Septic Abortion and Puerperal Infection Septic Abortion Introduction

Septic Abortion and Puerperal Infection

Septic Abortion: Introduction n n n History Physical Examination Problem list Differential diagnosis Investigation Management “Septic Abortion”

. . . History. . .



Physical Examination

Physical Examination A woman looked acutely ill Vital signs: BT 39. 0 oc BP 90/60 mm. Hg PR 90/min. RR 20/min. HEENT: not pale, no jaundice Heart: normal S 1 S 2 , no murmur Lungs: clear Abdomen: liver and spleen not palpable Tender with rebound tenderness at suprapubic region, no mass, active bowel sound

Physical Examination PV: NIUB - normal Vag. - bloody discharge, no foul smell Cx - os closed, excitation negative Ut. - enlarged, A/V, gestational 8 wk size, tender Adnx. - no mass

Problem list?

Problem list n n Bleeding per vagina after criminal abortion lower abdominal pain with rebound tenderness Fever Uterus 8 wk. size, tender

Differential diagnosis?

Differential diagnosis n Gynaecologic - Septic abortion Ectopic pregnancy - PID - UTI in pregnancy n Surgical - Acute appendicitis

Investigation?

Investigation n CBC n Beta - h. CG n Electrolyte, glucose, BUN, creatinine n Matching and grouping n Endocervical swab for cultures (eg, aerobic, anaerobic) and gram stain n Ultrasound n Abdominal x-ray

Investigation (14 �. �. 44(. 1 Complete Blood Count RBC 4. 35 x 106 /ml HGB 11. 6 g/dl HCT 34. 5% MCV 79 fl MCH 26. 7 pg MCHC 33. 7 g/dl RDW 14. 0% WBC 21. 7 x 103 /ml (H) NE 89. 4% (H) LY 6. 4% (L) MO 3. 2% EO 0. 5% (L) BA 0. 2%LUC 0. 3% PLT 292, 000/ ml

Investigation 2. Bacteriology Cervical swab - no growth 3. Blood Chemistry BUN 6. 0 mg/dl Haemoculture - no Creatinine 0. 6 mg/dl

Investigation Urinalysis Appearance - yellow Sp. gr. - 1. 010 p. H 7. 0 Protein negative, Glucose negative, Ketones negative, Bile/Urobilinogen negative, no RBC, WBC 0 -1, no bacteria 5. Serology and immunology anti HIV negative 4.

Management?

Management n n n Monitor vital signs - BT, BP, PR, RR Administer IV fluids through a large-bore angiocatheter to maintain blood pressure and urine output For patients who are unstable, administer oxygen and insert a Foley catheter Early antibiotic treatment may be guided by gram stain, but broad-spectrum coverage is recommended In patients with Rh negative, Rh immunoglobulin should be given

Management n n Perform evacuation of retained tissues from the uterine cavity, preferably by dilation and curettage (D&C)*. If D&C is not immediately available, high doses of oxytocin can be used Laparotomy may be needed if the above measures elicit no response A hysterectomy may be necessary in cases of uterine perforation, bowel injury, clostridial myometritis, and pelvic abscess* Management of septic shock, if present

Management 14)�. �. 44) 1. 5% DN/2 1000 ml x 1 i. v. drip 120 cc/hr. 2. Broad-spectrum antibiotics - Ampicillin 1 gm i. v. q 6 hr - Gentamicin 240 mg + 5% DW 100 cc i. v. drip in 1 hr, OD - Metronidazole 500 mg i. v. q 8 hr 3. Paracetamol (500) 2 tab prn for fever q 6 hr 4. TT 0. 5 ml i. m. stat, TAT 3000 unit i. m. after skin test negative 5. Dilation and Curettage , after at least 4 hours of broad-spectrum antibiotics

Operative note (14 �. �. 44( Preoperative diagnosis: septic criminal abortion Operation: Dilation and Curettage Anaesthesia: paracervical nerve block Position: lithotomy Operative finding: uterine sound 10 cm A/V, conceptus 2 gm, blood loss 20 cc Operative procedure: Dilation and Curettage

Pathology report (16 �. �. 44( GROSS: specimen, received in formalin, labeled with the patient’s name and conceptive product is irregular brown tissue weighing 2 g Block : A = conceptive product DIAGNOSIS: Endometrium : Hypersecretory endometrium with acute inflammation* NOTE: No chorionic villi seen*


Clinical improvement after D&C n Day 1 ������������� BT 37. 8 oc, BP 90/60 mm. Hg, PR 70/min. , RR 20/min. Abdomen - soft, mild tender at suprapubic region Management: Paracetamol, continue antibiotics i. v. , methergin i. m.
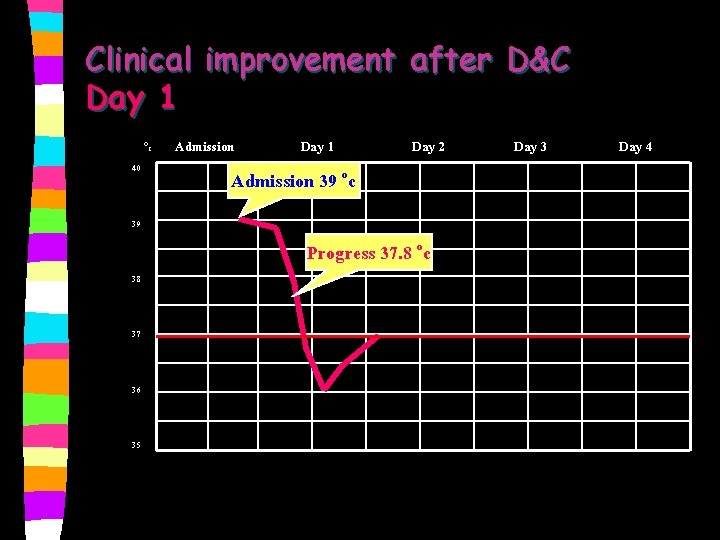
Clinical improvement after D&C Day 1 Oc 40 39 38 37 36 35 Admission Day 1 Day 2 Admission 39 oc Progress 37. 8 oc Day 3 Day 4

Clinical improvement after D&C n Day 2 ������������ BT 37. 0 oc, BP 110/60 mm. Hg, PR 88/min. , RR 20/min. Abdomen - no tenderness Management: Antibiotics i. v. ����� 48 �������� oral form
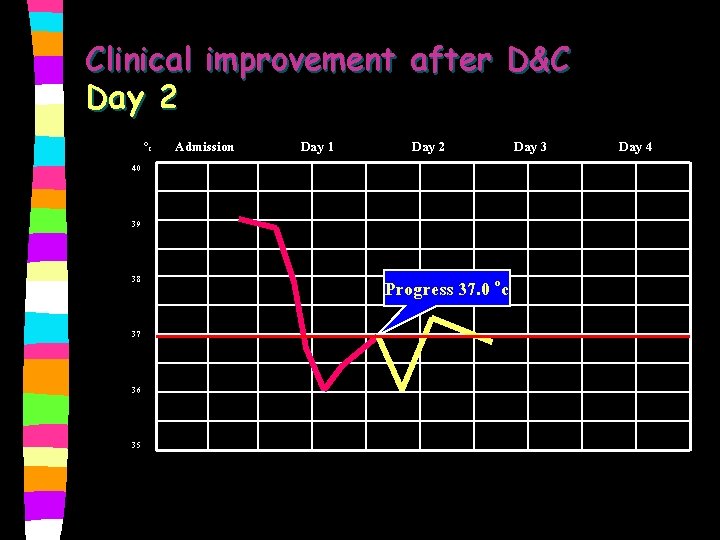
Clinical improvement after D&C Day 2 Oc 40 Admission Day 1 Day 2 39 38 37 36 35 Progress 37. 0 oc Day 3 Day 4

Clinical improvement after D&C n Day 3 BT 36. 8 oc, PR 84/min. Management: Augmentin p. o. * ��� DMPA i. m.
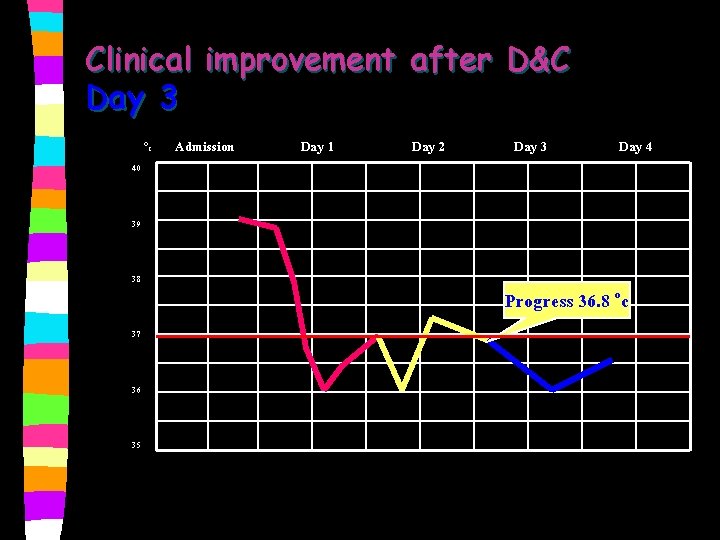
Clinical improvement after D&C Day 3 Oc 40 Admission Day 1 Day 2 Day 3 Day 4 39 38 37 36 35 Progress 36. 8 oc

Clinical improvement after D&C n Day 4 discharge Medications on discharge: Fe. SO 4, Paracetamol, Augmentin(625 mg) 1 x 3 pc
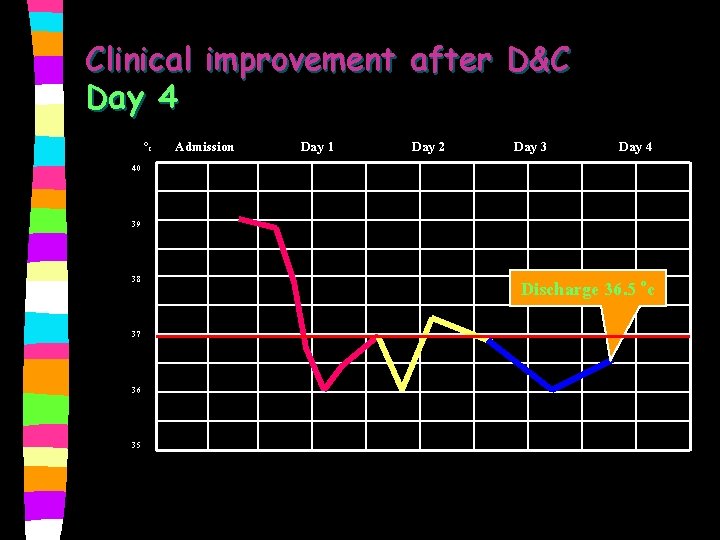
Clinical improvement after D&C Day 4 Oc 40 Admission Day 1 Day 2 Day 3 Day 4 39 38 37 36 35 Discharge 36. 5 oc


Puerperal Infection: Introduction n n n n History Physical Examination Labour record Progress note Differential diagnosis Investigation “Puerperal Infection” Questions

. . . History. . .

History ��������� 32 �� ����������� 1 st admission (27 �. �. 43) ��������� G 2 P 1 last 4 years (41 wk, NL, ����� ), GA 42 wk. By date LMP 5 �. �. 42 EDC 12 �. �. 43 ANC x 6 ����� x 1 �. �. ���� TT ��� Serology all negative Total Weight Gain 10. 9 Kg.


Physical Examination

Physical Examination Vital sign stable, HEENT - normal, H&L - normal Uterus - Fundal Height 3/4 > umbilicus Back of foetus ������ , cephalic presentation, FHS +ve, EFW 3000 g Pelvic examination Pelvis - adequate Cervix - soft consistency, effacement 20 %, os closed NST - reactive

Labour record
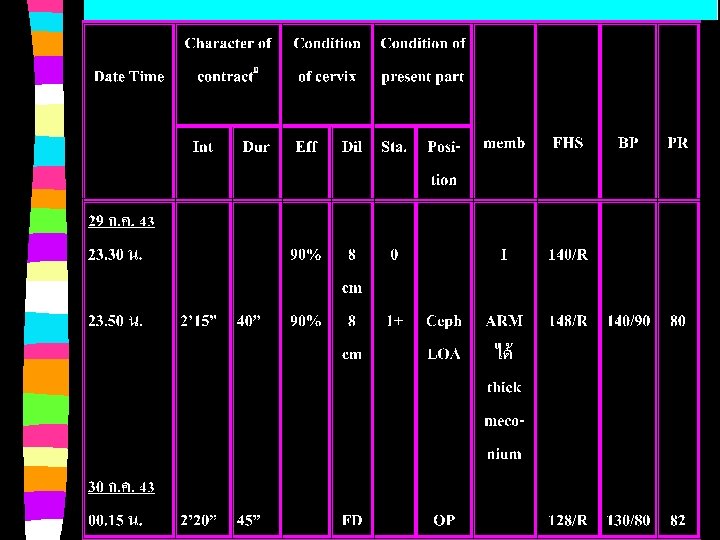

Labour record (Day 3 after admission) -Abnormal delivery, position - LOP -Procedure: Low F/E (right mediolateral episiotomy with subcuticular suture( -Indication: thick meconium amniotic fluid stain -Newborn: male, alive, 2850 g, 49. 5 cm. APGAR score 1 min. = 6 5 min. = 9 ������� ET tube for suction ��� O 2 ���� -Postpartum condition: normal

Progress note

Progress note n Postpartum Day 1 (31 �. �. 44) S: O: BT 38. 3 oc A: P- : n Postpartum Day 2 (1 �. �. 44) S: ������������ O: BT 38. 2 oc, BP 120/80 mm. Hg, PR 88/min. HEENT - not pale, no jaundice Heart - normal S 1 S 2, no murmur Lungs - clear

Progress note n Postpartum Day 2 (cont) O: Uterus - 2 FB < umbilicus, well contracted No active bleed per vagina A: Status postpartum Day 2 with fever P: ? ? ?


Plan for investigation n n CBC UA Haemoculture Cervical swab for gram stain and culture

Progress note n Postpartum Day 3 (2 �. �. 44) S: �������������������������������� O: BT 38. 0 oc Perineum - foul -smelling greenish yellow discharge per vagina CBC WBC 23400 (Granulocyte 81. 8 %) UA within normal limit A: F/E

Progress note n Postpartum Day 3 (cont) P: 1. For investigation - Pus from wound for gram stain - Pus from wound for culture 2. For treatment - Stitch off from episiotomy wound and dressing bid - Start antibiotic (Amoxycilline and Metronidazole p. o. ) 3. Monitor vital signs and clinical vaginal bleeding 4. No breast feeding

Investigation �� Gram stain: Gram negative rod - few Gram positive cocci - numerous �� culture for aerobes : E. coli - heavy growth �� Antimicrobial Susceptibility for E. coli: Susceptible to - ampicillin, amoxycillin, gentamicin, ceftriaxone, etc.

Clinical improvement after treatment n Postpartum Day 4 ���������������� , discharge ���������� n Postpartum Day 6 ����� discharge PV - MIUB: clean episiotomy wound - Vg: Lochia serosa - Cx: clean - Ut: slightly enlarged - Adx: free

Clinical improvement after treatment n Postpartum Day 9 S: ���������� ������������ O: Perineum - granulation tissue form over raw surface, no discharge, no foul smell A: F/E Status postpartum day 9 with infected episiotomy wound, clinical improved P: - 3 o suture episiotomy wound at OR - continue antibiotic - local care


“ Puerperal Infection” n n Treatment - Specific - Supportive - Symptomatic Prevention - �������� - ��� prophylactic antibiotics �����������������
Questions

. 1���������� septic abortion ������� ���. . . A. E. coli B. Group B beta-haemolytic streptococci C. Staphylococcal organisms D. Bacteroides species E. All of above E.

. 2 Complications �������� septic abortion ���. . . A. Peritonitis B. Pelvic Inflammatory Diseases C. Sepsis D. Septic shock E. All of above E.

. 3������ 23 �� ���������� 3 ������ BT 38. 3 oc BP 90/60 mm. Hg PR 128/min. RR 32/min A. ���������� broad-spectrum antibiotic ���. . . B. Haemoculture and septic workup C. Dilation and Curettage D. Resuscitate volume E. Ultrasound D.


. 5���������� Puerperal infection A. mastitis B. urinary tract infection C. respiratory tract infection D. typhoid fever E. all of above E.

- Slides: 61