Salford Malnutrition Taskforce Tony Ward Community Dietitian Salford




































- Slides: 50

Salford Malnutrition Taskforce Tony Ward Community Dietitian Salford Royal NHS Foundation Trust Salford CCG

Salford Malnutrition Taskforce • A multi-agency steering group is working together to reduce the prevalence of preventable malnutrition and dehydration in Salford. Formed 5 years ago under the auspices of the national pilot in partnership with Age UK.

Disease Related Malnutrition (DRM) • 10 -14% of the 65+ population is at risk of malnutrition, 93% of those at risk of malnutrition are in the community. Dehydration in older adults is associated with hospitalization and higher health and care costs. • DRM costs £ 29. 5 Billion in the UK.

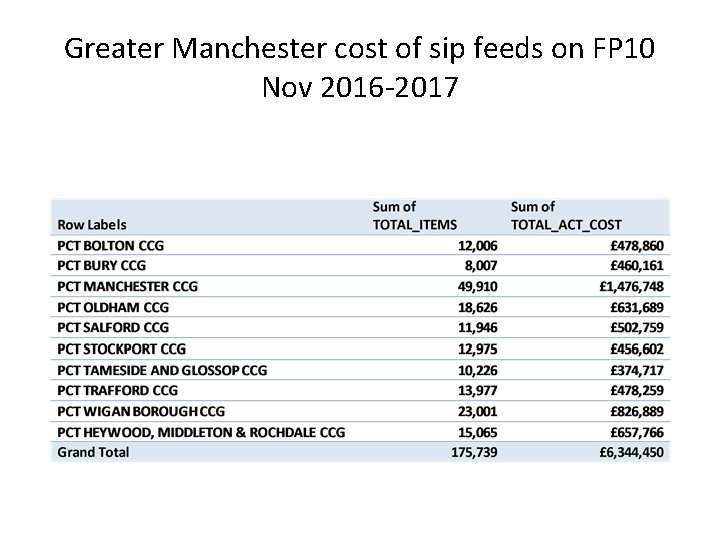
Greater Manchester cost of sip feeds on FP 10 Nov 2016 -2017



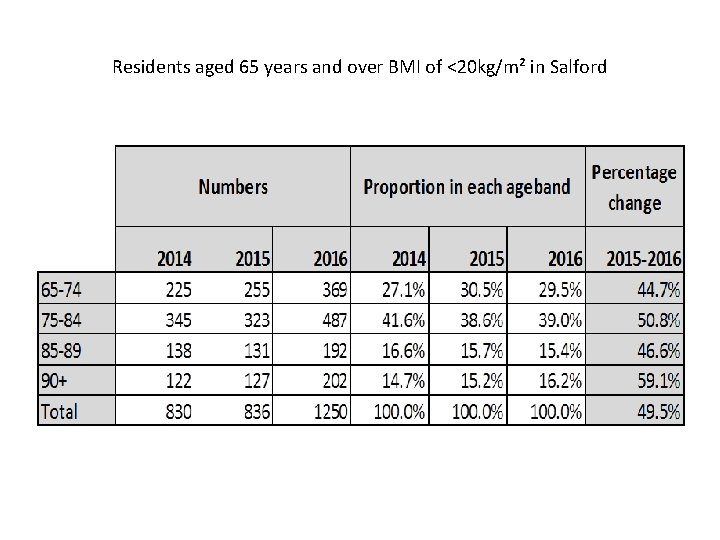
Residents aged 65 years and over BMI of <20 kg/m² in Salford

Task Force Achievements Raising Awareness • Fridge magnets, posters, leaflets and Quizzes • 2 awareness events • Supermarket tours • 1425 people reached • Impact – £ 300, 000 saved in supplements – Reduction in malnutrition related hospital admissions – 50% increase in reporting underweight BMI – Dash board created to malnutrition screening

Paperweight Armband, • a simple, non-clinical tool to identify malnutrition and has promoted its use across the community in Salford. Signpost early identification of malnutrition, • empowered non-clinical staff and volunteers to talk to older people about nutrition and raised awareness of how to eat well in later life https: //www. ageuk. org. uk/salford /about-us/improving-nutrition-and -hydration/the-paperweightarmband/

E-Learning Package • An e-learning package • Covering malnutrition and dysphagia. • Designed initially for hospital staff, • Adapted to make it accessible for community staff, Care home staff, volunteers and carers. http: //paperweightarmband. org. uk/

Innovation Bids • EAU (Emergency Admission unit) Project • Kafoodle • Speech and Language – Dysphagia Champions

I hope you all in enjoy the day Thank you

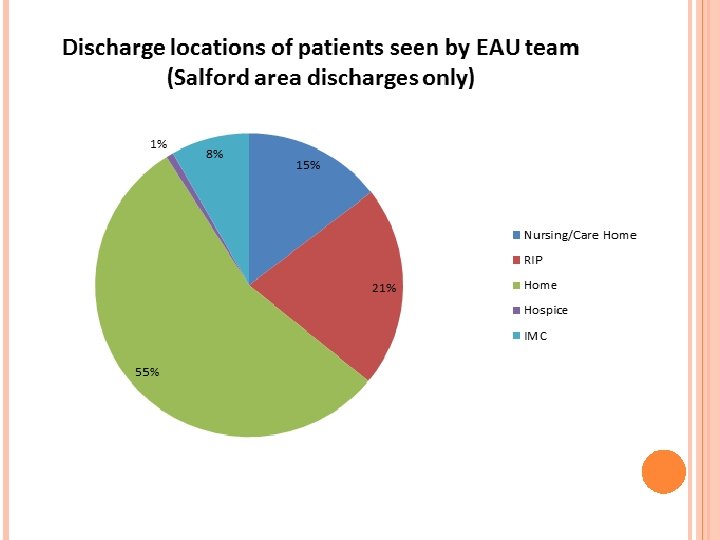
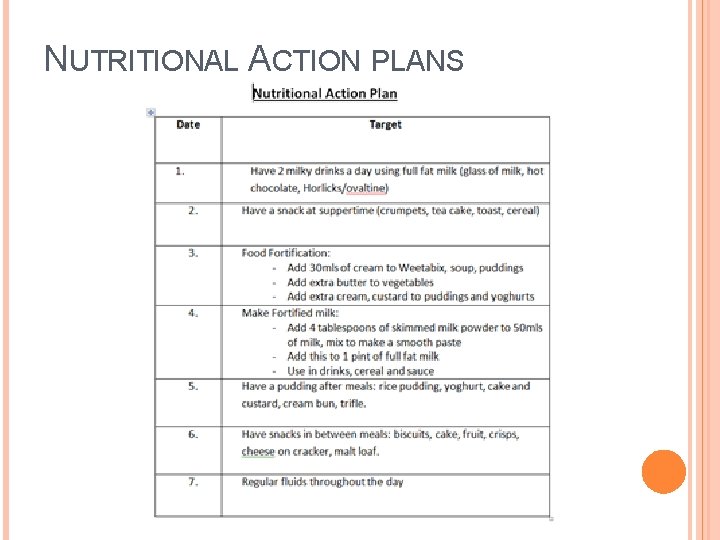
EAU INNOVATION PROJECT Nutritional Action Plans and Discharge

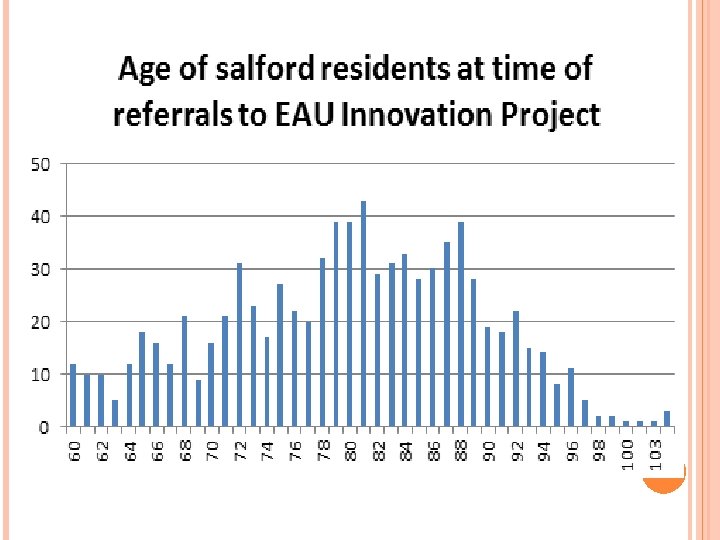
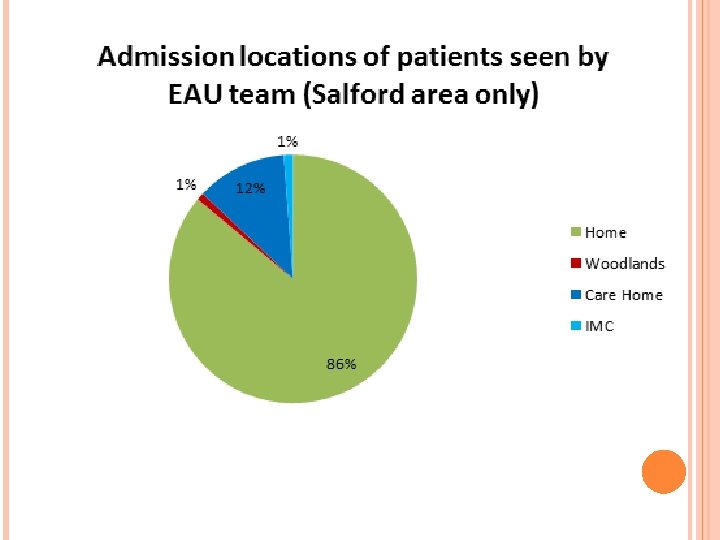
WHY DID WE SET UP THE PROJECT? People are living longer The longer people live, the more at risk of malnutrition they are Weight loss is not a normal part of ageing Innovation project was set up to support these individuals and look at what type of individuals we were engaging with.




Care homes have the opportunity to support the message that weight loss is not a normal part of aging Care homes are a unique place to identify people who are at risk, put in a plan, support them and help them.

NUTRITIONAL ACTION PLANS

ANY QUESTIONS?

Kafoodle Innovation Project Digitising Menus Revolutionising Nutrition in Health Care Tony Ward – Senior Dietitian Salford Royal NHS Foundation Trust

Salford CCG innovation bid: • 1 year project • Originally across 4 nursing homes • Total 162 beds The problem: • High referrals to dietetics • High usage of nutritional supplements £ 74114. 06/year 2017 • Hospital admissions from Care homes – total: 631 in 2018, average 53/month. • CQC inadequate homes 2 nd highest in UK The Bid

Driver diagram

Project aims: 1. To assess baseline data on nutritional status of care residences in 4 nursing homes. 2. Reduce dietetic high ‘MUST’ referrals by >10% in 9 months in 4 care homes by optimising the menu. 3. Ensure appropriate prescribing of supplements. 4. Ensure the nutritional values of meals are appropriate and adequate, while increasing efficiency in documentation, budgeting and meal planning. The Project

The reality: • • Different consistencies (IDDSI) and allergens. Managing food wastage. Ensuring nutritionally complete. Adapting meals to maintain a healthy weight or controlling diabetes. Catering for different choices/culture difference/religious beliefs. Catering for dementia. Managing stock and incorrect deliveries. Managing budgets. All can have an impact on the quality of life of a resident The Reality

Safeguarding residents and the care homes • • • Care home recipes were not documented Allergens were not clearly documented Nutritional content of meals was not recorded There was confusion over food fortification No consistency with allergens/nutrition/budget due to constantly changing recipes • No official guidelines for consistencies for individualised recipes and no guidelines to check if correct (IDDSI) • Over estimation of portions to ensure availability of choice is increasing wastage and cost • Premade meals v homemade meal – choice, cost, adaptability Safeguarding

Kafoodle Kitchen • All recipes will be recorded, analysed and costed - these can be printed off as a recipe card. • Recipes – are costed per portion and per batch. • Nutritional and allergen breakdown of the recipes. • Instructions can be recorded on the recipes to ensure they are made to the correct consistencies. • Provides a complete bank of recipes which can be organised by meal time for consistency. • Guidance of constancies of meals Kafoodle Meal planning • Build a meal plan that meets the nutritional requirements of all diners • Lets you know if you are in budget. • Alerts if a residents’ needs are not met. • Develop and save seasonal meal cycles, or those for a special day (Christmas etc. ) How can Kafoodle help?

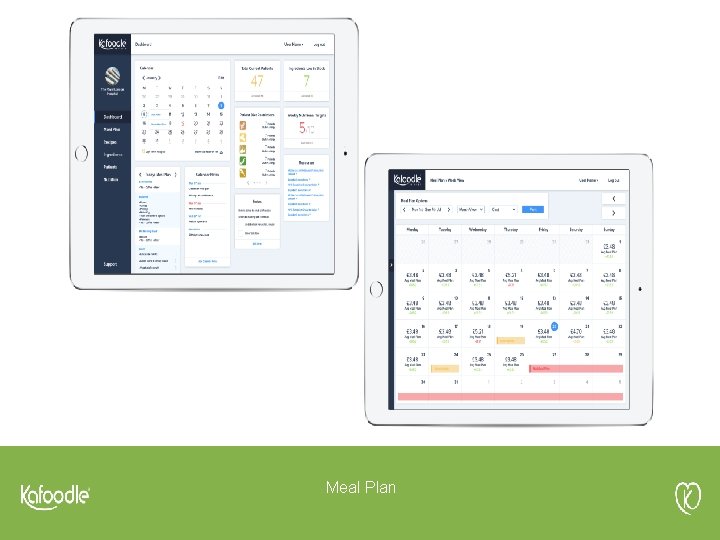
The Kafoodle Home Screen

Manage Ingredients

Store recipes

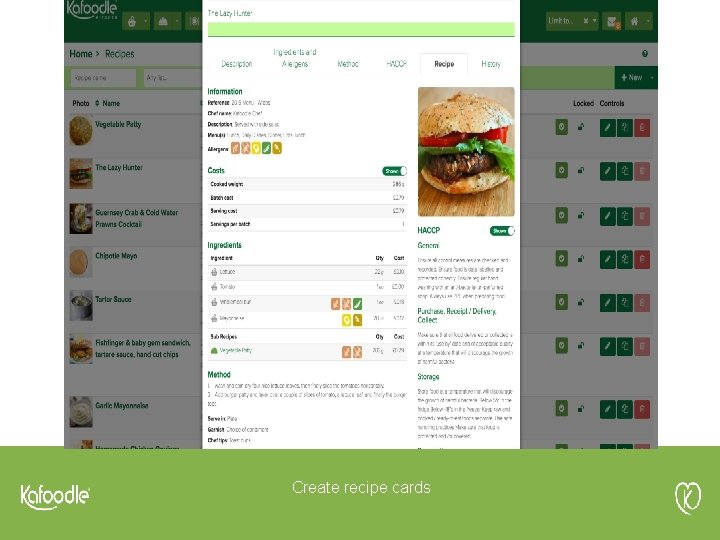
Create recipe cards

Meal Plan

With the Kafoodle software care homes are able to: • • • Improve the transparency of their nutrition and budgeting Meet CQC criteria reg 14 Meet food allergy legislation Save time and money Improve their service and reputation Kafoodle

e. PMO – electronic Personalised Meal Ordering • • • Record and monitor the intake of both food and beverages Save time Filter dishes by allergens, nutrition, medical condition or preference Track meals from order to delivery Set meal ordering times to as little as every half hour Record food temperature at various stages of production Refer to red, amber and green alerts Capture data and feedback for menu development Connect to live stock levels Residents can view images of the dishes they are selecting e. PMO

Dietitians remote input • Intake review • Meal plans can be changed Speech and Language Therapy • Change consistencies real time • IDDSI The future

Thank you I will now take any questions?

Dysphagia Care Home Champions Innovation Susanna Cox – Speech and Language Therapist April 2019

� Changing Why? population � Studies have shown that up to 60% of residents in care homes will have difficulties eating and drinking � Poor access to staff training and education affecting quality of management � Consequence can be patients are fed with unsafe diet and fluids increasing risk of choking, aspiration pneumonia and possible admission to hospital � Increased focus on safe swallowing from CQC

Focus for Dysphagia Champions 1. 2. 3. Introduction and establishment of IDDSI Establishment and confidence of supporting patients who are Risk Feeding Develop a risk assessment and support package for feeding residents with dysphagia


Case Study – Jane Olive Parker 1. What things can you identify that went wrong in this resident’s case? 2. What can we learn from this?

� “She should have been on a special diet of soft and pureed food…” � “she should have what was known as a 'stage three diet' - consisting only of semi-solid, soft or pureed food that could easily be digested” � “…a decision was made not to assess her directly but rely on a previous care plan” � “No new care plan was put in place and the transferred plan from Millbrook omitted any previous choking episodes, wrongly stating she could eat 'stage four foods” � “Served in her bedroom rather than in the dining area, she chose chicken was left unsupervised to eat”

IDDSI – What is it? International Dysphagia Diet Standardisation Initiative

Risk feeding protocol � Poor awareness in care homes with risk feeding � Seen as an easy option by care homes � May use terminology inappropriately � Protocol not communicated and resident given inappropriate foods/fluids � Over reliance on SLT and inappropriate referrals to the service � Advanced Care Planning may be missed � Unnecessary hospital admissions

Benefits if correctly implemented � Supporting residents in decision making regarding risk feeding � Improved Quality of Life for residents � Reduce unnecessary hospital admissions � Improved End of Life Care � Reduced inappropriate referrals to speech and language therapy

Our proposal � Identify 12 care homes based on residents with highest numbers prescribed thickener and highest referrers to SLT service � Identify 2 senior members of staff for each care home to be dysphagia care homes champions � Develop training package and resources � Roll out to identified care homes and evaluate

Any Questions? �Adult Community SALT team Tel: 0161 206 2333 �We take phone referrals / answer queries on the above number between 1 -3. 30 pm every week day �susanna. cox@srft. nhs. uk

Measuring success � Baseline number of hospital admissions from care homes with risk feeding protocol in place and repeat at end of project � Number of care homes identified and numbers of staff trained � Qualitative measure of staff confidence in understanding and managing dysphagia and understanding of risk feeding protocol – completed at baseline and at end of project � No of staff who have accessed Malnutrition and Swallowing Difficulties e-Learning

Measuring success All care homes will have written information and resources for relatives Evidence of paperwork and pathways in care plans –risk feeding, risk assessment for relatives feeding residents with dysphagia and discussions re advanced care planning Evidence of documentation in care plans/food and fluid charts with IDDSI descriptions for patients with dysphagia All care home staff are able to answer questions relevant to IDDSI descriptors and risk feeding when asked (through spot checks, questionnaires and interviews)

Maintaining success � Resource pack available for additional individual care homes requiring training for dysphagia champions � Community SLT team able to provide training to individual additional care homes within current staffing resources once project has finished � Able to provide ongoing dysphagia champion link meetings on biannual basis to all trained champions for updates once project has finished