SEPSIS SEPSIS A Spectrum Definitions Infection Infection is























































- Slides: 68

SEPSIS

SEPSIS – A Spectrum – Definitions • Infection — Infection is the invasion of normally sterile tissue by organisms. • Bacteremia — Bacteremia is the presence of viable bacteria in the blood. Sepsis and the systemic inflammatory response syndrome: Definitions, epidemiology, and prognosis, www. uptodate. com, accessed 3/18/14

SEPSIS – A Spectrum – Definitions • Systemic inflammatory response syndrome — SIRS is the clinical syndrome that results from a dysregulated inflammatory response to a noninfectious insult. It requires that two or more of the following abnormalities be present: • Temperature >38. 3ºC or <36ºC • Heart rate >90 beats/min • Respiratory rate >20 breaths/min or Pa. CO 2 <32 mm. Hg • WBC >12, 000 cells/mm 3, <4000 cells/mm 3, or >10 percent immature (band) forms Sepsis and the systemic inflammatory response syndrome: Definitions, epidemiology, and prognosis, www. uptodate. com, accessed 1/31/13 and 3/18/14

SEPSIS – A Spectrum – Definitions • Sepsis — Sepsis is the clinical syndrome that results from a dysregulated inflammatory response to an infection. Sepsis is defined as the presence (probable or documented) of infection together with systemic manifestations of infection. Diagnostic criteria for sepsis include infection (documented or suspected) and some of the following: Sepsis and the systemic inflammatory response syndrome: Definitions, epidemiology, and prognosis, www. uptodate. com, accessed 3/18/14

SEPSIS – A Spectrum – Definitions • General Variables T > 100. 9 or < 96. 8 HR > 90 bpm or > 2 std dev above ULN for age RR > 20 brpm Altered Mental Status Significant edema or positive fluid balance (>20 ml/kg over 24 hrs) Hyperglycemia >140 mg/dl in non-diabetic Sepsis and the systemic inflammatory response syndrome: Definitions, epidemiology, and prognosis, www. uptodate. com, accessed 3/18/14

SEPSIS – A Spectrum – Definitions • Inflammatory Variables Leukocytosis – WBC > 12, 000 Leukopenia – WBC < 4, 000 WBC WNL with > 10% bands Plasma nc. CRP > 2 std dev above ULN Plasma procalcitonin > 2 std dev above ULN Sepsis and the systemic inflammatory response syndrome: Definitions, epidemiology, and prognosis, www. uptodate. com, accessed 3/18/14

SEPSIS – A Spectrum – Definitions • Hemodynamic Variables Arterial hypotension – SBP < 90, MAP < 70, or SBP decrease > 40 mm. Hg from baseline or SBP < 2 std dev below LLN Sepsis and the systemic inflammatory response syndrome: Definitions, epidemiology, and prognosis, www. uptodate. com, accessed 3/18/14

SEPSIS – A Spectrum – Definitions • Organ Dysfunction Variables Arterial hypoxemia – Pa. O 2/Fi. O 2 < 300 Acute oliguria – UO < 0. 5 ml/kg/hr for 2 hrs Creatinine increase > 0. 5 mg/d. L Coagulopathy – INR > 1. 5 or a. PTT > 60 sec Absent bowel sounds Thrombocytopenia – plt < 100, 000 Hyperbilirubinemia – bili > 4 mg/d. L Sepsis and the systemic inflammatory response syndrome: Definitions, epidemiology, and prognosis, www. uptodate. com, accessed 3/18/14

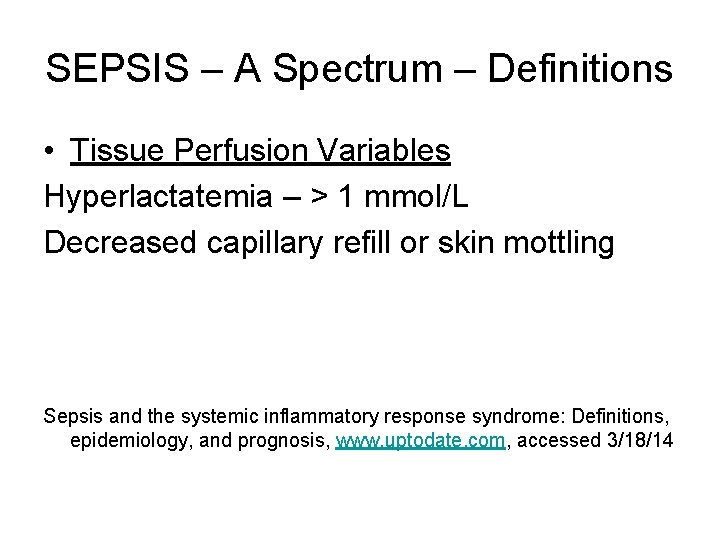
SEPSIS – A Spectrum – Definitions • Tissue Perfusion Variables Hyperlactatemia – > 1 mmol/L Decreased capillary refill or skin mottling Sepsis and the systemic inflammatory response syndrome: Definitions, epidemiology, and prognosis, www. uptodate. com, accessed 3/18/14

SEPSIS – A Spectrum – Definitions • Severe sepsis — Severe sepsis refers to sepsis plus at least one of the following signs of hypoperfusion or organ dysfunction: • Hypotension – SBP < 90, MAP < 70, or SBP decrease > 40 mm. Hg from baseline or SBP < 2 std dev below LLN • Lactate above ULN • Urine output <0. 5 m. L/kg for at least two hours despite adequate fluid resuscitation • Acute lung injury with Pa. O 2/Fi. O 2 < 250 with no pneumonia • Acute lung injury with Pa. O 2/Fi. O 2 < 200 with pneumonia • Platelet count < 100, 000 • Creatinine > 2 mg/d. L • Bilirubin > 2 mg/d. L • Coagulopathy with INR > 1. 5 Sepsis and the systemic inflammatory response syndrome: Definitions, epidemiology, and prognosis www. uptodate. com, accessed 3/18/14

SEPSIS – A Spectrum – Definitions • Septic shock — Septic shock is distributive (vasodilatory) shock defined as sepsis induced hypotension persisting despite adequate fluid resuscitation = 30 ml/kg crystalloid Sepsis and the systemic inflammatory response syndrome: Definitions, epidemiology, and prognosis, www. uptodate. com, accessed 3/18/14

SEPSIS – A Spectrum – Definitions • Multiple organ dysfunction syndrome — MODS refers to progressive organ dysfunction in an acutely ill patient, such that homeostasis cannot be maintained without intervention. It is at the severe end of the severity of illness spectrum of both SIRS and sepsis. MODS can be classified as primary or secondary: • Primary MODS is the result of a well-defined insult in which organ dysfunction occurs early and can be directly attributable to the insult itself (eg, renal failure due to rhabdomyolysis) • Secondary MODS is organ failure that is not in direct response to the insult itself, but is a consequence of the host’s response (eg, acute respiratory distress syndrome in patients with pancreatitis) There are no universally accepted criteria for individual organ dysfunction in MODS. However, progressive abnormalities of the following organ-specific parameters are commonly used as surrogate measures of organ function to diagnose MODS : • PO 2/Fi. O 2 ratio • Serum creatinine or urine output • Platelet count • Glasgow coma score • Serum bilirubin • Hypotension Sepsis and the systemic inflammatory response syndrome: Definitions, epidemiology, and prognosis www. uptodate. com, accessed 3/18/14

Case 1 • 75 Y. O. F. brought from N. H. with increased confusion, fever. In ED patient was lethargic, confused. Temp. 102. 5 F, BP 60/35, P 120. WBC was 24, 000 & U/A showed UTI What is your diagnosis? A. UTI B. Sepsis C. Severe Sepsis D. Septic Shock E. Who Cares

Case 1 • Above patient started on appropriate Abx as well as given Tylenol & 2 liter fluid bolus. 2 hours later pt. still lethargic, BP 70/40, P 110, temp. 99. 4 F What is your diagnosis? A. Sepsis B. Severe Sepsis C. Septic Shock D. Refractory Septic Shock E. Who knows

Case 1 • Above patient admitted to ICU, continued on appropriate Abx, IVF and Levophed. Pt. still lethargic, BP 80/45, P 104, Temp 98. 4 What is your diagnosis? A. Sepsis B. Severe Sepsis C. Septic Shock D. Refractory Septic Shock E. No idea

Case 2 • 72 Y. O. M. with history of Dementia had a fall at home. He has been having cough every time he eats and sometimes appeared to be choking with food. In ED temp. 101. 5, BP 110/65( close to his baseline), P. 80. M. S. at baseline per family. CXR with RLL infiltrate What is your diagnosis? A. Pneumonia B. Aspiration Pneumonia C. Sepsis D. Septic Shock E. None of above

Case 2 • You admitted the patient the beginning of your shift and started appropriate Abx, IVF. Several hours later while doing your rounds you found pt. more confused. Temp. 102. 2(despite Tylenol given), BP 108/62, P 110, R 24 What is your diagnosis? A. Pneumonia B. Aspiration Pneumonia C. Sepsis D. Septic Shock E. No idea

Case 3 • 75 Y. O. F. admitted for GI bleed. Foley catheter placed in ICU at time of admit. 4 days later pt. transferred to you with Foley in place. Several hours later you found patient confused, BP 120/70, P. 124, Temp 101. 9 What is your diagnosis? A. Pneumonia B. UTI C. SIRS D. Sepsis E. GI bleed

Case 3 • You call Dr. Alward regarding above pt. He ordered CXR, UA, CBC. CXR was negative, UA showed UTI, CBC pending. What is your diagnosis? A. Pneumonia B. UTI C. SIRS D. Sepsis E. All of above

SEPSIS Michael Williams DO, RPh Hospitalist Covenant Health. Care 2014

Objectives • • Get to know more about sepsis Get to know more about your patients Get better at “seein’ it comin’ a mile away” Get to know how you can start executing a series of interventions EARLY and just possibly save a patient’s life

SSC • Sepsis is a systemic, deleterious host response to infection leading to severe sepsis (acute organ dysfunction secondary to documented or suspected infection) and septic shock (severe sepsis plus hypotension not reversed with fluid resuscitation). Severe sepsis and septic shock are major healthcare problems, affecting millions of people around the world each year, killing 1 in 4 (and often more), and increasing in incidence. Similar to polytrauma, acute myocardial infarction, or stroke, the speed and appropriateness of therapy administered in the initial hours after sepsis develops are likely to affect the outcome.

Definition 2 • Sepsis is a clinical syndrome that complicates severe infection and is characterized by systemic inflammation and widespread tissue injury…tissues remote from the original insult display the cardinal signs of inflammation…

Definition 3 • Sepsis is SIRS (Systemic Inflammatory Response Syndrome) due to either a culture proven infection or an infection identified by visual inspection

So What Is SIRS? • SIRS is characterized by the presence of two or more of the following: • Temp > 100. 9°F or < 96. 8°F • HR > 90 bpm • RR > 20 or Pa. CO 2 < 32 mm Hg • WBC count > 12 k or < 4 k or > 10% bands

NOT SIRS

NOT Sepsis

Bedside Sepsis • • • Fever or Hypothermia Hyperventilation or SOB or Dyspnea Warm Skin or Cold and Clammy Possible Rash or Eruption Tachycardia Weakness or Malaise Chills and/or Rigors Confusion and/or Delirium Decreased Urine Output

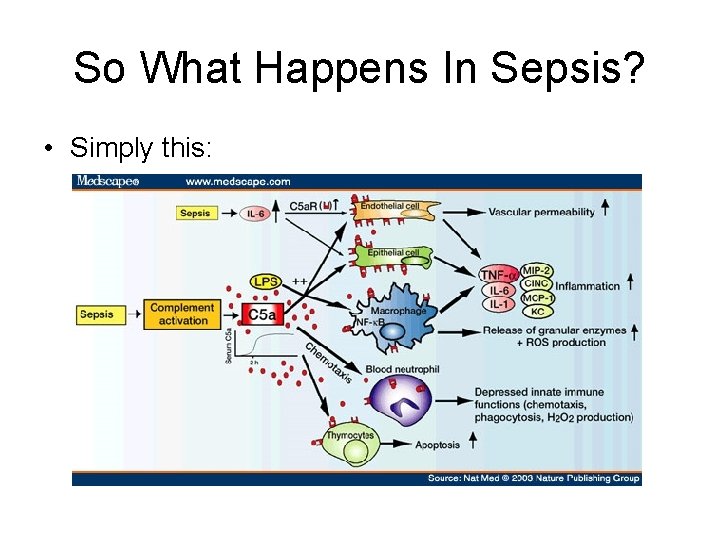
So What Happens In Sepsis? • Simply this:

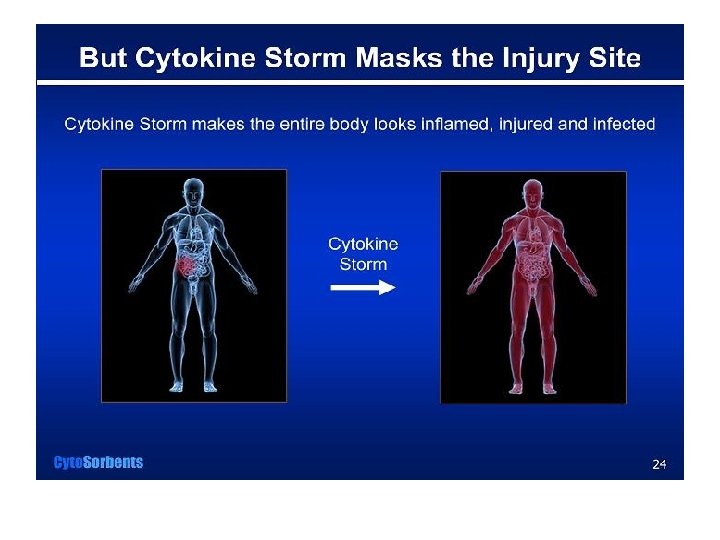
Let’s Break It Down • Sepsis results from the body’s natural inflammatory response directed against pathologic bacterial invasion, but the inflammation gets out of control and goes beyond the initial site of insult, affecting other distant organs and functions • Your septic patient is, therefore, just manifesting the signs and symptoms of this widespread inflammatory response

How Does This Get Started? • Remember, our environment (ie, the whole world) is populated with “critters” • Some good • Some bad

Good Critters • Beneficial organisms such as:

Bad Critters • Pathogenic bacteria, fungi, viruses such as:

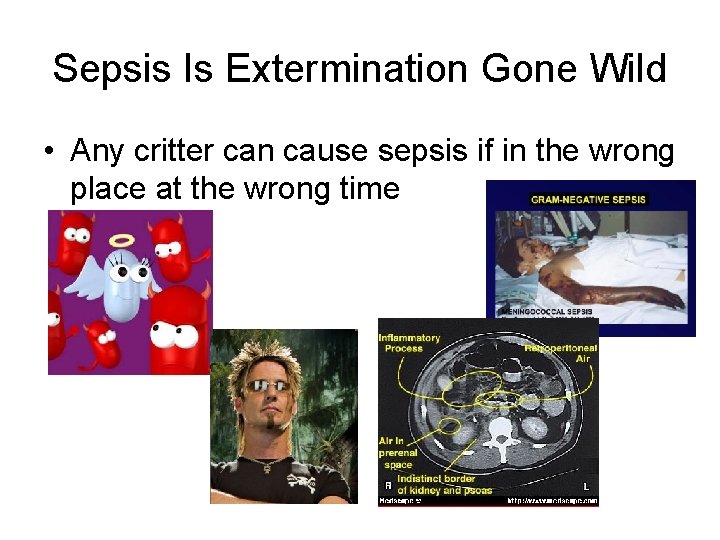
Sepsis Is Extermination Gone Wild • Any critter can cause sepsis if in the wrong place at the wrong time

The Inner Terminator • Everyone with an intact immune system will launch an attack on foreign invaders; if not, we’d all be like the “bubble boy” “It says Moops!”

Hasta La Vista, Baby • The immune system releases powerful reactive species, cytokines and toxins to neutralize threat

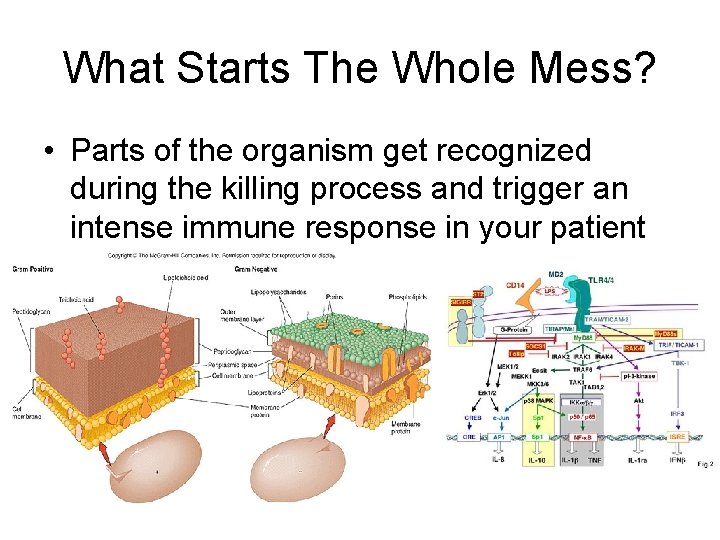
What Starts The Whole Mess? • Parts of the organism get recognized during the killing process and trigger an intense immune response in your patient

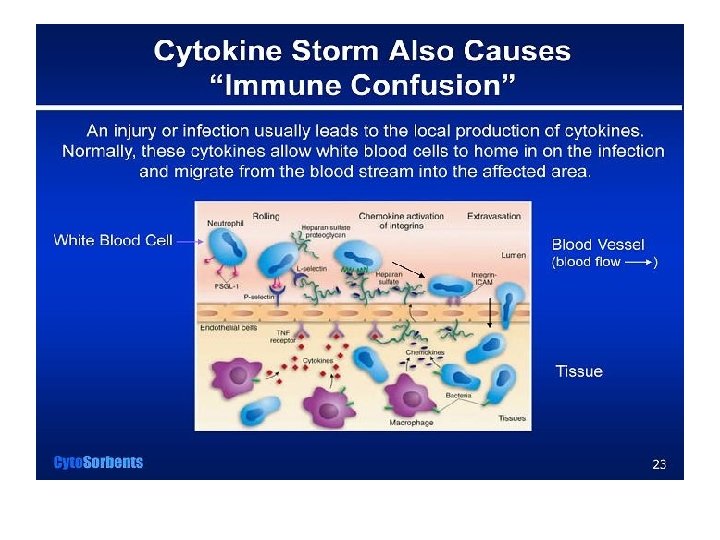
The Immune Response Intensifies • The normal process snowballs and a veritable feeding frenzy erupts

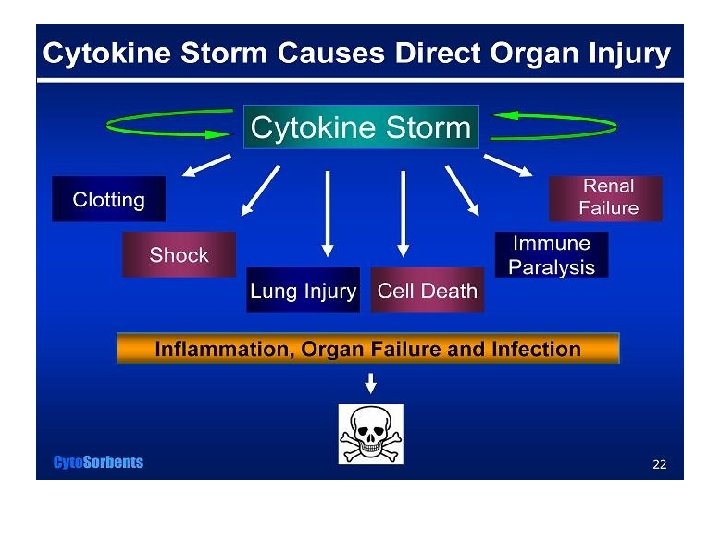
The Death Star Is Fully Functional • The cytotoxic efficacy of immunity is fine when targeted at the bad guys, but deadly when it overwhelms the patient’s body






On Your Mark, Get Set, Go! • Once you see the signs and symptoms of sepsis in your patient, the race is on to eliminate the infection before the body’s own extermination efforts spiral too far out of control • The body will try to kill the invader, but this can set off mechanisms that cause diffuse coagulation and resultant consumption coagulopathy, vascular leakage with tissue hemorrhage and edema, vascular dilatation and hypotension, etc, all leading to major organ dysfunction and failure

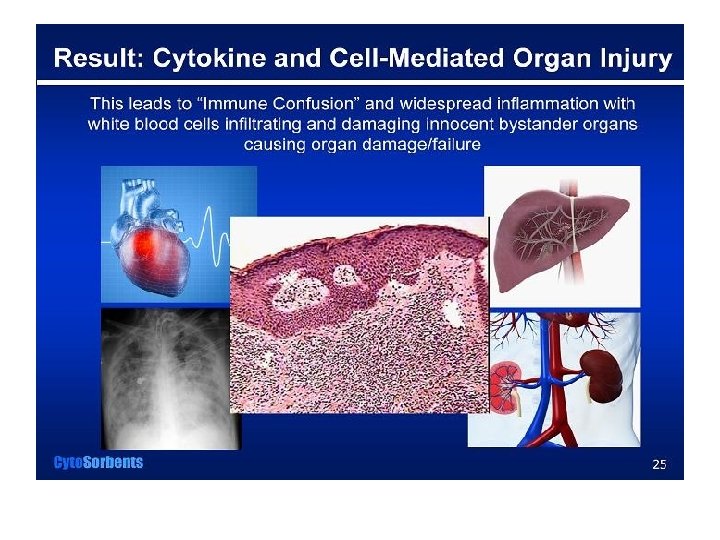
This Grim Story Is No Fairy Tale • Heart – decreased myocardial contractility aggravates systemic hypotension, decreasing blood flow to all of the body’s tissues, decreasing O 2 delivery and removal of toxic waste products everywhere • Lung – vascular leakage allows fluid into the alveoli causing pulmonary edema – fluid filled alveoli have decreased O 2 diffusion capacity, aggravating the decreased tissue oxygenation from circulatory collapse

Everything Means Everything • Liver – decreased blood flow and oxygenation lead to increased anaerobic metabolism (like everywhere else) and acidosis – shock liver, dysfunctional glucose control and decreased waste metabolism and elimination • Kidneys – hypotension and cytokine effects lead to decreased glomerular blood flow which decreases urine output leading to acute kidney injury which further decreases urine output – renal failure decreases systemic toxin removal

And I Mean Everything • Brain – decreased blood flow as well as glucose regulatory dysfunction and metabolic toxin buildup in the bloodstream leads to encephalopathy and altered mental status • Blood – nitric oxide, cytokines, acidosis and tissue factors released in the septic process cause vasodilatation and start the coagulation cascade – decreased effective circulating blood volume and thrombi blocking blood flow further, with, you guessed it, decreased O 2 delivery, etc

The Bottom Line • As we can see, sepsis only affects organs which depend on adequate nutrient and O 2 delivery and removal of waste products to maintain their normal function… • In essence the body’s immune response certainly seems like it can destroy the invader, but possibly only by destroying itself

So What Does All Of This Mean? • The signs and symptoms to recognize come from the underlying pathophysiology • Fever/Rigors – immune challenge • Tachypnea/Dyspnea – pulmonary edema and acidosis • Tachycardia – decreased cardiac output, hypotension and effective volume loss • Decreased UO – decreased renal blood flow and glomerular filtration cause kidney injury • Delirium – decreased cerebral blood flow, glucose problems and buildup of systemic toxins

The Game Is On • Like dominos, the first step starts the chain reaction that takes everything with it • Critters stimulate toxin, cytokine and mediator production which causes decreased blood flow to occur, which causes more cytokines and mediators to be released which damages organs that can’t do their jobs which leads to more toxin buildup, less tissue perfusion, etc • Is it any wonder that sepsis is in the top 10 causes of death according to the CDC?

What To Do? • If you believe your patient has sepsis: • Airway and Breathing – supplement O 2 and intubate if necessary • Circulation – treat hypotension and hypoperfusion with crystalloid administration – this would not be a good time to find the pt has no IV access • Treat the infection

Bugs And Drugs • If you believe that your patient is becoming septic, recall the definition – inflammatory signs plus infection; supportive care…then • Mental checklist of infectious processes: • Urine, especially if a foley is present • Skin, especially central access or wounds • Lung, keep in mind aspiration with AMS • Blood cultures

Better Living Through Chemistry • Start broad spectrum empiric antibiotic coverage ASAP • Urine – think gram negative organisms • Line/Wound – think skin flora • Lung – community acquired or health care associated, think aspiration with AMS • Cultures – always get them, before starting antibiotics if possible • Antibiotics can be narrowed later

Bottom Line circa 2006 • Administration of an antimicrobial effective for isolated or suspected pathogens within the first hour of documented hypotension was associated with a survival rate of 79. 9%. Each hour of delay in antimicrobial administration over the ensuing 6 hrs was associated with an average decrease in survival of 7. 6%.

• What’s the word In 2014? Freshest perspectives on good ol’ common sense…

We’re All In This Together • “Most of these recommendations are appropriate for the severe sepsis patient in the ICU and non-ICU settings. In fact, the committee believes that the greatest outcome improvement can be made through education and process change for those caring for severe sepsis patients in the non-ICU setting and across the spectrum of acute care. ” www. ccmjournal. org February 2013 • Volume 41 • Number 2

Cliff Notes circa 2013 • Have a high index of suspicion; you can’t diagnose what you don’t think of • Act quickly with ABCs and supportive care • Monitor closely for signs of deterioration, remember, this is a chain reaction • If you recall the pathophysiology, you can reinforce and target your bedside assessment and intervention

So what? • • Nurses are indispensible team members, period Examination - can’t treat what you don’t know Data – get vitals – portal into the pathophysiology Sure, there all kinds of things that the doctor needs to order – labs, ABGs, CTs, Xrays, EKGs, dopplers, echo, fluids, pressors, antibiotics, vent, etc • BUT – assessment and vitals can be done by you or others at the bedside with the equipment you already have available and without further orders – your judgment makes it happen and could save a life

Case 1 • 75 Y. O. F. brought from N. H. with increased confusion, fever. In ED patient was lethargic, confused. Temp. 102. 5 F, BP 60/35, P 120. WBC was 24, 000 & U/A showed UTI What is your diagnosis? A. UTI B. Sepsis C. Severe Sepsis D. Septic Shock E. Who Cares

Case 1 • Above patient started on appropriate Abx as well as given Tylenol & 2 liter fluid bolus. 2 hours later pt. still lethargic, BP 70/40, P 110, temp. 99. 4 F What is your diagnosis? A. Sepsis B. Severe Sepsis C. Septic Shock D. Refractory Septic Shock E. Who knows

Case 1 • Above patient admitted to ICU, continued on appropriate Abx, IVF and Levophed. Pt. still lethargic, BP 80/45, P 104, Temp 98. 4 What is your diagnosis? A. Sepsis B. Severe Sepsis C. Septic Shock D. Refractory Septic Shock E. No idea

Case 2 • 72 Y. O. M. with history of Dementia had a fall at home. He has been having cough every time he eats and sometimes appeared to be choking with food. In ED temp. 101. 5, BP 110/65( close to his baseline), P. 80. M. S. at baseline per family. CXR with RLL infiltrate What is your diagnosis? A. Pneumonia B. Aspiration Pneumonia C. Sepsis D. Septic Shock E. None of above

Case 2 • You admitted the patient the beginning of your shift and started appropriate Abx, IVF. Several hours later while doing your rounds you found pt. more confused. Temp. 102. 2(despite Tylenol given), BP 108/62, P 110, R 24 What is your diagnosis? A. Pneumonia B. Aspiration Pneumonia C. Sepsis D. Septic Shock E. No idea

Case 3 • 75 Y. O. F. admitted for GI bleed. Foley catheter placed in ICU at time of admit. 4 days later pt. transferred to you with Foley in place. Several hours later you found patient confused, BP 120/70, P. 124, Temp 101. 9 What is your diagnosis? A. Pneumonia B. UTI C. SIRS D. Sepsis E. GI bleed

Case 3 • You call Dr. Alward regarding above pt. He ordered CXR, UA, CBC. CXR was negative, UA showed UTI, CBC pending What is your diagnosis? A. Pneumonia B. UTI C. SIRS D. Sepsis E. All of above

SEPSIS • Where our helpful biological processes can become our mortal enemies. Capisce?

Powerpointus Terminatum QUESTIONS?