SchoolBased Medicaid Expanded Care May 2020 What is


School-Based Medicaid Expanded Care May 2020

What is Expanded Care? } Expanded care allows schools to potentially bill for services provided to Medicaid-eligible children that fall outside the Individual Education Program (IEP) Link to Centers for Medicare and Medicaid Services (CMS) guidance and policy: https: //www. medicaid. gov/sites/default/files/federalpolicy-guidance/downloads/smd-medicaid-payment-forservices-provided-without-charge-free-care. pdf 3

What does this mean for Kentucky? } April 28, 2019: State plan amendment (SPA) was submitted to CMS } Nov. 4, 2019: CMS approved Kentucky’s SPA IEPs in Kentucky 25% Medicaid Eligible Students 75% Medicaid Eligible Students IEPs in Kentucky https: //chfs. ky. gov/agencies/dms/spa/KY-19 -0003, %20 Approval%20 Documents. pdf 4
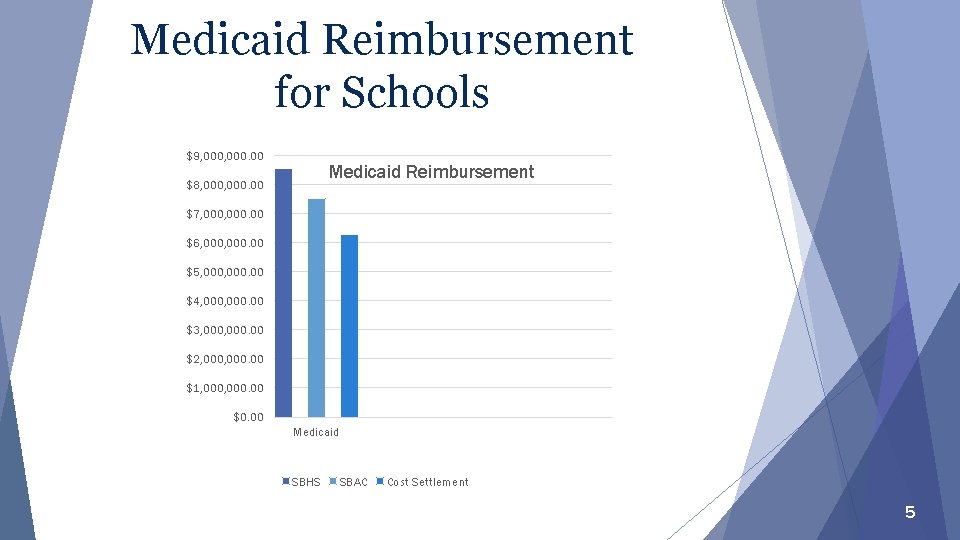
Medicaid Reimbursement for Schools $9, 000. 00 Medicaid Reimbursement $8, 000. 00 $7, 000. 00 $6, 000. 00 $5, 000. 00 $4, 000. 00 $3, 000. 00 $2, 000. 00 $1, 000. 00 $0. 00 Medicaid SBHS SBAC Cost Settlement 5

School-Based Administrative Claiming (SBAC) } SBAC offers reimbursement for the costs of administrative activities, such as outreach, that support the Medicaid program. } Allowable activities are: ● Medicaid outreach and related training ● Facilitating Medicaid eligibility application ● Health-related referral activities and monitoring of health service delivery ● Medical service program planning, policy development and interagency coordination ● Arranging for Medicaid-related transportation and provision of Medicaidrelated translation Link to the School-Based Administrative Claiming technical assistance document: https: //education. ky. gov/districts/Documents/Revised%20 KY%20 SBAC%20 Time%20 Study% 20 Document%2006132013. pdf 6

Cost Reporting Cost Settlement } Kentucky transitioned to a cost-based approach for the Fee for Service (FFS) program and Specialized Transportation beginning with the 2008 -2009 cost report period } FFS Cost Reports must be completed annually and are used to compare FFS “interim” payments received throughout the year to actual costs collected on the Cost Report } Cost Reports are interrelated with the FFS and Administrative Claiming Random Moment Time Study (RMTS) processes currently in place 7

Medicaid School-Based Health Services (SBHS) • The Medicaid School-Based Health Services (SBHS) program is a unique Medicaid program designed for local education agencies (LEAs). The goal of this program is to provide local school districts with another fiscal resource to offset the costs of providing school-based health-related services to students with disabilities in an educational setting under the Individuals with Disabilities Education Act (IDEA). The services provided are necessary for the student to benefit from special education. 8

Basic Requirements for Billing } Child must be Medicaid eligible } Parental consent } Child must have a reimbursable service listed in the IEP or service must be medically necessary } Practitioner must not be paid, 100% federally funded } Practitioner must be listed on annual application or an approved amendment 9

Medical Necessity } “Medically Necessary” or “Medical Necessity” means health care services that a practitioner, exercising prudent clinical judgment, would provide to a patient. } The CMS defines medical necessity as “services that meet accepted medical standards or items reasonable and necessary for the diagnosis or treatment of illness or injury or to improve the function of a malformed body member. ” } Per CMS, documentation for medical necessity may include clinical evaluations, physician evaluations, consultations, progress notes, physician’s records, records from other healthcare professionals and test reports. It is maintained by the physician and/or provider. For more information, please refer to the Program Integrity Manual, Pub 100 -08, Chapter 3, Section 3. 2. 3 A. Medicaid Regulation 907 KAR 1: 715. School-based Health Services 10

Medical Necessity Examples } A school conducts a screening for all children; the school may be able to bill for Medicaid-eligible children. } Johnny goes to see the nurse. Since he has Medicaid, the school may be able to bill for his visit with backup documentation. 11

Parental Consent } Notice of Parent Consent for School District’s Use of Public Benefits or Insurance (Medicaid) under 34 CFR § 300. 154(d)(2)(iv) } Parental consent must be obtained once, unless: ● The student moves from district and comes back. You must obtain parental consent again. ● Annual notification sent to parents ● The new parental consent covers IEP and Expanded Care services ● The dual consent doesn’t void the previous IEP consent If the parent denies consent, district may not bill Medicaid for any services provided in the school setting. 12

Best Practice – Parental Consent } KDE recommends the following: § Get dual parental signed for each child § Send parental consent with annual registration packets § Have an electronic backup of all parental consents § Have written policies and procedures regarding parental consent 13

Parental Consent Form KDE’s new parental consent that provides consent for IEP and Expanded Services students. 14

Covered Services The following services currently are eligible for Medicaid reimbursement when provided to a Medicaid-eligible student: } Nursing } Audiology } Speech-Language } Occupational Therapy } Physical Therapy } Mental Health } Incidental Interpreters } Orientation and Mobility 15
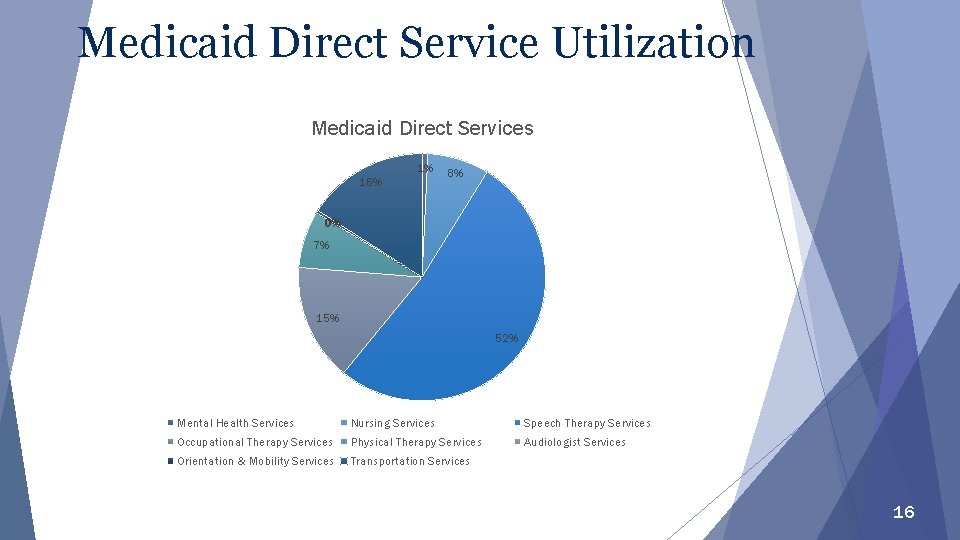
Medicaid Direct Service Utilization Medicaid Direct Services 1% 16% 8% 0% 7% 15% 52% Mental Health Services Nursing Services Speech Therapy Services Occupational Therapy Services Physical Therapy Services Audiologist Services Orientation & Mobility Services Transportation Services 16

Components to SBHS Billing } For the first year of “Expanded Access” services (ending June 30, 2020), claims will be reimbursed by Medicaid’s Physician Fee Schedule and there can be no duplication in 1905(a) services between IEP and Expanded Access Services. Practitioners who are providing services to IEP students would not be able to bill for services provided to those Medicaid students without an IEP/IFSP. } Therapy: ● Individual Therapy Face-to-face, one-on-one encounter between the student and practitioner ● Group Therapy Rehabilitation services which offer activities in a therapeutic environment that focus on the development and restoration of the skills of daily living Group must be comprised of 6 or fewer students 17

Evaluations } All parts are billable } When billing for an evaluation, you must bill the exact times and dates that you provide the evaluation ● Example: If you are providing an evaluation for Aubrey and you observe her on Monday at 12: 30 p. m. , test her on Wednesday at 10 a. m. , and then write the report on Friday at 2 p. m. , you will need to bill these exact times 18

Procedure Codes } There is an expanded list of procedure codes } Time-Based vs. Service-Based } Full list of procedure codes can be found at : https: //education. ky. gov/districts/Pages/School-Based. Medicaid-Services. aspx 19
![Rate of Providers Ø Unit Rate = ([Employee Hourly Rate] + [Hourly Employer Paid Rate of Providers Ø Unit Rate = ([Employee Hourly Rate] + [Hourly Employer Paid](http://slidetodoc.com/presentation_image/55ba86b43276594c65682ba04bcabc86/image-20.jpg)
Rate of Providers Ø Unit Rate = ([Employee Hourly Rate] + [Hourly Employer Paid Benefit Amount]) ÷ 4 The unit rate is then multiplied by the number of billable units when claims are transmitted to Medicaid. Example: Provider is paid $100 -per-hour base pay and $10 per hour in benefits. (100 + 10) ÷ 4 110 ÷ 4 $27. 50 = Unit Rate If therapist bills for 2 units of therapy, then the claim is transmitted as: (27. 50 unit rate) x (2 units of therapy) Amount Billed: $55. 00 20

Things to Remember … } Practitioners can’t be 100% federally funded } Practitioners must be included on the KDE Annual Application } *For the first year of “Expanded Access” services (ending June 30, 2020), claims will be reimbursed by Medicaid’s Physician Fee Schedule and there can be no duplication in 1905(a) services between IEP and Expanded Access Services. Practitioners who are providing services to IEP students would not be able to bill for services provided to those Medicaid students without an IEP/IFSP. ● Example: Dr. Jones, a psychologist, is providing behavioral health services to a Medicaid student with an IEP. He would not be able to bill for services provided to a Medicaid student without an IEP/IFSP while in the school-based setting. 21

Quality Assurance Ø KDE will mandate districts submit a quality assurance for the 2021 -2022 school year Ø Districts will provide their processes and policies to KDE when submitting their annual application Ø This program is in place to avoid program shortfalls, compliancy issues and improve future monitoring reviews 22

I’ve met all billing requirements, what’s next? } Identify point of contact for your district } Work on 2020 -2021 annual application } Create written policies and procedures } Get parental consent 23

Annual Application 24

GMAP Application Process Ø 2020 -2021 SBHS Medicaid application process is going electronic Ø This process will fulfill the recommended guidelines of Healthy at Work and provide a simpler process for districts Ø GMAP Login link: https: //gmap. education. ky. gov/ 25

What’s Next … } Be cautious of contractual agreements } Contact KDE if you have any questions } Reach out to your billing agents } Please attend our fall training! 26

Keep an eye out for …. } KDE’s School Based Best Practices mini webinar, coming in summer 2020 27

Contact Information KDE Contacts: Medicaid Contact: Stephanie O’Connor and Lindsey Kimbleton Lucy Senters Division of Budgets and Financial Management Kentucky Department of Education Sower Building, 5 th Floor 300 Sower Blvd. Frankfort, KY 40601 (502) 564 -1979 schoolbasedmedicaid@education. ky. gov Kentucky Department for Medicaid Services 6 th Floor West 275 East Main St. Frankfort, KY 40601 (502) 564 -6890 lucy. Senters@ky. gov 28

KDE School-Based Medicaid Website } http: //education. ky. gov/specialed/Pages/School. Based-Medicaid-Services. aspx } https: //www. medicaid. gov/sites/default/files/federa l-policy-guidance/downloads/smd-medicaidpayment-for-services-provided-without-charge-freecare. pdf 29

Questions 30
- Slides: 30