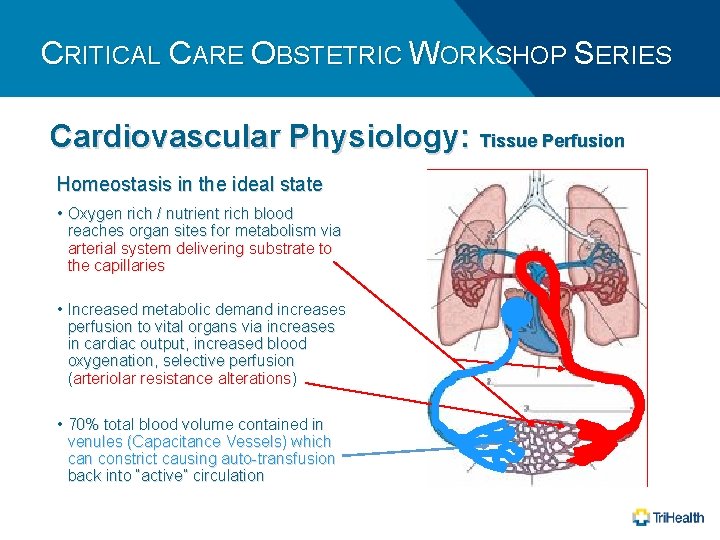
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Cardiovascular Physiology: Tissue Perfusion Homeostasis in the ideal state • Oxygen rich / nutrient rich blood reaches organ sites for metabolism via arterial system delivering substrate to the capillaries • Increased metabolic demand increases perfusion to vital organs via increases in cardiac output, increased blood oxygenation, selective perfusion (arteriolar resistance alterations) • 70% total blood volume contained in venules (Capacitance Vessels) which can constrict causing auto-transfusion back into “active” circulation
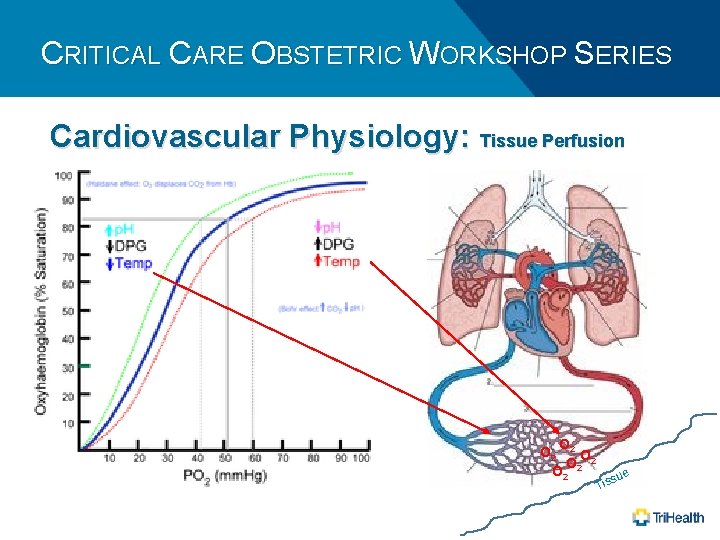
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Cardiovascular Physiology: Tissue Perfusion O O 2 2 Tis sue

CRITICAL CARE OBSTETRIC WORKSHOP SERIES Shock = inability to maintain this homeostasis Cellular Respiration Tissue perfusion Local tissue hypoxia Cell & mitochondrial death Multi-organ failure Death
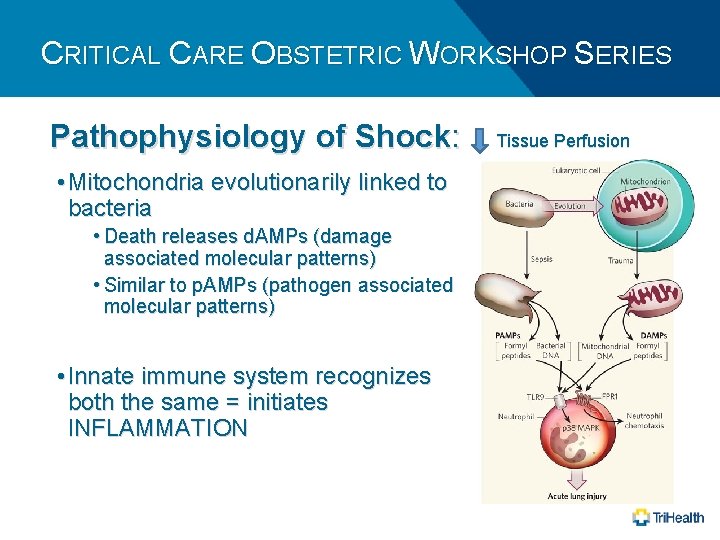
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Pathophysiology of Shock: • Mitochondria evolutionarily linked to bacteria • Death releases d. AMPs (damage associated molecular patterns) • Similar to p. AMPs (pathogen associated molecular patterns) • Innate immune system recognizes both the same = initiates INFLAMMATION Tissue Perfusion
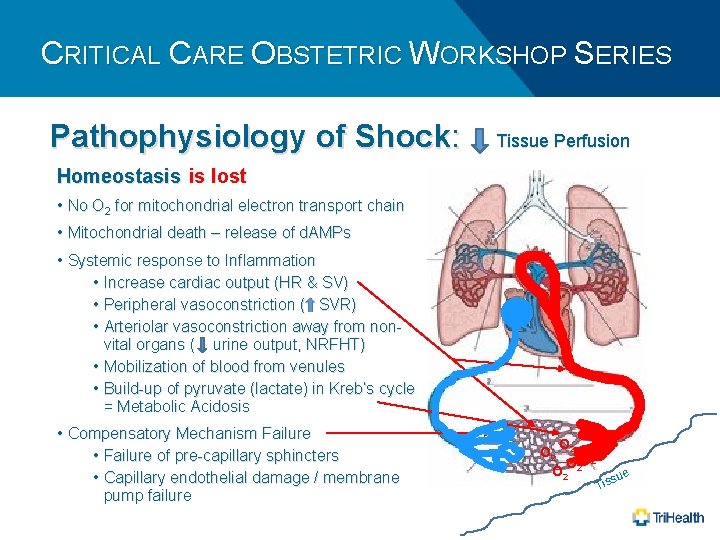
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Pathophysiology of Shock: Tissue Perfusion Homeostasis is lost • No O 2 for mitochondrial electron transport chain • Mitochondrial death – release of d. AMPs • Systemic response to Inflammation • Increase cardiac output (HR & SV) • Peripheral vasoconstriction ( SVR) • Arteriolar vasoconstriction away from nonvital organs ( urine output, NRFHT) • Mobilization of blood from venules • Build-up of pyruvate (lactate) in Kreb’s cycle = Metabolic Acidosis • Compensatory Mechanism Failure • Failure of pre-capillary sphincters • Capillary endothelial damage / membrane pump failure O O 2 2 Tis sue

CRITICAL CARE OBSTETRIC WORKSHOP SERIES Pathophysiology of Shock

CRITICAL CARE OBSTETRIC WORKSHOP SERIES Stages of Shock (Signs & Symptoms) • Pre-Shock (compensated) • Appropriate compensatory mechanisms are still homeostatic • Tachycardia • Modest change in BP • Shock (compensatory mechanisms become overwhelmed) • Signs & Symptoms of organ dysfunction • Symptomatic tachycardia • Dyspnea • Restlessness • Hypotension • Oliguria • Cool clammy skin • End-organ Dysfunction • • • Irreversible organ damage Multi-organ failure (anuria, acute renal failure, acidemia, recalcitrant hypotension) Obtundation, coma, death

TYPES OF SHOCK
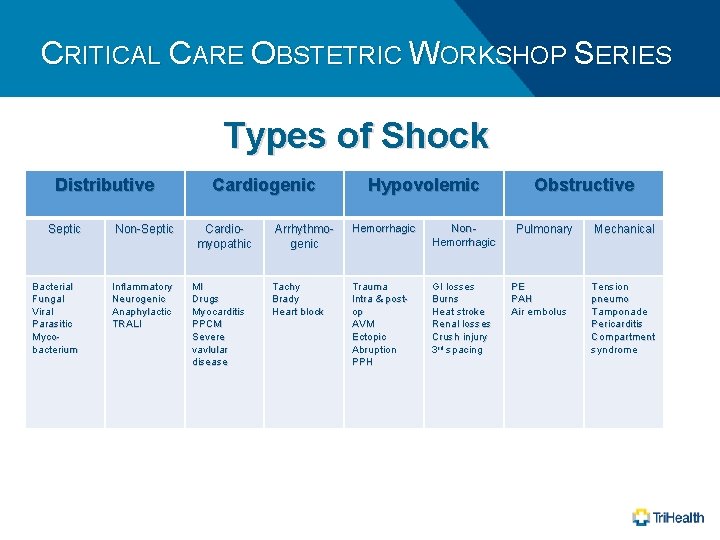
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Types of Shock Distributive Septic Bacterial Fungal Viral Parasitic Mycobacterium Non-Septic Inflammatory Neurogenic Anaphylactic TRALI Cardiogenic Cardiomyopathic MI Drugs Myocarditis PPCM Severe vavlular disease Hypovolemic Arrhythmogenic Hemorrhagic Non. Hemorrhagic Tachy Brady Heart block Trauma Intra & postop AVM Ectopic Abruption PPH GI losses Burns Heat stroke Renal losses Crush injury 3 rd spacing Obstructive Pulmonary PE PAH Air embolus Mechanical Tension pneumo Tamponade Pericarditis Compartment syndrome
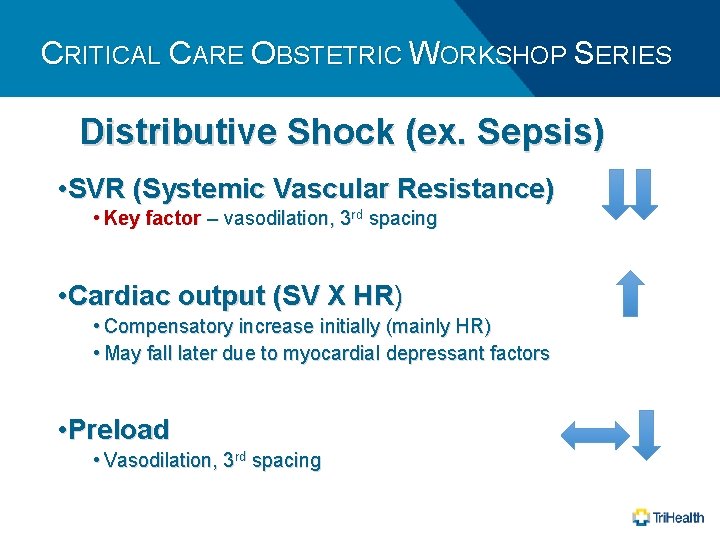
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Distributive Shock (ex. Sepsis) • SVR (Systemic Vascular Resistance) • Key factor – vasodilation, 3 rd spacing • Cardiac output (SV X HR) • Compensatory increase initially (mainly HR) • May fall later due to myocardial depressant factors • Preload • Vasodilation, 3 rd spacing

CRITICAL CARE OBSTETRIC WORKSHOP SERIES Pulse Pressure TOO SLOW < 40 MPH TOO FAST > 80 MPH
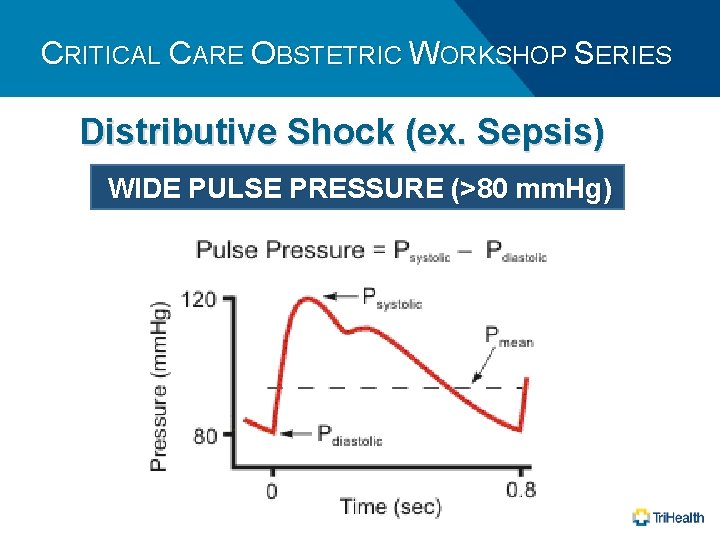
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Distributive Shock (ex. Sepsis) WIDE PULSE PRESSURE (>80 mm. Hg)
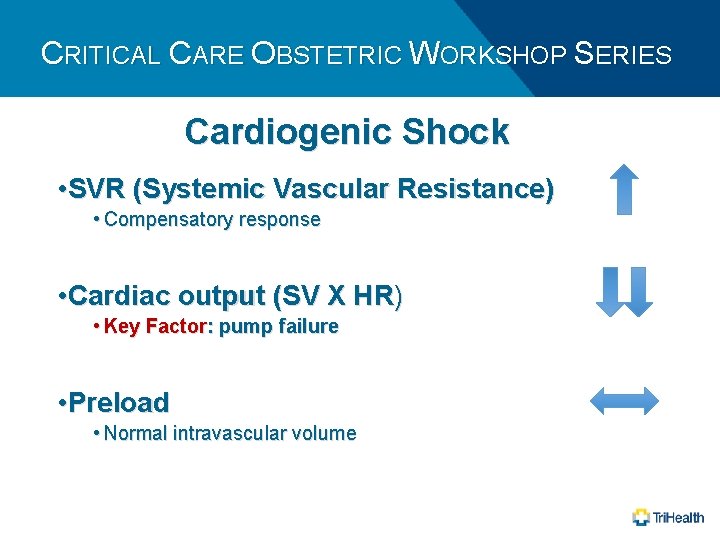
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Cardiogenic Shock • SVR (Systemic Vascular Resistance) • Compensatory response • Cardiac output (SV X HR) • Key Factor: pump failure • Preload • Normal intravascular volume
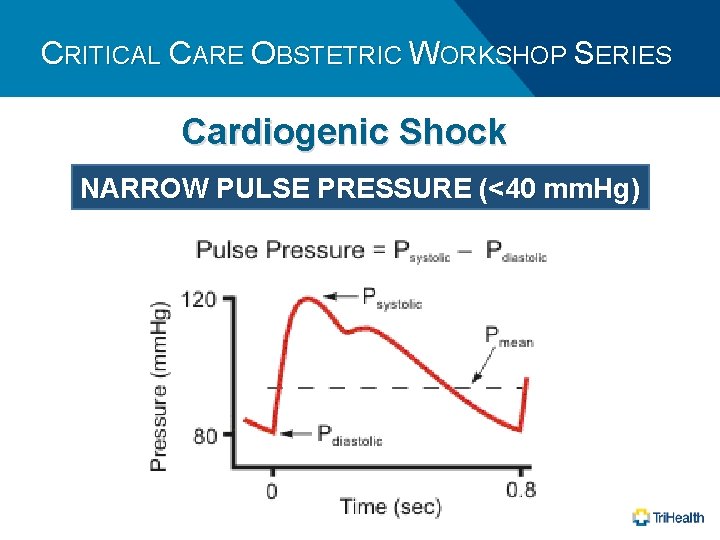
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Cardiogenic Shock NARROW PULSE PRESSURE (<40 mm. Hg)
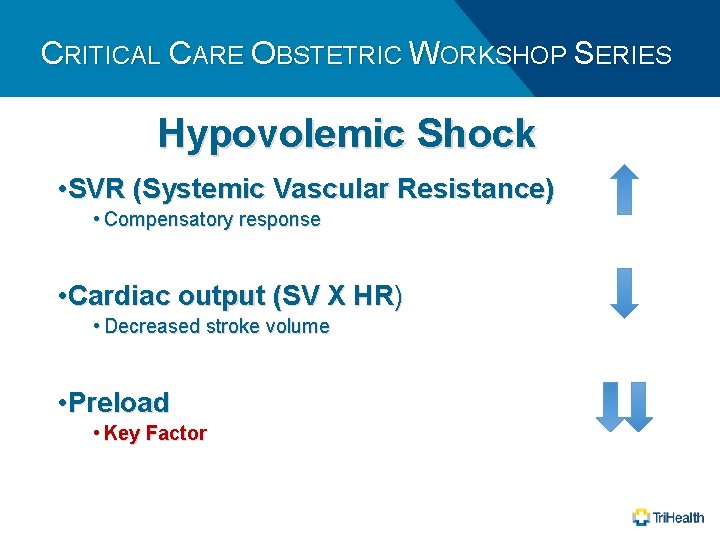
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Hypovolemic Shock • SVR (Systemic Vascular Resistance) • Compensatory response • Cardiac output (SV X HR) • Decreased stroke volume • Preload • Key Factor
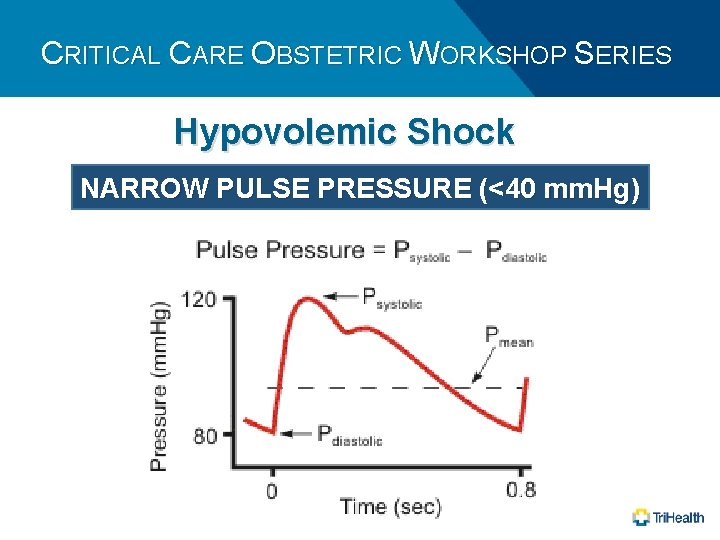
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Hypovolemic Shock NARROW PULSE PRESSURE (<40 mm. Hg)
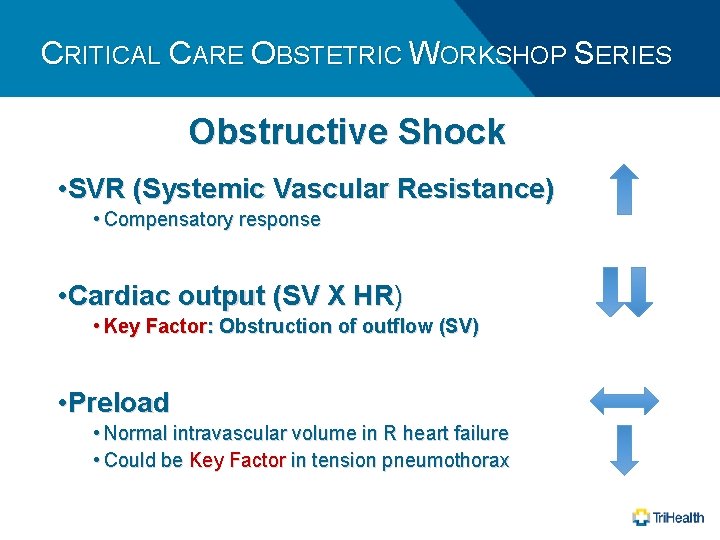
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Obstructive Shock • SVR (Systemic Vascular Resistance) • Compensatory response • Cardiac output (SV X HR) • Key Factor: Obstruction of outflow (SV) • Preload • Normal intravascular volume in R heart failure • Could be Key Factor in tension pneumothorax
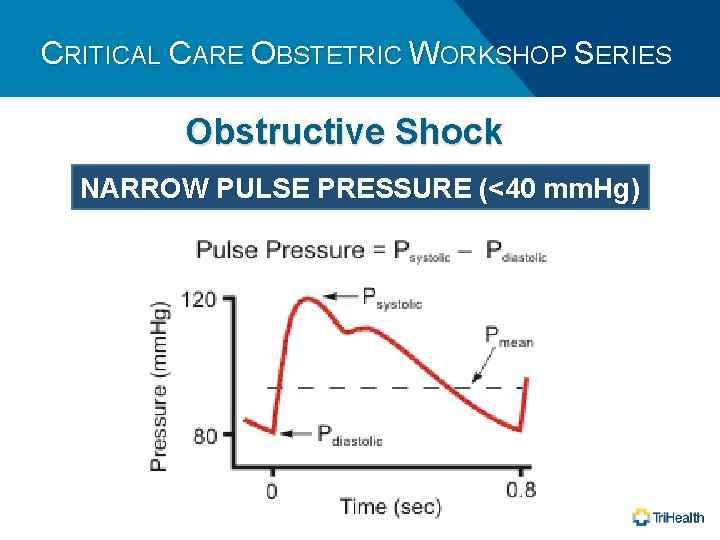
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Obstructive Shock NARROW PULSE PRESSURE (<40 mm. Hg)

MANAGEMENT OF SHOCK IN THE OBSTETRIC PATIENT

CRITICAL CARE OBSTETRIC WORKSHOP SERIES Initial Step-wise Approach Regardless of Type • Identify Stage of Shock • Multi-disciplinary Approach • Airway – ensure stable airway • IV access • Monitoring access / needs (arterial line, central line, PA catheter) • Fetal monitoring • Identify Cause & Type of Shock • Laboratory evaluation (CBC, CMP, Lactate, Coags, Cardiac enzymes & BNP, blood cultures, ABG) • Imaging (CXR, POC US) • IV Fluids (0. 5 -1 L bolus Ringer’s lactate) • Blood Products • Vasopressors

CRITICAL CARE OBSTETRIC WORKSHOP SERIES Approach by Type of Shock (Pregnant Patient) • Distributive • Cardiogenic • Hypovolemic • Obstructive
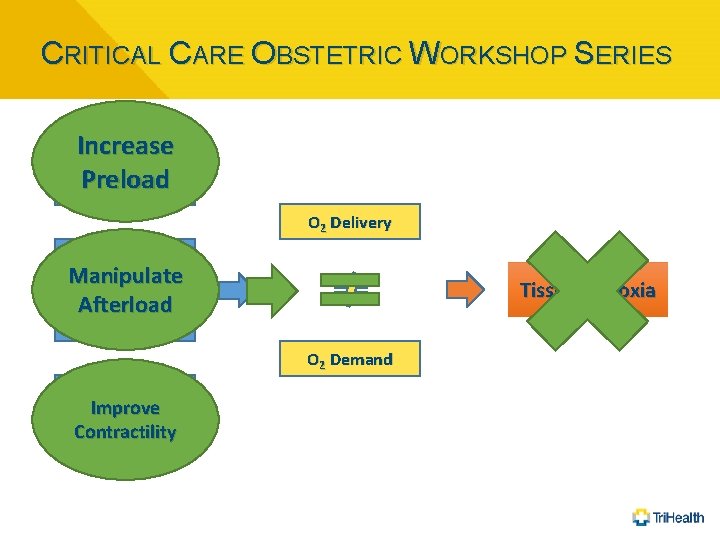
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Increase Preload Vasodilation O 2 Delivery IV volume depl. Manipulate Afterload Tissue Hypoxia Myocard Depres O 2 Demand Inc. Metabolism Improve Contractility
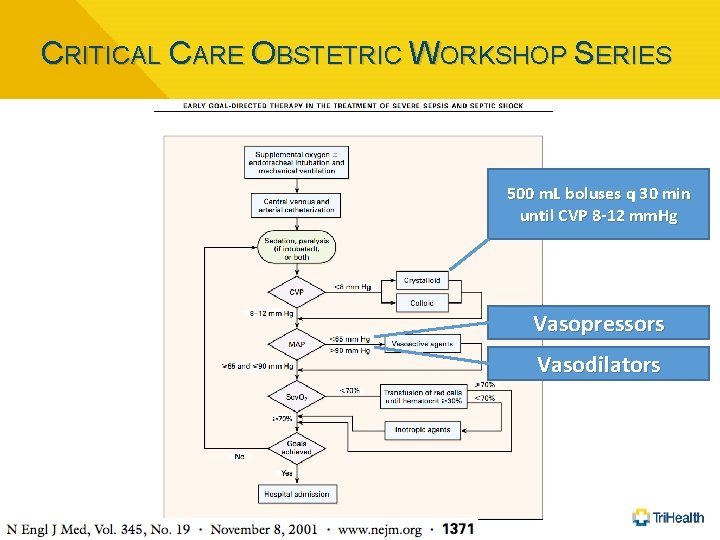
CRITICAL CARE OBSTETRIC WORKSHOP SERIES 500 m. L boluses q 30 min until CVP 8 -12 mm. Hg Vasopressors Vasodilators
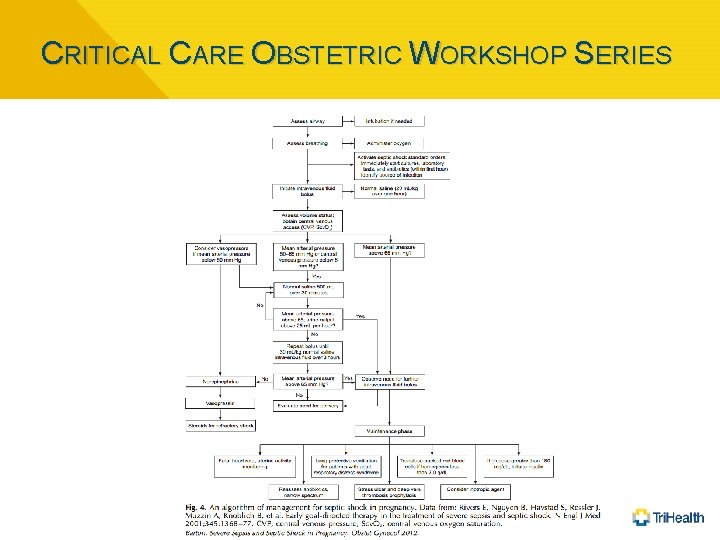
CRITICAL CARE OBSTETRIC WORKSHOP SERIES

CRITICAL CARE OBSTETRIC WORKSHOP SERIES Approach by Type of Shock (Pregnant Patient) • Distributive • Cardiogenic • Hypovolemic • Obstructive
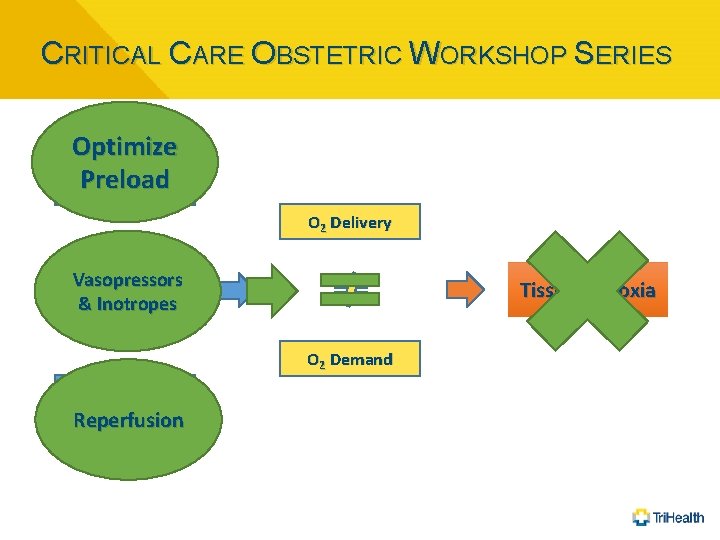
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Optimize Preload Hypotension O 2 Delivery Vasopressors & Inotropes Tissue Hypoxia Myocard Depres O 2 Demand Inc. Metabolism Reperfusion

CRITICAL CARE OBSTETRIC WORKSHOP SERIES Approach by Type of Shock (Pregnant Patient) • Distributive • Cardiogenic Hemorrhagic • Hypovolemic Non-hemorrhagic • Obstructive
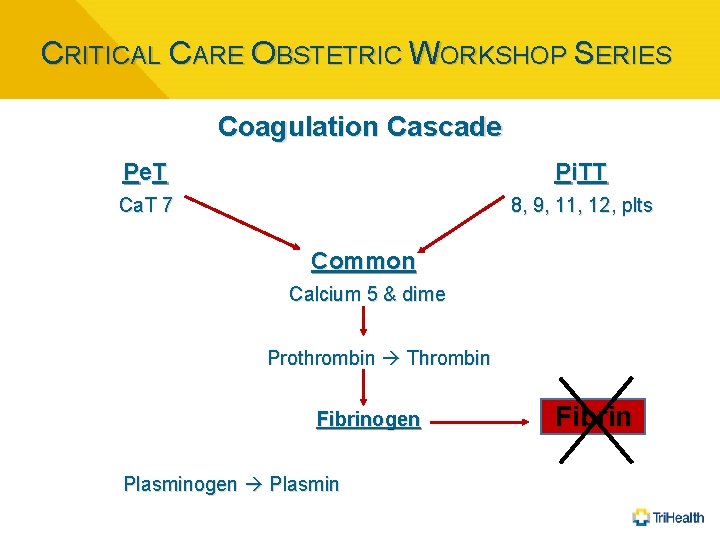
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Coagulation Cascade P e. T Pi. TT Ca. T 7 8, 9, 11, 12, plts Common Calcium 5 & dime Prothrombin Thrombin Fibrinogen Plasminogen Plasmin Fibrin

CRITICAL CARE OBSTETRIC WORKSHOP SERIES Considerations: Medical Approach • Avoid large volumes of crystalloid – transfuse blood products early • Transfusion should keep-up with blood loss • Essential to follow Coagulation Panel, CBC, K+, Ca+ very closely to guide selection & timing for replacement • INR > 1. 5 : Start with FFP • Platelets < 100, 000 : Start with Platelets • Fibrinogen < 200 : Start with Cyroprecipitate • Consider drawing Red-Top Tube and watching Surgical Approach • Atony • First line (after uterotonics): bimanual compression, balloon tamponade, uterine packing, uterine compression sutures and devascularization • Last line: aortic compression & hysterectomy • Morbidly Adherent Placenta • Plan for and move to hysterectomy without delay
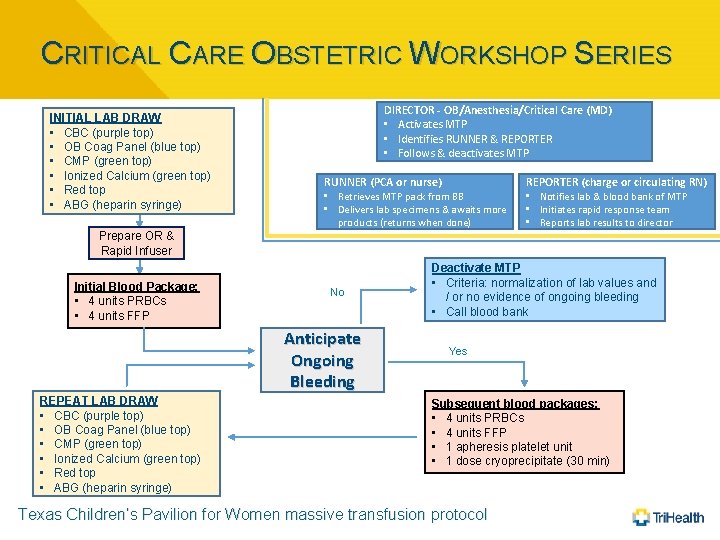
CRITICAL CARE OBSTETRIC WORKSHOP SERIES INITIAL LAB DRAW • CBC (purple top) • OB Coag Panel (blue top) • CMP (green top) • Ionized Calcium (green top) • Red top • ABG (heparin syringe) DIRECTOR - OB/Anesthesia/Critical Care (MD) • Activates MTP • Identifies RUNNER & REPORTER • Follows & deactivates MTP RUNNER (PCA or nurse) • Retrieves MTP pack from BB • Delivers lab specimens & awaits more products (returns when done) REPORTER (charge or circulating RN) • Notifies lab & blood bank of MTP • Initiates rapid response team • Reports lab results to director Prepare OR & Rapid Infuser Initial Blood Package: • 4 units PRBCs • 4 units FFP No Anticipate Ongoing Bleeding REPEAT LAB DRAW • CBC (purple top) • OB Coag Panel (blue top) • CMP (green top) • Ionized Calcium (green top) • Red top • ABG (heparin syringe) Deactivate MTP • Criteria: normalization of lab values and / or no evidence of ongoing bleeding • Call blood bank Yes Subsequent blood packages: • 4 units PRBCs • 4 units FFP • 1 apheresis platelet unit • 1 dose cryoprecipitate (30 min) Texas Children’s Pavilion for Women massive transfusion protocol

CRITICAL CARE OBSTETRIC WORKSHOP SERIES Approach by Type of Shock (Pregnant Patient) • Distributive • Cardiogenic • Hypovolemic • Obstructive
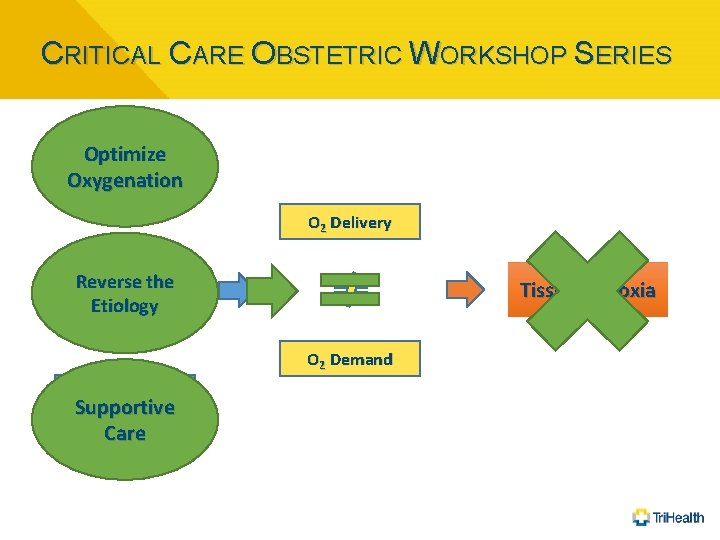
CRITICAL CARE OBSTETRIC WORKSHOP SERIES Optimize Oxygenation Hypoxia O 2 Delivery Reverse the Etiology the ↓Reverse Cardiac Output Tissue Hypoxia O 2 Demand Hypotension Supportive Care

CRITICAL CARE OBSTETRIC WORKSHOP SERIES THANK YOU!!
- Slides: 42