Semen Analysis and Sperm Preparation VASECTOMY TUTORIAL 4












- Slides: 13

Semen Analysis and Sperm Preparation VASECTOMY TUTORIAL (4)

Semen Analysis SA are mainly carried out to determine whether: A man has a reproductive problem that is causing infertility. A vasectomy or vasectomy reversal has been successful A semen analysis to test the effectiveness of a vasectomy is usually done 16 weeks after the vasectomy

Ways to Collect Semen Masturbation, directing the semen into a clean sample cup. Do not use a lubricant which can kill sperms Coitus interruptus - withdrawing the penis from the partner just before ejaculating follow by ejaculating into a clean sample cup. Coitus - by using a condom. A special (silicon) condom that does not contain any substance that kills sperm (spermicide). After ejaculation, carefully remove the condom from the penis. Tie a knot in the open end of the condom and place it in a container that can be sealed in case the condom leaks or breaks. Ordinary condoms should not be used since they usually contain spermicides

Semen analysis (post vasectomy) The specimen must be collected in the morning. You must not have had sex or masturbated for 48 hours before collecting the sample but should have had an abstinence period of no longer than seven days. First wash your hands and genitals with soap and water, please ensure complete removal of all soap residues and dry thoroughly.

Semen Collection Good and reliable SA results starts from semen collection, preferably by masturbation • Abstinence days 2 -6 • Pass urine • Wash hands with soap, dry • Collect the entire sample into the wide mouth sterile container, 70% of sperms is in the first part of the ejaculate • Keep the sample at body temperature, no sunlight • Deliver the sample within one hour of ejaculation

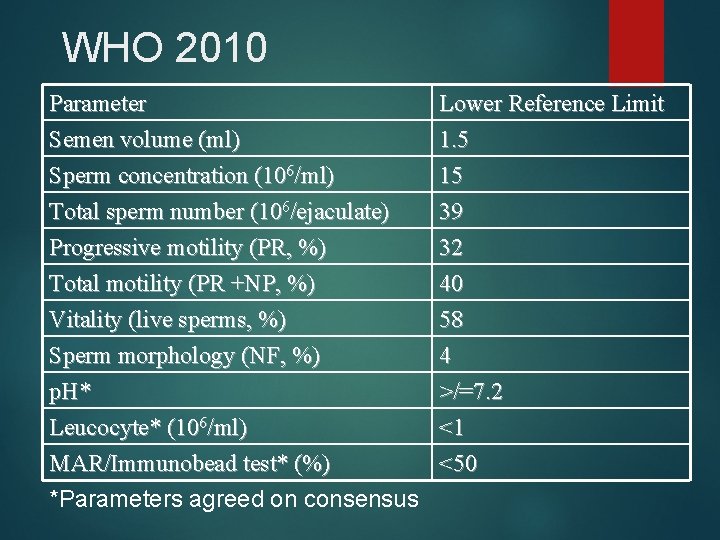
WHO 2010 Parameter Semen volume (ml) Sperm concentration (106/ml) Total sperm number (106/ejaculate) Lower Reference Limit 1. 5 15 39 Progressive motility (PR, %) Total motility (PR +NP, %) Vitality (live sperms, %) Sperm morphology (NF, %) p. H* Leucocyte* (106/ml) MAR/Immunobead test* (%) 32 40 58 4 >/=7. 2 <1 <50 *Parameters agreed on consensus

Terminologies of SA Oligospermia – sperm concentration <15 million/ml Asthenozoospermia – <40% grade (PR+NP) or < 32 PR% Teratozoospermia – <4% spermatozoa OAT =Oligo-astheno-teratozoospermia Azoospermia – no spermatozoa in semen Polyzoospermia – ++ high sperm concentration, >200 M/ml Hypospermia – semen volume < 1. 5 ml Hyperspermia – semen volume > 6. 0 ml Aspermia – no semen volume Pyospermia – leukocytes present in semen, >1 M/ml Hematospermia – red blood cell present in semen Necrozoospermia – “dead” sperm

EARLY FAILURE OF SURGERY Both technical failure (such as missed vasa deferentia) and early recanalisation of the vas deferens have been documented. In a large study of 16 796 vasectomy operations carried out within one centre in the UK, the surgeons reported a failure to achieve sterility in 72 men. This early failure rate was quoted as 0. 36%, and has been linked to operator experience Early failures were usually identified by the presence of motile spermatozoa in ejaculates examined three to six months postoperatively, and surveys have suggested that many surgeons will opt to repeat surgery as soon as possible.

LATE FAILURE Late failure is defined as the presence of spermatozoa in ejaculates after documented azoospermia in two post vasectomy semen analyses. Although uncommon, the late failure rate has been reported to be 0. 04– 0. 08%, and recanalisation is usually only discovered after pregnancy in the female partner. It has been suggested that because women may not inform their partners of a pregnancy for fear of being accused of infidelity, but may seek a termination, the late failure rate may be an underestimate. Similarly, the identification of spermatozoa in 9. 7% of ejaculates from a group of 186 men undergoing semen assessment prereversal of their vasectomy also suggests an under reporting of late recanalisation.

CLEARANCE The RCOG and FPA guidelines state that at least two azoospermic consecutive samples two to four weeks apart must be obtained before contraceptive precautions can be dispensed with. Recent studies have re-emphasised this period as appropriate. It is the responsibility of clinicians not the laboratory to communicate the results of semen assessments to their patients. A large proportion of patients (up to 25%) fail to submit post vasectomy semen specimens for assessment, 27, 28, 33 or fail to comply with instructions regarding sample collection, making reliable laboratory assessment impossible.

Special Clearance The persistence of scanty (less than 10, 000/ml) sperm in 2 consecutively examined semen samples at least 7 months after vasectomy.

Between 1980 and 1985, 6067 out-patient vasectomies were performed under local anaesthesia at the elliot smith clinic in oxford. During this period 151 men (2. 5%) were given a "special clearance". Further specimens of semen requested after a minimum follow-up of 3 years (range 3 -8); 50 patients supplied a specimen and all except 1 were azoospermic. No pregnancies attributable to failure of the vasectomy have been identified.

Special Clearance Persistent non-motile spermatozoa in the initial two ejaculates is not uncommon, with studies reporting up to 33% non-azoospermic samples at three months, and 10% of ejaculates containing non-motile sperm at six months. In one prospective study, the median time to azoospermia was 10 weeks, with most men (93%) being azoospermic by week Similarly, sperm can reappear in ejaculates 12 months after surgery, despite previous sperm free ejaculates. Discussion in the literature has suggested that the risk of pregnancy occurring from these non-motile sperm is small, and probably no more than the risk of pregnancy after two azoospermic semen samples, as a result of spontaneous recanalisation. It has been suggested that repeat ejaculates seven months after surgery are probably unnecessary because pregnancy is very unlikely to occur.