Screening Brief Intervention and Referral to Treatment Learning

Screening, Brief Intervention, and Referral to Treatment

Learning Objectives At the end of the session, participants will be able to: 1. Understand SBIRT’s role in preventing the effect of substance abuse on individual and public health 2. Identify substance use risk limits 3. Identify how screening is conducted in a practice setting 4. Practice how to use two screening tools 5. Identify MI basic steps and core skills for the brief intervention 6. Demonstrate and practice MI using core skills

What Is SBIRT? An intervention based on “motivational interviewing” strategies Screening: Universal screening for quickly assessing use and severity of alcohol; illicit drugs; and prescription drug use, misuse, and abuse Brief Intervention: Brief motivational and awareness-raising intervention given to risky or problematic substance users Referral to Treatment: Referrals to specialty care for patients with substance use disorders Treatment may consist of brief treatment or specialty AOD (alcohol and other drugs) treatment.

Leading Off: Defining the problem Substance use: Inappropriate consumption of medicines, drugs. Alcohol, over the counter and prescription drugs. Substance Misuse: consuming enough of a substance to put one’s physical or mental health at risk. Substance Abuse: using a substance in a maladaptive pattern resulting in significant impairment or distress (e. g. significant negative impact with Family, school/work or legal status) Substance Dependence: clinically significant impairment or distress as manifested by 3 or more of the following clinical criteria: Tolerance, withdrawal symptoms, substance taken in larger amounts than intended, unsuccessful attempts at decreasing use, disproportionate amount of time is spent on accessing and taking substance, important activities (social, occupational) are sacrificed to engage in use and continued use despite the person’s knowledge of the negative physiological and psychological effects the substance is having on their life.

Leading Off: Difference Between Abuse and Dependence Abuse is too much, too often. Using substance at unsafe levels, but the person still able to avoid using when they need or want to. Ø Once a month binge drinking, and or drug use Ø Using is having an impact on one of these aspects of the person’s life: family/social, legal status, education/ employment. Dependence is the inability to stop. The substance has become an integral, if not all encompassing, part of the person life. Ø Person to use or drink everyday or else they will experience withdrawal symptoms. Ø Person uses in the morning when they first wake up, or when they are at work. Ø Increased tolerance for substance of choice.

Alcohol vs Drug use: Key differences Ø Alcoholism tends to be insidious. Drug use can explode after several instances of using the substances Ø Drugs give a quicker, more intense high. Ø Increased risk of legal consequences for drug users. Ø More of a social stigma for drug users. Ø People with Alcohol Use Disorders can conceal their issues with more acceptable social rationale.

Detecting Risk Factors Early Screening can be a significant step toward effective intervention: The clinician is often the first point of contact. Early identification and intervention lead to better outcomes. Patients are often seen by a clinician because of a related physical problem. Source: Treatnet. (2008). Screening, assessment and treatment planning. Retrieved from http: //www. unodc. org/ddt-training/treatment/a. html

Effectiveness of SBIRT Data from SAMSHA grant programs demonstrate the impact of SBIRT on patient health: – Reduction in alcohol and drug use 6 months after receiving the intervention (41% of respondents reported abstinence from drugs and/or alcohol at followup, compared to 16% at baseline – Improvement in quality of life measures, including employment/education status, housing stability and 30 -day past arrest rates (95% of respondents reported no arrests in the past 30 days at follow-up, compared to 88% at baseline) – Reduction in risky behaviors, including fewer unprotected sexual encounters (injection drug use decreased from 3. 2% at baseline to 1. 5% at follow-up)

Effectiveness of SBIRT – Meta-analysis of brief alcohol intervention (19 trials of 5639 individuals, with 17 trials measuring ETOH consumption) 8 reported a significant effect of the intervention in the Primary Care setting, with reduced alcohol consumption for both men and women at six- and 12 month follow-ups (Bertholet et al. 2005) – SBIRT research has focused mainly on alcohol use, less on illicit drug users. However with the validation of the Alcohol, Smoking and Substance Involvement Screening Test (ASSIST), one study found Brief Interventions reduced scores in patients for all ASSIST measures (Humeniuk et al. 2012).

Based on Findings of Screening Dependent Use Harmful Use At-Risk Use Low Risk

A Positive Alcohol Screen = At-Risk Drinker Binge drink ( 5 for men or 4 for women/anyone 65+) Or patient exceeds regular limits? (Men: 2/day or 14/week Women/anyone 65+: 1/day or 7/week) NO Patient is at low risk. YES Patient is at risk. Screen for maladaptive pattern of use and clinically significant alcohol impairment using AUDIT.

How Much Is “One Drink”? 5 -oz glass of wine (5 glasses in one bottle) 12 -oz glass of beer (one can) 1. 5 -oz spirits 80 -proof 1 jigger Equivalent to 14 grams pure alcohol

AUDIT Alcohol Use Disorders Identification Test What is it? – Ten questions, self-administered or through an interview; addresses recent alcohol use, alcohol dependence symptoms, and alcohol-related problems – Developed by World Health Organization (WHO)

AUDIT Alcohol Use Disorders Identification Test What are the strengths? – Public domain—test and manual are free – Validated in multiple settings, including primary care – Brief, flexible – Focuses on recent alcohol use – Consistent with ICD-10 and DSM IV definitions of alcohol dependence, abuse, and harmful alcohol use Limitations? – Does not screen for drug use or abuse, only alcohol

Scoring the AUDIT (20+) Dependent Use Harmful Use (16‒ 19) At-Risk Use (8‒ 15) Low Risk (0‒ 7)

Prescription Drug Misuse Although many people take medications that are not prescribed to them, we are primarily concerned with— Opioids (oxycodone, hydrocodone, fentanyl, methadone) Benzodiazepines (clonazepam, alprazolam, diazepam) Stimulants (amphetamine, dextroamphetamine, methylphenidate) Sleep aids (zolpidem, zaleplon, eszopicione) Other assorted (clonidine, carisoprodol)

Common Illicit Drugs Marijuana (Cannabinoids): psychological dependence. Crack/Cocaine (Stimulants): short half-life, fast withdrawal. Heroin (Opioids): effects similar to prescription opioids. Crystal Methamphetamine (Stimulants) : Fast addiction, MSM. Ecstasy (Club Drug) LSD, Shrooms (Hallucinogens): small chance of dependence.

Prescreening for Drugs “How many times in the past year have you used an illegal drug or used a prescription medication for nonmedical reasons? ” (…for instance because of the feeling it caused or experiences you have…) If response is, “None, ” screening is complete. If response contains suspicious clues, inquire further. Sensitivity/Specificity: 100%/74% Source: Smith, P. C. , Schmidt, S. M. , Allensworth-Davies, D. , & Saitz, R. (2010). A single-question screening test for drug use in primary care. Arch Intern Med , 170(13), 1155− 1160.

A Positive Drug Screen ANY positive on the drug prescreen question puts the patient in an “at-risk” category. The followup questions are to assess impact and whether substance use is serious enough to warrant a substance use disorder diagnosis. Ask which drugs the patient has been using, such as cocaine, meth, heroin, ecstasy, marijuana, opioids, etc. Determine frequency and quantity. Ask about negative impacts.

Drug Abuse Screening Test (10) What is it? – Shortened version of DAST 28, containing 10 items, completed as selfreport or via interview. DAST(10) consists of screening questions for atrisk drug use that parallel the MAST (an alcohol screening instrument) – Developed by Addiction Research Foundation, now the Center for Addiction and Mental Health – Yields a quantitative index of problems related to drug misuse What are the strengths? – Sensitive screening tool for at-risk drug use What are the weaknesses? – Does not include alcohol use

Scoring the DAST(10) High Risk (6+) Harmful Use (3‒ 5) Hazardous Use (1‒ 2) Abstainers (0)

TWEAK SCREENING TOOL TOLERANCE – HOW MANY DRINKS DOES IT TAKE TO MAKE YOU FEEL HIGH? 2 OR MORE = 2 POINTS WORRY – HAVE CLOSE FRIENDS WORRIED OR COMPLAINED ABOUT YOUR DRINKING IN THE PAST YEAR? YES = 1 POINT EYE – OPENER – HAVE YOU EVER HAD A DRINK FIRST THING IN THE MORNING TO STEADY YOUR NERVES OR GET RID OF A HANGOVER? YES = 1 POINT AMNESIA – HAS ANYONE EVER TOLD YOU ABOUT THINGS THAT YOU SAID OR DID WHILE DRINKING THAT YOU DO NOT REMEMBER? YES = 1 POINT KUT DOWN – HAVE YOU FELT YOU OUGHT TO CUTDOWN ON YOUR DRINKING? YES = 1 POINT

CRAFFT- Adolescent Screening tool 1. Have you ever ridden in a CAR driven by someone (including yourself) who was high or had been using alcohol or drugs? 2. Do you ever use alcohol or drugs to RELAX, feel better about yourself, or fit in? 3. Do you ever use alcohol or drugs while you are by yourself ALONE? 4. Do you ever FORGET things you did while using alcohol or drugs? 5. Do your FAMILY or FRIENDS ever tell you that you should cut down on your drinking or drug use? 6. Have yo ever gotten into TROUBLE while you were using alcohol or drugs?

Key Points for Screening Screen everyone. Screen both alcohol and drug use including prescription drug abuse and tobacco. Use a validated tool. Prescreening is usually part of another health and wellness survey. Explore each substance; many patients use more than one. Follow up positives or "red flags" by assessing details and consequences of use. Use your MI skills and show nonjudgmental, empathic verbal and nonverbal behaviors during screening.

Motivational Interviewing Steps and Core skills

Definition of Motivational Interviewing “Motivational interviewing is a client-centered, directive method for enhancing intrinsic motivation to change by exploring and resolving ambivalence. ”

Applications of Motivational Interviewing MI enhances change for a range of behaviors: • Diet • Exercise • Reduction of alcohol and illicit drugs • Safer sex practices • Medication adherence (Burke et al. , 2003; Hettema et al. , 2005; Rubak et al. , 2005).

Four Steps of the MI Process 1. Engage (Express Empathy, Ask Open-Ended Questions) 2. Focus (Reflecting, Summarizing) 3. Evoke (Motivations, Concerns) 4. Plan (Raise Subject, Support Self-Efficacy)

Spirit of Motivational Interviewing üCollaborative (not confrontation) - Developing a partnership in which the patient’s expertise, perspectives, and input are central to the consultation - Fostering and encouraging power sharing in the interaction üEvocative - Motivation for change resides within the patient - Motivation is enhanced by eliciting and drawing on the patient’s own perceptions, experiences, and goals

Spirit of Motivational Interviewing üRespectful of autonomy (not authority) - Respecting the patient’s right to make informed choices facilitates change - The patient is in charge of his/her choices and responsible for the outcomes - Emphasize patient control and choice üCompassionate - Empathy for the experience of others - Desire to alleviate the suffering of others - Belief and commitment to act in the best interests of the patient
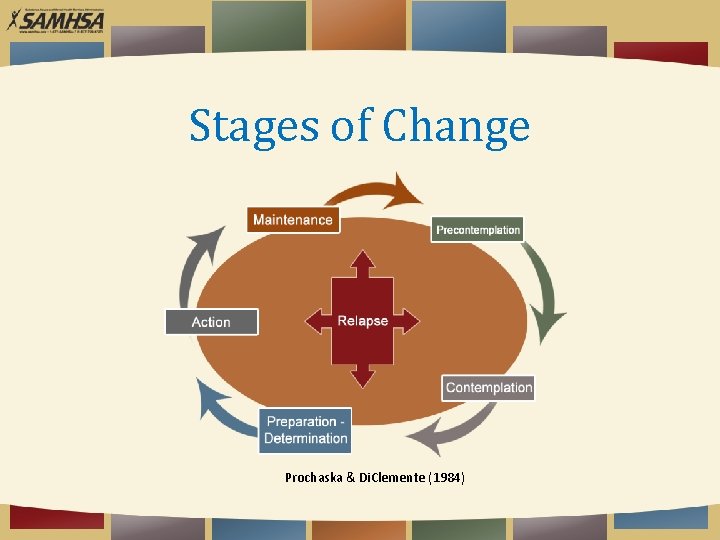
Stages of Change Prochaska & Di. Clemente (1984)
Stage Patient state Clinician goal Precontemplation The patient is not yet recognizing problem or considering change. Clinician’s goal is to build rapport and raise awareness. Clinician’s task is to inform and encourage. Contemplation The patient is evaluating reasons for and against change. Clinician’s goal is to build motivation. Clinician’s task is to explore and resolve ambivalence. Preparation The patient is planning for change. Clinician’s goal is to negotiate a plan. Clinician’s task is to facilitate decision-making. Action The patient is making the identified change(s). Clinician’s goal is to support implementation of the plan. Clinician’s task is to support self -efficacy. Maintenance The patient is working to sustain change(s). Clinician’s goal is to help maintain change. Clinician’s task is to prevent relapse.

Motivational Interviewing Core skills

Core MI Skills üOpen-Ended Questions üAffirmations üReflections üSummaries

Open-Ended Questions Using open-ended questions— Ø Enables the patient to convey more information Ø Encourages engagement Ø Opens the door for exploration

Open-Ended Questions What are open-ended questions? Gather broad descriptive information Require more of a response than a simple yes/no or fill in the blank Often start with words such as— – “How…” – “What…” – “Tell me about…” Usually go from general to specific

Closed-Ended Questions Present Conversational Dead Ends Closed-ended questions typically— Are for gathering very specific information Tend to solicit yes-or-no answers Convey impression that the agenda is not focused on the patient

Closed-Ended Questions Ø Avoid “Why? ” Questions • Puts patient in a passive, or defensive, role • No opportunity for patient to explore ambivalence

Learning Exercise Turning closed-ended question into an open-ended one. Do you feel depressed or anxious?

Affirmations What is an affirmation? Compliments or statements of appreciation and understanding – Praise positive behaviors – Support the person as they describe difficult situations

Affirmations Why affirm? Support and promote self-efficacy, prevent discouragement Build rapport Reinforce open exploration (patient talk) Caveat Must be done sincerely

Affirmations May Include: Commenting positively on an attribute: "You are determined to get your health back. ” A statement of appreciation: "I appreciate your efforts despite the discomfort you’re in. " A compliment: "Thank you for all your hard work today. "

Learning Exercise Provide an affirmation for each given patient scenario.

Reflective Listening Reflective listening is one of the hardest skills to learn. “Reflective listening is a way of checking rather than assuming that you know what is meant. ” (Miller and Rollnick, 2002)

Reflective Listening Why listen reflectively? – Demonstrates that you have accurately heard and understood the patient – Strengthens the empathic relationship

Reflective Listening Why listen reflectively? Ø Encourages further exploration of problems and feelings Ø Avoid the premature-focus trap Ø Can be used strategically to facilitate change

Levels of Reflection Simple Reflection—stays close Ø Repeating Ø Rephrasing (substitutes synonyms) Example Ø Patient: I hear what you are saying about my drinking, but I don’t think it’s such a big deal. Ø Clinician: So, at this moment you are not too concerned about your drinking.

Levels of Reflection Complex Reflection—makes a guess – Paraphrasing—major restatement, infers meaning, “continuing the paragraph” Examples Patient: “Who are you to be giving me advice? What do you know about drugs? You’ve probably never even smoked a joint! Clinician: “It’s hard to imagine how I could possibly understand. ” *** Patient: “I just don’t want to take pills. I ought to be able to handle this on my own. ” Clinician: “You don’t want to rely on a drug. It seems to you like a crutch. ”

Levels of Reflection Complex Reflection – Reflection of feeling—deepest Example Patient: My wife decided not to come today. She says this is my problem, and I need to solve it or find a new wife. After all these years of my using around her, now she wants immediate change and doesn’t want to help me! Clinician: Her choosing not to attend today’s meeting was a big disappointment for you.

Learning Exercise Turning patient statements into reflections. Ex: Work has been hectic and some wine helps me relax.

Summaries Periodically summarize what has occurred in the visit. Summary usages – Begin a session – End a session – Transition

Summaries Strategic summary—select what information should be included and what can be minimized or left out. Additional information can also be incorporated into summaries—for example, past conversations, assessment results, collateral reports, etc.

Examples Summaries – “So, let me see if I’ve got this right…” – “So, you’re saying… is that correct” – “Make sure I’m understanding exactly what you’ve been trying to tell me…” Double sided reflections are often highly effective as summaries to illustrate ambivalence.

Sustain Talk and Change Talk Sustain Talk Patient explanations for why they want to continue current activities Ø I don’t see how I could give up drinking Ø I don’t think I need to stop using heroin Change Talk Any statements the Patient makes about wanting to change current behaviors Ø Ø Desire for Change Ability to make Change Reasons for Change Need for Change

Increasing Change Talk Change talk is at the heart of MI. Through our conversations, we elicit— Desire – I wish…I want to…I’d like to Ability – I can…I could…I am able to…I would Reasons – It’s important because…There are good reasons to Need – I have to… Commitment- I intend to…I will…I plan to

Evoking Change Talk What has you thinking about changing? (Reveals desire) If you were to change, how would you do it? (evokes ability) What are your three most important reasons for wanting to change? (evokes reasons) How would things be different (better) if you decided to change? (reveals the need) Based on SBIRT 101 presentation by Alan Lyme

Learning Exercise Provide a reflection or affirmation for each patient statement. Remember: Change talk may not always be obvious.

Readiness Rulers: Confidence Readiness Importance Confidence Readiness rulers can address—

Readiness Ruler On a scale of 1 to 10, how ready are you to make a change?

Referral to Treatment Referral

What Is Treatment? Treatment may include— Counseling and other psychosocial rehabilitation services (Inpatient and outpatient services) Medications Involvement with self-help (AA, NA, Al-Anon) Complementary wellness (diet, exercise, meditation) Combinations of the above

Treatment Options Outpatient individual counseling- Patient meets with counselor and discusses various topics including coping skills, interpersonal relationships, psychiatric disorders and substance use. Outpatient group counseling- A group of patients meet to share information about their own lives and give feedback to other patients in a setting facilitated by a group leader. Groups often focus on topics like Anger Management, Relapse Prevention and Harm Reduction. Adult day treatment program- Patients can attend a day program that includes group and individual counseling, recreation activities, daily meals and medical care. Medication Assisted Therapy (MAT)- Combination of behavioral therapy and medications to treat substance use disorders, for example Methadone or Buprenorphine, or Naltrexone. Detox- Detox can occur inpatient or outpatient and is done under the supervision of medical staff to monitor withdrawal symptoms. Always needed for Patient withdrawing from alcohol due to delirium tremens. 28 -day program- Patient lives in the rehabilitation center for 28 days and attends individual and group therapy sessions.

Medication Assisted Treatment (MAT) Combination of medication and counseling Treatment options for opioid addiction: • Methadone • Buprenorphine • Naltrexone Emergency treatment for opioid overdose: • Naloxone

Referral Guidelines for Greatest Success Determine if patient is drug or alcohol dependent and needs medical detoxification (usually inpatient) A nondependent substance abuser is usually treated outpatient unless there are other risk factors Most patients can be successfully served in outpatient treatment

A Strong Referral to Appropriate Treatment Provider Is Key When your patient is ready— Make a plan with the patient. You or your staff should actively participate in the referral process. The warmer the referral handoff, the better the outcome. Decide how you will interact/communicate with the provider. Confirm your follow-up plan with the patient. Decide on the ongoing follow-up support strategies you will use.

What Is a Warm-Handoff Referral? The clinician directly introduces the patient to the treatment provider to confer trust and build rapport Evidence strongly indicates that warm handoffs are dramatically more successful than passive referrals

Common Mistakes To Avoid Rushing into “action” and making a treatment referral when the patient isn’t interested or ready Referring to a program that is full or does not take the patient’s insurance Not knowing your referral base Not considering pharmacotherapy in support of treatment and recovery Seeing the patient as “resistant” or “self-sabotaging” instead of having a chronic disease

Learning Exercise
- Slides: 68