SESSION 2018 2019 PROGRAM NAME B SC NUTRITION

SESSION : 2018 2019 PROGRAM NAME : B. SC. NUTRITION HONOURS COURSE NAME : BASIC DIETETICS SEMESTER - III

PAPER – C 7 T TOPIC : MODIFICATION IN FEEDING TECHNIQUES
parenteral Feeding Nutrition Concept & Definition: Nutrient preparation directly into vein PN Sterile, nutrient dense solution Infused intravenously Peripheral Venous Access / Central Venous Access Digestive tract Nourish those patients who are digesting & absorbing nutrients not capable of

parenteral Feeding Nutrition Indications: can not eat due to cancer of the pharynx, oesophagus will not eat due to some physiological & other problems should not eat due to surgery of the GI tract, inflammatory bowel diseases can not eat enough due to persistent nausea & anorexia can not be fed adequately by tube feeding hypermetabolic states like burns , severe infections etc.

parenteral Feeding Nutrition Duration: Maximum 48 to 72 hours. Objectives: To provide water & electrolytes q To correct electrolyte imbalance q To make up for the loss of tissue proteins q To provide energy to meet the daily needs of the patient q

parenteral Feeding Nutrition Venous Access for PN Support: Ø Peripheral Parenteral Nutrition (PPN) § Peripheral veins § Low concentration of solutions § Short duration (less than 10 days) § Does not meet all the nutritional needs of the patient § Short – term nutrition support

parenteral Feeding Nutrition Ø Total Parenteral Nutrition (TPN) § Central veins § Higher concentration solutions § Long duration § Reliably meet a person’s complete nutrient requirements § Long – term nutrition support

parenteral Feeding Nutrition Chemical composition of Parenteral Feed: v Carbohydrates • • • Mainly glucose, fructose, sorbitol & other carbohydrate derivatives Glucose 5% of solutions Higher concentration of glucose Thrombophlebitis Fructose 10 – 15% of solutions Minimum of 100 gm of glucose / day To prevent protein catabolism

parenteral Feeding Nutrition v Amino • • • Acids Protein hydrolysates & synthetic amino acid mixtures L amino acids Commercial amino acids are available in concentrations 3. 5, 5. 5, 7. 5, 8. 5, 10, 11 &15% v Fats • • • Emulsified fats Provide essential fatty acids & calories If toxic results are observed then fats have to be avoided

parenteral Feeding Nutrition v Vitamins • Especially vitamin B 12, folic acid & vitamin K v Electrolytes • • Sodium, potassium, chlorine, phosphorous, calcium & magnesium Trace elements : zinc, copper, chromium, manganese & iodine v Water • • Daily minimum requirement 1. 5 liter If any water losses then these should be made up

parenteral Feeding Nutrition Nutrient Contribution: ü ü 30 – 50% of the daily nutrients Remaining should be given by oral route Advantages: o o o Started easily Simple No delay in calorie intake Does not rely on gastric or intestinal function Less need for interruptions Safe

parenteral Feeding Nutrition Disadvantages / Complications � Catheter related complications o Arrhythmias o Pneumothorax o Thrombosis o Sepsis o Puncture of the subclavian artery � Infections o Septicaemia

parenteral Feeding Nutrition � Metabolic o o complications Hypoglycemia Azotemia Electrolyte disturbances Acid base balance disturbances � Nutritional o o o complications Rapid weight loss Vitamin deficiency Vitamin toxicity Trace element deficiency Essential fatty acid deficiency

parenteral Feeding Nutrition � Liver o o o complications Rise in SGOT Rise in alkaline phosphatase Fatty changes in the liver
TUBE FEEDING v Concept & Definition: TUBE NOSE Stomach Duodenum Jejunum

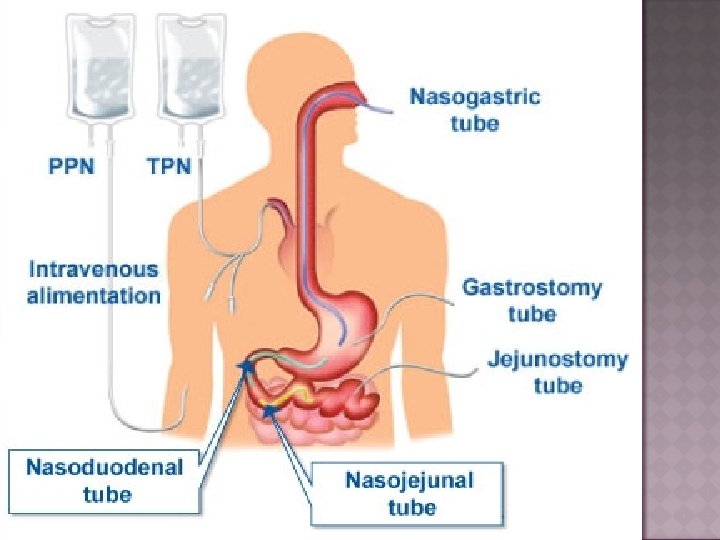
TUBE FEEDING q Nasogastric Feeding q Nasoduodenal Feeding q Nasojejunal Feeding These are short term feeding techniques (3 to 4 weeks)
TUBE FEEDING TUBE Surgical Procedure Gastrostomy Jejunostomy These are long term feeding techniques.

TUBE FEEDING v Characteristics § § § of Satisfactory Tube feeding Nutritionally adequate Well tolerated by patients Easily digested Easily prepared Inexpensive

TUBE FEEDING v Indications Those can’t swallow Ø Those who have persistent anorexia Ø Those who are semiconscious or unconscious Ø Those who have to be given unpalatable formula Ø Severely undernourished patients Ø Those who can’t digest & absorb foods Ø Post operative cases Ø

TUBE FEEDING v Apparatus • Tube used in this process – Ryles Tube • Soft, flexible tube • Thin, soft, polythene tube of 2 to 3 mm in diameter • Lubrication purpose – olive oil & liquid paraffin
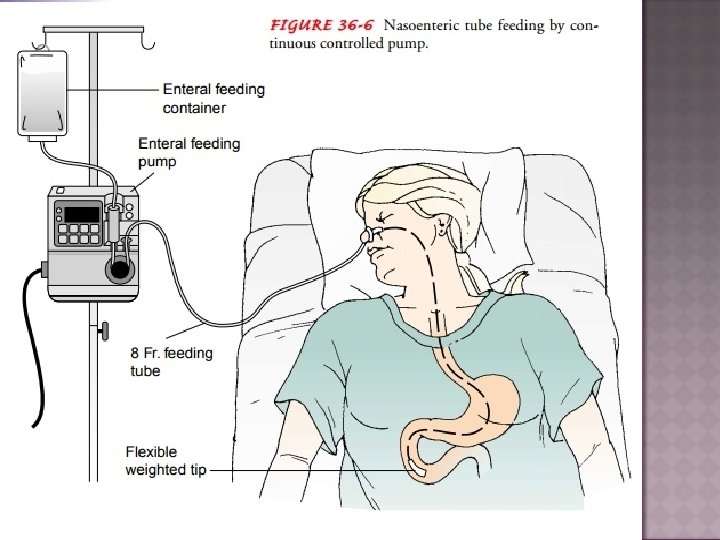

TUBE FEEDING v Composition of Tube feeding 3 types depending on its composition: Natural liquid foods § Glucose water, fruit juices, coconut water, whole or skim milk, strained soups of cooked vegetables, cereals, sugar solution, molasses etc. § Vegetable oil or cream & non fat dry milk are also incorporated.

TUBE FEEDING Blenderized Feeding ü Ordinary food items which can’t be swallowed should be blenderized & use for tube feeding. ü Foods can be precooked. ü Well tolerated, less commercial formula. expensive than a
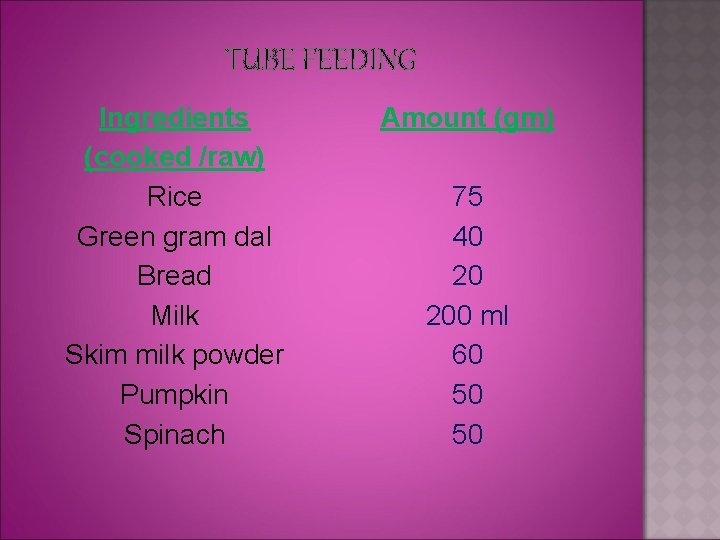
TUBE FEEDING Ingredients (cooked /raw) Rice Green gram dal Bread Milk Skim milk powder Pumpkin Spinach Amount (gm) 75 40 20 200 ml 60 50 50
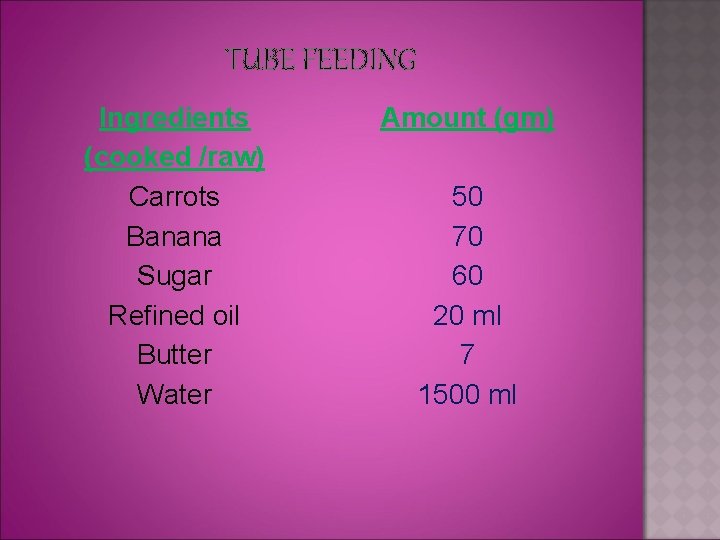

TUBE FEEDING Ingredients (cooked /raw) Carrots Banana Sugar Refined oil Butter Water Amount (gm) 50 70 60 20 ml 7 1500 ml

TUBE FEEDING Elemental Diet Normal foods may be replaced by preparation of protein or amino acid, fat & carbohydrate in easily assimilable forms § Commercially supplied polymeric mixtures can also be used. § The commercial preparation possess both advantages & disadvantage. Advantages: Ø Convenience Ø Constant composition Ø Presterilization Ø Minimal preparation time Ø Ease of administration §

TUBE FEEDING Disadvantages: • High cost • Unpleasant taste • Sometime high osmolarity v Contribution of Nutrients Energy: § An average adult patient will require 1500 to 2000 kcal § After surgery, injury, burns or in severe PEM about 3000 kcals should be provided § Inadequate calories can lead to wasting of muscles of the body

TUBE FEEDING Protein § Usually patients are given about 60 - 70 gms of protein except in case of hepatic coma, kidney failure etc. § If there is injury, surgery, burns or severe PEM about 100 to 200 gms of protein are needed. Fat § Fats may be given in the form of emulsion.

TUBE FEEDING Carbohydrate § Glucose, cane sugar, dextrin, maltose may be given to the patients § About 300 – 500 gms of carbohydrate may be given depending on the calorie needs. Fluid § About 2500 – 3000 ml. should be given daily to meet the normal requirements & to compensate for the fluid losses

TUBE FEEDING Electrolytes § Na. Cl, KCl & other such important electrolytes can be given according to the needs. Vitamins § All the essential vitamins may be supplied to the patients through tube feeding

TUBE FEEDING v Advantages q The gastric content can be analyzed. q Unpalatable drugs & formulas can be given. q Usually there are no risk of infections like in case of parenteral feeding. q A lot of fluid can be administered. q It can be continued for a long duration of time. q It is economical. q Adequate nutrition can be easily given by this method.

TUBE FEEDING v Disadvantage GI complications • Vomiting • Diarrhoea • Constipation • Abdominal pain • Gastric irritation Mechanical complications • Tube fractures • Leakage • Obstruction • Irritation

TUBE FEEDING Metabolic complications • Hypovolemia • Hyperkalemia • Hypophosphatemia • Hypertonic dehydration • Fluid overload
- Slides: 34