Safety Planning Intervention for Suicide Prevention Barbara Stanley

Safety Planning Intervention for Suicide Prevention Barbara Stanley, Ph. D. Yael Holoshitz, MD

Suicide: The Facts �Every day, approximately 90 Americans take their own life � 10, 000 more people die by suicide in the US than by homicide each year Centers for Disease Control and Prevention (CDC) Data & Statistics Fatal Injury Report for 2014

Scope of the Problem

Who Dies by Suicide? In 2013… � 41, 149 suicides were reported (In 2014, the number and rate increased 42, 773; 12. 93/100, 000) �the highest suicide rate (19. 1 per 100, 000) was among people 45 -64 years old �the suicide rate among adolescents and young adults aged 15 -24 was 10. 9 per 100, 000 � 0 f those who died by suicide, 77. 9% were male Centers for Disease Control and Prevention (CDC) Data & Statistics Fatal Injury Report for 2013
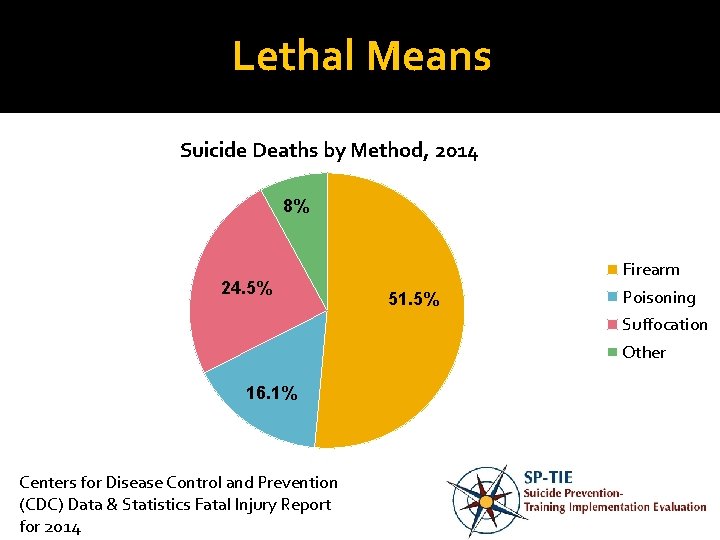
Lethal Means Suicide Deaths by Method, 2014 8% 24. 5% Firearm 51. 5% Poisoning Suffocation Other 16. 1% Centers for Disease Control and Prevention (CDC) Data & Statistics Fatal Injury Report for 2014

Risk Factors for Suicide � Psychiatric Disorders: At least 90% of people who kill themselves have a diagnosable psychiatric illness: Major depression Bipolar depression Schizophrenia Alcohol or other substance abuse Posttraumatic Stress Disorder Borderline Personality Disorder Eating Disorders

Risk Factors for Suicide �Past History of Attempted Suicide Between 20 -50 percent of people who die by suicide had previously attempted suicide. Those who have made serious suicide attempts are at much higher risk for death by suicide �Familial/Genetic Predisposition Familial history of suicide, suicide attempts, depression or other psychiatric illness

Suicide Attempts � For every suicide death, 3 -10 suicide attempts � About 2, 300 people in the US attempt suicide daily; this may be an underestimate � Many attempts never come to mental health professional or physician attention � Suicide attempts are the strongest known risk factor for suicide � Non-suicidal self injury places individuals at risk for suicidal behavior National Survey on Drug Use and Health 2013
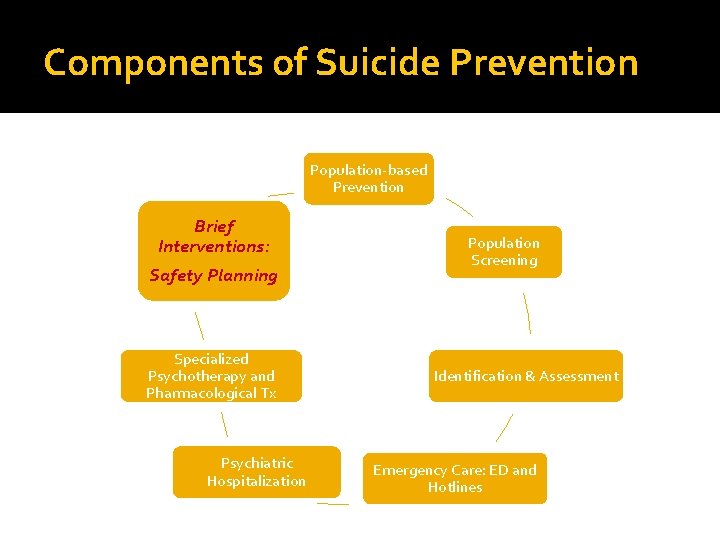
Components of Suicide Prevention Population-based Prevention Brief Interventions: Safety Planning Specialized Psychotherapy and Pharmacological Tx Psychiatric Hospitalization Population Screening Identification & Assessment Emergency Care: ED and Hotlines

What is a Brief Intervention? �A tool for use when contact is limited �Single session or several sessions �Teaching, informing, educating �Planning for future crises �Therapeutic Encounter �Outreach, follow-up (phone calls, letters, texts)

Why Use a Brief Intervention? Empirically Supported Psychotherapies and yet no decrease in suicide rate (WISQARS, 2012) We don’t always have the opportunity to engage outpatients in treatment.

Obstacles to outpatient treatment engagement �At risk individuals are difficult to engage in outpatient psychotherapy (Lizardi & Stanley, 2010; Trusz, et al. , 2011) � 11 -50% attempters refuse or drop out �Of those that attend treatment, 3 months following attempt, 38% have stopped (Monti et al. , 2003) �After a year, 73% of attempters will no longer be in any treatment (Krull & Hales 1988)

What is the Safety Plan Intervention (SPI)? � SPI is a clinical intervention that results in development of a one-page document to use when a suicidal crisis is emerging. �The individual at risk completes the SPI with the help of a clinician. � Suicide risk fluctuates over time and SPI is a plan for managing and decreasing suicidal feelings and for staying safe when these feelings emerge � Can be done in one brief session and refined over time.
Risk fluctuates over time RISK Danger of acting on suicidal feelings TIME

Tangible + Concrete Plan
SPI: Goal is Twofold Safety Planning Intervention (SPI) Reduce suicide risk Increase treatment motivation

How the SPI Was Developed �Developed to maintain safety of high-risk patients in outpatient treatment studies (Penn CT study; TASA study) �Borrows certain aspects of evidence-based suicide interventions �Later expanded for stand-alone intervention in VA and civilian ERs �Now identified as a Best Practice in the SPRCAFSP Registry of Best Practices/SP

SPI: Who is it for? �Individuals at increased risk but not imminently dangerous, i. e. in need of immediate rescue �Factors that increase risk: Past suicide attempt, psychiatric disorders (mood, psychosis), substance use, male gender, family history of suicide, chronic pain, access to lethal means, history of trauma, current suicidal ideation

Use of SPI During Crisis Contact �Crisis contact may be the ONLY contact a suicidal individual has with the mental health system. �Using the SPI during crisis contact can increase therapeutic capacity of the contact. �Sentinel event/teachable moment (Boudreaux, 2012): “strike while the iron is hot”
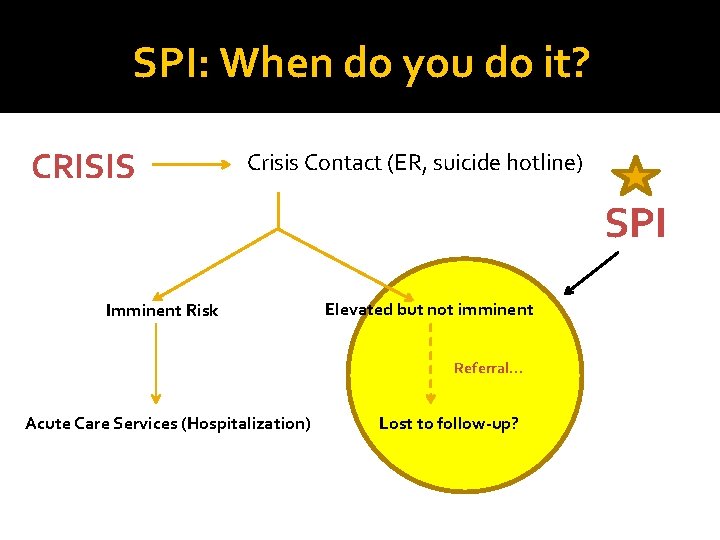
SPI: When do you do it? CRISIS Crisis Contact (ER, suicide hotline) SPI Imminent Risk Elevated but not imminent Referral… Acute Care Services (Hospitalization) Lost to follow-up?

Theoretical Foundation of SPI 1. 2. Suicide Risk Fluctuates with Time Problem solving capacity diminishes during crisis so over-practice with a specific template can help coping. Parallel to STOP-DROP-ROLL for fire safety. 3. Clinician and suicidal individual collaborate to determine cognitive and behavioral strategies to use during suicidal crises

Evidence-Based Risk Reduction Strategies �Means Restriction �Brief problem solving and coping skills (including distraction) �Enhancing social support, identifying emergency contacts �Motivational Enhancement for further treatment

Real-Time Intervention Contrast the Urgent Care Patient with a Suicide Attempt and the ED patient with a Fracture…

Real-Time Intervention SPI for suicidal ideation is equivalent to placing a cast on a fracture… Provides immediate Intervention and fills the gap between ER discharge and follow-up

SPI: An Overview �Creates a tool for participants to use in distress: step-wise increase in level of intervention Starts “within self” and builds to seeking help in the psychiatric emergency room �Plan is step-wise but individual can advance in steps without “completing” previous step… �SPI can be done in one brief session and altered over time

The SPI is NOT: �NOT a substitute for treatment �NOT help for an individual in imminent danger of attempting suicide �NOT a “no-suicide contract” Avoid “no-suicide contracts”– all this does is ask patients to promise to stay alive without telling them HOW or giving them the resources to cope

SPI: In Their Own Words… “I think it is very helpful, especially with people going through depression, with showing you and telling you how to use different coping skills…” “It hadn’t occurred to me before that I could do something about my suicidal feelings” Stanley et al. (2015) Psychiatric Services.

How Do We Begin? Lay down the foundation for safety planning by inviting the individual to tell the story of their suicide attempt or suicidal crisis.

Telling the Story �Beginning of the story When was the major decision point associated with suicide crisis/attempt/risk? What was the strong emotional reaction to a specific event (either external or internal) Follow backward in time �Suicidal individual should describe events and situations, as well as reactions to events, in as much detail as possible.

Allows clinician to… �Understand the function of suicidal behavior and thinking from the individual’s perspective �Empathize with strong feelings and desire to reduce distress �Refrain from immediate problem-solving without understanding the details and motivation for the suicide

SPI: The Details

Overview of SPI: 6 Steps 1. 2. 3. 4. 5. 6. Recognizing warning signs Employing internal coping strategies (without contacting another person) Socializing with others as a way of distraction Contacting family members or friends to help resolve crisis Contacting mental health professionals/agencies Reducing potential for use of lethal means

Clinical approach to the SPI � Thoughts, emotions, behavior, physical sensation, external cue � Clinician guides the patient through these 6 steps � Collaborative approach � Guides patient in generating their own ideas � Clinician refrains from giving patient ideas until they have had a chance to generate their own � Balance collaboration with directive approach to complete the 6 steps. � Include identification of obstacles to carrying out the steps and problem solving around them

Step 1: Recognize Early Warning Signs �Ask… “What do you experience when you start to think about suicide or feel extremely distressed? ” �Write down warning signs in individual’s own words… Thoughts, emotions, behavior, physical sensation, external cue
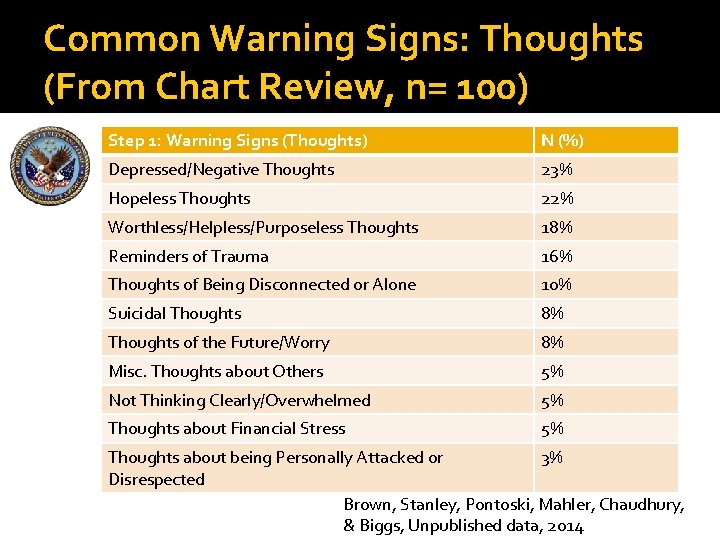
Common Warning Signs: Thoughts (From Chart Review, n= 100) Step 1: Warning Signs (Thoughts) N (%) Depressed/Negative Thoughts 23% Hopeless Thoughts 22% Worthless/Helpless/Purposeless Thoughts 18% Reminders of Trauma 16% Thoughts of Being Disconnected or Alone 10% Suicidal Thoughts 8% Thoughts of the Future/Worry 8% Misc. Thoughts about Others 5% Not Thinking Clearly/Overwhelmed 5% Thoughts about Financial Stress 5% Thoughts about being Personally Attacked or 3% Disrespected Brown, Stanley, Pontoski, Mahler, Chaudhury, & Biggs, Unpublished data, 2014
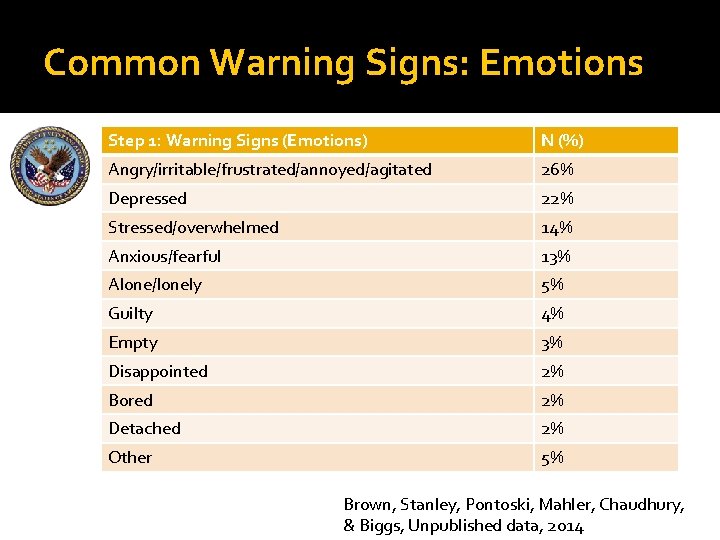
Common Warning Signs: Emotions Step 1: Warning Signs (Emotions) N (%) Angry/irritable/frustrated/annoyed/agitated 26% Depressed 22% Stressed/overwhelmed 14% Anxious/fearful 13% Alone/lonely 5% Guilty 4% Empty 3% Disappointed 2% Bored 2% Detached 2% Other 5% Brown, Stanley, Pontoski, Mahler, Chaudhury, & Biggs, Unpublished data, 2014
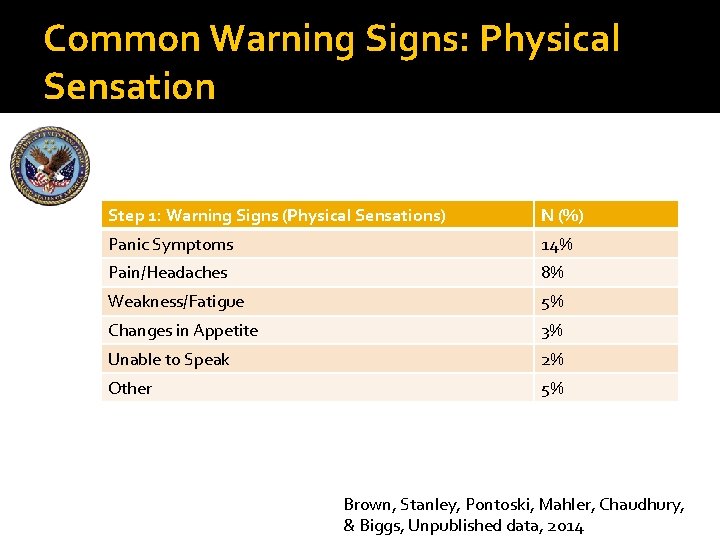
Common Warning Signs: Physical Sensation Step 1: Warning Signs (Physical Sensations) N (%) Panic Symptoms 14% Pain/Headaches 8% Weakness/Fatigue 5% Changes in Appetite 3% Unable to Speak 2% Other 5% Brown, Stanley, Pontoski, Mahler, Chaudhury, & Biggs, Unpublished data, 2014
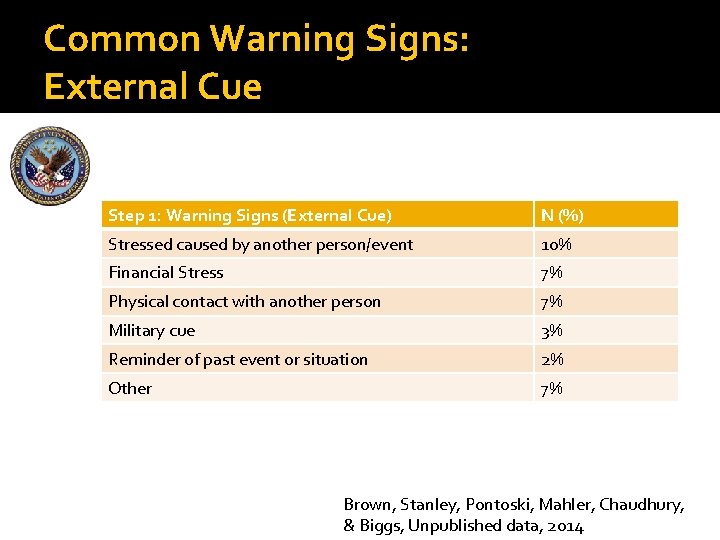
Common Warning Signs: External Cue Step 1: Warning Signs (External Cue) N (%) Stressed caused by another person/event 10% Financial Stress 7% Physical contact with another person 7% Military cue 3% Reminder of past event or situation 2% Other 7% Brown, Stanley, Pontoski, Mahler, Chaudhury, & Biggs, Unpublished data, 2014

Step 2: Internal Coping Strategies �Activities that an individual can do without contacting another person �Help refocus/distract; take their mind off problems; regulate emotions and reduce distress �May prevent suicidal ideation from escalating

Step 2: Internal Coping Strategies Ask… “What can you do, on your own, if you become suicidal again, to help yourself not act on your thoughts and urges? ”

Step 2: Internal Coping Strategies Coping with suicidal feelings alone, even briefly, can enhance self-efficacy, selfreliance and sense of power over suicidal urges.

Step 2: Internal Coping Strategies Examples: Watching TV/movies Taking a walk Listening to music Exercising Playing video games Reading Praying/medication Doing house chores Involvement in creative pursuits Self-care/self-soothing; Spending time with pets/animal Looking at photos of loved ones, etc…

Step 3: Socialization �Use if Step 2 does not resolve crisis �Socialization for distraction/support, to “take your mind off our problems” �Suicidal thoughts not revealed at this step �Two options: “healthy” social setting (coffee shop, park) Family, friends, acquaintances for support/distraction

Step 3: Socialization Ask… “Who helps you take your mind off your problems- at least for a little while? ” “Who do you enjoy socializing with? ” “Where do you think you could go that is a healthy environment for social interaction? ” “Are there places or groups that you can to take your mind off your problems? ”

Step 3: Socialization �Emphasize healthy settings (e. g. not usually neighborhood bar…) such as: bookstore, coffee shop, gym, park, shopping mall, theater, place of worship �List several people to contact, for back-ups family member, friend, roommate, neighbor, spouse, NA/AA sponsor, religious person
Step 4: Friends/Family for Support �If Step 3 does not resolve crisis/lower risk �Help individuals rely on their natural environment �Ask if safety plan can be shared with family �Identify potential obstacles, problem-solve ways to overcome them

Step 4: Friends/Family for Support Ask… “Who are the people you can call to reveal your suicidal feelings? ” “How willing would you be to contact the friends and family on this list? ” “What are some potential barriers and how we work through them beforehand? ” can

Step 5: Professionals/Agency �If Step 4 does not resolve crisis or lower risk �Clinicians or agencies to turn to for help during crisis �List names, numbers, locations of: Clinicians Local ER or other emergency services Suicide Prevention Hotline 800 -273 -TALK (8255)

Step 6: Reducing the Potential for Use of Lethal Means �Last step of safety planning intervention Rationale: after completing the SPI, the individual is more likely to have a sense of alternatives to suicidal behavior, and therefore more likely to discuss means restriction…

Step 6: Reducing the Potential for Use of Lethal Means �Ask what means they would consider during suicidal crisis (pills, sharps, firearm) �ALWAYS ask about access to firearm, even if they do not mention this
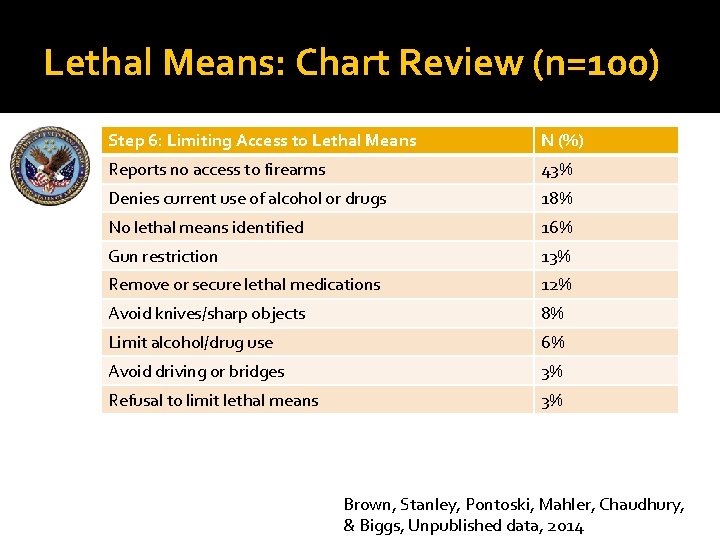
Lethal Means: Chart Review (n=100) Step 6: Limiting Access to Lethal Means N (%) Reports no access to firearms 43% Denies current use of alcohol or drugs 18% No lethal means identified 16% Gun restriction 13% Remove or secure lethal medications 12% Avoid knives/sharp objects 8% Limit alcohol/drug use 6% Avoid driving or bridges 3% Refusal to limit lethal means 3% Brown, Stanley, Pontoski, Mahler, Chaudhury, & Biggs, Unpublished data, 2014

Implementation: Likeliness of Use? Ask… “Where will you keep your safety plan? ” “How will you remember that you have a safety plan when you are in crisis? ” “How likely is it that you will use the safety plan when you notice warning signs? ” “How can you fight the urge, if present, to not try to help yourself? ”
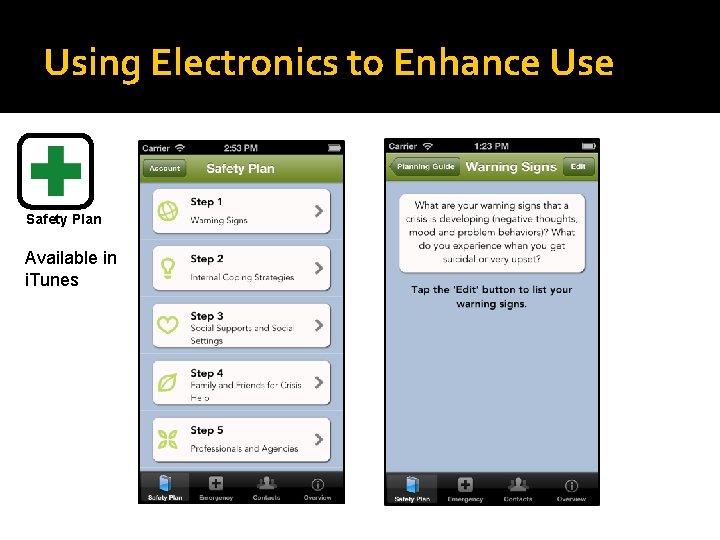
Using Electronics to Enhance Use Safety Plan Available in i. Tunes

Effectiveness of SPI � 100 moderate-risk veterans were given the SPI in VA Emergency Departments. Followup interview 3 months to 2 years post-visit… All remembered SPI done in the ED All could say where their plan was currently 91% felt that the safety plan was very helpful in making them feel connected to and cared for at the VA High Satisfaction with the SPI Stanley et al. (2015) Psychiatric Services.

SPI: In Their Own Words… “Gave me the opportunity to more clearly define signs, when my mood is beginning to deteriorate and when to start taking steps to prevent further worsening…” “How has the safety plan helped me? It has saved my life more than once…” Stanley & Brown (2015). Psychiatric Services .

Resources � Stanley B & Brown GK, A Brief Intervention to Mitigate Suicide Risk. Cognitive and Behavioral Practice, 19: 2, May 2012, 256 -64. � Safety planning in the VA (Stanley & Brown VA Safety Planning Manual, 2008). � SPI designated as a Best Practice by the SPRC/AFSP Registry of Best Practices for Suicide Prevention. � Safety Plan Template: www. suicidesafetyplan. com.

Resources �http: //practiceinnovations. org/Initiatives/Suic ide-Prevention Links to archived webinars on the Safety Planning Intervention
- Slides: 57