Scabies n Sarcoptis scabiei var hominis n 8



Scabies n Sarcoptis scabiei var. hominis n 8 legs n female: 0. 4× 0. 3 mm, male: 0. 22× 0. 18 mm n Two to three eggs daily and total 10 -25 egg are laid by fertilized female in burrows; after 72 -84 hours larvae emerge and after 3 molts (8 -10 days), leave the burrow for surface and became adult mite
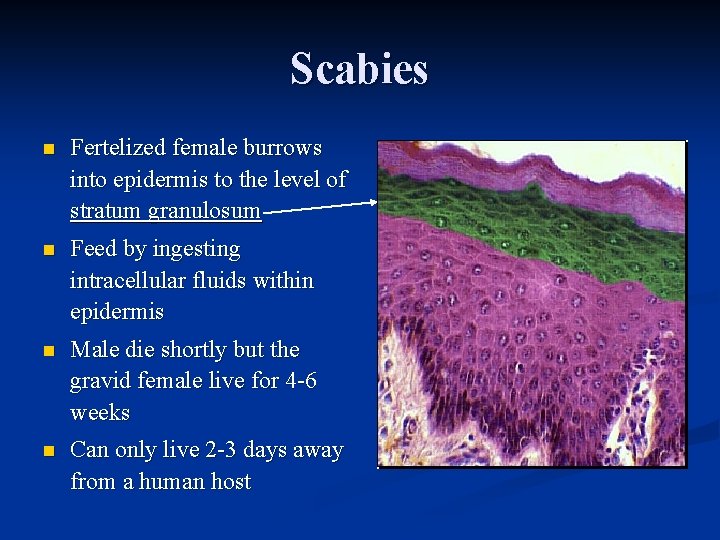
Scabies n Fertelized female burrows into epidermis to the level of stratum granulosum n Feed by ingesting intracellular fluids within epidermis n Male die shortly but the gravid female live for 4 -6 weeks n Can only live 2 -3 days away from a human host
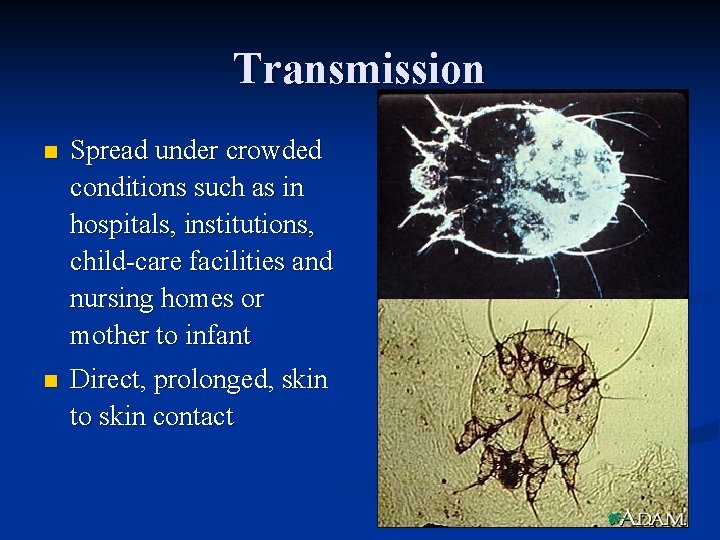
Transmission n Spread under crowded conditions such as in hospitals, institutions, child-care facilities and nursing homes or mother to infant n Direct, prolonged, skin to skin contact

Signs and symptoms of Scabies n n n Incubation period: 3 -4 weeks vs. 1 -4 days Pimple-like irritations, burrows or rash of the skin, especially the webbing of fingers, skin folds, penis, breast. Intense itching, esp. at night A background eczematous eruption may be present and is probably related to hypersensitivity. Few than one hundred mites in healthy host.
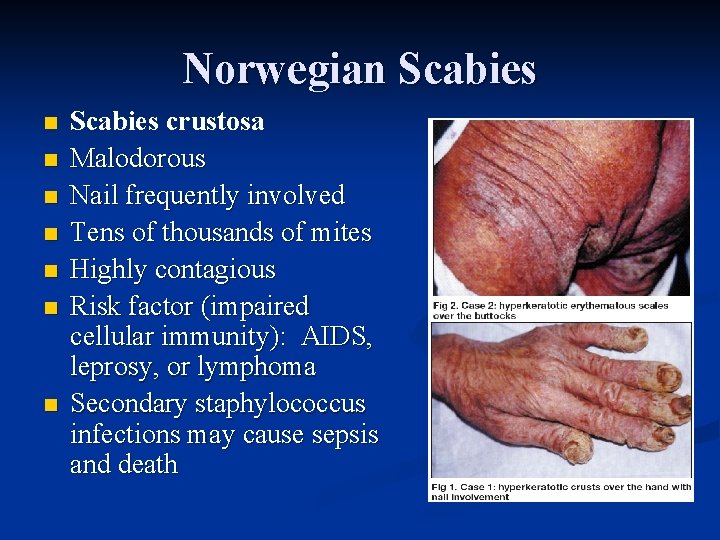
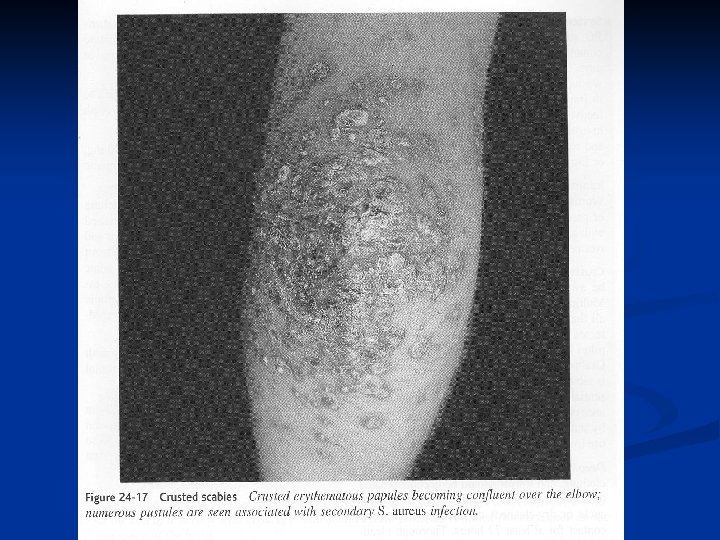
Norwegian Scabies n n n n Scabies crustosa Malodorous Nail frequently involved Tens of thousands of mites Highly contagious Risk factor (impaired cellular immunity): AIDS, leprosy, or lymphoma Secondary staphylococcus infections may cause sepsis and death
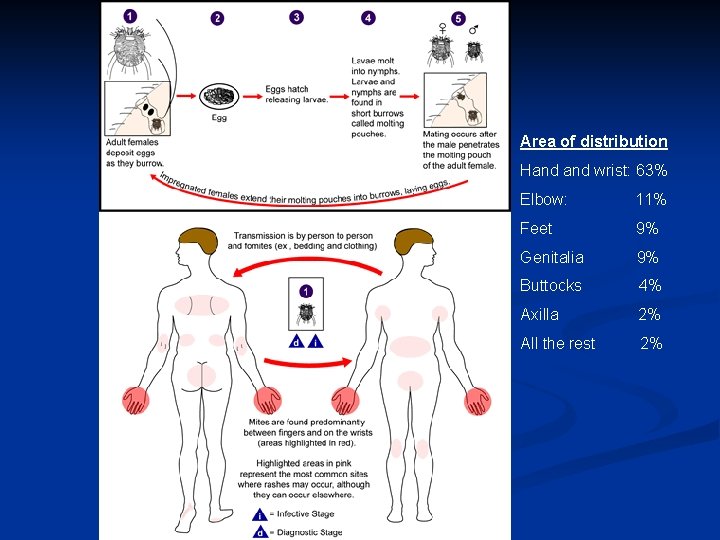
Area of distribution Hand wrist: 63% Elbow: 11% Feet 9% Genitalia 9% Buttocks 4% Axilla 2% All the rest 2%

Histopathology n Female mite may be identified within her tunnel in the stratum corneum. n Simply a lymphocytic perivascular infiltrate, often rich in eosinophils and often associated with an excoriation. n Nodular scabies show a deep and dense perivascular infiltrate of lymphocytes, plasma cells, eosinophils and atypical mononuclear cells.
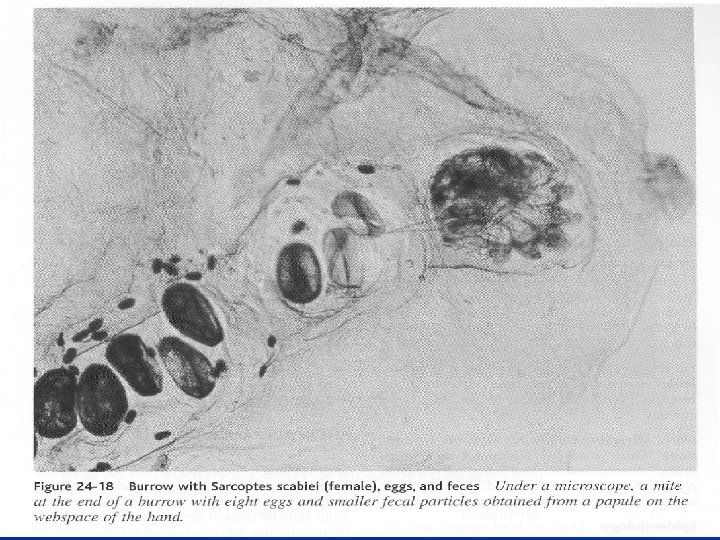
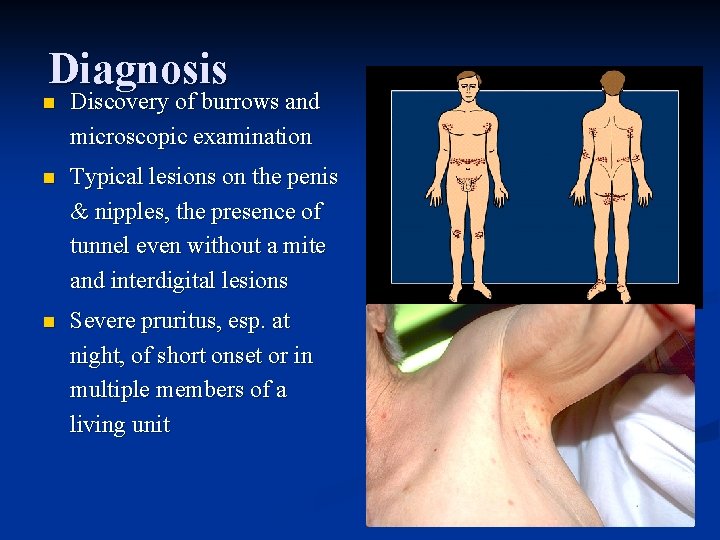
Diagnosis n Discovery of burrows and microscopic examination n Typical lesions on the penis & nipples, the presence of tunnel even without a mite and interdigital lesions n Severe pruritus, esp. at night, of short onset or in multiple members of a living unit

Scabies test n n n n Look for a nonexcoriated papule Place two to three drops of ink over the papules Wipe the area with an alcohol prep Place a drop of mineral oil on the skin Scrape the area or pinch the area and superficially shave the top layer of skin Place the specimen on a glass slide, apply coverslip and examine at 10 x magnification Female adult (0. 4 mm long), male (0. 2 mm long)

Clinical Picture
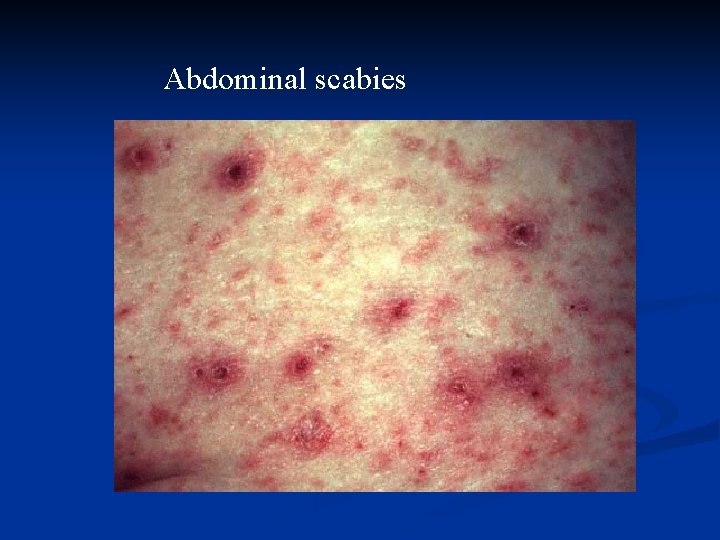
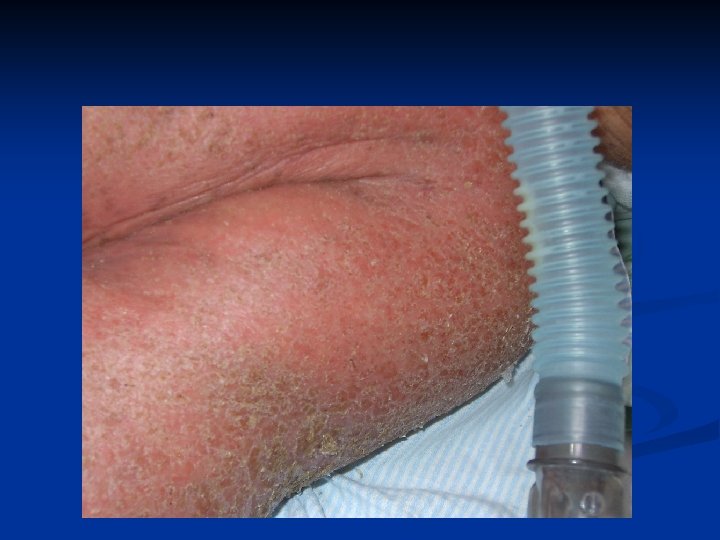
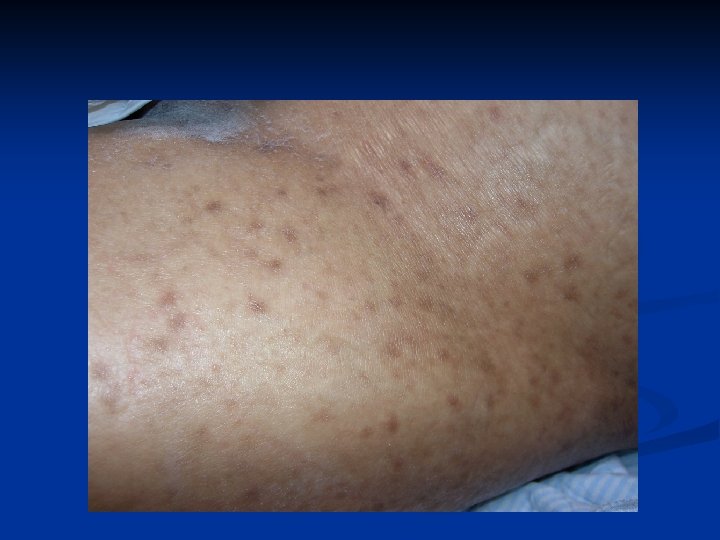
Abdominal scabies
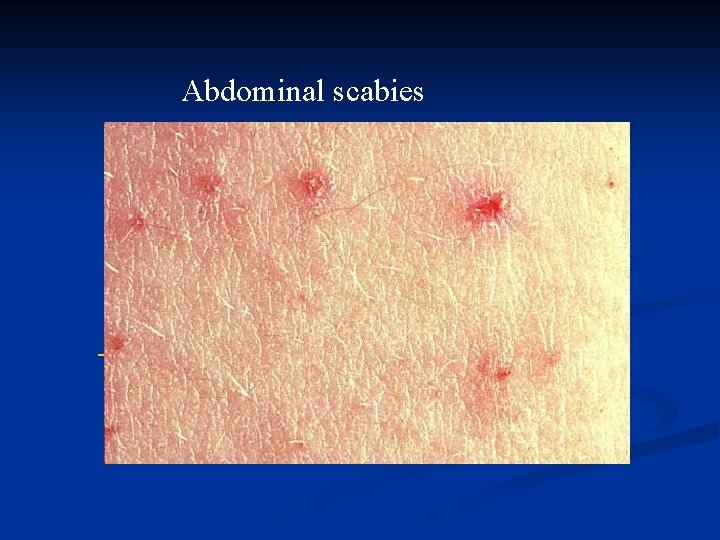
Abdominal scabies
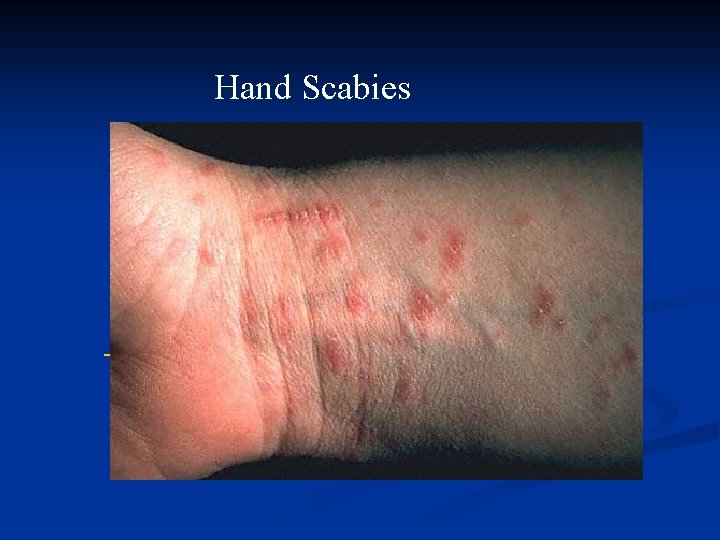
Hand Scabies
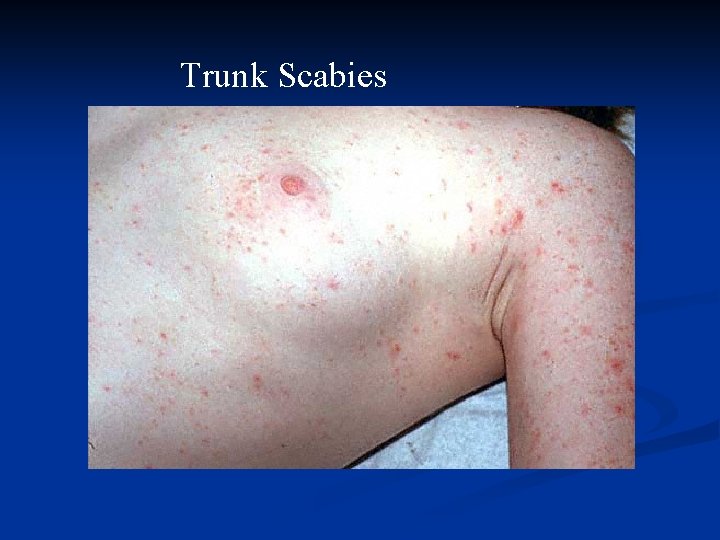
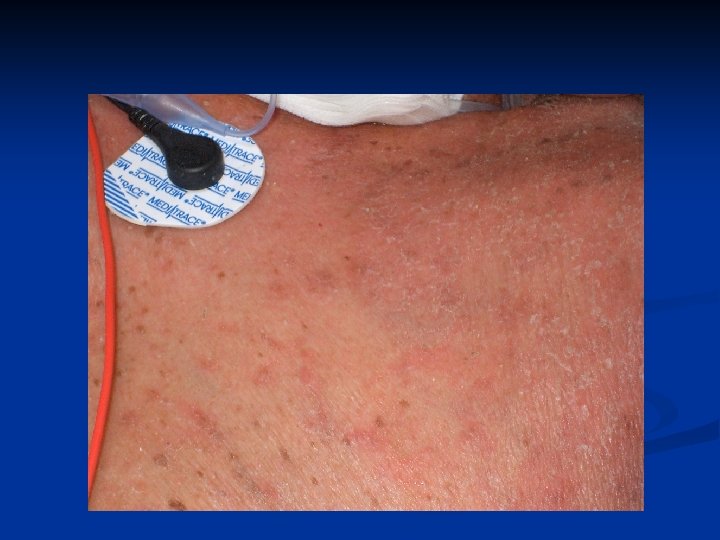
Trunk Scabies
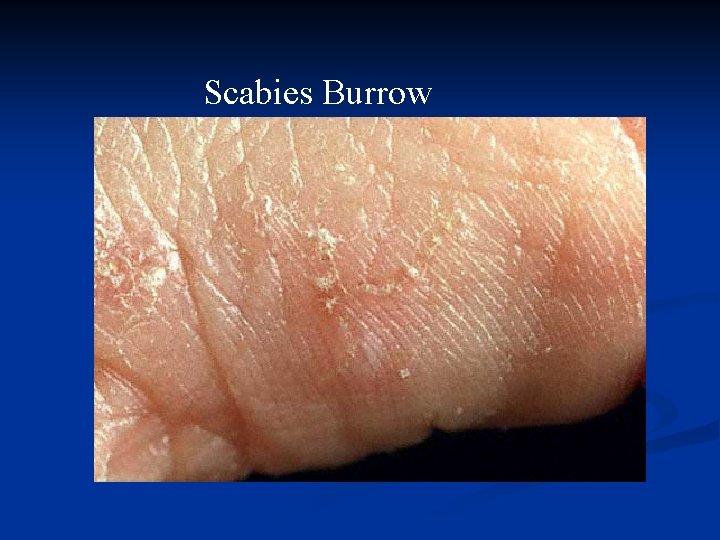
Scabies Burrow
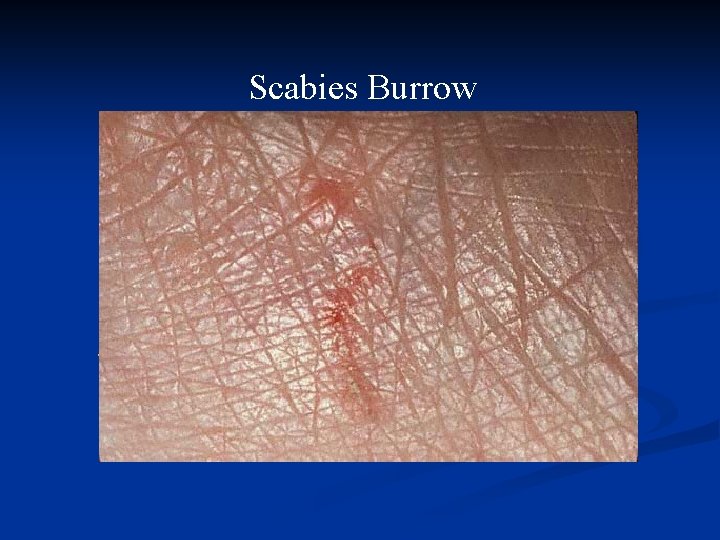
Scabies Burrow
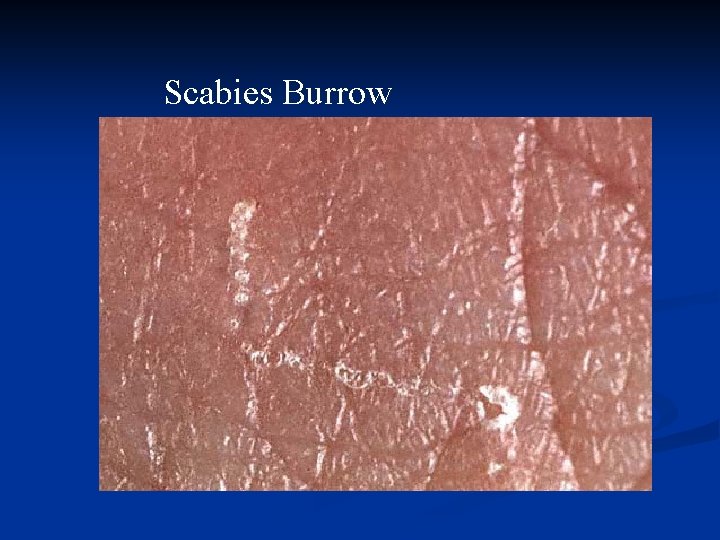
Scabies Burrow
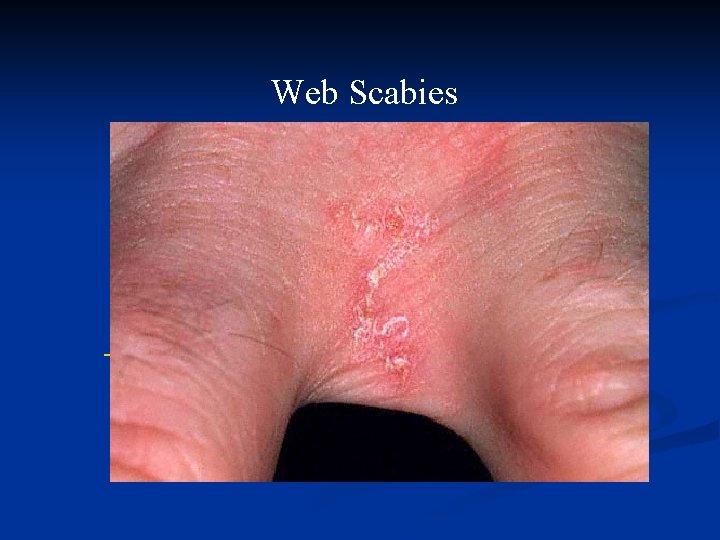
Web Scabies
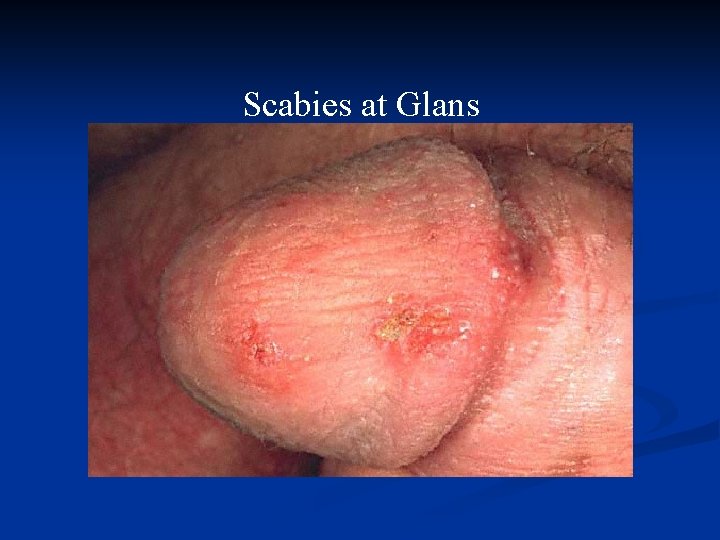
Scabies at Glans
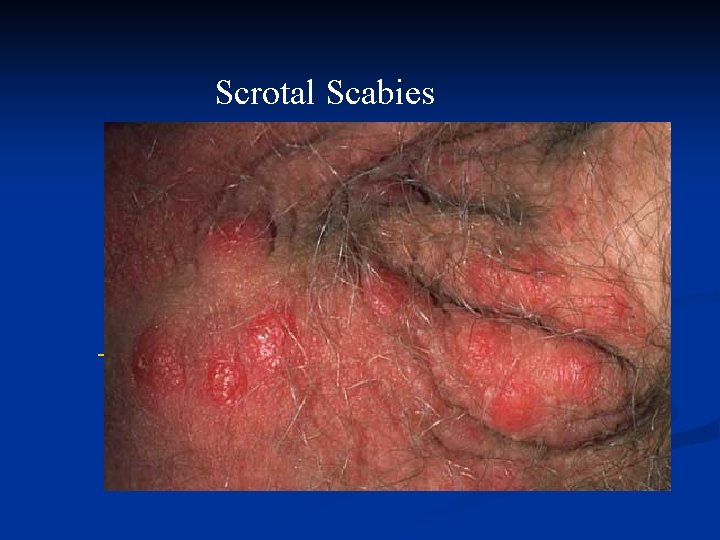
Scrotal Scabies
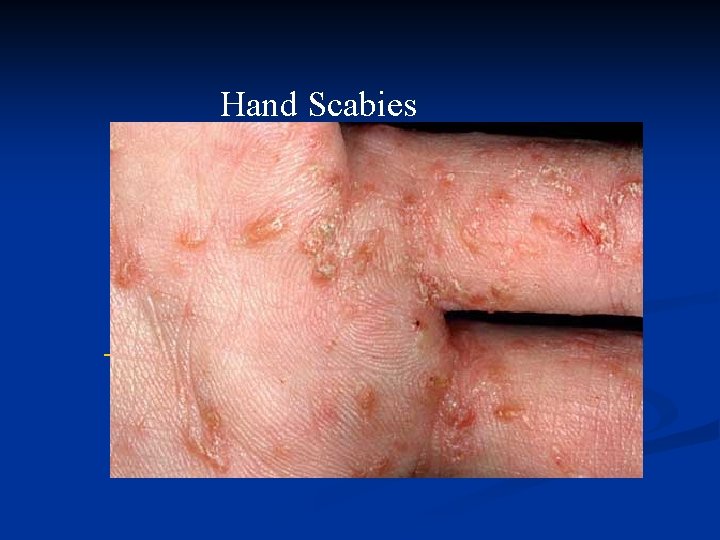
Hand Scabies

Treatment n 1% gamma benzene hexachloride (Lindane, Scabi cream), for 8 -12 hours; not for young children, pregnant women, nursing women due to neurological diseases and not shortly after a bath n Sulfur n Permethrin (5% dermal cream): for 8 -12 hours, more effective but more expensive n 25% Benzyl benzoate emulsion for 24 hours n Crotamiton (10%): less effective n Ivermectin in single dose (200 ug/kg); for crusted scabies: q 2 w x. II

Lindane (gamma benzyl hexachloride) n Mechanism of action/Effect: n n n A central nervous system (CNS) stimulant when absorbed systemically. stimulate the nervous system, resulting in convulsions and death. Dry the skin well before applying it. Apply enough lindane to cover the entire skin surface from the neck down, including the soles of your feet, and rub in well. Leave lindane on for 8 to 12 hours, then remove by washing thoroughly

Sulfur 6% in petrolatum Precipitated sulfur 6% in petrolatum n The oldest known treatment of scabies. n Safe and effective and the treatment of choice in infants <2 mo and pregnant or lactating women. n Sulfur is less acceptable to patients secondary to its odor and messy application. n Apply topically to entire trunk and extremities hs for 3 consecutive nights n

Permethrin n n n A neurotoxin that causes paralysis and death in ectoparasites. It is the most common treatment used today for scabies. Drug of choice (DOC), particularly for infants, young children, and pregnant or breastfeeding women. The lotion should be applied over the entire body, including the face and scalp in infants. Left on for 8 -12 hours and then rinsed. Reapplication one week later is advised; however, no controlled studies exist that show that 2 applications are better than one. No cases of scabies resistant to permethrin have been documented.

Benzyl benzoate (BB) n Action of mechanism: Unknown, may act on the nervous system of the parasite, resulting in its death Washing, rinsing, and drying skin well before using benzyl benzoate n Drying skin well if bath or shower is taken before use of benzyl benzoate n Cover entire skin surface from neck down, including soles of feet; rubbing in well Leaving benzyl benzoate on skin for 24 hours Removing BB by washing thoroughly with soap and warm water Rinsing thoroughly; drying with clean towel Washing hands immediately after using to remove any BB that may be on them Repeating treatment for severe infestation n n n

Crotamiton 10% (Eurax) Mechanism of action is unknown. n Associated with frequent treatment failures n Wash thoroughly and scrub away any loose scales, apply thin layer topically from neck to toes, gently massage into skin and leave on; a second application should be applied after 24 h; bathe 48 h after the last application n

Ivermectin n n Veterinary anthelmintic and formerly restricted in human medicine to tx onchoceriasis (nematodes) Interruption of gamma-aminobutyric acid-induced neurotransmission and invertebrates are selectively paralyzed by the drug. Half life: 16 hours Currently use in tx of cutaneous parasitosis such as cutaneous larva currens, cutaneous larva migrans and human ecotparasitosis, mainly head lice and scabies

Short-coming of permethrin and lindane in an institutional setting Understaffed n Difficulty in applying cream n Treatment-related dermatitis can be difficult to distinguish from persistent scabies n

Therapeutic Efficacy and safety of Ivermectin and Lindane in the Tx of Human Scabies Chouela EN et al. Arch Dermatol 1999; 135: 651 -5 Design: randomized, prospective, controlled, double-blind, double-dummy, and parallel clinical study. n Patients: outpatients, hospitalized patients, and thosed referred patients. n Intervention: Single oral dose of ivermectin (150 -200 ug/kg) or topical application of 1% lindane solution. Repeated 15 days later if clinically not cured n

Therapeutic Efficacy and safety of Ivermectin and Lindane in the Tx of Human Scabies n Results: Chouela EN et al. Arch Dermatol 1999; 135: 651 -5 43(19 vs. 24) /53 (81%) completed the study n At day 15, 14(74%) in ivermectin tx group were healed, 13(54%) in lindane tx group were healed. n At day 29, 18 (95%) in ivermectin tx group and 23(95%) in lindane tx group were healed n n Conclusion: Ivermectin is as effective as lindane for the tx of scabies

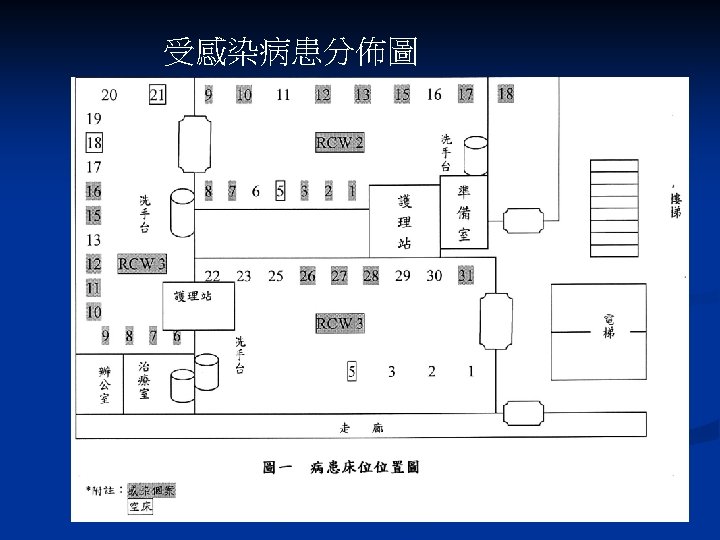
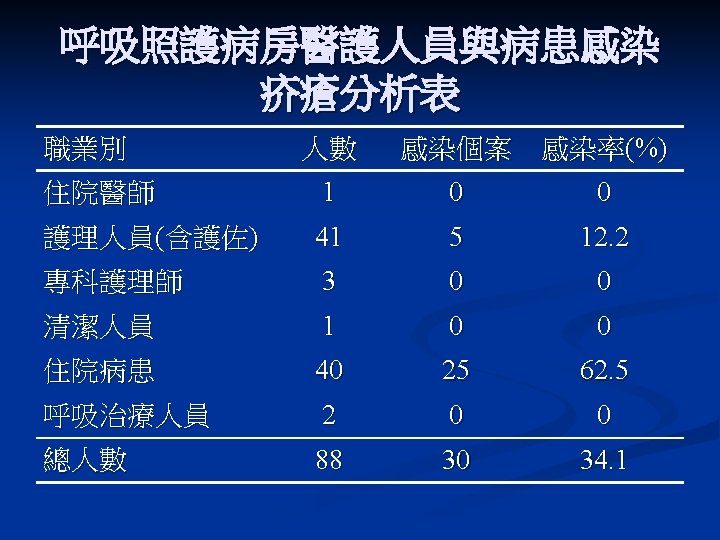
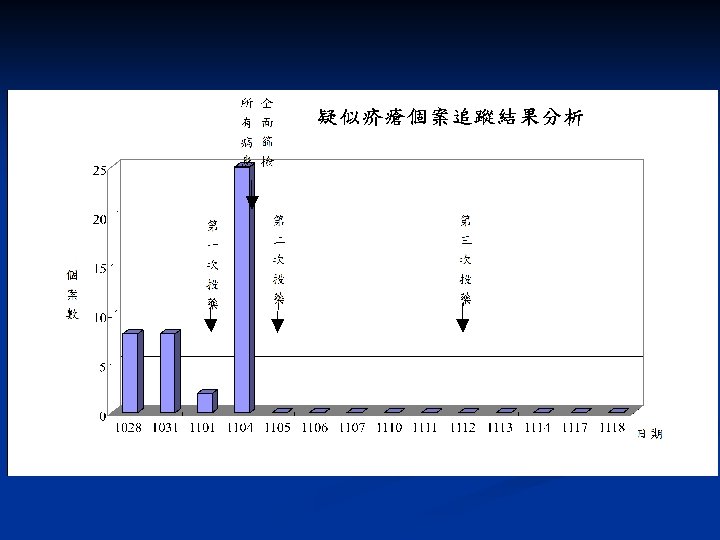
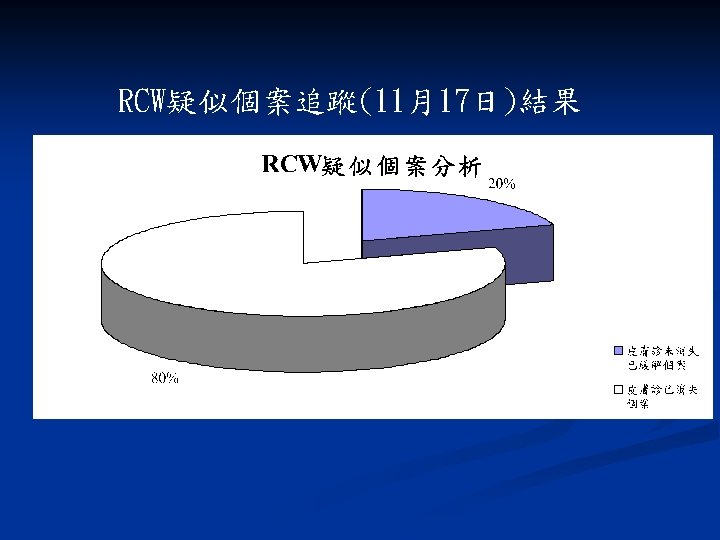
Nosocomial Scabies in an extended care Veterans Affairs Medical Center n Four nurse reported pruritic skin rash to IC officer n n Four nurse reported pruritic skin rash to IC officer Index case: 76 y/o with CLL, Norwegian scabies 112 persons were affected during 3 subsequent outbreak Control measures: n n n 1% lindane or 10% crotamiton use qw x II Contact isolation Contacts, including household member and staff member undergo similar treatment Launder clothing and bedding in hot water after scabicide application Active surveillance program for early detection Am J Infect Control 1995; 23: 44 -9

Eradication of Nosocomial Scabies Category Cases Exposed Attack rate (%) Control measures Outbreak Staff 1 (Feb ’ 91) Patients 42 160 26. 3 22 255 8. 6 Lindane (1%) or crotamiton (10%) t/u x 2; close to new admission; launder clothing and bedding in hot water scabicide application Outbreak Staff 2 (July ’ 91) Patients 10 67 14. 9 7 89 7. 9 Outbreak Staff 3 (Nov ’ 91) Patients 7 110 6. 4 8 163 4. 9 Rotation of nurses was suspended Investigation: Identify index case; Determine personnel contacts; Dx of scabies was made clinically by the presence of typical pruritic rash. Jimenez-Lucho et al. AJIC 1995; 23: 44 -9

Scabies in Chronic Health Care Institutions n n n Scabies in institution---Residents: 10/59; Staff: 16/34; Staff relative: 7/15 Control measures: All residents, residents’ family members who visited them and their families and staff members’ families were treated. Bath then 1% lindane from neck down for 12 hours then another bath and the linen and clothing was changed again All formites were changed prior to treatment 10% precipitated sulfur ointment was applied to Norwegian cases for two 24 -hour-applications 1 week apart. Arch Dermatol 1992; 128: 1257 -60
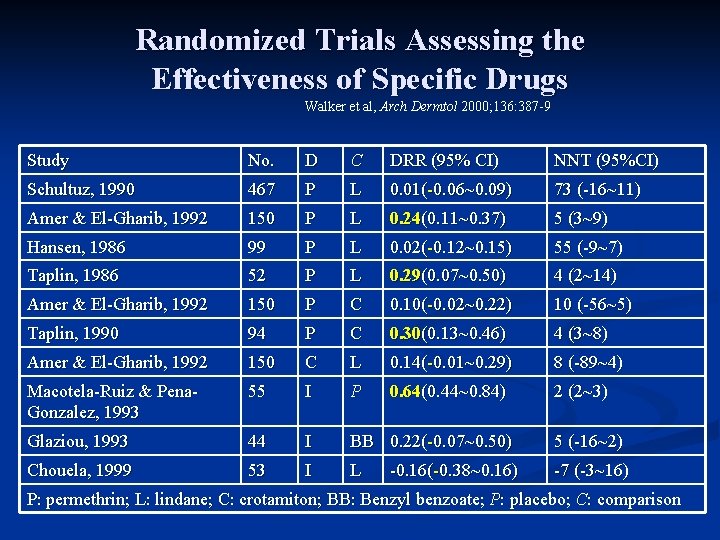
Randomized Trials Assessing the Effectiveness of Specific Drugs Walker et al, Arch Dermtol 2000; 136: 387 -9 Study No. D C DRR (95% CI) NNT (95%CI) Schultuz, 1990 467 P L 0. 01(-0. 06~0. 09) 73 (-16~11) Amer & El-Gharib, 1992 150 P L 0. 24(0. 11~0. 37) 5 (3~9) Hansen, 1986 99 P L 0. 02(-0. 12~0. 15) 55 (-9~7) Taplin, 1986 52 P L 0. 29(0. 07~0. 50) 4 (2~14) Amer & El-Gharib, 1992 150 P C 0. 10(-0. 02~0. 22) 10 (-56~5) Taplin, 1990 94 P C 0. 30(0. 13~0. 46) 4 (3~8) Amer & El-Gharib, 1992 150 C L 0. 14(-0. 01~0. 29) 8 (-89~4) Macotela-Ruiz & Pena. Gonzalez, 1993 55 I P 0. 64(0. 44~0. 84) 2 (2~3) Glaziou, 1993 44 I BB 0. 22(-0. 07~0. 50) 5 (-16~2) Chouela, 1999 53 I L -7 (-3~16) -0. 16(-0. 38~0. 16) P: permethrin; L: lindane; C: crotamiton; BB: Benzyl benzoate; P: placebo; C: comparison





Control Measure n n n Use medication as directed. Notify and treat all partners and household members. Abstain from intimate or sexual contact until treatment is completed successfully. Wash infested clothing and linen on the hot cycle setting. Dry on hot cycle for at least 20’. Infested articles that cannot be laundered may be drycleaned or placed in a bag for 2 weeks.




- Slides: 57