Severe Birth asphyxia Bavornvit Maliwan MD Epidemiology 21000

Severe Birth asphyxia Bavornvit Maliwan , MD


Epidemiology • 2/1000 in developed country. • 20/1000 in developing country where accessed to ANC is limited. • 15 -20% die in neonatal period • 25% of the survivor left with permanent neurological deficit.

Introduction • Birth asphyxia is lack of blood flow or gas exchange to or from the fetus in the period immediately before, during, or after the birth process. • The results are to vital organs and neurological organs. • Anaerobic glycolysis and lactic acidosis will occur.
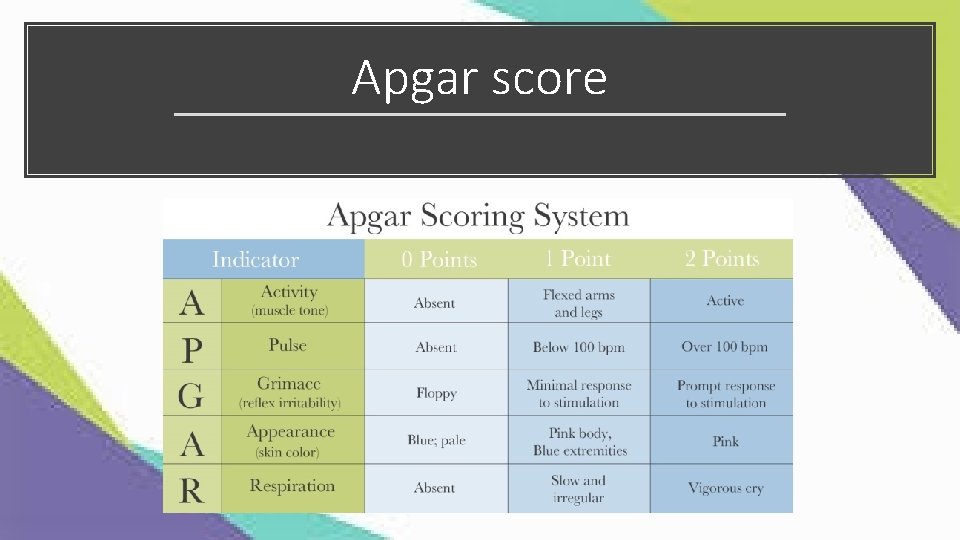
Apgar score

Definition of severe birth asphyxia • Severe birth asphyxia • APGAR 5 minute 0 -3 • Fetal acidosis (p. H<7) • hypoxic-ischemic encephalopathy • Multiorgan involvement

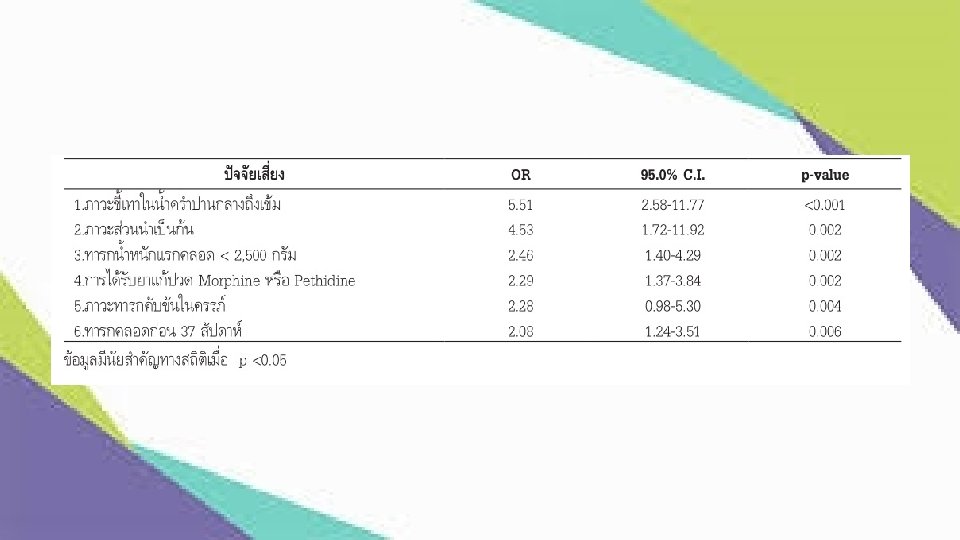
Risk factor

Maternal factor • Age <17 • Age >35 • ANC <4 • Primagravidarum • Multiparity • GDM • Hypertension

Intrapartum factor • Breech • Chorioamniitis • Poly-Oligohydramnios • Thick meconium • PPROM • Sedative • V/E F/E • C/S

Fetus factor • IUGR • Twin • BW <2500 g • GA <37 • Fetal distress

Other • Uterine factor : Utering rupture • Placenta factor : abruptio placenta , cord compression , nuchal cord • Infection



Pathophysiology • Immediate primary neuronal injury : low O 2 and glucose to brain. • Low ATP >>> Defect in Na-K pump >>> Sodium enter cells >> then water >>cell swelling >> depolarization >> cell death • Cell death release Glutamate which increase intracellular calcium and cause cell death • Latent period ( 6 hrs ) reperfusion occurs. • Secondary injury neuronal injury occurs over the next 24 -48 hours : • Blood flow from reperfusion at damage area, releasing toxic neurotransmitter.
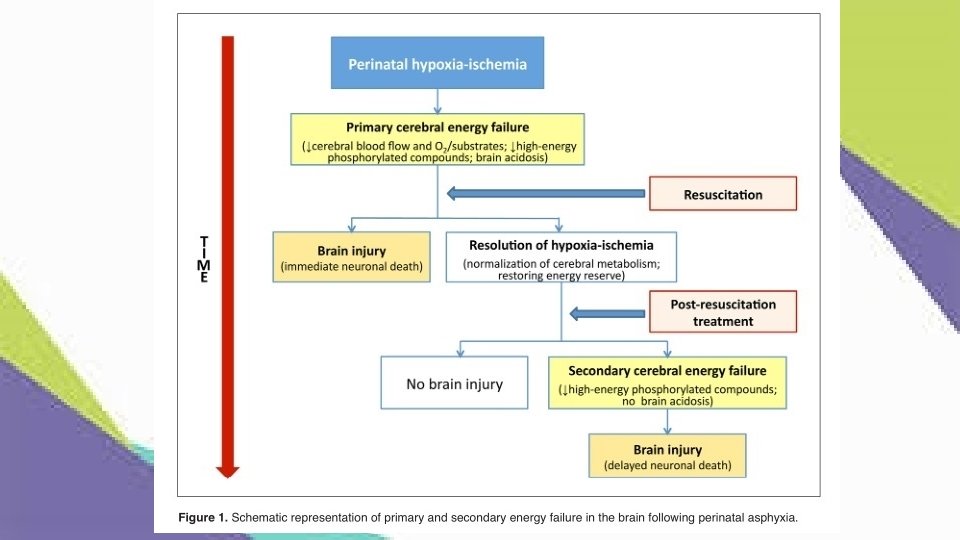

History and Physical • Organ specific symptom : MI, kidney, liver, RDS, pulmonary hypertension, hypoxic-ischemic encephalopathy ***

Myocardial infarction • Dyspnea • ST elevation – depression • CKMB Trop. T elevation

Respiratory distress syndrome • Tachypnea • Nasal flaring • Grunting • Intercostal, subxiphoid, and subcostal retractions • Cyanosis

Pulmonary hypertension • Increased pulmonary artery pressure (PAP) • Vasoconstriction

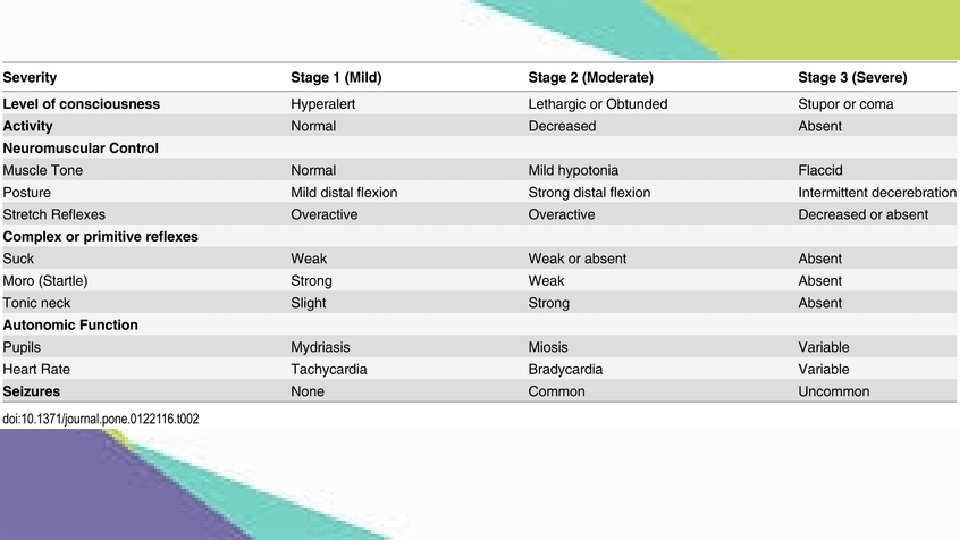
Hypoxic-ischemic encephalopathy *** • Sarnat I : Sympathetic : neonates will be hyper-alert , prolong wakefulness , DTR 3+ • Sarnat II : parasympathetic : lethargic , miosis , bradycardia , low DTR , distal flexion , hypersecretion , seizure • Sarnat III : seizure , decrease level of conscious , flaccid tone , low DTR , abnormal EEG

Evaluation • CXR : need for intubation • ABG : degree and cause of hypoxemia • Transaminase level and coag : Liver function • Trop. T CKMB EKG : Myocardial injury • BUN Cr : kidney status • Glucose : Hypoglycemia

Treatment • Therapeutic hypothermia : in 6 hr to prevent secondary injury • (decrease mortality 62% disability 48%) • Intubation , surfactant , O 2 , inhaled nitric oxide : RDS , pulmonary hypertension • Blood products : Coagulopathy • Vassopressor : MI • Renal dysfunction : careful use on crystalloid and blood product

Side effects of Therapeutic hypothermia • Peripheral vasoconstriction • Diuresis • Cardiac dysfunction • Arrhythmias • Coagulopathy • Thrombocytopenia • Leukocyte dysfunction • Pulmonary hypertension • Sclerema (calcium deposits in the skin)


Ref: • Pathophysiology, clinical manifestations, and diagnosis of respiratory distress syndrome in the newborn • Richard Martin, MD Mar 29, 2018. • https: //www. uptodate. com/contents/pathophysiology-clinicalmanifestations-and-diagnosis-of-respiratory-distress-syndrome-in-the newborn? search=pediatric%20 rds&source=search_result&selected. Tit le=1~150&usage_type=default&display_rank=1

Ref • Pulmonary hypertension in children: Classification, evaluation, and diagnosis • Mary P Mullen, MD Mar 06, 2019. • https: //www. uptodate. com/contents/pulmonary-hypertension-inchildren-classification-evaluation-anddiagnosis? search=pediatric%20 pulmonary%20 hypertension&source= search_result&selected. Title=1~150&usage_type=default&display_ra nk=1

Thank You
- Slides: 30