Sedation Analgesia and Tapering Guidelines for Endotracheally intubated
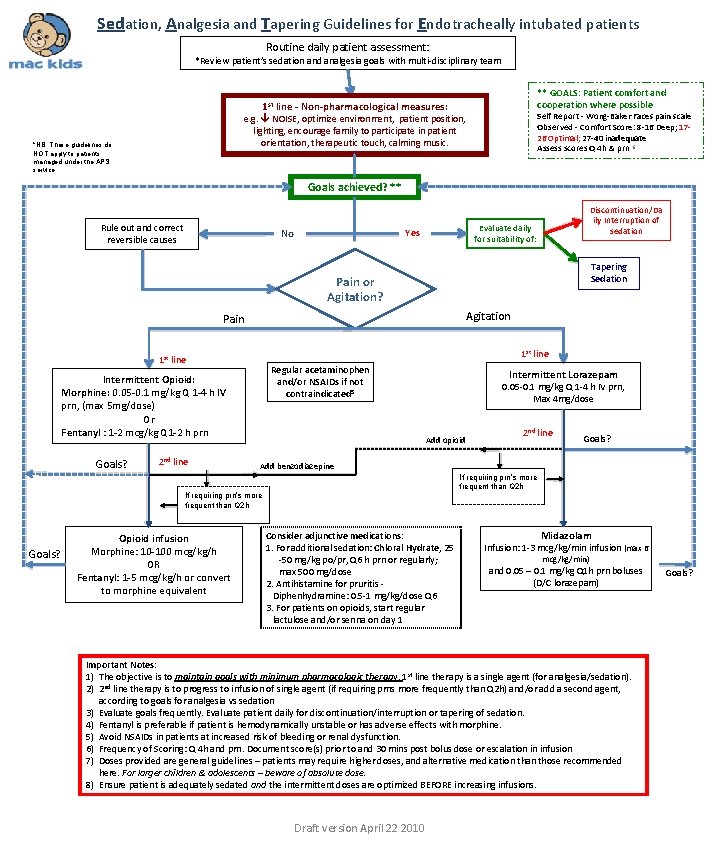
Sedation, Analgesia and Tapering Guidelines for Endotracheally intubated patients Routine daily patient assessment: *Review patient’s sedation and analgesia goals with multi-disciplinary team ** GOALS: Patient comfort and cooperation where possible 1 st line - Non-pharmacological measures: Self Report - Wong-Baker Faces pain scale Observed - Comfort Score: 8 -16 Deep; 1726 Optimal; 27 -40 inadequate Assess scores Q 4 h & prn 6 e. g. NOISE, optimize environment, patient position, lighting, encourage family to participate in patient orientation, therapeutic touch, calming music. *NB. These guidelines do NOT apply to patients managed under the APS service Goals achieved? ** Rule out and correct reversible causes No Discontinuation/Da ily Interruption of sedation Evaluate daily for suitability of : Yes Tapering Sedation Pain or Agitation? Agitation Pain 1 st line Regular acetaminophen and/or NSAIDs if not contraindicated 5 Intermittent Opioid: Morphine: 0. 05 -0. 1 mg/kg Q 1 -4 h IV prn, (max 5 mg/dose) Or Fentanyl : 1 -2 mcg/kg Q 1 -2 h prn Goals? 2 nd line Intermittent Lorazepam 0. 05 -0. 1 mg/kg Q 1 -4 h IV prn, Max 4 mg/dose Add opioid Goals? Add benzodiazepine If requiring prn’s more frequent than Q 2 h Opioid infusion Morphine: 10 -100 mcg/kg/h OR Fentanyl: 1 -5 mcg/kg/h or convert to morphine equivalent 2 nd line Consider adjunctive medications: 1. For additional sedation: Chloral Hydrate, 25 -50 mg/kg po/pr, Q 6 h prn or regularly; max 500 mg/dose 2. Antihistamine for pruritis Diphenhydramine: 0. 5 -1 mg/kg/dose Q 6 3. For patients on opioids, start regular lactulose and/or senna on day 1 Midazolam Infusion: 1 -3 mcg/kg/min infusion (max 6 mcg/kg/min) and 0. 05 – 0. 1 mg/kg Q 1 h prn boluses (D/C lorazepam) Important Notes: 1) The objective is to maintain goals with minimum pharmacologic therapy. 1 st line therapy is a single agent (for analgesia/sedation). 2) 2 nd line therapy is to progress to infusion of single agent (if requiring prns more frequently than Q 2 h) and/or add a second agent, according to goals for analgesia vs sedation 3) Evaluate goals frequently. Evaluate patient daily for discontinuation/interruption or tapering of sedation. 4) Fentanyl is preferable if patient is hemodynamically unstable or has adverse effects with morphine. 5) Avoid NSAIDs in patients at increased risk of bleeding or renal dysfunction. 6) Frequency of Scoring: Q 4 h and prn. Document score(s) prior to and 30 mins post bolus dose or escalation in infusion 7) Doses provided are general guidelines – patients may require higher doses, and alternative medication than those recommended here. For larger children & adolescents – beware of absolute dose. 8) Ensure patient is adequately sedated and the intermittent doses are optimized BEFORE increasing infusions. Draft version April 22 2010 Goals?
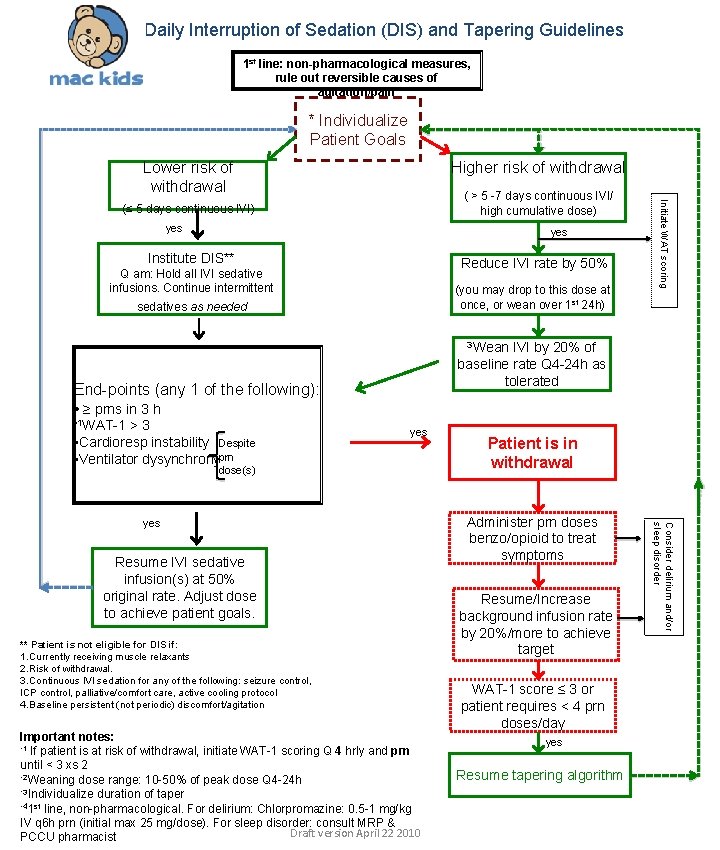
Daily Interruption of Sedation (DIS) and Tapering Guidelines 1 st line: non-pharmacological measures, rule out reversible causes of agitation/pain * Individualize Patient Goals Lower risk of withdrawal Higher risk of withdrawal yes Institute DIS** Reduce IVI rate by 50% Q am: Hold all IVI sedative infusions. Continue intermittent (you may drop to this dose at once, or wean over 1 st 24 h) sedatives as needed Initiate WAT scoring ( > 5 -7 days continuous IVI/ high cumulative dose) (≤ 5 days continuous IVI) 3 Wean IVI by 20% of baseline rate Q 4 -24 h as tolerated End-points (any 1 of the following): • ≥ prns in 3 h • 1 WAT-1 >3 • Cardioresp instability Despite • Ventilator dysynchronyprn yes dose(s) Resume IVI sedative infusion(s) at 50% original rate. Adjust dose to achieve patient goals. ** Patient is not eligible for DIS if: 1. Currently receiving muscle relaxants 2. Risk of withdrawal. 3. Continuous IVI sedation for any of the following: seizure control, ICP control, palliative/comfort care, active cooling protocol 4. Baseline persistent (not periodic) discomfort/agitation Important notes: • 1 If patient is at risk of withdrawal, initiate WAT-1 scoring Q 4 hrly and prn until < 3 xs 2 • 2 Weaning dose range: 10 -50% of peak dose Q 4 -24 h • 3 Individualize duration of taper • 41 st line, non-pharmacological. For delirium: Chlorpromazine: 0. 5 -1 mg/kg IV q 6 h prn (initial max 25 mg/dose). For sleep disorder: consult MRP & Draft version April 22 2010 PCCU pharmacist Administer prn doses benzo/opioid to treat symptoms Resume/Increase background infusion rate by 20%/more to achieve target WAT-1 score ≤ 3 or patient requires < 4 prn doses/day yes Resume tapering algorithm Consider delirium and/or sleep disorder yes Patient is in withdrawal

Comfort Scale: (Score after a 2 min period of observation) fre PAIN Scales: use to supplement the COMFORT scale, in patients who are cognitively and physically able to respond (e. g. age ≥ 3 years) Draft version April 22 2010

DAILY INTERRUPTION OF SEDATION (DIS) What is DIS = focused downward titration of sedatives over time Objectives: daily “wake-up”; minimize pharmacological intervention and prevent adverse events; optimise patient outcomes Rationale: DIS in adults has been shown to facilitate spontaneous breathing, and has been associated with decreased mortality, hospital stay, withdrawal and delirium, improved ventilator free days and psychological outcomes Patient is not eligible for DIS if: 1. Currently receiving muscle relaxants 2. Risk of opioid/sedation withdrawal. 3. Continuous IVI sedation for: • seizure control • ICP control • palliative/comfort care • active cooling protocol 4. Baseline persistent (not periodic) discomfort/agitation Draft version April 22 2010
- Slides: 4