Sarcoidosis therapy Rob Vassallo MD Mayo Clinic Rochester

Sarcoidosis therapy Rob Vassallo, MD Mayo Clinic, Rochester, MN. Pneumotrieste 2014 April 7 -9, 2014. © 2013 MFMER | slide-1

Disclosures • I have no financial disclosures relevant to this presentation. © 2013 MFMER | slide-2
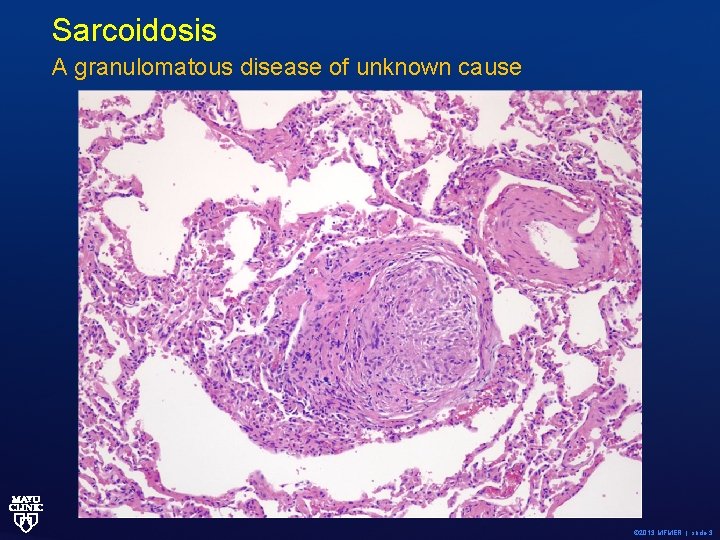
Sarcoidosis A granulomatous disease of unknown cause © 2013 MFMER | slide-3

Is it sarcoidosis? Not all granulomas = sarcoidosis • Must rule out infection including mycobacterial or fungal. • If there is a prior history of recurrent infections (bronchitis, pneumonia, sinusitis etc) must think of common variable immune deficiency (rule out with Ig. G, Ig. A and Ig. M determination). • Consider other causes of granulomatous diseases (example Crohn’s disease). © 2013 MFMER | slide-4
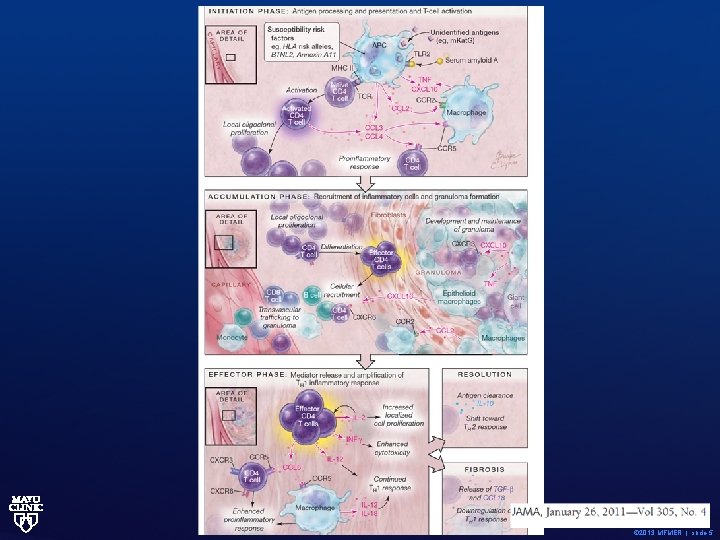
© 2013 MFMER | slide-5

Pharmacologic therapy for Sarcoidosis Structure of today’s presentation • 1. First option of management is observation. • 2. Mainstay of pharmacologic therapy are corticosteroids • 3. Many so-called second line agents: • Methotrexate • Azathioprine • Hydroxychloroquine • Pentoxifylline • 4. Other agents: ? 3 rd line or for use in selected or difficult situations including TNF inhibitors, cyclophosphamide, cyclosporine etc. • 5. Discuss difficult situations at end. © 2013 MFMER | slide-6

Treatment of acute sarcoidosis Observation vs NSAID vs brief Corticosteroid therapy © 2013 MFMER | slide-7

Treatment of acute sarcoidosis § Observation alone is sufficient in many cases. § NSAIDs for arthritic symptoms. § Prednisone 0. 5 -1 mg/kg/day once daily or every other day in some instances: § Hypercalcemia § Marked arthritic symptoms § Acute neurologic involvement (Facial nerve) § If treat with steroids, plan for rapid taper and close follow-up. Löfgren S. Acta Med Scand 1953 145 (6): 424– 431. © 2013 MFMER | slide-8

Treatment of chronic sarcoidosis Chronic sarcoidosis = >24 months duration DG James Q J Med 1983; 208: 525– 33. © 2013 MFMER | slide-9

Sarcoidosis Indications for therapy (topical or systemic) General principles § 1. Hypercalcemia § 2. Organ involvement with the potential of impaired organ function if left untreated – example: § Pulmonary parenchymal involvement § Ocular involvement § Cardiac disease (conduction disease or myocardial) § Neurologic (central or peripheral) § Cutaneous disease. § Muscle, liver etc. © 2013 MFMER | slide-10

Do all patients with pulmonary sarcoidosis require treatment? Simple answer: NO! 63 -year old with biopsy proven sarcoid Asymptomatic © 2013 MFMER | slide-11
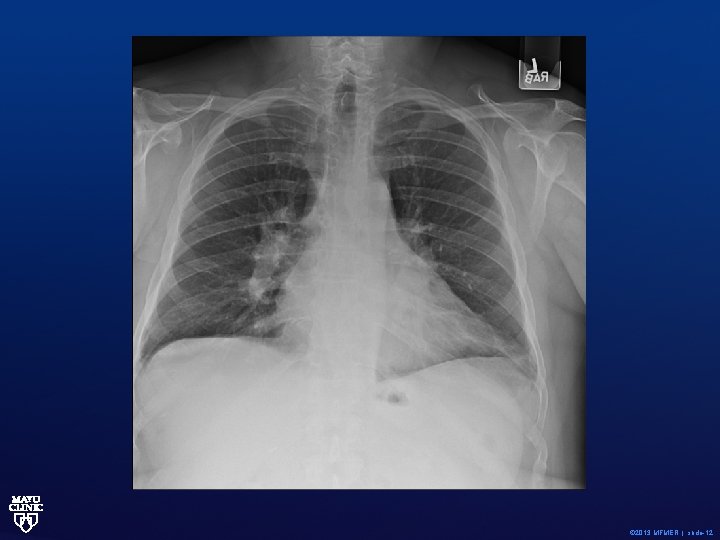
© 2013 MFMER | slide-12

Cardiopulmonary exercise test • The patient exercised for ten minutes and achieved a peak workload of 200 watts. This was a maximal study with oxygen consumption at 80% of the predicted max. • The cardiac response to activity was normal. The HR increased appropriately with activity. The blood pressure response appeared appropriate. The cardiac output increased from 4. 7 L/min at rest to 12. 1 L/min at mid activity. • The ventilatory response to exercise was normal increasing to a peak of 80% of maximal predicted. Oxygen saturation was maintained throughout. No evidence of ventilatory limitation noted. © 2013 MFMER | slide-13

Recommendation • Continue to stay active. • Age appropriate vaccination. • Follow up in 1 year with PFT and chest X ray – sooner if new symptoms develop. © 2013 MFMER | slide-14

Role of inhaled or topical steroids • Relatively limited role, generally for management of mild disease (airway of mild ocular involvement). • Consider trial of inhaled corticosteroid in patients with airway involvement (mild). © 2013 MFMER | slide-15

Corticosteroids in sarcoidosis Often work really well at controlling disease activity, but. . . § 1. Intolerable glucocorticoid side effects. § 2. Progression of disease despite adequate glucocorticoid therapy (0. 5 mg/kg/day). § 3. Need for a glucocorticoid-sparing agent in a patient who requires long-term glucocorticoid therapy and is concerned re long-term side effects. § 4. Patient refusal to take glucocorticoids. © 2013 MFMER | slide-16

Sarcoidosis Therapy Intolerance to corticosteroids – Methotrexate as a secondline agent © 2013 MFMER | slide-17

Methotrexate for sarcoidosis What’s the evidence? • Methotrexate is an immunosuppressive and anti -inflammatory agent. • Can be administered orally or intramuscularly. • The initial dosage = 7. 5 mg once per week, with progressive increases until reaching 10 -20 mg per week. • Folic acid must also be administered, and CBC and liver function must be periodically checked. 1. 2. Curr Opin Pulm Med 2013, 19: 545– 561 Thorax, 1999; 54: 742 -6. © 2013 MFMER | slide-18
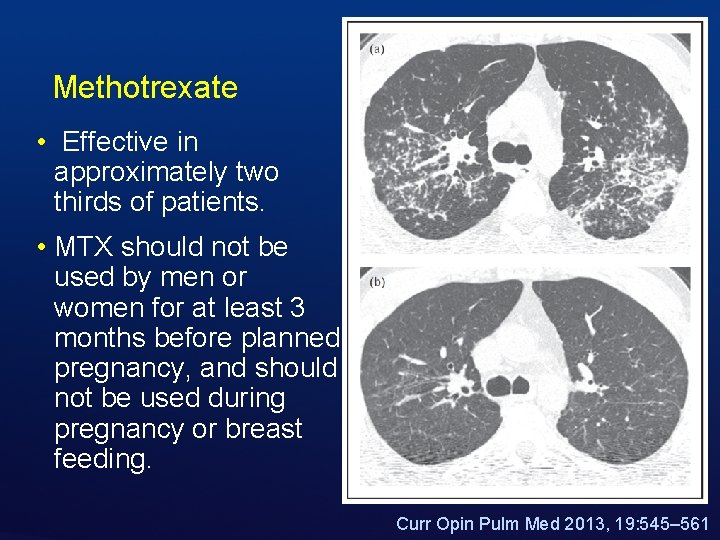
Methotrexate • Effective in approximately two thirds of patients. • MTX should not be used by men or women for at least 3 months before planned pregnancy, and should not be used during pregnancy or breast feeding. Curr Opin Pulm Med 2013, 19: 545– 561

Methotrexate Toxicity concerns and monitoring • 1. Lung toxicity – hypersensitivity • 2. Liver toxicity – much more significant concern. See recent review. Would stop after every 1 gram total of methotrexate therapy and assess need to continue. • 3. Bone marrow toxicity – uncommon with folic acid supplementation. • 4. Teratogenicity © 2013 MFMER | slide-20

Sarcoidosis Therapy Clinical Case: Intolerance to corticosteroids – Azathioprine © 2013 MFMER | slide-21

Clinical Case • 41 -year-old nonsmoker with a solitary kidney who has a diagnosis of histopathologically proven non-necrotizing granulomatous inflammation affecting the skull, the spine and lungs. • The patient has been successfully treated with oral corticosteroid therapy and has developed many side effects. • She is intolerant of steroids. © 2013 MFMER | slide-22
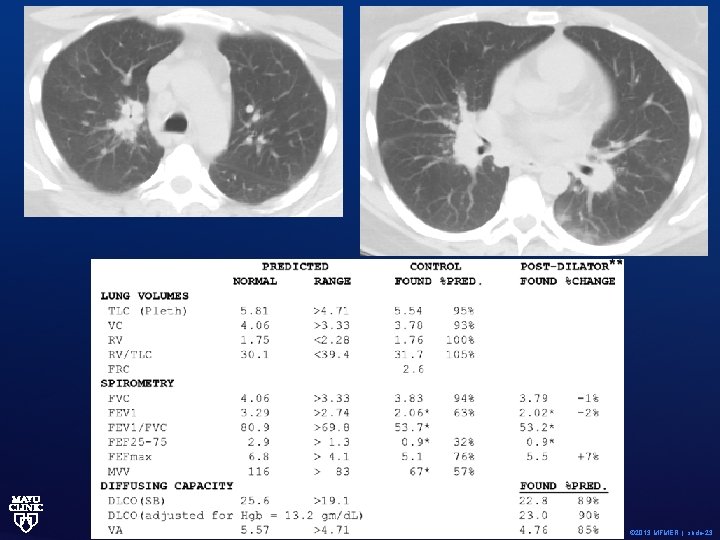
© 2013 MFMER | slide-23
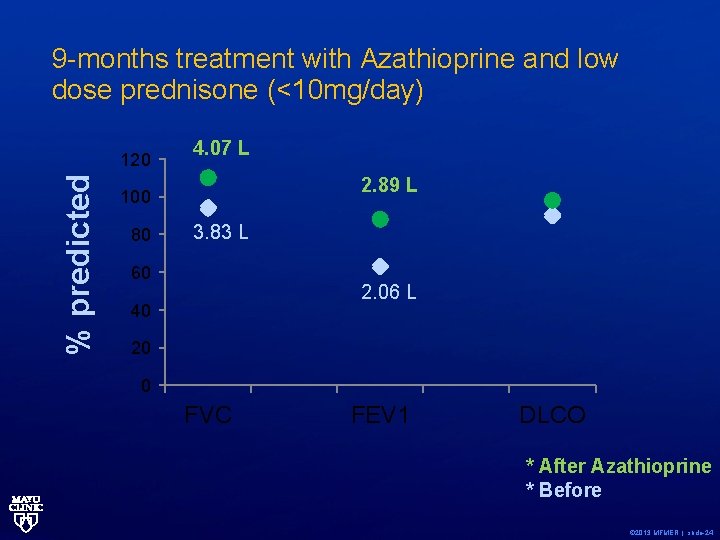
9 -months treatment with Azathioprine and low dose prednisone (<10 mg/day) % predicted 120 4. 07 L 2. 89 L 100 80 3. 83 L 60 2. 06 L 40 20 0 FVC FEV 1 DLCO * After Azathioprine * Before © 2013 MFMER | slide-24

Azathioprine • No randomized studies – case reports and case series. • Consider in patients intolerant of methotrexate or unable to take methotrexate due to contraindications. • Limited data suggests similar efficacy profile as methotrexate. © 2013 MFMER | slide-25

© 2013 MFMER | slide-26

Azathioprine Toxicity concerns • Liver toxicity • Bone marrow toxicity • Check TPMT (thiopurine methyl transferase enzyme) level before starting. • Infection risk. • Pneumocystis prophylaxis. © 2013 MFMER | slide-27

Sarcoidosis therapy “Special situations” Treatment of Neurologic Sarcoidosis © 2013 MFMER | slide-28

Neurologic involvement: Clinical Case • 44 -year-old lady with progressive imbalance and unsteadiness, episodic vomiting, and weight loss. • The neurologic examination showed ataxia of gait, without limb ataxia or extraocular movement abnormalities or nystagmus. • Spinal fluid exam showed elevated protein, low glucose; total nucleated cell count was 92 /μl with predominantly lymphocytes. There was positive oligoclonal banding. © 2013 MFMER | slide-29

Case • Conjunctiva, right, biopsy: Non-necrotizing granulomatous inflammation. • Brain, right frontal, biopsy: Non-necrotizing granulomatous inflammation with giant cells extensively involving the leptomeninges. GMS stain for fungi and auramine-rhodamine stain for mycobacteria were negative. © 2013 MFMER | slide-30

Neurosarcoidosis Principles of Treatment • Always establish the diagnosis by tissue before beginning treatment • Corticosteroids are the cornerstone for treatment • Plan for a minimum of six months of therapy • Steroid-sparing agents have less experience based success then corticosteroids. • MRI GAD enhancing lesions take months to improve on successful treatment © 2013 MFMER | slide-31

Neurosarcoidosis Treatment • TNF- blockers • inflixamib (Remicade) • 5 mg/kg IV at initiation, 2 weeks, 4 weeks, then q 4 weeks IV • continue 3 -6 months depending on response • follow a target parameter at 3 months © 2013 MFMER | slide-32

TNF-alpha inhibitors in sarcoidosis • In the selected review, 232 patients (89. 9%) were treated with Infliximab and 26 (10. 0%) were treated with Etanercept. • In 2 RCTs, favorable response of the lung disease was reported with Infliximab. • In the cases series, results were diverse. Maneiro et al. Semin Arthritis Rheum. 2012 Aug; 42(1): 89 -103. © 2013 MFMER | slide-33

TNF-alpha inhibitor therapy in sarcoidosis • Mean weighted rates of events per 100 patient years • Adverse events: 39. 9 • Infections: 22. 1 • Serious infections: 5. 9 • Malignancy: 1. 0 • At this point in time, there is insufficient evidence to routinely support the use of TNFalpha inhibitor therapy, except in selected cases. © 2013 MFMER | slide-34

Sarcoidosis Therapy Hypercalcemia © 2013 MFMER | slide-35

Treatment of Hypercalcemia in Sarcoidosis • Adequate hydration • Avoidance of exposure to sunlight, calcium/Vitamin D supplementation, adherence to low calcium diet • Prednisone 40 mg/day for 1 week, reduction to 20 mg/day within 1 -2 weeks, maintenance of 10 mg/day or every other day with attempts to discontinue prednisone if chronic renal dysfunction is not present. • Hydroxychloroquine in steroid resistant or steroid intolerant patients. © 2013 MFMER | slide-36

Sarcoidosis therapy Clinical Case: Severe constitutional symptoms with Stage I pulmonary sarcoid. © 2013 MFMER | slide-37

Clinical Case. • 59 -year-old non-smoker complained of low grade fevers x 7 days, joint aches, and mild shortness of breath. • Otherwise feels fine. • Physical exam if totally unremarkable. Eyes normal. Joints normal. Lung exam is normal. No skin findings. • Normal lung function on PFTs. • Calcium level normal. © 2013 MFMER | slide-38
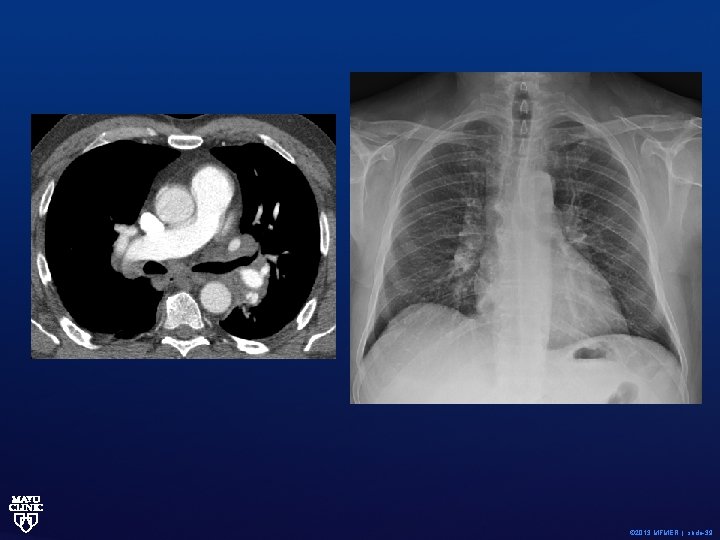
© 2013 MFMER | slide-39

Fatigue in sarcoidosis: clinical case • 51 yr-old non-smoker. Well until 8 weeks prior to presentation: felt fatigue, discomfort in the hips and subjective fever. About 2 weeks prior to referral, he developed fevers [102 to 104 range] and dry cough. • Main symptoms include fatigue and lethargy, anorexia and weight loss of about twenty to thirty pounds. • Physical examination was normal © 2013 MFMER | slide-40
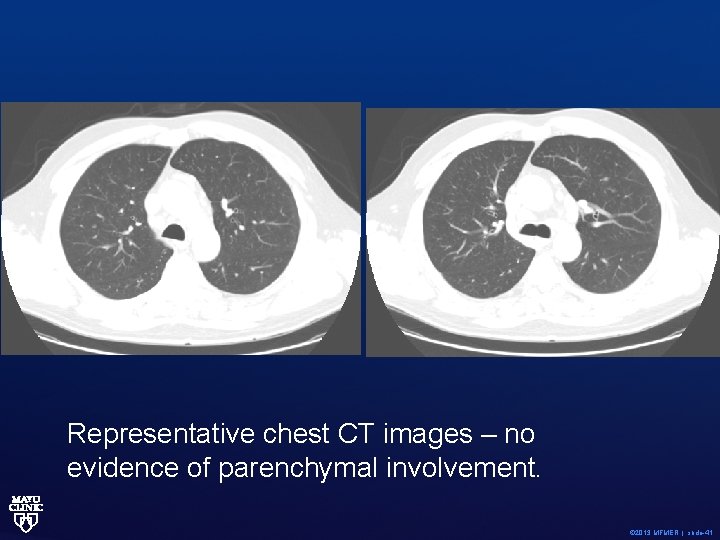
Representative chest CT images – no evidence of parenchymal involvement. © 2013 MFMER | slide-41
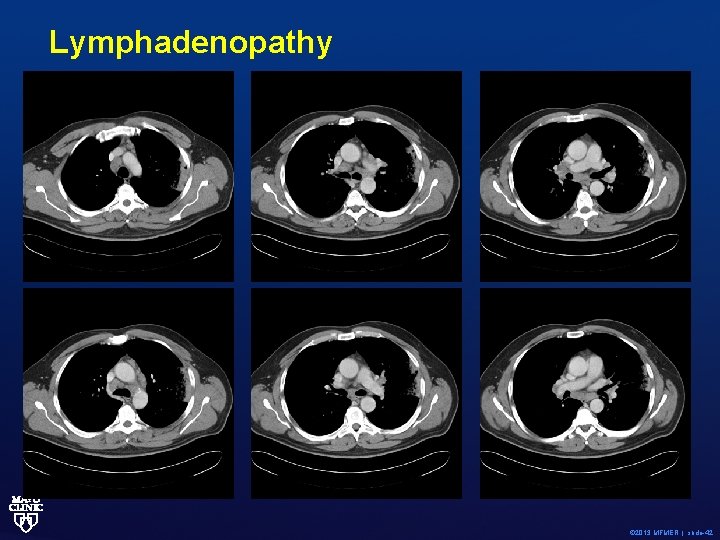
Lymphadenopathy © 2013 MFMER | slide-42
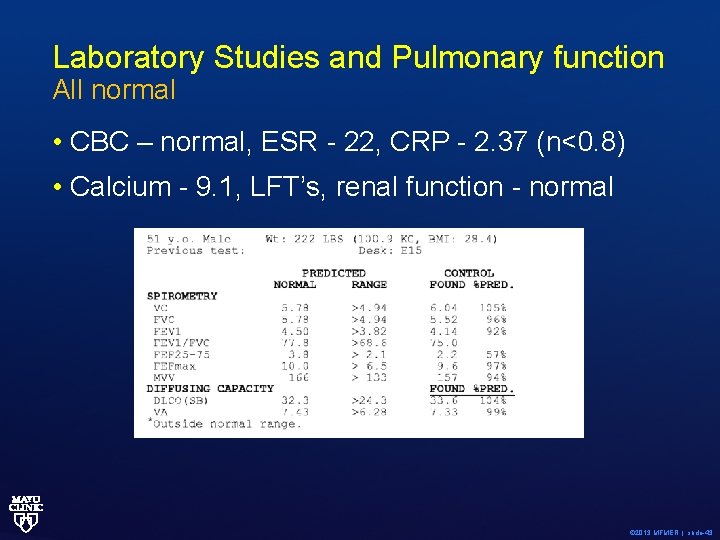

Laboratory Studies and Pulmonary function All normal • CBC – normal, ESR - 22, CRP - 2. 37 (n<0. 8) • Calcium - 9. 1, LFT’s, renal function - normal © 2013 MFMER | slide-43

Surgical Pathology • Left supraclavicular lymph node (1. 3 x 0. 8 x 0. 4 cm) Epithelioid granulomas © 2013 MFMER | slide-44

How would you manage? • 1. Patient has normal lung function and Stage 1 pulmonary sarcoidosis. • 2. Absence of hypercalcemia, ocular involvement, cardiac, neurologic, cutaneous or hepatic involvement. • 3. Although organ function is normal, he is debilitated by fatigue. • Observe or treat? What would you treat with? © 2013 MFMER | slide-45

Fatigue in Sarcoidosis • Common complaint for patients with sarcoid: incidence reported 30 -70%. • Cause is unclear, ? role for TNF- , IL-1 b, IL-6. • Not always related to disease extent (pts. with Stage 1 disease may have more fatigue than patients with more advanced disease). • May last for a significant period of time (>6 months) one report quotes 5% of patients with sarcoid develop a “post-sarcoidosis chronic fatigue syndrome”. © 2013 MFMER | slide-46

• A cross-sectional study performed in 38 sarcoidosis patients. • Patients with fatigue (n=25) suffered more frequently from other symptoms, compared to those without fatigue (n=13). • No relationship was found between fatigue and ACE or lung function impairment. • Patients with fatigue had higher levels of CRP and REE compared to those without fatigue. © 2013 MFMER | slide-47

Management • First need to make sure nothing else is going on – rule out other medical conditions like thyroid disease, sleep disorders, adrenal insufficiency, depression, occult malignancy etc. • No good data on drugs! • Low dose prednisone, hydroxychloroquine, and tricylic antidepressants have all been suggested as useful for management. • My patient – treated with low dose prednisone for 6 months. © 2013 MFMER | slide-48

Other general principles • Pneumocystis prophylaxis • Prophylactic vaccinations • Age appropriate cancer screening • TB screening • Osteoporosis prophylaxis • Counselling regarding effect on pregnancy • Thiopurine methyl transferase (TPMT) level © 2013 MFMER | slide-49

• Grazie © 2013 MFMER | slide-50
- Slides: 50