Section of Pathology and Tumour Biology Development of

Section of Pathology and Tumour Biology Development of laboratory models to study Breast Cancer Deborah Holliday Breast Research Group Section of Pathology & Tumour Biology

Outline § Introduction to the cells found in breast tissue § Changes in breast cells during breast cancer § Designing a model of breast cancer § methods § Use of the model: A tool for looking at cancer progression
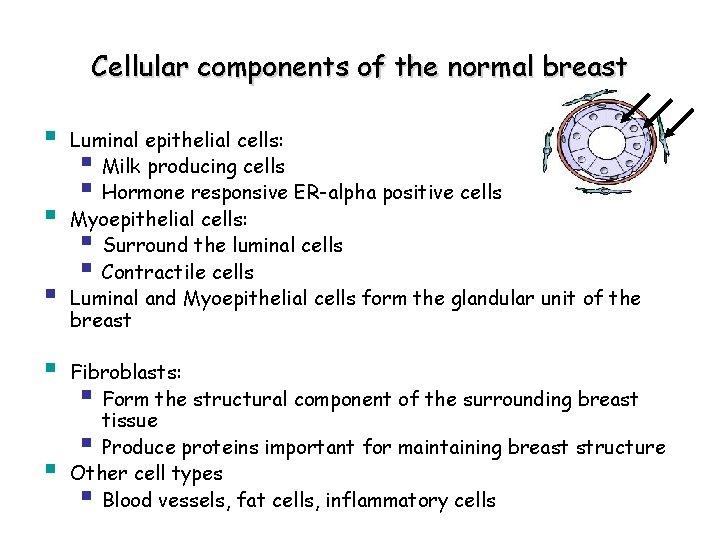
Cellular components of the normal breast § § § Luminal epithelial cells: § Milk producing cells § Hormone responsive ER-alpha positive cells Myoepithelial cells: § Surround the luminal cells § Contractile cells Luminal and Myoepithelial cells form the glandular unit of the breast Fibroblasts: § Form the structural component of the surrounding breast tissue § Produce proteins important for maintaining breast structure Other cell types § Blood vessels, fat cells, inflammatory cells
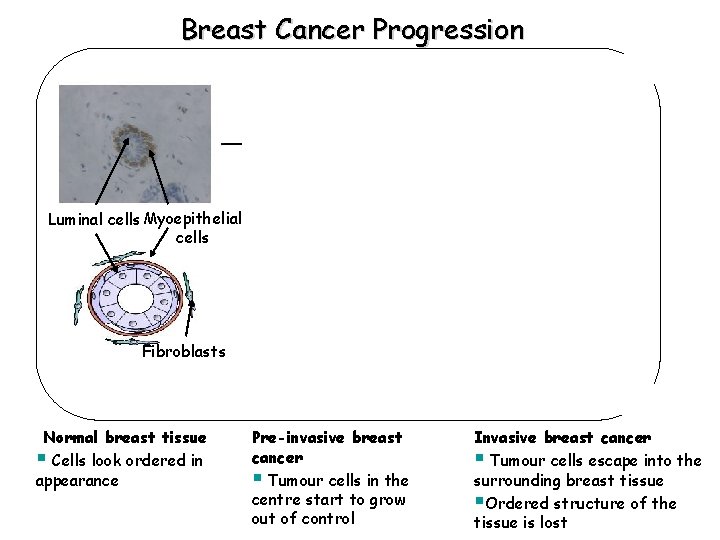
Breast Cancer Progression Luminal cells Myoepithelial cells Tumour cells Fibroblasts Normal breast tissue § Cells look ordered in appearance Pre-invasive breast cancer § Tumour cells in the centre start to grow out of control Invasive breast cancer § Tumour cells escape into the surrounding breast tissue §Ordered structure of the tissue is lost

Pre-invasive breast cancer: Ductal carcinoma in situ (DCIS) § DCIS is characterised by confinement of tumour cells § § to the breast glandular unit DCIS accounts for 40% of screen detected breast carcinoma 25 -30% of untreated DCIS will progress to invasive carcinoma

Problems with treatment of DCIS n n Mastectomy n Patient is cured but ? Overtreatment ? Conservative surgery n A proportion of tumours will recur n Some of those will progress to invasive carcinoma Important to define which DCIS cases are likely to progress A better understanding of the biology of tumour invasion may reveal new targets for therapies

Designing a human model of breast cancer § The model would need to include 3 major cell types involved in breast cancer: § Tumour cells. § Myoepithelial cells (protector cells). § Fibroblasts (tumour helper cells). § Cells would need to be grown in culture conditions which resemble those in the body: § Able to grow in 3 dimensions rather than on a plastic Petri dish. C Such a model would be a valuable tool: C To help us understand how breast cancer progresses. C To allow us to test new drugs for therapy. C To potentially identify new targets for future drug development.

Methods §We isolated cells from normal breast tissue or from breast cancer tissue and grew then in a 3 dimensional matrix of collagen. § By labelling our cells with different colours we were able to identify the different cell types in our model. § We used the model to investigate whether fibroblasts are able to make pre-invasive lesions become invasive. Myoepithelial cells Luminal cells Fibroblasts Collagen I Culture media
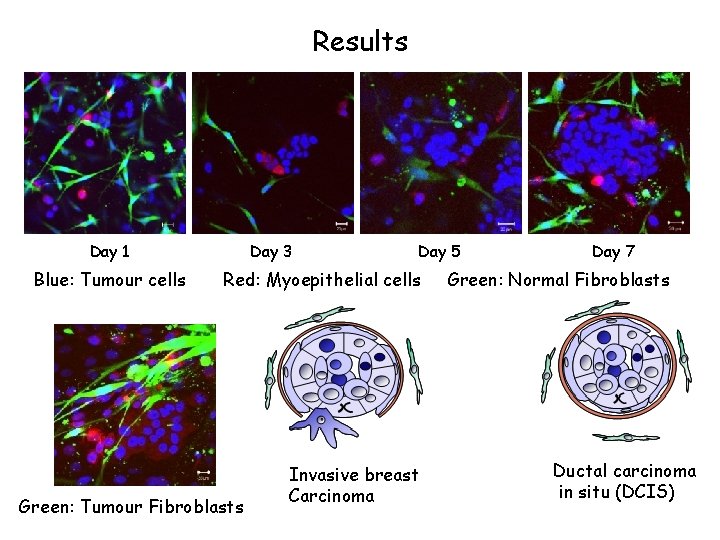
Results B Day 1 Day 3 Blue: Tumour cells Day 5 Red: Myoepithelial cells Day 7 Green: Normal Fibroblasts F Green: Tumour Fibroblasts Invasive breast Carcinoma Ductal carcinoma in situ (DCIS)
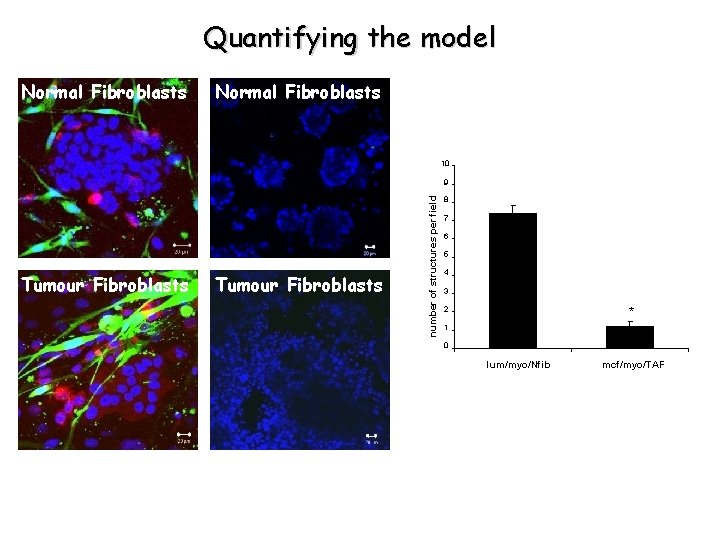
Quantifying the model Normal Fibroblasts 10 Tumour Fibroblasts number of structures per field 9 8 7 6 5 4 3 2 * 1 0 lum/myo/Nfib mcf/myo/TAF

Summary • We have a model which we can use to study the biology of breast cancer • This will help us understand how breast cancer progresses How we are using the model • Different tumour cells to represent different types of breast cancer • Different fibroblasts to understand why in some patients cancer progresses faster than in others • Include drugs into the model with tumour fibroblasts to see if we can prevent ‘invasion’ – Established drugs – New Drugs = pre-clinical drug screen

Section of Pathology and Tumour Biology Using 3 D models to study radioresistance in Breast Cancer Laura Smith Breast Research Group Section of Pathology & Tumour Biology

Outline § Radiotherapy § Issues with radiotherapy § What would help overcome these issues? § The use of 3 D models

Radiotherapy § Reduces risk of the cancer coming back § Is given to many breast cancer patients § All patients having breast conserving surgery § Patients having a mastectomy but at high risk of the cancer coming back

Issues with Radiotherapy § Unpleasant side effects § Short term § Long term § Stressful regime § Daily hospital visits 5 days/ week for 3 weeks § Limited availability of treatment machines § Long waiting lists in some areas § Not all patients will benefit § Some patients cancer will come back anyway

Overcoming these issues § Better patient selection § Estrogen Receptor for Tamoxifen therapy § HER 2 for Herceptin therapy § Nothing analogous to guide radiotherapy § Why do some cancers respond well to radiotherapy whilst others do not? § What factors are involved? § Radio-sensitizing drugs?

Our Study § It is not only cancer cells that are exposed to radiotherapy but also the fibroblasts § Do fibroblasts influence breast cancer cell response to radiotherapy? § Do fibroblasts differentially influence the response of different breast cancer types?
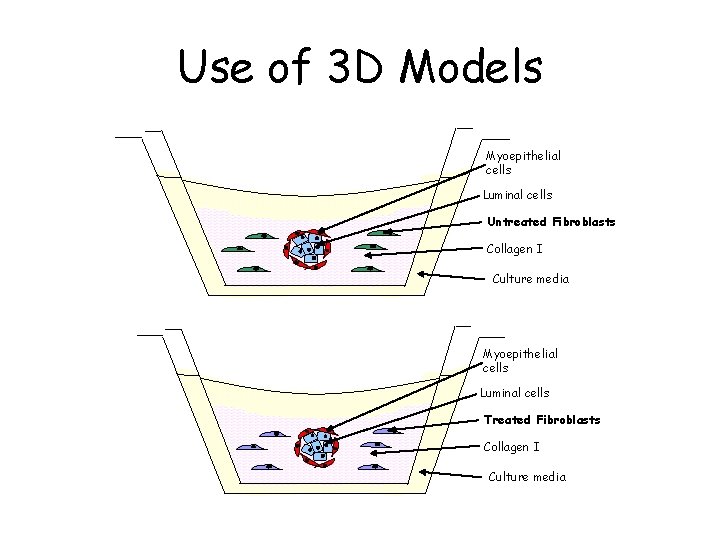
Use of 3 D Models Myoepithelial cells Luminal cells Untreated Fibroblasts Collagen I Culture media Myoepithelial cells Luminal cells Treated Fibroblasts Collagen I Culture media
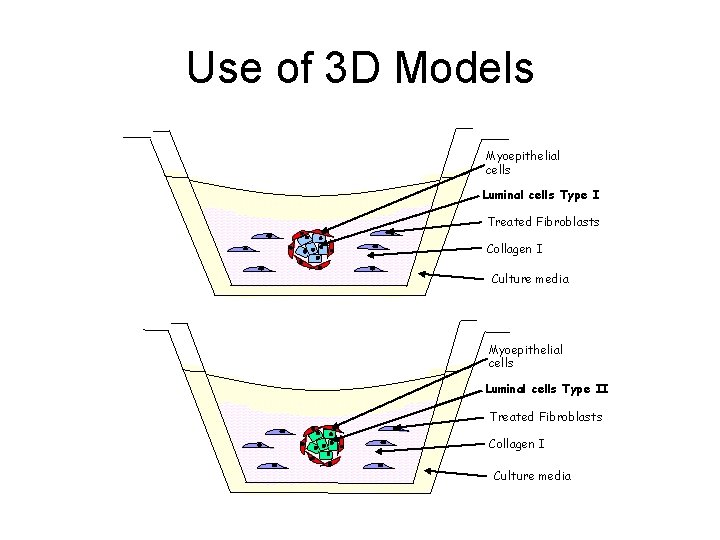
Use of 3 D Models Myoepithelial cells Luminal cells Type I Treated Fibroblasts Collagen I Culture media Myoepithelial cells Luminal cells Type II Treated Fibroblasts Collagen I Culture media

Summary § Reduce side effects and improve quality of life for patients that will not benefit § Allow drs to select another type of treatment that will work for these patients § Reduce waiting times for those patients that will benefit thereby increasing survival
- Slides: 20