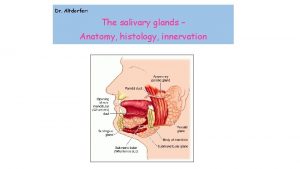
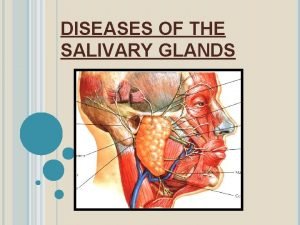
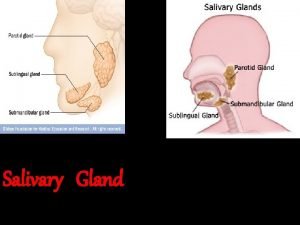
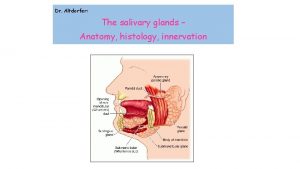
Salivary Glands Major Salivary Glands Parotid gland Submandibular

Salivary Glands
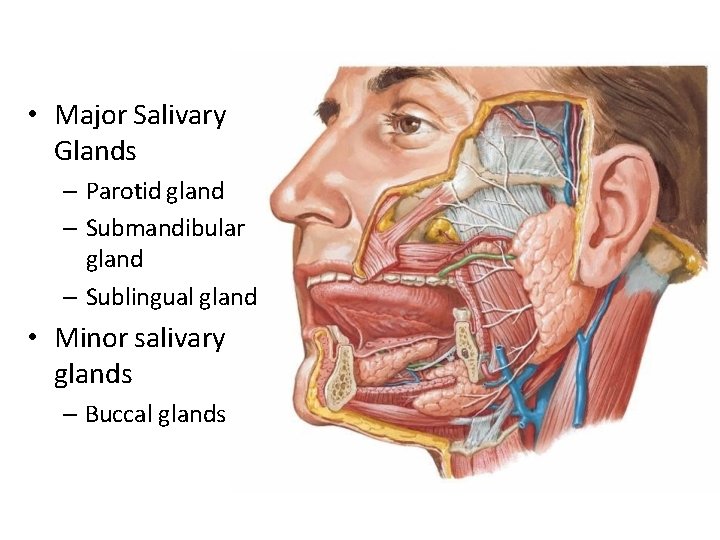
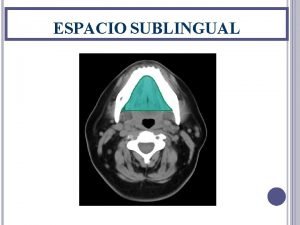
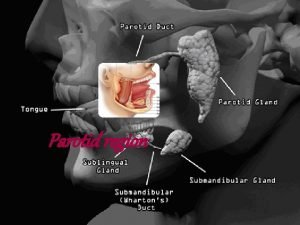
• Major Salivary Glands – Parotid gland – Submandibular gland – Sublingual gland • Minor salivary glands – Buccal glands
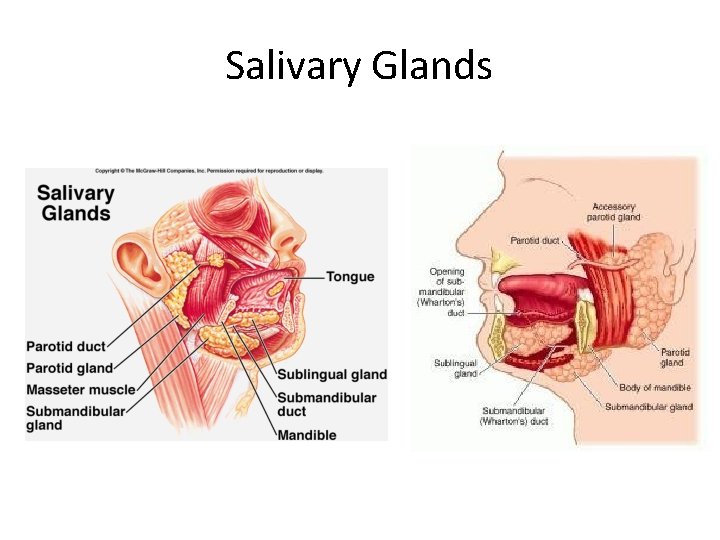
Salivary Glands

Major glands/Secretions • Parotid: Serous • Submandibular: Mucous & Serous • Sublingual: Mucous & Serous

Secretions • The salivary glands facilitate the process of tasting food, initiate its digestion and permit its swallowing. • These glands also protect the body by secreting the antibacterial agents lysozyme and lactoferrin as well as the secretory immunoglobulin A (Ig. A)

Salivary Glands Paired Branched tubuloalveolar glands Covered with capsule (connective tissue) Capsula gives septa that subdivide the glands into lobes and lobules. • Individual acini are also invested by thin connective tissue elements. • •
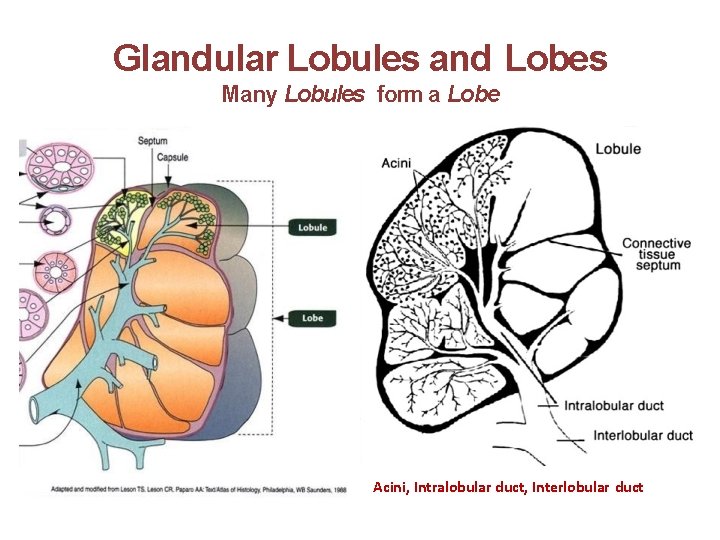
Glandular Lobules and Lobes Many Lobules form a Lobe Acini, Intralobular duct, Interlobular duct
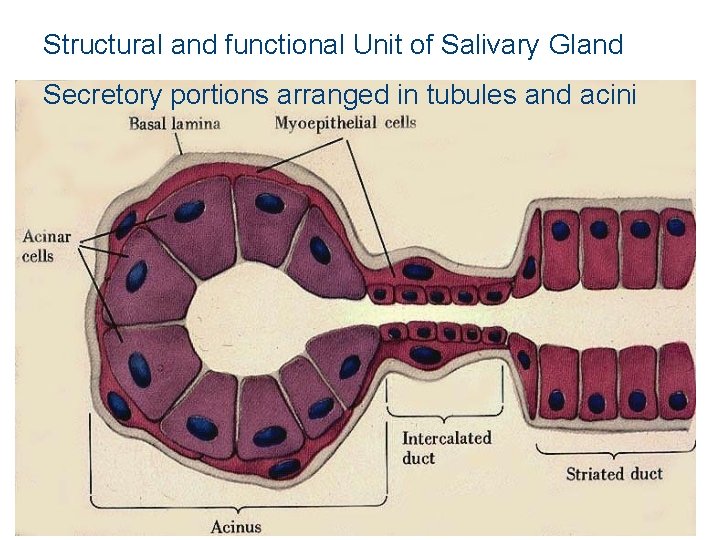
Structural and functional Unit of Salivary Gland Secretory portions arranged in tubules and acini

Secretory Portions • Tubules and acini composed of three types of cells – Serous cells: produce a thin watery secretion – Mucous cells: produce a more viscous secretion – Myoepithelial cells
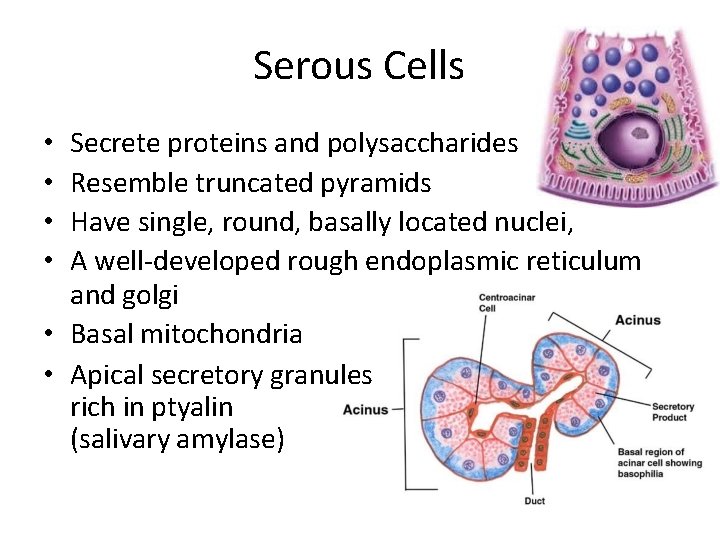
Serous Cells Secrete proteins and polysaccharides Resemble truncated pyramids Have single, round, basally located nuclei, A well-developed rough endoplasmic reticulum and golgi • Basal mitochondria • Apical secretory granules rich in ptyalin (salivary amylase) • •
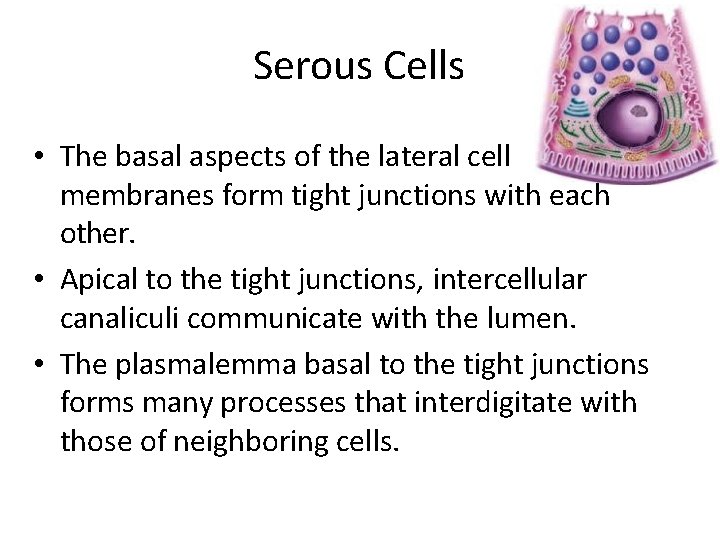
Serous Cells • The basal aspects of the lateral cell membranes form tight junctions with each other. • Apical to the tight junctions, intercellular canaliculi communicate with the lumen. • The plasmalemma basal to the tight junctions forms many processes that interdigitate with those of neighboring cells.

Serous Acini
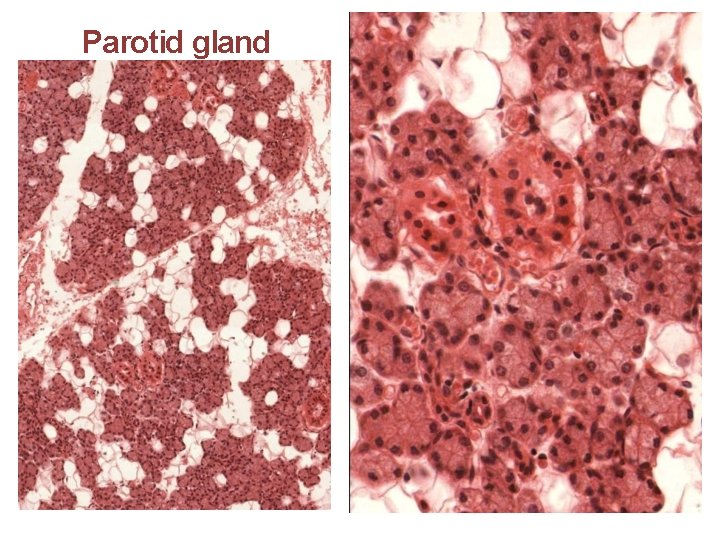
Parotid gland
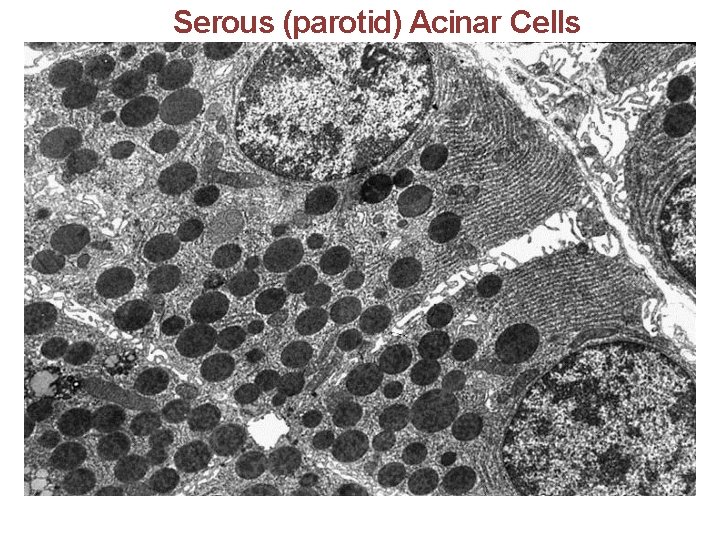
Serous (parotid) Acinar Cells

Mucous Cells • The shape is similar with serous cells • Their nuclei also basally located but are flattened • Have fewer mitochondria, less RER and greater golgi apparatus because of their secretory product include carbonhydrate.
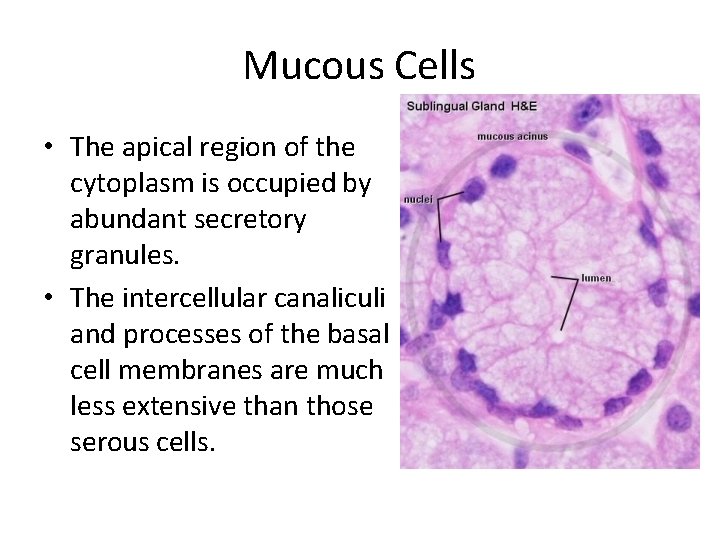
Mucous Cells • The apical region of the cytoplasm is occupied by abundant secretory granules. • The intercellular canaliculi and processes of the basal cell membranes are much less extensive than those serous cells.
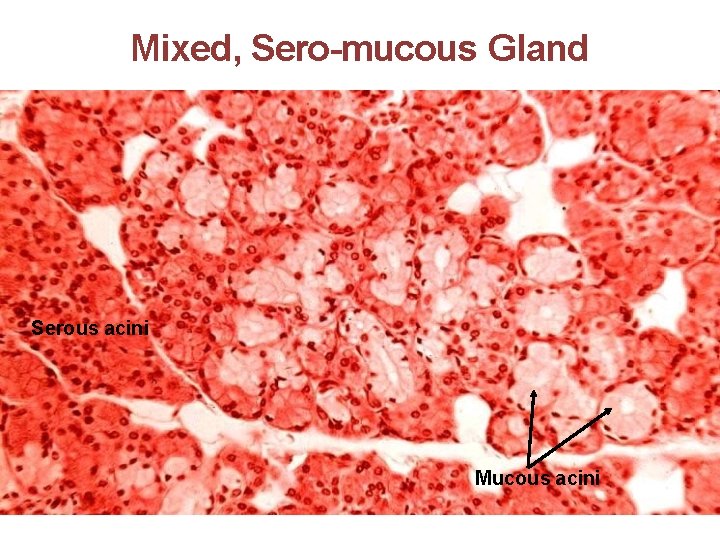
Mixed, Sero-mucous Gland Serous acini Mucous acini
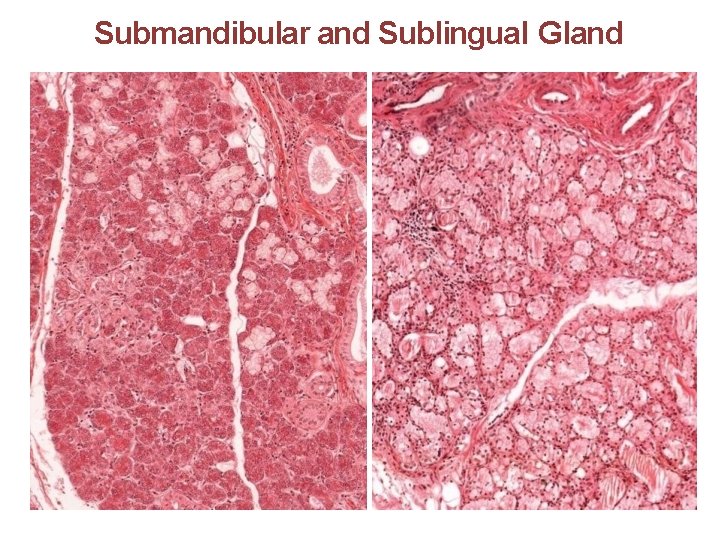
Submandibular and Sublingual Gland

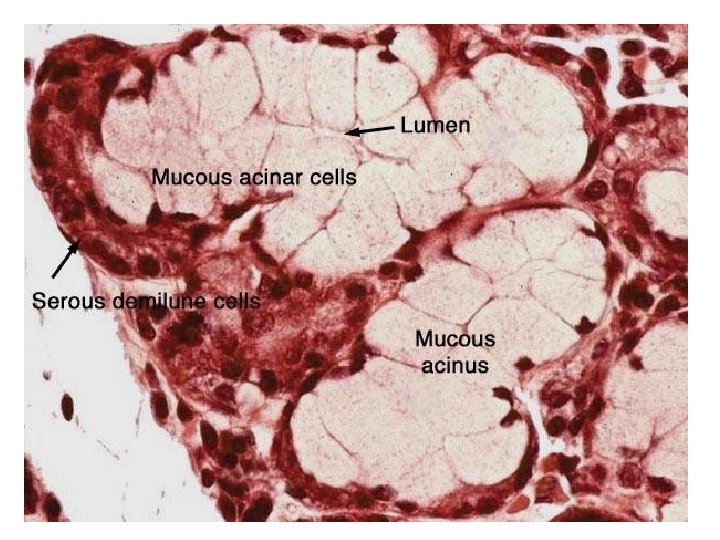
Serous Demilune (Giannuzi) • Serous acini covered the mucous acini
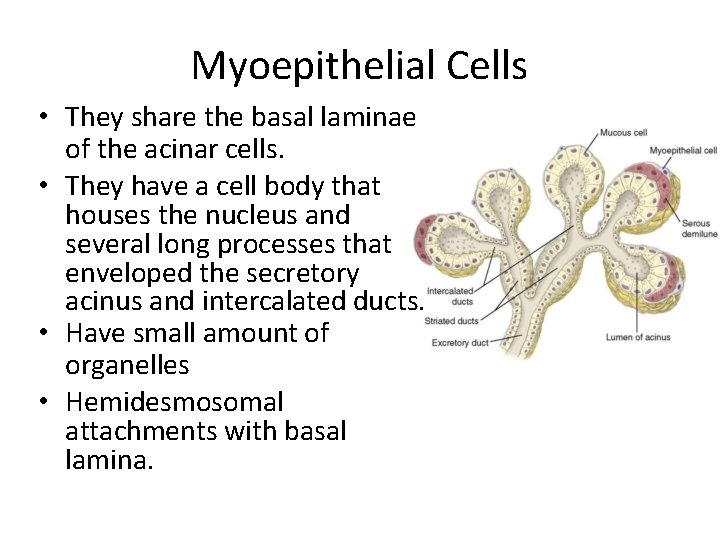
Myoepithelial Cells • They share the basal laminae of the acinar cells. • They have a cell body that houses the nucleus and several long processes that enveloped the secretory acinus and intercalated ducts. • Have small amount of organelles • Hemidesmosomal attachments with basal lamina.
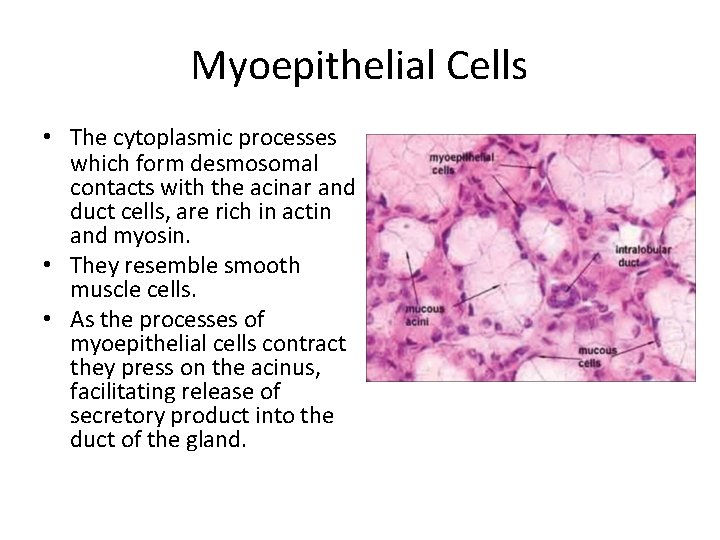
Myoepithelial Cells • The cytoplasmic processes which form desmosomal contacts with the acinar and duct cells, are rich in actin and myosin. • They resemble smooth muscle cells. • As the processes of myoepithelial cells contract they press on the acinus, facilitating release of secretory product into the duct of the gland.

Myoepithelial Cell
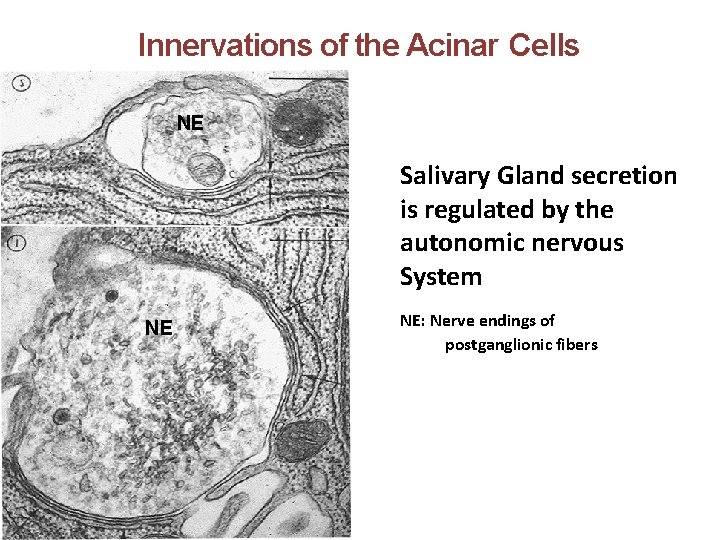
Innervations of the Acinar Cells NE Salivary Gland secretion is regulated by the autonomic nervous System NE NE: Nerve endings of postganglionic fibers
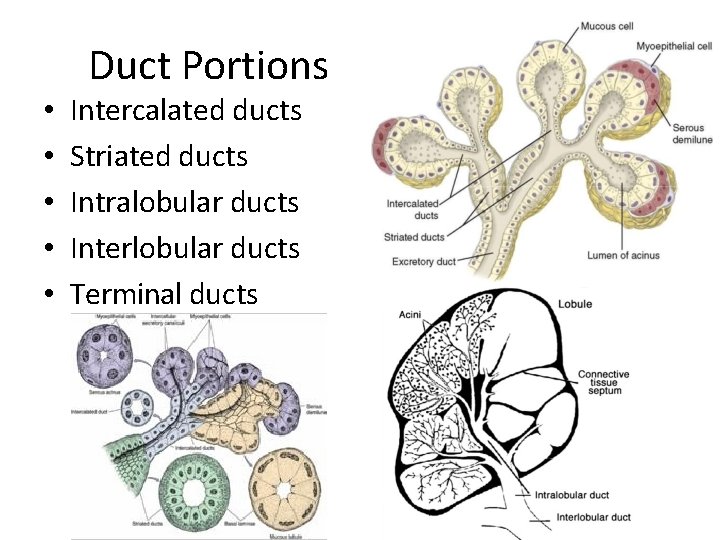
Duct Portions • • • Intercalated ducts Striated ducts Intralobular ducts Interlobular ducts Terminal ducts
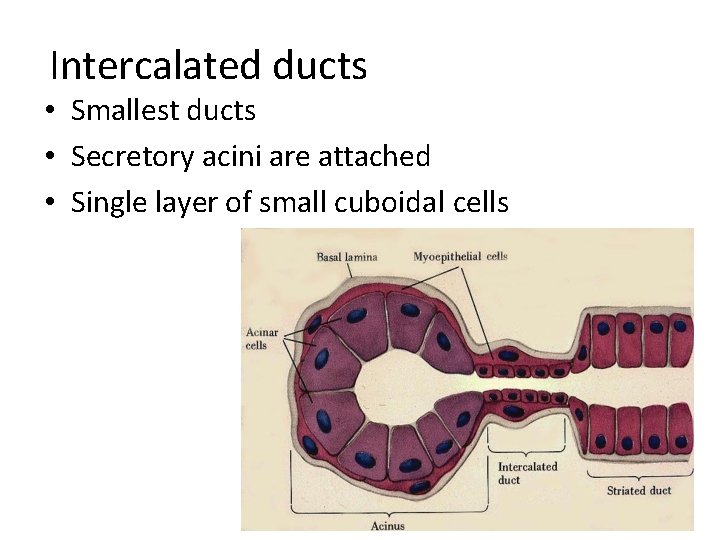
Intercalated ducts • Smallest ducts • Secretory acini are attached • Single layer of small cuboidal cells

Striated Ducts • Intercalated ducts merge • Single layer of cuboidal or low columnar cells • The basolateral membranes of these cells are highly folded and have longitudinaly arranged mitochondria • The basolateral cell membranes of these cells have sodium adenosine triphosphatase pump.

Intercalated (blue) and Striated (green) Ducts
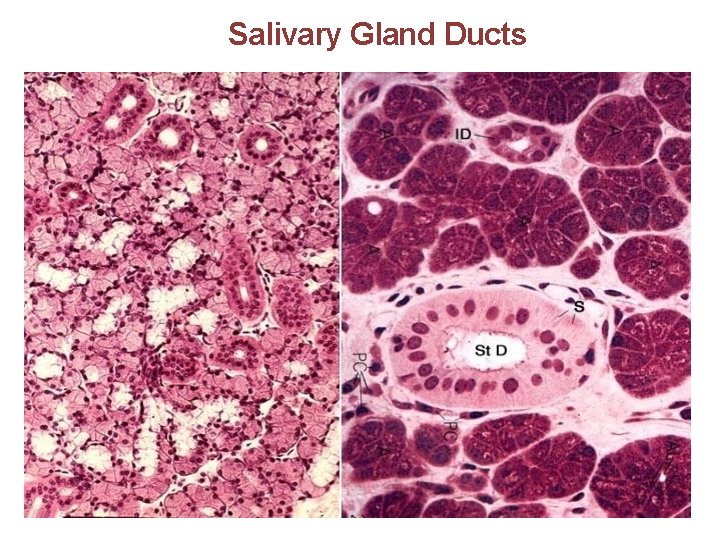
Salivary Gland Ducts
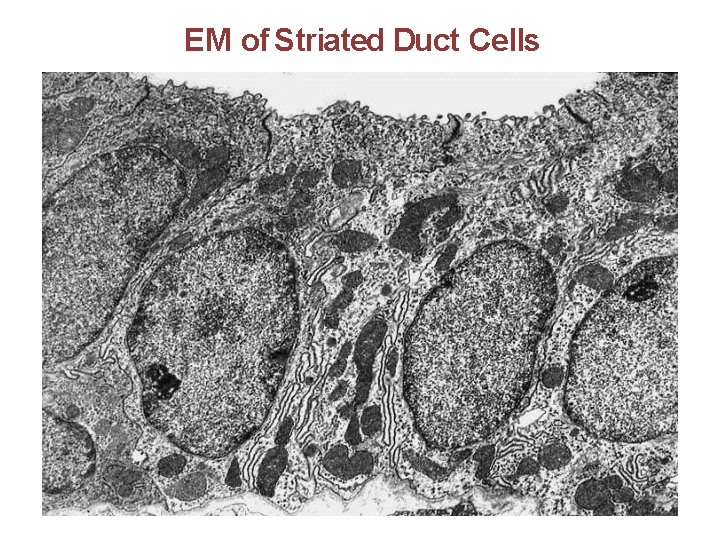
EM of Striated Duct Cells

Intralobular Ducts • Striated ducts join with each other forming intralobular ducts of increasing caliber which are surrounded by more abundant connective tissue elements.

Intra and Inter Lobular Ducts

Ducts • Ducts arising from lobules unite to form interlobular ducts. • The terminal duct of the gland deliveres saliva into the oral cavity.
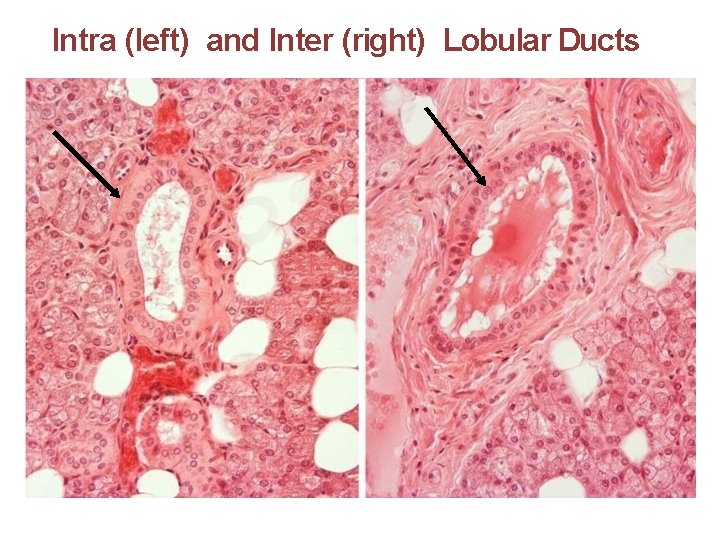
Intra (left) and Inter (right) Lobular Ducts

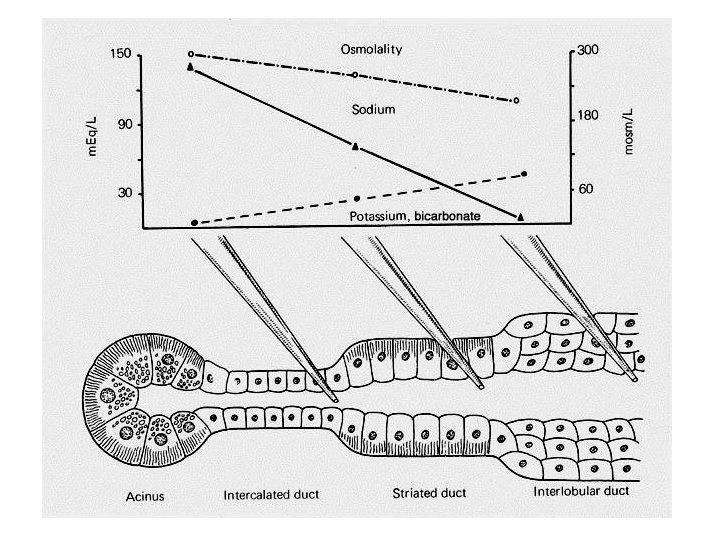
Role of Striated Ducts in Saliva Production

Saliva Secretion About 1, 000 ml/day Submandibular Glands Parotid Glands Sublingual Glands Minor Salivary Glands Flow Rate 0. 3 ml/min (Unstimulated) Stimulation Autonomic Nervous System Composition Varies with flow rate 65 -70% 20 -25% 4 -5% 5 -8%

Composition of Saliva Water Ions: Bicarbonate, potassium, sodium, chloride, etc Glycoproteins Mucus Proteins: Enzymes – Amylase (parotid gland), nucleases, Cells: Desquamated Epithelial cells Leukocytes p. H: ~ 7. 0 etc.

Saliva Functions • Lubricating and cleansing of the oral cavity • Antibacterial activity • Participating in the taste sensation bu dissolving food material • Initial digestion via action of ptyalin and salivary lipase • Aiding swallowing by moistening the food and permitting the formation of bolus • Participating in the clotting and wound healing processes

Saliva Production • The saliva manufactured by the aciner cells, called primary saliva, is isotonic with plasma. • The primary saliva is modified by the cells of the striated ducts by removing sodium and chloride ions from it and secreting potassium and bicarbonate ions into it. • There after, the altered secretion is called secondary saliva.

Saliva Production • • • Secretory Ig. A Lactoferrin Lysozyme Thiocyanate Kallikrein (converts bradykinin: a vasodilatator)
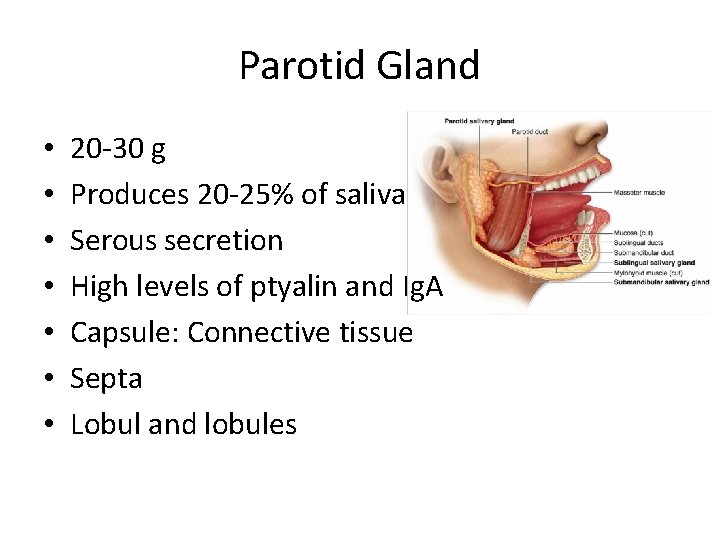
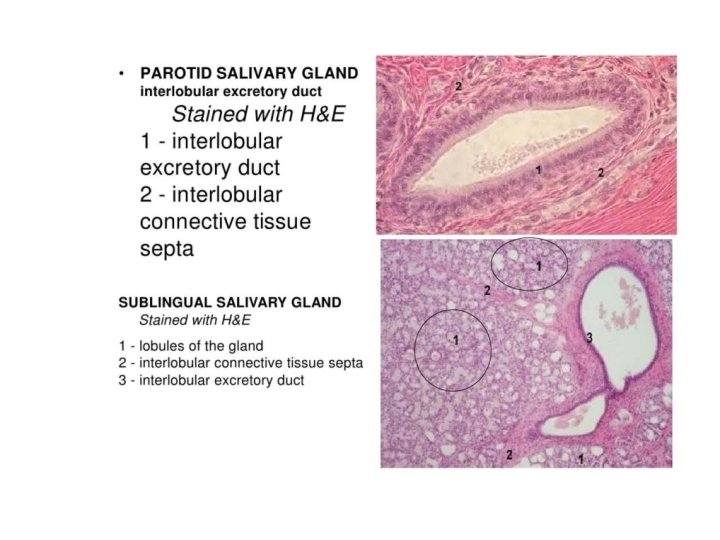
Parotid Gland • • 20 -30 g Produces 20 -25% of saliva Serous secretion High levels of ptyalin and Ig. A Capsule: Connective tissue Septa Lobul and lobules
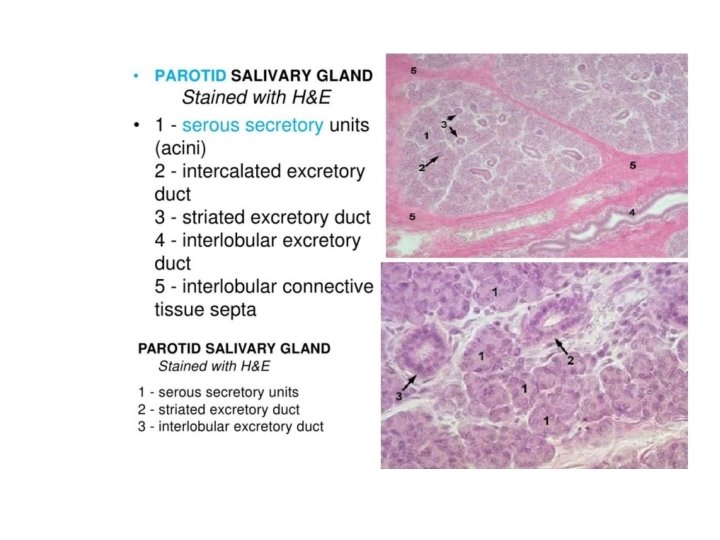
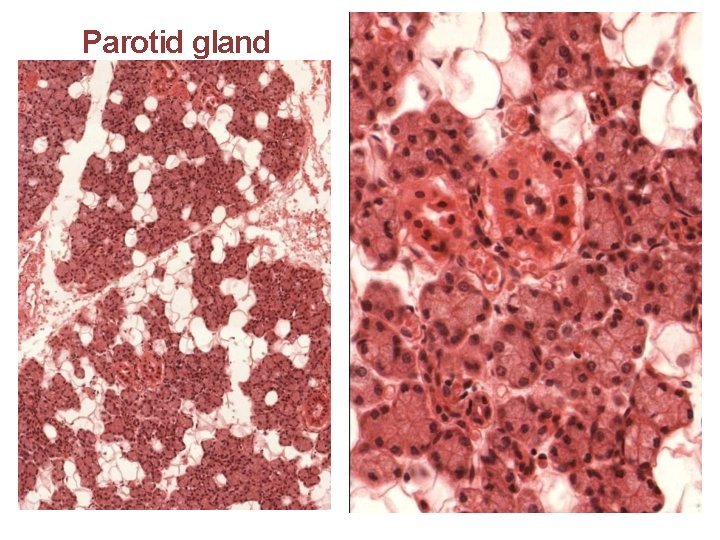
Parotid gland
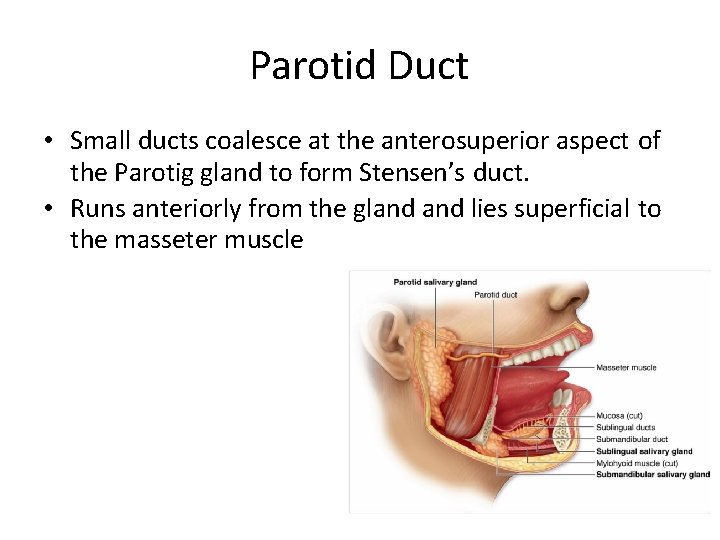
Parotid Duct • Small ducts coalesce at the anterosuperior aspect of the Parotig gland to form Stensen’s duct. • Runs anteriorly from the gland lies superficial to the masseter muscle


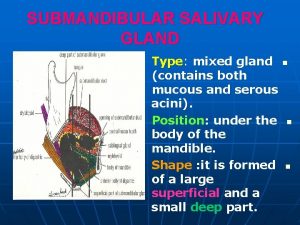
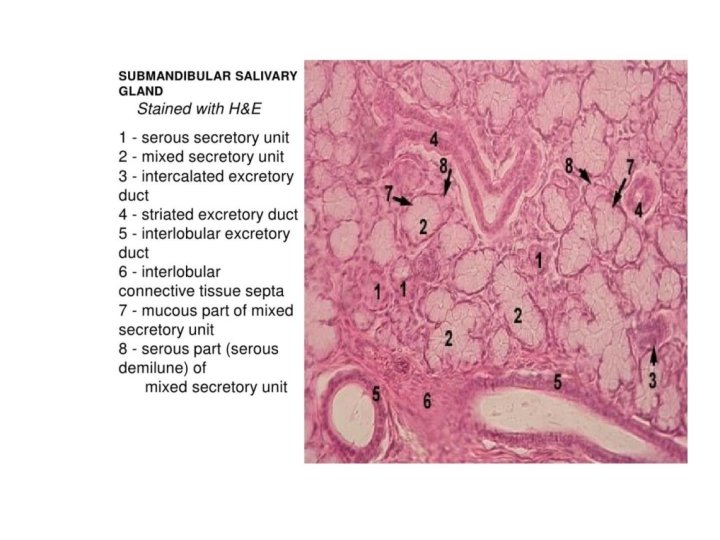
Submandibular Gland • 12 -15 g • 90% of acini produce serous saliva • The striated ducts of the submandibular gland are much longer than those of other salivary glands. • Serous acini more than mucous acini • Capsule: Connective tissue • Septa • Lobul and lobules

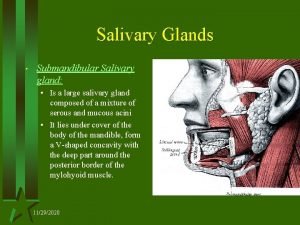
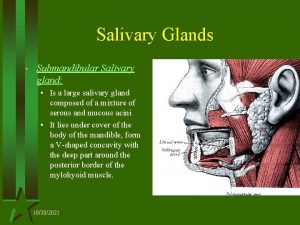
Submandibular gland • Located in the submandibular triangle of the neck, inferior & lateral to mylohyoid muscle. • The posterior-superior portion of the gland curves up around the posterior border of the mylohyoid and gives rise to Wharton’s duct.

Submandibular gland • Located in the submandibular triangle of the neck, inferior & lateral to mylohyoid muscle. • The posterior-superior portion of the gland curves up around the posterior border of the mylohyoid and gives rise to Wharton’s duct.
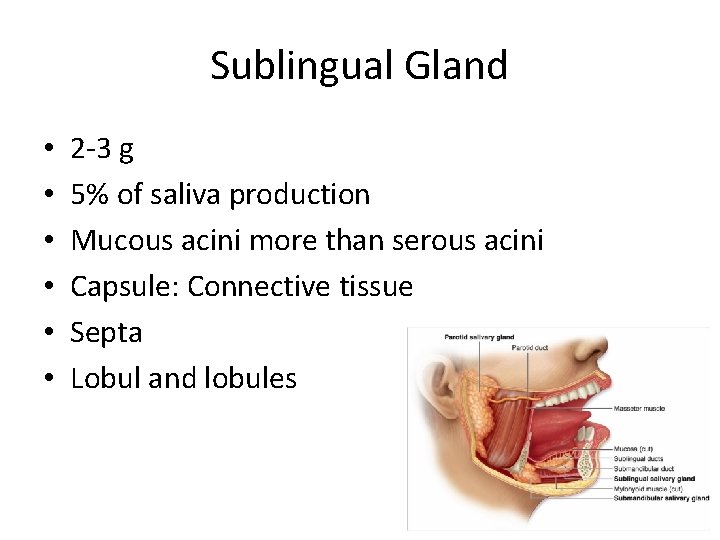
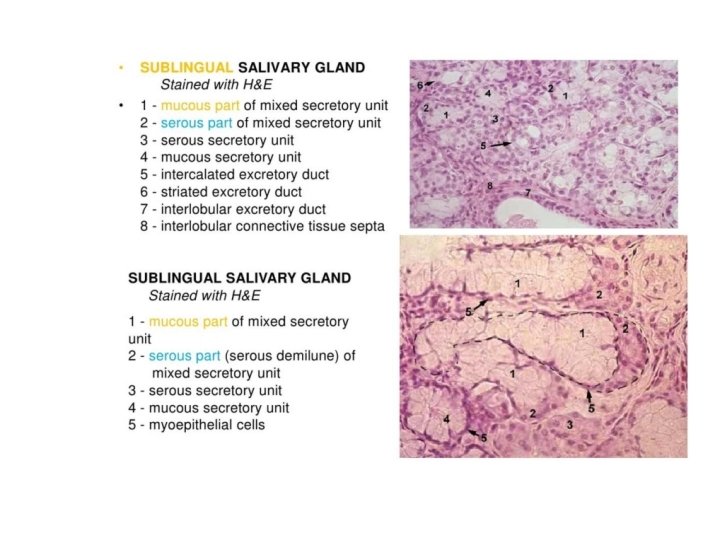
Sublingual Gland • • • 2 -3 g 5% of saliva production Mucous acini more than serous acini Capsule: Connective tissue Septa Lobul and lobules

Sublingual glands • The ducts of the sublingual glands are called Bartholin’s ducts. • In most cases, Bartholin’s ducts consists of 8 -20 smaller ducts of Rivinus. These ducts are short and small in diameter.


Development of the salivary glands • epithelial pouches of the oral cavity (6 th – 8 th week) • the intergrowth into the adjacent ectomesenchyme its connective tissue comes from the neural crest • parenchyme ( secretion) comes from the proliferating oral epithelium – ectoderm gl. parotis – endoderm gl. submandibularis et sublingualis

Embryology Brief overview of salivary gland development. Schematic diagram of the 4 stages of salivary gland development: initial bud, pseudoglandular, canalicular, and terminal bud stage. Laminin-producing epithelia in end buds are indicated in light grey (pseudoglandular stage). Laminin-producing epithelia are only present in end buds but not in the stalk portion during Br. M. A schematic diagram of the 3 steps in branching morphogenesis, stalk elongation, cleft formation, and dichotomization is also shown. Salivary mesenchyme is indicated in dark grey, and epithelia in white. mes: mesenchyme; e: epithelium; e. b: epithelial bud.

Embryology • The parotid anlagen are the first to develop, followed by the submandibular gland, and finally the sublingual gland. • Parenchymal tissue (secretory) of the glands arises from the proliferation of oral epithelium.

Embryology • The stroma (capsule and septae) of the glands originates from mesenchyme that may be mesodermal or neural crest in origin.

Parotid development • Although the parotid anlagen are the first to develop, they become encapsulated AFTER the Submandibular and Sublingual glands. • This delayed encapsulation is critical because after the encapsulation of the Submandibular and Sublingual glands but BEFORE encapsulation of the parotid, the lymphatic system develops.

Parotid development • Therefore, there are intraglandular lymph nodes and lymphatic channels entrapped within the parotid gland. • Parotid gland is also unique because its epithelial buds grow, branch and extend around the divisions of the facial nerve.

Embryology • The epithelial buds of each gland enlarge, elongate and branch initially forming solid structures. • Branching of the glandular mass produces arborization. • Each branch terminates in one or two solid end bulbs.

Embryology • Elongation of the end bulb follows and lumina appears in their centers, transforming the end bulbs into terminal tubules. • These tubules join the canalizing ducts to the peripheral acini.

Duct Canalization • Canalization results from mitotic activity of the outer layers of the cord outpacing that of the inner cell layers • Canalization is complete by 6 th month post conception.

Acinar cells • At around the 7 -8 th month in utero, secretory cells (acini) begin to develop around the ductal system.
- Slides: 65