SAPIEN 3 Outcomes In Bicuspid vs Tricuspid Aortic

SAPIEN 3 Outcomes In Bicuspid vs. Tricuspid Aortic Valve Stenosis: A Propensity Matched Analysis from US TVT Registry Raj Makkar M. D. Director, Interventional Cardiology and Cardiac Cath Cardiac Lab Cedars-Sinai Medical Center, Los Angeles, CA

Disclosures • Research grants, Consultant and Proctor for Edwards, Abbott, Medtronic and Claret Medical 2

Collaborators • • • 3 Sun-Han Yoon, MD Michael Rinaldi, MD Eric Skipper, MD Pinak Shah, MD Gilbert Tang, MD Tsuyoshi Kaneko, MD Cedars-Sinai Medical Center, Los Angeles, CA Carolinas Health Care, Charlotte, NC Carolinas Heath Care, Charlotte, NC Brigham and Women’s Hospital, Boston, MA Mount Sinai Health System, New York, NY Brigham and Women’s Hospital, Boston, MA
Background & Objective • As TAVR becomes a therapeutic option for younger and healthier patients, bicuspid aortic valves will be seen more often. • Outcomes in patients with bicuspid valves with early generation THVs were suboptimal. • Pivotal clinical trials evaluating the SAPIEN 3 transcatheter valve have excluded patients with bicuspid aortic valves. Therefore, limited clinical data has been reported in this subset of patients. • We sought to compare the outcomes of TAVR with SAPIEN 3 in patients with native bicuspid with those with tricuspid aortic valves in the real-world STS/ACC TVT Registry. 1 Yoon 4 et al. TAVR with early and new generation devices in bicuspid aortic valve stenosis. JACC 2016; 68: 1195 -1205
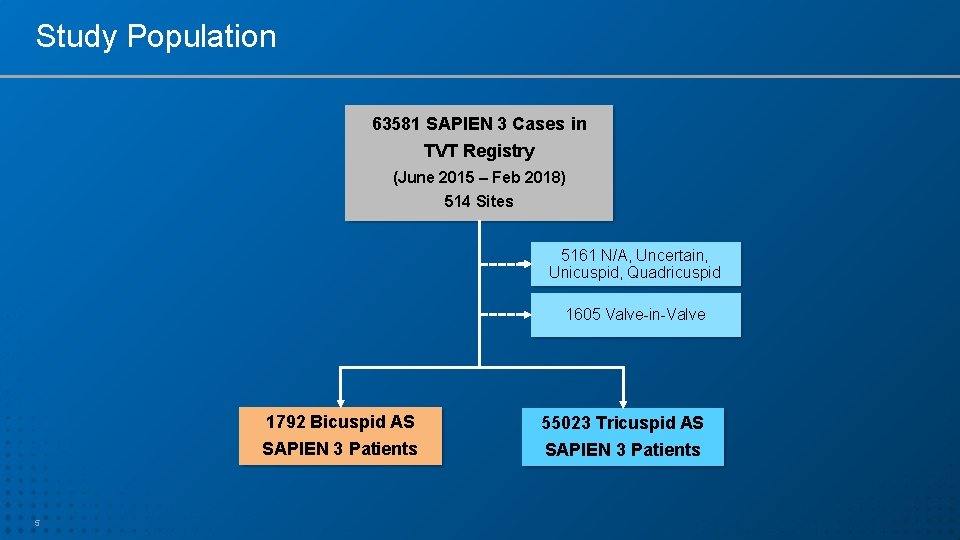
Study Population 63581 SAPIEN 3 Cases in TVT Registry (June 2015 – Feb 2018) 514 Sites 5161 N/A, Uncertain, Unicuspid, Quadricuspid 1605 Valve-in-Valve 5 1792 Bicuspid AS 55023 Tricuspid AS SAPIEN 3 Patients
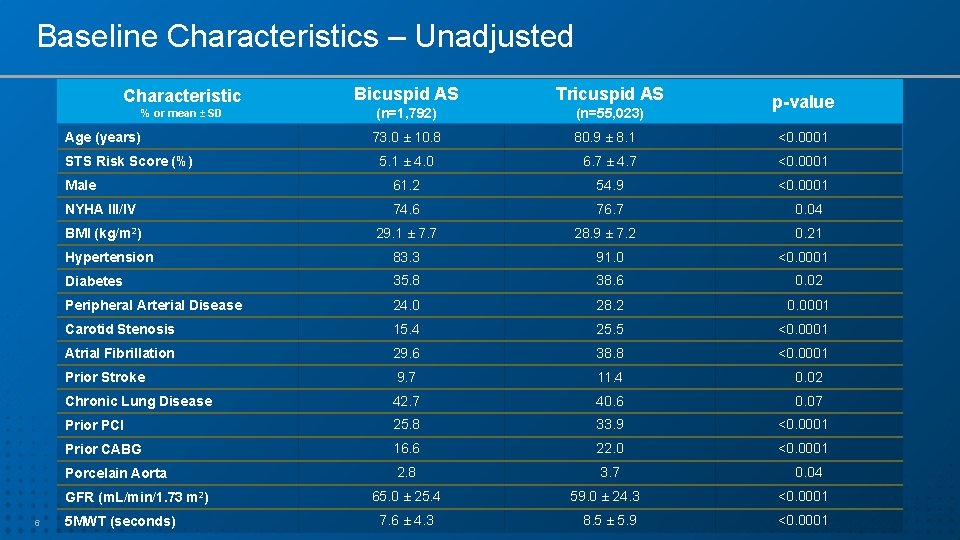
Baseline Characteristics – Unadjusted Characteristic % or mean ± SD Age (years) Tricuspid AS (n=1, 792) (n=55, 023) 73. 0 ± 10. 8 p-value 80. 9 ± 8. 1 <0. 0001 5. 1 ± 4. 0 6. 7 ± 4. 7 <0. 0001 Male 61. 2 54. 9 <0. 0001 NYHA III/IV 74. 6 76. 7 BMI (kg/m 2) 29. 1 ± 7. 7 STS Risk Score (%) 28. 9 ± 7. 2 0. 04 0. 21 Hypertension 83. 3 91. 0 Diabetes 35. 8 38. 6 0. 02 Peripheral Arterial Disease 24. 0 28. 2 0. 0001 Carotid Stenosis 15. 4 25. 5 <0. 0001 Atrial Fibrillation 29. 6 38. 8 <0. 0001 Prior Stroke 9. 7 11. 4 0. 02 Chronic Lung Disease 42. 7 40. 6 0. 07 Prior PCI 25. 8 33. 9 <0. 0001 Prior CABG 16. 6 22. 0 <0. 0001 Porcelain Aorta 2. 8 3. 7 GFR (m. L/min/1. 73 m 2) 6 Bicuspid AS 5 MWT (seconds) 65. 0 ± 25. 4 7. 6 ± 4. 3 <0. 0001 0. 04 59. 0 ± 24. 3 <0. 0001 8. 5 ± 5. 9 <0. 0001
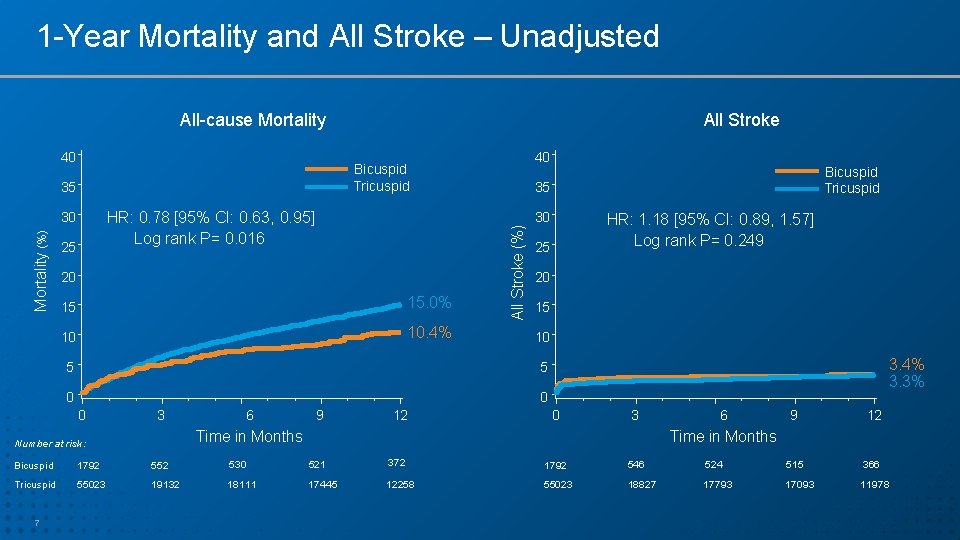
1 -Year Mortality and All Stroke – Unadjusted All-cause Mortality 40 40 Bicuspid Tricuspid HR: 0. 78 [95% CI: 0. 63, 0. 95] Log rank P= 0. 016 30 25 20 15 15. 0% 10 10. 4% 30 20 15 10 5 0 0 3 6 9 12 HR: 1. 18 [95% CI: 0. 89, 1. 57] Log rank P= 0. 249 25 5 0 Bicuspid Tricuspid 35 All Stroke (%) 35 Mortality (%) All Stroke 3. 4% 3. 3% 0 3 Time in Months Number at risk: 6 9 12 Time in Months Bicuspid 1792 552 530 521 372 1792 546 524 515 366 Tricuspid 55023 19132 18111 17445 12258 55023 18827 17793 17093 11978 7
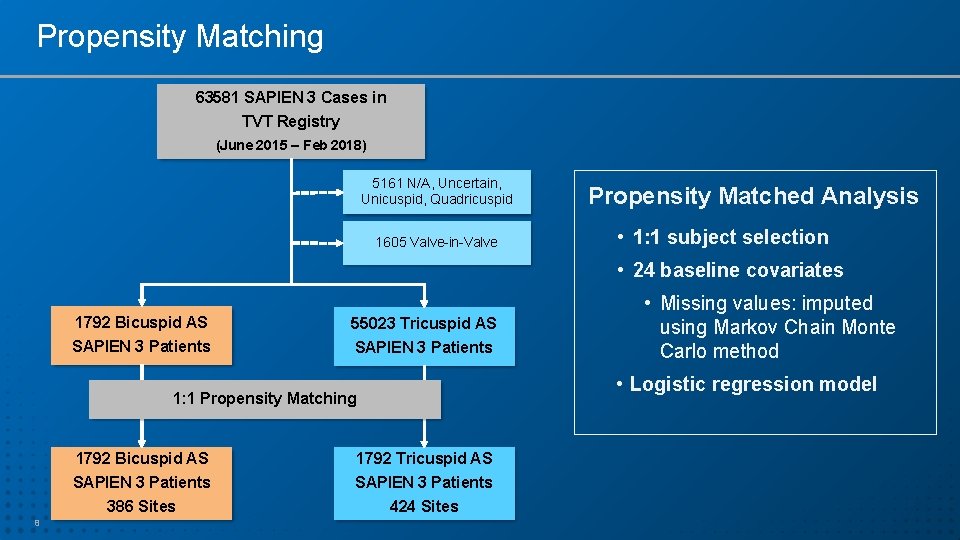
Propensity Matching 63581 SAPIEN 3 Cases in TVT Registry (June 2015 – Feb 2018) 5161 N/A, Uncertain, Unicuspid, Quadricuspid 1605 Valve-in-Valve Propensity Matched Analysis • 1: 1 subject selection • 24 baseline covariates 1792 Bicuspid AS SAPIEN 3 Patients 55023 Tricuspid AS SAPIEN 3 Patients • Logistic regression model 1: 1 Propensity Matching 8 • Missing values: imputed using Markov Chain Monte Carlo method 1792 Bicuspid AS SAPIEN 3 Patients 1792 Tricuspid AS SAPIEN 3 Patients 386 Sites 424 Sites
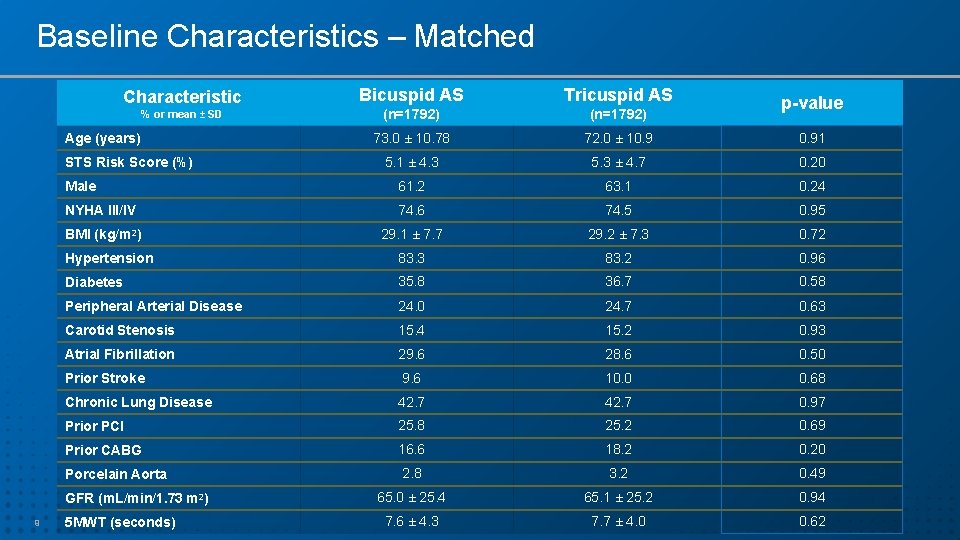
Baseline Characteristics – Matched Bicuspid AS Tricuspid AS (n=1792) 73. 0 ± 10. 78 72. 0 ± 10. 91 5. 1 ± 4. 3 5. 3 ± 4. 7 0. 20 Male 61. 2 63. 1 0. 24 NYHA III/IV 74. 6 74. 5 0. 95 BMI (kg/m 2) 29. 1 ± 7. 7 29. 2 ± 7. 3 0. 72 Hypertension 83. 3 83. 2 0. 96 Diabetes 35. 8 36. 7 0. 58 Peripheral Arterial Disease 24. 0 24. 7 0. 63 Carotid Stenosis 15. 4 15. 2 0. 93 Atrial Fibrillation 29. 6 28. 6 0. 50 Prior Stroke 9. 6 10. 0 0. 68 Chronic Lung Disease 42. 7 0. 97 Prior PCI 25. 8 25. 2 0. 69 Prior CABG 16. 6 18. 2 0. 20 Porcelain Aorta 2. 8 3. 2 0. 49 65. 0 ± 25. 4 65. 1 ± 25. 2 0. 94 7. 6 ± 4. 3 7. 7 ± 4. 0 0. 62 Characteristic % or mean ± SD Age (years) STS Risk Score (%) GFR (m. L/min/1. 73 m 2) 9 5 MWT (seconds) p-value
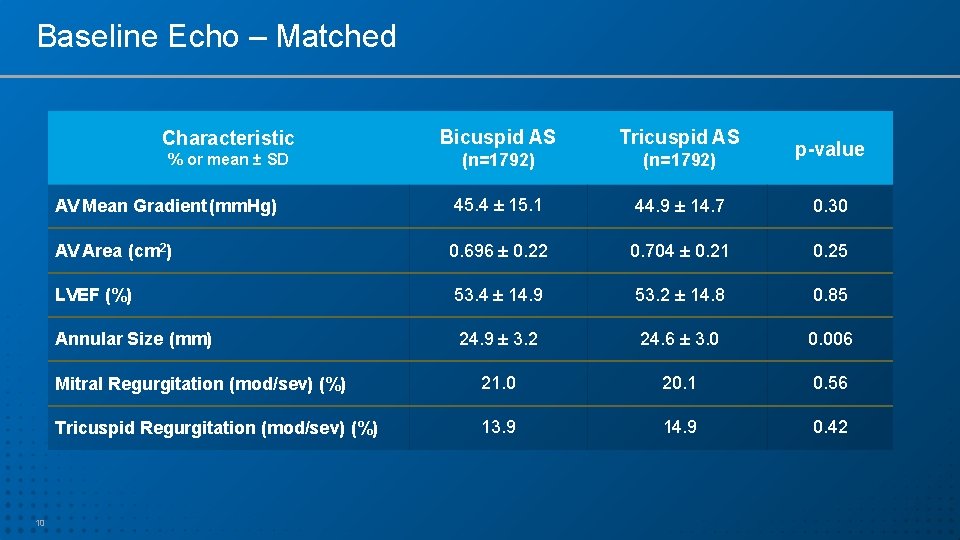
Baseline Echo – Matched 10 Characteristic Bicuspid AS Tricuspid AS % or mean ± SD (n=1792) AV Mean Gradient (mm. Hg) 45. 4 ± 15. 1 44. 9 ± 14. 7 0. 30 AV Area (cm 2) 0. 696 ± 0. 22 0. 704 ± 0. 21 0. 25 LVEF (%) 53. 4 ± 14. 9 53. 2 ± 14. 8 0. 85 Annular Size (mm) 24. 9 ± 3. 2 24. 6 ± 3. 0 0. 006 Mitral Regurgitation (mod/sev) (%) 21. 0 20. 1 0. 56 Tricuspid Regurgitation (mod/sev) (%) 13. 9 14. 9 0. 42 p-value
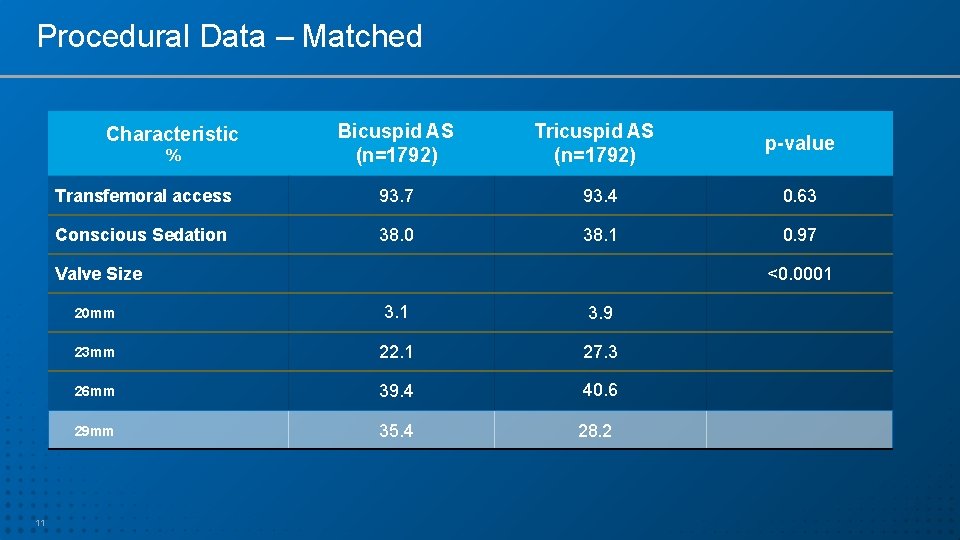
Procedural Data – Matched Characteristic % Bicuspid AS (n=1792) Transfemoral access 93. 7 93. 4 0. 63 Conscious Sedation 38. 0 38. 1 0. 97 Valve Size 11 p-value <0. 0001 20 mm 3. 1 3. 9 23 mm 22. 1 27. 3 26 mm 39. 4 40. 6 29 mm 35. 4 28. 2
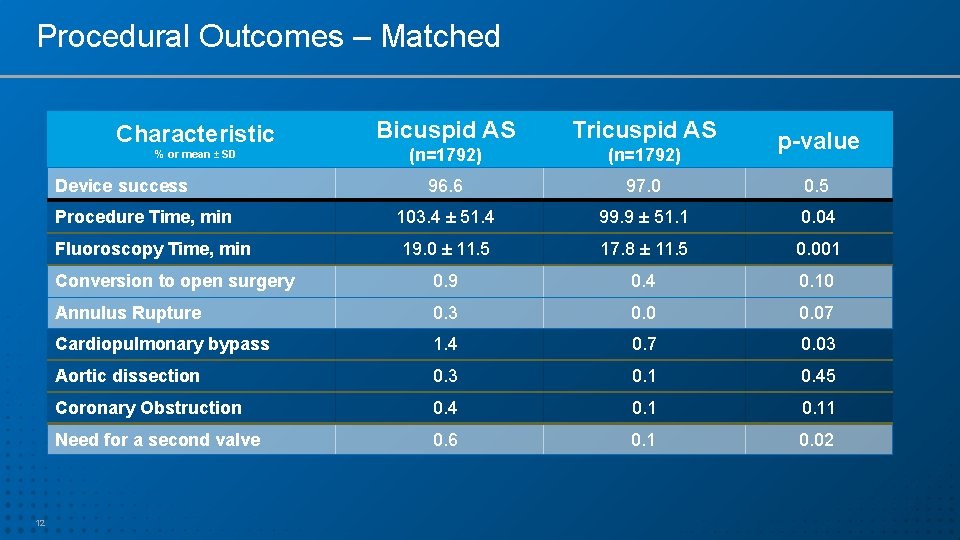
Procedural Outcomes – Matched Bicuspid AS Tricuspid AS (n=1792) 96. 6 97. 0 0. 5 103. 4 ± 51. 4 99. 9 ± 51. 1 0. 04 19. 0 ± 11. 5 17. 8 ± 11. 5 0. 001 Conversion to open surgery 0. 9 0. 4 0. 10 Annulus Rupture 0. 3 0. 07 Cardiopulmonary bypass 1. 4 0. 7 0. 03 Aortic dissection 0. 3 0. 1 0. 45 Coronary Obstruction 0. 4 0. 11 Need for a second valve 0. 6 0. 1 0. 02 Characteristic % or mean ± SD Device success Procedure Time, min Fluoroscopy Time, min 12 p-value
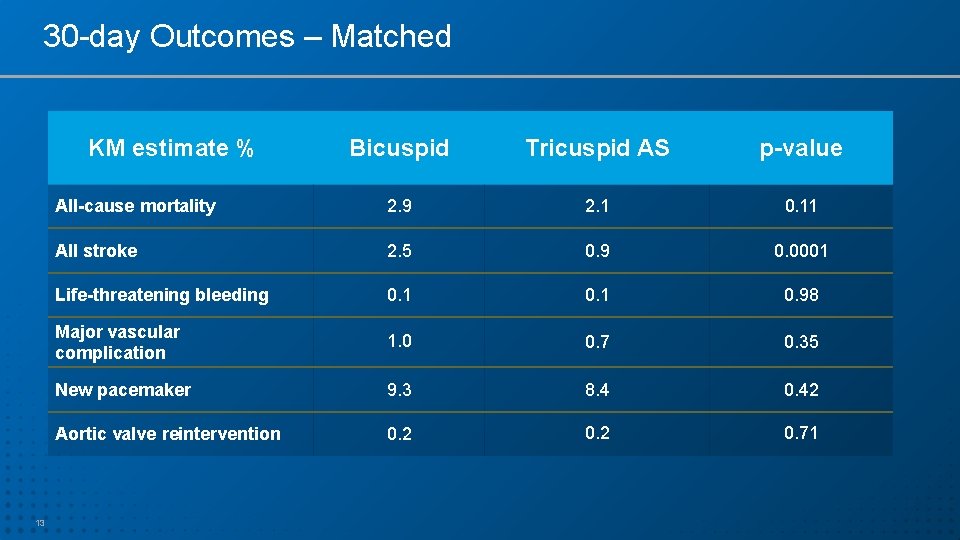
30 -day Outcomes – Matched KM estimate % 13 Bicuspid Tricuspid AS p-value All-cause mortality 2. 9 2. 1 0. 11 All stroke 2. 5 0. 9 0. 0001 Life-threatening bleeding 0. 1 0. 98 Major vascular complication 1. 0 0. 7 0. 35 New pacemaker 9. 3 8. 4 0. 42 Aortic valve reintervention 0. 2 0. 71
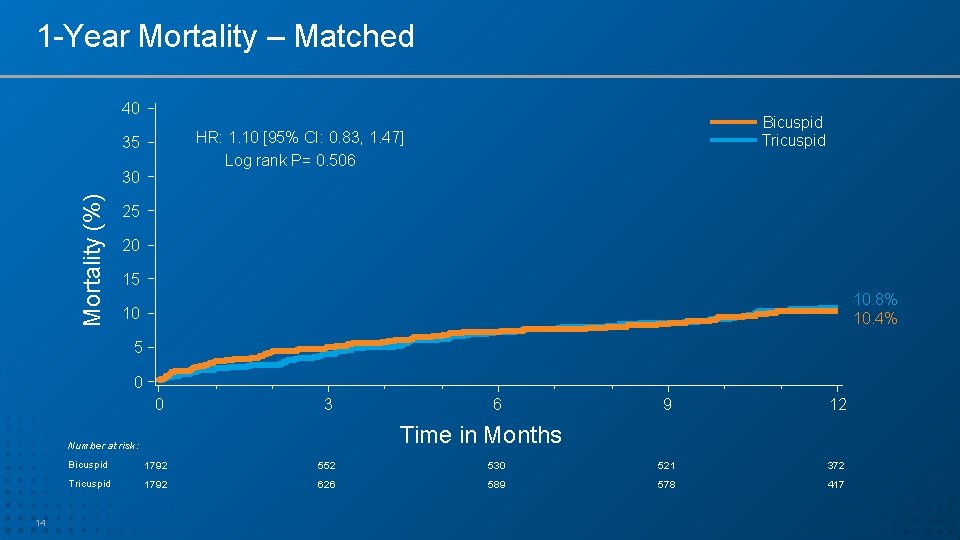
1 -Year Mortality – Matched 40 HR: 1. 10 [95% CI: 0. 83, 1. 47] Log rank P= 0. 506 35 30 Mortality (%) Bicuspid Tricuspid 25 20 15 10. 8% 10. 4% 10 5 0 0 3 9 12 Time in Months Number at risk: 14 6 Bicuspid 1792 552 530 521 372 Tricuspid 1792 626 589 578 417
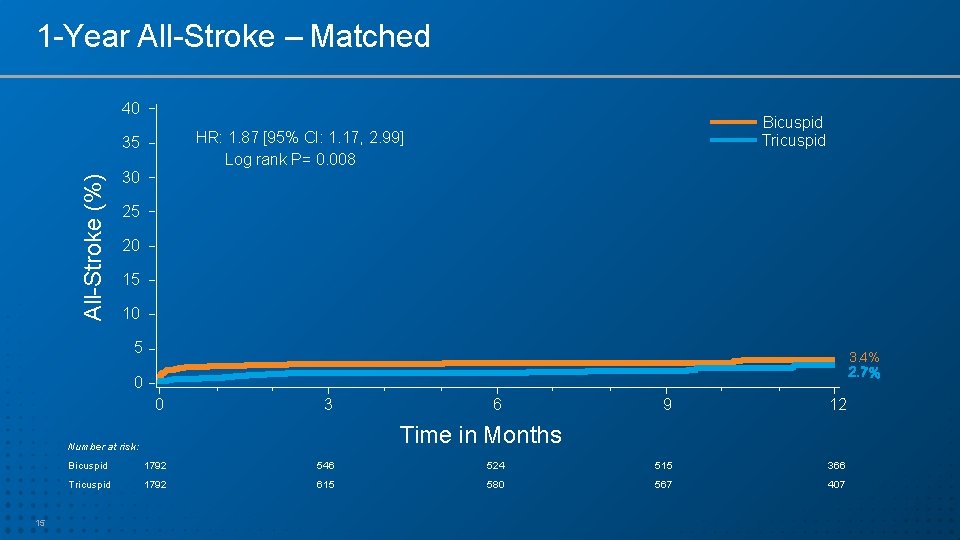
1 -Year All-Stroke – Matched 40 35 All-Stroke (%) Bicuspid Tricuspid HR: 1. 87 [95% CI: 1. 17, 2. 99] Log rank P= 0. 008 30 25 20 15 10 5 3. 4% 0 0 3 9 12 Time in Months Number at risk: 15 6 Bicuspid 1792 546 524 515 366 Tricuspid 1792 615 580 567 407
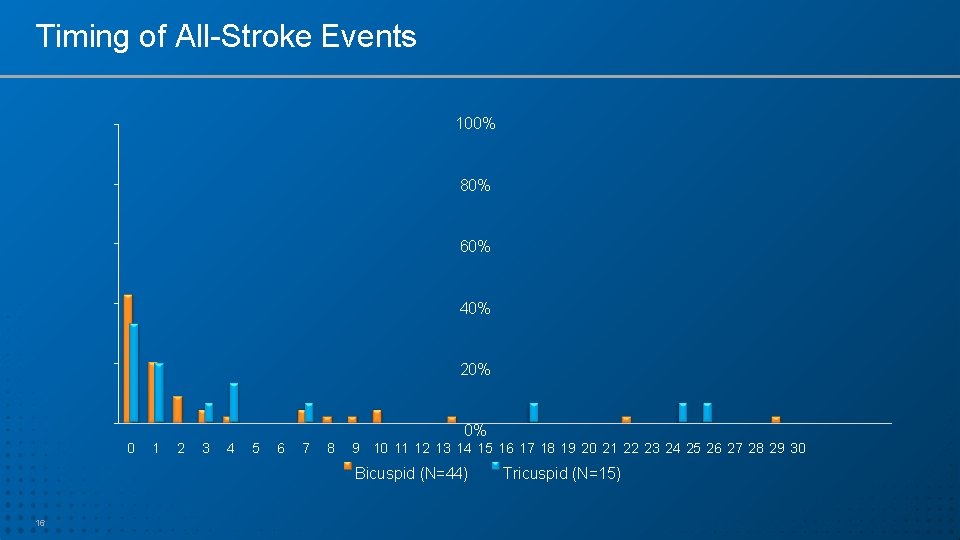
Timing of All-Stroke Events 100% 80% 60% 40% 20% 0% 0 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 Bicuspid (N=44) 16 Tricuspid (N=15)
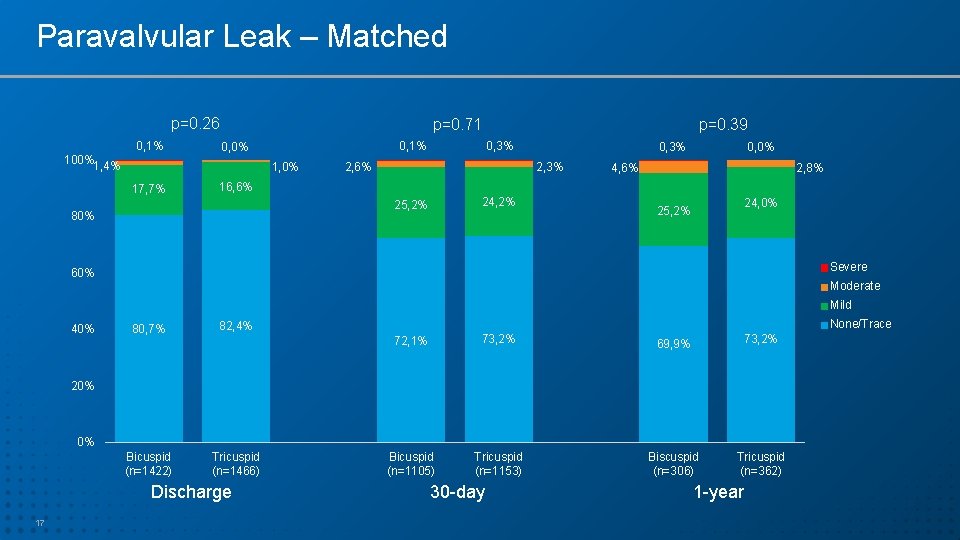
Paravalvular Leak – Matched p=0. 26 100% 1, 4% 0, 1% p=0. 71 1, 0% 17, 7% 0, 3% 0, 1% 0, 0% p=0. 39 2, 6% 0, 3% 2, 3% 0, 0% 4, 6% 2, 8% 16, 6% 24, 2% 25, 2% 80% 24, 0% 25, 2% Severe 60% Moderate Mild 40% 80, 7% None/Trace 82, 4% 72, 1% 73, 2% 69, 9% 73, 2% Bicuspid (n=1105) Tricuspid (n=1153) Biscuspid (n=306) Tricuspid (n=362) 20% 0% Bicuspid (n=1422) Tricuspid (n=1466) Discharge 17 30 -day 1 -year
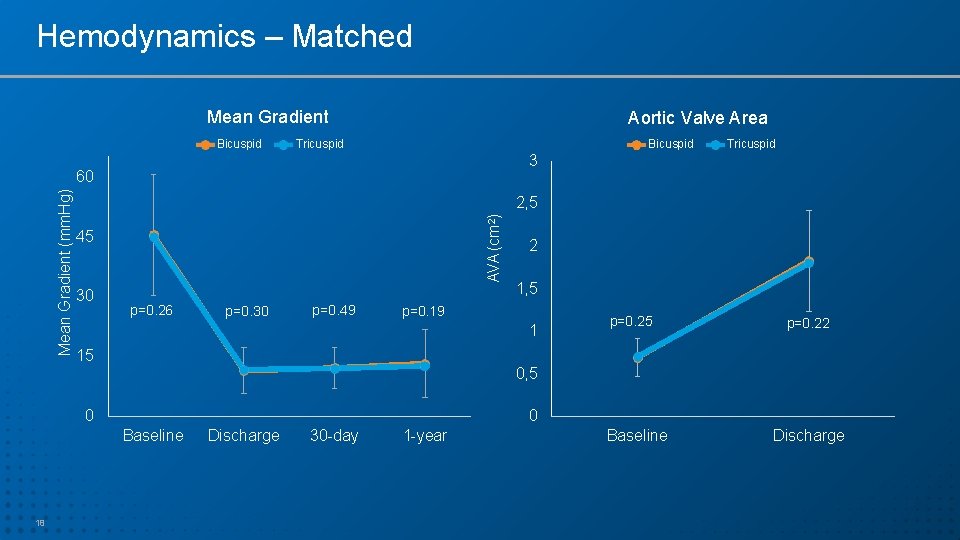
Hemodynamics – Matched Mean Gradient Bicuspid Aortic Valve Area Bicuspid Tricuspid 3 2, 5 AVA (cm 2) Mean Gradient (mm. Hg) 60 45 30 p=0. 26 p=0. 30 p=0. 49 2 1, 5 p=0. 19 1 15 p=0. 22 0, 5 0 0 Baseline 18 Tricuspid Discharge 30 -day 1 -year Baseline Discharge
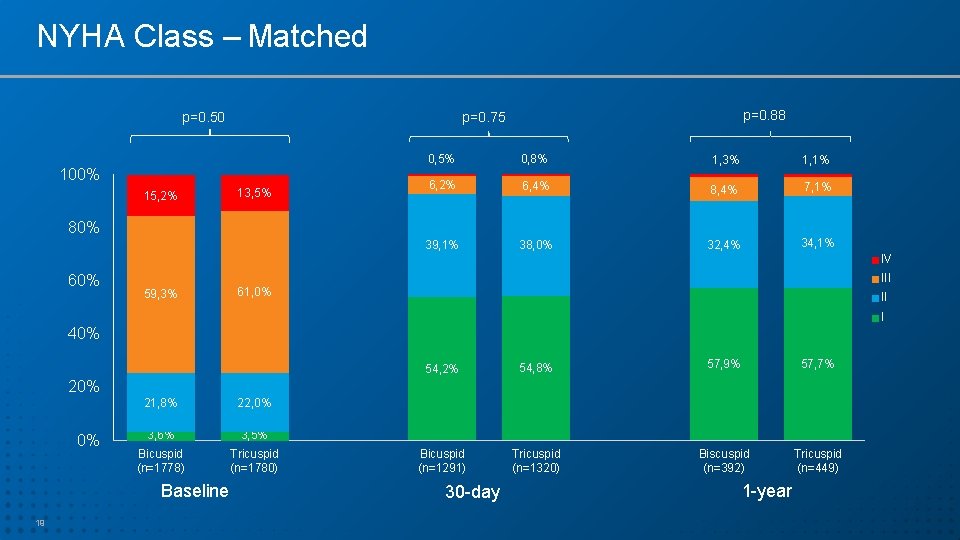
NYHA Class – Matched p=0. 50 100% 15, 2% p=0. 88 p=0. 75 13, 5% 0, 8% 1, 3% 1, 1% 6, 2% 6, 4% 8, 4% 7, 1% 39, 1% 38, 0% 32, 4% 34, 1% 80% IV 60% III 59, 3% 61, 0% II I 40% 54, 2% 54, 8% 57, 9% 57, 7% Bicuspid (n=1291) Tricuspid (n=1320) Biscuspid (n=392) Tricuspid (n=449) 20% 0% 21, 8% 22, 0% 3, 6% 3, 5% Bicuspid (n=1778) Tricuspid (n=1780) Baseline 19 30 -day 1 -year
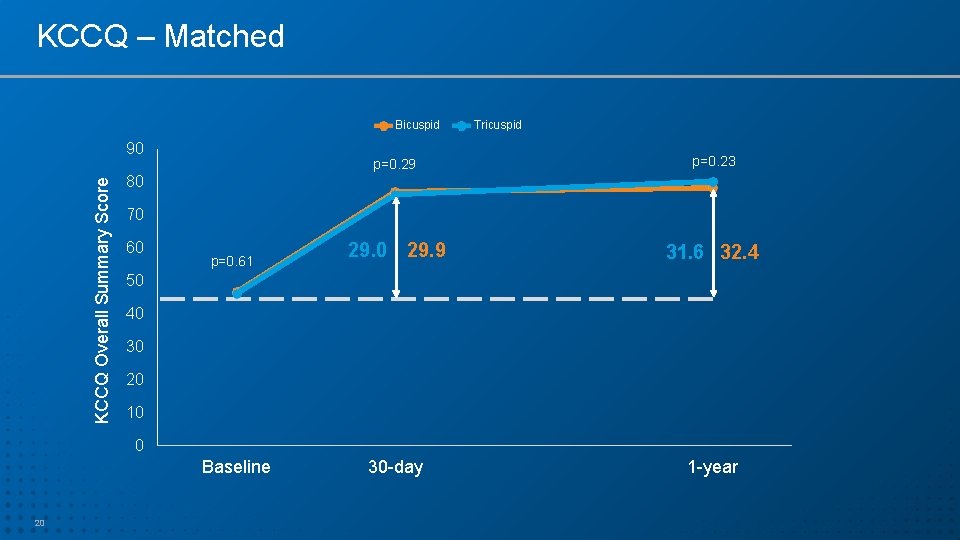
KCCQ – Matched Bicuspid KCCQ Overall Summary Score 90 Tricuspid p=0. 29 p=0. 23 29. 0 29. 9 31. 6 32. 4 30 -day 1 -year 80 70 60 p=0. 61 50 40 30 20 10 0 Baseline 20

Limitations • The STS/ACC TVT Registry, while mandatory for reimbursement, is mostly site reported and unadjudicated • Specific type of bicuspid (Sievers 0, 1 or 2) not specified • Not a randomized study and no comparison with surgical AVR 21

Summary • Patients with bicuspid AS were significantly younger and relatively healthier than tricuspid AS patients. • TAVR with SAPIEN 3 in this bicuspid AS population exhibited high device success (96. 6%) and low rates of procedural complications: – Less than 1% annulus rupture, need for second valve or conversion to surgery • The matched tricuspid AS cohort experienced very low rates of serious complications like annulus rupture (0. 0%) and stroke (0. 9%). • 30 -day stroke rate (2. 5%) was significantly higher in the bicuspid AS cohort as compared to the matched tricuspid AS cohort (0. 9%), and followed a similar peri-procedural time distribution. 22

Summary – Cont. • Hemodynamic outcomes (gradients and EOA) after TAVR in bicuspid AS were similar to tricuspid AS with SAPIEN 3 THV • Rates of significant PVL were low and similar between the 2 groups. • QOL improvement in both cohorts was remarkably high, sustained over time and similar between the 2 groups (~30 points increase in KCCQ score). • 1 -year survival was high and similar between the matched bicuspid and tricuspid AS patients. 23

Conclusion and Clinical Implications • TAVR with SAPIEN 3 in bicuspid AS appears safe and effective and maybe considered as a treatment option for patients at high and intermediate risk for surgery • Since the relatively higher stroke rates in bicuspid TAVR were largely peri-procedural, they might be reduced by the use of cerebral embolic protection devices • These data additionally support enrollment of carefully selected low surgical risk bicuspid AS patients in TAVR trials 24

THANK YOU
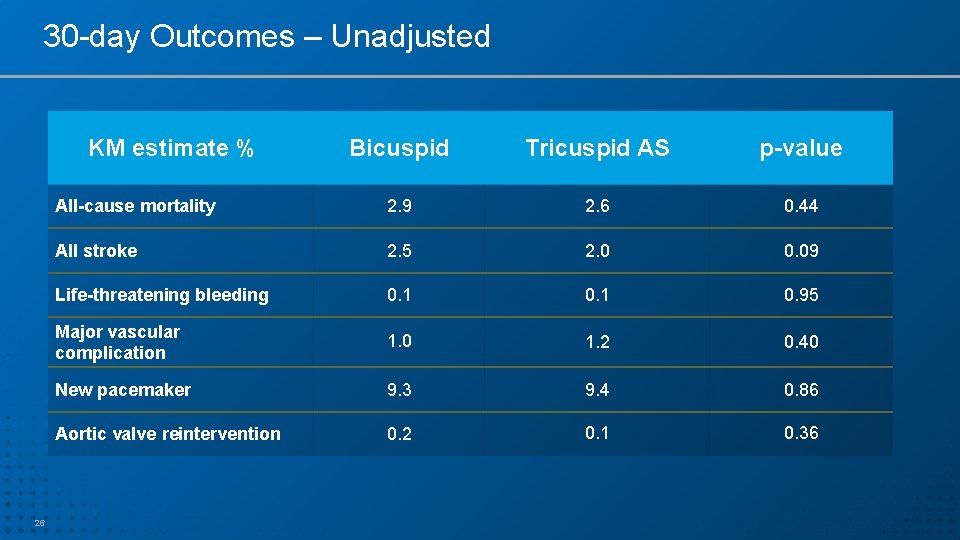
30 -day Outcomes – Unadjusted KM estimate % 26 Bicuspid Tricuspid AS p-value All-cause mortality 2. 9 2. 6 0. 44 All stroke 2. 5 2. 0 0. 09 Life-threatening bleeding 0. 1 0. 95 Major vascular complication 1. 0 1. 2 0. 40 New pacemaker 9. 3 9. 4 0. 86 Aortic valve reintervention 0. 2 0. 1 0. 36

Summary • Patients with bicuspid AS were significantly younger and relatively healthier than tricuspid AS patients. • TAVR with SAPIEN 3 in this bicuspid AS population exhibited high device success (96. 6%) and low rates of procedural complications: – Less than 1% annulus rupture, need for second valve or conversion to surgery 27 • The matched tricuspid AS cohort experienced exceedingly low rates of serious complications like annulus rupture (0. 0%) and all-stroke (0. 9%). • The all-stroke rate (2. 5%) was significantly higher in the bicuspid AS cohort as compared to the matched tricuspid AS cohort (0. 9%), and followed a similar peri-procedural time distribution. • The hemodynamic outcomes (AV gradients and EOA) after TAVR in bicuspid AS were similar to tricuspid AS • Rates of significant PVL were low and similar between the 2 groups. • QOL improvement in both cohorts was remarkably high, sustained over time and similar between the 2 groups (~30 points in KCCQ score). • 1 -year survival was high and similar between the 2 matched groups.
- Slides: 27