Sharon Decker RN Ph D ACNSBS CCRN ANEF

Sharon Decker, RN, Ph. D. , ACNS-BS, CCRN, ANEF The Role of Debriefing and Guided Reflection in Simulation

Objectives • Compare the strategies and models of debriefing and guided reflection. • Explore the integration of debriefing and guided reflection during simulation.

Introduction: Changes in Society • Experiencing more chronic co-morbidities • Under 10 of age experiencing co-morbidities • Living longer with increased chronic health needs • Expect more input in health care decisions • A broader view of medicine and health

Health Educators’: Challenge #1 How have these changes impactedhow we deliver education? competencies required for our discipline?

Introduction Challenges for the Health Educator “requires complex, sophisticated judgments and psychomotor skills…” (p. 128) IOM, Crossing the Quality Chasm (2001)

Federal Committions § Institute of Medicine (2004) • recommended teaching environments – Require demonstration of competencies in patient-care delivery, evidence-based practice, quality improvement, and informatics

Health Educators’: Challenge #2 New nursing graduates have difficulty transferring knowledge and skills to the practice setting Clarke & Aiken, 2003 Del Bueno, 2005

And … “New graduates…. not prepared for the new quality improvement environment will require additional costly orientation and training. ” Finkelman, A & Kenner, C. , 2007

Have we changed the methods used in teaching and assessing clinical competence to meet the changing environment?

Support for simulation by regulation agencies: For example: National Council of State Boards of Nursing(2005) Prelicensure nursing educational programs might include innovative teaching strategies (simulation) that complement clinical experiences

Support for simulation Nursing faculty to “be open to a variety of clinical teaching models” including virtual reality and simulated clinical experience AACN, 2003, p. 13

Support for simulation “New information and technologies may require new skills. And new technologies, such as simulation, may enhance skills…” (p. 129) IOM, Crossing the Quality Chasm (2001)

National Council of State Boards of Nursing Simulation defined: An educational process where learning experiences are simulated to imitate the working environment and require the learner to demonstrate the procedural techniques, decision-making, and critical thinking needed to provide safe and competency patient care.

Regulation agencies: For example: United States Medical Licensure Examination Assesses clinical skills through simulated patient interactions (Standardized patients) Objective Structured Clinical Examinations (OSCE’s) allows measurement of skills in communication, professionalism, and physical assessment

Regulation agencies: National Board for Respiratory Care Includes a Clinical Simulation Examination which consists of 10 separate patient management problems The National Registry of Emergency Medical Technicians Investigating the use of high-fidelity simulation to assess psychomotor and decision making skills

Simulation as an Educational Strategy Unique teaching tool that requires the educator to ● develop competencies with a new set of skills ● and be a risk taker.

Professional Charge for the Future § Therefore, if we must reinvent clinical teaching in practice based learning environments Could simulation be one mechanism for safe practice based learning?

Promoting Reflective Thinking Experience alone does not guarantee learning Need the integration of reflection (Boud, Keogh, & Walker, 1985) Simulation = Patient Care Experience + Debriefing and/or Guided Reflection

Adult Learning Principles Diverse Learning Styles Visual (realism, fidelity of the environment) Auditory (verbal responses) Tactile (hear and lung sounds) Kinesthetic (handling equipment)

Adult Learning Principles Constructivism Learning = process of constructing meaning Educator functions as a collaborative facilitator Includes experiential learning Active engagement Reflective thought

Reflection: Defined The process that allows practitioners to uncover and expose thoughts, feelings and behaviors A form of self-assessment/analysis that forces practitioners to face incongruity and uncomfortable facts

Philosophic Framework Dewey (1910, 1916) • Learning is dependent upon integration of experience with reflection and of theory with practice SchÖn (1987) • Learning promoted through the use of a “reflective practicum” – learning environment realistic in which faculty act as coach

Philosophic Framework Kolb (1984) • Learning enhanced through a synergistic transaction between learner and the environment Bandura (1977) • Learning enhanced – self-confidence promoted with active learning

Reflection SchÖn Reflection-on-action – After the event – Think back – gain understanding Reflection-in-action – During – Prompted by unexpected event Knowing-in-action (Thoughtful Thinking) – Unconscious, initiative knowing

Stages of Reflective Thinking Non reflectors § Don’t identify relationships Reflectors § Identified relationships between new and past knowledge Critical reflectors § Identified relationships and demonstrated self-analysis Mezirow, J. (1981) Wong, Kember, Chung, & Yan (1995)

Reflective Thinking Enhances learning from experience Helps expand clinical knowledge Promotes reflective practice Improves clinical judgment Glaze, J. E. (2001) Paget, T. (2001) Murphy, J. I. (2004)

Reflective Thinking Patient care varies with the nurse’s reflective abilities § minimal reflective abilities = illness oriented patient care; § reflective skills = care based on the individualized needs of the client. Conway (1998)

But, learning from reflection is not automatic demands active involvement in a clinical experience (Teekman, 2000) and guidance throughout the reflective process (Johns, 1996; Tanner, 1999).

Barriers & Outcomes of Reflective Thinking Barriers Outcomes § Previous learning § Heightened self-confidence § Fixations § Empathy § Socialization (as a nurse) § Understanding § Organizational culture § Better patient care

Environment and Tools Environment § Safe – non-threatening, trustful § Circle § Confidential § Time equal to or longer then the scenario

Setting the Ground Rules Confidential Review objectives and expectations Professional courtesy § No interruptions § Respect Supportive not judgmental § Don’t talk about anyone not present § Positive before negative Listen

Audio-Visual Integration • Be proficient with the equipment • Do not show a segment unless it is to be discussed • Show only 3 to 4 critical segments • Index critical segments § Introduce each segment • “This segment occurred … discuss what you were thinking as you…” § Show the segment § Pause – all the learner to self-critique

Discussion Do you include audio-visual segment during each simulation? When would they be appropriate? Thing to think about: Confidentiality forms Archiving of materials

Faculty Role and Responsibilities Dual role – facilitator and instructor Facilitator guide learner Self-discovery Instructor enhance understanding of “deficiencies”

Faculty Role and Responsibilities Set expectations (outline the process) Guide the session Facilitate according to level of engagement Include “quiet” learners Integrate instructional points Reinforce

Faculty Role and Responsibilities Give your analysis last Keep the discussion “learner centered” Be an active listener Use silence and pauses Use questioning – if appropriate to encourage discussions identify issues explore other options “Was there anything that occurred during the situation that made you uncomfortable? ” “What could you have done…? ”

Break What is the difference between Debriefing and Guided Reflection?

Debriefing

Debriefing A process in which after an experience the learner is lead through a purposeful discussion related to the experience Lederman, 1992; Fanning & Gaba, 2007

Debriefing: Purpose Correct errors Identify different ways of handling event next time Encourage self-assessment Promote reflective thinking

Debriefing - When During – (Frozen) § Emphasize teaching § Defuse a deteriorating situation § Redirect § Limit embarrassment After

Facilitation Techniques with Debriefing High-Level Facilitation – guidance Intermediate-Level Facilitation – elicit continued or deeper discussion and analysis Low-Level Facilitation – refrain from interrupting and review objective

Debriefing Models Questioning What did you experience? How did you perform overall? What have you learned? How would you change your performance? How can you apply learning to the future?

Debriefing Models Plus - Delta Plus + Examples of good behaviors Delta – Behaviors to improve on Include both what and how

Debriefing Models Advocacy – Inquiry § “I noticed …. ” § “I’m concerned…” § “I was wondering…”

Debriefing Summary Correct any errors Video for discussion

Guided Reflection

Guided Reflection The process that allows practitioners to uncover and expose thoughts, feelings and behaviors An active process of self-monitoring initiated by a state of doubt or puzzlement occurring during or after an experience

Guided Reflection: Purpose Promotes insightfulness Leads to discovery of new knowledge New knowledge – to be applied in future situations

Guided Reflection: When Immediately after the experience

Guided Reflection: faculty (facilitator’s) role § Facilitator § Learners who make their own discoveries – even if disappointing are more likely to acknowledge and own these discoveries then if these insights are pointed out to them. – Dewey, 1938

Guided Reflection: Models
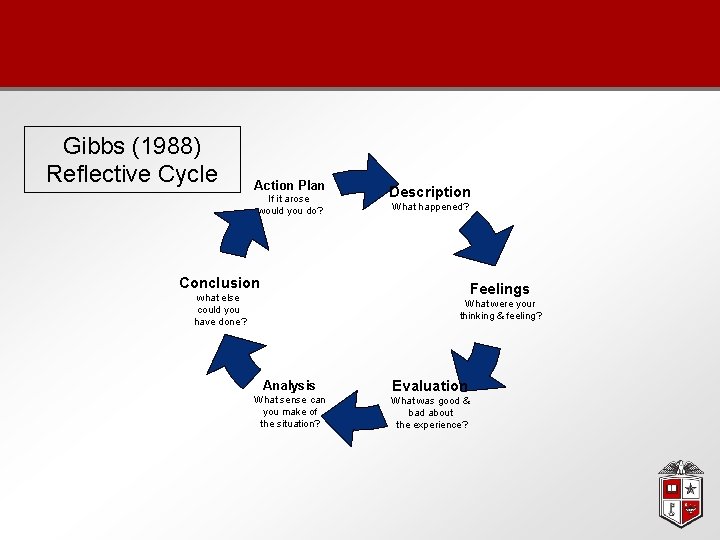
Gibbs (1988) Reflective Cycle Action Plan If it arose would you do? Description What happened? Conclusion Feelings what else could you have done? What were your thinking & feeling? Analysis What sense can you make of the situation? Evaluation What was good & bad about the experience?
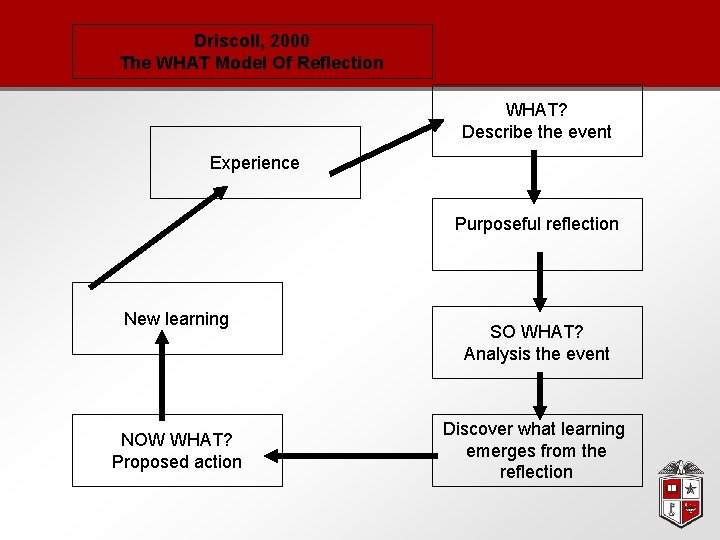
Driscoll, 2000 The WHAT Model Of Reflection WHAT? Describe the event Experience Purposeful reflection New learning NOW WHAT? Proposed action SO WHAT? Analysis the event Discover what learning emerges from the reflection

Johns, 1995, 1996 (Based on Carper’s Ways of Knowing) Aesthetics “learning and knowing self” grasping, interpreting, envisioning and responding” Describe what influenced your actions during the scenario. Personal “understanding personal dynamics and the ability to cope with the situation” Discuss your satisfaction with your actions during this scenario.

Johns, Ethics “knowing what is right and wrong and being committed to take action on this basis” Describe how your personal values and beliefs influenced your actions during this experience. Empirics “identifying and acknowledging lack of knowledge” Describe the knowledge and skills you have that influenced your decision making during this experience.

Johns, Reflexivity “resolve the contradictions between what the practitioner’s aim to achieve and actual practice, with the intent to achieve more desirable and effective practice” Describe situations you have experienced as a student nurse that influenced your decision making during this experience. Describe how this experience could have been handled differently.

Decker’s (Based on Johns Work) 1. 2. 3. 4. 5. 6. 7. 8. Talk to me about the problem your patient was having What was your main goal during this simulation? Tell me what influenced your actions during the scenario. Talk to me about how this experience made you feel and how satisfied you are with the actions you initiated? Talk to me about how your personal values and beliefs influenced your actions during this experience. Talk to me about the knowledge and skills you have that helped you provide patient care during this simulated experience. Talk to me about experiences you have had that influenced what you did during this scenario. What would you do different if we went back into the patient’s room and repeated the scenario right now?
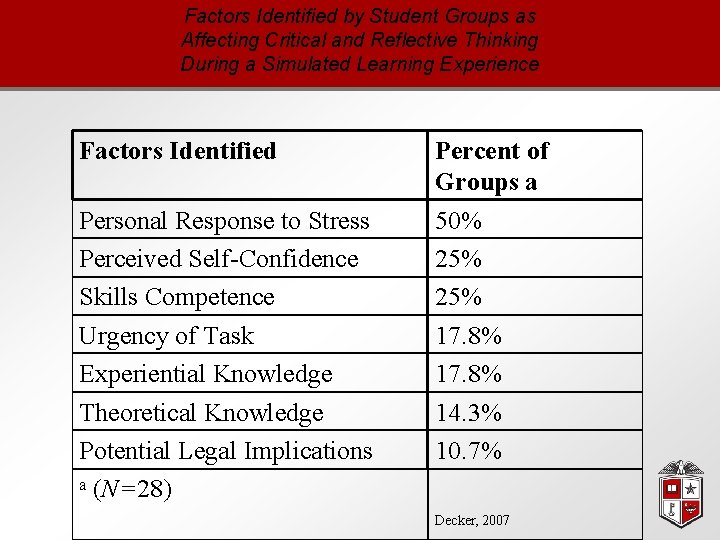
Factors Identified by Student Groups as Affecting Critical and Reflective Thinking During a Simulated Learning Experience Factors Identified Personal Response to Stress Perceived Self-Confidence Skills Competence Urgency of Task Experiential Knowledge Theoretical Knowledge Potential Legal Implications a (N=28) Percent of Groups a 50% 25% 17. 8% 14. 3% 10. 7% Decker, 2007

Additional Factors Identified • having tunnel vision (fixations) or focusing inappropriately on past experience, • being resistant to change or having a defensive attitude, • having poor communication skills, • the inability to access appropriate resources both technical and human, and • the learner’s cultural background. Decker, 2007

Discussion As faculty how can we resolve these barriers?

Summary: Reflection Can be learned Sufficient Time Worthy experience § Active experiential learning § Clinically relevant § Learn by: • building knowledge on existing knowledge • discovering what they know & what they do not know Insight

Reflective Thinking Learning from reflection is not automatic – It demands active involvement in clinical experience and guidance

References AACN, (2005). Faculty shortages in baccalaureate and graduate nursing programs: Scope of the problem and strategies for expanding the supply. AACN: Washington Boud, D. , Koegh, R. , & Walker, D. (1985). Promoting reflection in learning: A model. In D. Boud, R. Keogh & D. Walker (Eds. ), Reflection: turning experience into learning (pp. 18 – 40). London: Kogan Page. Clarke, S. P. , & Aiken, L. H. (2003). Failure to rescue: Needless deaths are prime examples of the need for more nurses at the bedside. American Journal of Nursing, 103(9), 42 -47. Del Bueno, D. (2005). A crisis in critical thinking [Electronic version]. Nursing Education Perspectives, 26(5), 278 -282. Decker, S. (2007). Integrating guided reflection into simulated learning experiences. In Jeffries, P. R. (ed), Simulation in nursing education from conceptualization to evaluation. New York, NY: National League for Nursing. Dreifuerst, K. T. (2009). The essential of debriefing in simulation learning: A concept analysis. Nursing Education Perspectives, 30(2), 109 -114.

References Finkelman, A. & Kenner, C. (2007). Teaching IOM: implications of the IOM report for nursing education, American Nurses Association, Silver Spring, Maryland. Glaze, J. (2002). Stages in coming to terms with reflection: Student advanced nurse practitioners’ perceptions of their reflective journeys. Journal of Advanced Nursing, 37(3), 265– 272. Jeffries, P. R. (2007). Simulation in nursing education form conceptualization to evaluation. New York, NY: National League for Nursing. Johns, C. (1995). Framing learning through reflection within Carper’s fundamental ways of knowing in nursing. Journal of Advanced Nursing, 22(2), 226– 234. Johns, C. (1996). Visualizing and realizing caring in practice through guided reflection. Journal of Advanced Nursing, 24(6), 1135– 1143. Mezirow, J. (1981). Transformative dimensions of adult learning. San Francisco: Jossey-Bass.

References Murphy, J. I. (2004). Using focused reflection and articulation to promote clinical reasoning: An evidence-based teaching strategy. Nursing and Health Care Perspectives, Nursing and Healthcare, 25(5), 226– 231. National League for Nursing (NLN). (2005, May). Position statement: Transforming nursing education. Retrieved July 9, 2006, from http: //www. nln/aboutnln/Position. Statements/transforming 0520005. pdf Nehring, W. M. & Lashley, F. R. (2010). High-Fidelity Patient Simulation in Nursing Education. Sudbury, MA: Jones and Barlett Publishers. Paget, T. (2001). Reflective practice and clinical outcomes: Practitioners’ views on how reflective practice has influenced their clinical practice. Journal of Clinical Nursing, 10(2), 204 -214. Wong, F. K. Y. , Kember, D. , Chung, L. Y. F. , & Yan, L. (1995). Assessing the level of student reflection from reflective journals. Journal of Advanced Nursing, 22, 48 -57.
- Slides: 66