Selective Spinal Immobilization Matt Dunn DO Dept of

Selective Spinal Immobilization Matt Dunn, DO Dept. of Emergency Medicine Albany Medical Center

Objectives u Understand the background of spinal immobilization. u Understand the rationale for developing a selective spinal immobilization protocol. u Review the data on the selective spinal immobilization. u Cases and application of protocol

The Problem u Between 2 -4% of blunt trauma patients sustain cervical spine injury u Early trauma education suggested mechanism of injury as a sole reason for treatment of presumed spinal injury u EMS education resulted in increased practice of cervical immobilization
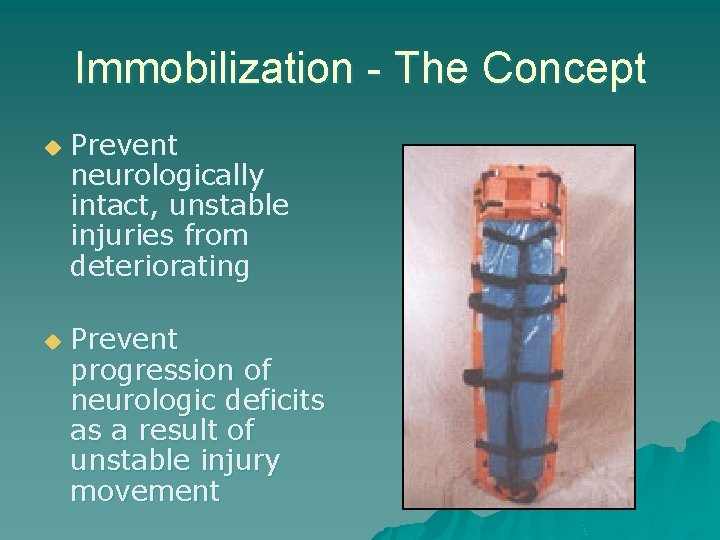
Immobilization - The Concept u u Prevent neurologically intact, unstable injuries from deteriorating Prevent progression of neurologic deficits as a result of unstable injury movement

Why not immobilize everybody? u 99. 5 -96% of EMS trauma patients do not have a spine injury u EMS provider confusion/education u Immobilization causes patient pain and anxiety…possibly injury u Patient refusal for immobilization

Why not board and collar everybody? u Time consuming for EMS/ED u Unnecessary transports u Immobilization is uncomfortable u Time immobilized = Increased pain Potential trauma Risk of aspiration Vulnerable position

Cervical Spine Evaluation EMS vs. ED Perspectives u EMS – Who is at risk for cervical injury such that injury might be exacerbated with EMS movement / transport? u ED – Who is at risk for cervical injury such that radiographic studies need to be done to elucidate question of injury?

What’s all the fuss u Why is this such a big deal? – Time – Money – Health issues

Why not film/immobilize everybody? >1, 000 U. S. Patients receive cervical radiography each year u >97% of exams are negative u Cost exceeds $175, 000 each year u Patient exposure to radiation u – ~3000 cases of thyroid cancer/yr Immobilization causes pain and anxiety u Slows time to disposition u

Cervical Spine Evaluation EMS vs. ED Perspectives u EMS – Who is at risk for cervical injury such that injury might be exacerbated with EMS movement / transport? u ED – Who is at risk for cervical injury such that radiographic studies need to be done to elucidate question of injury?

Can we recognize who may have injuries? Yes! National Emergency XRadiography Utilization Study NEXUS!

National Emergency XRadiography Utilization Study Hypothesis: Blunt trauma vicitms have virtually no risk of cervical spine injury if they meet all of the following criteria: u No Neurologic deficit u No posterior midline tenderness u No evidence of ETOH/Tox u No other distracting painful injury

NEXUS Criteria u No Neurologic deficit posterior midline tenderness evidence of ETOH/Tox other distracting painful injury

NEXUS Definition: Altered Neurologic function u GCS 14 or less – disoriented to person, place, time, events u Inability to remember 3 objects at 5 min. u Any focal deficit – Numbness, tingling, weakness u Delayed/inappropriate external stimuli response to

NEXUS Criteria u No posterior midline tenderness – Specific to midline spinal tenderness u Not considered positive if there is tenderness on the sides of the neck

NEXUS Definition: Intoxication Patients should be considered intoxicated if they have 1) History of recent intoxication or ingestion 2) Evidence of intoxication on exam

What is a significant distracting injury? Ill-defined in the literature: u “Distracting Painful Injuries associated with Cervical Spinal Injuries in Blunt Trauma”* suggests: 1)Any long bone fracture 2) Visceral injury necessitating surgical consult u * Ullrich, et al. AEM 2001; 8: 25 -29.

What is a significant distracting injury? #2 3) Large laceration, degloving or crush 4) Large burns 5) any injury producing acute functional impairment u Ultimately up to clinician. – Use to increase sensitivity

NEXUS u 21 Centers enrolled 34, 069 Blunt trauma victims who underwent cervical spine radiography.

NEXUS -Results u 818 patients with fracture identified u All except 8 were identified by clinical decision rule u Sensitivity 99% (95% CI 98 -99. 6%)
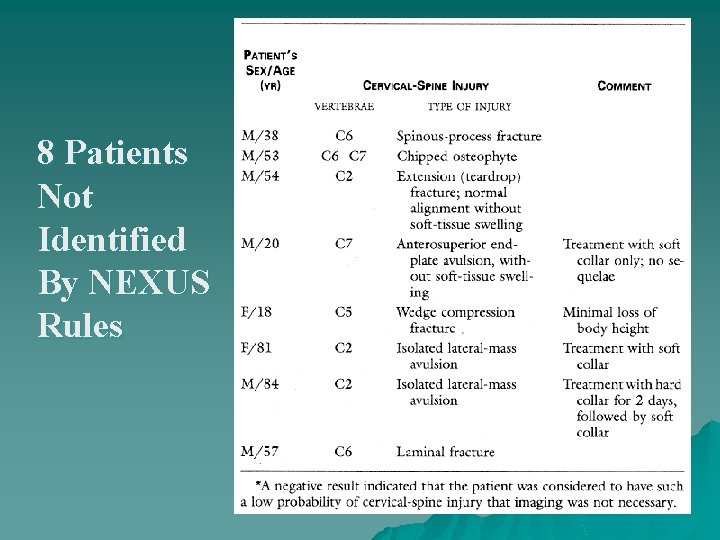
8 Patients Not Identified By NEXUS Rules

NEXUS u Performed in hospital setting u Can this be applied to the prehospital setting? u With less training, will an EMT/Paramedic miss a fracture? – Protocol is straightforward.

Purpose a Selective Spinal Immobilization Protocol u Identify and immobilize 100% of patients at risk for unstable injuries u Identify and NOT immobilize patients who have NO risk for cervical spine injury…

Burton JH, Dunn MG, Harmon NR, Hermanson TA, Bradshaw JR. A Statewide, Prehospital Emergency Medical Service Selective Patient Spine Immobilization Protocol. Journal of Trauma: Injury, Infection, and Critical Care, 2006; 61: 161 -166.
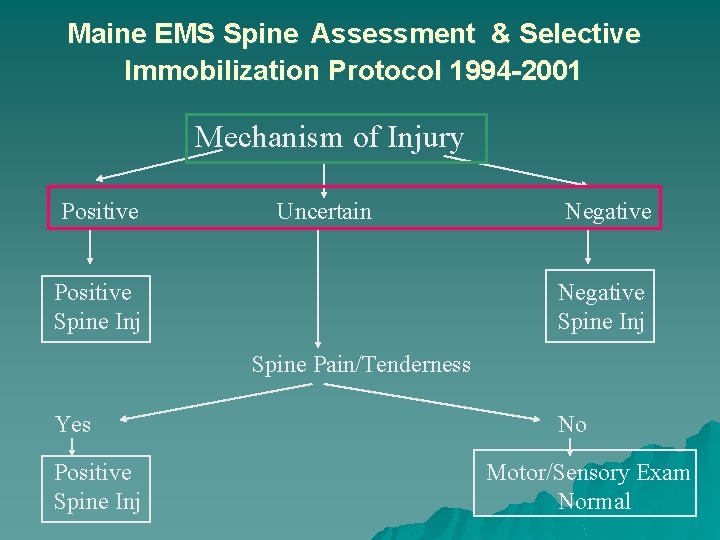
Maine EMS Spine Assessment & Selective Immobilization Protocol 1994 -2001 Mechanism of Injury Positive Uncertain Positive Spine Inj Negative Spine Inj Spine Pain/Tenderness Yes Positive Spine Inj No Motor/Sensory Exam Normal
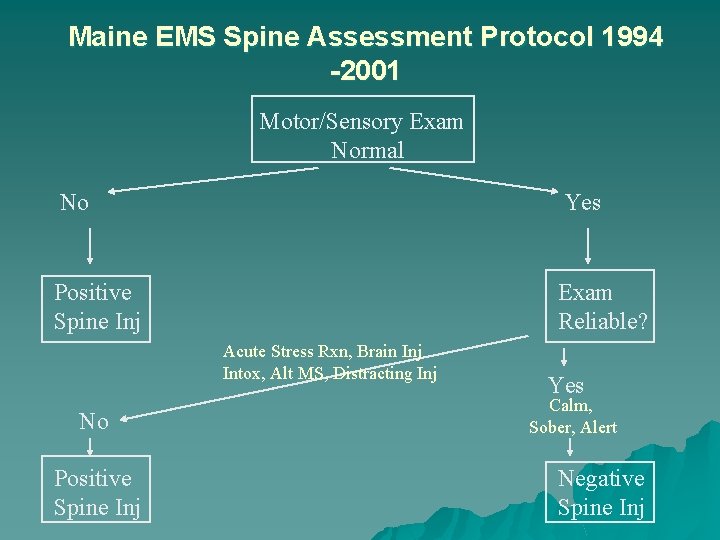
Maine EMS Spine Assessment Protocol 1994 -2001 Motor/Sensory Exam Normal No Yes Positive Spine Inj Exam Reliable? Acute Stress Rxn, Brain Inj Intox, Alt MS, Distracting Inj No Positive Spine Inj Yes Calm, Sober, Alert Negative Spine Inj


Stable Spine Injuries UNStable Spine Injuries

Not Clinically Significant Spine Injuries
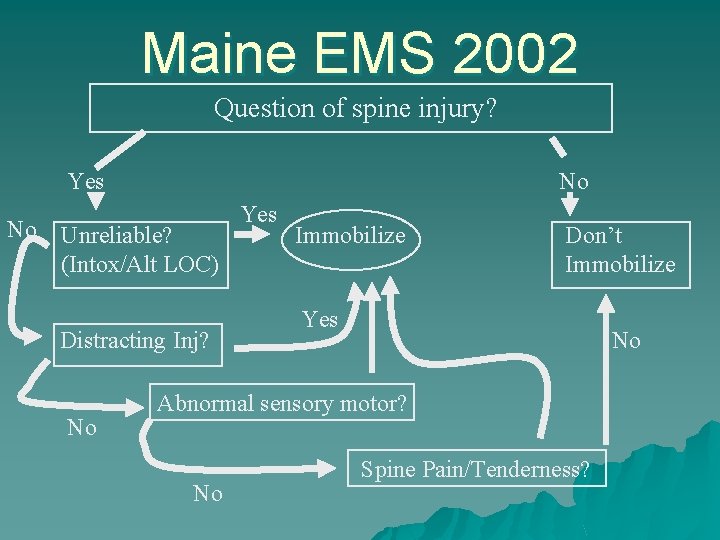
Maine EMS 2002 Question of spine injury? Yes No No Unreliable? (Intox/Alt LOC) Distracting Inj? No Yes Immobilize Don’t Immobilize Yes No Abnormal sensory motor? No Spine Pain/Tenderness?

Study Objective To evaluate the outcomes associated with a statewide, emergency medical services (EMS) protocol for selective spinal immobilization in the trauma patient.
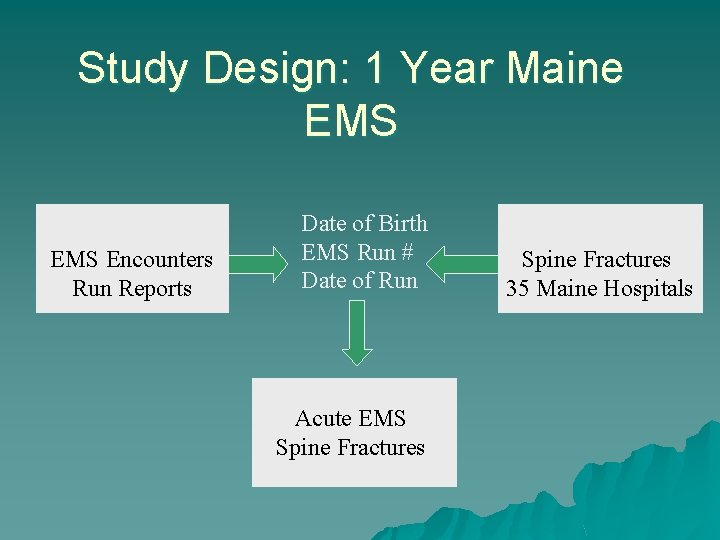
Study Design: 1 Year Maine EMS Encounters Run Reports Date of Birth EMS Run # Date of Run Acute EMS Spine Fractures 35 Maine Hospitals

EMS Run Report Demographic and Clinical Data u u u u Age, gender. . . Chief complaint categorization: Medical vs Trauma Subcategorization of chief complaint Drug/Procedure interventions Immobilization interventions: cervical collar, long board, KED Vital signs, GCS Narrative

Maine Hospital Database Demographic and Clinical Data u Age, gender. . . Injury and admission source categorization u Diagnosis Coding: ICD-9 u Spine injury interventions: CPT Definition u “Unstable”

Focused Clinical Data Review for All Spine Fracture Patients u u Demographics Injury categorization: Medical vs Trauma Immobilization interventions: cervical collar, long board, KED Diagnosis and Procedure coding u. Narrative
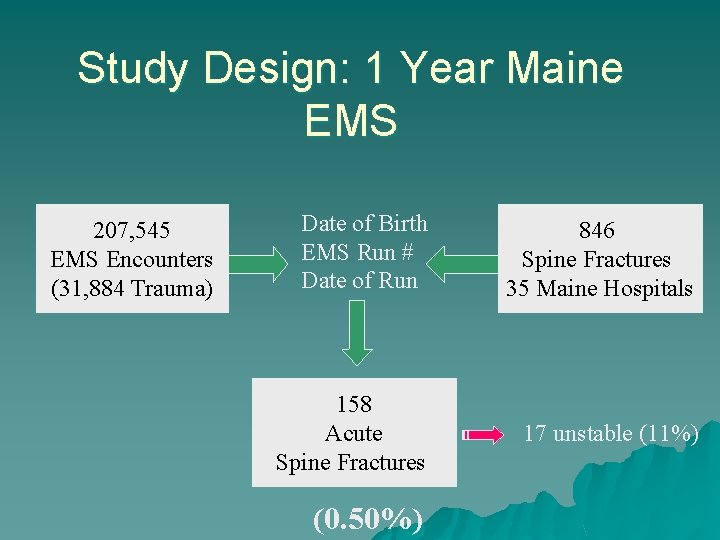
Study Design: 1 Year Maine EMS 207, 545 EMS Encounters (31, 884 Trauma) Date of Birth EMS Run # Date of Run 846 Spine Fractures 35 Maine Hospitals 158 Acute Spine Fractures 17 unstable (11%) (0. 50%)

Fractures by Spine Location
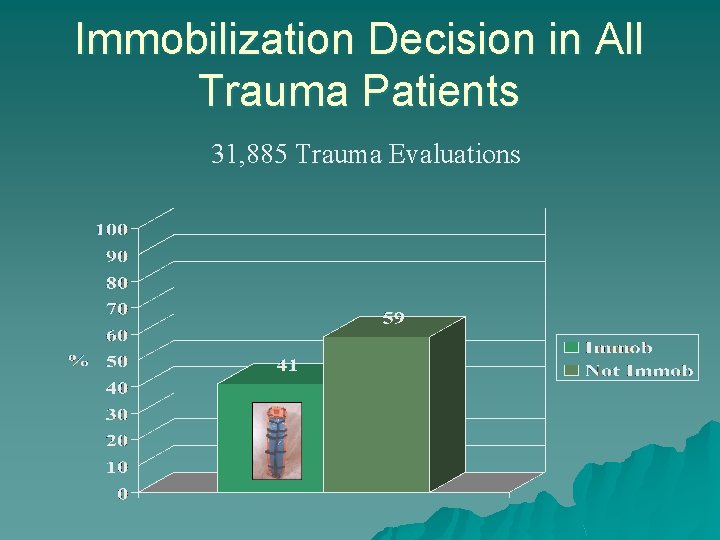
Immobilization Decision in All Trauma Patients 31, 885 Trauma Evaluations
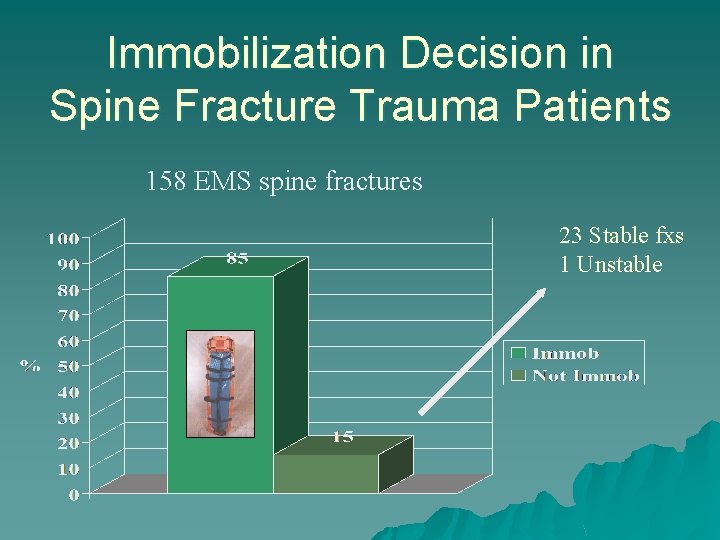
Immobilization Decision in Spine Fracture Trauma Patients 158 EMS spine fractures 23 Stable fxs 1 Unstable

Missed Fracture Patient Outcomes 1 Unstable Injury: 86 yof - fall off couch one week before 911 call T 6/7 subluxation Treated with operative fusion

Nonimmobilized Fractures by Spine Location
24 Non-Immobilized Spine Fracture Trauma Patients A G E

Conclusions u The use of this statewide, EMS spine assessment protocol resulted in a decision not to immobilize greater than half of all trauma patients assessed. u The incidence of spine fractures in EMS-assessed trauma patients in this rural state was 0. 50%

Conclusions u Approximately 15% of patients with a documented spine fracture do not appear to have been immobilized with the use of this EMS spine assessment protocol. u The use of this statewide, EMS spine assessment protocol resulted in one nonimmobilized, unstable spine fracture patient in approximately 32, 000 trauma encounters.

Limitations Large sample size is dependent on database methodology and data inherent within the database. u Database linkage methodology u Decision not to immobilize does not mean the decision rule/protocol was negative…EMS providers may be selectively choosing not to immobilize certain patients. u Education and practice disparities across large state with 6 EMS regions (one set of state protocols). u
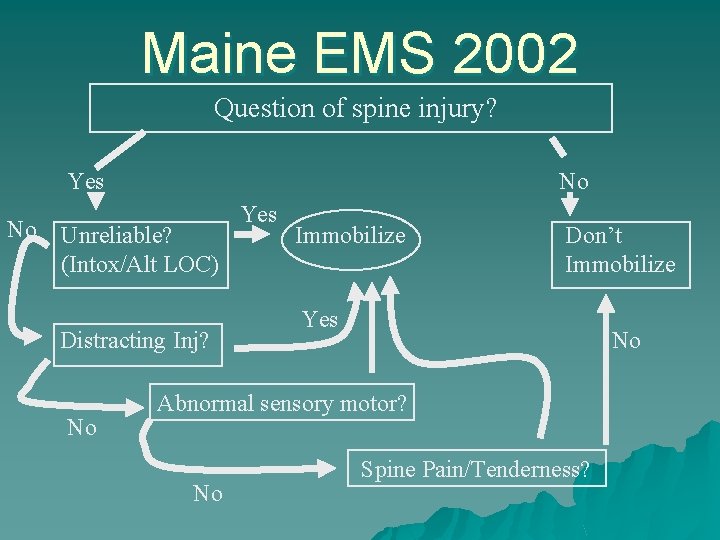
Maine EMS 2002 Question of spine injury? Yes No No Unreliable? (Intox/Alt LOC) Distracting Inj? No Yes Immobilize Don’t Immobilize Yes No Abnormal sensory motor? No Spine Pain/Tenderness?

Maine EMS 2004: QA Sensitivity for fractures: 84. 8% Negative Predictive Value: 99. 9% Sensitivity for unstable fracture: 94. 1% Negative Predictive Value for unstable: 99. 9%

EMS older patient spine conundrum – Nexus: Be Selective on Everyone – Canadian: Don’t apply to pts > 65 yoa

Maine EMS 2004: QA -Outcomes followup study: 31, 885 encounters -QA Study: 2220 QA sheets in the state 9 fractures (0. 45%)
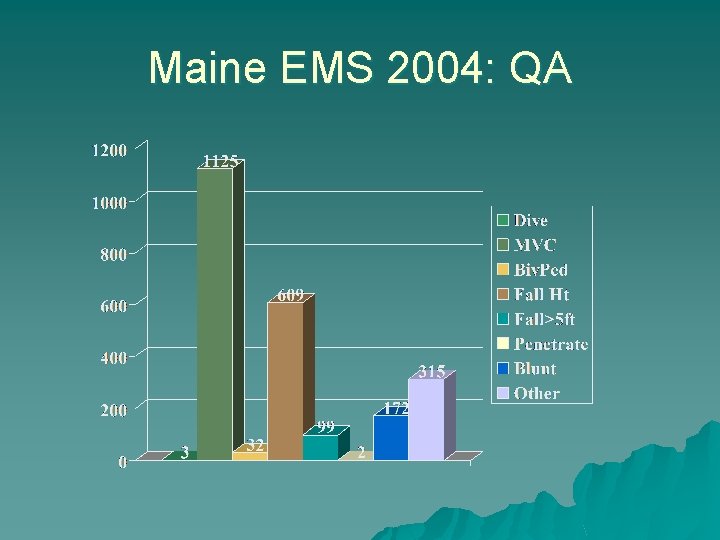
Maine EMS 2004: QA
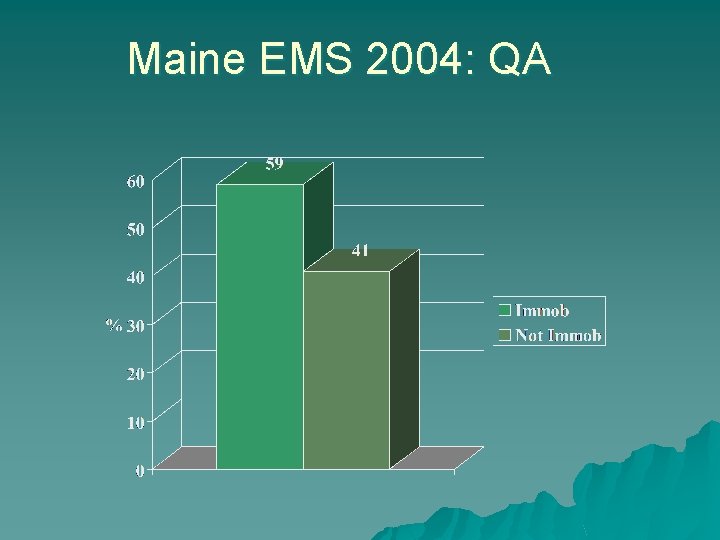
Maine EMS 2004: QA
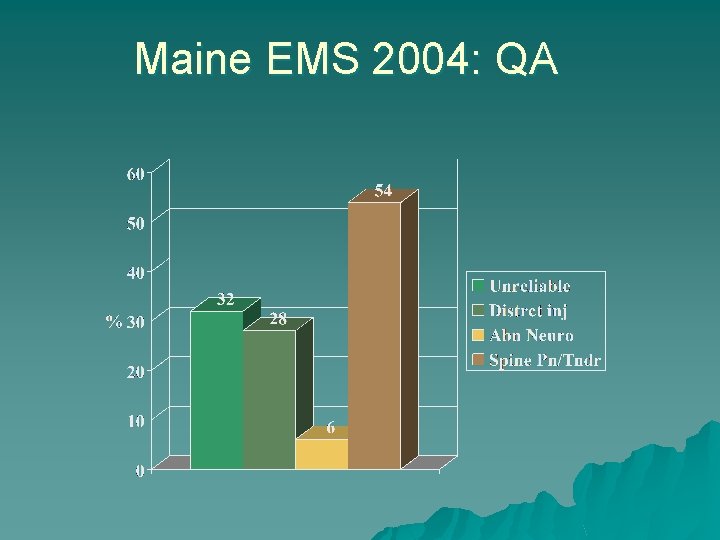
Maine EMS 2004: QA
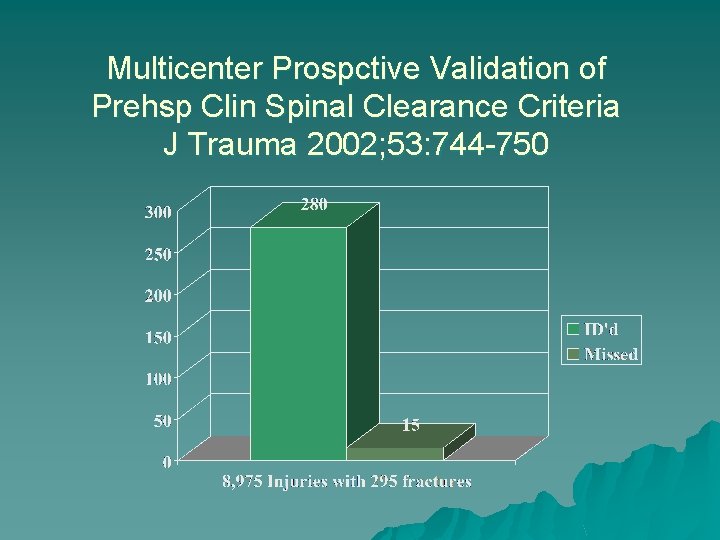
Multicenter Prospctive Validation of Prehsp Clin Spinal Clearance Criteria J Trauma 2002; 53: 744 -750

Multicenter Prospctive Validation of Prehsp Clin Spinal Clearance Criteria J Trauma 2002; 53: 744 -750

Multicenter Prospctv Validation of Prehsp Clin Spinal Clearance Criteria J Trauma 2002; 53: 744 -750 2 unstable injuries: 71 yom fall, c 1/2 odontoid fx Treated with halo and pain rx 47 yom head on MVC, T 6/7 sublx Treated with operative fusion
- Slides: 55