Salivary Gland Neoplasm Dr Saad AlMuhayawi M D


























- Slides: 43

Salivary Gland Neoplasm Dr. Saad Al-Muhayawi. M. D. , FRCSC Associate Professor & Consultant ORL Head & Neck Surgery









Salivary gland neoplasm 1. Major salivary gland a. Parotid gland b. Submandibular gland c. Sublingual gland 2. Minor salivary gland 600 – 1, 000 minor salivary gland distributed throughout the mucosa of the upper aerodigestive tract (more common in the soft and hard palate).

80% of salivary gland tumor occur in the parotid. 10 – 15% in the minor salivary gland. 5 – 10% in the submandibular gland. 80% of the parotid tumor are benign. The most common is pleomorphic adenoma. 50% of the submandibular gland tumor are benign. 30% of the minor salivary gland are benign.

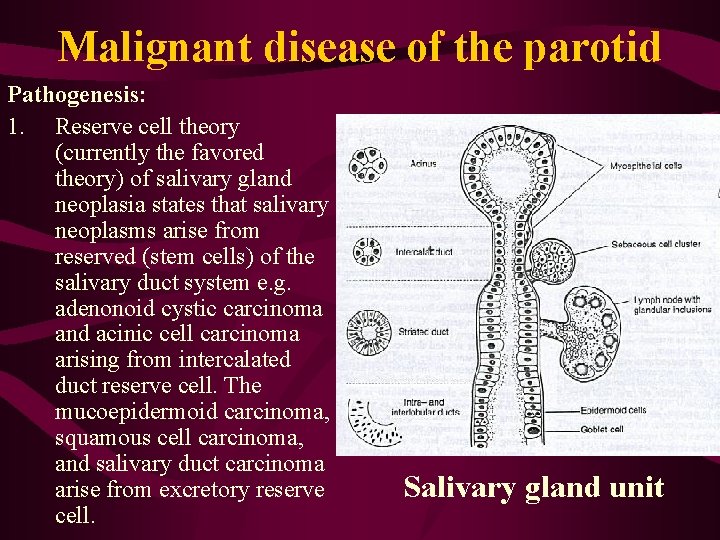
Malignant disease of the parotid Pathogenesis: 1. Reserve cell theory (currently the favored theory) of salivary gland neoplasia states that salivary neoplasms arise from reserved (stem cells) of the salivary duct system e. g. adenonoid cystic carcinoma and acinic cell carcinoma arising from intercalated duct reserve cell. The mucoepidermoid carcinoma, squamous cell carcinoma, and salivary duct carcinoma arise from excretory reserve cell. Salivary gland unit

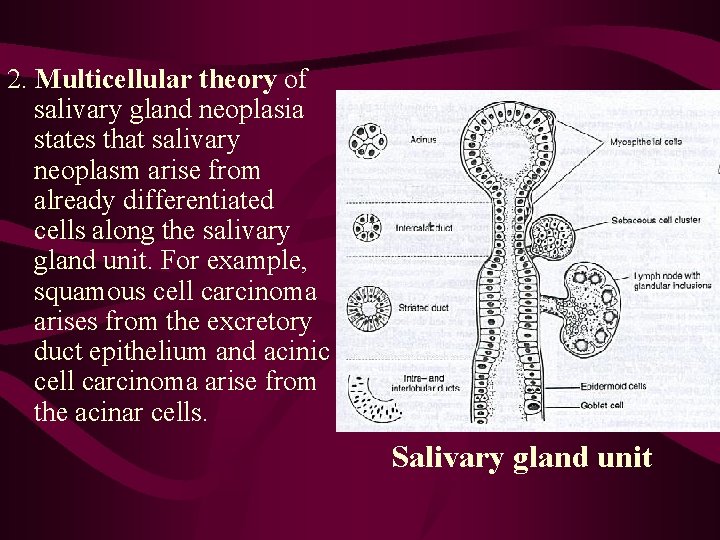
2. Multicellular theory of salivary gland neoplasia states that salivary neoplasm arise from already differentiated cells along the salivary gland unit. For example, squamous cell carcinoma arises from the excretory duct epithelium and acinic cell carcinoma arise from the acinar cells. Salivary gland unit

What are the most common benign tumor of the parotid? 1. Pleomorphic adenoma (benign mixed tumor). 2. Warthin’s tumor (papillary cyst adenoma lypmhomatosum). 3. Monomorphic adenoma a. Basal cell adenoma b. Canalicular adenomas c. Oncocytoma d. Myoepitheliomas 4. Granular cell tumor 5. Hemangioma

What are the most common malignant neoplasm of the parotid gland? 1. Mucoepidermoid carcinoma – 40% It can high, intermediate, and low-grade base on the clinical behavior and the tumor differentiation which is related to the percentage of mucinous to epidermoid cell. 2. Adenoid cystic carcinoma – 10% Adenoid cystic carcinoma are unique among the salivary gland tumors because of their indolent and protracted clinical course. Characterized by preneural spread including skip lesions. The disease thus specific survival continuous to declined for more than 20 years after initial treatment.

3. Acinic cell carcinoma – 10 – 15 % of It is considered a low-grade tumor. 4. Malignant mixed tumor - 7% It is considered a high-grade malignancy. 5. Polymorphous low grade adenocarcinoma – 10% It is a low-grade variant of adenocarcinoma. 6. Adeno carcinoma – 10% It is a high-grade with poor prognosis. 7. Squamous cell carcinoma – 4% It is high-grade, more common in elderly patients, and can confused with high-grade mucoepidermoid carcinoma.

The malignant parotid tumor can be classified into: 1. High-grade: aggressive behavior, local invasion, and lymph node metastasis. - high grade mucoepidermoid carcinoma - adenoid cystic carcinoma - carcinoma ex phelomorphic adenoma - adenocarcinoma - aquamous cell carcinoma - undifferentiated carcinoma

2. Low-grade malignancy - low grade mucoepidermoid carcinoma - pholymorphous low grade adenocarcinoma - acinic cell carcinoma - low grade adenocarcinoma - basal cell carcinoma 3. Intermediate grade - intermediate grade mucoepidermoid carcinoma - intermediate grade adenocarcinoma - oncocytic carcinoma

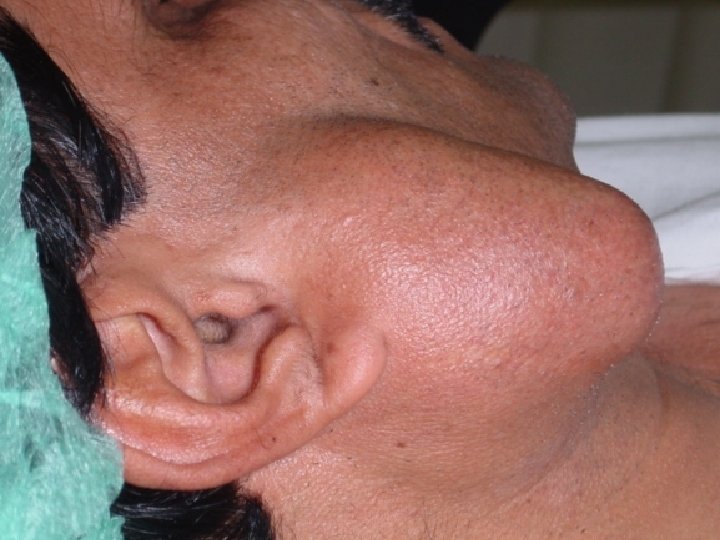
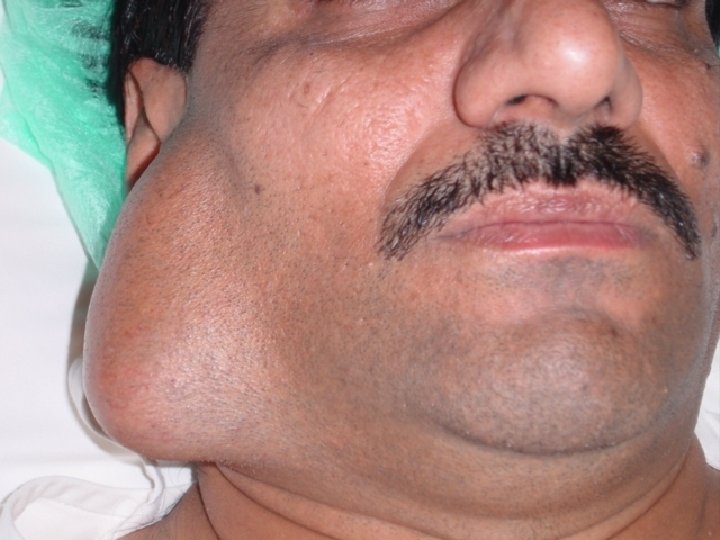
Evaluation of patients with a parotid mass 1. History Important points in the history: - Parotid mass (duration, rate of the growth, presence of pain) - Facial paralysis - Cervical lymphadenopathies - Eyes and joints symptoms - History of exposure to radiation

2. Examination - Size of the mass - Skin fixation - Cervical adenopathies - Facial nerve functions 3. Investigation C. T. and MRI are both effective modalities for imaging the size, the local, and the regional extension of the primary tumor and the neck metastasis. C. T. saliography – it replaced now by highresolution contrasted C. T. and MRI.

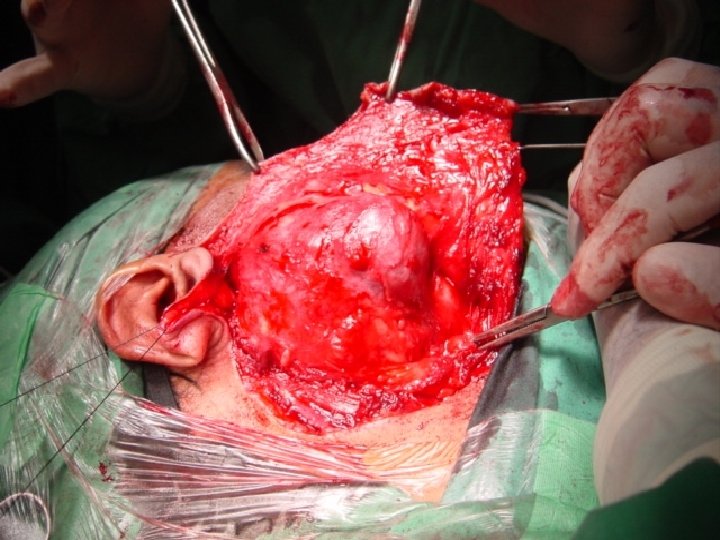
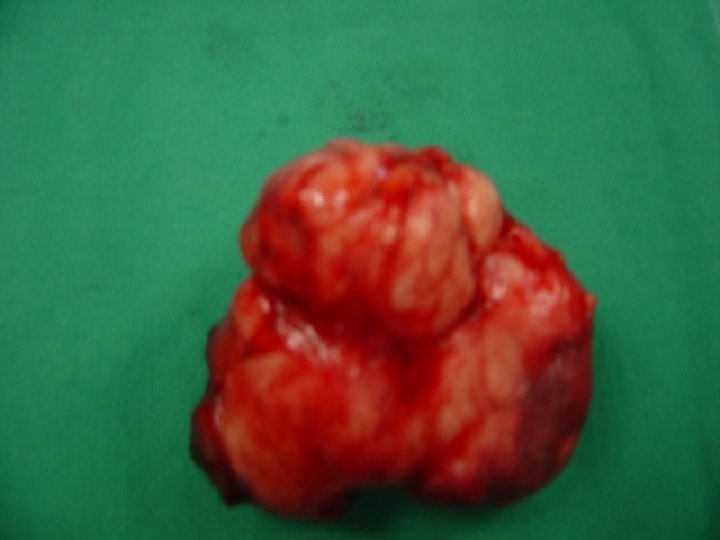
4. FNAB - The accuracy is around 90% depend on the techniques of aspirate and the cytopathologist. 5. Superficial parotidectomy is considered as a diagnostic and therapeutic for most benign tumors.

The post-operative complications: 1. Skin flap necrosis 2. Hematoma 3. Salivary fistula and sialoseles – it presents as an opening in the suture line below the lobule of the ear. 4. Facial nerve paralysis – which could be: a. Temporarily: 5 – 10% of the patients. b. Permanent: less than 2% of the cases. 5. Numbness of the ear due to injury of great auricular nerve.

6. Xerostomia not common in the superficial parotidectomy (30% of salivary producing tissue). 5. Frey’s syndrome (Gustatory sweating syndrome) Incidence in 50% of the patients. Etiology: post-operative growth of the interrupted preganglionic parasympathetic nerve branches to the parotid into the more superficial sweat glands. The diagnosis is usually made from the history but can be confirmed by the starch-iodine test.

What is starch-iodine test? Paint the affected skin with iodine, dust the skin with the starch, feed the patient. The appearance of bluish discoloration of the overlying skin due to reaction of starch and iodine in the presence of moisture (sweat.

How do you treat Frey’s syndrome? Although frey’s syndrome is usually a minor problem, it may require treatment which include: 1. Parasymphatholytic creams such as glycopyrrolate lotion may also be applied to the skin or scopolamine cream 3%. 2. Apply anti-perspirant to avoid sweating. 3. Jacobsen’s neurectomy via tympanotomy approach. 4. Elevating skin flap and placing tissue such as fascia, dermis, or creating SCM muscle flap and if there is a big defect you can use regional flap as a PMMF.

Facial nerve paralysis In parotid malignancy a. Patient with clinically pre-op facial nerve paralysis. What to do? Intra-operative resection of the involved part of the facial nerve and primary grafting using greater auricular nerve or sural nerve. Post-operative radiotherapy (high-grade)

b. Patient with a normal facial function but intra-operative involvement of the facial nerve. What to do? Careful dissection of the tumor of the facial nerve without sacrifying the facial nerve and followed-up with radiotherapy treatment.

During an operation on the parotid, where do you find the facial nerve?

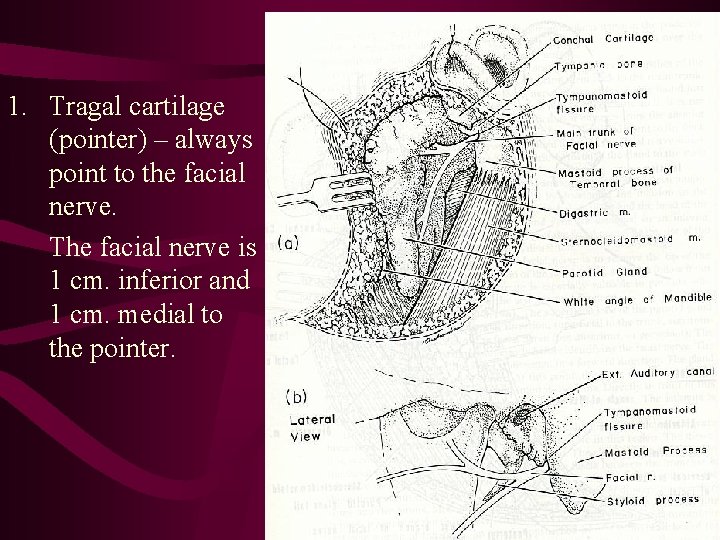
1. Tragal cartilage (pointer) – always point to the facial nerve. The facial nerve is 1 cm. inferior and 1 cm. medial to the pointer.

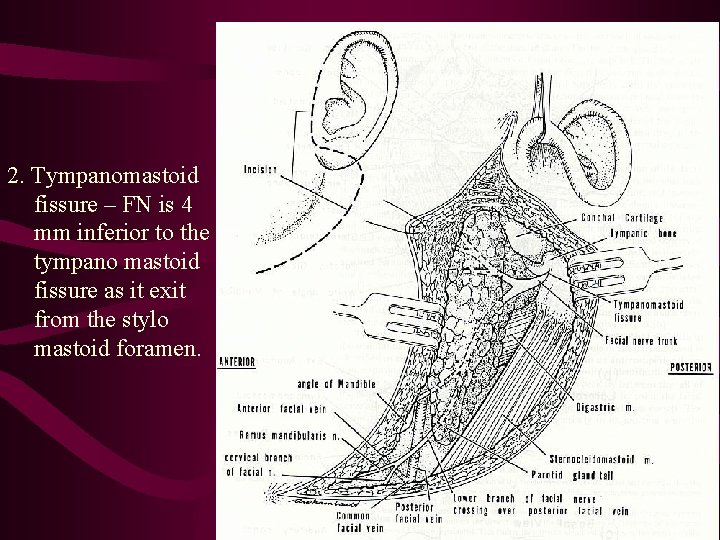
2. Tympanomastoid fissure – FN is 4 mm inferior to the tympano mastoid fissure as it exit from the stylo mastoid foramen.

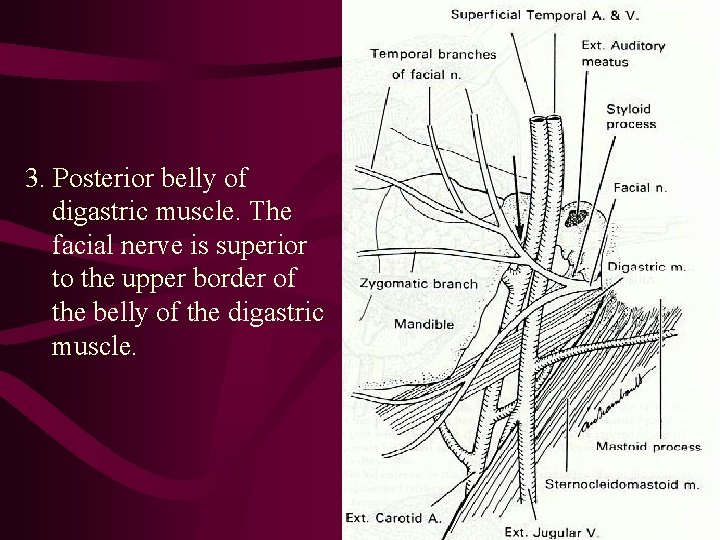
3. Posterior belly of digastric muscle. The facial nerve is superior to the upper border of the belly of the digastric muscle.

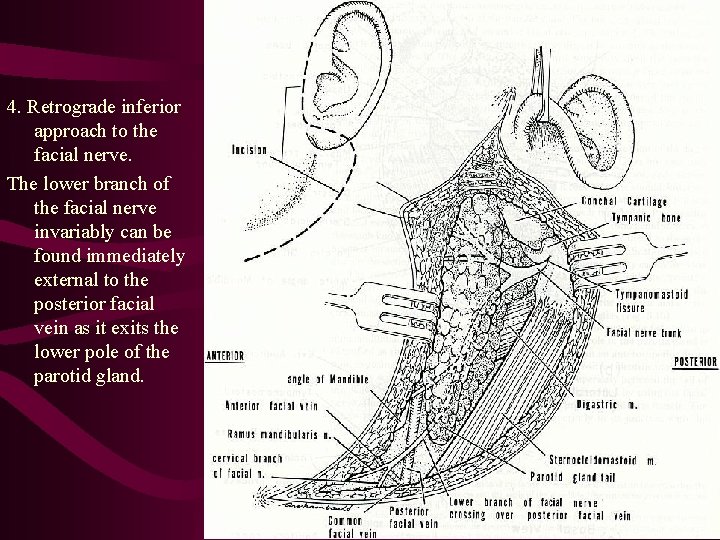
4. Retrograde inferior approach to the facial nerve. The lower branch of the facial nerve invariably can be found immediately external to the posterior facial vein as it exits the lower pole of the parotid gland.

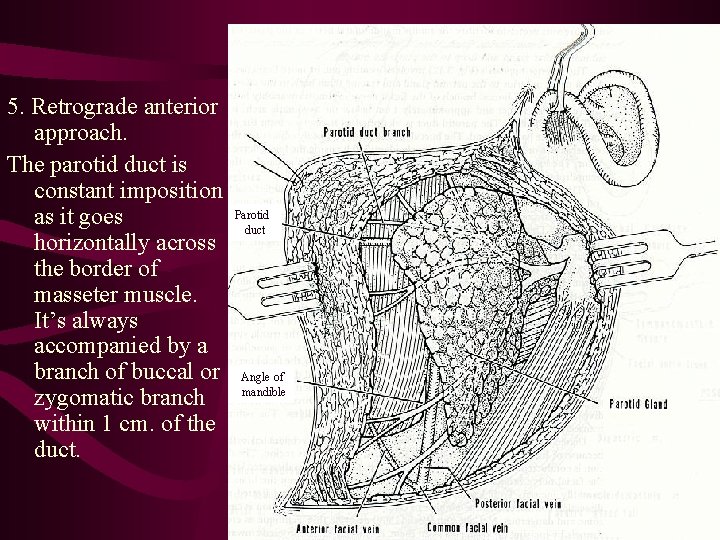
5. Retrograde anterior approach. The parotid duct is constant imposition as it goes horizontally across the border of masseter muscle. It’s always accompanied by a branch of buccal or zygomatic branch within 1 cm. of the duct. Parotid duct Angle of mandible

Does the grading make difference in management of the parotid malignancy?

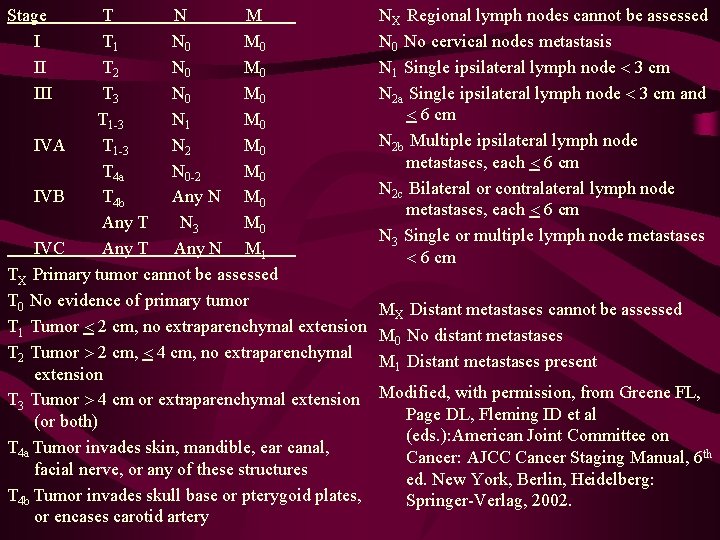
Stage I II III T N M T 1 N 0 M 0 T 2 N 0 M 0 T 3 N 0 M 0 T 1 -3 N 1 M 0 IVA T 1 -3 N 2 M 0 T 4 a N 0 -2 M 0 IVB T 4 b Any N M 0 Any T N 3 M 0 IVC Any T Any N M 1 TX Primary tumor cannot be assessed T 0 No evidence of primary tumor T 1 Tumor 2 cm, no extraparenchymal extension T 2 Tumor 2 cm, 4 cm, no extraparenchymal extension T 3 Tumor 4 cm or extraparenchymal extension (or both) T 4 a Tumor invades skin, mandible, ear canal, facial nerve, or any of these structures T 4 b Tumor invades skull base or pterygoid plates, or encases carotid artery NX Regional lymph nodes cannot be assessed N 0 No cervical nodes metastasis N 1 Single ipsilateral lymph node 3 cm N 2 a Single ipsilateral lymph node 3 cm and 6 cm N 2 b Multiple ipsilateral lymph node metastases, each 6 cm N 2 c Bilateral or contralateral lymph node metastases, each 6 cm N 3 Single or multiple lymph node metastases 6 cm MX Distant metastases cannot be assessed M 0 No distant metastases M 1 Distant metastases present Modified, with permission, from Greene FL, Page DL, Fleming ID et al (eds. ): American Joint Committee on Cancer: AJCC Cancer Staging Manual, 6 th ed. New York, Berlin, Heidelberg: Springer-Verlag, 2002.

Group 1: T 1 and T 2 NO low-grade malignancy Treatment is excision of the tumor with cuff of a normal tissue. Facial nerve is preserved. Regional lymph node evaluated at the time of surgery. No post-op radio therapy unless the resection margin is not clear.

Group 2: T 1 and T 2 NO high-grade malignancy Treatment is total parotidectomy with excision of the first echolon node (digastric and submandibular nodes). Facial nerve involvement: a. patient with facial paralysis pre-operatively. Resection of the facial nerve with primary grafting. b. patient with normal facial function pre-op. Resect the tumor of the facial and post-operative wide field radiation.

Group 3: T 3 NO or any N+ high-grade or recurrent cancer. Treatment is total parotidectomy Modified radical neck dissection Post-operative wide field radiotherapy Facial nerve as in group 2

Group 4: include all T 4 tumor Treatment is radical parotidectomy with modified radical neck dissection and resection of masseter muscle, part of the mandible or mastoid or ear canal as required. Resection of the facial nerve with the tumor and primary grafting. Followed by wide field post-operative radiotheray.

Points to remember in parotid surgery: 1. Pre-op evaluation: general condition of the patient, hemoglobin, LFT and U & E’s 2. Consenting patients for possible facial weakness. 3. Operating in bloodless field by: a. hypotensive technique b. elevation of the head of the bed c. delicate tissue handling d. proper hemostasis

4. Using facial nerve monitoring during operation and at the end of operation. 5. Exposure of the eye and the operative side of the face. 6. Modified blair incision. 7. Landmark for the facial nerve.

Indications of neck dissection 1. Neck dissection is a recommended treatment of the neck for the malignant salivary gland tumor, when? 2. If there is a clinically cervical adenopathies (15%). Parotid tumor bigger than 4 cm, why? (the risk of occult metastasis over 20%). 3. High grade malignancy, why? (the risk of occult metastasis over 25%).

Indications of post-operative radiotherapy 1. 2. 3. 4. 5. 6. 7. 8. High-grade tumor Gross or microscopic residual disease Tumor involving or close to the facial nerve Recurrent disease Documented lymph node metastasis Extraparotid extension Deep lobe cancers All T 3 and T 4 cancers