SCREENING FOR BREAST CANCER THE OBSTETRICS GYNECOLOGICAL SOCIETY

SCREENING FOR BREAST CANCER THE OBSTETRICS & GYNECOLOGICAL SOCIETY OF BHOPAL & AMPOGS RESEARCH PUBLIC WELFARE SOCIETY

SCREENING TOOLS • Clinical Breast examination • Breast self examination • Mammography • Ultrasonography/elastography • FNAC • Cytology of nipple discharge
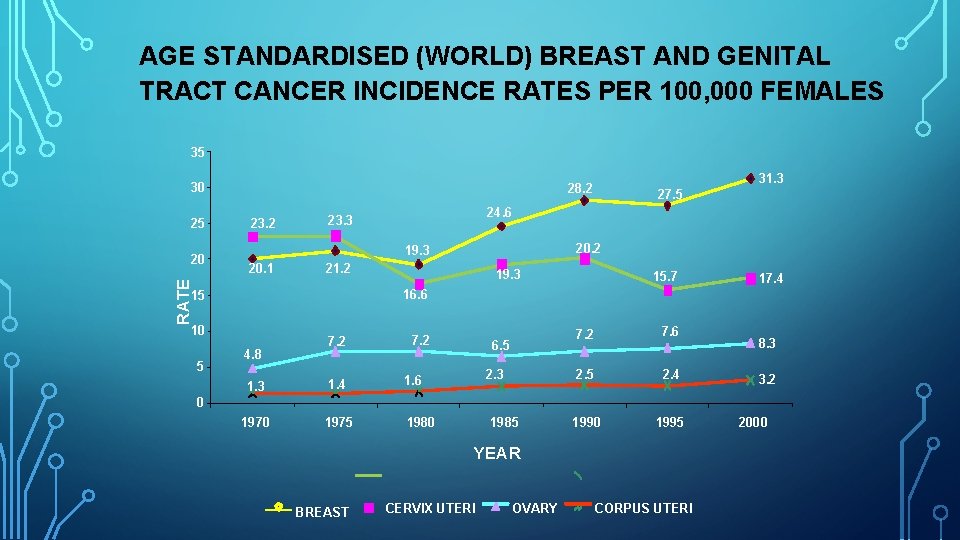
AGE STANDARDISED (WORLD) BREAST AND GENITAL TRACT CANCER INCIDENCE RATES PER 100, 000 FEMALES 35 30 25 23. 2 21. 2 19. 3 15. 7 17. 4 16. 6 15 10 5 20. 2 19. 3 20. 1 27. 5 24. 6 23. 3 RATE 20 31. 3 28. 2 4. 8 7. 2 1. 3 1. 4 1. 6 1970 1975 1980 6. 5 2. 3 7. 2 7. 6 2. 5 2. 4 1990 1995 8. 3 3. 2 0 1985 YEAR BREAST CERVIX UTERI OVARY CORPUS UTERI 2000
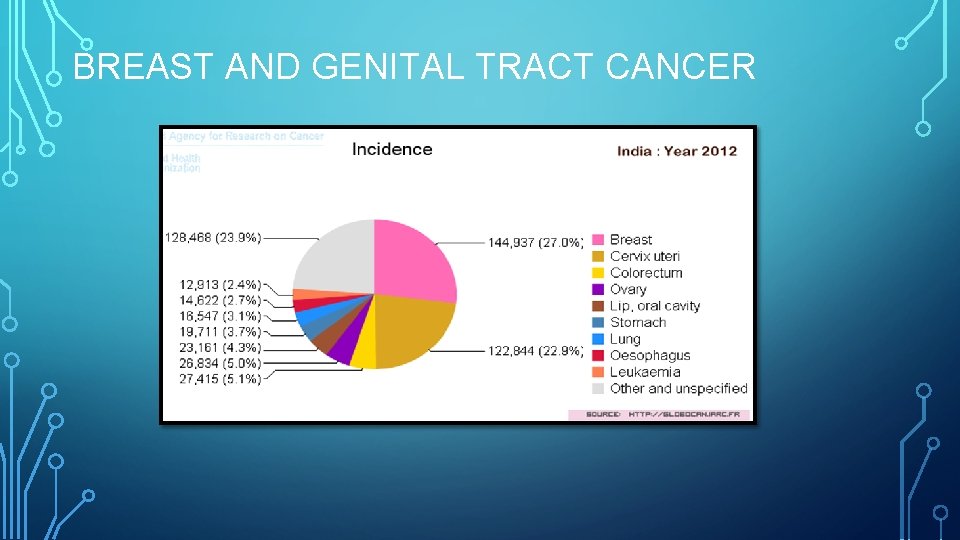
BREAST AND GENITAL TRACT CANCER

BREAST CANCER INCIDENCE • Most common cancer in women worldwide. • Most common cause of death from cancer among women. • More than three fourths of these women in developing countries are diagnosed in advanced stage of the disease. If these lesions are detected early, most breast cancers can be effectively treated with good outcome. • In India 144, 937 women were newly detected with breast cancer in 2012, of which 70, 218 women died. Roughly, for every 2 women newly diagnosed with breast cancer in India, one dies of this disease.

WHO TO BE SCREENED • • Women between the ages of 40 -60 years of age • Women with high Risk factors can be offered screening from age 30 years such as All women identified with a breast mass that has previously not been clinically evaluated need to be screened for breast cancer • • Age over 40 No children or children after 30 years of age Mother or sister with breast cancer History of breast biopsies or breast cancer Initiation of menses before 12 years of age Overweight Screening to be every 2 years

CLINICAL BREAST EXAMINATION - TIPS • • Be sensitive to the woman by giving her opportunities to express any concerns before and during the examination. Respect the woman’s sense of privacy. If the woman is anxious, assure her that you will do your best to make the examination comfortable. Throughout the examination, approach the woman slowly and avoid any sudden or unexpected movements. Do not rush through the examination. Perform each step gently and ask her if she is having any discomfort during any part of the examination. Be aware of her facial expressions and body movements as indications that she is uncomfortable. Always take into consideration any cultural factors when deciding what clothing the woman should remove. Have a clean sheet or drape to cover the woman’s breast if needed. These examinations should be performed in a clean, well-lit, private examination or procedure room that has a source of clean water. A female assistant should be available to accompany the woman when a male clinician is the examiner.


GETTING READY • • Tell the woman you are going to examine her breasts. • Wash your hands thoroughly with soap and water and dry them with a clean, dry cloth or allow them to air dry before beginning the examination. • If there are open sores or nipple discharge, put new examination or high-level disinfected surgical gloves on both hands. • Ask the woman to undress till the waist. With the woman undressed from the waist up, have her sit on the examining table with her arms at her sides. • Examine both in sitting and lying down position This is a good time to ask if she has noted any changes in her breasts and whether she does monthly breast self-examinations. Tell the woman that you will show her how to do a breast self-examination before she leaves.

PERFORMING A CBE • • • Steps of examination - CBE involves two main parts: • 4 positions Inspection to identify physical signs of breast cancer. Palpation which involves using the finger pads to physically examine all areas of breast tissue including lymph nodes (underarm area) to identify lumps • • Arms by the side of trunk. Raising arms over the head. Pressing on the hips. Leaning forward.

INSPECTION • In the sitting position first visually inspect the breast, initially when woman is sitting up right with arms on her hips, and then with her arms raised over head. • Note any change in symmetry of breast shape, size, skin changes–skin dimpling or retraction or ulceration the level of both nipples, retraction of nipple(s), inverted nipple. •

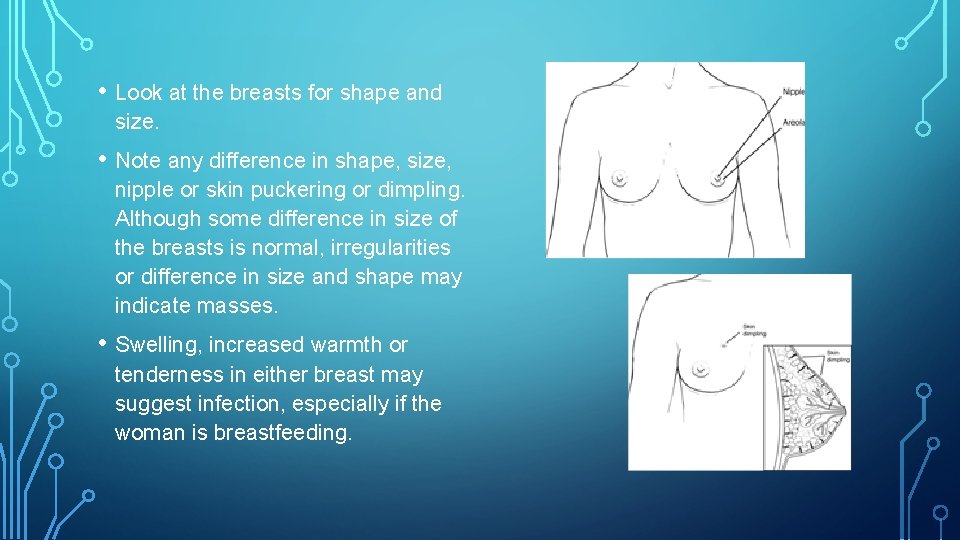
• Look at the breasts for shape and size. • Note any difference in shape, size, nipple or skin puckering or dimpling. Although some difference in size of the breasts is normal, irregularities or difference in size and shape may indicate masses. • Swelling, increased warmth or tenderness in either breast may suggest infection, especially if the woman is breastfeeding.
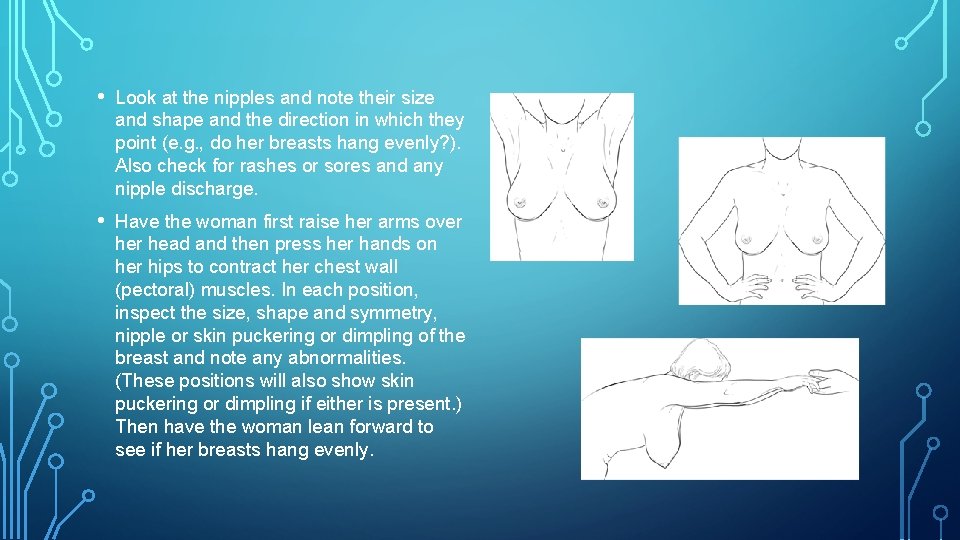
• Look at the nipples and note their size and shape and the direction in which they point (e. g. , do her breasts hang evenly? ). Also check for rashes or sores and any nipple discharge. • Have the woman first raise her arms over head and then press her hands on her hips to contract her chest wall (pectoral) muscles. In each position, inspect the size, shape and symmetry, nipple or skin puckering or dimpling of the breast and note any abnormalities. (These positions will also show skin puckering or dimpling if either is present. ) Then have the woman lean forward to see if her breasts hang evenly.

PALPATION • • Have the woman lie down on the examining table. • • Place a clean sheet or drape over the breast you are not examining. • Use “Dial of clock method” for palpation, first use the finger pads of the middle three fingers to palpate the entire breast, in overlapping circular motions, one area at a time. Repeat both parts of the examination on both the left and rights breasts. Placing a pillow under her shoulder on the side being examined will spread the breast tissue and may help in examining the breast. Place the woman’s left arm over head. Look at the left breast to see if it looks similar to the right breast and whethere is puckering or dimpling.

WOMAN IN LYING DOWN POSITION Palpation pressure The finger pads of middle three fingers should be used to palpate the breast in circular motion • Light pressure for superficial breast tissue • Medium pressure for intermediate layer • Deep pressure for tissue close to chest wall
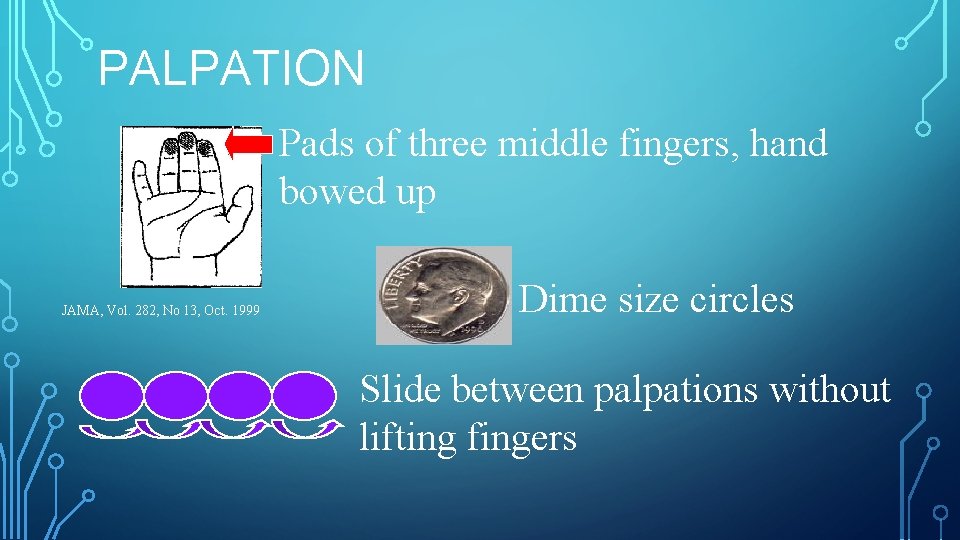
PALPATION Pads of three middle fingers, hand bowed up JAMA, Vol. 282, No 13, Oct. 1999 Dime size circles Slide between palpations without lifting fingers
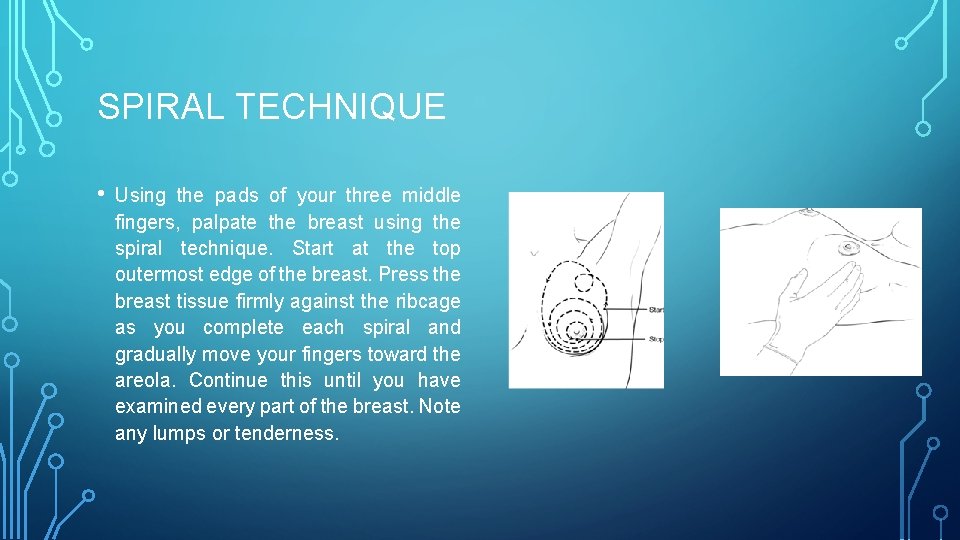
SPIRAL TECHNIQUE • Using the pads of your three middle fingers, palpate the breast using the spiral technique. Start at the top outermost edge of the breast. Press the breast tissue firmly against the ribcage as you complete each spiral and gradually move your fingers toward the areola. Continue this until you have examined every part of the breast. Note any lumps or tenderness.

CHECK FOR NIPPLE DISCHARGE • Using the thumb and index finger, gently squeeze the nipple of the breast. Note any discharge: clear, cloudy or bloody. Any cloudy or bloody discharge expressed from the nipple should be noted in the woman’s record. Although it is normal to have some cloudy discharge from either or both breasts up to a year after giving birth or stopping breastfeeding, rarely it may be due to cancer, infection or a benign tumor or cyst. Repeat these steps for the right breast.
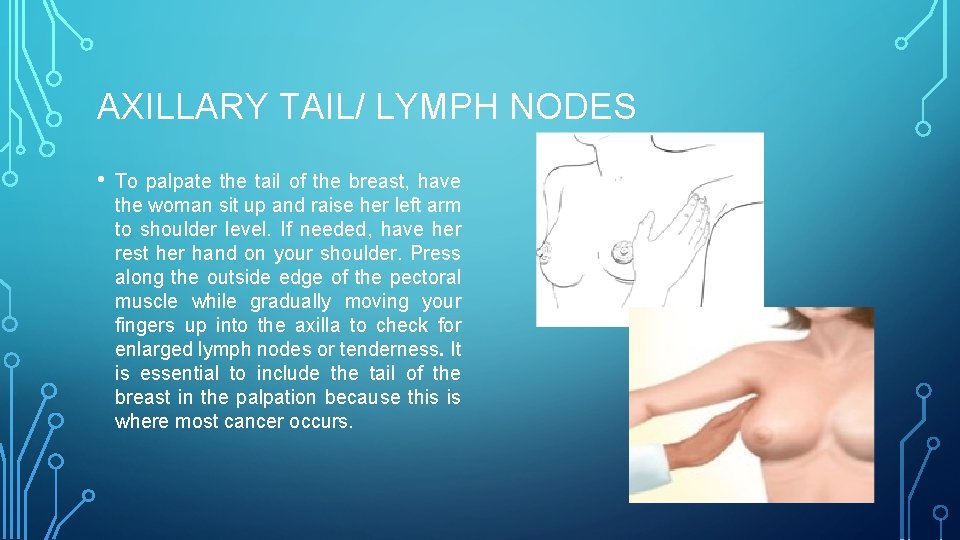
AXILLARY TAIL/ LYMPH NODES • To palpate the tail of the breast, have the woman sit up and raise her left arm to shoulder level. If needed, have her rest her hand on your shoulder. Press along the outside edge of the pectoral muscle while gradually moving your fingers up into the axilla to check for enlarged lymph nodes or tenderness. It is essential to include the tail of the breast in the palpation because this is where most cancer occurs.

DIAL OF A CLOCK METHOD Palpation will be done in each segment until entire breast is covered. • Pads of finger (not tips of fingers) of middle three fingers (index, middle and ring) with hand held in slightly bowed position will be used for palpation. • In the “dial of a clock” method the whole breast is palpated as if it was a dial of a clock, 12 O’ clock being the highest point at upper edge of breast just below the midclavicular point and 6 O’ clock being at the inframammary crease. The palpation is begun at 12 O’clock from periphery to the nipple by describing small circles of about 3 cm in diameter. Following circular movement of the “pad of fingers” 3 times with increasing pressure and without lifting the fingers, the next circle is felt towards the nipple , overlapping with the previous circle to about half in diameter. Once the areola and nipple area is reached, the next segment /sector is palpated at 1 -O’clock. The procedure of palpation with “pad of 3 fingers” is repeated sequentially at 2 0’ clock, 3 0’, 4 0’, 5 0’, 6 0’, 7 0’, 8 0’, 9 0’, 10 0’ and 11 0’. If a lump is detected, its size should be measured using a Vernier caliper. The palpation of mammary ducts is done by gently rolling the ducts between the index finger and the thumb. Any thickening, tenderness or discharge is noted while palpating the mammary ducts. In case of retraction of the nipple an attempt is made to pull the nipple forward to see if the nipple could be brought forward or not and if any lump is present underneath the areola, whether the nipple and the ducts are tethered to the lump or not. The skin overlying the lump is gently pinched and moved with the fingers to see if the skin could be moved freely from /off the lump. If the skin is free from the lump but the movement of lump away from skin causes dimpling of skin, the skin is considered “tethered”. If no movement of skin is possible, it is considered “fixed”. The fixity of lump to underlying pectoralis major muscle is ascertained by requesting the lady to push her hand against the hip to contract the muscle and then moving the lump.



• Note any discharge from the nipple(s), colour of the discharge, swelling/ lumps, consistency of the lumps, swelling in the armpit (axillary area), above the collar bone (supraclavicluar area) and root of the neck (infraclavicular area). • • Repeat this step for the right side. • The optimal time for a CBE in a premenopausal woman is 5 -10 days after the onset of menses, avoiding the week before the period is preferable. Postmenopausal women may have CBE performed at any time. On average, the time required to perform a CBE ranges is 6 to 8 minutes • • Show the woman how to perform breast self-examination. After completing the examination, have the woman dress herself. Explain any abnormal findings and what, if anything, needs to be done. If the examination is entirely normal, tell her everything is normal and healthy and when she should return for a repeat examination (i. e. , annually or if she finds any changes on breast self-examination). Record your findings

LYMPH NODE EXAMINATION • Request the patient to sit on a bed or a stool. For axillary nodes palpation, pectoralis muscle is relaxed by examiner supporting patient’s forearm with his own forearm, while facing the patient. The medial or central, pectoral and lateral axillary nodes were palpated from in front while supraclavicular, infraclavicular and posterior axillary nodes were palpated in sitting position with examiner standing behind the patient. • Please record the findings of a skin change, nipple discharge, any lump and lymph node enlargement in axilla or neck on Case record form in a pictorial manner.

INTERPRETATION & DOCUMENTATION The results of CBE will be interpreted in the following ways: • Normal/negative: No abnormality on visual inspection or palpation • Abnormal: Definite asymmetric finding on either visual inspection or palpation. Presence of lump(s) in the breast, any swellings in the armpit, recent nipple retraction or distortion, skin dimpling or retraction , ulceration, any nipple discharge

WARNING SIGNS The changes that can be seen are: Unusual increase in the size of one breast Puckering of the skin Swelling in upper arm One breast hangs unusually lower Dimpling or puckering of a nipple or areola Change in the appearance of the nipple Milky or bloody discharge from the nipple The changes that can be found on feeling the breasts are: Lump in the breast Enlargement of lymph nodes in axilla or neck

BREAST SELF EXAMINATION • It is best to examine your breasts 7– 10 days after the first day of the menstrual period. (This is the time when the breasts are less likely to be swollen and tender). • You should examine your breasts every month, even after your menstrual period has stopped forever. If you are no longer menstruating, you should pick the same day each month (e. g. , the first day of the month) to examine your breasts. • Breast self-examination can be done after bathing or before going to sleep. Examining your breasts as you bathe will allow your hands to move easily over your wet skin.
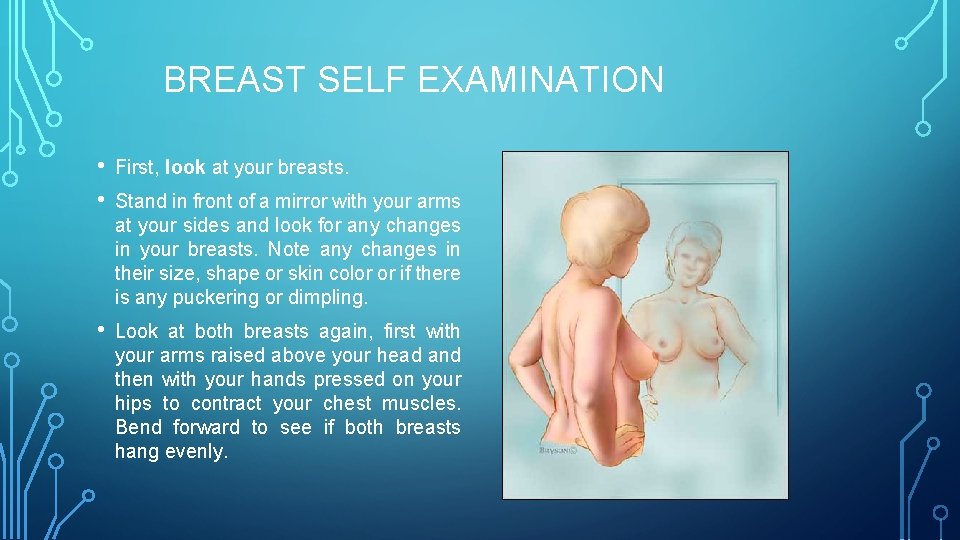
BREAST SELF EXAMINATION • • First, look at your breasts. • Look at both breasts again, first with your arms raised above your head and then with your hands pressed on your hips to contract your chest muscles. Bend forward to see if both breasts hang evenly. Stand in front of a mirror with your arms at your sides and look for any changes in your breasts. Note any changes in their size, shape or skin color or if there is any puckering or dimpling.
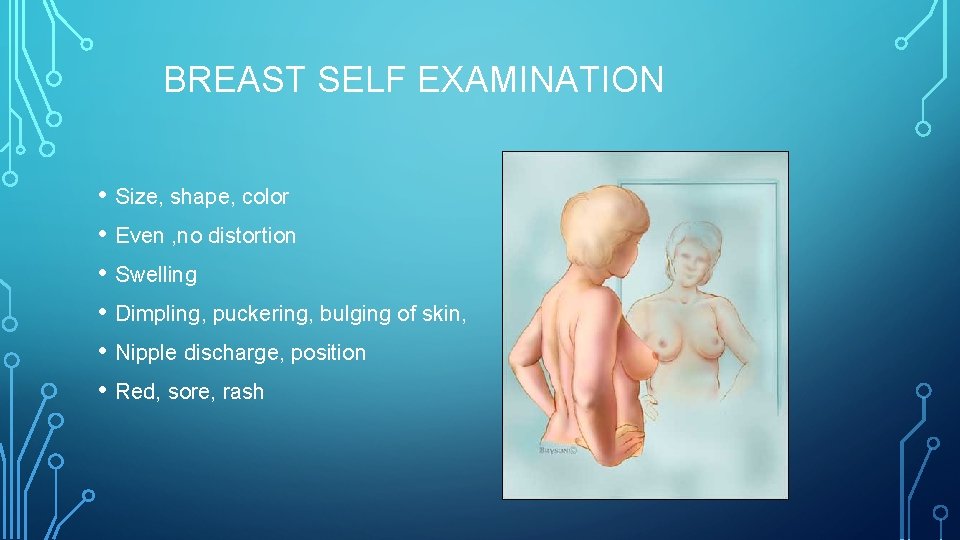
BREAST SELF EXAMINATION • Size, shape, color • Even , no distortion • Swelling • Dimpling, puckering, bulging of skin, • Nipple discharge, position • Red, sore, rash
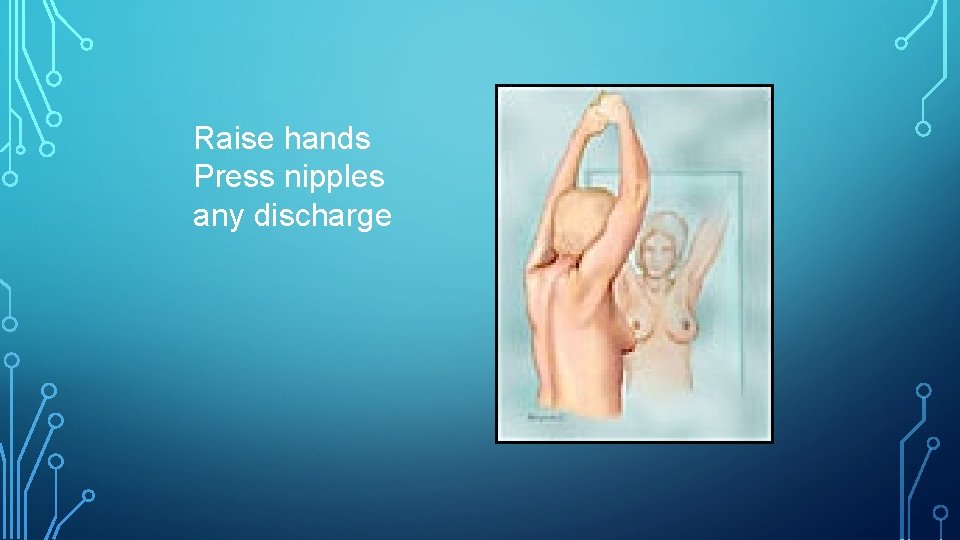
Raise hands Press nipples any discharge

Lie flat, arm below, with opposite hand rotatory movements, feel for any irregularity in breast. Collarbone to abdomen, armpit to cleavage. • • Then, feel your breasts. • Raise your left arm over your head. Use your right hand to press firmly on your left breast with the flat surface (fat pads) of your three middle fingers. Start at the top of the left breast and move your fingers around the entire breast in a large spiral or circular motion. Feel for any lumps or thickening. Continue to move around the breast in a spiral direction and inward toward the nipple until you reach the nipple. • Be sure to check the areas between the breast and the underarm and the breast and the collarbone. • Raise your right arm over your head and repeat the examination for the right breast. You may examine your breasts while standing up or lying down. If you examine your breasts while lying down, it will help to place a folded towel or pillow under the shoulder of the breast you are examining.

In shower, soap hands, raise one arm, feel with opposite

WHAT TO LOOK FOR • • • A change in the size or shape of the breast. • If your breasts are usually lumpy, you should note how many lumps you feel and their locations. Next month, you should note if there any changes in the size or shape (smooth or irregular). Using the same technique every month will help you know if any changes occur. • Any nipple discharge that looks like blood or pus, especially if you are not breastfeeding, should be reported to your healthcare provider. • There may be some discharge from one or both breasts for up to a year after having a baby or stopping breastfeeding A puckering or dimpling of the breast skin. A lump or thickening in or near the breast or underarm area. If the lump is smooth or rubbery and moves under the skin when you push it with your fingers, do not worry about it. But if it is hard, has an uneven shape and is painless, especially if the lump is in only one breast and does not move even when you push it, you should report it to your healthcare provider.

CLINICAL ALGORITHM CBE Positive Negative Evaluation by surgeons Reentry into primary screening Normal Mammography Ultrasonography FNAC Core biopsy Suspicious of malignancy Refer to Medical College/ Regional Cancer Centre for staging/treatment
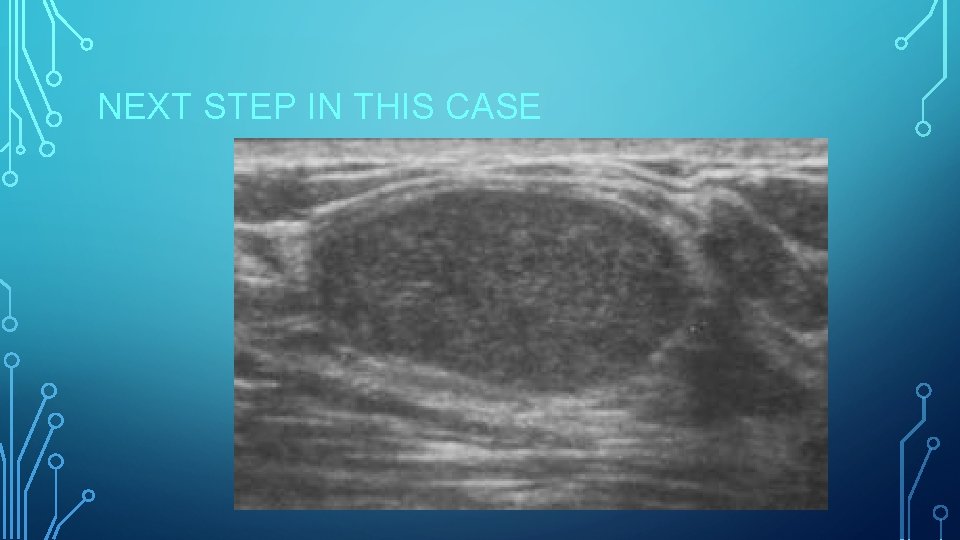
NEXT STEP IN THIS CASE
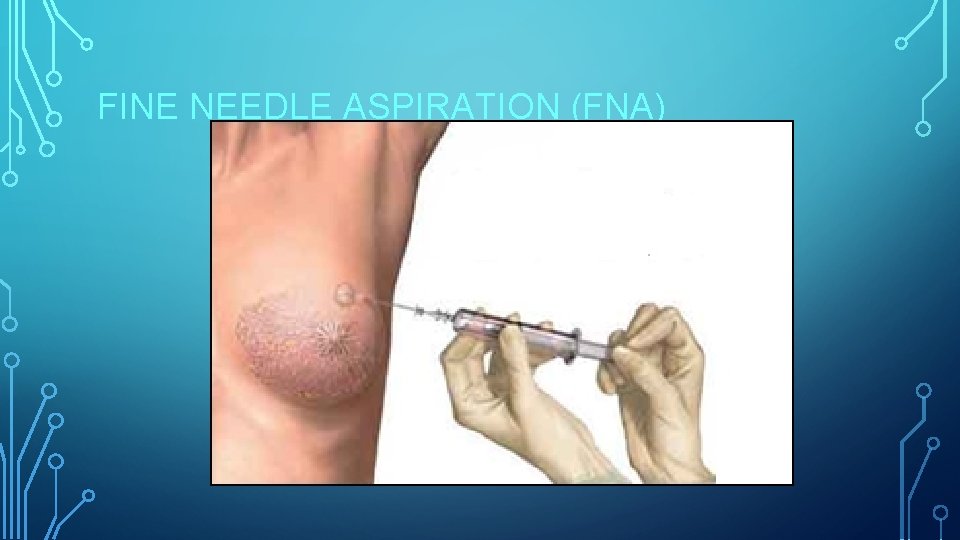
FINE NEEDLE ASPIRATION (FNA)
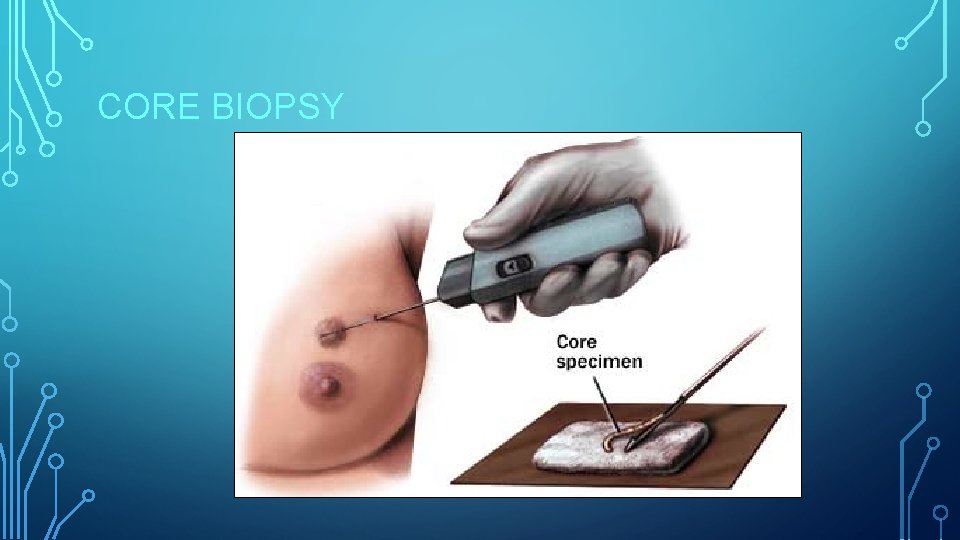
CORE BIOPSY
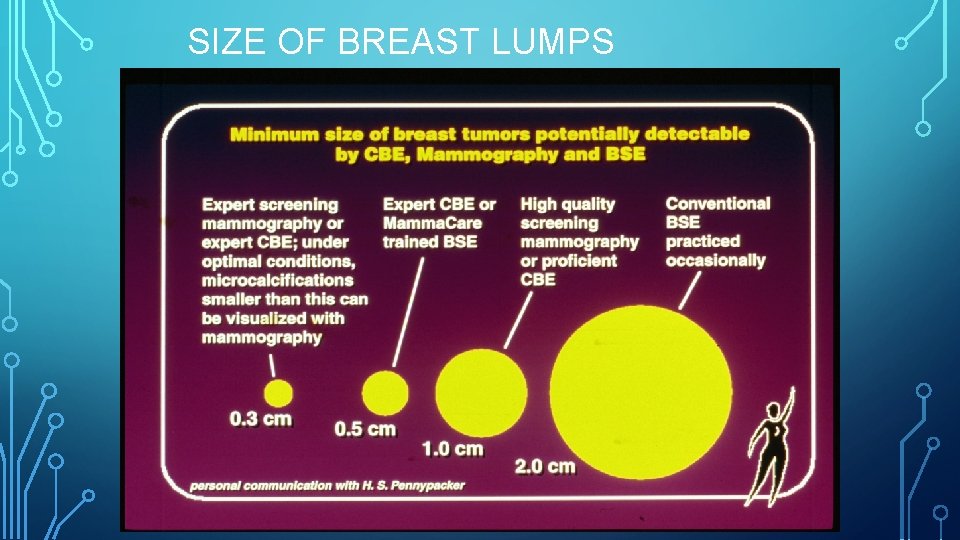
SIZE OF BREAST LUMPS

MANAGEMENT OF BREAST CANCER

RISK FACTORS FOR BREAST CANCER • • Female Aging First degree relative had breast cancer / ovarian cancer. Menstrual history: early onset, late menopause Child birth >30 yrs Long term HRT, 30% increased risk. Oral Contraceptives, risk slight, risk returns to normal once the use of OC’s has been discontinued. Prior radiation exposure to breast at young age. • Breast disease • Atpyical Hyperplasia • Intraductal carcinoma in situ • Intralobular carcinoma in situ • • • Obesity, high BMI Diet rich in Fats, Alcohol Genetic risk factor • BRCA-1 • BRCA-2 • P 53 • Her-2/neu

BREAST CANCER RISK ASSESSMENT Modified Gail model, 7 factors to calculate risk: • • • Age>35 years First degree relative with breast cancer Prior breast biopsies – atypical ductal hyperplasia Age at menarche Age at first child birth Ethinicity Risk of developing breast cancer is indicated by composite score of relative risk for each factor.

FACTORS THAT INFLUENCE SURVIVAL • Age at diagnosis • Tumor size • Stage at diagnosis • Biologic characteristics of tumor: • Hormone receptor status (less significant) • HER 2
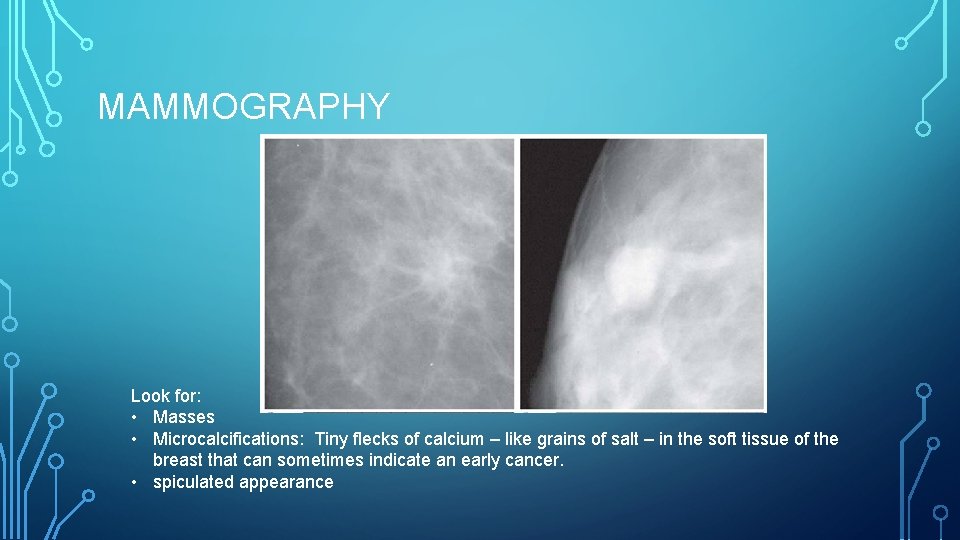
MAMMOGRAPHY Look for: • Masses • Microcalcifications: Tiny flecks of calcium – like grains of salt – in the soft tissue of the breast that can sometimes indicate an early cancer. • spiculated appearance

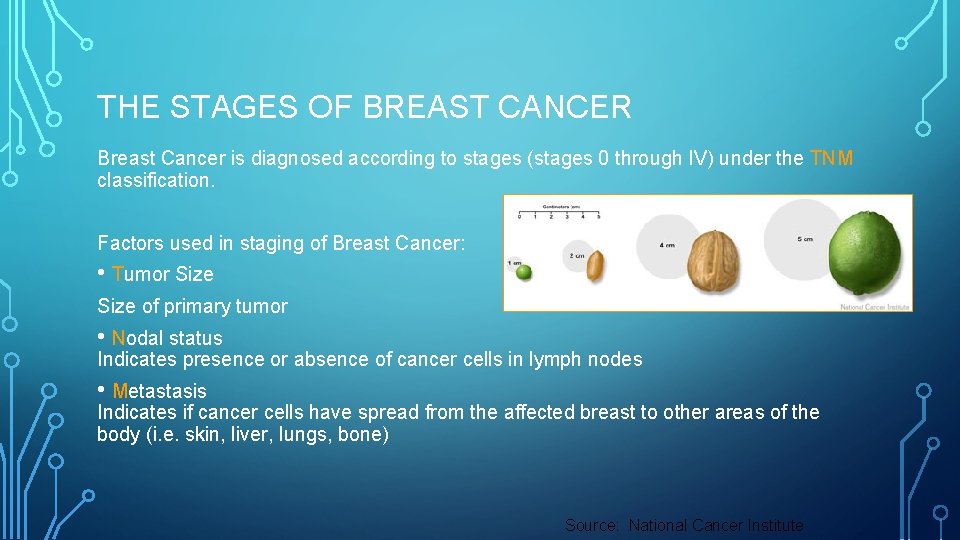
THE STAGES OF BREAST CANCER Breast Cancer is diagnosed according to stages (stages 0 through IV) under the TNM classification. Factors used in staging of Breast Cancer: • Tumor Size of primary tumor • Nodal status Indicates presence or absence of cancer cells in lymph nodes • Metastasis Indicates if cancer cells have spread from the affected breast to other areas of the body (i. e. skin, liver, lungs, bone) Source: National Cancer Institute

STAGING BREAST CANCER Stage 0 Ductal carcinoma in situ (DCIS) is very early breast cancer that has not spread beyond the duct. Stage I Tumor is < 2 cm and has not spread outside the breast. Stage IIA No tumor is found in the breast, but cancer is found in the axillary lymph nodes, or tumor is ≤ 2 cm and has spread to the axillary lymph nodes, or tumor is 2 -5 cm but has not spread to the axillary lymph nodes. Stage IIB Tumor is 2 -5 cm and has spread to the axillary lymph nodes or is > 5 cm but still confined to the breast. Source: National Cancer Institute

ADVANCED BREAST CANCER Stage IIIA The tumor in the breast is smaller than 5 centimeters and the cancer has spread to underarm lymph nodes that are attached to each other or to other structures, OR the tumor is more than 5 centimeters across and the cancer has spread to the underarm lymph nodes. Stage IIIB Tumor has spread to tissue near the breast (i. e. the skin or chest wall) and may have spread to lymph nodes within the breast area or under the arm. Stage IIIC Tumor has spread to the lymph nodes beneath the collarbone and near the neck, and may have spread to the lymph nodes within the breast area or under the arm and to the tissues near the breast. Stage IV Tumor has spread to other organs of the body (i. e. lungs, liver, or brain). Source: National Cancer Institute

BREAST CANCER TREATMENT TNM stage 0 Surveillance LCIS, DCIS Physical exam, mammography, MRI Surgery DCIS: Lumpectomy if DCIS in 1 area, Mastectomy if DCIS in 2 area or large or multifocal Radiotherapy DCIS Usually accompanies lumpectomy Hormonal therapy DCIS In selected ER+ve, for 5 yrs lowers cancer risk.

BREAST CANCER TREATMENT TNM stage 1 & 2 Breast conservative Surgery Lumpectomy Quadrantectomy Radiotherapy Axillary dissection Affected breast chest wall Adjuvant chemotherapy Combination chemotherapy 3 -6 mths Adjuvant Hormonal therapy Premenopausal: tamoxifen in ER+ve, Postmenopausal: Tamoxifen & aromatase inhibitor.

BREAST CANCER TREATMENT TNM stage 3 Surgery Lumpectomy Mastectomy Radiotherapy Chest wall, regional lymph nodes Adjuvant chemotherapy Combination chemotherapy 4 -6 mths Adjuvant Hormonal therapy If ER+ve or PR+ve,

BREAST CANCER TREATMENT TNM stage 4 Surgery Select cases to relieve symptoms Radiotherapy Select cases to relieve symptoms and control local disease. Chemotherapy Primary treatment, single agent or Combination chemotherapy. Hormonal therapy If ER+ve or PR+ve, Monoclonal antibody HER 2 +ve

LOCAL THERAPY: SURGERY Local therapy provides adequate control of locoregional disease, includes surgery and radiotherapy. Surgery: • Mastectomy: Modified radical with sentinel LN evaluation Radical /total mastectomy with sentinel LN evaluation May include breast reconstruction • Breast conservation surgery: Wide local excision Quadrantectomy Lumpectomy , includes axillary dissection if disease invasive.

COMPLICATIONS OF SURGERY • Lymphedema • • 10 -305 women who undergo axillary dissection 3% if sentinel node biopsy only • Numbness • Reduced shoulder mobility • Psychosocial problems of mastectomy • Phantom breast sensation

LOCAL THERAPY: RADIOTHERAPY • Adjuvant radiotherapy in ESBC • • Reduces risk of recurrence May improve survival • Radiotherapy in MBC • Relieves symptoms such as pain, in pts with bone, brain metastasis while not effecting a cure.

RT: METHODS OF DELIVERY • External beam irradiation, to entire breast. • Partial breast irradiation, including brachytherapy • • Radioactive seeds/pellets placed internally near site of tumor for local effects. • 5 yr survival rates comparable to whole breast RT. Can deliver high dose rate radiation, allowing shorter treatment regimes compared to traditional RT

SYSTEMIC THERAPY FOR BREAST CANCER • Hormonal therapy • Chemotherapy • Targeted therapy • Clinical trails provide support for optimal implementation for above therapies in pts with breast cancer.
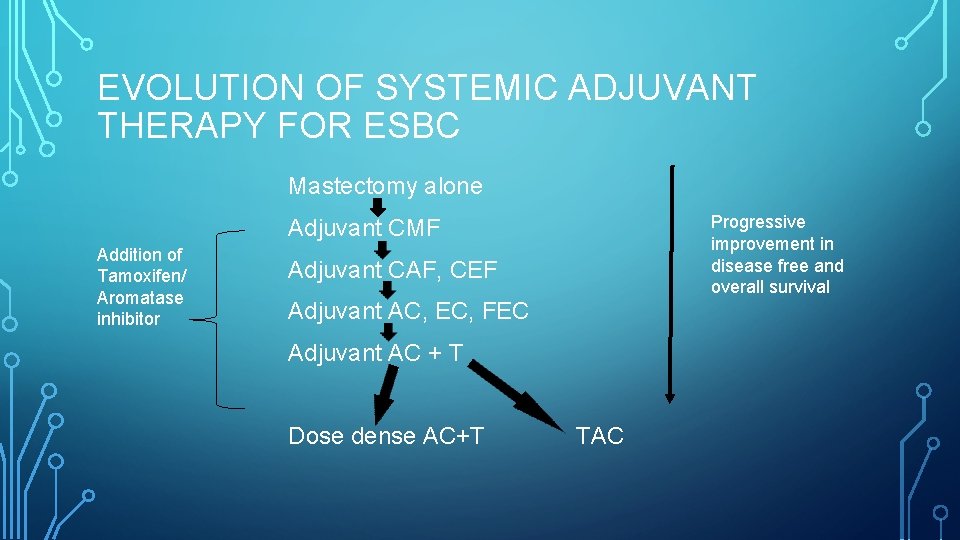
EVOLUTION OF SYSTEMIC ADJUVANT THERAPY FOR ESBC Mastectomy alone Progressive improvement in disease free and overall survival Adjuvant CMF Addition of Tamoxifen/ Aromatase inhibitor Adjuvant CAF, CEF Adjuvant AC, EC, FEC Adjuvant AC + T Dose dense AC+T TAC
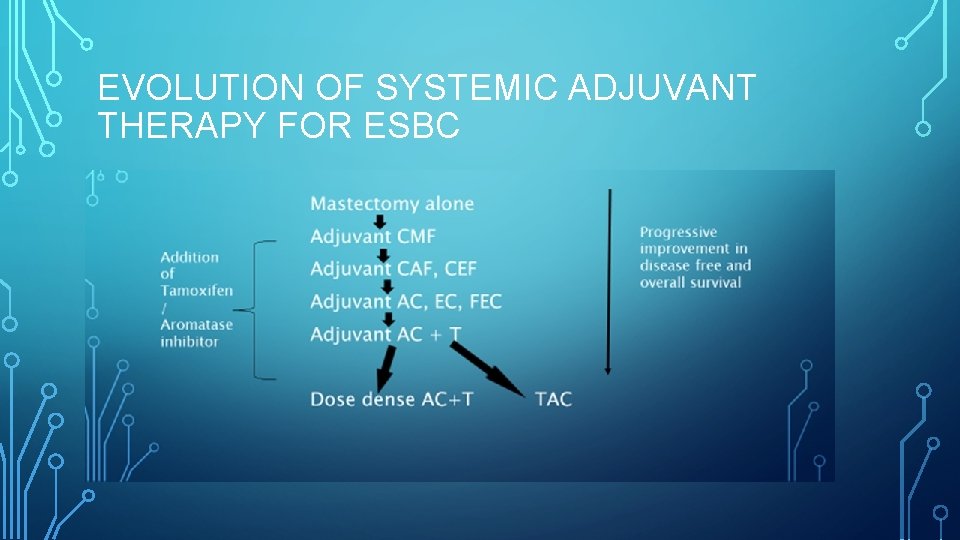
EVOLUTION OF SYSTEMIC ADJUVANT THERAPY FOR ESBC

PREFERRED CT: MBC Single agent options: • • Anthracycline – doxorubicin, epirubicin taxane: - paclitaxel, docetaxel Capecitabine Others – vinoretbine, irinotecan Combination options • • • CAF/FAC -docetaxel, capecitabine AT – paclitaxel, gemcitabine FEC CMF AC, EC – paclitaxel, carboplatin, trastuzumab. • • • Single drug/combination controversial topic • Sequential therapy may be appropriate for pts with indolent disease or nonvisceral MBC> Combinations preferred in MBC Newer combinations improve outcome & manageable safety profile

SUMMARY: ADJUVANT CT IN ESBC • Adjuvant CT improves survival in. ESBC • Improved survival outcomes demonstrated with CMF • Regimes with anthracycline or a taxane improve outcome • Dose dense approach has demonstrated benefit in disease free and overall survival.

TARGETED THERAPY OPTIONS IN BC • HER 2 inhibitor family • Antibodies • • Small molecules • • Trastuzumab Gefitinib Erlotinib Lapafarnib Angiogenesis inhibitor • Antibodies • Bevacizumab

CONCLUSIONS • Although breast cancer incidence has increased, mortality rates due to breast cancer are reducing. • Advances in conventional therapy include less radical surgery and reduced radiation field. • Cytotoxic CT advances include improved types, doses, scheduling. • Improvements in hormonal therapy. • Newer target therapy • Treatment regimes: individualized.
- Slides: 64