Safety Hygiene B 260 Fundamentals of Nursing Cindy

Safety & Hygiene B 260: Fundamentals of Nursing Cindy Bemis MSN, RN, NE-BC

Concept: Safety • Safety is often defined as freedom from psychological and physical injury. Safety refers to the prevention of patient injury caused by health care errors. • The QSEN safety competency for a nurse is defined as “Minimizes risk of harm to patients and providers through both system effectiveness and individual performance. ”

TO ERR IS HUMAN: BUILDING A SAFER HEALTH SYSTEM • Health care in the United States is not as safe as it should be--and can be. At least 44, 000 people, and perhaps as many as 98, 000 people, die in hospitals each year as a result of medical errors that could have been prevented, according to estimates from two major studies. Even using the lower estimate, preventable medical errors in hospitals exceed attributable deaths to such feared threats as motor-vehicle wrecks, breast cancer, and AIDS.

BUILDING A SAFER HEALTH SYSTEM • Medical errors can be defined as the failure of a planned action to be completed as intended or the use of a wrong plan to achieve an aim. Among the problems that commonly occur during the course of providing health care are: adverse drug events and improper transfusions, surgical injuries and wrong-site surgery, suicides, restraint-related injuries or death, falls, burns, pressure ulcers, and mistaken patient identities. • Published Nov. 1999

Patient Identification • FIRST and best way to identify for the RIGHT patient is to have them STATE their name and birthday. • SECOND is to check the name bracelet. • BOTH of these should be done prior to any patient contact • Bar Scan when giving medications/drawing blood, where available

FALLS • A patient fall, defined as a sudden, unintentional change in position, coming to rest on the ground or other lower level, is among the most commonly reported adverse hospital events, with more than 1 million occurring annually. MORE THAN 1 MILLION FALLS OCCUR EVERY YEAR

FALLS • Approximately 30% of falls result in some type of injury, and 10% result in serious injury, such as head trauma and fracture. Among older adults, falls are especially dangerous because of their increased causation of morbidity and mortality.

Fall Assessment Tools • Assessment of a patient’s risk factors for falling is essential in determining specific needs and developing targeted interventions to prevent falls. – Morse Fall Scale: used at Community Hospital – Hendricks II Fall Risk Scale – John Hopkins Fall Risk Scale: used at the IU Health Hospitals

Morse Fall Scale Item 1. History of falling; immediate or within 3 months 2. Secondary diagnosis Scale Scoring No 0 Yes 25 No 0 Yes 15 ______ 3. Ambulatory aid Bed rest/nurse assist Crutches/cane/walker Furniture 0 15 30 4. IV/Heparin Lock No 0 Yes 20 5. Gait/Transferring Normal/bedrest/immobile Weak Impaired 6. Mental status Oriented to own ability Forgets limitations Risk Level No Risk MFS Score 0 - 24 Low Risk 25 - 50 High Risk ≥ 51 ______ 0 10 20 ______ 0 15 Action Good Basic Nursing Care Implement Standard Fall Prevention Interventions Implement High Risk Fall Prevention Interventions

Hendrick II Fall Risk Model Risk Factor (≥ 5 = High Risk) Risk Factor Risk Points Confusion/disorientation 4 Depression 2 Altered elimination 1 Dizziness/vertigo (subjective) 1 Gender (male) 1 Any prescribed anti-epileptics 2 Any prescribed benzodiazepines 1 Get-up-and-go “Rising from Chair” Able to rise in single movement Pushes up, successful in one attempt Multiple attempts but successful Unable to rise without assistance 0 1 3 4

Johns Hopkins Fall Risk Assessment Tool Complete the Following and Calculate Fall Risk Score Age (Single-Select) 60 -69 years (1 point) 70 -79 years (2 points) ≥ 80 years (3 points) Fall History (Single-Select) One fall within 6 months before admission (5 points) Elimination, Bowel and Urine (Single-Select) Incontinence (2 points) Urgency or frequency (2 points) Urgency/frequency and incontinence (4 points) Medications: Includes PCA/opiates, Anticonvulsants, Antihypertensives, Diuretics, Hypnotics, Laxatives, Sedatives, and Antipsychotics(Single-Select) On one high risk drug (3 points) On two or more high-risk drugs (5 points) Sedated procedure within last 24 hours (7 points)

Johns Hopkins Fall Risk Assessment Tool Complete the Following and Calculate Fall Risk Score Patient Care Equipment: Any equipment that tethers patient (e. g. IV infusion, chest tube, indwelling catheters, SCDs, etc. ) (Single-Select) One present (1 point) Two present (2 points) Three present (3 points) Mobility (multi-select, choose all that apply and add points together) Requires assistance or supervision for mobility, transfer, or ambulation (2 points) Unsteady gait (2 points) Visual or auditory or impairment affecting mobility (2 points) Cognition (Multi-select, choose all that apply and add points together) Altered awareness of immediate physical environment (1 point) Impulsive (2 points) Lack of understanding of one’s physical and cognitive limitations (4 points) Mod Risk: 6 -13 points High Risk >13 points Total Points _____

Automatic Fall Risk FALL RISK FACTOR CATEGORY Scoring not completed for the following reason(s) ( check any that apply): Complete paralysis, or completely immobilized. Implement basic safety (low fall risk) interventions. Patient has a history of more than one fall within six months before admission. Implement high fall risk interventions throughout hospitalization. Patient has experienced a fall during this hospitalization. Implement high fall risk interventions throughout hospitalization. Patient is deemed high fall risk per protocol (e. g. seizure precautions). Implement high fall risk interventions per protocol.

Assisted Fall • Always use a gait belt when assisting a patient to ambulate • If the patient begins to fall, gently assist in lowering them to the ground using the gait belt
Falls • Meeting the needs to prevent a fall. – Rounding – Call light – Urinal – Bedside commode – Bedside table – Night light – Trip hazards

Place care light with in reach

Fall Precautions Set bed alarm while patient is in bed
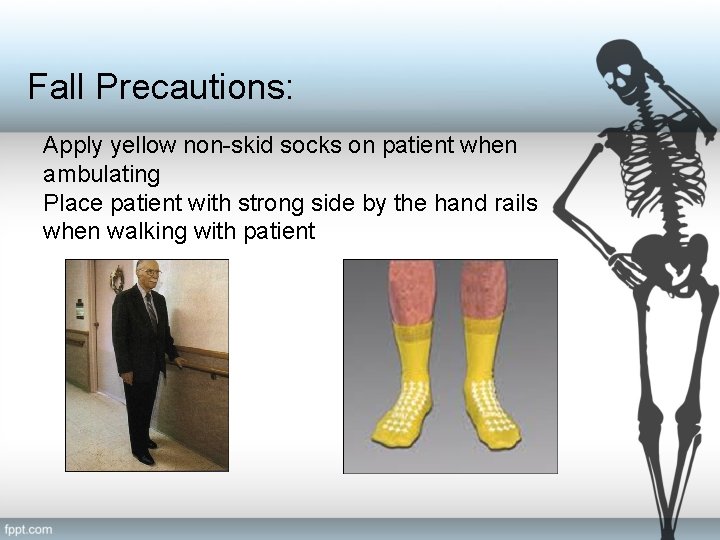
Fall Precautions: Apply yellow non-skid socks on patient when ambulating Place patient with strong side by the hand rails when walking with patient
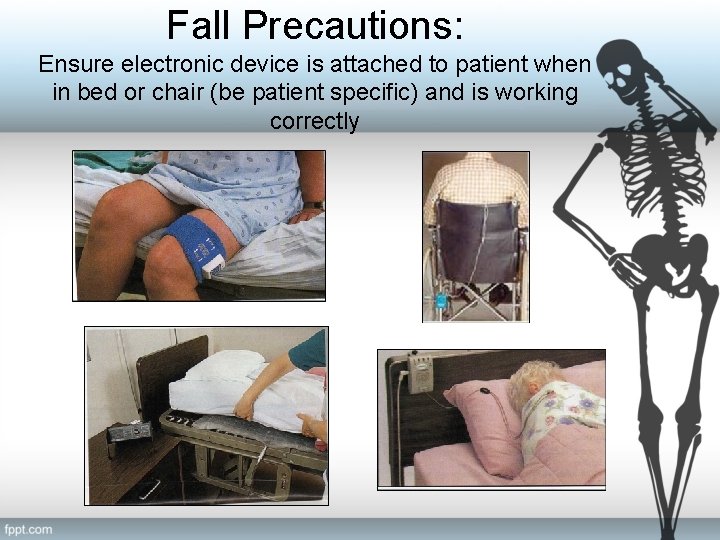
Fall Precautions: Ensure electronic device is attached to patient when in bed or chair (be patient specific) and is working correctly
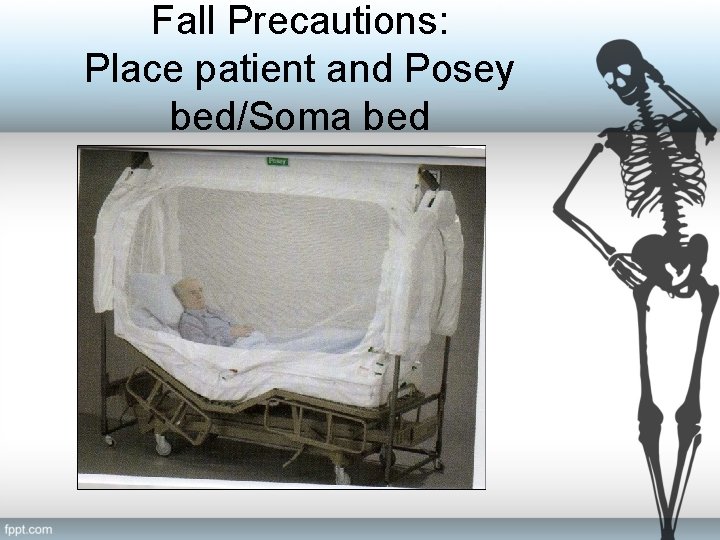
Fall Precautions: Place patient and Posey bed/Soma bed
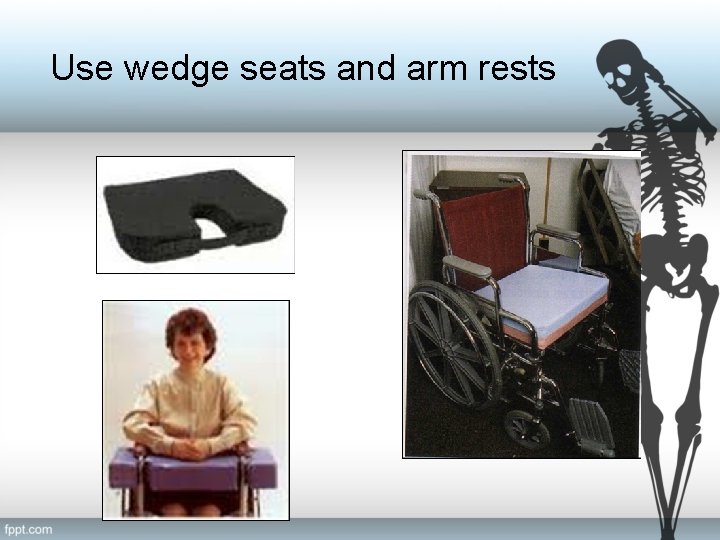
Use wedge seats and arm rests

Do Not Use 4 Side Rails
- Slides: 22