Selfadministration of medication in hospital the perspectives of










![Participants (n=124) Male (%) Age (mean [range]) Level of education (%) Primary school or Participants (n=124) Male (%) Age (mean [range]) Level of education (%) Primary school or](https://slidetodoc.com/presentation_image_h/263615f21a7ef43bcfbcc9634a8b2c12/image-20.jpg)



- Slides: 28

Self-administration of medication in hospital: the perspectives of patients and health care providers Prof. dr. Tinne Dilles dra. Toke Vanwesemael www. Nu. Pha. C. eu

Introduction Health • “the ability to adapt and self-manage in the face of social, physical, and emotional changes” SELF-MANAGEMENT • paternalistic approach active partner in health and disease management Self-management of medication The process in which patients prepare and consume medications themselves rather than a health professional taking over this role. Advantages: • Increased patient satisfaction • Improvement of adherence to pharmacotherapy • Improvement of self-care competences • Safety? • Time? Page 2 Huber, 2011; Orem, 2001, Barnason, 2010; Bolster, 2010; Lam, 2011; Tran, 2011; Wright, 2006

Belgium Prevalence of self-administration (1, 269 hospitalized patients) Actual prevalence – at least one medicine: 22% – >50% of medicines: 14% – All medicines: 6% Potential prevalence – 41% would be able to fully self-administer (perspective nurses) Support (59 hospital departments) 18 % has a procedure. 7% has a screening tool Page 3

Research aim To explore health care providers’ and patients’ perspectives concerning self-administration of medication whilst in hospital, and to describe adaptations required for implementation. Page 4

Methodology Qualitative study – Descriptive research design (Sandelowski, 2000) – October 2014 – January 2015 – Random selected wards of 1 regional & 2 university hospitals – Purposive sampling strategy • Nurses, physicians, hospital pharmacists Exclusion: not directly involved in management of patients’ medication • Patients Exclusion: <18 years, mentally and/or physically not able to participate – Semi-structured interviews (SWOT – conditions) – Qualitative content analysis (Hsieh & Shannon, 2005) Page 5

Qualitative descriptive design SWOT OF SELF-MANAGEMENT OF MEDICATION Page 6

Participants • 6 physicians; a pulmonologist, geriatricians, an endocrinologist, a cardiologist and a nephrologist. • 11 nurses; pulmonology-nephrology, gastro-oncology, geriatrics, general surgery, endocrinology, nephrology, neurology, gastroenterology and cardiologynephrology • 6 hospital pharmacists; • 7 patients; gastro-oncology, pulmonology-nephrology, general surgery, endocrinology, nephrology, gastroenterology and cardiology-nephrology. Page 7

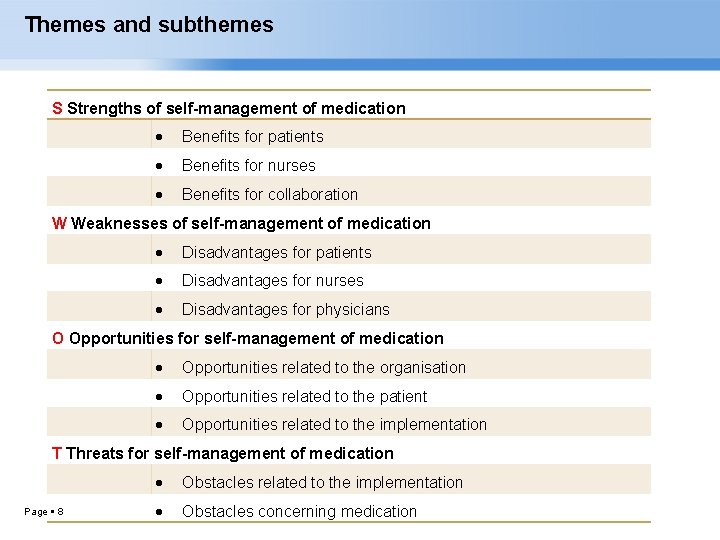
Themes and subthemes S Strengths of self-management of medication Benefits for patients Benefits for nurses Benefits for collaboration W Weaknesses of self-management of medication Disadvantages for patients Disadvantages for nurses Disadvantages for physicians O Opportunities for self-management of medication Opportunities related to the organisation Opportunities related to the patient Opportunities related to the implementation T Threats for self-management of medication Obstacles related to the implementation Obstacles concerning medication Page 8

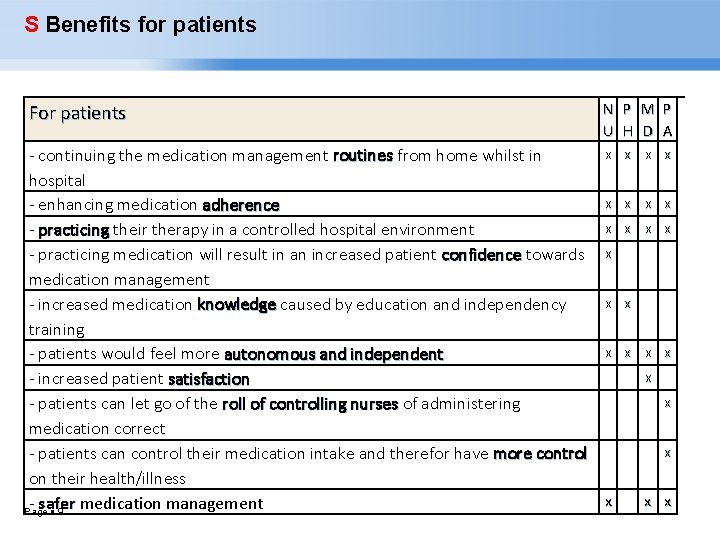
S Benefits for patients For patients - continuing the medication management routines from home whilst in routines hospital - enhancing medication adherence - practicing their therapy in a controlled hospital environment - practicing medication will result in an increased patient confidence towards confidence medication management - increased medication knowledge caused by education and independency knowledge training - patients would feel more autonomous and independent - increased patient satisfaction - patients can let go of the roll of controlling nurses of administering medication correct - patients can control their medication intake and therefor have more control on their health/illness - safer medication management Page 9 N P M P U H D A x x x x x x x x x x

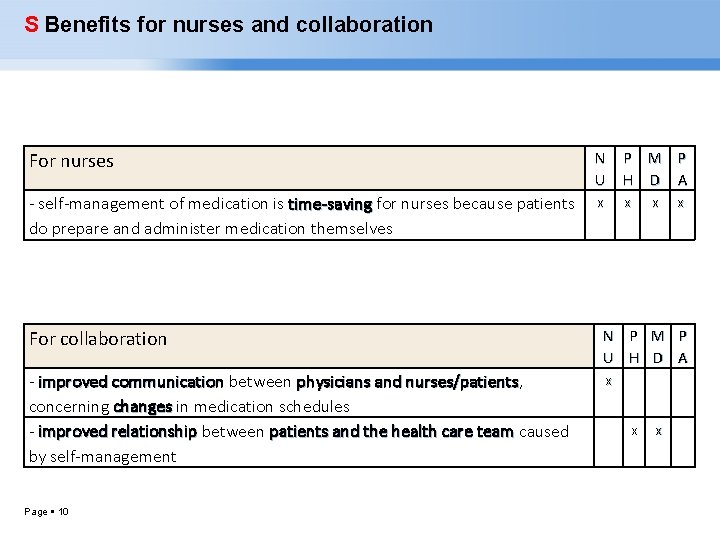
S Benefits for nurses and collaboration N U x - self-management of medication is time-saving for nurses because patients time-saving P M P H D A x x x For nurses do prepare and administer medication themselves For collaboration - improved communication between physicians and nurses/patients, nurses/patients concerning changes in medication schedules changes - improved relationship between patients and the health care team caused by self-management Page 10 N P M P U H D A x x x

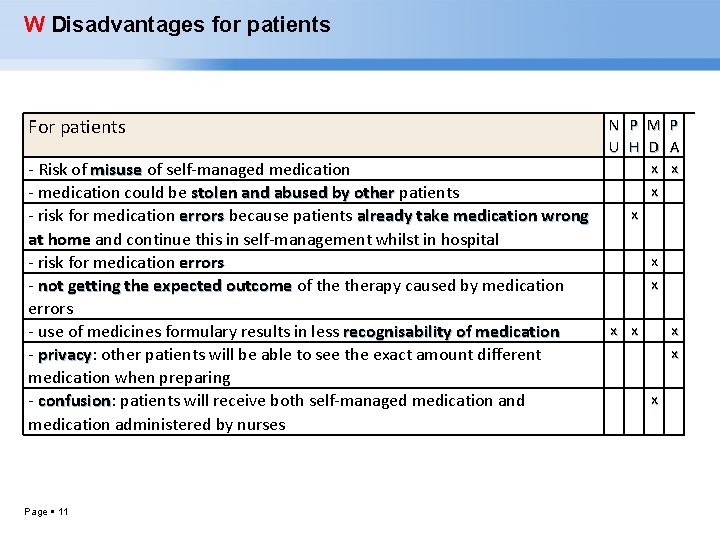
W Disadvantages for patients For patients - Risk of misuse of self-managed medication misuse - medication could be stolen and abused by other patients - risk for medication errors because patients already take medication wrong errors at home and continue this in self-management whilst in hospital home - risk for medication errors - not getting the expected outcome of therapy caused by medication errors - use of medicines formulary results in less recognisability of medication - privacy: other patients will be able to see the exact amount different privacy medication when preparing - confusion: patients will receive both self-managed medication and confusion medication administered by nurses Page 11 N U P H x M D x x P A x x x x

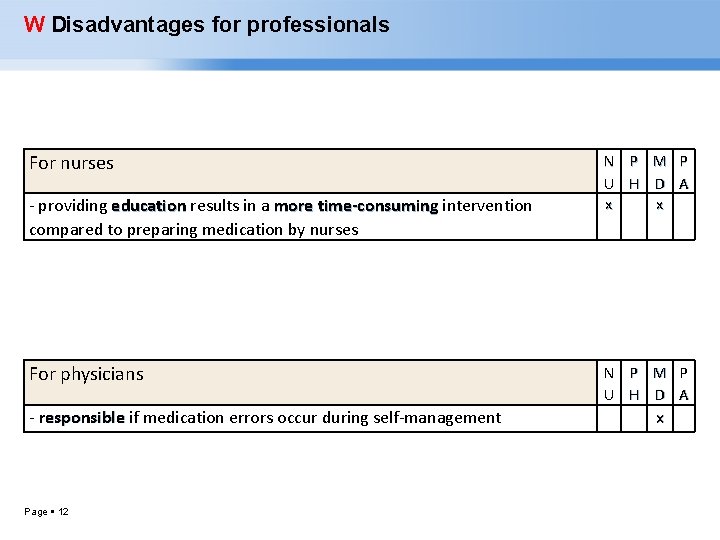
W Disadvantages for professionals For nurses - providing education results in a more time-consuming intervention education compared to preparing medication by nurses N P M P U H D A x x For physicians N P M P U H D A - responsible if medication errors occur during self-management responsible Page 12 x

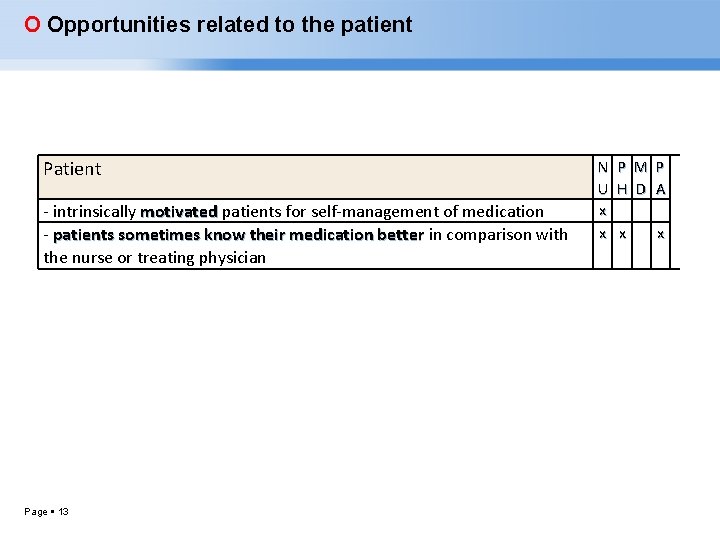
O Opportunities related to the patient Patient - intrinsically motivated patients for self-management of medication motivated - patients sometimes know their medication better in comparison with the nurse or treating physician Page 13 N U x x P H x M D P A x

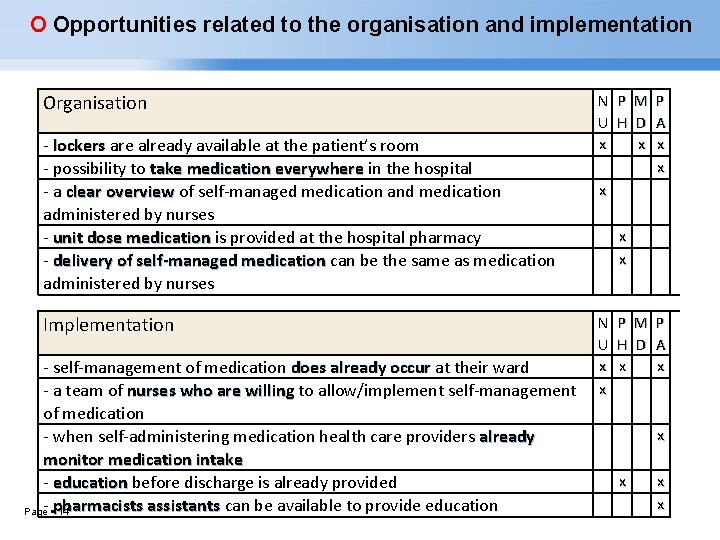
O Opportunities related to the organisation and implementation Organisation - lockers are already available at the patient’s room lockers - possibility to take medication everywhere in the hospital - a clear overview of self-managed medication and medication overview administered by nurses - unit dose medication is provided at the hospital pharmacy - delivery of self-managed medication can be the same as medication administered by nurses Implementation - self-management of medication does already occur at their ward - a team of nurses who are willing to allow/implement self-management of medication - when self-administering medication health care providers already monitor medication intake - education before discharge is already provided education - pharmacists assistants can be available to provide education Page 14 N U x x P H M D x P A x x x N U x x P H x M D P A x x x

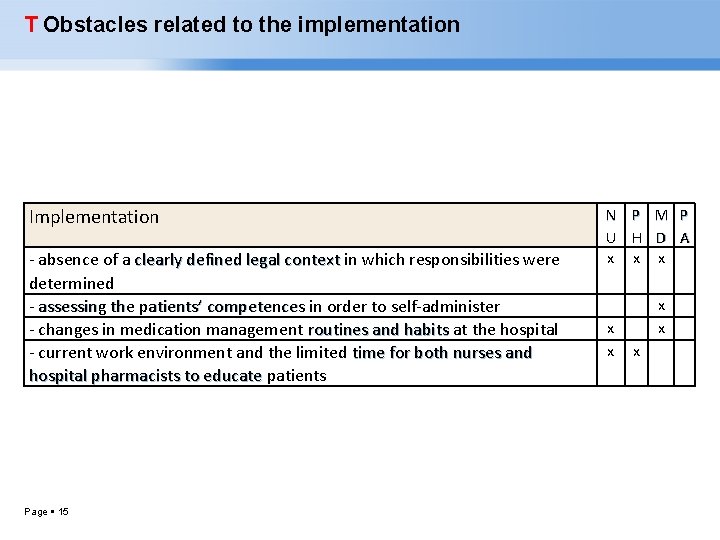
T Obstacles related to the implementation Implementation - absence of a clearly defined legal context in which responsibilities were clearly defined legal context determined - assessing the patients’ competences in order to self-administer assessing the patients’ competences - changes in medication management routines and habits at the hospital routines and habits - current work environment and the limited time for both nurses and hospital pharmacists to educate patients hospital pharmacists to educate Page 15 N P M P U H D A x x x x

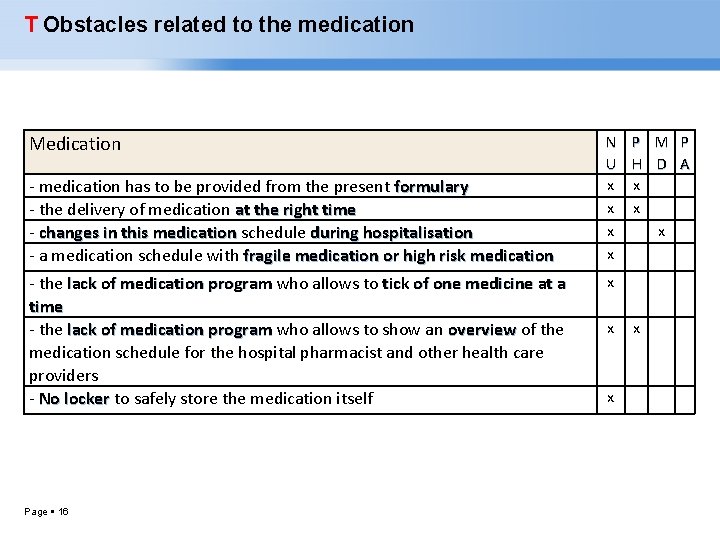
T Obstacles related to the medication Medication - medication has to be provided from the present formulary - the delivery of medication at the right time - changes in this medication schedule during hospitalisation - a medication schedule with fragile medication or high risk medication - the lack of medication program who allows to tick of one medicine at a time - the lack of medication program who allows to show an overview of the medication schedule for the hospital pharmacist and other health care providers - No locker to safely store the medication itself Page 16 N P M P U H D A x x x x

Conditions to allow self-management in hospital Patient: Self-management before admission and after discharge Patient is willing to self-manage and to take responsibility Adequate mental and physical condition Adequate knowledge about self-managed medication Medication: Low risk medication Regimen not to complex No intravenous, intramuscular, subcutaneous medication Organisation: Software to support self-management (overview, distinction, registration) Clear legal context (responsibilities) Monitoring system Lockers for medication Protocol and flow chart including medication logistics and interprofessional communication Page 17

A quantitative survey desing PATIENTS’ ATTITUDES TOWARDS SELF-MANAGEMENT OF MEDICATION Page 18

Methodology Qualitative study Cross-sectional observational study in 1 regional & 2 university hospitals (November-December 2015) Only results of patients are presented Randomly selected wards, all hospitalized patients – Patients Exclusion: <18 years, mentally and/or physically not able to participate not present on the ward at the time of data collection, not Dutch speaking Structured questionnaire Page 19
![Participants n124 Male Age mean range Level of education Primary school or Participants (n=124) Male (%) Age (mean [range]) Level of education (%) Primary school or](https://slidetodoc.com/presentation_image_h/263615f21a7ef43bcfbcc9634a8b2c12/image-20.jpg)
Participants (n=124) Male (%) Age (mean [range]) Level of education (%) Primary school or lower Secondary school Bachelor or higher Educated/ working in healthcare (%) Total LOS (nights) in the past 2 years (%) 0 1 -5 6 -10 11 -15 16 -30 >30 Page 20 46. 0 60. 0 [18 -97] 20. 1 55. 6 24. 2 18. 9 15. 3 29. 0 13. 7 4. 0 15. 3 22. 6

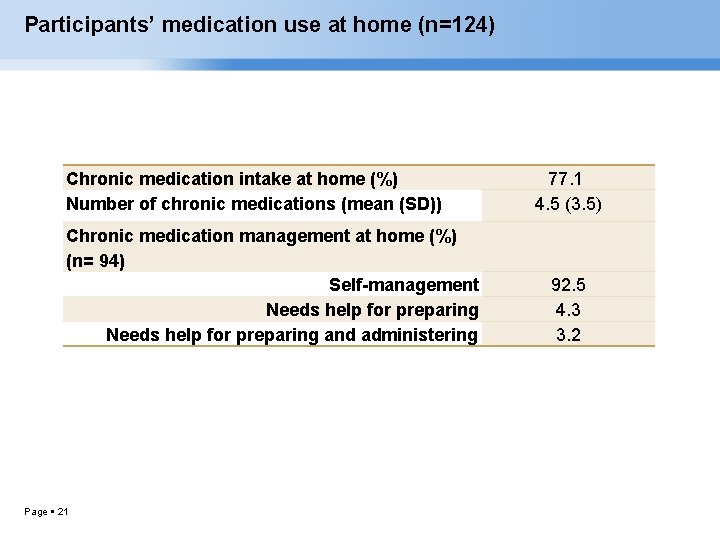
Participants’ medication use at home (n=124) Chronic medication intake at home (%) Number of chronic medications (mean (SD)) Chronic medication management at home (%) (n= 94) Self-management Needs help for preparing and administering Page 21 77. 1 4. 5 (3. 5) 92. 5 4. 3 3. 2

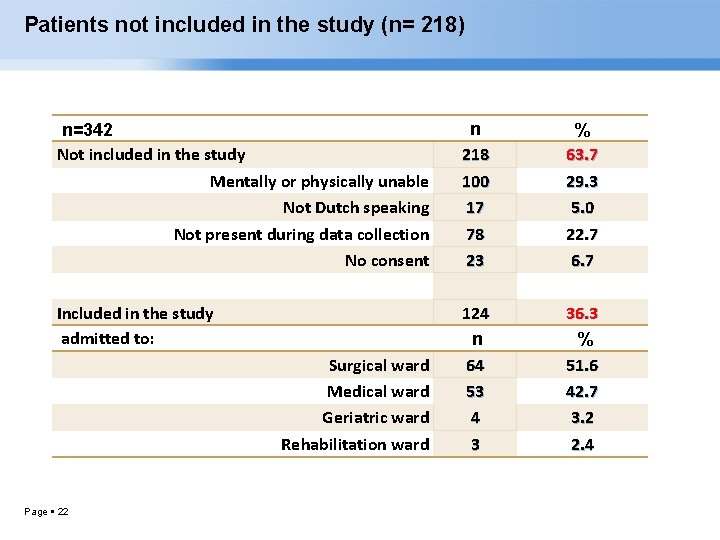
Patients not included in the study (n= 218) n=342 Not included in the study Mentally or physically unable Not Dutch speaking Not present during data collection No consent n 218 100 17 78 23 % 63. 7 29. 3 5. 0 22. 7 6. 7 Included in the study admitted to: 124 n 64 53 4 3 36. 3 % 51. 6 42. 7 3. 2 2. 4 Surgical ward Medical ward Geriatric ward Rehabilitation ward Page 22

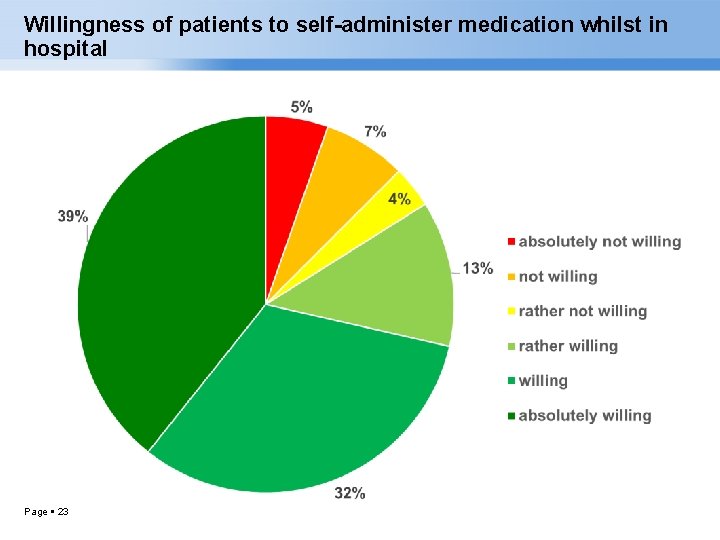
Willingness of patients to self-administer medication whilst in hospital Page 23

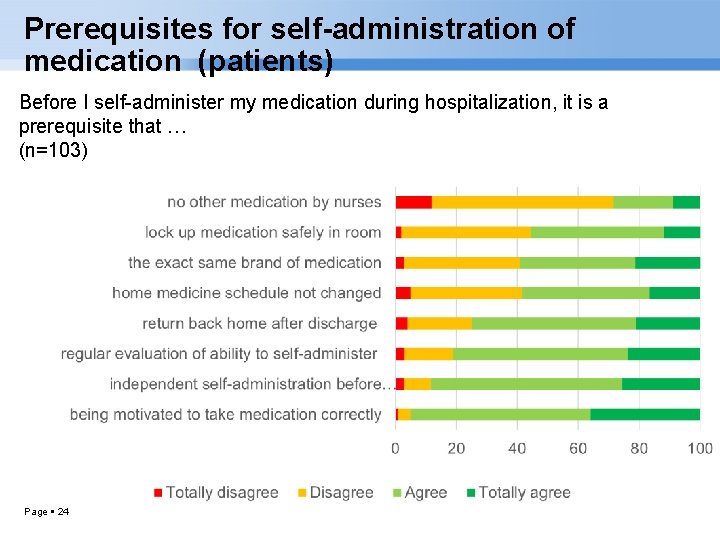
Prerequisites for self-administration of medication (patients) Before I self-administer my medication during hospitalization, it is a prerequisite that … (n=103) Page 24

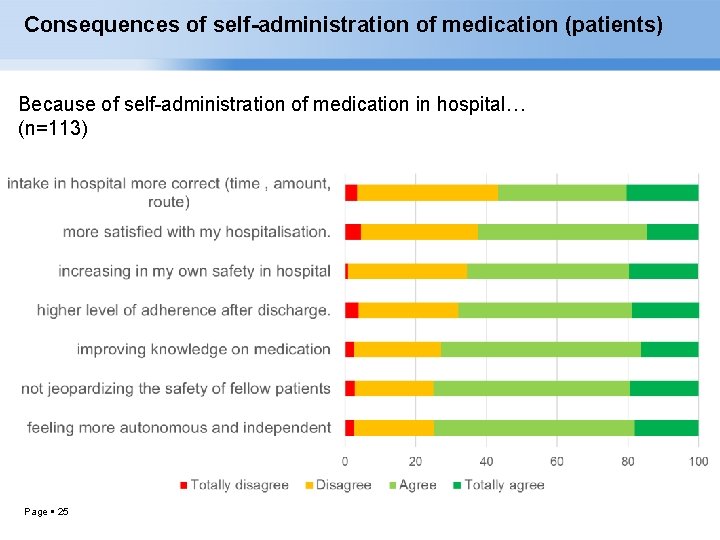
Consequences of self-administration of medication (patients) Because of self-administration of medication in hospital… (n=113) Page 25

Conclusions and Implications for practice • General perceptions on self-management were very positive • Some obstacles need to be resolved to facilitate implementation • Study provides knowledge about SWOT for self-management of medication in hospital concerning important stakeholders, required to 1. Develop toolbox to support self-management of medication 2. Develop a structured, safe and controllable procedure for selfmanagement of medication 3. Improve the quality of self-management of medication in practice 4. Maximize the potential benefits of self-management of medication for patients 5. Test the effects of self-management of medication in hospitals in a quatitative experimental design Page 26

References Barnason, S. , Zimmerman, L. , Hertzog, M. , & Schulz, P. (2010). Pilot testing of a medication self-management transition intervention for heart failure patients. West J Nurs Res, 32(7), 849 - 870. Bolster, D. , & Manias, E. (2010). Person-centred interactions between nurses and patients during medication activities in an acute hospital setting: qualitative observation and interview study. Int J Nurs Stud, 47(2), 154 -165. doi: 10. 1016/j. ijnurstu. 2009. 05. 021 Huber, M. , Knottnerus, J. A. , Green, L. , van der Horst, H. , Jadad, A. R, Kromhout, D. , Leonard, B. , Lorig, K. , Loureiro, M. I. , van der Meer, J. W. M. , Schnabel, P. , Smith, R. , van Weel, C. , Smid, H. (2011). How should we define health? BMJ, 343. Lam, P. , Elliott, R. A. , & George, J. (2011). Impact of a self-administration of medications programme on elderly inpatients' competence to manage medications: a pilot study. J Clin Pharm Ther, 36(1), 80 -86. Orem, D. E. (2001). Nursing: Concepts of practice. St. Louis, MO: Mosby. Tran, T. , Elliott, R. A. , Taylor, S. E. , & Woodward, M. C. (2011). A Self-Administration of Medications Program to Identify and Address Potential Barriers to Adherence in Elderly Patients (January). Ann Pharmacother. doi: 10. 1345/aph. 1 P 473 Wright, J. , Emerson, A. , Stephens, M. , & Lennan, E. (2006). Hospital inpatient self-administration of medicine programmes: a critical literature review. Pharm World Sci, 28(3), 140 -151. Self. MED: Self-Administration of Medication in Hospital: A Prevalence Study in Flanders, Belgium. Vanwesemael T, Van Rompaey B, Petrovic M, Boussery K, Dilles T. J Nurs Scholarsh. 2017 May; 49(3): 277 -285. doi: 10. 1111/jnu. 12290. Epub 2017 Apr 4 Self. MED: Self-management of medication during hospitalisation: health care providers’ and patients’ perspectives Vanwesemael T, Boussery K. , Fraeyman J. , Manias E. , Dilles T. Submitted for publication Page 27

www. Nu. Pha. C. eu https: //pbs. twimg. com/media/Bi. EMm. WYIc. AA 5 js 0. jpg Page 28