Sepsis PALS April 24 2017 Disclosures No Conflict

















- Slides: 31

Sepsis PALS April 24, 2017

Disclosures No Conflict of Interests or Potential Conflicts of Interests to Declare

Objectives 1)Review the differences between adult and pediatric septic shock 2)Identify key elements during the initial management of pediatric sepsis that will improve patient outcomes

Pediatric vs. Adult Sepsis Cardiac Dysfunction Dehydration Sepsis Vasoplegia

Pediatric vs. Adult Sepsis Cardiac Dysfunction Dehydration Sepsis Vasoplegia

Pediatric vs. Adult Sepsis Cardiac Dysfunction Dehydration Sepsis Vasoplegia

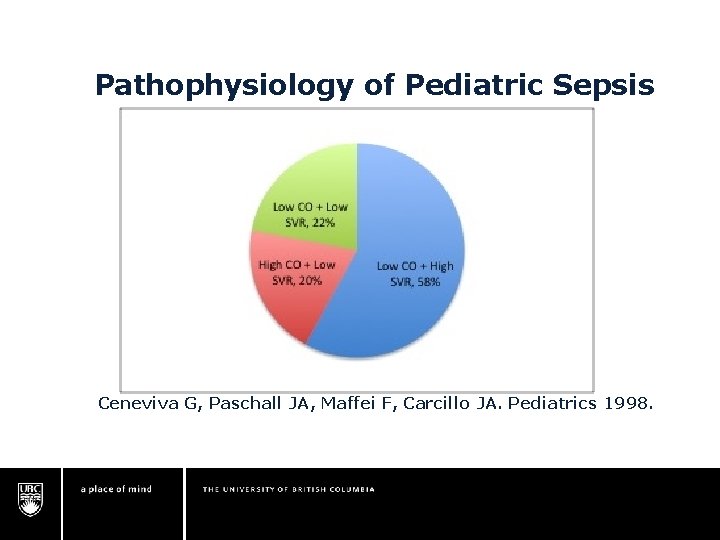
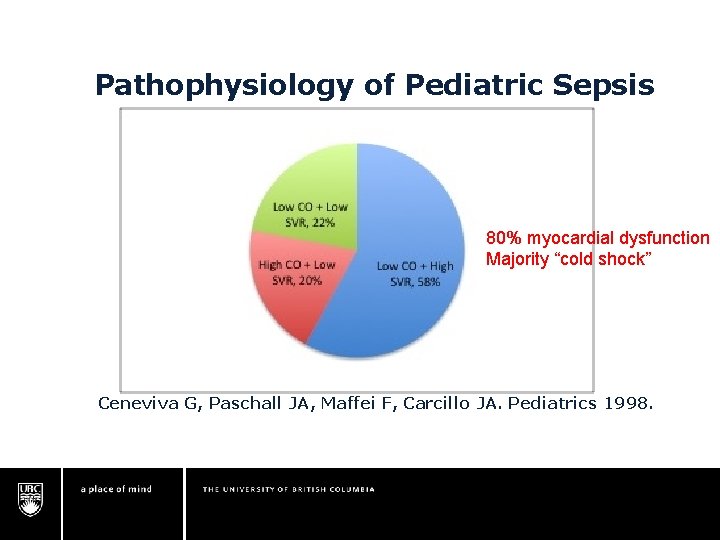
Pathophysiology of Pediatric Sepsis Ceneviva G, Paschall JA, Maffei F, Carcillo JA. Pediatrics 1998.

Pathophysiology of Pediatric Sepsis 80% myocardial dysfunction Majority “cold shock” Ceneviva G, Paschall JA, Maffei F, Carcillo JA. Pediatrics 1998.

Goals of Therapy 1)Recognition of sepsis within 5 minutes 1)IV access within 5 minutes 1)Antibiotic delivery within 60 minutes 1)Delivery of 60 m. L/kg fluids within 60 minutes 1)Administration of vasoactive substance within 60 minutes 2010 PALS Guidelines: Septic Shock

Recognition of Sepsis Suspected infection suggested by hyper or hypothermia AND: Cold Shock (Majority) Warm Shock (Minority) Decreased or altered LOC Prolonged CRT > 2 secs Diminished pulses Mottled cool extremities Decreased urine output Decreased or altered LOC Flash capillary refill Bounding peripheral pulses Wide pulse pressure Decreased urine output Note: Hypotension is not a required feature

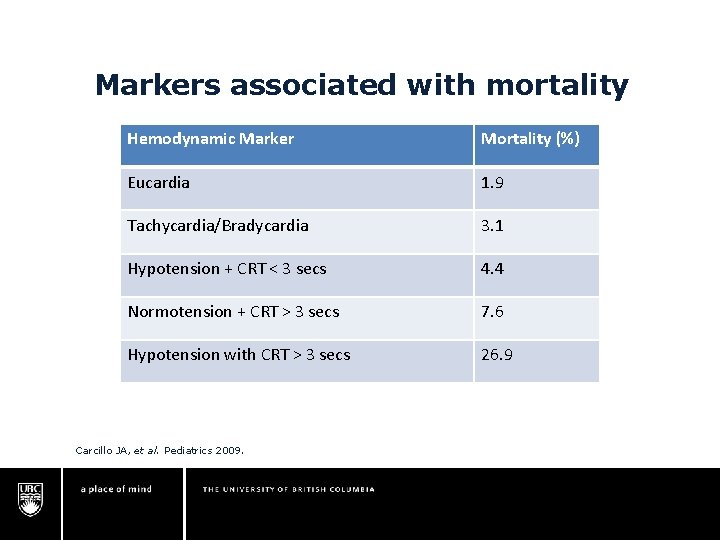
Markers associated with mortality Hemodynamic Marker Mortality (%) Eucardia 1. 9 Tachycardia/Bradycardia 3. 1 Hypotension + CRT < 3 secs 4. 4 Normotension + CRT > 3 secs 7. 6 Hypotension with CRT > 3 secs 26. 9 Carcillo JA, et al. Pediatrics 2009.

Goals of Therapy 1)Recognition of sepsis within 5 minutes 1)IV access within 5 minutes 1)Antibiotic delivery within 60 minutes 1)Delivery of 60 m. L/kg fluids within 60 minutes 1)Administration of vasoactive substance within 60 minutes 2010 PALS Guidelines: Septic Shock

IV Access IO insertion Rapid and successful insertion Equivalent pharmacokinetics ACCM 2007 Guidelines Peripheral inotropes until central access obtained Recommendation: If rapid IV access is not achieved, IO should be inserted Voight J, Waltzman M, Lottenberg L. Ped Emerg Care 2012. 2007 ACCM Guidelines 2010 PALS Guidelines

Goals of Therapy 1)Recognition of sepsis within 5 minutes 1)IV access within 5 minutes 1)Antibiotic delivery within 60 minutes 1)Delivery of 60 m. L/kg fluids within 60 minutes 1)Administration of vasoactive substance within 60 minutes 2010 PALS Guidelines: Septic Shock

Antibiotic Therapy Antibiotic therapy within the first hour: Decreased mortality by 13. 5% 7. 6% decrease in survival for each hour delayed Antibiotic Choice (no source): Cloxacillin 50 mg/kg IV q 6 h OR Vancomycin 15 mg/kg IV Cefotaxime 50 mg/kg IV q 6 h Antibiotic Choice (source): www. childhealthbc. ca Aneja RK, Varughese-Aneja R, Vetterly CG, Carcillo JA. Curr Infect Dis Rep 2011. Gaieski DF, et al. Crit Care Med 2010. Kumar A, et al. Crit Care Med 2006.

Goals of Therapy 1)Recognition of sepsis within 5 minutes 1)IV access within 5 minutes 1)Antibiotic delivery within 60 minutes 1)Delivery of 60 m. L/kg fluids within 60 minutes 1)Administration of vasoactive substance within 60 minutes 2010 PALS Guidelines: Septic Shock

IV fluid administration Crystalloid vs. Albumin 3 adult metanalyses published in 2014 Pediatric data weak Albumin may have some advantage Recommendation: Availability should dictate choice of crystalloid or albumin. Jian L, Jian S, Zhang M, Zheng Z, Ma Y. PLo. S One 2014. Xu JY, et al. Crit Care 2014. Pater A, Laffan MA, Waheed U, Brett SJ. BMJ 2014. Akech S, Ledermann H, Maitland K. BMJ 2010. Maitland K, et al. Clin Infect Dis 2005 Ford N, Hargreaves S, Shanks L. PLo. S One 2012.

IV fluid administration ACCM 2007 Target 60 m. L/kg within first 15 minutes PALS 2010//2015 Target 60 m. L/kg within first 1 hour Goal of fluid resuscitation Restoring normal mental status, restoring threshold HRs, CRT < 3 secs, palpable peripheral pulses, normal blood pressure Carcillo JA, Davis AL, Zaritsky A. JAMA 1991. Wills BA, et al. NEJM 2005.

IV fluid administration Methods for rapid fluid administration 1)Rapid Infuser 1)Pressure Bag 1)Push-Pull Technique

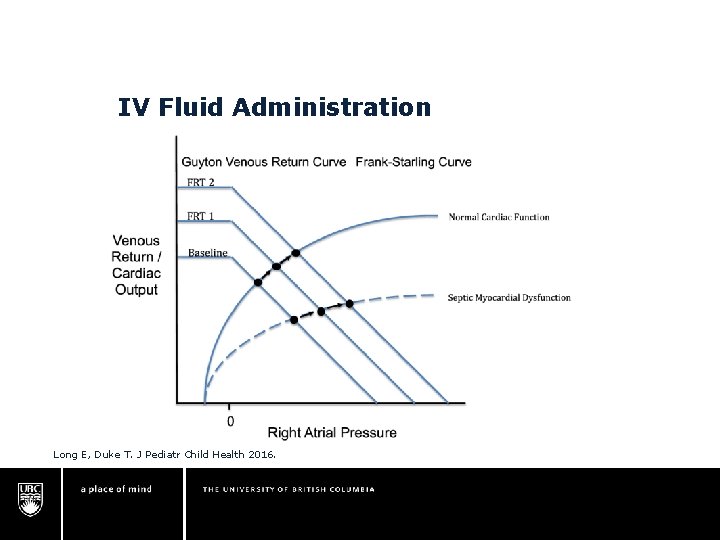
IV Fluid Administration Long E, Duke T. J Pediatr Child Health 2016.

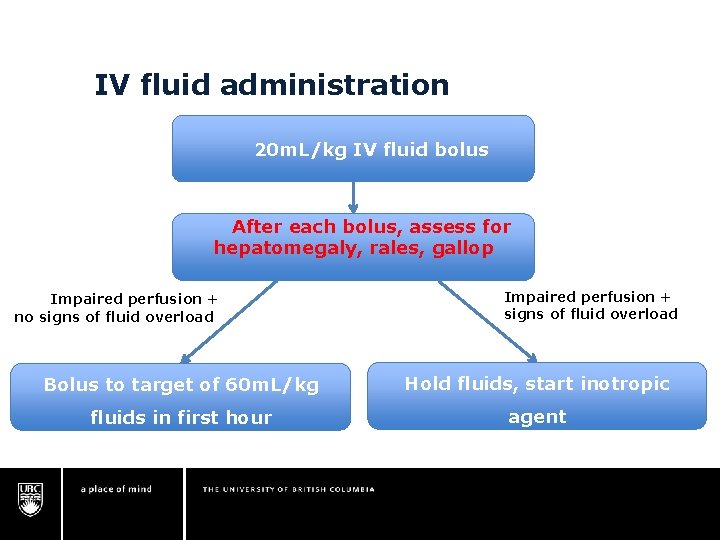
IV fluid administration 20 m. L/kg IV fluid bolus After each bolus, assess for hepatomegaly, rales, gallop Impaired perfusion + no signs of fluid overload Impaired perfusion + signs of fluid overload Bolus to target of 60 m. L/kg Hold fluids, start inotropic fluids in first hour agent

Goals of Therapy 1)Recognition of sepsis within 5 minutes 1)IV access within 5 minutes 1)Antibiotic delivery within 60 minutes 1)Delivery of 60 m. L/kg fluids within 60 minutes 1)Administration of vasoactive substance within 60 minutes 2010 PALS Guidelines: Septic Shock

Vasoactive Agents Early inotropes improves mortality, and can be run peripherally Traditionally dopamine was initial agent New Recommendations (initial agent): Peripherally Epinephrine (0. 05 to 0. 3 mcg/kg/min) Centrally Epinephrine (cold shock) or norepinephrine (warm Ninis N, et al. BMJ 2005. ACCM 2007 El-wither N, Cornell T, Kissoon N, Shanley TP. Open Inflamm J 2011. www. childhealthbc. ca shock)

Airway and Breathing High-flow oxygen Intubate patients with: Substantially increased work of breathing Hypoventilation Altered LOC or obtundation Consider intubation in: Patients with persistent or worsening shock >40 m. L/kg ACCM 2007. Booy R, et al. Arch Dis Child 2001.

Airway and Breathing Intubation Medications: Atropine 0. 02 mg/kg (0. 1 to 1 mg) Ketamine 1 to 2 mg/kg Avoid Etomidate* IV fluids and vasoactive agents before and during intubation Tarquinio KM, et al. Pediatr Crit Care Med 2015. ACCM 2007 PALS 2010 Gu WJ, Wang F, Tang L, Liu JC. Chest 2015.

Glucose and Calcium Glucose demands increase in sepsis High risk of hypoglycemia Ionized calcium frequently low in sepsis Treat if i. Ca < 1. 10 mmol/L Recommendations: Run IV D 10 NS at maintenance Correct hypocalcemia

Steroids Paucity of literature in pediatric patients Trend to benefit to steroids in pediatric sepsis Recommendations: Steroids should be given in patients with purpura fulminans, previous steroid therapies for chronic illness, hypothalamic/pituitary or adrenal abnormalities (including CAH) Dose: 1 – 2 mg/kg (insufficiency) to 50 mg/kg (shock reversal) Baseline cortisol level prior to administration Menon K, Mc. Nally D, Choong K, Sampson M. Pediatr Crit Care Med 2013. ACCM 2007

Future Directions Fluid-Sparing Strategies FEAST Trial SQUEEZE Trial Albumin vs. Crystalloid Epinephrine vs. Dopamine 2 studies suggesting benefit with epinephrine Maitland K, et al. NEJM 2011. Ford N, Hargreaves S, Shanks L. PLo. S One 2012. Ventura AMC, et al. CCMJ 2015. Ramaswamy KN, et al. PCCM 2016.

Summary Recognize Sepsis! www. childhealthbc. ca Airway/Breathing Atropine + Ketamine Avoid Etomidate Fluids and vasoactive agents Circulation Early IO insertion Rapid fluid delivery 60 m. L/kg in first hour IF no fluid overload Epinephrine 1 st line agent

Summary Antibiotics Deliver in 1 st hour: Cefotaxime + Cloxacillin/Vancomycin Glucose and Calcium Run D 10 NS at maintenance + normalize ionized calcium Steroids Patients with absolute adrenal insufficiency Call for help early!

Thank You Questions?