Sentinel Injuries in Physical Abuse Leslie Strickler DO

Sentinel Injuries in Physical Abuse Leslie Strickler DO FAAP Associate Professor of Pediatrics University of New Mexico Children’s Hospital Medical Director, Child Abuse Response Team (CART)

Objectives • Define sentinel injury • Identify common presentations of sentinel injury • Sentinel injury case review • Review recommended medical evaluation in presentations of sentinel injuries

Definitions of Sentinel Injury • A visible or otherwise detectable minor injury in a pre-mobile infant that is poorly explained therefore concerning for child abuse • Often clinically insignificant from a treatment perspective • Heal quickly and completely without direct sequelae

Definition of sentinel injury An injury recognized retrospectively as being an indicator of abuse • Typically involves pre-mobile infants • Is recognized by caretaker, and often includes history inconsistent with cause or severity of injury • An injury associated with a higher rate of diagnosis of abuse

Types of Sentinel Injury • Sentinel Injury breakdown • 80% bruises • Including subconjunctival hemorrhage • 11% Intraoral injury • 7% fracture Sheets, L. et al. Sentinel Injury in Infants Evaluated for Child Physical Abuse. Pediatrics 2013; 131: 701 -707.

Frequency and Significance of Sentinel Injury • Retrospective Case Control • 401 infants <12 months pf age evaluated by hospital based child abuse team • Of 200 diagnosed as abused, 27. 5% had sentinel injuries • Of 100 indeterminate for abuse, 8% had sentinel injuries • Of 101 non-abused infants, 0% had sentinel injuries Sheets, L. et al. Sentinel Injury in Infants Evaluated for Child Physical Abuse. Pediatrics 2013; 131: 701 -707

Case 1 • 4 -month-old female, presented to UNM pediatric urgent care clinic with CC of right arm redness and decreased use/movement discovered by parents after waking from sleep. No trauma reported.

Case 1 • Exam noted discomfort on abduction and flexion of right shoulder and swelling of right upper arm • X-ray: acute transverse fracture of right humeral diaphysis • No other injuries on skeletal survey and head CT • Bruising to pad of right index finger identified on CART exam

Acute humerus fracture
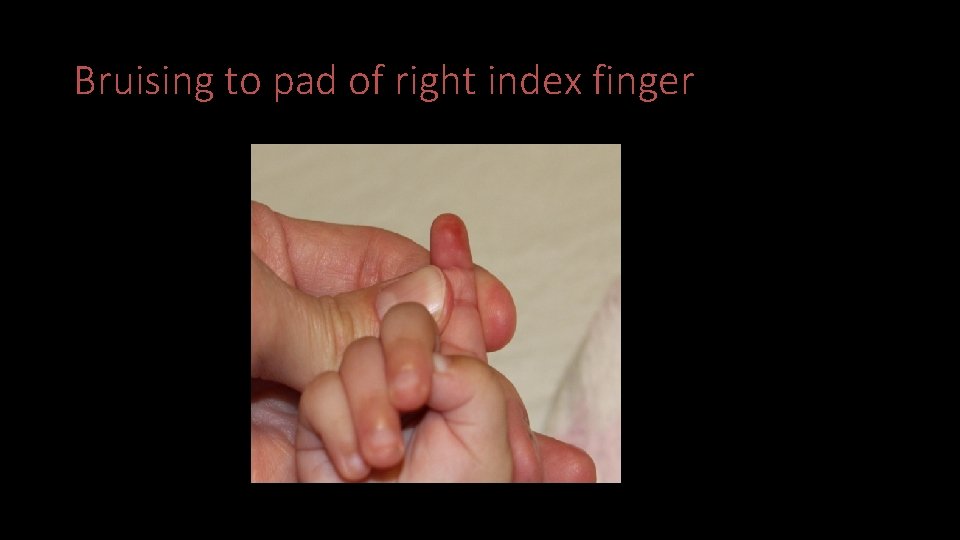
Bruising to pad of right index finger

Case 1 • Medical record review revealed visit to UNM Pediatric Emergency Department approx. 2 weeks prior for small bleeding cut under tongue noted by father after infant woke from a nap. • This history was not independently disclosed by parents during CART consultation

Case 1 Prior ED Course • No history of trauma other than parental report that infant puts things in her mouth due to teething • No PO intake by infant since injury noted • ED exam noted small linear laceration inferior to tongue, anterior to frenulum without active bleeding. No other injuries on exam. • Differential Diagnosis: Mouth laceration, NAT • Discharged without PO challenge due parental persistence in desiring to go home • No Referral to protective services or child abuse pediatrician

Case 2 • 3 -month-old male, presented to community ED after father reported noting a “pop” after infant’s arm inadvertently became stuck behind his back during swaddling.

Case 2 • X-ray identified acute oblique mid to distal diaphyseal fracture of the left humerus. • Father then changed history stating he fell while holding the baby, and the baby’s arm was outstretched. • CYFD/Law Enforcement notified and infant transferred to UNM for CART consult
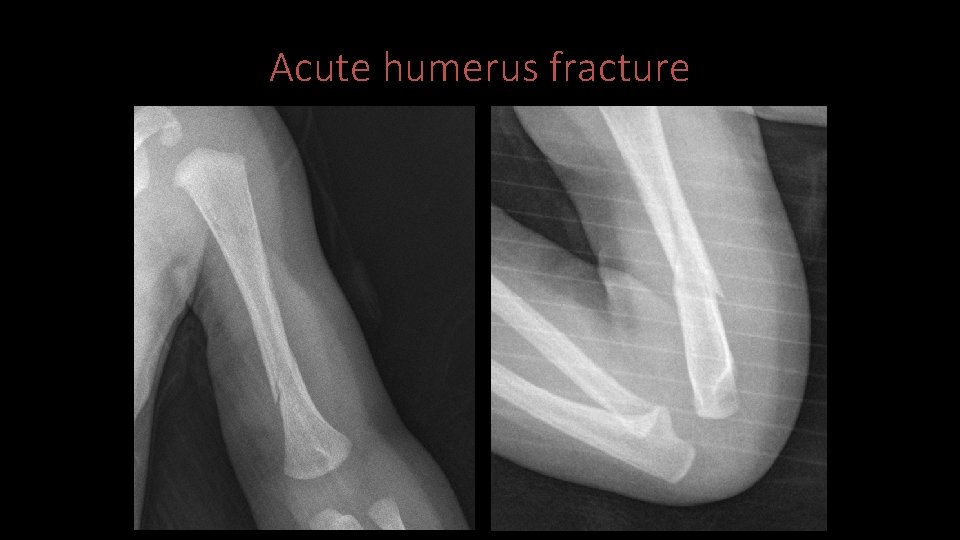
Acute humerus fracture

Case 2 • CART exam notable for healed transection of superior labial frenulum, left upper arm swelling, and multiple linear petechial bruises on the left leg • No additional injuries identified on skeletal survey and head CT
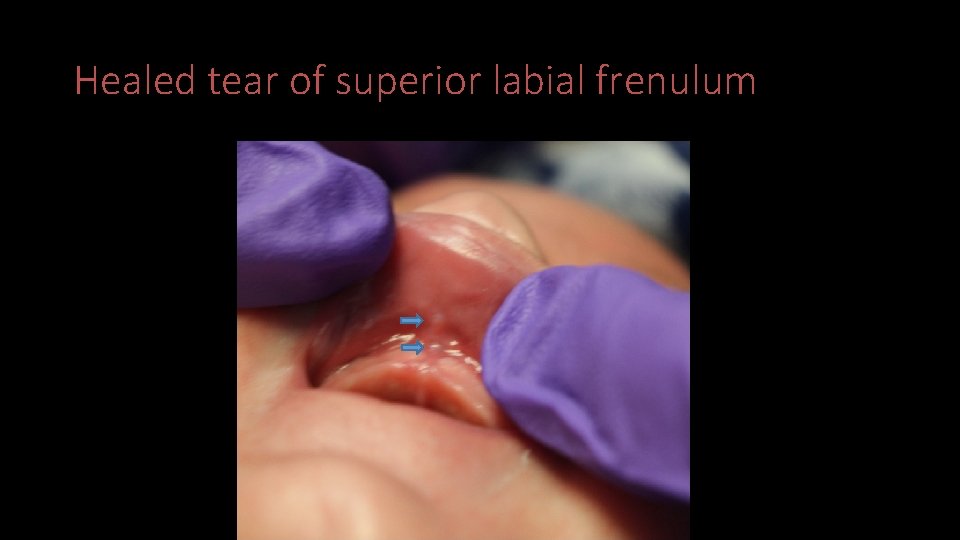
Healed tear of superior labial frenulum
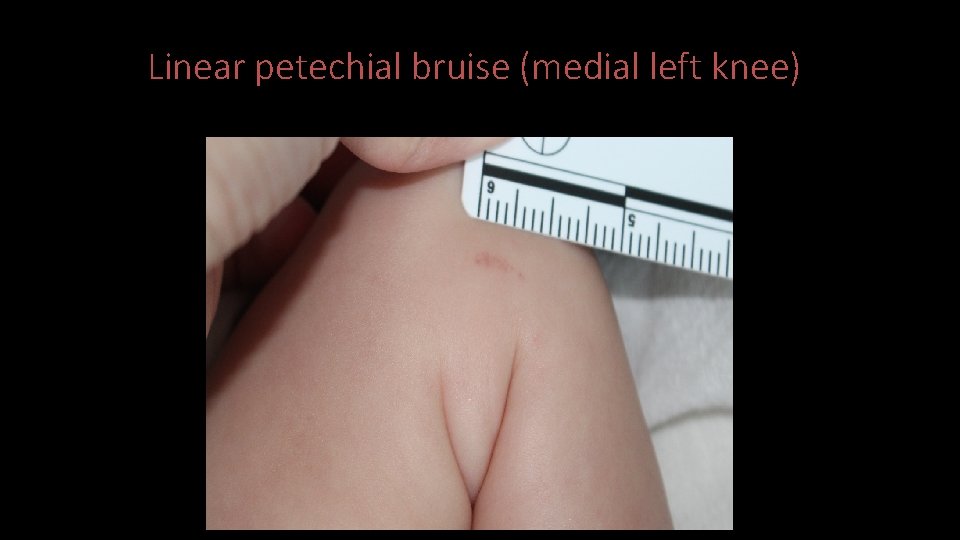
Linear petechial bruise (medial left knee)
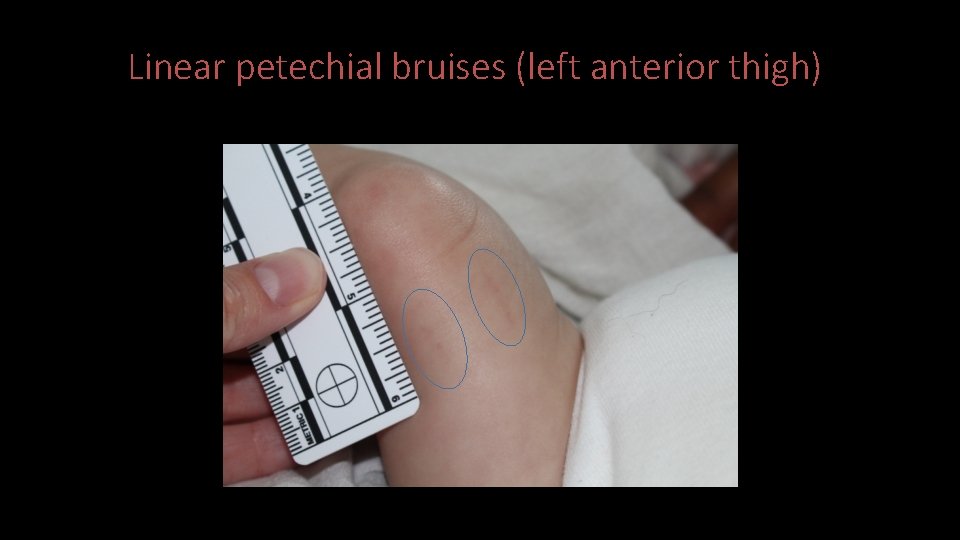
Linear petechial bruises (left anterior thigh)
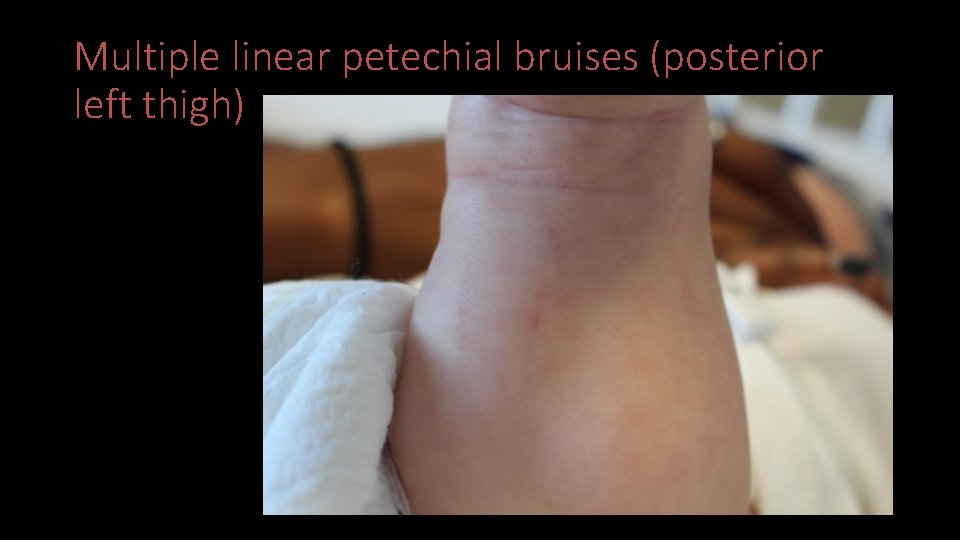
Multiple linear petechial bruises (posterior left thigh)

Case 2 • CART medical record review revealed UNM Peds ED visit approx. 2 weeks prior and admission for fussiness, poor feeding, and intermittent bleeding of a “lesion” on the mucosa of the central upper lip, pointed out by father to clinicians. • No trauma history was reported • 3 day admission with initial IVF requirement • Discharge without clear “inciting” event identified, no referral to protective services or child abuse pediatrician

Case 3 2 month infant admitted to community hospital with fever and Streptococcus pneumonia bacteremia and meningitis.

Case 3 • Fever recurred near day 10 of antibiotic treatment • Chest x-ray obtained which revealed a healing clavicle fracture • Same fracture was recognized in retrospect on chest x-ray obtained at admission • Infant transferred to UNM due to concern for physical abuse

Case 3 • Skeletal survey • Multiple healing rib fractures • One corner metaphyseal fracture • Scapular fracture • Fractures of phalanges • Physical Exam • Healing tear of superior labial frenulum • History • Mother reported frequent intra-oral bleeding on ROS
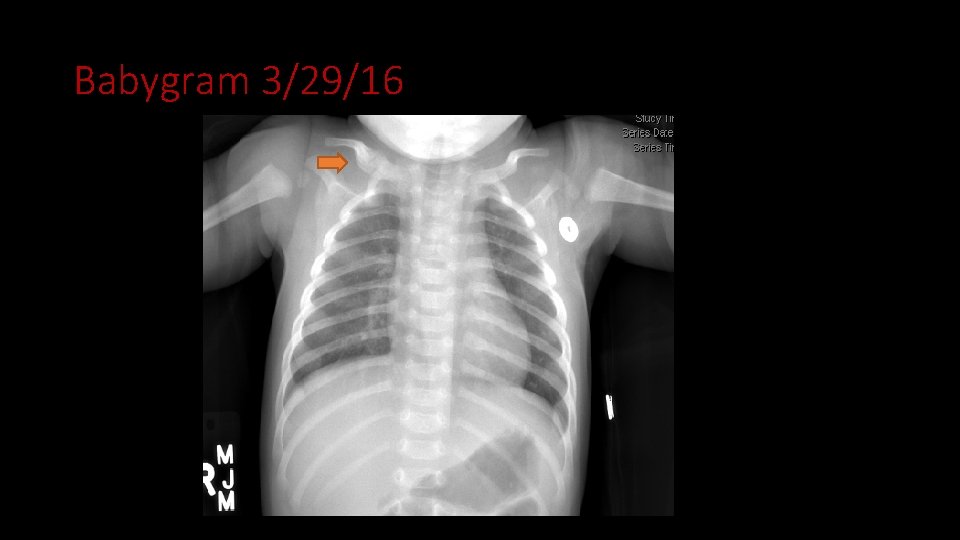
Babygram 3/29/16
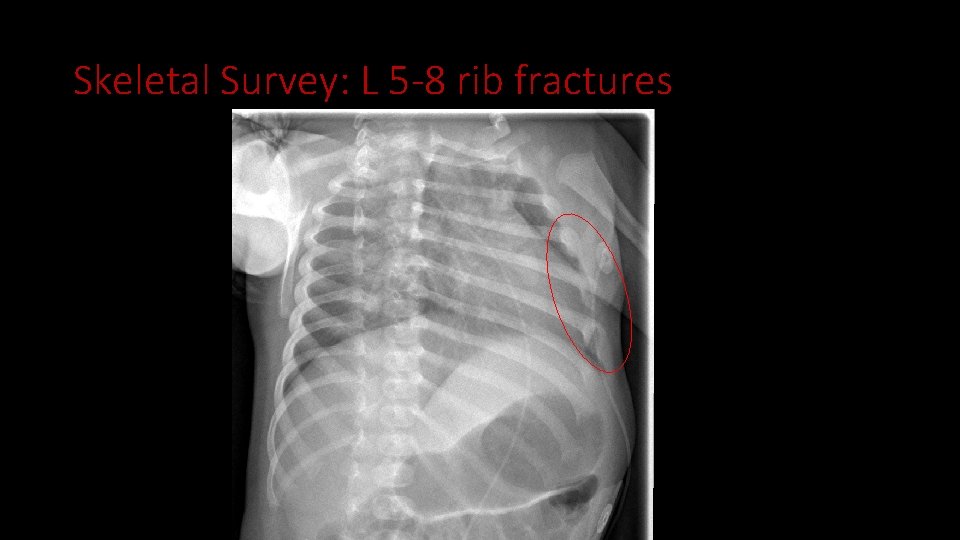
Skeletal Survey: L 5 -8 rib fractures
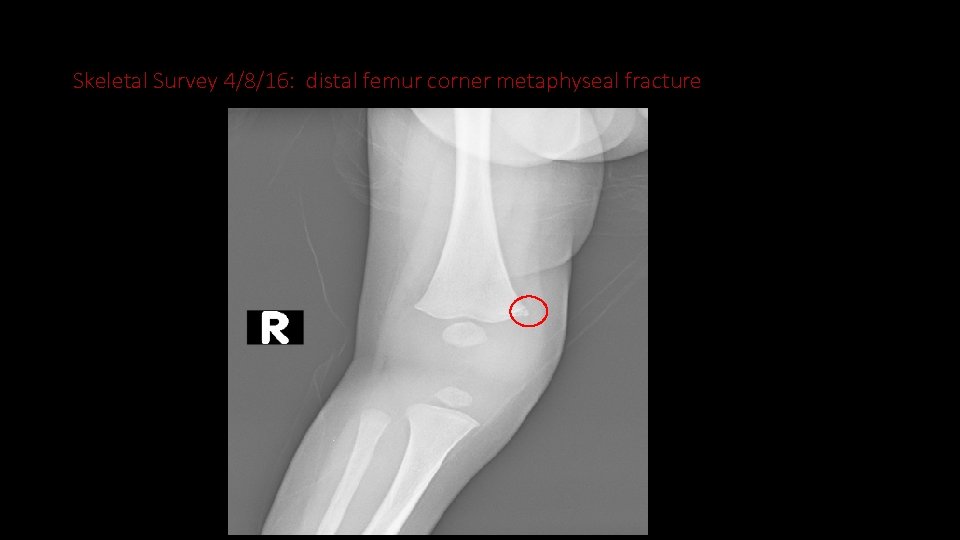
Skeletal Survey 4/8/16: distal femur corner metaphyseal fracture
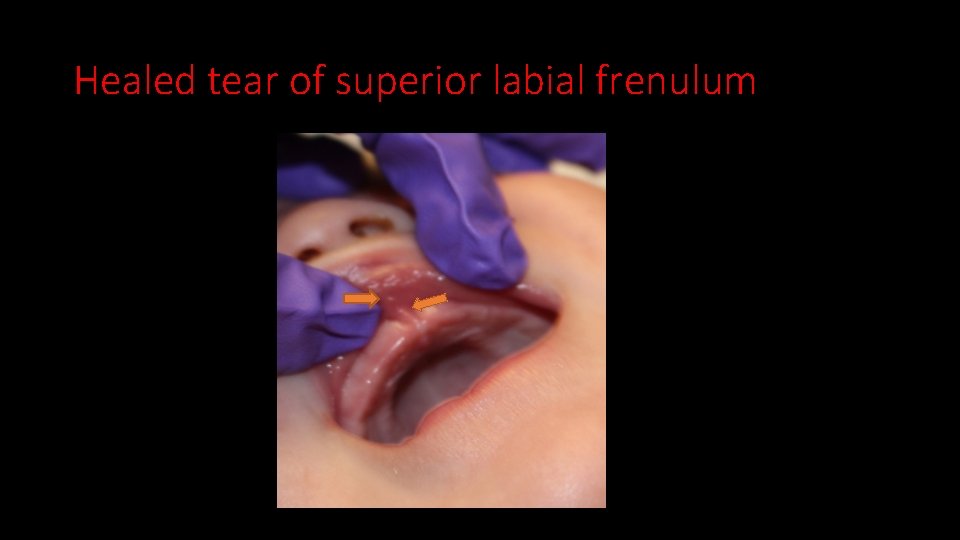
Healed tear of superior labial frenulum

Case 3 • Medical Record Review • urgent care visit 2 weeks prior to meningitis diagnosis for bruising of tongue, and abrasion to palate and lower inner lip. • Variable traumatic histories provided including infant striking face on father’s shoulder and infant’s tooth causing oral injury *Infant was edentulous • Reported epistaxis 2 days prior to meningitis diagnosis *Streptococcus Pneumonia is typical nasopharyngeal flora

Clinical course at UNM • Prolonged S. pneumoniae meningitis course complicated by ventriculitis and empyema requiring PICC line and extended parenteral therapy

Oral/Nasal Injuries • History: unexplained epistaxis, hematemesis, choking/gagging, feeding difficulty, or respiratory distress • Perform a thorough intra-oral/nasopharyngeal examination for history of oral bleeding or epistaxis in a young infant • Mechanisms: direct blow to mouth or forced insertion of object into mouth or nose • Refer to a Child Abuse Pediatrician! Maguire S. Diagnosing abuse: a systematic review of torn frenum and other intra-oral injuries. Arch Dis Child, 2007; 92: 1113 -1117. Walton L. Nasal bleeding in non-accidental injury in an infant. Arch Dis Child, 2010; 95: 54 -54.
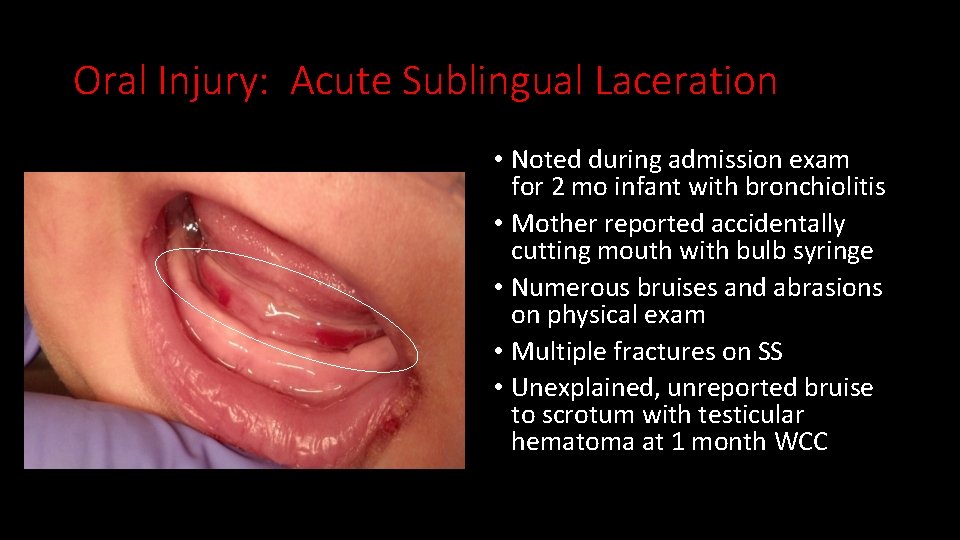
Oral Injury: Acute Sublingual Laceration • Noted during admission exam for 2 mo infant with bronchiolitis • Mother reported accidentally cutting mouth with bulb syringe • Numerous bruises and abrasions on physical exam • Multiple fractures on SS • Unexplained, unreported bruise to scrotum with testicular hematoma at 1 month WCC
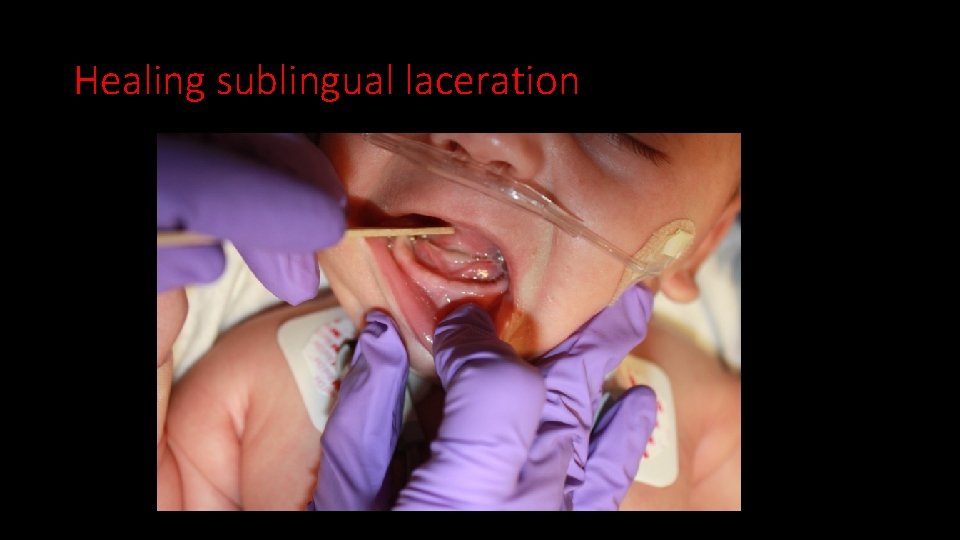
Healing sublingual laceration
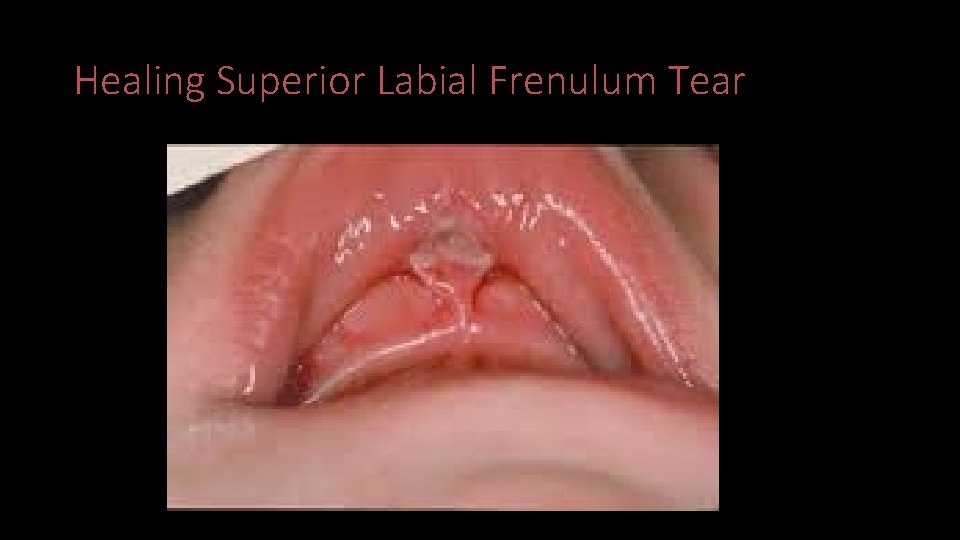
Healing Superior Labial Frenulum Tear

Medical Evaluation in Sentinel Injury • Detailed medical history and history of injury/presentation • Thorough medical examination with attention to skin, oral cavity, neurologic, and palpatory musculoskeletal exam

Medical Evaluation in Sentinel Injury • IMAGING • SKELETAL SURVEY (SS) • 11 -13% of children <2 years of age evaluated for suspected abuse have occult injury on SS • 25 -30% of children <2 years of age with a clinical diagnosis of physical abuse have occult injury on SS Belfer, RA et al. Use of the skeletal survey in the evaluation of child maltreatment. Am J Emer Med. 2001; 19(2): 122 -124 Day, F et al. A retrospective case series of skeletal surveys in children with suspected non-accidental injury. J Clin Forensic Med. 2006; 13(2): 55 -59

Medical Evaluation in Sentinel Injury • NEUROIMAGING (Non-contrast Head CT or MRI) • Approx. 30 -40% of neurologically normal children < 2 years of age with high risk presentation for abuse have occult head injury identified on imaging. • Laskey, A et al. Occult head trauma in young suspected victims of physical abuse. J Pediatr. 2004; 144: 719 -722 • Rubin, D et al. Occult head injury in high risk abused children. Pediatrics. 2003; 111: 1382 -1386.

Clinical Pearls • Further explore any history or sign of injury in pre-mobile infants • If it doesn’t cruise, it shouldn’t bruise, break, or bleed from it’s mouth or nose! • Perform detailed oral cavity exam on all infants presenting with history of bleeding/injury, difficulty feeding, difficulty breathing, hemoptysis, hematemesis, or epistaxis • Refer unexplained injury in pre-mobile infants • Protective Services • Law Enforcement • CART

Parting Thoughts • Child Abuse is an under-reported national epidemic • Children in New Mexico are disproportionately affected • Ignoring abuse will not make it go away • Severity escalates with time • Report suspicion, refer for evaluation • Accurate diagnosis is prevention!

Thriving New Mexico Child!
- Slides: 40