Sedation and Analgesia Protocols in a CommunityBased Intensive

Sedation and Analgesia Protocols in a Community-Based Intensive Care Unit DOES DAILY TRACKING IMPROVE CONCORDANCE? Richard Nadeau, BMSc 1 Robert J Anderson, MD FRCPC 1, 2 David Boyle, MD FRCPC 1, 2 1 Northern Ontario School of Medicine 2 Hôpital régional de Sudbury Regional Hospital (HRSRH) Department of Anaesthesia and Critical Care Medicine

Funding and Disclosure Funding for this project provided by the Northern Ontario School of Medicine Founding Dean Summer Medical Student Research Award (2009) No conflicts of interest to disclose (all authors)

From Theory to Practice
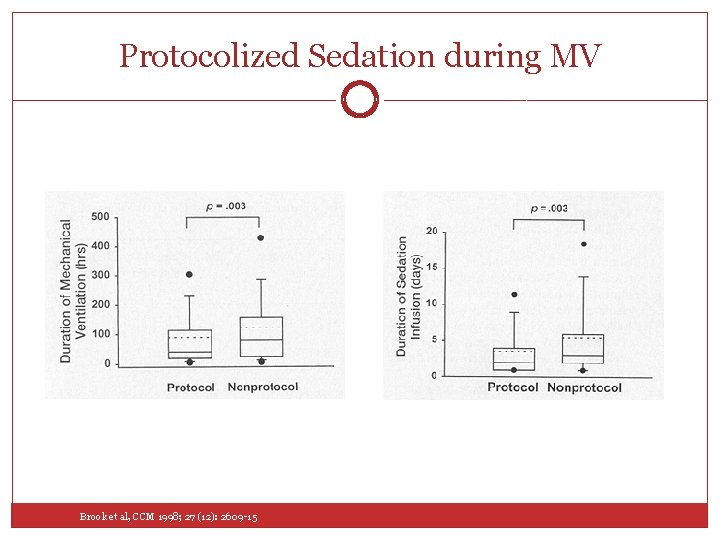
Protocolized Sedation during MV Brook et al, CCM 1998; 27 (12): 2609 -15
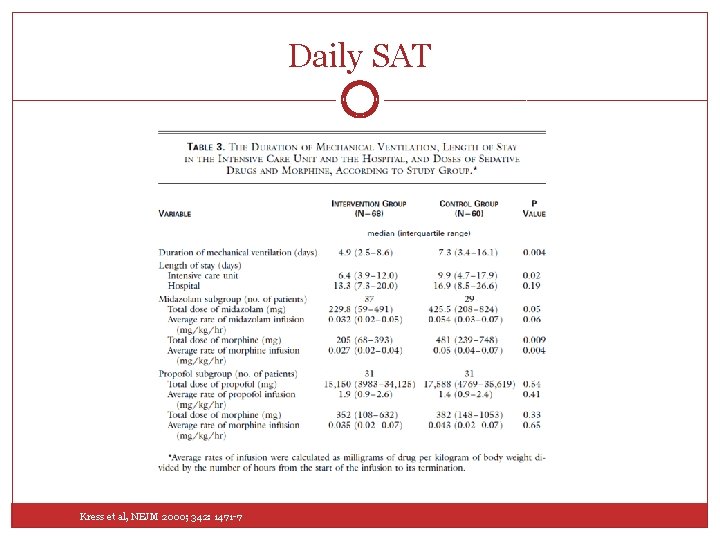
Daily SAT Kress et al, NEJM 2000; 342: 1471 -7
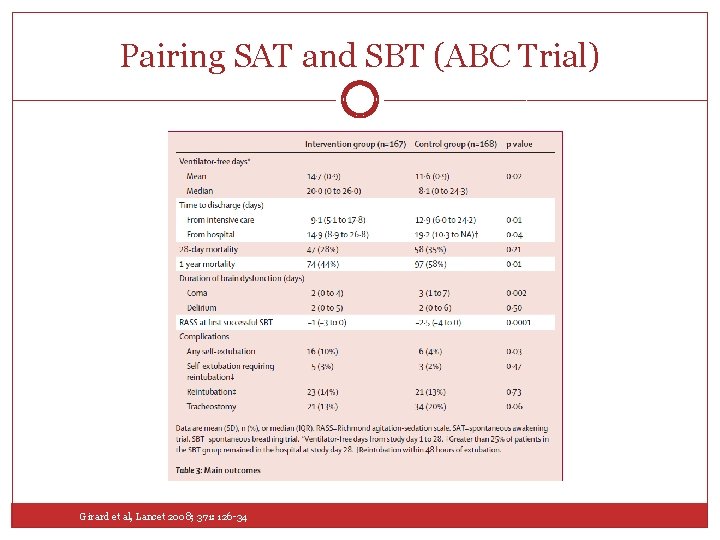
Pairing SAT and SBT (ABC Trial) Girard et al, Lancet 2008; 371: 126 -34

Titrating to the Sedation Analgesia Scale “A sedation goal or endpoint should be established and regularly redefined for each patient. Regular assessment and response to therapy should be systematically documented. ” (Grade of recommendation = C) “The use of a validated sedation assessment scale (SAS, MAAS, or VICS) is recommended. ” (Grade of recommendation = B) Jacobi et al. Clinical practice guidelines for the sustained use of sedatives and analgesics in the critically ill adult. CCM 2002; 30 (1): 119 -41
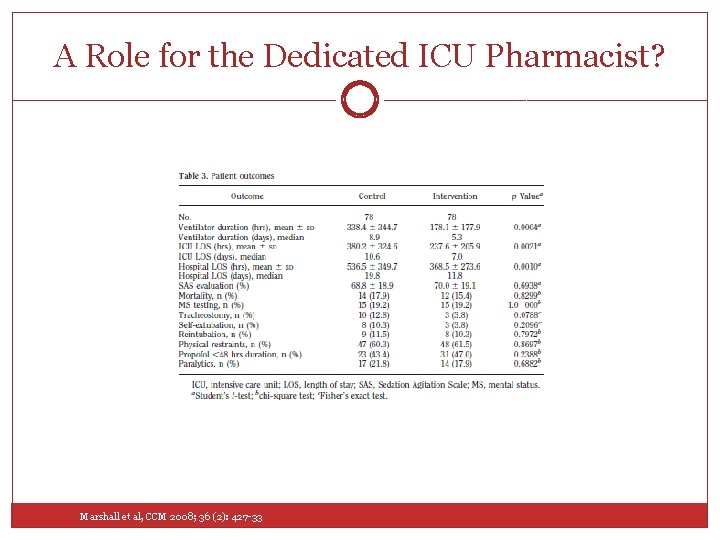
A Role for the Dedicated ICU Pharmacist? Marshall et al, CCM 2008; 36 (2): 427 -33

Study Design Hypothesis: Having an auditor present to give daily feedback to the ICU Care Team will improve concordance to the protocol. Setting: HRSRH Medical/Surgical ICU Control group: Retrospective chart review Intervention group: Daily audit and feedback of ICU Care Team Primary outcome measure: Concordance in proper utilization of the Protocol Secondary outcome measures: Duration of mechanical ventilation (days) Amount of sedative administered Propofol, BZD, opioids, ketamine and haloperidol
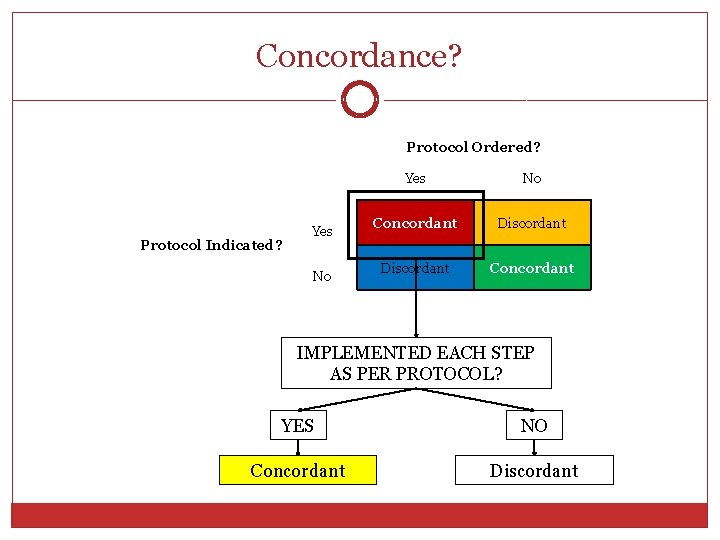
Concordance? Protocol Ordered? Protocol Indicated? Yes No Concordant Discordant Concordant IMPLEMENTED EACH STEP AS PER PROTOCOL? YES NO Concordant Discordant
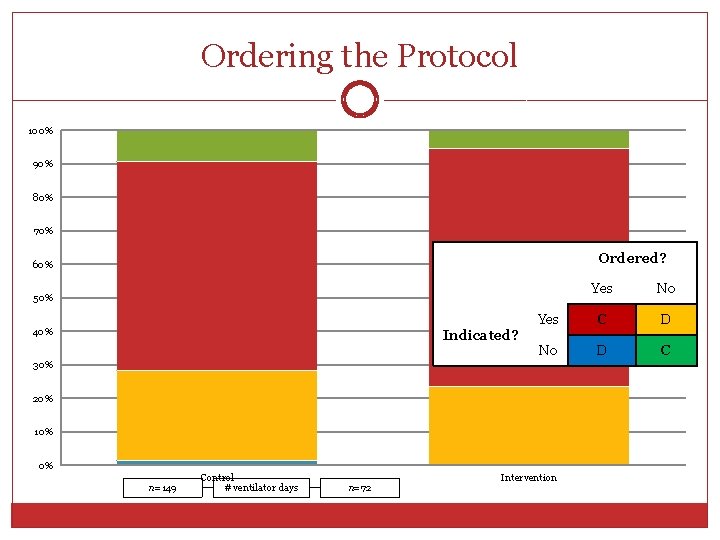
Ordering the Protocol 100% 90% 80% 70% 60% Protocol not ordered when it shouldn't have Ordered? been ordered 50% Protocol ordered when it should have been Yes No ordered Protocol not ordered when it should have been C Yes D ordered 40% Indicated? Protocol ordered when it shouldn't have been No D C ordered 30% 20% 10% 0% n=149 Control # ventilator days n=72 Intervention
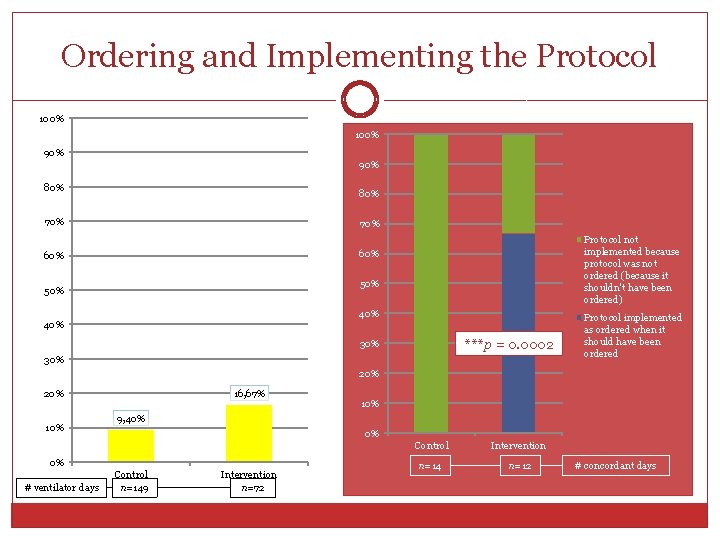
Ordering and Implementing the Protocol 100% 90% 80% 70% Protocol not implemented because protocol was not ordered (because it shouldn't have been ordered) 60% 50% 40% ***p = 0. 0002 30% Protocol implemented as ordered when it should have been ordered 20% 16, 67% 20% 10% 9, 40% 0% 0% # ventilator days 10% Control n=149 Intervention n=72 Control Intervention n=14 n=12 # concordant days
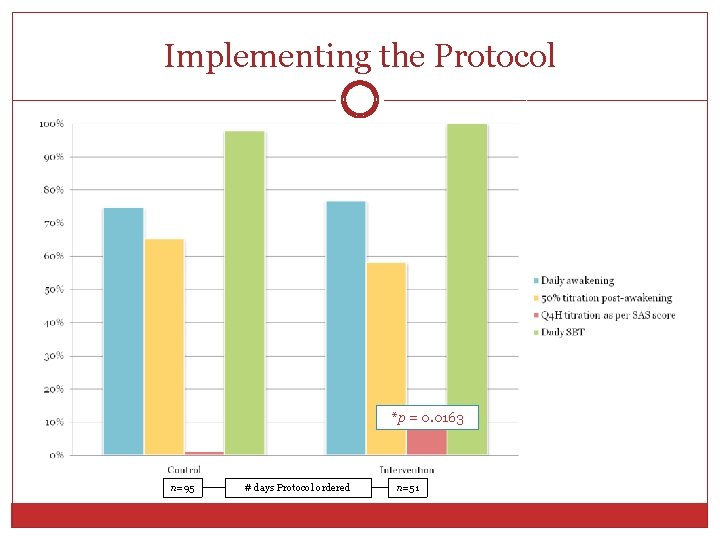
Implementing the Protocol *p = 0. 0163 n=95 # days Protocol ordered n=51
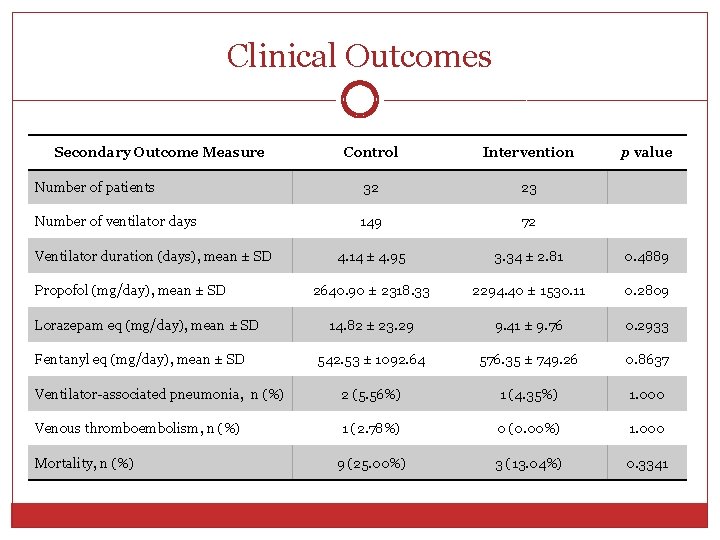
Clinical Outcomes Secondary Outcome Measure Control Intervention Number of patients 32 23 Number of ventilator days 149 72 4. 14 ± 4. 95 3. 34 ± 2. 81 0. 4889 2640. 90 ± 2318. 33 2294. 40 ± 1530. 11 0. 2809 14. 82 ± 23. 29 9. 41 ± 9. 76 0. 2933 542. 53 ± 1092. 64 576. 35 ± 749. 26 0. 8637 Ventilator-associated pneumonia, n (%) 2 (5. 56%) 1 (4. 35%) 1. 000 Venous thromboembolism, n (%) 1 (2. 78%) 0 (0. 00%) 1. 000 9 (25. 00%) 3 (13. 04%) 0. 3341 Ventilator duration (days), mean ± SD Propofol (mg/day), mean ± SD Lorazepam eq (mg/day), mean ± SD Fentanyl eq (mg/day), mean ± SD Mortality, n (%) p value

Conclusions and Discussion Baseline concordance not very good Modest benefit of having auditor present Improved ICU Care Team concordance when Protocol is ordered Better sedative titration as per SAS Is there a place for dedicated ICU pharmacist in a community-based ICU? Limitations

Acknowledgments Dr. Rob Anderson All members of the ICU Care Team Northern Ontario School of Medicine QUESTIONS?
- Slides: 16