Sexual Reproduction Female Reproductive System Gonad Ovaries ovarian




- Slides: 11

Sexual Reproduction

Female Reproductive System

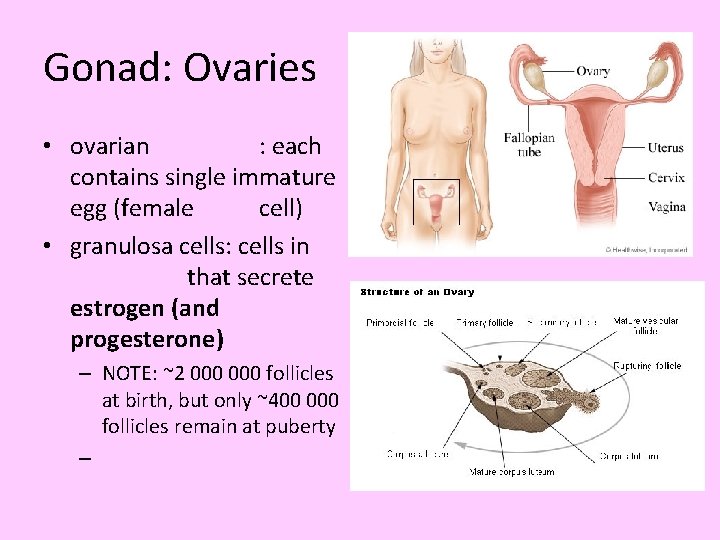
Gonad: Ovaries • ovarian : each contains single immature egg (female cell) • granulosa cells: cells in that secrete estrogen (and progesterone) – NOTE: ~2 000 follicles at birth, but only ~400 000 follicles remain at puberty –

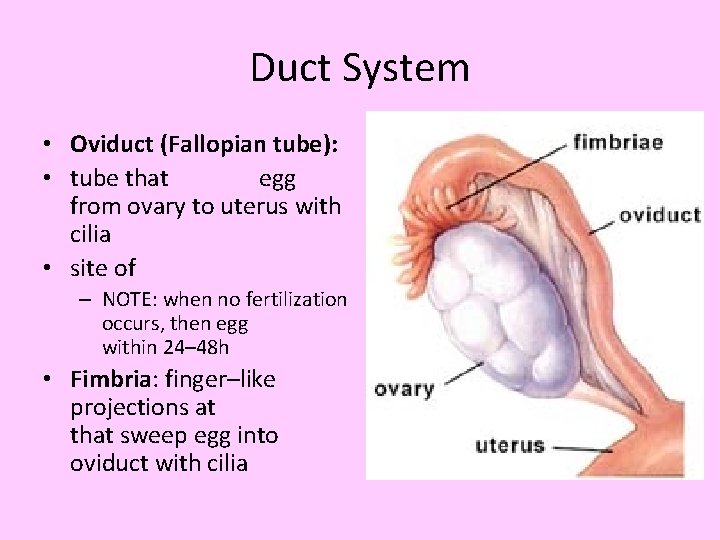
Duct System • Oviduct (Fallopian tube): • tube that egg from ovary to uterus with cilia • site of – NOTE: when no fertilization occurs, then egg within 24– 48 h • Fimbria: finger–like projections at that sweep egg into oviduct with cilia

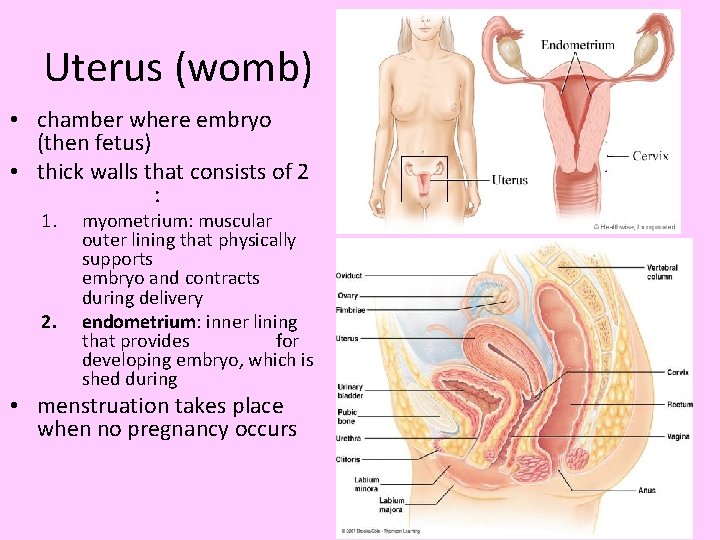
Uterus (womb) • chamber where embryo (then fetus) • thick walls that consists of 2 : 1. 2. myometrium: muscular outer lining that physically supports embryo and contracts during delivery endometrium: inner lining that provides for developing embryo, which is shed during • menstruation takes place when no pregnancy occurs

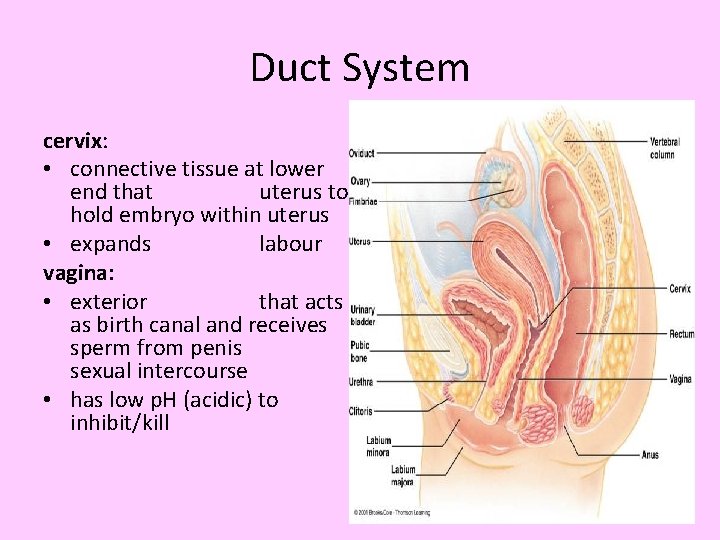
Duct System cervix: • connective tissue at lower end that uterus to hold embryo within uterus • expands labour vagina: • exterior that acts as birth canal and receives sperm from penis sexual intercourse • has low p. H (acidic) to inhibit/kill

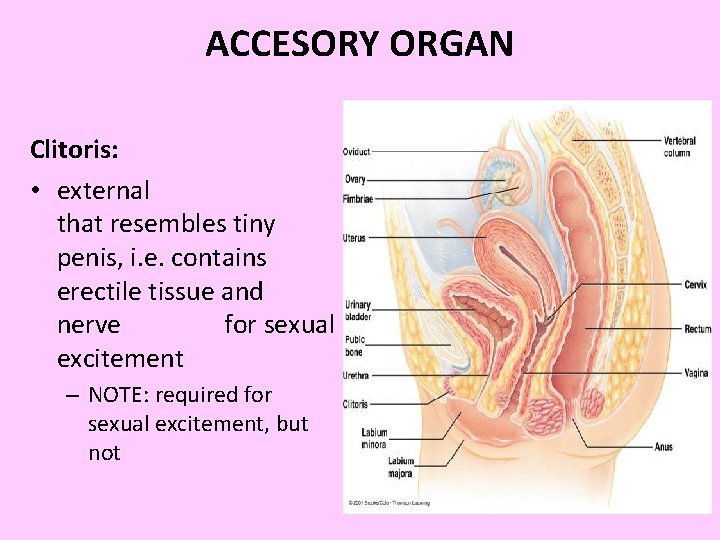
ACCESORY ORGAN Clitoris: • external that resembles tiny penis, i. e. contains erectile tissue and nerve for sexual excitement – NOTE: required for sexual excitement, but not

Female Hormones • FSH – Follicle Stimulating Hormone – Produced by the – Promotes the progesterone) – Too much end. • pituitary of a follicle in the ovary (which secretes estrogen and in body inhibits FSH secretion, and the follicular phase comes to an LH – Luteinizing Hormone – Produced by the Pituitary – Promotes the development of the corpus (secretes some progesterone and estrogen) – Too much progesterone in inhibits LH secretion, and as a result the corpus luteum begins to degenerate • Estrogen – Responsible for sex characteristics in females (hair and fat distribution) – Required for breast development • Progesterone – Involved in menstrual cycle – Pregnancy (embryo development) – for female sex characteristics

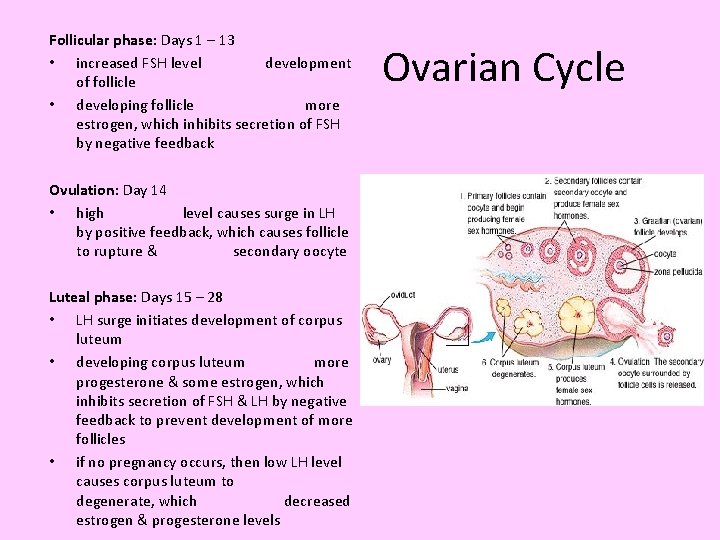
Follicular phase: Days 1 – 13 • increased FSH level development of follicle • developing follicle more estrogen, which inhibits secretion of FSH by negative feedback Ovulation: Day 14 • high level causes surge in LH by positive feedback, which causes follicle to rupture & secondary oocyte Luteal phase: Days 15 – 28 • LH surge initiates development of corpus luteum • developing corpus luteum more progesterone & some estrogen, which inhibits secretion of FSH & LH by negative feedback to prevent development of more follicles • if no pregnancy occurs, then low LH level causes corpus luteum to degenerate, which decreased estrogen & progesterone levels Ovarian Cycle

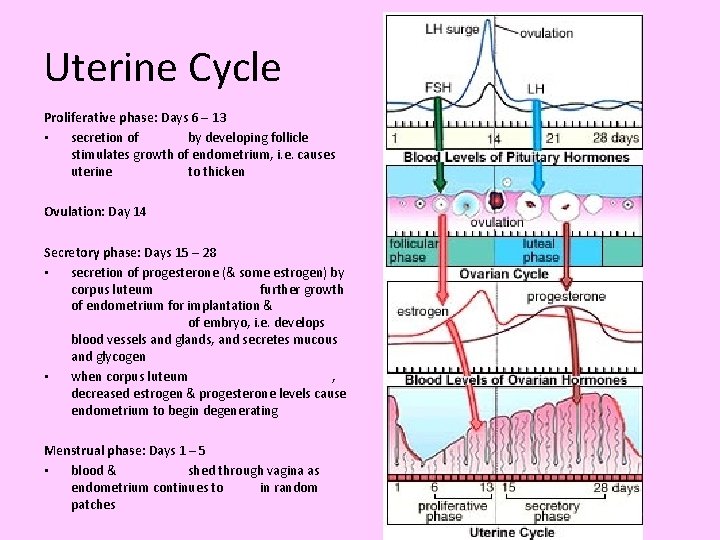
Uterine Cycle Proliferative phase: Days 6 – 13 • secretion of by developing follicle stimulates growth of endometrium, i. e. causes uterine to thicken Ovulation: Day 14 Secretory phase: Days 15 – 28 • secretion of progesterone (& some estrogen) by corpus luteum further growth of endometrium for implantation & of embryo, i. e. develops blood vessels and glands, and secretes mucous and glycogen • when corpus luteum , decreased estrogen & progesterone levels cause endometrium to begin degenerating Menstrual phase: Days 1 – 5 • blood & shed through vagina as endometrium continues to in random patches

• • identify and give functions for each of the following: – ovaries (follicles and corpus luteum) – oviducts (fallopian tubes) – uterus – endometrium – cervix – vagina – clitoris describe the functions of estrogen describe the sequence of events in the ovarian cycle, with reference the follicular phase, ovulation, and the luteal phase describe the sequence of events in the uterine cycle, with reference to menstruation, the proliferative phase, and the secretory phase describe the control of the ovarian and uterine cycles by hormones including gonadotropin-releasing hormone (Gn. RH), follicle-stimulating hormone (FSH), luteinizing hormone (LH), estrogen, and progesterone describe the hormonal changes that occur as a result of implantation, including – production of human chorionic gonadotropin (HCG) to maintain the corpus luteum – increased production of progesterone by the corpus luteum describe a positive feedback mechanism involving oxytocin